Published online Apr 15, 2026. doi: 10.4251/wjgo.v18.i4.115687
Revised: December 11, 2025
Accepted: January 19, 2026
Published online: April 15, 2026
Processing time: 154 Days and 23 Hours
Colorectal cancer (CRC) presents a significant global health burden, with considerable variation in survival following curative surgery. Identifying patients at high risk of poor outcomes is crucial for tailored treatment and surveillance strategies. Evidence indicates that individual prognostic markers, whether tumor-associated or inflammation-based, offer limited predictive value. This study posits that a combined model integrating carcinoembryonic antigen (CEA), neutrophil-to-lymphocyte ratio (NLR), and platelet-to-lymphocyte ratio (PLR) will provide a more accurate and robust prediction of postoperative survival in patients with CRC than any single biomarker alone.
To evaluate the prognostic value of combined CEA, NLR, and PLR in CRC.
This study retrospectively enrolled 120 CRC patients who underwent radical resection from July 2021 to July 2022. Based on three-year survival status, patients were classified into a mortality group (43 patients) and a survival group (77 patients). Baseline NLR, PLR, and CEA levels were compared between groups. Cox proportional hazards regression and receiver operating characteristic curve analyses were used to identify survival risk factors and evaluate prognostic utility.
Among 120 patients, 43 died within 3 years postoperatively, yielding a mortality rate of 35.83%. Comparing clinical data between groups, the deceased group displayed significantly higher serum levels of NLR, PLR, and CEA than the surviving group, along with a higher proportion of tumors > 5 cm in diameter and distant metastases (P < 0.05). Cox regression analysis demonstrated that elevated postoperative serum NLR, PLR, and CEA levels constitute risk factors for postoperative survival in CRC patients. Receiver operating characteristic curve analysis revealed that the area under the curve for predicting postoperative survival using NLR, PLR, and CEA individually were 0.896, 0.805, and 0.880, correspondingly. The integrated area under the curve for the three biomarkers was 0.977, indicating significantly higher predictive value than any single marker (P < 0.0001).
Combined assessment of inflammatory markers NLR, PLR and tumor marker CEA provides valuable prognostic information for CRC patient survival.
Core Tip: This study investigated the predictive value of the inflammatory markers neutrophil-to-lymphocyte ratio and platelet-to-lymphocyte ratio combined with the tumor marker carcinoembryonic antigen for postoperative survival in patients with colorectal cancer. The results showed that the combined detection of the three markers demonstrated significantly superior predictive efficacy compared to any single indicator, providing an efficient and convenient clinical tool for assessing the prognosis of colorectal cancer patients.
- Citation: Wang T, Liu C, Jiang J. Clinical prediction of carcinoembryonic antigen combined with neutrophil-to-lymphocyte ratio and platelet-to-lymphocyte ratio for postoperative survival in colorectal cancer. World J Gastrointest Oncol 2026; 18(4): 115687
- URL: https://www.wjgnet.com/1948-5204/full/v18/i4/115687.htm
- DOI: https://dx.doi.org/10.4251/wjgo.v18.i4.115687
Colorectal cancer (CRC), a malignant tumor rooted in the mucosal epithelium of the colon and rectum, constitutes a substantial global public health burden. Globally, it ranks as the third most commonly diagnosed cancer and the second primary leading cause of cancer mortality[1]. In recent years, with changes in lifestyle, adjustments in dietary patterns, and the continuous deepening of population aging, the disease burden of CRC has shown a persistent upward trend. Statistical data reveal that over 1900000 new CRC cases were documented across the globe in 2020, while the number of deaths caused by this disease stood at 930000. Forecasts indicate that by 2040, new case incidence will rise to 3200000, and mortality figures will hit 1600000, posing a significant threat to public health[2]. Currently, surgery remains the primary treatment for CRC. However, surgical intervention itself imposes significant physical trauma on patients, potentially triggering a range of postoperative complications. Moreover, postoperative recovery and survival outcomes vary considerably among different patients. Therefore, there exists a critical demand in clinical settings for a convenient and accurate prognostic assessment tool to predict postoperative survival in CRC patients. This would enable clinicians to develop treatment plans and improve patient survival outcomes[3]. In recent years, inflammation-related biomarkers obtainable through routine blood tests have garnered widespread attention for their value in cancer prognosis assessment due to advantages such as ease of detection, low cost, and minimal technical requirements. Among these, neutrophil-to-lymphocyte ratio (NLR) and platelet-to-lymphocyte ratio (PLR) are the most widely reported inflammatory markers. Studies have confirmed that the dynamic changes in preoperative NLR and PLR hold significant predictive value for postoperative performance, the development of complications, and adverse prognostic outcomes in patients suffering from CRC[4-6]. Beyond inflammatory mediators, the tumor marker carcinoembryonic antigen (CEA) also holds a pivotal role in the diagnostic and therapeutic processes of CRC. CEA is a glycoprotein widely expressed in various malignancies including CRC and gastric cancer. Cell adhesion molecule 6, a participant in the CEA family, operates as a glycosylphosphatidylinositol-anchored glycoprotein and is distributed on the cell surface. Elevated expression of this marker is frequently observed in diverse types of malignancies, encompassing pancreatic, breast, non-small cell lung, gastric, and CRCs, promoting tumor progression, invasion, and metastasis[7,8]. Preoperative CEA measurement also serves as a method for predicting postoperative prognosis in CRC patients[9]. Although earlier research has documented the functions of NLR, PLR, and CEA in prognostic assessment for CRC patients, systematic investigation into the predictive value of combined testing for postoperative survival in CRC patients remains lacking. Therefore, this study aims to systematically analyze preoperative NLR, PLR, and CEA levels in CRC patients and assess the predictive value of their combined application for postoperative survival. The objective is to provide a novel approach for assessing postoperative survival in CRC patients and to offer a reference basis for developing individualized clinical management strategies.
This study was performed involving 120 patients who received surgical resection for CRC at The First Affiliated Hospital of Hebei North University from July 2021 to July 2022. The patient group consisted of 66 men and 54 women, aged between 42 and 75 years. All patients underwent preoperative serum NLR, PLR, and CEA testing, followed by a 3-year follow-up.
Inclusion criteria: (1) Pathologically and radiologically confirmed CRC; (2) Clinically assessed as suitable for radical resection; (3) No severe hepatic or renal impairment; (4) No infectious diseases affecting the heart or lungs; (5) No hematologic disorders affecting neutrophils, monocytes, or lymphocytes; and (6) Full understanding of the study and signed informed consent.
Exclusion criteria: (1) Patients with concomitant malignancies such as gastric or lung cancer; (2) Perioperative mortality; (3) Incomplete case documentation; (4) History of prior colorectal surgery; and (5) Postoperative loss to follow-up or refusal to participate in follow-up.
The sample size was calculated based on the formula proposed by Hsieh and Lavori[10]: N = [(Z1-α/2 + Z1-β)2]/[P(1 - R2)σ2 B2]. With reference to the study by Zhang et al[11], the 3-year mortality rate for CRC patients was set at 45.0%. The coefficient R² from the regression analysis of CEA as the dependent variable against other covariates was set to 0.2; the variance σ2 of CEA was set to 1; and the log hazard ratio B was set to 0.6. The calculation was performed using PASS 15.0 software. With a significance level of 0.05 and a statistical power of 0.9, the minimum required sample size was determined to be 82 cases. Accounting for an estimated dropout rate of 20%, a minimum of 103 cases was required. Therefore, a final total of 120 cases were included for analysis, which meets the sample size requirements for this study.
Clinical data collection: Drawing upon prior literature regarding postoperative outcomes in CRC patients and incorporating expert input, the baseline data survey form for CRC patients was developed. Investigators underwent standardized training and followed a uniform protocol to collect clinical data from study subjects. The following set of variables was recorded for analysis: (1) Patient gender, age, and body mass index; (2) Tumor-related characteristics: Tumor size, tumor location, clinical stage, depth of invasion, histological subtype, presence of distant metastasis; and (3) Serum levels of inflammatory markers NLR and PLR, and tumor marker CEA.
Serum NLR, PLR, and CEA testing: All patients underwent testing within one week prior to surgery. To ensure accuracy and reliability of results, patients fasted for 8 hours before testing to maintain a fasting state. Five milliliters of blood were collected from the patient’s antecubital vein and divided into two tubes: (1) Two milliliters of the sample was dispensed into an EDTA anticoagulant tube. A Sysmex XN-1000 automated hematology analyzer was used to measure the complete blood count, after which counts of neutrophils, lymphocytes, and platelets were obtained. The NLR and PLR were then computed based on these counts; and (2) Three milliliters is placed into a clotting tube. Centrifuge at 3000 r/minute for 10 minutes to isolate serum. Detect CEA levels using the AutoLumo A2000 Plus chemiluminescent immunoassay analyzer. The detection range is 3-1000 ng/mL, with a normal reference value < 5.0 ng/mL.
Follow-up protocol: Follow-up duration commenced on the day of patient discharge. Monitoring was conducted via telephone, outpatient visits, or readmission. Follow-up intervals were quarterly for the first-year post-surgery, then biannually from years 2 to 3. Overall length of survival is delineated as the interval from the date of curative surgery to death resulting from any cause. If a patient survives beyond 3 years of follow-up or dies from non-CRC causes, the last follow-up date is used as the censored endpoint.
SPSS 25.0 software was utilized to conduct statistical analyses. Continuous variables were presented as mean ± SD, and intergroup comparisons were carried out with Student’s t test. Categorical variables were summarized in the form of n (%), while comparisons of these variables between groups were conducted by χ2 test. To identify independent prognostic factors influencing postoperative survival, multivariate Cox regression analysis was applied. The predictive efficacy of individual indicators and combined indicator panels was evaluated through the use of receiver operating characteristic (ROC) curves. Statistical significance was defined at P < 0.05 throughout all analyses.
Follow-up through July 2025 revealed that 43 of the 120 patients died from CRC-related causes, resulting in a 3-year postoperative mortality rate of 35.83%. Comparison of clinical data between the two groups showed statistically significant differences in tumor-related characteristics: Tumor size and distant metastasis status. The percentage of patients with tumors exceeding 5 cm in diameter was significantly higher in the deceased group than in the surviving group with tumors of the same size (P < 0.05). Simultaneously, the proportion of patients with distant metastasis in the mortality group was considerably greater than that in the survival group (P < 0.05). However, no statistically significant intergroup disparities were observed in the comparisons of sex, age, body mass index, tumor location, and disease stage (P > 0.05; Table 1). NLR, PLR, and CEA measurements revealed that the percentage of inflammatory markers NLR and PLR were markedly elevated in non-survivors compared to survivors (P < 0.0001). Serum tumor marker CEA levels were likewise markedly elevated in non-survivors compared to survivors (P < 0.0001; Table 2).
| Clinical data | Survival group (n = 77) | Death group (n = 43) | t/χ2 | P value | |
| Gender | Male | 42 (54.55) | 24 (55.81) | 0.018 | 0.893 |
| Female | 35 (45.45) | 19 (44.19) | |||
| Age (years) | 60.32 ± 6.85 | 61.02 ± 7.01 | 0.5313 | 0.5962 | |
| Body mass index (kg/m2) | 21.77 ± 1.49 | 21.65 ± 1.54 | 0.4179 | 0.6768 | |
| Tumor size (cm) | ≤ 5 | 47 (61.04) | 14 (32.56) | 8.955 | 0.003 |
| > 5 | 30 (38.96) | 29 (67.44) | |||
| Tumor location | Colon | 39 (50.65) | 21 (48.84) | 0.036 | 0.849 |
| Rectum | 38 (49.35) | 22 (51.16) | |||
| Clinical stage | I-II | 31 (40.26) | 14 (32.56) | 0.698 | 0.403 |
| III-IV | 46 (59.74) | 29(67.44) | |||
| Depth of invasion | T1-T2 | 48 (62.34) | 25 (58.14) | 0.204 | 0.651 |
| T3-T4 | 29 (37.66) | 18 (41.86) | |||
| Histological subtype | Adenocarcinoma | 35 (45.45) | 21 (48.84) | 0.127 | 0.772 |
| Others | 42 (54.55) | 22 (51.16) | |||
| Distant metastasis | Yes | 1 (1.30) | 5 (11.63) | 4.21 | 0.040 |
| No | 76 (98.70) | 38 (88.37) |
| Indicator | Survival group (n = 77) | Death group (n = 43) | t/χ2 | P value |
| NLR (%) | 2.98 ± 0.57 | 4.83 ± 1.25 | 11.11 | < 0.0001 |
| PLR (%) | 136.26 ± 2.54 | 162.33 ± 27.67 | 8.232 | < 0.0001 |
| CEA (ng/mL) | 12.19 ± 4.51 | 20.17 ± 5.29 | 8.722 | < 0.0001 |
Multivariate Cox regression analysis was performed with tumor size, distant metastasis, NLR, PLR, and CEA as independent variables, and postoperative patient survival status (1 = death, 0 = survival) as the dependent variable. Results indicated that tumor size and distant metastasis did not significantly influence postoperative survival in the multivariate model (P > 0.05). Conversely, serum NLR, PLR, and CEA levels demonstrated significant effects on postoperative survival in regression analysis, establishing them as independent predictors of patient survival (P < 0.05; Table 3).
| Factors | β | SE | Wald | OR (95%CI) | P value |
| Tumor size | 0.331 | 0.348 | 0.905 | 1.393 (0.704-2.758) | 0.341 |
| Distant metastasis | 0.299 | 0.320 | 0.873 | 1.348 (0.720-2.524) | 0.350 |
| NLR | 0.460 | 0.143 | 10.327 | 1.585 (1.197-2.098) | 0.001 |
| PLR | 0.021 | 0.007 | 8.414 | 1.021 (1.007-1.036) | 0.004 |
| CEA | 0.123 | 0.027 | 21.163 | 1.131 (1.073-1.192) | 0.000 |
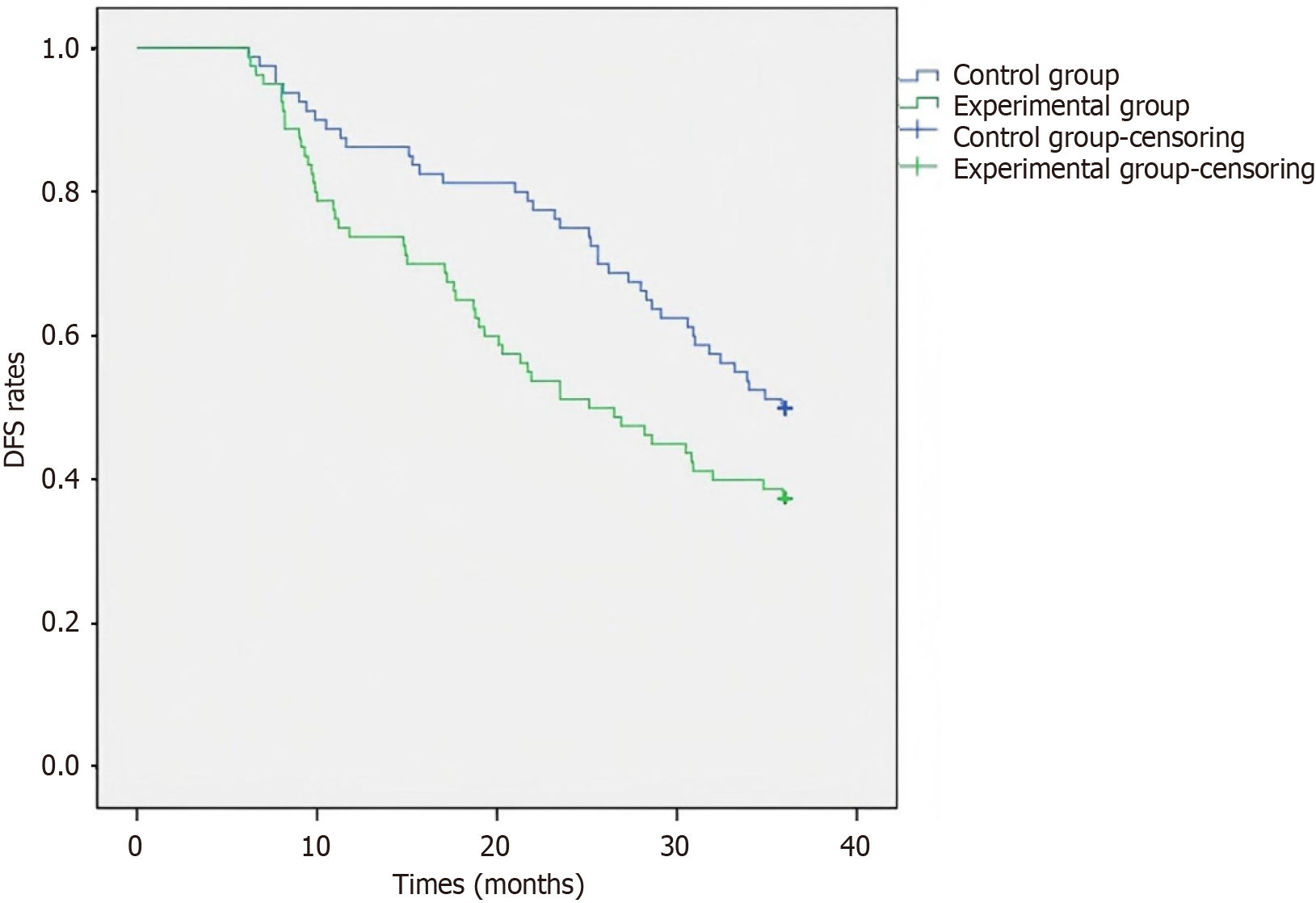
Using postoperative survival and mortality outcomes of CRC patients as the standard, probability values for predicting CRC prognosis were calculated via a Cox regression model to plot ROC curves. The predictive performance of individual markers and combined detection was then evaluated through ROC curve analysis. Results showed that NLR, PLR, and CEA attained area under the curve (AUC) values of 0.896, 0.805, and 0.880; sensitivities of 76.74%, 76.74%, and 81.40%; and true negative rates of 96.10%, 98.70%, and 80.52%, respectively; CEA alone yielded an AUC of 0.880, sensitivity of 81.40%, and specificity of 80.52%. Combined detection of NLR, PLR, and CEA elevated the AUC to 0.977 with sensitivity reaching 97.67%, demonstrating significant improvements in both AUC and sensitivity compared to individual markers. The specificity was 93.51%, slightly lower than that of PLR alone but higher than that of CEA alone. The differences between combined detection and individual detection metrics were statistically significant (P < 0.0001; Table 4, Figure 1).
| Indicator | AUC | Optimal cutoff | Youden index | Sensitivity (%) | Specificity (%) | 95%CI | P value |
| NLR | 0.896 | 4.01 | 0.7284 | 76.74 | 96.10 | 0.828-0.945 | < 0.0001 |
| PLR | 0.805 | 141.14 | 0.7544 | 76.74 | 98.70 | 0.723-0.872 | < 0.0001 |
| CEA | 0.880 | 15.49 | 0.6192 | 81.40 | 80.52 | 0.817-0.923 | < 0.0001 |
| Joint detection | 0.977 | 0.9118 | 97.67 | 93.51 | 0.931-0.996 | < 0.0001 |
As one of the most prevalent malignancies globally, CRC constitutes a key threat to public health and continues to be a principal cause of cancer-related mortality. Surgery remains the main treatment modality for CRC, yet postoperative survival outcomes vary significantly among patients, making postoperative survival assessment a persistent core challenge in clinical practice[12]. Serum biomarkers offer advantages such as simplicity, accessibility, objectivity, cost-effectiveness, rapidity, and accuracy. Currently, multiple serum biomarkers have been demonstrated to hold significant value in diagnosing various cancers and predicting cancer prognosis[13-15]. In this study, clinical data from 120 patients diagnosed with CRC were analyzed retrospectively to evaluate the prognostic value of combining the systemic inflammatory indicators (NLR and PLR) with the CEA, a tumor marker, in postoperative survival among CRC patients. The aim is to provide more efficient and reliable clinical tools for assessing postoperative survival in CRC.
As early as the 19th century, Virchow and others first proposed the concept that inflammation is closely associated with tumors. Follow-up studies have further confirmed that inflammatory cells and cytokines within the tumor microenvironment are pivotal in driving tumor growth and progression, via mechanisms such as enhancing tumor cell proliferation, speeding up tumor angiogenesis, and suppressing the body’s immune function[16]. In terms of specific mechanisms, inflammatory cells such as neutrophils or platelets can enhance tumor inflammatory responses, thereby driving tumor proliferation, invasion, and metastasis. Lymphocytes, conversely, can eliminate tumor cells by inducing cytotoxic immune responses. The functional balance between inflammatory and immune cells directly correlates with cancer patient prognosis[17]. The NLR, computed from routine blood cell counts, often indicates poorer prognosis when elevated during cancer diagnosis and treatment[18]. Earlier research investigations have confirmed that NLR correlates with reduced overall survival (OS) and increased recurrence risk in patients with various malignancies, including oropharyngeal cancer[19] and breast cancer[20]. For CRC patients, preoperative NLR levels not only reflect systemic inflammatory status but also indicate the body’s immune response capacity against tumors[21]. This study’s findings indicate that when comparing non-survivors and survivors, the former exhibited significantly higher NLR levels. Moreover, multivariate Cox regression analysis identified NLR serving as a separate correlate for postoperative survival in patients with CRC. These results align with those reported in previous studies, suggesting that elevated NLR may promote postoperative disease progression and increase mortality risk in CRC patients by exacerbating inflammatory responses and suppressing immune function.
The PLR acts as another commonly employed marker linked to inflammation that holds significant importance in tumor prognosis assessment. Studies demonstrate that among individuals suffering from advanced non-small cell lung cancer receiving immunotherapy, low PLR levels are closely associated with prolonged OS and progression-free survival (PFS), as well as improved objective response rate and disease control rate[22]. Among patients with a diagnosis of gastric cancer and who received immune checkpoint inhibitor treatment, raised PLR levels had a significant connection to worse OS and reduced PFS[23]. In this investigation, PLR levels were markedly elevated in non-survivors compared to survivors. Furthermore, Cox regression analysis revealed that the PLR was an independent predictor of postoperative survival in individuals with CRC, further confirming its validity as an effective prognostic indicator. Elevated PLR levels may indicate poor postoperative survival outcomes.
CEA is an acidic glycoprotein and one of the leading frequently utilized tumor markers in clinical settings. Under physiological conditions, CEA is primarily expressed in fetal gastrointestinal tissues, with extremely low serum levels in adults. Elevated CEA levels are closely associated with poor prognosis in tumors. Consequently, serum CEA concentration is extensively utilized for tumor prognosis and recurrence monitoring[24]. For example, in patients with pancreatic ductal adenocarcinoma, combined serum CEA and carbohydrate antigen 19-9 testing effectively assesses tumor aggressiveness, predicts recurrence rates, and estimates OS[25]. The findings of this study demonstrate that CEA levels exhibited a notable elevation in non-survivors when contrasted with surviving individuals. Furthermore, CEA was established acting as an independent predictor of postoperative survival in CRC patients, demonstrating an AUC of 0.880, sensitivity of 81.40%, and specificity of 80.52% when used alone for prognosis. This demonstrates that CEA has predictive utility for survival outcomes following surgery in CRC.
In clinical practice, NLR and PLR are commonly employed in conjunction with others for the diagnosis and prognostic evaluation of various cancer types. For instance, among individuals diagnosed with central non-small cell lung carcinoma, elevated NLR, MLR and PLR simultaneously indicate poor prognosis[26]. In ovarian cancer patients, combined NLR and PLR testing more accurately predicts OS and PFS[27]; among individuals diagnosed with locally advanced gastric carcinoma, pre-treatment combined NLR and PLR can predict tumor regression grade after neoadjuvant chemotherapy[28]. For CRC diagnosis, combined NLR, red blood cell distribution width, and PLR testing yields higher accuracy than single-marker assessment[29]. However, individual markers often fail to provide a comprehensive reflection of the complex biology underlying tumors. NLR and PLR only indicate inflammatory and immune states but cannot directly reflect tumor cell proliferation or invasive capacity. Although CEA correlates with tumor biology, its limited specificity precludes its use as an independent diagnostic tool, necessitating its combination with imaging and multiple biomarkers[24]. For instance, the combination of NLR, prognostic nutritional index, D-Dimer, CD3 T cells, and CEA offers valuable insight for the early screening and auxiliary diagnosis of CRC[30]. In advanced non-small cell lung cancer, computed tomography examination combined with CEA detection significantly improves lesion detection rates[31]. In CRC, NLR, PLR, and CEA have been established as potential and readily accessible prognostic biomarkers[32]. Therefore, this study combined the advantages of NLR, PLR, and CEA to explore their joint predictive value for postoperative survival in CRC patients. ROC curve analysis based on the Cox regression model for predicting the prognosis of CRC demonstrated that the AUCs for predicting postoperative survival using NLR, PLR, and CEA alone were 0.896, 0.805, and 0.880, respectively. The combination of all three markers achieved an AUC of 0.977 and a sensitivity of 97.67%, significantly outperforming each individual marker (P < 0.0001). These findings indicate that NLR, PLR, and CEA collectively reflect patients’ systemic status from inflammatory and tumor biological perspectives, enabling prediction of postoperative survival. Their combined use effectively overcomes the limitations of individual markers, significantly enhancing predictive accuracy and providing more reliable clinical evidence for precisely assessing postoperative survival prognosis in CRC patients.
Analysis of the potential reasons may include the following aspects. First, elevated NLR and PLR together reflect a state of chronic inflammation and immune suppression in the body, which can promote the growth and metastasis of CEA-positive tumor cells. Second, tumor cells can recruit and activate neutrophils and platelets by secreting various inflammatory factors, leading to increased NLR and PLR and forming a vicious cycle. Finally, NLR, PLR, and CEA are collectively involved in shaping the tumor microenvironment. The interaction among neutrophils, platelets, and CEA-positive tumor cells promotes angiogenesis, immune escape, and extracellular matrix remodeling, thereby creating favorable conditions for tumor cell survival, proliferation, and metastasis.
However, the multivariate Cox regression analysis in this study revealed that after incorporating the predictive factors NLR, PLR, and CEA, tumor size and distant metastasis did not emerge as independent prognostic predictors within this model. This finding diverges from the research of Bae et al[33] and Liu et al[34], among others. We posit several potential explanations for this discrepancy. Firstly, this study included only 120 cases. The relatively small sample size may have reduced the statistical power to detect the effects of these variables, preventing them from reaching significance. Secondly, there is a potential for multicollinearity among NLR, PLR, CEA, and tumor size/distant metastasis. Larger tumors or those that have metastasized are often associated with more pronounced systemic inflammatory responses and higher tumor burden, which correspondingly elevate NLR, PLR, and CEA levels[35]. These markers may, to a considerable extent, reflect biological information related to tumor size, invasion, and metastasis. Research suggests that when blood-based indicators, which more directly and sensitively reflect tumor biological behavior, are introduced into a prognostic model, the independent predictive value of some macroscopic pathological variables may be attenuated or absorbed[36]. However, this by no means diminishes the clinical importance of tumor size and distant metastasis. On the contrary, it suggests that NLR, PLR, and CEA may serve as readily accessible surrogate or complementary indicators that integrate local tumor characteristics with systemic response, offering a novel perspective for prognostic assessment.
There are certain limitations in this study: Firstly, as a singlecenter retrospective analysis, it is susceptible to selection bias and information bias, which may affect the generalizability of the findings. Secondly, although the sample size met the minimum statistical requirement, 120 cases remain relatively limited. Thirdly, due to the observational timeframe, patients were only followed up for three years, which may not capture some longterm events, thereby restricting the extrapolation of the conclusions over a longer period. Fourthly, certain important prognostic factors such as microsatellite instability were not controlled for in the analysis. In the future, it will be necessary to further validate the clinical value of combining NLR, PLR, and CEA in predicting postoperative survival in CRC patients by expanding the sample size, conducting multicenter collaborative studies, incorporating additional potential influencing factors, and extending the followup duration. Furthermore, integrating these markers with other novel biomarkers may enable the development of more comprehensive and precise postoperative survival prediction models for CRC, thereby providing stronger support for clinical treatment.
In summary, serum inflammatory markers NLR and PLR, along with the tumor marker CEA, are all factors independently correlated with postoperative survival results in patients who have CRC. The combined detection of these three markers demonstrates high predictive value for postoperative survival, offering a simple and cost-effective approach that can provides a valuable clinical tool to forecast prognosis of CRC patients after undergoing surgery.
| 1. | Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin. 2021;71:209-249. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76817] [Cited by in RCA: 69607] [Article Influence: 13921.4] [Reference Citation Analysis (45)] |
| 2. | Morgan E, Arnold M, Gini A, Lorenzoni V, Cabasag CJ, Laversanne M, Vignat J, Ferlay J, Murphy N, Bray F. Global burden of colorectal cancer in 2020 and 2040: incidence and mortality estimates from GLOBOCAN. Gut. 2023;72:338-344. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1885] [Cited by in RCA: 1509] [Article Influence: 503.0] [Reference Citation Analysis (8)] |
| 3. | Molenaar CJ, van Rooijen SJ, Fokkenrood HJ, Roumen RM, Janssen L, Slooter GD. Prehabilitation versus no prehabilitation to improve functional capacity, reduce postoperative complications and improve quality of life in colorectal cancer surgery. Cochrane Database Syst Rev. 2022;5:CD013259. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 65] [Cited by in RCA: 71] [Article Influence: 17.8] [Reference Citation Analysis (0)] |
| 4. | Shevchenko I, Grigorescu CC, Serban D, Cristea BM, Simion L, Gherghiceanu F, Costea AC, Dumitrescu D, Alius C, Tudor C, Onisai M, Gradinaru S, Dascalu AM. The Value of Systemic Inflammatory Indices for Predicting Early Postoperative Complications in Colorectal Cancer. Medicina (Kaunas). 2024;60:1481. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 10] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 5. | Yamamoto T, Kawada K, Obama K. Inflammation-Related Biomarkers for the Prediction of Prognosis in Colorectal Cancer Patients. Int J Mol Sci. 2021;22:8002. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 397] [Cited by in RCA: 337] [Article Influence: 67.4] [Reference Citation Analysis (8)] |
| 6. | Naszai M, Kurjan A, Maughan TS. The prognostic utility of pre-treatment neutrophil-to-lymphocyte-ratio (NLR) in colorectal cancer: A systematic review and meta-analysis. Cancer Med. 2021;10:5983-5997. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 111] [Cited by in RCA: 97] [Article Influence: 19.4] [Reference Citation Analysis (8)] |
| 7. | Turner MA, Lwin TM, Amirfakhri S, Nishino H, Hoffman RM, Yazaki PJ, Bouvet M. The Use of Fluorescent Anti-CEA Antibodies to Label, Resect and Treat Cancers: A Review. Biomolecules. 2021;11:1819. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 16] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 8. | Wu G, Wang D, Xiong F, Wang Q, Liu W, Chen J, Chen Y. The emerging roles of CEACAM6 in human cancer (Review). Int J Oncol. 2024;64:27. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 52] [Cited by in RCA: 41] [Article Influence: 20.5] [Reference Citation Analysis (0)] |
| 9. | Lakemeyer L, Sander S, Wittau M, Henne-Bruns D, Kornmann M, Lemke J. Diagnostic and Prognostic Value of CEA and CA19-9 in Colorectal Cancer. Diseases. 2021;9:21. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 146] [Cited by in RCA: 107] [Article Influence: 21.4] [Reference Citation Analysis (0)] |
| 10. | Hsieh FY, Lavori PW. Sample-size calculations for the Cox proportional hazards regression model with nonbinary covariates. Control Clin Trials. 2000;21:552-560. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 293] [Cited by in RCA: 260] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 11. | Zhang Q, Xu R, Zhen W, Bai X, Li Z, Zhang Y, Wu W, Yao Z, Li X. Competing risk and random survival forest models for predicting survival in post-resection elderly stage I-III colorectal cancer patients. Sci Rep. 2025;15:24269. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 12. | Futoh Y, Kumagai Y, Miyato H, Ozawa H, Kanamaru R, Sadatomo A, Ohnishi Y, Koinuma K, Horie H, Yamaguchi H, Lefor AK, Sata N, Kitayama J. Peripheral low-density granulocytes after colorectal cancer surgery in predicting recurrence. BJS Open. 2023;7:zrac154. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 13. | Acharya S, Hegde U, Acharya AB. The clinicopathological implications of serum IL-33 and sST2 as cancer biomarkers: A narrative review. J Oral Biol Craniofac Res. 2025;15:645-658. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 14. | Wu X, Wu H, Liu L, Qiang G, Zhu J. Serum zinc level and tissue ZIP4 expression are related to the prognosis of patients with stages I-III colon cancer. Transl Cancer Res. 2020;9:5585-5594. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 12] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 15. | Sato K, Hikita H, Shigekawa M, Soma K, Yamauchi R, Sung J, Kato S, Sasaki Y, Kudo S, Fukumoto K, Shirai K, Murai K, Tahata Y, Yoshioka T, Nishio A, Saito Y, Kodama T, Sasaki Y, Tatsumi T, Takehara T. The serum tenascin C level is a marker of metabolic disorder-related inflammation affecting pancreatic cancer prognosis. Sci Rep. 2024;14:12028. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 16. | Balkwill F, Mantovani A. Inflammation and cancer: back to Virchow? Lancet. 2001;357:539-545. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6201] [Cited by in RCA: 5754] [Article Influence: 230.2] [Reference Citation Analysis (3)] |
| 17. | Nakamoto S, Ohtani Y, Sakamoto I, Hosoda A, Ihara A, Naitoh T. Systemic Immune-Inflammation Index Predicts Tumor Recurrence after Radical Resection for Colorectal Cancer. Tohoku J Exp Med. 2023;261:229-238. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 63] [Cited by in RCA: 56] [Article Influence: 18.7] [Reference Citation Analysis (0)] |
| 18. | Cupp MA, Cariolou M, Tzoulaki I, Aune D, Evangelou E, Berlanga-Taylor AJ. Neutrophil to lymphocyte ratio and cancer prognosis: an umbrella review of systematic reviews and meta-analyses of observational studies. BMC Med. 2020;18:360. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 540] [Cited by in RCA: 486] [Article Influence: 81.0] [Reference Citation Analysis (1)] |
| 19. | Ng SP, Bahig H, Jethanandani A, Sturgis EM, Johnson FM, Elgohari B, Gunn GB, Ferrarotto R, Phan J, Rosenthal DI, Frank SJ, Fuller CD, Garden AS. Prognostic significance of pre-treatment neutrophil-to-lymphocyte ratio (NLR) in patients with oropharyngeal cancer treated with radiotherapy. Br J Cancer. 2021;124:628-633. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 29] [Cited by in RCA: 27] [Article Influence: 5.4] [Reference Citation Analysis (0)] |
| 20. | Grassadonia A, Graziano V, Iezzi L, Vici P, Barba M, Pizzuti L, Cicero G, Krasniqi E, Mazzotta M, Marinelli D, Amodio A, Natoli C, Tinari N. Prognostic Relevance of Neutrophil to Lymphocyte Ratio (NLR) in Luminal Breast Cancer: A Retrospective Analysis in the Neoadjuvant Setting. Cells. 2021;10:1685. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 33] [Cited by in RCA: 24] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 21. | Chen W, Yi HJ, Chen XQ, Xie WZ, Tang XK, Ye JW, Peng X, Zhang Y, Liang JL, Huang MJ. Prognostic value of the NLR combined with CIP2A in the serum of patients with colorectal cancer. BMC Surg. 2021;21:297. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 22. | Zhou K, Cao J, Lin H, Liang L, Shen Z, Wang L, Peng Z, Mei J. Prognostic role of the platelet to lymphocyte ratio (PLR) in the clinical outcomes of patients with advanced lung cancer receiving immunotherapy: A systematic review and meta-analysis. Front Oncol. 2022;12:962173. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 44] [Cited by in RCA: 40] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 23. | Hou S, Song D, Zang Y, Hao R, Li L, Zhu J. Prognostic relevance of platelet lymphocyte ratio (PLR) in gastric cancer patients receiving immune checkpoint inhibitors: a systematic review and meta-analysis. Front Oncol. 2024;14:1367990. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 5] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 24. | Niedzielska J, Jastrzębski T. Carcinoembryonic Antigen (CEA): Origin, Role in Oncology, and Concentrations in Serum and Peritoneal Fluid. J Clin Med. 2025;14:3189. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 21] [Article Influence: 21.0] [Reference Citation Analysis (0)] |
| 25. | Ermiah E, Eddfair M, Abdulrahman O, Elfagieh M, Jebriel A, Al-Sharif M, Assidi M, Buhmeida A. Prognostic value of serum CEA and CA19-9 levels in pancreatic ductal adenocarcinoma. Mol Clin Oncol. 2022;17:126. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 40] [Cited by in RCA: 38] [Article Influence: 9.5] [Reference Citation Analysis (0)] |
| 26. | Han R, Zhang F, Hong Q, Visar D, Zhan C, Zhao C, Wang F, Zhang S, Li F, Li J, Mu J. NLR, MLR, and PLR are adverse prognostic variables for sleeve lobectomy within non-small cell lung cancer. Thorac Cancer. 2024;15:1792-1804. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 8] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 27. | Zhang CL, Jiang XC, Li Y, Pan X, Gao MQ, Chen Y, Pang B. Independent predictive value of blood inflammatory composite markers in ovarian cancer: recent clinical evidence and perspective focusing on NLR and PLR. J Ovarian Res. 2023;16:36. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 59] [Cited by in RCA: 53] [Article Influence: 17.7] [Reference Citation Analysis (0)] |
| 28. | Wang W, Tong Y, Sun S, Tan Y, Shan Z, Sun F, Jiang C, Zhu Y, Zhang J. Predictive value of NLR and PLR in response to preoperative chemotherapy and prognosis in locally advanced gastric cancer. Front Oncol. 2022;12:936206. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 40] [Cited by in RCA: 36] [Article Influence: 9.0] [Reference Citation Analysis (1)] |
| 29. | Chen W, Xin S, Xu B. Value Research of NLR, PLR, and RDW in Prognostic Assessment of Patients with Colorectal Cancer. J Healthc Eng. 2022;2022:7971415. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 47] [Cited by in RCA: 44] [Article Influence: 11.0] [Reference Citation Analysis (0)] |
| 30. | Ding R, Chen Z, He M, Cen H, Liu Z, Su Y. Application Value of Combined Detection of NLR, PNI, D-Dimer, CD3(+) T Lymphocytes, and CEA in Colorectal Cancer Screening. Dis Markers. 2022;2022:7913025. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 31. | Nasralla A, Lee J, Dang J, Turner S. Elevated preoperative CEA is associated with subclinical nodal involvement and worse survival in stage I non-small cell lung cancer: a systematic review and meta-analysis. J Cardiothorac Surg. 2020;15:318. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 43] [Cited by in RCA: 40] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 32. | Ming-Sheng F, Mei-Ling D, Xun-Quan C, Yuan-Xin H, Wei-Jie Z, Qin-Cong P. Preoperative Neutrophil-to-Lymphocyte Ratio, Platelet-to-Lymphocyte Ratio, and CEA as the Potential Prognostic Biomarkers for Colorectal Cancer. Can J Gastroenterol Hepatol. 2022;2022:3109165. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 29] [Cited by in RCA: 29] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 33. | Bae JH, Song J, Kim JH, Kye BH, Lee IK, Cho HM, Lee YS. Lateral Lymph Node Size and Tumor Distance From Anal Verge Accurately Predict Positive Lateral Pelvic Lymph Nodes in Rectal Cancer: A Multi-Institutional Retrospective Cohort Study. Dis Colon Rectum. 2023;66:785-795. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 11] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 34. | Liu J. Septin-9 gene methylation and carcinoembryonic antigen as key biomarkers in colorectal cancer: A retrospective study on prognosis and recurrence. Medicine (Baltimore). 2025;104:e44095. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 35. | Xiao Z, Wang X, Chen X, Zhou J, Zhu H, Zhang J, Deng W. Prognostic role of preoperative inflammatory markers in postoperative patients with colorectal cancer. Front Oncol. 2023;13:1064343. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 15] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 36. | Zou Y, Glickman H, Pelmus M, Maleki F, Bahoric B, Lecavalier-Barsoum M, Enger SA. Tumour nuclear size heterogeneity as a biomarker for post-radiotherapy outcomes in gynecological malignancies. Phys Imaging Radiat Oncol. 2025;35:100793. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |