Published online Apr 6, 2026. doi: 10.12998/wjcc.v14.i10.117286
Revised: January 16, 2026
Accepted: March 4, 2026
Published online: April 6, 2026
Processing time: 119 Days and 23.7 Hours
Robotic liver resection has progressively pushed the boundaries of minimally invasive hepatopancreatobiliary surgery. The recently introduced da Vinci single-port (SP) system enables placement of a multiple-channel cannula through a single 2.5-4 cm incision and aims to limit parietal trauma while maintaining the advantages of current multi-port robotic platforms. Here, we report the first Ita
A 51-year-old woman with a history of breast cancer presented with a 15-mm metastasis in segment II of the liver. Following multidisciplinary assessment, a robotic left lateral sectionectomy was performed using a supra-umbilical 4-cm incision. Docking time was 20 min, and the total operative time was 255 min, with 50 mL of blood loss and 30 min of intermittent hepatic pedicle clamping. No drains were placed. Postoperative pain was ≤ 1 on the Visual Analog Scale, and the patient was discharged on postoperative day 3 without any complications. Histology showed a 12-mm breast cancer metastasis with 2-mm clear margins and good cosmesis.
According to published case series and comparative studies, SP robotic liver resections are technically feasible and safe, with reduced postoperative pain, shorter hospital stays, and improved cosmesis. However, current evidence is limited to selected minor resections, and longer follow-up is necessary to validate the oncological outcomes.
Core Tip: This case highlights the feasibility and safety of performing a left lateral segmentectomy for a segment II liver metastasis from breast carcinoma performed using the da Vinci single-port (SP) platform, underscoring the potential advantages of SP robotic surgery in complex hepatic resections.
- Citation: Caringi S, Delvecchio A, Casella A, Ferraro V, Riccelli U, Stasi M, Manzia TM, Tedeschi M, Memeo R. Robotic left lateral sectionectomy with the da Vinci single-port system: A case report. World J Clin Cases 2026; 14(10): 117286
- URL: https://www.wjgnet.com/2307-8960/full/v14/i10/117286.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i10.117286
The introduction of robotic platforms has revolutionized surgery, particularly hepatopancreatobiliary (HPB) surgery. The advantages of robotic surgery in HPB procedures are now widely recognized, combining the benefits of minimally invasive surgery with robotic technologies[1-3]. With the advantages of 3D visualization, wristed instrument control, increased dexterity, and integrated energy devices, the robotic platform allows complex surgeries, including liver transplantation, to be performed in a minimally invasive manner[2,4-6].
For many years, the da Vinci multi-port system has been the predominant robotic platform and has improved over time with the introduction of new models. Unlike previous models, the most recent platform is the da Vinci single-port (SP) system, an innovation designed to facilitate complex surgeries through a single incision, further reducing surgical invasiveness[7,8].
In this paper, we aim to share our experience with the new system, including a video of the first liver resection performed in Italy using the da Vinci SP system, the operating room setup (ORS), and key intraoperative technical aspects.
This case report was prepared in accordance with the CARE guidelines.
The patient was a 51-year-old woman with an American Society of Anesthesiologists classification of II and a body mass index of 22.5 kg/m2.
The patient underwent annual outpatient oncological follow-ups, which included computed tomography (CT) scans. One of these scans revealed a lesion in the second hepatic segment, which was suspected to be a metastasis.
Four years earlier, the patient had undergone a quadrantectomy of the right breast with sentinel lymph node biopsy, followed by adjuvant chemotherapy and radiotherapy for breast cancer.
The personal and family history of the patient was unremarkable.
The patient was in excellent general condition, with good vital signs and a normal general physical examination.
The patient’s blood test results, including carbohydrate antigen 15-3 and carcinoembryonic antigen values, were within normal ranges when measured shortly before the oncology follow-up outpatient visit.
The case was reviewed by our oncology board, comprising HPB surgeons, radiologists, interventional radiologists, oncologists, radiotherapists, endoscopists, and gastroenterologists. The board recommended upfront surgery, which in this case consisted of a left lateral liver sectionectomy.
Single breast cancer liver metastasis of 12 mm.
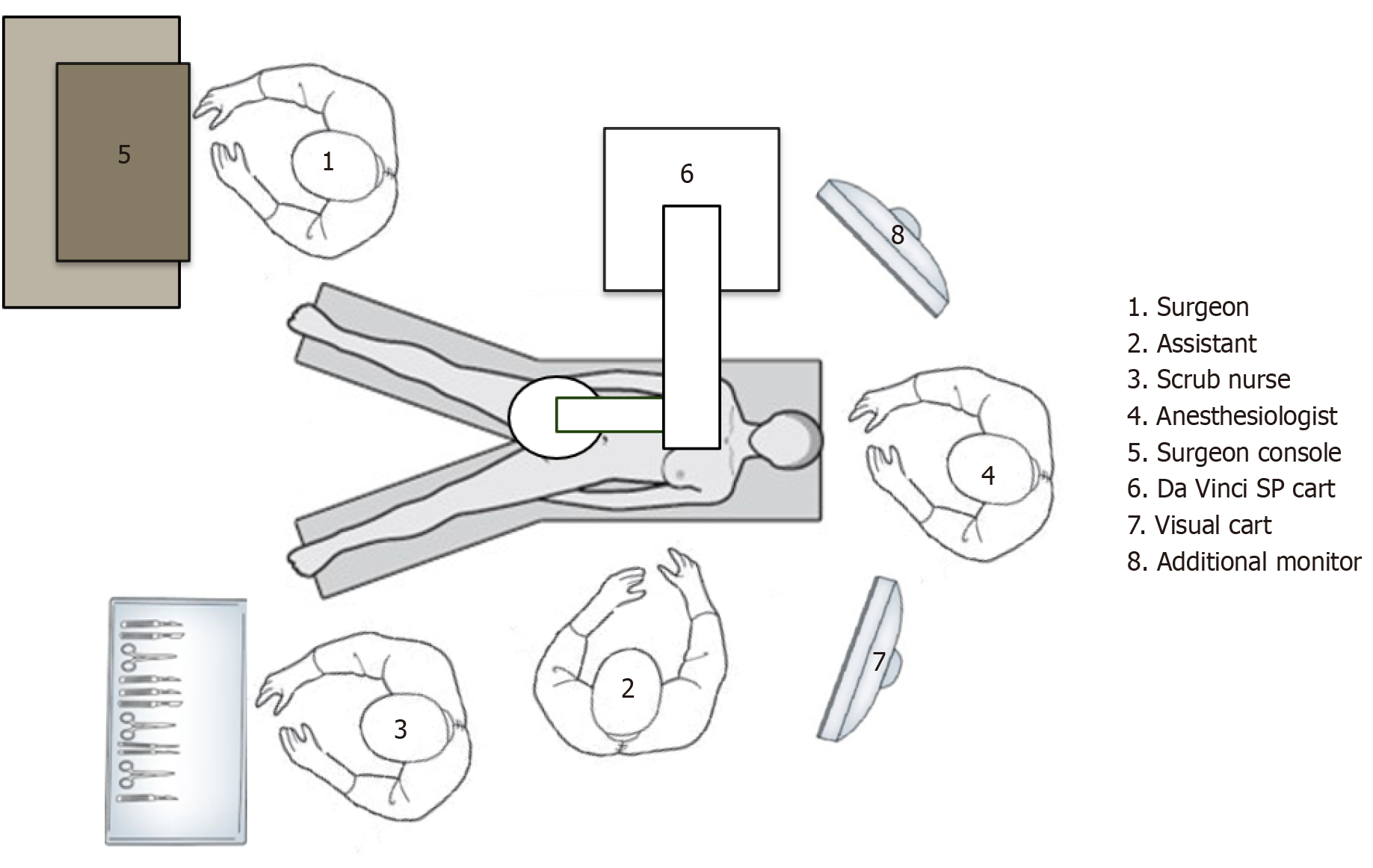
The ORS (Figure 1) is an often underestimated yet crucial step in surgery[9,10]. Correct ORS has been shown to improve efficiency, teamwork, and safety, and decrease interruptions and infections. This ORS was decided upon in agreement with surgeons, anesthetists, scrub nurses, and intuitive clinical specialists.
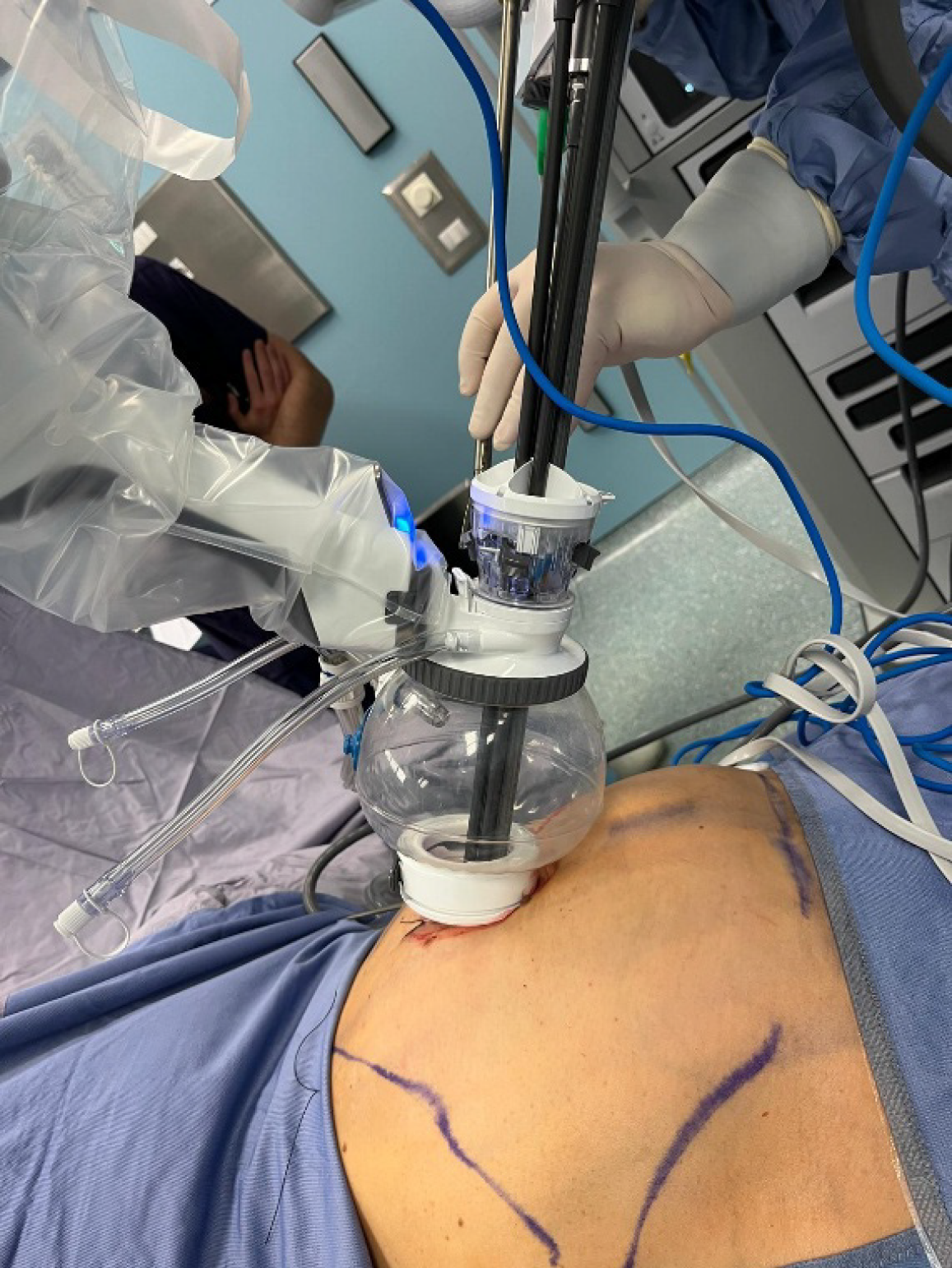
Docking is a crucial step for the success of robot-assisted procedures, and based on our initial experience, SP docking is faster and easier than multi-port docking. In a multi-port system, the distances between trocars, assisting ports, and the target zone must be carefully calibrated to ensure optimal system maneuverability and effective assistance from the bedside surgeon. With the SP system, these requirements are eliminated, as an incision of 2.5-4 cm is sufficient to position the Access Port Kit©, a device consisting of a wound protector, a short entry guide, and the access port (Figure 2).
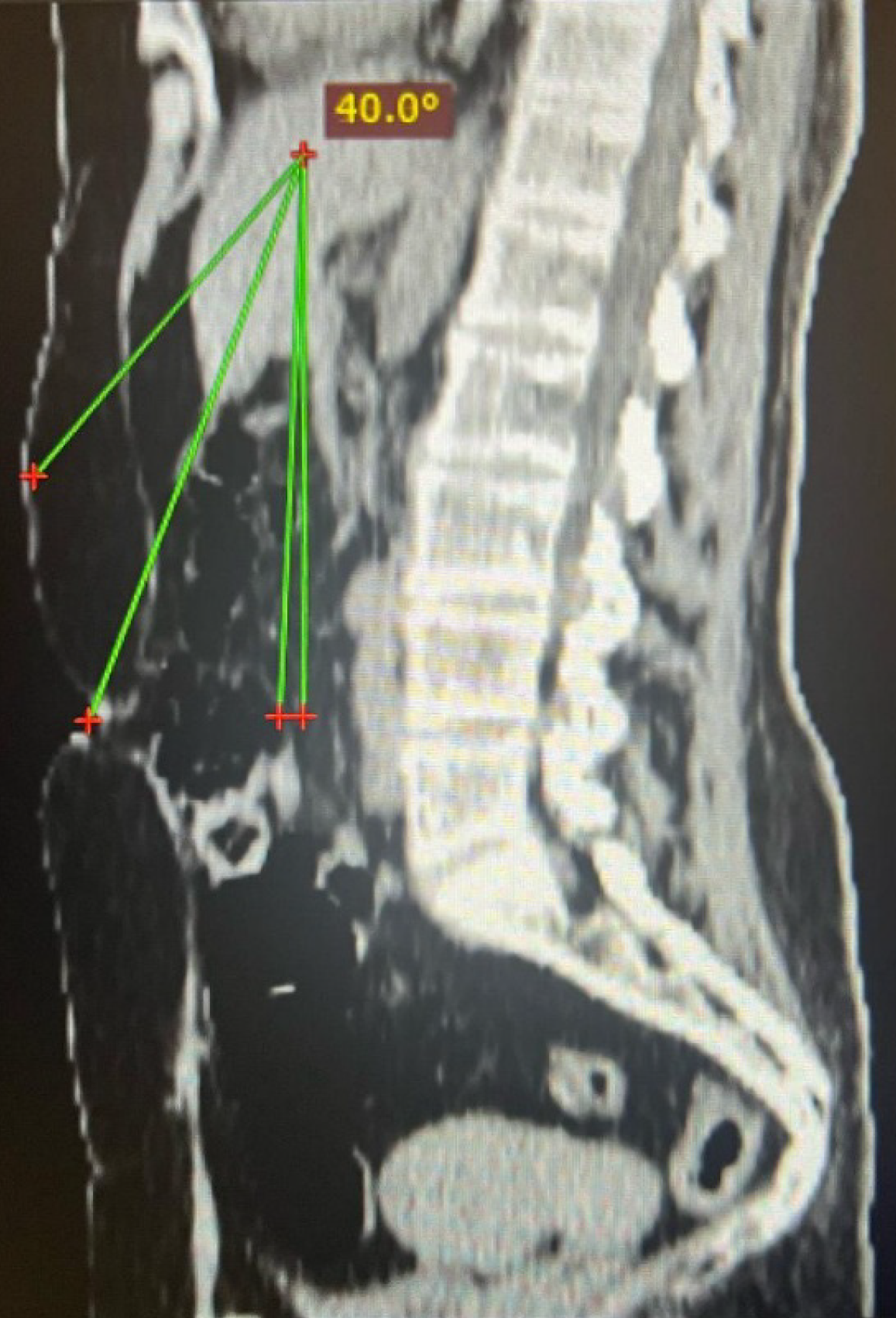
In the SP system, there is no organ targeting as in the multi-port system. However, based on our experience, we have started to perform preoperative organ targeting (POT) using preoperative CT scans (Figure 3). Using this method, we are able to optimize the site of the median incision with good approximation, taking into account the length of the SP instruments and their working angles. These two parameters are crucial because an excessive distance leads to uncom
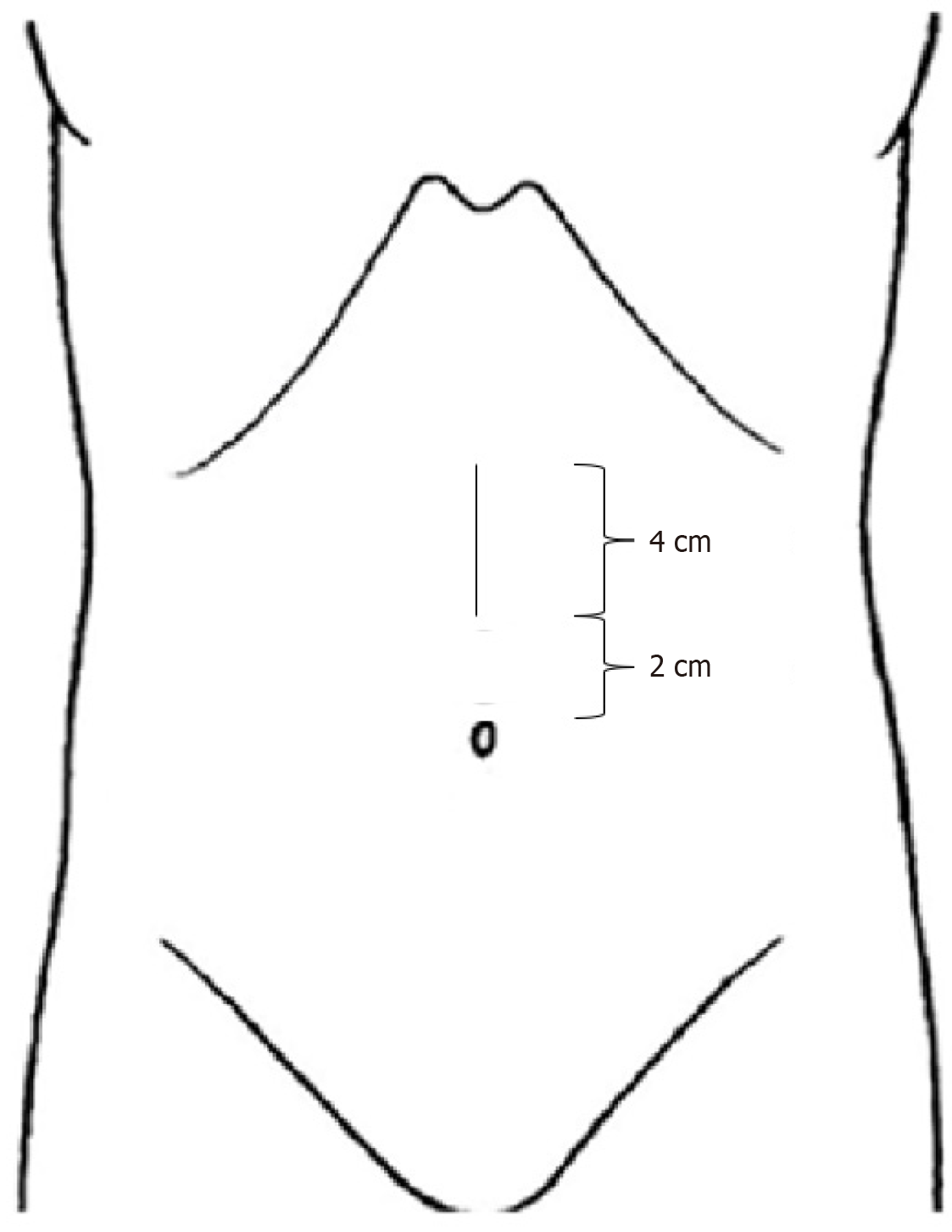
By analyzing the images in our preoperative surgical meeting, we observed that the lesion was close to the left hepatic vein. Therefore, we decided to perform a left lateral sectionectomy, an intervention of intermediate difficulty, according to the TAMPA classification system[11]. Using POT, we performed a median incision of approximately 4 cm, starting 2 cm above the umbilicus (Figure 4).
As in any robotic liver resection, the procedure begins with opening the falciform ligament, sectioning the round liga
The resected liver segment was then placed in an EndoBag and extracted from the median incision after SP dedocking.
The total duration of the procedure was 255 min, including 20 min of docking time. Estimated blood loss was 50 mL, and hepatic hilum clamping was performed for 30 min. Surgical drainage was not performed. The patient had no post
On the final histological examination, the lesion was confirmed to be a 12-mm liver metastasis from the breast cancer, with 2-mm clear surgical margins.
At the 3-month outpatient follow-up, the patient was in excellent general condition, reported no problems, and was fully satisfied with the surgical incision.
The da Vinci SP robotic system is a significant advancement in minimally invasive surgery. Compared with established multi-port robotic platforms, the da Vinci SP system presents certain technical advantages and limitations that are particularly relevant in hepatobiliary surgery. In multi-port systems, instrument triangulation is achieved by spatially separating the trocars, allowing for a wide range of approaches and robust exposure, particularly during parenchymal transection and vascular control. In contrast, the SP system relies on the intracorporeal articulation of instruments deployed through a single cannula, which may limit external triangulation; however, this limitation is at least partially compensated by the use of fully wristed instruments and an articulated camera.
Maneuverability in SP surgery generally allows for peripheral and anterior liver segments procedures. However, deep or posterior lesions may pose challenging conditions owing to restricted retraction angles and limited countertraction. Thus, exposure depends more on precise preoperative planning, optimal port positioning, and effective use of the third robotic arm. Vascular control can be safely performed in SP procedures in selected cases; however, the absence of multiple assistant ports may limit immediate access for suction, retraction, or rapid bleeding control, increasing reliance on bedside assistants through a single access port.
Although initial experience suggests that SP robotic liver resections can be performed with acceptable perioperative results in highly selected patients, current evidence remains limited to small case reports and isolated publications[15-17]. Therefore, caution must be exercised when interpreting the available data to assess safety, determine relative superiority, or support adoption in routine clinical practice.
Among the larger comparative studies, 304 patients underwent robotic cholecystectomy, of whom 145 were treated using the da Vinci SP system and 159 using the Xi system. In the SP group, mean operating times were slightly shorter (45.7 min vs 49.8 min), docking times were significantly shorter (5.7 min vs 8.8 min, P = 0.024), early postoperative pain was modestly reduced, and hospital length of stay and morbidity rates were comparable[15].
Another comparative study included 30 consecutive patients with chronic cholecystitis or gallstones who underwent robotic SP cholecystectomy or Si single-site robotic cholecystectomy[16]. The mean docking time for the SP procedures was 5.2 min, the mean dissection time was approximately 14.6 min, and the mean operative time was approximately 75.1 min. The average hospital stay was 1.5 days, and both immediate postoperative pain and pain at discharge were significantly decreased. Learning curve analysis for SP cholecystectomy showed that pre-console, docking, and overall operation times diminished with experience, whereas console time remained relatively constant. This suggests that most of the learning curve lies less in performing the surgery itself than in completing all the preparatory procedures.
The technical feasibility of more challenging hepatobiliary procedures has been demonstrated in several case reports. A left lateral sectionectomy performed without an additional port has a docking time of 8 min, a total operative time of approximately 135 min, and an estimated blood loss of approximately 50 mL. In a previous study, the reported pain scores were low (3/10 at the time of discharge, 1/10 on postoperative day 2), the patient was discharged on day 5, and no intraoperative complications occurred[18]. Another study described a left lateral sectionectomy in a patient with intrahepatic duct stones and distal common bile duct stones (combined biliary tract surgery) using the SP system. The docking time was 8 min, and the estimated blood loss was 50 mL. The patient had a good postoperative recovery, was discharged on day 5, and reported a pain (immediate postoperative Numeric Rating Scale) score of 4/10, which de
The overall safety was acceptable in these relatively small and selected series, with minimal severe complications and low rates of conversion. In most SP minor hepatectomy cases, operative blood loss was minimal, hospital stays were typically short (1-5 days), and postoperative pain scores improved satisfactorily. A comparative series evaluating SP and other robotic single-site or multi-port methods has shown a preference for SP procedures in terms of docking and op
The advantages of the SP system for hepatobiliary surgery include improved cosmesis through an SP approach, fewer incisions with potentially reduced wound complications, lesser postoperative pain, shorter docking times, enhanced ergonomics with wristed instruments, and the availability of third-arm retraction assistance. The SP platform overcomes the limitations of earlier single-site robotic platforms, such as limited instrument articulation, lack of a third arm, and instrument collisions. The SP system also allows for an easier setup compared with some multi-port systems.
The limitations of this report include case selection bias, as most SP hepatobiliary procedures are performed in patients with small peripheral lesions and good anatomy. Advanced resections, such as those for large tumors near major vascular structures or requiring complex bile duct reconstructions, are rarely reported. One constraint relates to instrumentation: Staplers and certain energy devices are not yet fully optimized for the SP system, and the lack of assistant-port access may restrict exposure, retraction, suction, or immediate bleeding control. Cost and resource utilization have also not been directly quantified for the SP system in hepatobiliary surgery. Oncological outcomes, including negative margin rates, disease-free survival, and recurrence rates, have not been well reported, especially for malignant diseases.
Future studies should include prospective comparative trials of SP vs multiport robotic and laparoscopic approaches in hepatobiliary surgery with universal outcomes such as oncologic results, patient-reported outcome measures of pain and quality of life, cost assessment, and long-term follow-up for malignancy[8,15-19]. SP-compatible instruments such as staplers, energy sources, and retractors need further development to facilitate safer and more effective major resections. Simulation and SP-specific training courses may help reduce early operative inefficiencies. Selection criteria for the SP system in hepatobiliary surgery need to be developed based on lesion size and location, patient anatomy, liver function, and comorbidities to optimize patient outcomes and avoid complications.
The da Vinci SP system represents an innovative paradigm shift toward greater minimally invasive capability in hepatobiliary surgery and appears technically feasible in carefully selected cases of minor hepatic resection. The possible benefits include reduced parietal trauma, enhanced cosmesis, and easier docking. At present, it remains unclear whether this technology will prove safer, more effective, or preferable to established multi-port SP systems. Future studies are likely to further clarify its role with respect to oncological efficacy and cost-effectiveness.
| 1. | Delvecchio A, Conticchio M, Inchingolo R, Ratti F, Magistri P, Belli A, Ceccarelli G, Izzo F, Spampinato MG, Angelis ND, Pessaux P, Piardi T, Di Benedetto F, Aldrighetti L, Memeo R. Robotic Major Hepatectomy in Elderly Patient. Cancers (Basel). 2024;16:2083. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 8] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 2. | Ceccarelli G, Avella P, Muttillo EM, Conticchio M, Tebala GD, Piccolo G, Romano L, Memeo R, Rocca A; LIVER-MIND (Minimally Invasive Surgery and pareNchyma transection Devices) Study Group. Devices for minimally invasive liver parenchyma transection: the SICE (Italian Society of Endoscopic Surgery) Italian and International survey. Surg Endosc. 2025;39:4822-4838. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 3. | Caringi S, Delvecchio A, Conticchio M, Ratti F, Magistri P, Belli A, Ceccarelli G, Izzo F, Spampinato MG, De'Angelis N, Pessaux P, Piardi T, Di Benedetto F, Aldrighetti L, Memeo R. Robotic Liver Resection for Hepatocellular Carcinoma: A Multicenter Case Series. Cancers (Basel). 2025;17:415. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 4. | Delvecchio A, Caringi S, De Palma C, Brischetto G, Filippo R, Casella A, Ferraro V, Stasi M, Memeo R, Tedeschi M. Step-by-Step Description of Standardized Technique for Robotic Pancreatoduodenectomy. Curr Oncol. 2025;32:302. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 5. | Dehlawi A, Memeo R, DE Blasi V, Mercoli HA, Mutter D, Marescaux J, Pessaux P. Robotic hepatectomies: advances and perspectives. Minerva Chir. 2016;71:407-414. [PubMed] |
| 6. | Delvecchio A, Conticchio M, Riccelli U, Ferraro V, Ratti F, Gelli M, Anelli FM, Laurent A, Vitali GC, Magistri P, Assirati G, Felli E, Wakabayashi T, Pessaux P, Piardi T, Di Benedetto F, de'Angelis N, Briceño-Delgado J, Adam R, Cherqui D, Aldrighetti L, Memeo R. Laparoscopic versus open liver resection for hepatocellular carcinoma in elderly patients: a propensity score matching analysis. HPB (Oxford). 2022;24:933-941. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 14] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 7. | Intuitive Surgical Inc. Da Vinci SP surgical system overview, 2023. Available from: https://www.intuitive.com/en-us/products-and-services/da-vinci/sp. |
| 8. | Kim WJ, Choi SB, Kim WB. Feasibility and Efficacy of Single-Port Robotic Cholecystectomy Using the da Vinci SP® Platform. JSLS. 2022;26:e2021.00091. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 19] [Reference Citation Analysis (0)] |
| 9. | Pasquer A, Ducarroz S, Lifante JC, Skinner S, Poncet G, Duclos A. Operating room organization and surgical performance: a systematic review. Patient Saf Surg. 2024;18:5. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 40] [Article Influence: 20.0] [Reference Citation Analysis (0)] |
| 10. | Quan X. Can Operating Room Design Make Orthopedic Surgeries Shorter, Safer, and More Efficient?: A Quasi-Experimental Study. HERD. 2024;17:7-22. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 1] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 11. | Al Harakeh H, Ross SB, Milivojev Covilo K, Mendez M, Onkendi E, Shah M, Mavani PT, Polanco P, Martinie J, Iannitti D, Hogg M, Hays S, Mehdi SA, Helton S, Geller D, Simo K, El-Hayek K, Warner S, Gudmundsdottir H, Cleary S, Alseidi A, Tohme S, Castillo S, Vanterpool G, Esposito G, Sucandy I. External validation of Tampa Difficulty Scoring System for robotic liver resection using Americas Minimally Invasive Liver Surgery Registry (AMILES). Surg Endosc. 2025;39:8524-8531. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 12. | Sugioka A, Kato Y, Tanahashi Y, Yoshikawa J, Kiguchi G, Kojima M, Yasuda A, Nakajima S, Uyama I. Standardization of Anatomic Liver Resection Based on Laennec's Capsule. Surg Gastroenterol Oncol. 2020;25:57. [DOI] [Full Text] |
| 13. | Chiarella LL, Muttillo EM, Fichtner-Feigl S, Ratti F, Magistri P, Belli A, Ceccarelli G, Izzo F, Spampinato MG, Ercolani G, De Angelis N, Ammendola M, Pessaux P, Piardi T, Di Benedetto F, Aldrighetti L, Tedeschi M, Memeo R. MAMBA (Moisture Assisted Multiple BipolAr) technique vs Robo-lap approach in robotic liver resection. Is it possible a full robotic approach for parenchymal transection? A propensity score matching analysis. Surg Endosc. 2025;39:2721-2728. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 8] [Reference Citation Analysis (0)] |
| 14. | Karcioglu O, Topacoglu H, Dikme O, Dikme O. A systematic review of the pain scales in adults: Which to use? Am J Emerg Med. 2018;36:707-714. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 846] [Cited by in RCA: 690] [Article Influence: 86.3] [Reference Citation Analysis (0)] |
| 15. | Cruz CJ, Huynh F, Kang I, Lee WJ, Kang CM. Initial experiences of robotic SP cholecystectomy: a comparative analysis with robotic Si single-site cholecystectomy. Ann Surg Treat Res. 2021;100:1-7. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 18] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 16. | Ramacciotti N, Celotto F, Pinto F, Cassiani J, Danieli G, Spolverato G, Morelli L, Bianco FM. Learning Curve for da Vinci Single-Port Robotic System Cholecystectomy. Surg Laparosc Endosc Percutan Tech. 2025;35:1-7. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 17. | Caringi S, Delvecchio A, Casella A, Palma C, Ferraro V, Filippo R, Stasi M, Tralli N, Manzia TM, Tedeschi M, Memeo R. The da Vinci Single-Port Robotic Platform in General Surgery: A Scoping Review of Current Applications and Outcomes. J Clin Med. 2025;14:8212. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 18. | Kim WJ, Park PJ, Choi SB, Kim WB. Case report of pure single-port robotic left lateral sectionectomy using the da Vinci SP system. Medicine (Baltimore). 2021;100:e28248. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 16] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 19. | Kim WJ, Kim WB, Choi SB. Technical feasibility of single-port robotic left lateral sectionectomy using the da Vinci SP surgical platform. Int J Surg. 2022;100:106500. [RCA] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |