Published online Apr 26, 2026. doi: 10.12998/wjcc.v14.i12.118091
Revised: February 4, 2026
Accepted: March 19, 2026
Published online: April 26, 2026
Processing time: 112 Days and 8.5 Hours
Situs inversus totalis (SIT) is a rare congenital anomaly characterized by complete mirror-image transposition of thoracic and abdominal organs. The presence of gallstone disease in these patients represents a diagnostic and technical challenge, particularly when laparoscopic cholecystectomy is indicated.
We report two cases of symptomatic gallstone disease in patients with SIT. The first case involved a 27-year-old female diagnosed with cholelithiasis following radiological evaluation, while the second case involved a 45-year-old male pre
Laparoscopic cholecystectomy in patients with SIT is safe and feasible when meticulous preoperative imaging and careful adaptation of surgical technique are employed. Awareness of mirror-image anatomy and strict adherence to the critical view of safety are essential to minimize the risk of iatrogenic injury.
Core Tip: Situs inversus totalis is a rare anatomical condition that presents unique diagnostic and technical challenges during laparoscopic cholecystectomy. This case series emphasizes the importance of thorough preoperative imaging to clearly define biliary anatomy and identify any associated anomalies. It also highlights the need for careful adaptation of surgical technique, including mirror-image port placement and ergonomic adjustments by the surgical team. Strict adherence to the critical view of safety remains essential to minimize the risk of bile duct injury and to ensure safe, effective, and re
- Citation: Bhati G, Capolupo GT, Bhati K, Gupta A, Bansal R, Sai Srinija P, Caricato M, Carannante F. Laparoscopic cholecystectomy in patients with situs inversus totalis: Two case reports and review of literature. World J Clin Cases 2026; 14(12): 118091
- URL: https://www.wjgnet.com/2307-8960/full/v14/i12/118091.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i12.118091
Situs inversus totalis (SIT) is a rare congenital condition characterized by complete mirror-image transposition of both thoracic and abdominal organs[1]. Its reported incidence ranges from 1 in 5000 live births to 1 in 20000 live births[2]. Although the condition itself is usually asymptomatic, it may pose significant diagnostic and technical challenges when surgical intervention is required, particularly in minimally invasive procedures. In SIT, the heart and stomach are typically located on the right side of the midline, whereas the liver and gallbladder are positioned on the left[3]. In some patients, SIT may be associated with Kartagener syndrome, a subset of primary ciliary dyskinesia characterized by chronic sinusitis, bronchiectasis, and infertility[4]. Gallstone disease in patients with SIT is uncommon, and diagnosis may be delayed due to atypical symptom localization[5]. Advanced imaging modalities are therefore essential to ac
Case 1: Intermittent epigastric pain for one year.
Case 2: Intermittent colicky abdominal pain for six months.
Case 1: A 27-year-old female reported intermittent, dull, non-radiating epigastric pain relieved by medication, without associated gastrointestinal or systemic symptoms.
Case 2: A 45-year-old male reported intermittent colicky abdominal pain relieved by medication.
Both patients had no relevant past medical or surgical history.
No significant personal or family history was reported in either case.
Physical examination was unremarkable in both patients.
Case 1: Laboratory investigations revealed anemia with mild biochemical abnormalities; viral markers were negative (Table 1 and Figure 1).
| Investigations | Value | Normal range |
| Haemoglobin | 9.4 g/dL | 13.0-17.0 |
| TLC | 9.2 × 103/uL | 4.0-10.0 |
| RBS | 160 g/dL | 80.0-140.0 |
| Liver function tests | ||
| SGOT | 23 IU/L | 0.0-35.0 |
| SGPT | 27 IU/L | 0.0-41.0 |
| ALP | 83 IU/L | 40.0-129.0 |
| Albumin | 3.2 g/dL | 3.5-5.2 |
| Bilirubin | 1.4 mg/dL | 0.1-1.2 |
| Renal function tests | ||
| Serum urea | 27 mg/dL | 17.0-43.0 |
| Serum creatinine | 1.2 mg/dL | 0.6-1.1 |
| Serum Na+ | 135 mmol/L | 136.0-145.0 |
| Serum K+ | 4.2 mmol/L | 3.5-5.0 |
| Viral markers | ||
| HCV | Non-reactive | |
| HBsAg | Non-reactive | |
| HIV | Non-reactive | |
Case 2: Laboratory tests showed elevated bilirubin and alkaline phosphatase levels (Table 1 and Figure 1).
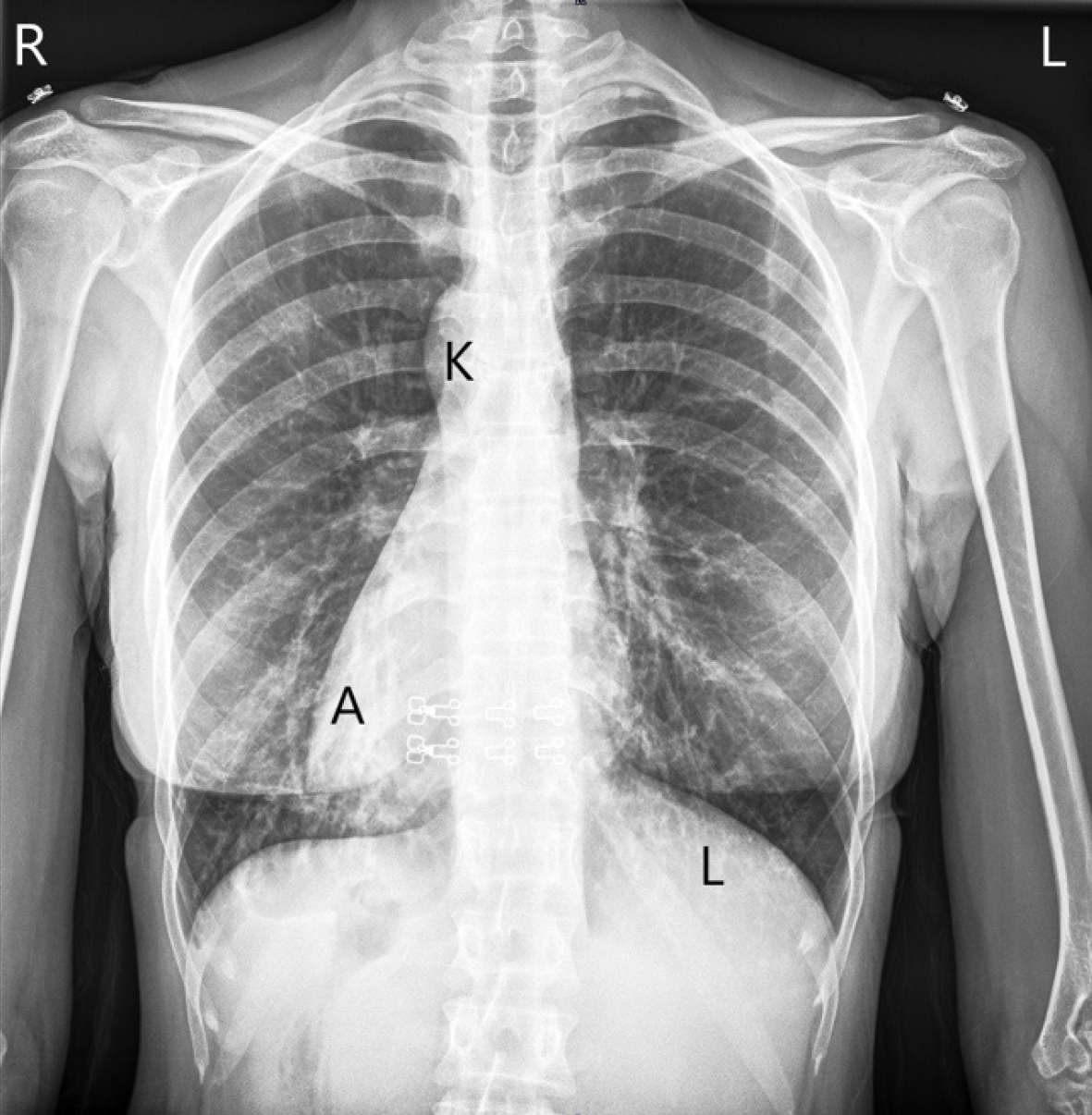
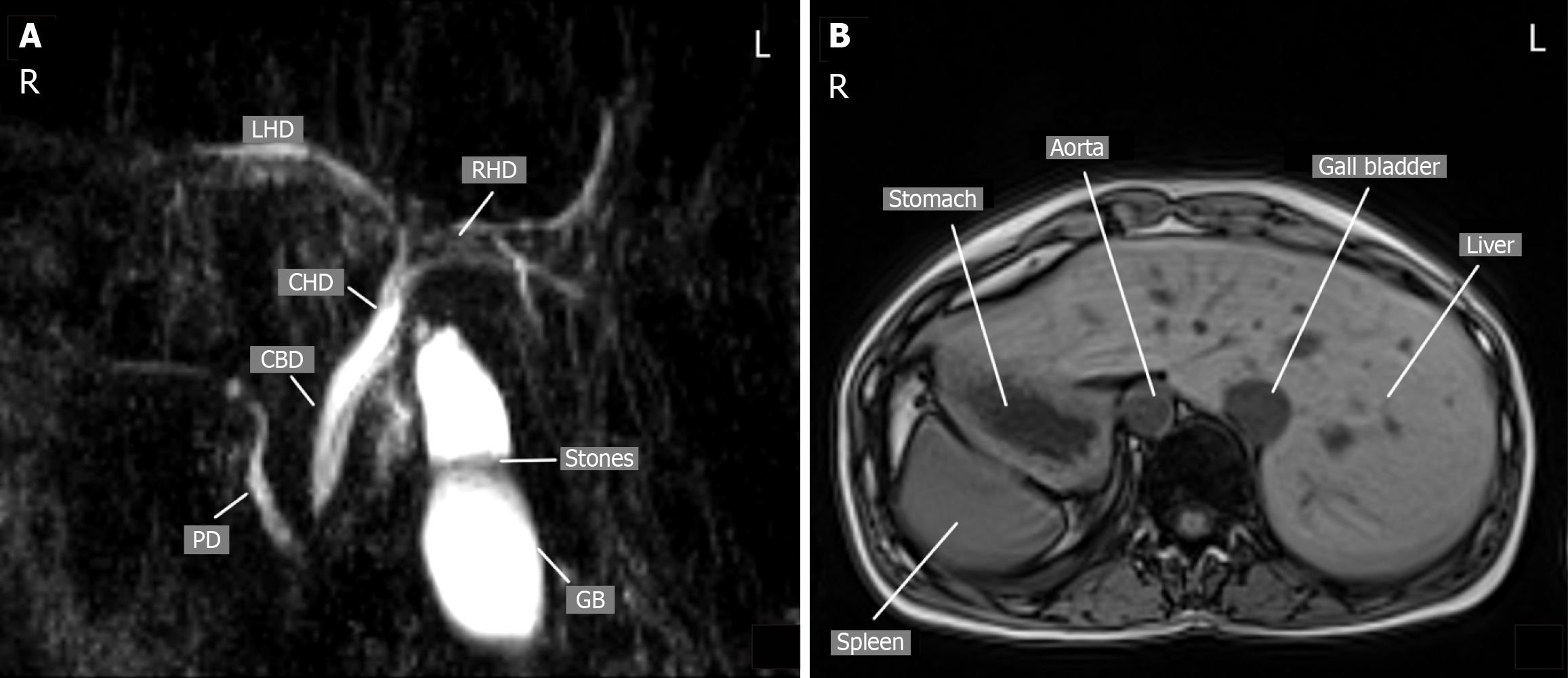
Case 1: Chest radiography demonstrated dextrocardia. Abdominal ultrasonography and magnetic resonance cholangiopancreatography confirmed cholelithiasis and SIT (Figure 2).
Case 2: Abdominal ultrasonography revealed gallstones and distal common bile duct calculi. Imaging confirmed SIT (Figure 3).
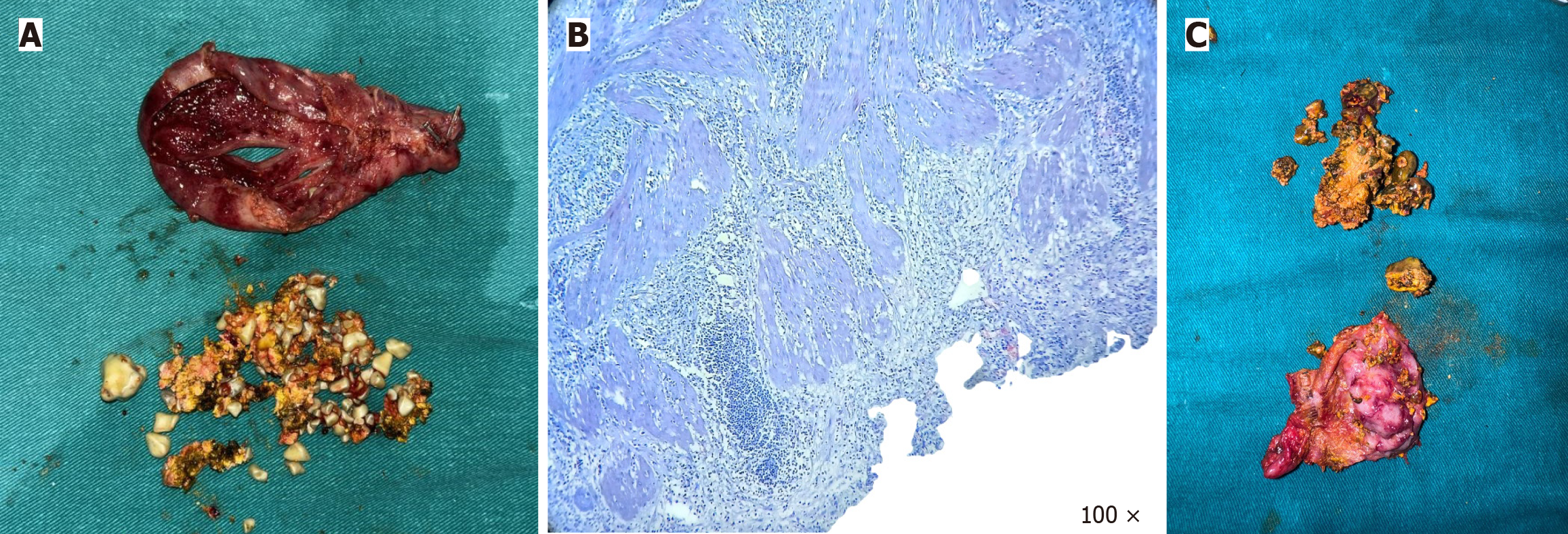
Symptomatic cholelithiasis in SIT (case 1) and cholelithiasis with choledocholithiasis in SIT (case 2) (Figure 4).
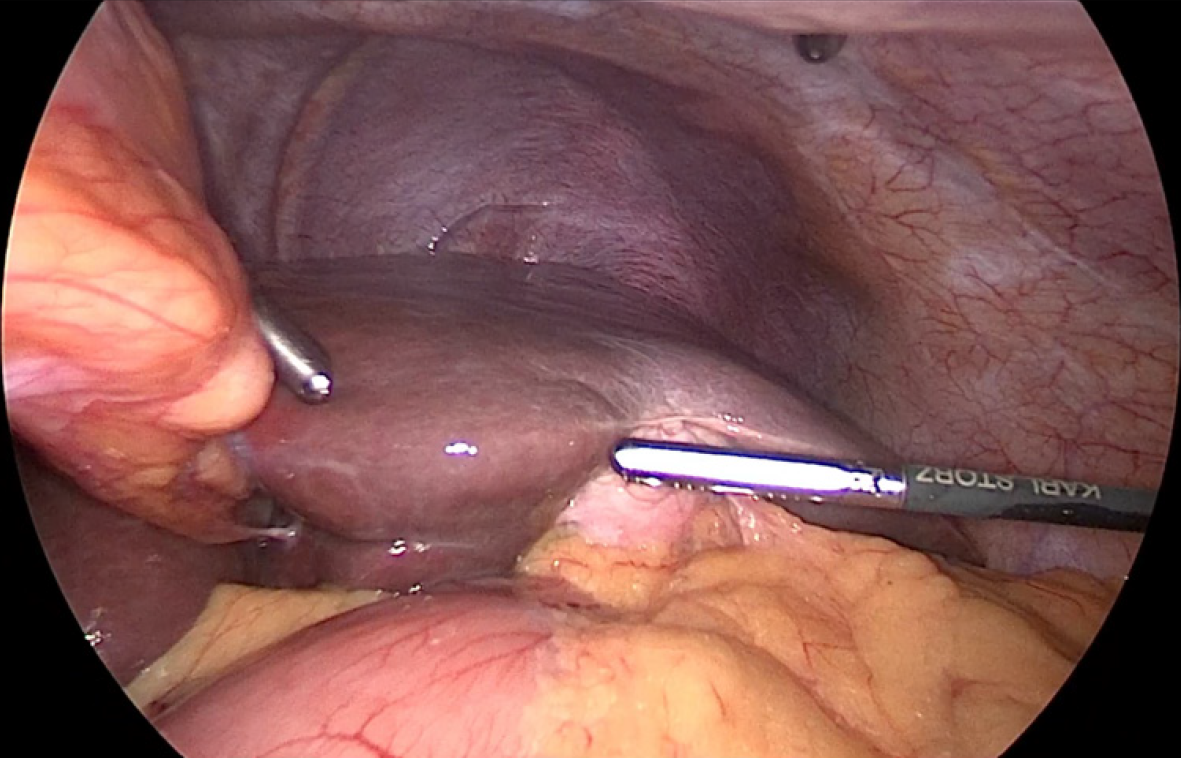
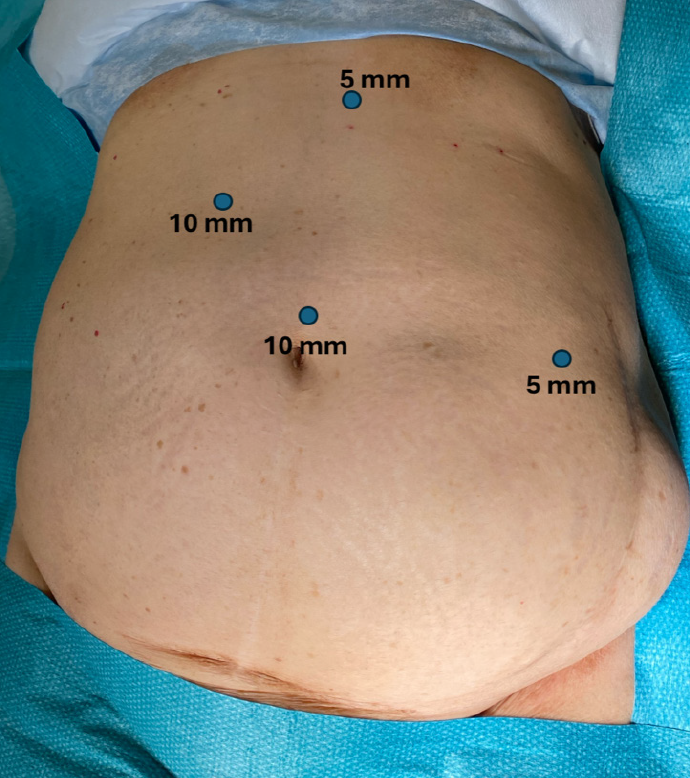
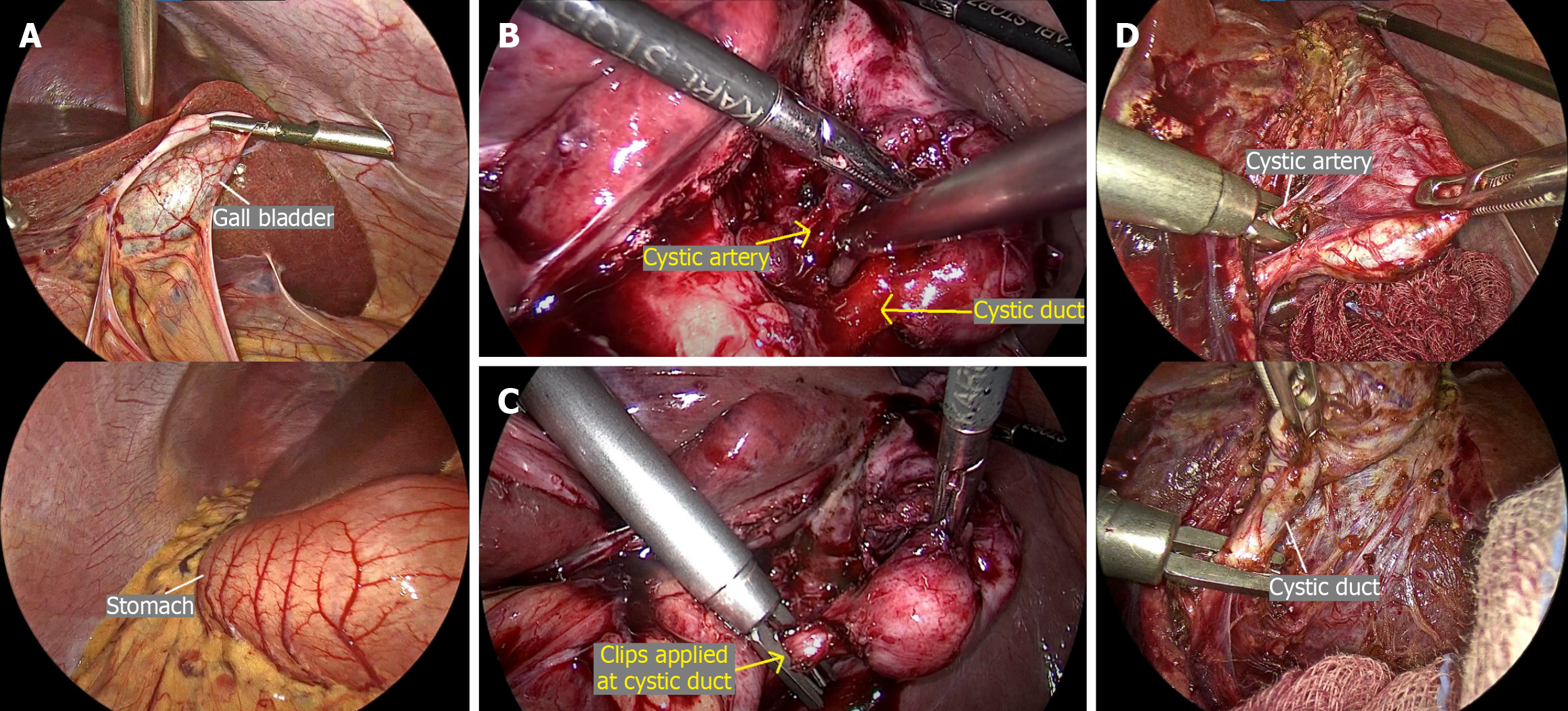
Both patients underwent elective laparoscopic cholecystectomy using a mirror-image four-port configuration (Figure 5). In both cases, the critical view of safety was achieved prior to division of the cystic duct and artery. Intraoperative findings confirmed left-sided gallbladder anatomy (Figure 6A). Dissection was carried out with careful orientation to Rouvier’s sulcus, and the critical view of safety was achieved before division of the cystic duct and artery (Figure 6B and C). The gallbladder was retrieved through the epigastric port (Figure 6D).
Both patients had an uneventful postoperative course and were discharged on postoperative day one. Clinical follow-up at 30 days and 6 months revealed no complications or recurrent biliary symptoms.
SIT results from abnormal left-right axis determination during early embryogenesis. Although the exact mechanisms remain incompletely understood, disruptions in molecular signaling pathways during gastrulation have been implicated. Unlike intestinal malrotation, SIT involves a complete mirror-image arrangement of thoracic and abdominal organs without rotational anomalies of foregut-derived structures. The prevalence of gallstone disease in patients with SIT appears comparable to that of the general population; however, clinical presentation is often atypical, with pain localized to the left upper quadrant or epigastrium. This may lead to diagnostic delay unless a high index of suspicion is main
Since the first report of laparoscopic cholecystectomy in SIT in 1991[8], more than 40 cases have been described in the literature, with an increasing number reported in recent years. Cumulative evidence consistently demonstrates that laparoscopic cholecystectomy is safe and feasible in this setting, with low complication rates and favorable postoperative outcomes. The primary technical challenge arises from mirror-image anatomy, which affects surgeon orientation, port placement, and hand dominance. Most authors advocate a mirrored four-port configuration that preserves triangulation and ergonomic principles. Surgeon positioning varies among reports, and no single approach has proven superior; therefore, operative strategy should be tailored to surgeon experience and institutional practice[9,10]. Achievement of the critical view of safety remains the cornerstone of safe cholecystectomy in SIT. Meticulous dissection and unequivocal identification of the cystic duct and artery are mandatory to prevent bile duct injury. Selective use of intraoperative cholangiography may be considered in cases with unclear anatomy or associated choledocholithiasis. Although al
| Ref. | Age (in years) and sex | Symptoms | Diagnoses | Treatment |
| AlKhlaiwy et al[3], 2019 | 40, male | Epigastric and left upper quadrant pain for 1 month, associated with intermittent nausea and vomiting | Cholelithiasis | Laparoscopic cholecystectomy |
| Ponce et al[13], 2020 | 61, female | Colic abdominal pain, with predominance of it in the left upper quadrant, associated with nausea, of weekly frequency | Cholelithiasis | Laparoscopic cholecystectomy |
| Du et al[14], 2020 | 56, female | Nausea, severe chest pain, and epigastric pain | Cholelithiasis | Laparoscopic cholecystectomy |
| Lakhey et al[10], 2025 | 30, female | Colicky abdominal pain located over the epigastric and left hypochondrium regions | Cholelithiasis | Laparoscopic cholecystectomy |
| Jhobta et al[15], 2018 | 23.female | Intermittent left upper abdomen discomfort and dyspepsia | Cholelithiasis | Laparoscopic cholecystectomy |
| Jang et al[16], 2019 | 37, male | Persistent indigestion | Chronic cholecystitis with gallstones | Laparoscopic cholecystectomy |
| Sheik-Ali et al[17], 2019 | 57, female | Epigastric pain | Acute cholecystitis | Laparoscopic cholecystectomy |
| Mohammed and Arif[18], 2019 | 28, male | Epigastric pain and left hypochondrial pain | Cholelithiasis | Laparoscopic cholecystectomy |
| Hernández-Marín and Guevara-Valerio[19], 2020 | 66, male | Epigastric pain | Cholelithiasis | Laparoscopic cholecystectomy |
| Herrera Ortiz et al[20], 2021 | 46, female | Non-bilious vomiting and left-sided abdominal pain | Symptomatic cholelithiasis | Laparoscopic cholecystectomy |
| Garnica-Rosales et al[21], 2021 | 26, female | Sudden, intense abdominal pain in the left hypochondrium | Cholelithiasis | Laparoscopic cholecystectomy |
| Meng et al[22], 2022 | 32, male | Left upper abdominal pain | Chronic cholecystitis | Laparoscopic cholecystectomy |
| He et al[23], 2022 | 53, female | Intermittent left upper abdominal pain | Cholelithiasis | Laparoscopic cholecystectomy |
| Montalvo-Javé et al[24], 2022 | 44, female | Colicky epigastric pain that radiated to the right scapula | Cholelithiasis | Laparoscopic cholecystectomy |
| Suleimanov et al[25], 2022 | 38, female | Left upper abdominal and epigastric pain and nausea | Cholelithiasis | Laparoscopic cholecystectomy |
| Abu-Oddos et al[26], 2023 | 24, male | Epigastric pain | Cholelithiasis | Laparoscopic cholecystectomy |
| M et al, 2023[27] | Middle-aged male | Pain in the left hypochondrium | Cholelithiasis | Laparoscopic cholecystectomy |
| Raut et al[28], 2023 | 38, male | Backache and vomiting | Cholelithiasis | Laparoscopic cholecystectomy |
| Nguyen et al[29], 2024 | 33, female | Episodic left upper quadrant pain and diffuse epigastric pain | Cholelithiasis | Laparoscopic cholecystectomy |
| Nassr et al[30], 2024 | 34, female | Left upper quadrant pain | Cholelithiasis | Laparoscopic cholecystectomy |
| Althunayan et al[31], 2024 | 40, female | Pain was located in LUQ, radiating to the back, associated with vomiting | Cholelithiasis | Laparoscopic cholecystectomy |
| Cunningham et al[32], 2024 | 54, male | Epigastric pain, dysphagia, and weight loss | Cholelithiasis | Laparoscopic cholecystectomy |
| Abdullah et al[33], 2025 | 52, male | Intermittent left upper quadrant abdominal pain | Cholelithiasis | Laparoscopic cholecystectomy |
| Vázquez-Guerra et al[34], 2025 | 49, female | Repetitive postprandial colic pain in the epigastrium | Acute calculus cholecystitis | Laparoscopic cholecystectomy |
| Li et al[35], 2025 | 67, female | Abdominal pain | Cholecystolithiasis | Laparoscopic cholecystectomy |
| Wu et al[36], 2025 | 73, female | Epigastric pain | FGBD and potential gallbladder ectopia | Laparoscopic cholecystectomy |
Laparoscopic cholecystectomy in patients with SIT is safe and feasible when supported by thorough preoperative imaging and careful adaptation of surgical technique. Awareness of mirror-image anatomy, appropriate port placement, and strict adherence to the critical view of safety are essential to achieving favorable outcomes and minimizing iatrogenic injury.
| 1. | Wood GO. Situs inversus totalis and disease of the biliary tract. Arch Surg. 1940;40:885. [DOI] [Full Text] |
| 2. | Ren JJ, Li SD, Geng YJ, Xiao R. Modified laparoscopic cholecystectomy technique for treatment of situs inversus totalis: A case report. J Int Med Res. 2017;45:1261-1267. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 13] [Article Influence: 1.4] [Reference Citation Analysis (1)] |
| 3. | AlKhlaiwy O, AlMuhsin AM, Zakarneh E, Taha MY. Laparoscopic cholecystectomy in situs inversus totalis: Case report with review of techniques. Int J Surg Case Rep. 2019;59:208-212. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 24] [Article Influence: 3.4] [Reference Citation Analysis (1)] |
| 4. | Eitler K, Bibok A, Telkes G. Situs Inversus Totalis: A Clinical Review. Int J Gen Med. 2022;15:2437-2449. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 179] [Cited by in RCA: 137] [Article Influence: 34.3] [Reference Citation Analysis (2)] |
| 5. | Leigh MW, Pittman JE, Carson JL, Ferkol TW, Dell SD, Davis SD, Knowles MR, Zariwala MA. Clinical and genetic aspects of primary ciliary dyskinesia/Kartagener syndrome. Genet Med. 2009;11:473-487. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 372] [Cited by in RCA: 300] [Article Influence: 17.6] [Reference Citation Analysis (0)] |
| 6. | Takeda T, Haraguchi N, Yamaguchi A, Uemura M, Miyake M, Miyazaki M, Ikeda M, Sekimoto M. Laparoscopic sigmoidectomy in a case of sigmoid colon cancer with situs inversus totalis. Asian J Endosc Surg. 2019;12:111-113. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 17] [Article Influence: 2.4] [Reference Citation Analysis (1)] |
| 7. | Adams SD, Stanton MP. Malrotation and intestinal atresias. Early Hum Dev. 2014;90:921-925. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 85] [Cited by in RCA: 100] [Article Influence: 8.3] [Reference Citation Analysis (1)] |
| 8. | Campos L, Sipes E. Laparoscopic cholecystectomy in a 39-year-old female with situs inversus. J Laparoendosc Surg. 1991;1:123-5; discussion 126. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 56] [Article Influence: 1.6] [Reference Citation Analysis (1)] |
| 9. | Yaghan RJ, Gharaibeh KI, Hammori S. Feasibility of laparoscopic cholecystectomy in situs inversus. J Laparoendosc Adv Surg Tech A. 2001;11:233-237. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 38] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 10. | Lakhey P, Shrestha M, Sharma R, Lakhey PJ. Laparoscopic Cholecystectomy in Situs Inversus Totalis: A Case Report. Clin Case Rep. 2025;13:e70222. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 11. | Ozsoy M, Haskaraca MF, Terzioglu A. Single incision laparoscopic cholecystectomy (SILS) for a patient with situs inversus totalis. BMJ Case Rep. 2011;2011:bcr0820114581. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 0.4] [Reference Citation Analysis (1)] |
| 12. | Han HJ, Choi SB, Kim CY, Kim WB, Song TJ, Choi SY. Single-incision multiport laparoscopic cholecystectomy for a patient with situs inversus totalis: report of a case. Surg Today. 2011;41:877-880. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 19] [Article Influence: 1.3] [Reference Citation Analysis (1)] |
| 13. | Ponce Leon F, Fiorencio MH, Leal CP, Santos AR. Laparoscopic cholecystectomy in a patient with situs inversus totalis after videolaparoscopic sleeve-Case report. Int J Surg Case Rep. 2020;71:202-204. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 14. | Du T, Hawasli A, Summe K, Meguid AA, Lai C, Sadoun M. Laparoscopic Cholecystectomy in a Patient with Situs Inversus Totalis: Port Placement and Dissection Techniques. Am J Case Rep. 2020;21:e924896. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (1)] |
| 15. | Jhobta RS, Gupta A, Negi B, Negi K. Single-incision laparoscopic cholecystectomy using conventional instruments in situs inversus totalis. BMJ Case Rep. 2018;11:e226404. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (1)] |
| 16. | Jang EJ, Roh YH. Single Port Laparoscopic Cholecystectomy in a Patient with Situs Inversus Totalis: A Case Report. J Minim Invasive Surg. 2019;22:81-84. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 3] [Article Influence: 0.4] [Reference Citation Analysis (1)] |
| 17. | Sheik-Ali S, Appleton S, Ojukwu N, Sheik-Ali S. Acute cholecystitis in a patient with heterotaxic anatomy and partial situs inversus. Ann R Coll Surg Engl. 2019;101:e169-e171. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 6] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 18. | Mohammed AA, Arif SH. Laparoscopic cholecystectomy for left-sided gall bladder in situs inversus totalis patient, a technically demanding procedure. Ann Med Surg (Lond). 2019;47:1-4. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 8] [Article Influence: 1.1] [Reference Citation Analysis (1)] |
| 19. | Hernández-Marín JD, Guevara-Valerio H. Consideraciones técnicas para colecistectomía laparoscópica en paciente con situs inversus totalis: presentación de caso y revisión de la literatura. Cir Cir. 2020;88:5-8. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 20. | Herrera Ortiz AF, Lacouture JC, Sandoval Medina D, Gómez Meléndez LJ, Uscategui R. Acute Cholecystitis in a Patient With Situs Inversus Totalis: An Unexpected Finding. Cureus. 2021;13:e15799. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 10] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 21. | Garnica-Rosales AU, Martínez-Valdés JA, Villalpando-Velázquez JA, Lagunas-Quiroz E. Acute cholecystitis in a situs inversus totalis. Case report. Cir Cir. 2021;89:28-32. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 22. | Meng Y, Guo H, Peng J, Zhang X, Yang X. Modified laparoscopic cholecystectomy for cholecystolithiasis with situs inversus totalis: A case report. Asian J Surg. 2022;45:978-979. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 0.5] [Reference Citation Analysis (1)] |
| 23. | He T, Zou J, Song H, Yi B, Sun K, Yang J, Lei T, Xu L, Li G. Laparoscopic Cholecystectomy in a Patient With Situs Inversus Totalis Presenting With Cholelithiasis: A Case Report. Front Surg. 2022;9:874494. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (1)] |
| 24. | Montalvo-Javé EE, Arroyo-Paredes PS, Corona-Torres MJ, Rodríguez-Báez A. Laparoscopic cholecystectomy in a patient with situs inversus totalis. Rev Gastroenterol Mex (Engl Ed). 2022;87:486-488. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 25. | Suleimanov V, Al Asker H, Al Hawaj K, Alhashim IW, Al Rebh FN. Laparoscopic Cholecystectomy in a Morbidly Obese Patient With Situs Inversus Totalis: A Case Report. Cureus. 2022;14:e32304. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 26. | Abu-Oddos N, Abu-Jeyyab M, Al Mse'adeen M, Rawshdeh A, Al-Jafari M, Abu-Oddos SI, Shahin M, Rawashdeh B. Laparoscopic Cholecystectomy in a Patient with Situs Inversus Totalis and a Double Superior Vena Cava. Am J Case Rep. 2023;24:e938774. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 27. | M VB, Vaddavalli VV, Abuji K, Palle P, Ramavath K. Two Surgeons' Technique for Laparoscopic Cholecystectomy in Situs Inversus for a Right-Handed Surgeon: Technical and Ergonomic Considerations. Cureus. 2023;15:e38161. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 28. | Raut S, Limbu Y, Pudasaini P, Gongal S, Maharjan DK. Laparoscopic Cholecystectomy in Situs Inversus Totalis with Stage 5 Chronic Kidney Disease: A Case Report. JNMA J Nepal Med Assoc. 2023;61:893-896. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 29. | Nguyen C, Schutter D. Adaptability in the Midst of Anatomical Challenges: A Case of Situs Inversus Totalis in Laparoscopic Cholecystectomy. Cureus. 2024;16:e58770. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 30. | Nassr B, Nassr H, Allouzi A, Abdalla A, Shaheen T, Alkhatabi A, Alkhatabi O. Reversing the Norm: Successful Cholecystectomy in a Patient With Situs Inversus. Cureus. 2024;16:e59957. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 31. | Althunayan SA, AlRubaysh NS, Alshaban JA, Ali SO. Acute Cholecystitis in a Patient With Situs Inversus. Cureus. 2024;16:e60172. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 32. | Cunningham B, Blades D, McArdle G. Laparoscopic cholecystectomy in situs inversus totalis-surgical technique and procedure safety using anatomical checkpoints. J Surg Case Rep. 2024;2024:rjae450. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 33. | Abdullah HS, Alomar TH, Alamri RS, Alalawi AA. Gallstones in a Looking-Glass: A Case Report on the Successful Laparoscopic Management of Cholelithiasis in Situs Inversus Totalis. Cureus. 2024;16:e67734. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 34. | Vázquez-Guerra XC, Rosales-Isais JA, Hernandez-Garza VI, Valdivia-Balderas JM, Alvarez-Lozada LA, Quiroga-Garza A. Intraoperative Diagnosis of Situs Inversus Totalis in Laparoscopic Cholecystectomy: Taking Into Consideration Patient-Centered Care in a Limited-Resource Case. Cureus. 2025;17:e78501. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 35. | Li Z, Ouyang Y, Ding K. Single-Incision Laparoscopic Cholecystectomy in Situs Inversus Totalis: A Case Report. Am J Case Rep. 2025;26:e946523. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 36. | Wu JR, Wang CC, Li BY, Li JH, Zhang T, Li ZY. Concomitant functional gallbladder disorder and left-sided gallbladder: A case report. World J Gastrointest Endosc. 2025;17:107059. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |