Published online Apr 26, 2026. doi: 10.12998/wjcc.v14.i12.117790
Revised: January 19, 2026
Accepted: March 19, 2026
Published online: April 26, 2026
Processing time: 118 Days and 16.7 Hours
Hepatic tuberculosis is rare, and is difficult to diagnose in the early stage of the disease. It is easily masked by the symptoms of pulmonary tuberculosis or other types of tuberculosis, and is often misdiagnosed as hepatitis, liver cancer or liver abscess. At present, there is a lack of relevant epidemiological statistics on the incidence of liver tuberculosis. However, the incidence of liver tuberculosis worldwide is approximately 3.5% of extrapulmonary tuberculosis.
A 52-year-old male patient underwent laparoscopic partial hepatectomy with release of intestinal adhesions due to hepatic tuberculosis. Prior to surgery, the patient had a past history of pulmonary tuberculosis, which was currently con
The specificity and sensitivity of laboratory tests for hepatic tuberculosis are low. Hepatic tuberculosis is difficult to distinguish from fatty liver, viral hepatitis and liver cancer.
Core Tip: We report a patient with hepatic tuberculosis who underwent laparoscopic partial hepatectomy. Following surgery, the patient’s symptoms of fever and abdominal pain were significantly improved.
- Citation: Jing GX, He JY, Gu GQ. Laparoscopic partial hepatectomy for the treatment of hepatic tuberculosis: A case report. World J Clin Cases 2026; 14(12): 117790
- URL: https://www.wjgnet.com/2307-8960/full/v14/i12/117790.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i12.117790
When the normal immune system of the human body is destroyed due to large doses of glucocorticoids, severe viral infection or human immunodeficiency virus, etc., this may result in low immunity and, such as the use of large doses of glucocorticoids, severe viral infection, and the attack of human immunodeficiency virus, etc., then Mycobacterium tuberculosis can pass through the intestine, stomach, lymphatic vessels, etc., via the blood stream, or due to lymph nodes near the portal vein being ruptured by external causes. This allows Mycobacterium tuberculosis to successfully enter the liver and bile system, and cause liver disease[1,2]. The main reason for the occurrence of secondary liver tuberculosis is reduced immunity. At present, there are few reports on laparoscopic partial hepatectomy for hepatic tuberculosis.
The patient was a 52-year-old woman with the main symptoms of low-grade fever, abdominal pain, low-grade fever, and night sweats.
The patient developed pain in the right upper quadrant of the abdomen without obvious inducement 20 days previously. The pain was intermittent and dull, lasting approximately 2 hours each time, but was tolerable. This was accompanied by low fever and night sweats. Maximum body temperature was 38.3 °C. The patient was diagnosed and treated in Mianyang Central Hospital, and no significant improvement was observed after antibiotic treatment.
The patient was diagnosed with tuberculous peritonitis in a local hospital one year ago. He received long-term isoniazid and rifampicin. No reexamination was carried out.
The patient had no special medical history and no significant family history.
On physical examination, the patient was conscious and cooperative. The abdomen was soft, with mild tenderness in the right upper quadrant, and there was no obvious rebound or muscle tension.
Laboratory tests showed the following: Hemoglobin 131 g/L, white blood cell count 6460/μL; platelet count 272 × 109/L; high-sensitivity C-reactive protein 35.79 mg/L; procalcitonin 0.060 ng/mL; albumin 39.9 g/L; prealbumin 112 mg/L. Preoperative tuberculin antibody test, purified protein derivative of tuberculin (PPD) skin test, acid fast staining of sputum smear and sputum culture were negative.
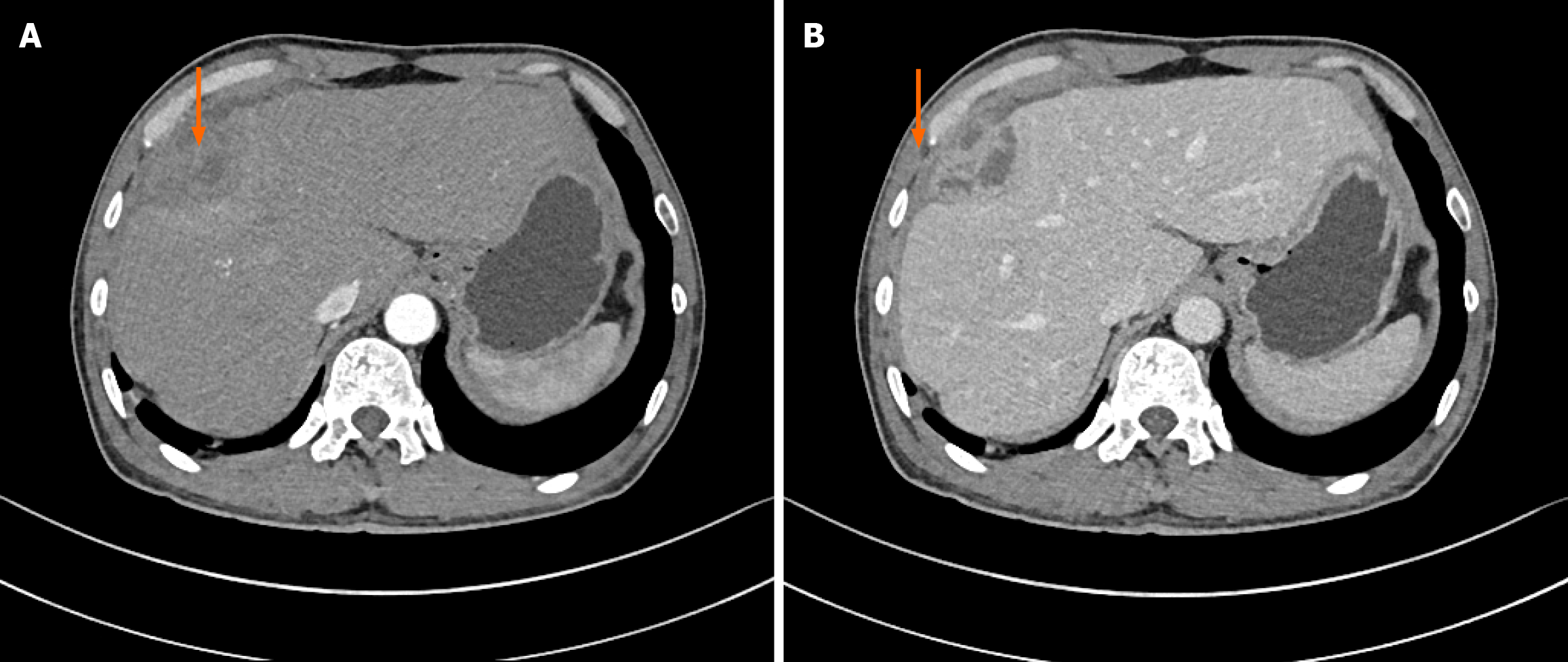
Abdominal enhanced computed tomography (CT) showed that the medial segment of the left lobe of the liver was clumpy with a slightly low density shadow, an unclear boundary with the surrounding area, uneven internal density, the lesion was approximately 6.4 cm × 3.7 cm in size with a thick wall, uneven continuous circular medium enhancement on the enhanced scan, and a nodular enhancement shadow in the arterial phase. A small amount of perihepatic effusion and slight thickening of adjacent peritoneum were observed (Figure 1). The middle hepatic veins and major hepatic arteries were not invaded by the tumor.
Liver tuberculosis.
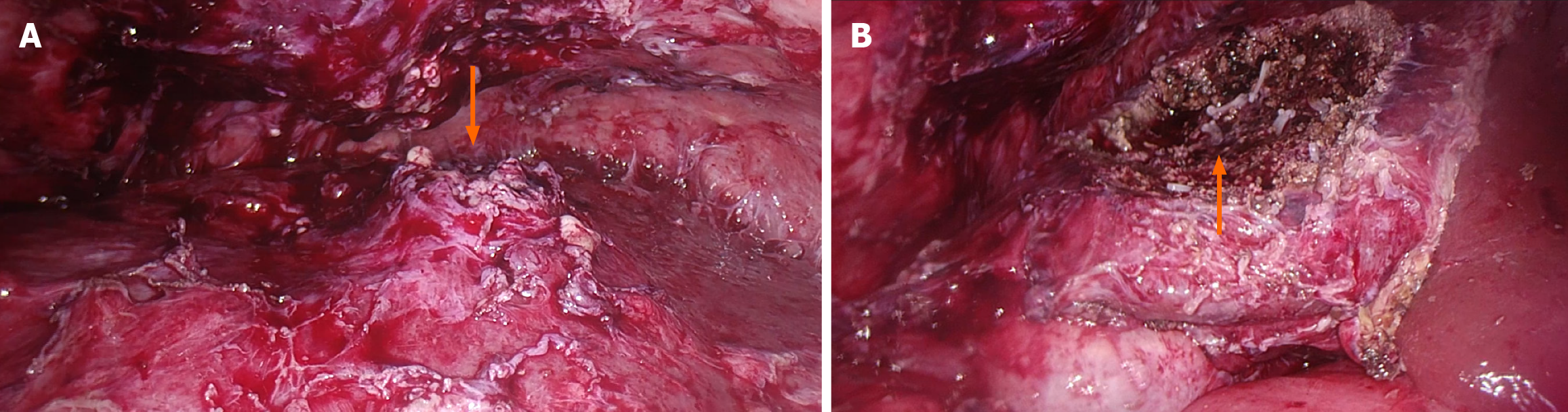
The relevant auxiliary examinations were completed before surgery. Intraoperative ultrasonography again confirmed a hard mass with a diameter of 4 cm × 4 cm and poor mobility in the medial left lobe of the liver. Laparoscopic partial hepatectomy was performed without vascular anastomosis and hepaticojejunostomy. The operation was successfully performed without blood transfusion (Figure 2). The operation time was 207 minutes, and the estimated blood loss was less than 50 mL.
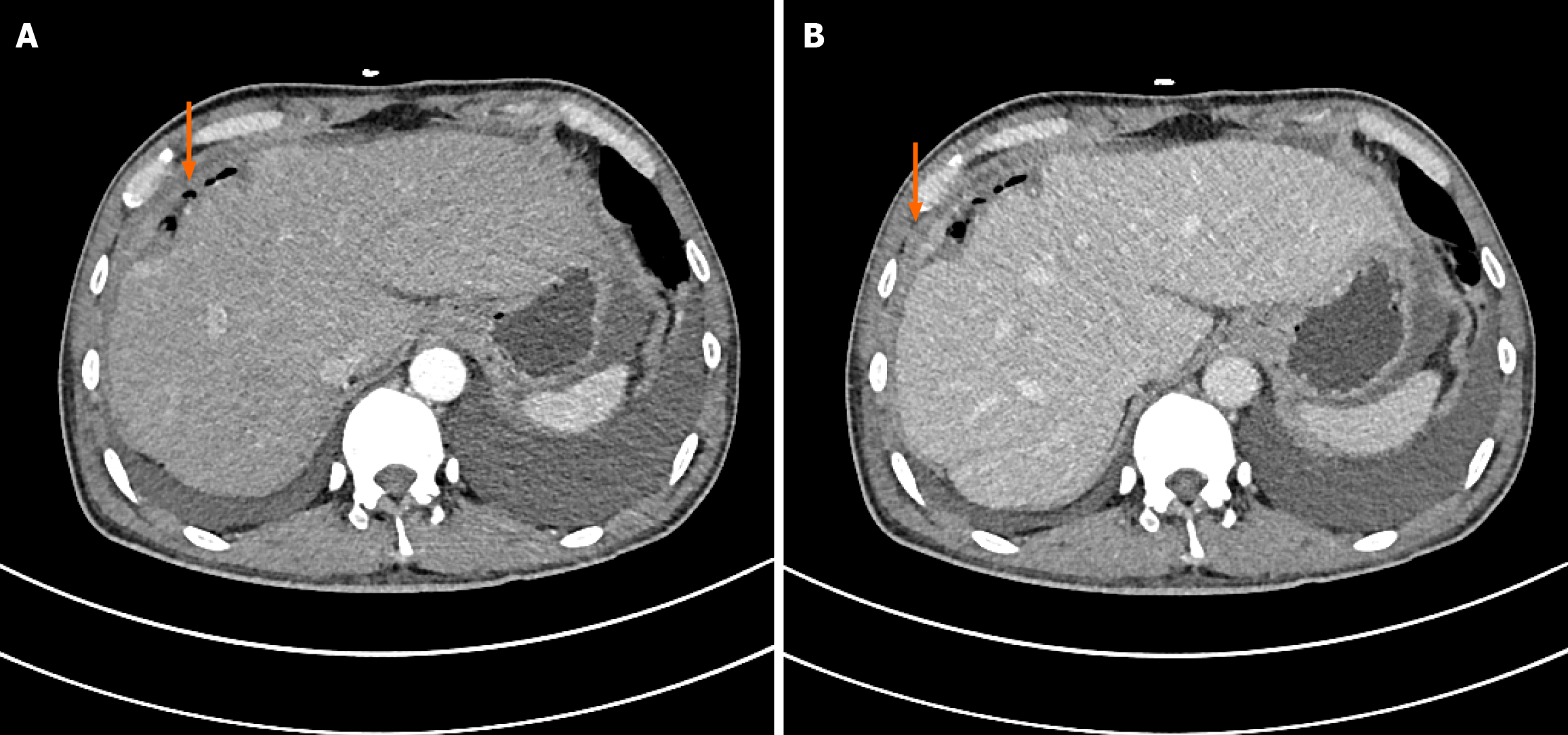
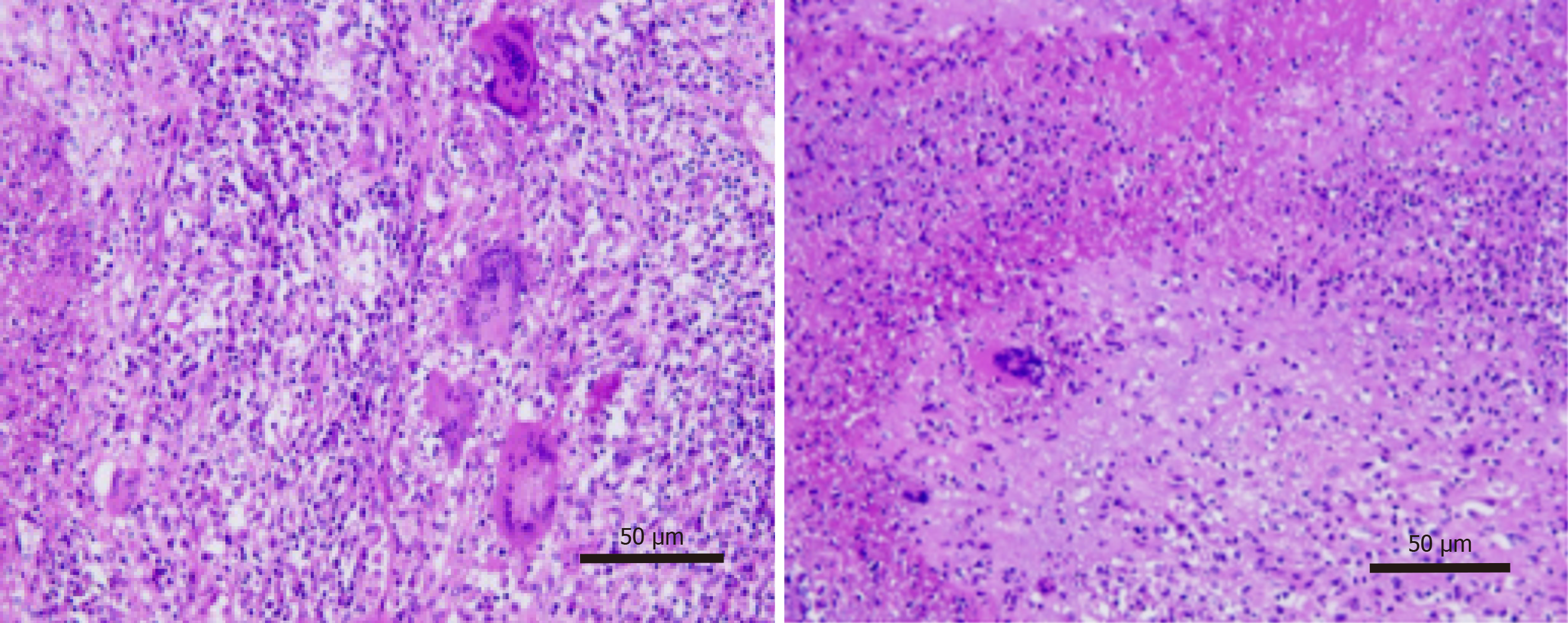
Ostoperative laboratory tests showed that the patient’s liver function and coagulation function were only mildly abnormal: Albumin 30.6 g/L; aspartate aminotransferase 159 U/L; plasma prothrombin time 13.3 seconds; prothrombin time activity 65.1%. The patient was discharged six days after surgery, and no recurrence or metastasis was observed during follow-up 1 month, 3 months, and 6 months after surgery (Figures 3 and 4).
Hepatic tuberculosis is a mycobacterial infection that can occur secondary to tuberculosis due to bile inhibition and liver immune dysfunction. Liver tuberculosis is often occult, and can be divided into nodular type, miliary type and tuberculoma type. Miliary type is the most common type. Hepatoduodenal ligament lymph node tuberculosis is an abdominal lymph node tuberculosis, which can be spread by the blood, lymphatic tract or direct invasion of neighboring organs. Hepatic tuberculosis and hepatoduodenal ligament lymph node tuberculosis can clinically manifest as fever, fatigue, night sweats and other symptoms, and laboratory tests can show accelerated sedimentation rate and positive tuberculin test, but these tests are not specific; thus, the diagnosis is difficult[3].
Liver tuberculosis is very rare and usually occurs due to tuberculosis spread via the hepatic artery or intestinal tuberculosis spread via the portal vein[4].
At present, the classification of hepatic tuberculosis is confusing. Levine classified hepatic tuberculosis into miliary tuberculosis, cumulative pulmonary tuberculosis, primary hepatic tuberculosis, focal tuberculoma or abscess, and tuberculous cholangitis[5]. Shekhar divided liver tuberculosis into common miliary type-related liver tuberculosis, primary miliary type liver tuberculosis, primary liver tuberculosis tumor or abscess, and 50%-80% of liver tuberculosis is common miliary type, while the proportion of primary liver tuberculosis is less than 1%. Common miliary type is spread by Mycobacterium tuberculosis via the hepatic artery, while primary liver tuberculosis is often formed via the portal vein. Hilar vein blood oxygen is low, which is one of the reasons why primary liver tuberculosis is rare[6].
The basic pathological changes in hepatic tuberculosis are chronic granulomatous inflammation, which can be manifested as caseous necrosis, liquefaction necrosis, fibrosis and calcification at different pathological stages. In these different pathological states, the imaging features of liver tuberculosis are different[7,8]. Liver tuberculosis is divided into diffuse type, mass type, abscess type and calcification type by ultrasound, and the diffuse type is characterized by diffuse hyperechoic lesions. The pathological features of mass type are chronic granuloma and caseous necrosis. The ultrasound images show low echoic lesions, a clear boundary and uneven internal echoes. The pathology of abscess type is li
Although the diagnosis of primary hepatic tuberculosis is difficult, attention should be paid to the following conditions: Young patients with chronic low fever, wasting, anemia, and hypoproteinemia; Patients with a history of tuberculosis; Color ultrasound/CT/magnetic resonance imaging indicated that the infection was accompanied by scattered internal calcification[11,12]. Tuberculosis antibody detection, PPD, acid fast staining of sputum smear and sputum culture should be performed for the above patients. If the results of the above tests are negative, a puncture biopsy of the mass is required, and when the diagnosis is confirmed, medical treatment is required[13]. A liver puncture biopsy provides a definite diagnosis of the liver nodules. If puncture biopsy fails to confirm the diagnosis or a malignant mass is suspected, laparoscopic exploration can be performed[14]. If an abscess is found, incision and drainage and tissue biopsy are required. If a solid mass is present, a partial hepatectomy is performed and a rapid intraoperative pathologic examination is necessary to determine whether lymph node dissection should be performed. Anti-tuberculosis therapy is routinely given after surgery[15,16]. All patients included in the present study received regular anti-tuberculosis therapy after surgery.
Appropriate surgical intervention and regular postoperative anti-tuberculosis therapy are effective in treating liver tuberculosis.
| 1. | Mishra S, Taneja S, De A, Muthu V, Verma N, Premkumar M, Duseja A, Singh V. Tuberculosis in Cirrhosis - A Diagnostic and Management Conundrum. J Clin Exp Hepatol. 2022;12:278-286. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 12] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 2. | Jha DK, Pathiyil MM, Sharma V. Evidence-based approach to diagnosis and management of abdominal tuberculosis. Indian J Gastroenterol. 2023;42:17-31. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 54] [Cited by in RCA: 51] [Article Influence: 17.0] [Reference Citation Analysis (1)] |
| 3. | McMullan GS, Lewis JH. Tuberculosis of the Liver, Biliary Tract, and Pancreas. Microbiol Spectr. 2017;5. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 1.6] [Reference Citation Analysis (1)] |
| 4. | Hara Y, Yanagita T, Ishii K, Nakamura K. Portal Vein Thrombosis Caused by Miliary Tuberculosis. Intern Med. 2024;63:1181-1182. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 5. | Levine DM, Dutta NK, Eckels J, Scanga C, Stein C, Mehra S, Kaushal D, Karakousis PC, Salamon H. A tuberculosis ontology for host systems biology. Tuberculosis (Edinb). 2015;95:570-574. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 9] [Article Influence: 0.8] [Reference Citation Analysis (1)] |
| 6. | Vohra S, Dhaliwal HS. Miliary Tuberculosis. 2024 Jan 30. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. [PubMed] |
| 7. | Gupta P, Kumar S, Sharma V, Mandavdhare H, Dhaka N, Sinha SK, Dutta U, Kochhar R. Common and uncommon imaging features of abdominal tuberculosis. J Med Imaging Radiat Oncol. 2019;63:329-339. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 36] [Article Influence: 5.1] [Reference Citation Analysis (1)] |
| 8. | Pereira JM, Madureira AJ, Vieira A, Ramos I. Abdominal tuberculosis: imaging features. Eur J Radiol. 2005;55:173-180. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 144] [Cited by in RCA: 105] [Article Influence: 5.0] [Reference Citation Analysis (1)] |
| 9. | Chong VH, Lim KS. Hepatobiliary tuberculosis. Singapore Med J. 2010;51:744-751. [PubMed] |
| 10. | Sharma M, Karikalan M, Dandapat P, Asok Kumar M, Beena V, Chandra Mohan S, Ilayaraja S, Mathur A, Bhawal A, Pawde AM, Sharma AK. Tuberculosis in free-ranging and captive wild animals: Pathological and molecular diagnosis with histomorphological differentiation of granulomatous lesions. Microb Pathog. 2022;172:105752. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 10] [Reference Citation Analysis (1)] |
| 11. | Nakagawa M. [Factors for the onset of and the exacerbation of tuberculosis. 4. Clinical factors related to the onset and exacerbation of tuberculosis. b. Middle-aged and elderly patients]. Kekkaku. 1999;74:747-752. [PubMed] |
| 12. | Huang Q, Wang CC, Liu YG, Zhao CM, Zhang TP, Liu Y, Wang H. Clinical relevance of genetic polymorphisms in WNT signaling pathway (SFRP1, WNT3A, CTNNB1, WIF-1, DKK-1, LRP5, LRP6) on pulmonary tuberculosis in a Chinese population. Front Immunol. 2022;13:1011700. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 13. | Varshney P, Kumar Kapoor V. Hepato-pancreato-biliary tuberculosis: A review. Turk J Surg. 2024;40:95-103. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 14. | Noomene R, Ouakaa A, Jouini R, Maamer AB, Cherif A. What remains to surgeons in the management of abdominal tuberculosis? A 10 years experience in an endemic area. Indian J Tuberc. 2017;64:167-172. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 15. | Jatoi NN, Ashraf M, Shaikh VF, Nasir S, Jatoi HN. Tuberculosis Presenting as Ruptured Liver Abscess and Inferior Vena Cava Thrombosis in a Pediatric Patient. Ochsner J. 2023;23:343-346. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 16. | Dey J, Gautam H, Venugopal S, Porwal C, Mirdha BR, Gupta N, Singh UB. Tuberculosis as an Etiological Factor in Liver Abscess in Adults. Tuberc Res Treat. 2016;2016:8479456. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 6] [Article Influence: 0.6] [Reference Citation Analysis (1)] |