Published online Apr 6, 2026. doi: 10.12998/wjcc.v14.i10.118053
Revised: February 10, 2026
Accepted: March 6, 2026
Published online: April 6, 2026
Processing time: 100 Days and 23.3 Hours
Achieving reliable pulpal anesthesia during root canal treatment of hypomineralized second primary molars (HSPM) is clinically challenging, as structural al
To evaluate the anesthetic efficacy of 4% articaine vs 2% lignocaine, when admi
The study comprised 20 pediatric participants, each undergoing two treatment sessions. At the initial appointment, children were randomized to receive either 4% articaine or 2% lignocaine, with the alternate anesthetic administered in the second session as part of the split-mouth design. Injection discomfort and anes
The participants had a mean age of 7.15 ± 0.67 years. Pain scores during injection showed no statistically significant difference between articaine and lignocaine when assessed using either the WBFPRS or the FLACC scale. In contrast, during access cavity preparation, articaine produced significantly lower pain ratings on both the WBFPRS and the FLACC scale. Furthermore, during instrumentation, articaine continued to yield reduced pain responses, with a statistically significant difference observed on the FLACC scale, although the WBFPRS did not reach statistical significance.
Articaine 4% exhibited superior anesthetic performance compared with lignocaine 2%, particularly during access cavity preparation and canal instrumentation in HSPM. Although both agents showed comparable pain levels during injection, articaine achieved more profound and consistent pulpal anesthesia throughout operative phases of treatment. These findings suggest that articaine may represent a more reliable anesthetic agent for endodontic management of HSPM.
Core Tip: Achieving effective pulpal anesthesia in hypomineralized second primary molars is often challenging with conventional local anesthetics. This split-mouth clinical study demonstrates that 4% articaine provides superior intraoperative anesthetic efficacy compared with 2% lignocaine during root canal treatment of hypomineralized second primary molars, particularly during access cavity preparation and canal instrumentation. While both agents showed comparable discomfort during injection, articaine achieved more profound and consistent pulpal anesthesia. The findings underscore the clinical importance of selecting anesthetic agents with enhanced tissue penetration for hypomineralized teeth and provide evidence-based guidance for improving pain control and treatment outcomes in pediatric endodontic practice.
- Citation: D’Souza OK. Comparative evaluation of anesthetic efficacy of articaine vs lignocaine during root canal therapy in hypomineralized second primary molars. World J Clin Cases 2026; 14(10): 118053
- URL: https://www.wjgnet.com/2307-8960/full/v14/i10/118053.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i10.118053
Developmental defects of enamel represent one of the most common conditions affecting children globally[1]. They frequently present in multiple forms, one of which is molar incisor hypomineralization, a condition that predominantly affects one or more first permanent molars, with or without involvement of the incisors[2]. Hypomineralization is a qualitative enamel defect resulting from disturbances during the initial stages of calcification and/or enamel maturation, leading to enamel of normal thickness but increased porosity and fragility due to reduced protein content and disorganisation of the enamel prisms[3]. These enamel defects are clinically evident as well-demarcated areas of altered trans
Lesions resembling those seen in molar incisor hypomineralization have also been identified in second primary molars and primary canines[5]. Hypomineralized second primary molars (HSPM) is the currently accepted term for the con
Hypomineralized enamel acts as a poor thermal insulator, resulting in inadequate pulpal protection from external temperature changes. Consequently, affected teeth often exhibit hypersensitivity to hot and cold stimuli. Persistent thermal stress induces pulpal inflammation and pH alterations in the periapical tissues, leading to heightened excitability of pulpal nerve fibers, which respond to lower-than-normal levels of stimulation. Clinically, this manifests as a hyper
Several local anesthetic agents are available for use in children, with the most commonly employed being 4% articaine and 2% lignocaine. Although numerous studies have compared 2% lignocaine with 4% articaine in pediatric patients, the findings have been inconsistent[10]. To date, there is no randomized clinical study comparing lignocaine with articaine when an inferior alveolar nerve block (IANB) is used for local anesthesia of HSPMs. Hence, the study aimed to evaluate the anesthetic efficacy of 4% articaine vs 2% lignocaine, when administered as an IANB for root canal therapy of HSPM.
This split-mouth, double-blinded, randomized controlled trial was conducted in the Department of Pedodontics and Preventive Dentistry at Goa Dental College and Hospital, Bambolim, Goa, India over a period of five months (from August 2025 to December 2025). Ethical approval was obtained from the Institutional Ethics Committee of Goa Dental College and Hospital (No. GDCH/IRB/V-2025/RPN29-29), and the study was prospectively registered with the Clinical Trials Registry of India (CTRI/2025/08/092581; dated August 7, 2025). Each child was administered 2% lignocaine with 1:80000 epinephrine and 4% articaine with 1:100000 epinephrine in a split-mouth design.
The study included medically and mentally healthy children aged six to nine years with bilateral mandibular HSPMs, diagnosed according to the criteria proposed by Ghanim et al[11], presenting with signs of irreversible pulpitis and requiring root canal therapy. Children demonstrating positive or definitely positive behavior, as classified by the Frankl Behavior Rating Scale were included[12]. The participating children were not receiving any analgesic or sedative medication at the time of enrolment, and written informed consent was obtained from their parents or legal guardians prior to participation. Children with a known hypersensitivity to the local anesthetic agents used in the study and those presenting with non-vital pulp in the involved teeth were excluded.
The study was designed as a split-mouth crossover trial. The sample size was calculated using G*Power software (version 3.1.9.4), with an alpha error probability of 5% (α = 0.05) and a statistical power of 95% (β = 0.05). Based on the expected differences in pain scores between the two anesthetic agents[10], a minimum of 20 children (40 paired sites) was required, and all were included in the study. A total of 32 children were assessed for eligibly.
Randomization of anesthetic type for each injection was performed using a computer-generated random numbers table. Twenty injections were assigned to either 4% articaine or 2% lignocaine, with the injection site (right or left) also ran
Injection pain and the effectiveness of anesthesia were assessed using both subjective and objective measures. Subjective pain was evaluated with the Wong-Baker Faces Pain Rating Scale (WBFPRS)[13]. Objective assessment was performed using the Face, Legs, Activity, Cry, and Consolability (FLACC) scale[14]. The effectiveness of anesthesia was specifically assessed during access cavity preparation and canal instrumentation.
All procedures were performed by the same investigator. Before starting the session, the investigator explained the WBFPRS to the child. The child randomly received either an IANB of 4% articaine or 2% lignocaine at each session. The assistant, upon identifying the anesthetic solution, drew it into a 27G syringe, taking care to do so out of the investigators and child’s view. Subsequently, the assistant selected a sealed envelope from the allocation box to determine whether the injection would be administered on the right or left molar. Local anesthesia was administered via an IANB following confirmation of negative aspiration. The child was asked to indicate the face that represents his/her feeling during the injection on the WBFPRS. The FLACC score during administration of anesthesia was recorded by an assistant not involved in the intervention. The pain experienced by the child was further assessed during opening the pulp chamber with endodontic burs and when the endodontic files were introduced into the root canals. If the patient experienced pain, the dental treatment was halted, and the pain level during the procedure was recorded using the WBFPRS and the FLACC scale. An anesthetic failure was considered if pain persisted and intrapulpal anesthesia was required. In such cases, the highest scores on the WBFPRS and the FLACC scale were recorded. The second session was carried out one week later, with the contralateral tooth receiving anesthesia and treatment using the alternate anesthetic solution, following the same protocol as the first session.
Statistical analysis was performed using the IBM SPSS version 26.0 software. Continuous variables, such as age and weight, were summarized as mean ± SD, while categorical variables, including gender and behavior scores, were expressed as n (%). Pain scores measured using the WBFPRS and FLACC scale were treated as ordinal data and com
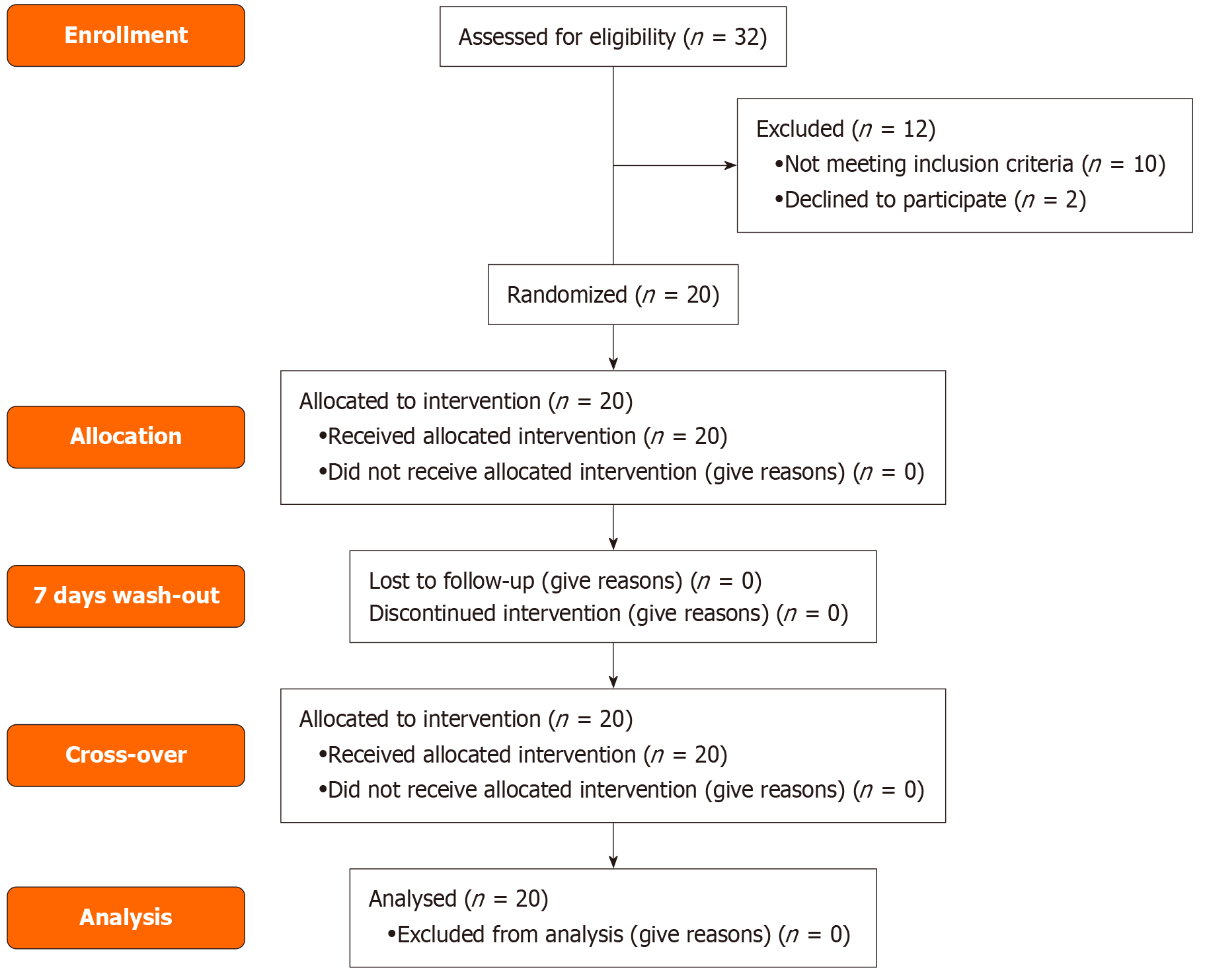
The flow of participants through the study is presented in the CONSORT diagram (Figure 1).
A total of 20 children (12 males, 8 females) with a mean age of 7.15 ± 0.67 years and mean weight of 25.4 ± 1.47 kg participated in the study. According to the Frankl Behavior Rating Scale, during the first visit, 6 children (44%) exhibited positive behavior and 14 (56%) demonstrated definitely positive behavior. At the second visit, positive behavior was observed in 9 children (45%), while 11 children (55%) showed definitely positive behavior (Table 1).
| Baseline characteristics | |
| Age | 7.15 ± 0.67 |
| Gender | Males: 12 (60) |
| Females: 8 (40) | |
| Weight | 25.4 ± 1.47 |
| Frankl behaviour rating-visit 1 | Positive: 6 (44) |
| Definitely positive: 14 (56) | |
| Frankl behaviour rating-visit 2 | Positive: 9 (45) |
| Definitely positive: 11 (55) | |
Pain experienced during anesthetic injection did not differ significantly between 4% articaine and 2% lignocaine. Ac
| Item | No hurt (0) | Little bit (2) | Little more (4) | Even more (6) | Whole lot (8) | Hurt worst (10) | Median (interquartile range) | P value |
| Articaine | 3 (15.0) | 8 (40.0) | 5 (25.0) | 3 (15.0) | 1 (5.0) | 0 (0.0) | 2 (2, 4) | 0.16 |
| Lignocaine | 7 (35.0) | 7 (35.0) | 4 (20.0) | 1 (5.0) | 1 (5.0) | 0 (0.0) | 2 (0, 4) |
| Item | Relaxed (1) | Mild (2) | Moderate (3) | Severe (4) | Median (interquartile range) | P value |
| Articaine | 8 (40.0) | 8 (40.0) | 3 (15.0) | 1 (5.0) | 2 (1, 2) | 0.856 |
| Lignocaine | 7 (35.0) | 8 (40.0) | 5 (25.0) | 0 (0.0) | 2 (1, 2) |
During access opening, children receiving 4% articaine experienced significantly less pain compared with those receiving 2% lignocaine. On the WBFPRS, the median pain response for articaine corresponded to “no hurt”, whereas lignocaine demonstrated a median response corresponding to “hurts little bit”, with the difference reaching statistical significance (P = 0.043; Table 4). Assessment using the FLACC scale further supported this finding, with articaine showing a median response consistent with “relaxed", compared with "mild pain" for lignocaine (P = 0.010; Table 5). A total of four children in the lignocaine group experienced severe pain and required supplementary anesthesia. These results indicate superior anesthetic efficacy of articaine during access cavity preparation.
| Item | No hurt (0) | Little bit (2) | Little more (4) | Even more (6) | Whole lot (8) | Hurt worst (10) | Median (interquartile range) | P value |
| Articaine | 10 (50.0) | 9 (45.0) | 1 (5.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 1 (0, 2) | 0.043a |
| Lignocaine | 5 (25.0) | 9 (45.0) | 2 (10.0) | 3 (15.0) | 1 (5.0) | 0 (0.0) | 2 (0, 4) |
| Item | Relaxed (1) | Mild (2) | Moderate (3) | Severe (4) | Median (interquartile range) | P value |
| Articaine | 14 (70.0) | 5 (25.0) | 1 (5.0) | 0 (0.0) | 1 (1, 2) | 0.010a |
| Lignocaine | 5 (25.0) | 9 (45.0) | 2 (10.0) | 4 (20.0) | 2 (1, 3) |
Since four children in the lignocaine group required supplementary anesthesia during access cavity preparation, they were given the worst WBFPRS and FLACC scale scores during canal instrumentation. According to the WBFPRS, the majority of children in the articaine group reported “no hurt” or “hurts little bit”, whereas lignocaine showed greater variability, with some children reporting “hurt worst” (P = 0.132; Table 6). FLACC scale assessments mirrored this trend: (1) 85% of children in the articaine group were "relaxed", 15% exhibited "mild pain"; and (2) Whereas in the lignocaine group, 60% were "relaxed", 20% experienced "severe pain" (P = 0.032; Table 7). These findings indicate that articaine provided slightly lower and more consistent pain scores compared with lignocaine during root canal instrumentation.
| Item | No hurt (0) | Little bit (2) | Little more (4) | Even more (6) | Whole lot (8) | Hurt worst (10) | Median (interquartile range) | P value |
| Articaine | 15 (75.0) | 5 (25.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0, 0) | 0.132 |
| Lignocaine | 10 (50.0) | 5 (25.0) | 1 (5.0) | 0 (0.0) | 0 (0.0) | 4 (20.0) | 0 (0, 10) |
| Item | Relaxed (1) | Mild (2) | Moderate (3) | Severe (4) | Median (interquartile range) | P value |
| Articaine | 17 (85.0) | 3 (15.0) | 0 (0.0) | 0 (0.0) | 1 (1, 1) | 0.032a |
| Lignocaine | 12 (60.0) | 3 (15.0) | 1 (5.0) | 4 (20.0) | 1 (1, 2) |
Effective local anesthesia helps build patient-dentist trust, reduces fear and anxiety, and encourages a positive attitude toward dental care. Conversely, inadequate pain management during dental procedures can lead to considerable physical discomfort as well as adverse psychological effects[15]. Hypomineralized teeth present a significant clinical challenge during the administration of local anesthesia. At present, there is insufficient evidence to determine the most effective local anesthetic agent for achieving adequate anesthesia in HSPM. Hence, the present split-mouth, double-blinded randomized controlled trial compared the anesthetic efficacy of 4% articaine and 2% lignocaine administered as IANB for root canal therapy in mandibular HSPM.
The diagnostic criteria proposed by Ghanim et al[11] were employed to identify HSPM due to their standardised, validated, and widely accepted framework that ensures diagnostic consistency and reproducibility, which is essential in clinical research where subjective interpretation of enamel defects may introduce examiner bias. By providing clear definitions and visual reference standards, these criteria facilitate reliable differentiation of HSPM from other developmental enamel defects such as fluorosis, enamel hypoplasia, and early carious lesions.
In the present study, pain assessment was performed using both the WBFPRS and the FLACC scale to obtain a comprehensive and age-appropriate evaluation of pain in pediatric patients. The WBFPRS is a validated self-report pain scale that is simple, child-friendly, and widely used in clinical and dental settings for children. It enables children to express pain intensity visually, thereby improving the accuracy in subjective pain reporting and enhancing cooperation during dental procedures[13]. However, self-reported pain scores may be influenced by cognitive development, anxiety, or communication limitations, especially in younger children or those experiencing dental fear. To overcome this limitation, the FLACC scale was additionally employed as an objective behavioural pain assessment tool. The FLACC scale ev
Injection pain is influenced by multiple factors, including solution pH, rate of injection, tissue distension, and psychological factors, rather than solely the anesthetic agent used[17]. Articaine 4% has a lower solution pH (2.43) than lig
In contrast, significant differences were observed during access cavity preparation, where children receiving articaine experienced lower pain scores compared with those receiving lignocaine. This observation holds clinical significance because access cavity preparation can elicit increased pain in hypomineralized teeth as a result of enhanced dentinal sensitivity and underlying pulpal inflammation. Hypomineralized enamel and dentin exhibit increased porosity, reduced mineral density, and altered tubular structure, facilitating rapid stimulus transmission to the pulp and lowering the pain threshold[20,21]. These pathological changes may partly explain the reduced efficacy of lignocaine in achieving adequate pulpal anesthesia in HSPM.
The superior performance of articaine observed in this study may be attributed to its unique pharmacological pro
During canal instrumentation, articaine produced more consistent and lower pain responses than lignocaine, as indicated by FLACC scores. In contrast, several children in the lignocaine group required supplementary anesthesia during access cavity preparation and were therefore categorized as anesthetic failures. However, as no previous clinical studies have specifically evaluated anesthetic efficacy in HSPM, direct comparisons with existing literature could not be made.
The behavioural implications of inadequate anesthesia are particularly important in paediatric patients. Children experiencing pain during treatment are more likely to exhibit anxiety, negative behaviour, and reduced cooperation, which can compromise treatment outcomes and long-term dental attitudes[25]. The improved anesthetic reliability of articaine observed in this study may therefore have beneficial effects beyond pain control, contributing to better be
Despite its strengths, including a split-mouth design, blinding, and the use of both subjective and objective pain assessment tools, this study has certain limitations. The relatively small sample size and restriction to mandibular HSPMs limit the generalizability of the findings. Additionally, the study evaluated only IANB administration; future studies should explore alternative techniques such as buccal infiltration, intraosseous anesthesia, or combined approaches. Long-term outcomes and post-operative pain were also not assessed and warrant further investigation.
Within the limitations of this study, 4% articaine demonstrated superior anesthetic performance compared with 2% lignocaine, particularly during access cavity preparation and canal instrumentation in HSPM. While both anesthetic agents produced comparable pain responses during injection, articaine provided more profound and sustained pulpal anesthesia during the operative phases of treatment. This was reflected by lower pain scores, greater patient comfort, and reduced need for supplementary anesthesia when articaine was used. The more consistent anesthetic efficacy observed with articaine suggests that it may be a more reliable and effective local anesthetic agent for the endodontic management of HSPM in pediatric patients.
I gratefully acknowledge the Department of Pedodontics and Preventive Dentistry, Goa Dental College and Hospital, for their support throughout the study. I also sincerely thank the parents of the patients for their cooperation and trust.
| 1. | Owen ML, Ghanim A, Elsby D, Manton DJ. Hypomineralized second primary molars: prevalence, defect characteristics and relationship with dental caries in Melbourne preschool children. Aust Dent J. 2018;63:72-80. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 28] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 2. | Weerheijm KL, Jälevik B, Alaluusua S. Molar-incisor hypomineralisation. Caries Res. 2001;35:390-391. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 402] [Cited by in RCA: 457] [Article Influence: 18.3] [Reference Citation Analysis (0)] |
| 3. | Americano GC, Jacobsen PE, Soviero VM, Haubek D. A systematic review on the association between molar incisor hypomineralization and dental caries. Int J Paediatr Dent. 2017;27:11-21. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 99] [Cited by in RCA: 143] [Article Influence: 15.9] [Reference Citation Analysis (0)] |
| 4. | Borrego-Martí N, Peris-Corominas R, Maura-Solivellas I, Ferrés-Padró E, Ferrés-Amat E. Hypomineralisation of second primary molars and primary canines: Prevalence and description of lesions in a population of 153 patients visited at a hospital paediatric dentistry service. Eur J Paediatr Dent. 2021;22:237-242. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 5. | Elfrink ME, Schuller AA, Weerheijm KL, Veerkamp JS. Hypomineralized second primary molars: prevalence data in Dutch 5-year-olds. Caries Res. 2008;42:282-285. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 87] [Cited by in RCA: 96] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 6. | Singh R, Srivastava B, Gupta N. Prevalence and Pattern of Hypomineralized Second Primary Molars in Children in Delhi-NCR. Int J Clin Pediatr Dent. 2020;13:501-503. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 7. | Lima LJS, Ramos-Jorge ML, Soares MEC. Prenatal, perinatal and postnatal events associated with hypomineralized second primary molar: a systematic review with meta-analysis. Clin Oral Investig. 2021;25:6501-6516. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 18] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 8. | Almuallem Z, Busuttil-Naudi A. Molar incisor hypomineralisation (MIH) - an overview. Br Dent J. 2018. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 80] [Cited by in RCA: 93] [Article Influence: 11.6] [Reference Citation Analysis (0)] |
| 9. | Weerheijm KL. Molar incisor hypomineralization (MIH): clinical presentation, aetiology and management. Dent Update. 2004;31:9-12. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 124] [Cited by in RCA: 157] [Article Influence: 7.1] [Reference Citation Analysis (0)] |
| 10. | Haidar M, Raslan N. Comparative study of articaine 4% versus lidocaine 2% in the local anesthesia of permanent mandibular first molars affected by MIH: a randomized controlled trial. Eur Arch Paediatr Dent. 2023;24:621-630. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 11. | Ghanim A, Silva MJ, Elfrink MEC, Lygidakis NA, Mariño RJ, Weerheijm KL, Manton DJ. Molar incisor hypomineralisation (MIH) training manual for clinical field surveys and practice. Eur Arch Paediatr Dent. 2017;18:225-242. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 142] [Article Influence: 15.8] [Reference Citation Analysis (0)] |
| 12. | Sharma A, Tyagi R. Behavior Assessment of Children in Dental Settings: A Retrospective Study. Int J Clin Pediatr Dent. 2011;4:35-39. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 27] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 13. | Wong DL, Baker CM. Pain in children: comparison of assessment scales. Pediatr Nurs. 1988;14:9-17. [PubMed] |
| 14. | Crellin DJ, Harrison D, Santamaria N, Babl FE. Systematic review of the Face, Legs, Activity, Cry and Consolability scale for assessing pain in infants and children: is it reliable, valid, and feasible for use? Pain. 2015;156:2132-2151. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 201] [Cited by in RCA: 169] [Article Influence: 15.4] [Reference Citation Analysis (1)] |
| 15. | American Academy of Pediatric Dentistry. Use of local anesthesia for pediatric dental patients. The Reference Manual of Pediatric Dentistry. Chicago, IL: American Academy of Pediatric Dentistry, 2025: 407-414 Available from: https://www.aapd.org/research/oral-health-policies--recommendations/use-of-local-anesthesia-for-pediatric-dental-patients/. |
| 16. | Merkel SI, Voepel-Lewis T, Shayevitz JR, Malviya S. The FLACC: a behavioral scale for scoring postoperative pain in young children. Pediatr Nurs. 1997;23:293-297. [PubMed] |
| 17. | Meechan JG. Pain control in local analgesia. Eur Arch Paediatr Dent. 2009;10:71-76. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 19] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 18. | Martin E, Lee A, Jennings E. Articaine: dental practitioner use, basis of perception and evidence-based dentistry-a cross-sectional study. BDJ Open. 2022;8:20. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 19. | Jorgenson K, Burbridge L, Cole B. Comparison of the efficacy of a standard inferior alveolar nerve block versus articaine infiltration for invasive dental treatment in permanent mandibular molars in children: a pilot study. Eur Arch Paediatr Dent. 2020;21:171-177. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 11] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 20. | de Castro CRN, Lima CCB, Costa LC, Silva RNC, Pascotto RC, de Moura MS, Almeida de Deus Moura LF, Moura de Lima MD. Hypomineralized Teeth Have a Higher Frequency of Dental Hypersensitivity. Pediatr Dent. 2021;43:218-222. [PubMed] |
| 21. | Rodd HD, Boissonade FM, Day PF. Pulpal status of hypomineralized permanent molars. Pediatr Dent. 2007;29:514-520. [PubMed] |
| 22. | Kakroudi SH, Mehta S, Millar BJ. Articaine hydrochloride: is it the solution? Dent Update. 2015;42:88-90, 92. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 14] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 23. | Akhtar N, Brizuela M, Stenhouse PD. Local Anesthetic Drugs Used In Dentistry. 2025 Jan 23. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. [PubMed] |
| 24. | Becker DE, Reed KL. Local anesthetics: review of pharmacological considerations. Anesth Prog. 2012;59:90-101; quiz 102. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 299] [Cited by in RCA: 427] [Article Influence: 30.5] [Reference Citation Analysis (1)] |
| 25. | Klinberg G. Dental anxiety and behaviour management problems in paediatric dentistry--a review of background factors and diagnostics. Eur Arch Paediatr Dent. 2008;9 Suppl 1:11-15. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 65] [Article Influence: 4.6] [Reference Citation Analysis (1)] |