Published online Apr 6, 2026. doi: 10.12998/wjcc.v14.i10.118527
Revised: February 3, 2026
Accepted: March 9, 2026
Published online: April 6, 2026
Processing time: 87 Days and 22.1 Hours
Crohn’s disease (CD) is a chronic inflammatory bowel disorder characterized by transmural inflammation and granuloma formation. Extraintestinal manifesta
We describe an 18-year-old male with Crohn’s colitis who concurrently presented with renal impairment. Renal biopsy revealed acute interstitial nephritis with a single non-necrotizing granuloma. Initial steroid therapy led to partial impro
This case highlights a rare presentation of Crohn’s-related renal granuloma suc
Core Tip: Renal granulomatous inflammation is an exceedingly rare extraintestinal manifestation of Crohn’s disease (CD) and lacks established management guidelines. We report a biopsy-confirmed case of CD-associated renal granuloma with interstitial nephritis demonstrating sustained renal and intestinal response to infliximab therapy. This case underscores the importance of considering immune-mediated renal involvement in CD and suggests that disease-targeted biologic therapy may represent an effective treatment approach for this rare manifestation.
- Citation: Terlato M, Gao W, Pillay L, Williams D, Segal JP, Macrae F, Christensen B. Renal granuloma as an extraintestinal manifestation in Crohn’s disease: A case report. World J Clin Cases 2026; 14(10): 118527
- URL: https://www.wjgnet.com/2307-8960/full/v14/i10/118527.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i10.118527
Crohn’s disease (CD) is a type of inflammatory bowel disease (IBD) that represents immune-mediated inflammation of the gastrointestinal tract (GIT)[1]. CD can have variable disease location across the GIT and varying phenotypes (stricturing, fistulizing, and penetrating forms), requiring multiple modalities of investigation prior to diagnosis. Skip lesions across the GIT and histological evidence of granulomas are more suggestive of CD than ulcerative colitis[2]. CD-related granulomas may manifest outside the GIT, with the most commonly reported sites being lymph nodes, mes
An 18-year-old male was referred with a one-year history of abdominal pain, bloody diarrhoea, and bloating.
At the time of referral, he was undergoing investigation for autoimmune renal disease by a nephrologist and had been commenced on prednisone prior to gastroenterology review. His gastrointestinal symptoms were well controlled on a high dose of prednisone (50 mg), with relapse occurring during steroid tapering.
His medical history included previous gastrointestinal helminth infection (treated), Giardia gastroenteritis, and lactose intolerance. There was no significant non-steroidal anti-inflammatory drug use.
There was no family history of CD or colorectal cancer.
Physical examination showed a soft abdomen with generalized abdominal tenderness but no signs of peritonism.
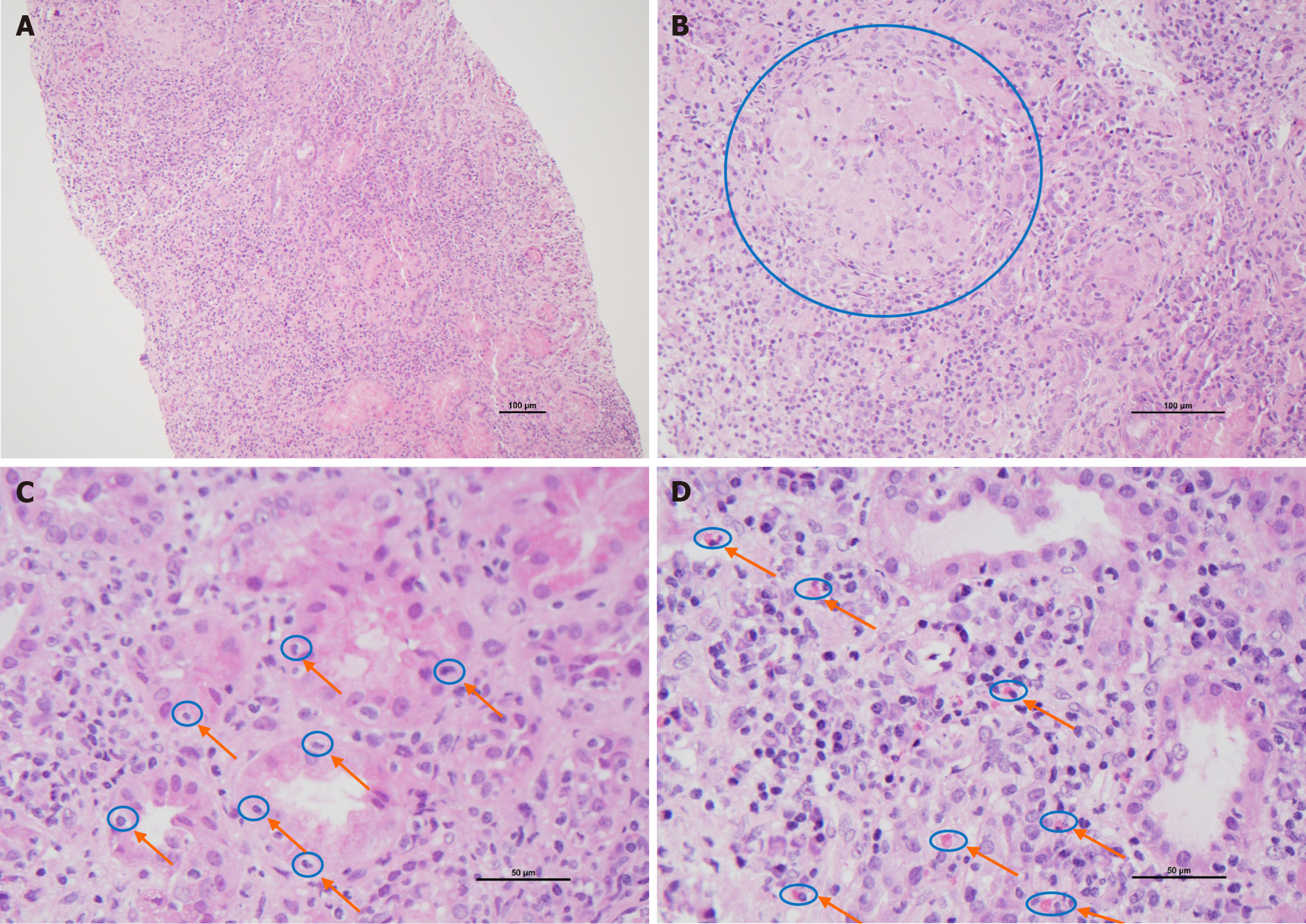
Laboratory investigations revealed hemoglobin of 122 g/L, white cell count of 15.6 × 109/L, erythrocyte sedimentation rate of 40 mm/hour, creatinine of 194 μmol/L, estimated glomerular filtration rate of 55 mL/minute, and albumin of 38 g/L. Fecal calprotectin was elevated at 307 μg/g. Renal biopsy was performed following negative infectious, immune, and metabolic screening and in the absence of significant nephrotoxic drug exposure. Histopathology demonstrated acute interstitial nephritis without chronic damage and a single granuloma (Figure 1). Urinalysis confirmed pyuria.
An ultrasound examination of the kidneys was performed, and the renal ultrasound showed mild vesicoureteral reflux.
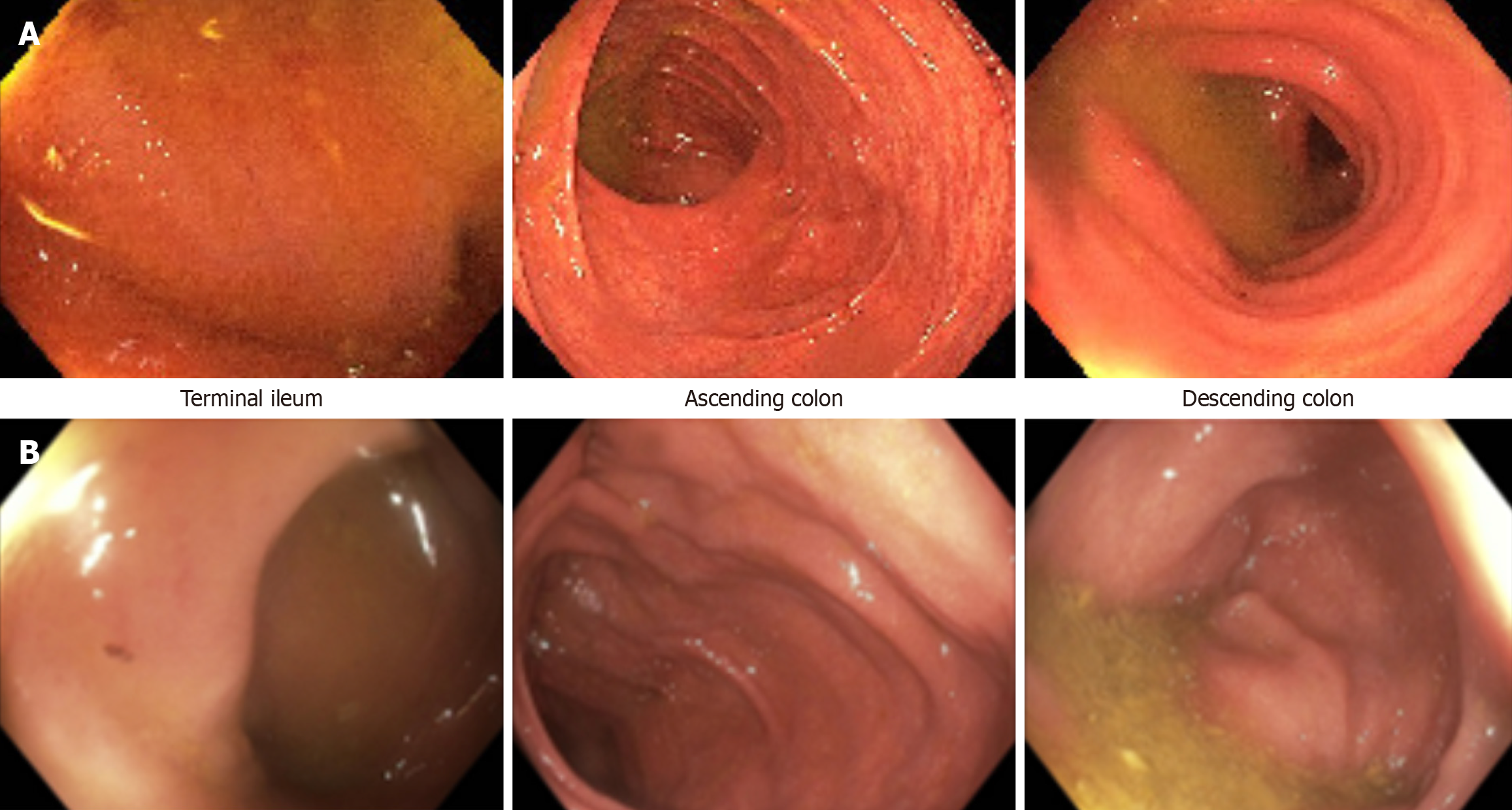
CD was diagnosed on colonoscopy, which demonstrated pancolitis, and histopathology revealed mild chronic colitis with non-necrotizing granulomas (Figure 2A). Further investigations showed negative antinuclear antibody, antineutrophil cytoplasmic antibody, complement levels (C3 and C4), hepatitis B and hepatitis C serology, human immunodeficiency virus testing, and QuantiFERON-TB Gold assay. Chest X-ray was normal. The patient was diagnosed with CD-associated renal granuloma with interstitial nephritis.
Steroid tapering was undertaken, followed by intravenous infliximab induction and subsequent maintenance therapy with subcutaneous infliximab administered every two weeks. Both renal function and gastrointestinal symptoms im
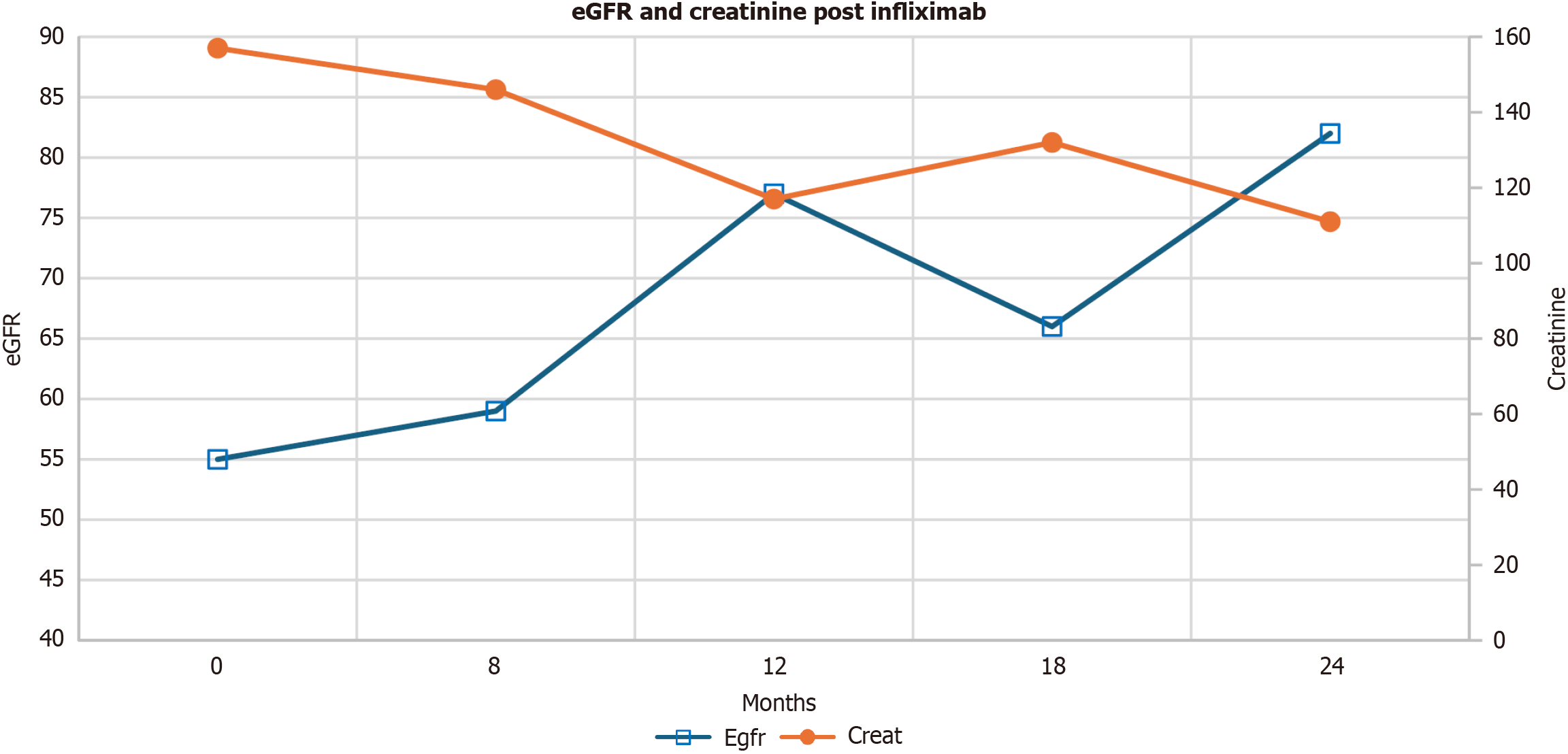
Colonoscopy performed one year after diagnosis demonstrated endoscopic remission (Figure 2B), accompanied by ongoing improvement in renal function and resolution of pyuria (Figure 3).
We describe an exceptionally rare EIM of CD: Biopsy-confirmed renal granulomatous inflammation consistent with CD, which has been rarely reported in the literature. Following standard induction with corticosteroids, the patient demonstrated marked improvement in renal function after initiation of infliximab therapy. To the best of our knowledge, we report the first instance of renal granulomatous disease successfully treated with subcutaneous infliximab mono
| Ref. | Age (years) | Treatment | Renal impairment | Resolution of renal impairment | Follow up |
| Archimandritis and Weetch[5], 1993 | 22 | Sulfasalazine, prednisolone | BUN 10 mmol to 19.9 mmol, CrCl reduced to 14-15 mL/minute2 | Yes | Followed up in 4 years: Remission |
| Baumer et al[6], 1999 | 21 | Elevated serum Cr 394 μmol/L | NA | Followed up in 4 years: ESRD | |
| Unal et al[7], 2008 | 43 | Prednisolone | Elevated serum Cr 256 μmol/L and CrCl 32.6 mL/minute2 | Mild improvement | Followed up in 2 months and 4 months post diagnosis of granuloma on biopsy |
| Marcus et al[8], 2008 | 16 | Steroids, infliximab | Elevated serum 221 μmol/L to 186 μmol/L, CrCl 35 mL/minute2 | No | Followed up in 6 months: No improvement in renal function |
| Marcus et al[8], 2008 | 11 | Prednisolone, 6MP, infliximab, 5-ASA | Elevated serum Cr 168 μmol/L at diagnosis | No | Follow up at time of writing: No improvement in renal function despite improving intestinal symptoms |
| Semjén et al[9], 2011 | 50 | Nephrectomy | Elevated serum Cr | NA | Nil follows up |
| Polci et al[10], 2012 | 56 | Steroid, anti-TNF | Serum Cr 97 μmol/L to 256 μmol/L, BUN 79 mg/dL, eGFR 24 mL/minute2 | No | Follow-up in 1 year: Worsening renal function |
| Colvin et al[11], 2014 | 23 | 5-ASA ceased, prednisolone | Serum Cr 71-133 μmol/L to 203 μmol/L in 2 months | Mild improvement | Follow-up in 21 months: Improved renal function |
| Saha et al[12], 2014 | 17 | Prednisone, azathioprine, infliximab | Serum Cr 398 μmol/L (reference 0.7-1.2 mg/dL), eGFR 18 mL/minute2 | Mild improvement | 26 months post renal biopsy: Referred for renal transplant |
| Timmermans et al[13], 2016 | 19 | Prednisone, + tacrolimus | Elevated serum Cr 177 μmol/L, eGFR 43 mL/minute2 | Mild improvement | Follow up renal function: Serum Cr 133 μmol/L, eGFR 60 mL/minute/1.73 m2 |
| Timmermans et al[13], 2016 | 22 | Prednisone, mycophenolate mofetil, ciclosporine | Serum Cr increased from 101 μmol/L to 160 μmol/L, eGFR 37 mL/minute2 | No | Follow up: ESRD |
| Han et al[14], 2022 | 19 | Prednisolone, infliximab | Elevated serum Cr 237 μmol/L | Yes | Follow up in 11 months: Improved Cr 2.12 μmol/L |
The first case of renal granuloma was described by Archimandritis and Weetch[5] in 1993, where they reported a severe case of Crohn’s colitis associated with renal impairment. Renal biopsies revealed chronic interstitial nephritis with local periglomerulofibrosis and granuloma formation. More recently, in 2011, a case of biopsy-proven renal granuloma with tumor-like radiological appearance was reported in a patient with long-standing CD without any evidence of diffuse renal disease or renal impairment[9]. There are well-established renal complications secondary to CD, and these are con
The pathogenesis of CD-related renal interstitial disease remains poorly understood. During a CD flare, highly activated T cells against gastrointestinal antigens circulate in the peripheral circulation. These primed T cells are thought to simultaneously undergo cross-reactivity against renal interstitial antigens. This subsequently stimulates differentiation into effector cell populations, including cytotoxic T cells, which cause direct cellular toxicity in the renal interstitium[13]. Timmermans et al[13] also report that levels of soluble interleukin-2 receptor, a marker of T-cell activation, correlate with disease activity in cases of granulomatous interstitial nephritis (GIN) in CD. Thus, interleukin-2 signaling may also play a role in disease pathogenesis[13].
GIN is an uncommon histopathological diagnosis, found in less than 1% of native kidney biopsies[13,16]. Reported causes of GIN include drug hypersensitivity reactions, chronic inflammatory diseases including renal sarcoidosis, and infections, including Mycobacterium tuberculosis[16-18].
In a case series of 38 patients with GIN, 44.7% of cases were drug-induced, of which non-steroidal anti-inflammatory drugs and antibiotics were most commonly associated[17]. In the wider literature, antibiotics including clarithromycin, ciprofloxacin, and vancomycin; anticonvulsants including phenytoin; and allopurinol, alendronate, and immunotherapy agents have all been identified as potential culprit agents[16,17,19].
Five-aminosalicylate (5-ASA) medications, commonly used in the treatment of mild-to-moderate severity IBD, are also known to cause nephrotoxicity[20]. 5-ASA-related renal disease is typically characterized by chronic TIN, as described in a multicenter study of 151 cases of 5-ASA medication-related nephrotoxicity in IBD patients. However, the same study also identified four 5-ASA-treated patients with a histopathological diagnosis of non-necrotizing GIN[20]. Colvin et al[11] also report an isolated case of GIN in CD with concomitant 5-ASA use. Determining whether GIN is a result of the disease process itself or 5-ASA nephrotoxicity in these cases is challenging[11,20]. Thus, it may be appropriate to with
Renal sarcoidosis is one of the most common causes of GIN[13,17,19]. Bijol et al[17] reported that 28.9% of cases were secondary to renal sarcoidosis in their case series, of which many patients had an established history of sarcoidosis and the presence of granulomas in other organs. This is similar to another case series by Joss et al[19], describing 27.8% of GIN cases due to renal sarcoidosis. Of note, GIN caused by sarcoidosis frequently responds to steroid therapy[18]. Thus, a lack of response in renal function to steroids alone favors a diagnosis of CD over sarcoidosis in our case. GIN associated with granulomatosis with polyangiitis, eosinophilic granulomatosis with polyangiitis, and TIN with uveitis syndrome have also been described[18,19].
Excluding infections is an essential step in the work-up of GIN. Tuberculosis is the most common infectious cause and is particularly prevalent in India. Rarely, GIN may also be caused by fungal infections, toxoplasmosis, Epstein-Barr virus, and Escherichia coli. Of note, poor response to steroid therapy may indicate an infectious cause for GIN and should pro
Renal granuloma is a distinct histopathological finding seen within the interstitial inflammatory infiltrate in GIN. Granulomas can be further classified as necrotizing or non-necrotizing, which may help differentiate the cause. Renal sarcoidosis, CD-related GIN, and drug-induced GIN typically present with non-necrotizing granulomas. Necrotizing granulomas are more commonly seen in GIN secondary to tuberculosis, fungal infections, and granulomatosis with poly
Evidence regarding the use of anti-tumor necrosis factor (TNF)-α agents in CD-related renal disease is limited. Only isolated case reports exist detailing the use of infliximab for TIN secondary to CD[8,21]. Saha et al[12] describe a case of granulomatous TIN as the initial presentation of CD treated with infliximab 5 mg/kg, with subsequent improvement in renal function, stabilization of creatinine, and improvement in gastrointestinal symptoms. A break in infliximab therapy for seven months caused rapid deterioration in renal function, which later improved following treatment re-initiation[12]. Stanton et al[21] report a case of non-granulomatous TIN and progression to chronic kidney disease as an initial EIM of CD. In this case, infliximab 5 mg/kg was successful in stabilizing creatinine levels and maintaining gastrointestinal symptom-free remission. On the other hand, Marcus et al[8] describe two pediatric cases with suboptimal responses to infliximab. In a case of granulomatous TIN in CD, there was improvement in gastrointestinal symptoms with infliximab; however, elevated serum creatinine persisted. In the second case of non-granulomatous TIN in CD, there was an initial gastrointestinal and renal response to infliximab; however, relapse of gastrointestinal symptoms was mirrored by new el
The mechanism of action of infliximab in the treatment of CD-related renal disease is not well elucidated. Stanton et al[21] postulate that in granulomatous TIN, infliximab acts to reduce TNF-α in the renal tubules directly, mirroring its effect on granulomatous disease elsewhere in the body. Rather, in non-granulomatous TIN, it is suggested that treatment of CD itself subsequently alleviates renal disease. Of note, renal function response to infliximab may also be impacted by the severity of interstitial fibrosis and tubular atrophy and progression to chronic kidney disease, as well as the degree of pre-renal insults secondary to exacerbated intestinal losses in CD[12].
Our case report illustrates that a treatment regimen directed towards CD, vs traditional therapy for acute interstitial nephritis, was successful in improving renal impairment, particularly with steroid weaning as per Crohn’s colitis protocol and introduction of a steroid-sparing agent with an anti-TNF inhibitor, infliximab. We additionally show that sub
This report has several important limitations. Firstly, as a single-patient case study, the ability to generalize our proposed treatment efficacy - particularly the use of subcutaneous infliximab - is inherently limited. Secondly, the rarity of Crohn’s-related renal granulomatous disease restricts meaningful comparison with pre-existing cases and therefore potential for establishing a relationship between other therapies and clinical improvement. Thirdly, while alternative causes of GIN were extensively investigated, the possibility of multifactorial or overlapping etiologies, including prior medication exposure, cannot be fully excluded. Fourthly, our team did not have evidence from longitudinal or serial renal histopathological assessments to determine response or remission to treatment; therefore, we relied on biochemical and clinical improvement as surrogate markers. Finally, ongoing longer-term follow-up is required to determine the durability of res
Given the extreme rarity of this presentation and the reliance on isolated case reports, further work is needed to better characterize the clinical behavior, immunopathological mechanisms, and optimal treatment strategies for Crohn’s-related renal granulomatous disease. Establishing collaborative case series would allow for more robust assessment of ther
In summary, we describe a highly uncommon EIM of CD - a case of biopsy-proven renal granulomatous inflammation, a condition for which evidence-based management strategies remain undefined. Our case demonstrates that treatment directed at controlling CD itself - specifically steroid induction followed by infliximab therapy - can lead to significant renal function improvement. Notably, this is, to our knowledge, the first reported case showing successful and sustained clinical response with subcutaneous infliximab monotherapy, highlighting its potential role as an effective steroid-sparing treatment option in Crohn’s-related GIN.
| 1. | Lamb CA, Kennedy NA, Raine T, Hendy PA, Smith PJ, Limdi JK, Hayee B, Lomer MCE, Parkes GC, Selinger C, Barrett KJ, Davies RJ, Bennett C, Gittens S, Dunlop MG, Faiz O, Fraser A, Garrick V, Johnston PD, Parkes M, Sanderson J, Terry H; IBD guidelines eDelphi consensus group, Gaya DR, Iqbal TH, Taylor SA, Smith M, Brookes M, Hansen R, Hawthorne AB. British Society of Gastroenterology consensus guidelines on the management of inflammatory bowel disease in adults. Gut. 2019;68:s1-s106. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1995] [Cited by in RCA: 1768] [Article Influence: 252.6] [Reference Citation Analysis (8)] |
| 2. | Feakins RM; British Society of Gastroenterology. Inflammatory bowel disease biopsies: updated British Society of Gastroenterology reporting guidelines. J Clin Pathol. 2013;66:1005-1026. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 183] [Cited by in RCA: 141] [Article Influence: 10.8] [Reference Citation Analysis (4)] |
| 3. | Eade MN, Cooke WT, Williams JA. Liver disease in Crohn's disease. A study of 100 consecutive patients. Scand J Gastroenterol. 1971;6:199-204. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 22] [Article Influence: 0.4] [Reference Citation Analysis (1)] |
| 4. | Janiak M, Jabłońska A, Skrobot K, Perdyan A, Pieńkowska J, Adrych K. Hepatic granulomas as an extraintestinal manifestation of Crohn disease. Pol Arch Intern Med. 2020;130:240-241. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 5. | Archimandritis AJ, Weetch MS. Kidney granuloma in Crohn's disease. BMJ. 1993;307:540-541. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 26] [Article Influence: 0.8] [Reference Citation Analysis (1)] |
| 6. | Baumer P, Brocard JF, Kohn W, Bedossa P, Charpentier B. [Severe chronic interstitial nephritis associated with Crohn's disease, but not with mesalazine?]. Gastroenterol Clin Biol. 1999;23:1400-1402. [PubMed] |
| 7. | Unal A, Sipahioglu MH, Akgun H, Yurci A, Tokgoz B, Erkilic K, Oymak O, Utas C. Crohn's disease complicated by granulomatous interstitial nephritis, choroidal neovascularization, and central retinal vein occlusion. Intern Med. 2008;47:103-107. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 15] [Article Influence: 0.8] [Reference Citation Analysis (1)] |
| 8. | Marcus SB, Brown JB, Melin-Aldana H, Strople JA. Tubulointerstitial nephritis: an extraintestinal manifestation of Crohn disease in children. J Pediatr Gastroenterol Nutr. 2008;46:338-341. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 27] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 9. | Semjén D, Fábos Z, Pakodi F, Vincze A, Szabó I, Degrell P, Csete M, Tornóczky T. Renal involvement in Crohn's disease: granulomatous inflammation in the form of mass lesion. Eur J Gastroenterol Hepatol. 2011;23:1267-1269. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 7] [Article Influence: 0.5] [Reference Citation Analysis (1)] |
| 10. | Polci R, Mangeri M, Faggiani R, Cristi E, Ranalli TV, Feriozzi S. Granulomatous interstitial nephritis in a patient with Crohn's disease. Ren Fail. 2012;34:1156-1159. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (1)] |
| 11. | Colvin RB, Traum AZ, Taheri D, Jafari M, Dolatkhah S. Granulomatous interstitial nephritis as a manifestation of Crohn disease. Arch Pathol Lab Med. 2014;138:125-127. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 20] [Article Influence: 1.7] [Reference Citation Analysis (1)] |
| 12. | Saha MK, Tarek H, Sagar V, Abraham P. Role of tumor necrosis factor inhibitor in granulomatous interstitial nephritis secondary to Crohn's disease. Int Urol Nephrol. 2014;46:229-233. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 0.5] [Reference Citation Analysis (1)] |
| 13. | Timmermans SA, Christiaans MH, Abdul-Hamid MA, Stifft F, Damoiseaux JG, van Paassen P. Granulomatous interstitial nephritis and Crohn's disease. Clin Kidney J. 2016;9:556-559. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 1.4] [Reference Citation Analysis (1)] |
| 14. | Han JS, Choi BS, Park CW, Choi YJ, Yang CW, Lee HH, Ban TH. Crohn’s Disease Identified as Granulomatous Tubulointerstitial Nephritis. Korean J Med. 2022;97:186-190. [DOI] [Full Text] |
| 15. | Corica D, Romano C. Renal Involvement in Inflammatory Bowel Diseases. J Crohns Colitis. 2016;10:226-235. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 115] [Cited by in RCA: 106] [Article Influence: 10.6] [Reference Citation Analysis (1)] |
| 16. | Figueiredo AC, Rodrigues L, Sousa V, Alves R. Granulomatous interstitial nephritis: a rare diagnosis with an overlooked culprit. BMJ Case Rep. 2019;12:e229159. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 17. | Bijol V, Mendez GP, Nosé V, Rennke HG. Granulomatous interstitial nephritis: a clinicopathologic study of 46 cases from a single institution. Int J Surg Pathol. 2006;14:57-63. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 83] [Cited by in RCA: 85] [Article Influence: 8.5] [Reference Citation Analysis (1)] |
| 18. | Janssen U, Naderi S, Amann K. Idiopathic granulomatous interstitial nephritis and isolated renal sarcoidosis: Two diagnoses of exclusion. SAGE Open Med. 2021;9:20503121211038470. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 6] [Article Influence: 1.2] [Reference Citation Analysis (1)] |
| 19. | Joss N, Morris S, Young B, Geddes C. Granulomatous Interstitial Nephritis. Clin J Am Soc Nephrol. 2007;2:222-230. [RCA] [DOI] [Full Text] [Cited by in Crossref: 118] [Cited by in RCA: 105] [Article Influence: 5.5] [Reference Citation Analysis (1)] |
| 20. | Heap GA, So K, Weedon M, Edney N, Bewshea C, Singh A, Annese V, Beckly J, Buurman D, Chaudhary R, Cole AT, Cooper SC, Creed T, Cummings F, de Boer NK, D'Inca R, D'Souza R, Daneshmend TK, Delaney M, Dhar A, Direkze N, Dunckley P, Gaya DR, Gearry R, Gore S, Halfvarson J, Hart A, Hawkey CJ, Hoentjen F, Iqbal T, Irving P, Lal S, Lawrance I, Lees CW, Lockett M, Mann S, Mansfield J, Mowat C, Mulgrew CJ, Muller F, Murray C, Oram R, Orchard T, Parkes M, Phillips R, Pollok R, Radford-Smith G, Sebastian S, Sen S, Shirazi T, Silverberg M, Solomon L, Sturniolo GC, Thomas M, Tremelling M, Tsianos EV, Watts D, Weaver S, Weersma RK, Wesley E, Holden A, Ahmad T. Clinical Features and HLA Association of 5-Aminosalicylate (5-ASA)-induced Nephrotoxicity in Inflammatory Bowel Disease. J Crohns Colitis. 2016;10:149-158. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 102] [Cited by in RCA: 87] [Article Influence: 8.7] [Reference Citation Analysis (2)] |
| 21. | Stanton B, Caza T, Huang D, Beg MB. Tubulointerstitial Nephritis as the Initial Presentation of Crohn's Disease and Successful Treatment with Infliximab. ACG Case Rep J. 2017;4:e24. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 0.8] [Reference Citation Analysis (1)] |