Published online Mar 26, 2026. doi: 10.12998/wjcc.v14.i9.118800
Revised: February 11, 2026
Accepted: March 5, 2026
Published online: March 26, 2026
Processing time: 72 Days and 9.8 Hours
Aspergillus sydowii (A. sydowii) is a ubiquitous saprophytic mold that is only rarely implicated in human disease. Pulmonary infection due to A. sydowii is exceedingly uncommon, particularly in immunocompetent individuals. With increasing environmental exposure and advances in fungal diagnostic techniques, rare Aspergillus species are increasingly being recognized as causative agents of respiratory infections.
A 25-year-old immunocompetent female healthcare worker from northwestern India presented with a two-week history of persistent cough, dyspnea, and sputum production. Chest computed tomography showed focal peribronchial thickening with nodular opacities in the left lower lobe. Sputum microscopy demonstrated fungal elements, and fungal culture on Sabouraud dextrose agar yielded a mold that was identified as A. sydowii by lactophenol cotton blue mount and confirmed by matrix-assisted laser desorption/ionization time-of-flight mass spectrometry. The patient was treated with oral voriconazole, resulting in marked clinical improvement.
This case highlights A. sydowii as a rare but important cause of pulmonary infection in immunocompetent individuals. Early recognition using advanced mycological techniques such as MALDI-TOF mass spectrometry is essential for accurate diagnosis and appropriate management.
Core Tip: Pulmonary infections caused by rare Aspergillus species can occur even in immunocompetent hosts and may present with nonspecific respiratory symptoms. This case emphasizes the importance of considering uncommon fungal pathogens in persistent respiratory illness and highlights the role of advanced diagnostic tools such as MALDI-TOF mass spectrometry in achieving accurate species-level identification.
- Citation: Choudhary S. Pulmonary Aspergillus sydowii infection in an immunocompetent host from Northwestern India: A case report. World J Clin Cases 2026; 14(9): 118800
- URL: https://www.wjgnet.com/2307-8960/full/v14/i9/118800.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i9.118800
Pulmonary aspergillosis encompasses a broad spectrum of clinical manifestations and most commonly affects immunocompromised individuals[1]. Although Aspergillus fumigatus remains the predominant etiological agent, non-fumigatus Aspergillus species are increasingly recognized with the widespread adoption of advanced fungal diagnostic techniques[2].
Aspergillus sydowii (A. sydowii) is a saprophytic filamentous fungus widely distributed in soil, decaying vegetation, and occasionally marine environments, and has only rarely been implicated in human disease[3]. Human infections caused by A. sydowii are exceedingly uncommon, with sporadic reports describing cutaneous, sinonasal, pulmonary involvement, and otomycosis, predominantly in immunocompromised hosts[4]. The pathogenic potential of A. sydowii in immunocompetent individuals remains poorly understood.
Notably, in the Indian context, A. sydowii is better recognized for its ecological significance than for its role in clinical disease[5]. Consequently, pulmonary disease caused by A. sydowii, especially in immunocompetent hosts, remains un
A 25-year-old female healthcare worker presented with cough associated with expectoration and progressive shortness of breath for two weeks.
There was no history of fever, hemoptysis, chest pain, night sweats, or weight loss.
There was no history of asthma, chronic obstructive pulmonary disease, tuberculosis, or recurrent respiratory infections.
The patient was a non-smoker with no history of alcohol use. There was no significant family history or known exposure to marine environments. No empirical antibiotics were given.
Vital signs were stable. Respiratory examination revealed mild wheezing without crackles. Oxygen saturation was normal on room air.
Hematological evaluation revealed peripheral eosinophilia with an absolute eosinophil count of 1250 cells/µL. Renal and liver function tests were within normal limits. Screening tests for tuberculosis, human immunodeficiency virus infection, and cystic fibrosis were negative. The patient demonstrated moderately elevated inflammatory markers, with a C-reactive protein level of 38 mg/L and leukocytosis (total leukocyte count 17000 cells/µL), while the erythrocyte sedimentation rate was only mildly elevated at 23 mm/hour.
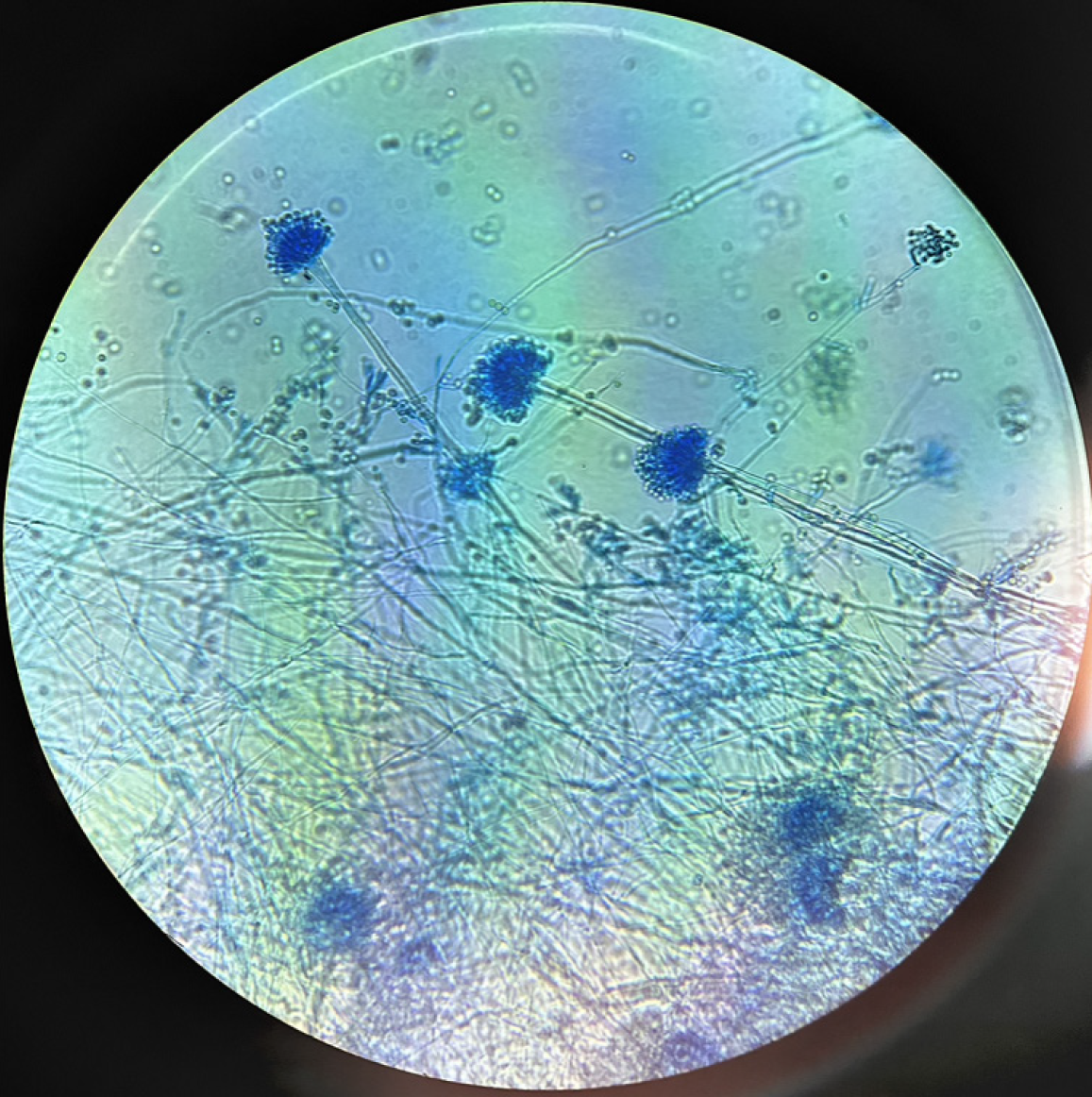
Gram staining of sputum showed few pus cells with no identifiable bacteria. Potassium hydroxide preparation demonstrated fungal hyphae. Bacterial culture was sterile, while fungal culture on Sabouraud dextrose agar yielded a mold (Figure 1). Lactophenol cotton blue mount showed morphological features consistent with Aspergillus species (Figure 2). Definitive identification as A. sydowii was confirmed by MALDI-TOF mass spectrometry. Fungal biomarkers were assessed using the Platelia Aspergillus enzyme-linked immunosorbent assay (Sanofi Pasteur, Freiburg, Germany) for serum galactomannan and the Fungitell assay (Associates of Cape Cod, Inc., United States) for (1→3)-β-D-glucan. The galactomannan index was positive (1.96), while the β-D-glucan level was in the intermediate range (76 pg/mL).
High-resolution computed tomography of the chest showed peribronchial thickening with surrounding nodules and areas of ground-glass opacification in the posterior basal segment of the left lower lobe, suggestive of an infective etiology.
Pulmonary infection caused by A. sydowii in an immunocompetent host.
Based on the fungal culture results, confirmation by matrix-assisted laser desorption/ionization time-of-flight mass spectrometry, and positive serum galactomannan assay, the patient was initiated on oral voriconazole at a dose of 200 mg twice daily. Antifungal therapy was continued for six weeks and was well tolerated, with no reported adverse effects.
Significant clinical improvement was observed within four weeks of initiating antifungal therapy. The patient was followed up at two-month intervals and showed complete resolution of respiratory symptoms. A repeat computed tomography scan was not performed as the patient remained asymptomatic.
Pulmonary aspergillosis is classically associated with immunocompromised states; however, an increasing number of reports have documented Aspergillus infections in immunocompetent individuals. Environmental exposure, occupational risk, and improved diagnostic capabilities have contributed to this evolving clinical recognition. The present report describes a rare case of pulmonary infection caused by A. sydowii in an immunocompetent young female healthcare worker, adding to the limited literature on the pathogenic potential of this uncommon Aspergillus species.
A. sydowii is a saprophytic filamentous fungus widely distributed in soil, decaying vegetation, and marine envi
The clinical presentation of pulmonary A. sydowii infection is nonspecific and overlaps with common respiratory conditions such as bacterial pneumonia, pulmonary tuberculosis, allergic bronchopulmonary aspergillosis, and other fungal infections[5]. In the present case, respiratory symptoms were limited to cough, dyspnea, and sputum production, without systemic features such as fever, weight loss, or night sweats. The presence of peripheral eosinophilia further complicated the diagnostic process by raising the possibility of allergic or parasitic etiologies. Such diagnostic ambiguity has been described in previously reported cases and often contributes to delayed or missed diagnosis.
Radiological manifestations of pulmonary aspergillosis in immunocompetent hosts are variable and lack specificity. Ground-glass opacities, peribronchial thickening, and nodular lesions findings observed in this patient have been described in prior reports of non-invasive and subacute fungal pulmonary infections. These imaging features can mimic viral pneumonitis, bronchiolitis, or organizing pneumonia, emphasizing the need for microbiological confirmation in establishing an etiological diagnosis.
Microbiological diagnosis remains central to identifying uncommon Aspergillus species. In this case, direct microscopy using potassium hydroxide preparation revealed fungal elements, and fungal culture enabled isolation of the organism. Species-level identification of A. sydowii is challenging based on morphology alone because of overlap with other Aspergillus species. The use of matrix-assisted laser desorption/ionization time-of-flight mass spectrometry was instrumental in achieving definitive identification, underscoring the role of advanced mycological techniques in modern diagnostic workflows, particularly for cryptic and emerging fungal pathogens.
Fungal biomarkers provided supportive evidence of active Aspergillus infection in this patient. Serum galactomannan was positive, while β-D-glucan levels were in the intermediate range. Although these assays are primarily validated in immunocompromised populations, several studies have demonstrated their utility as adjunctive diagnostic tools in selected immunocompetent patients when interpreted in conjunction with clinical, radiological, and microbiological findings[6]. Importantly, these biomarkers are not species-specific and should not be used in isolation; however, their positivity in the present case increased diagnostic confidence and supported initiation of antifungal therapy[7].
A review of the limited published literature reveals only a small number of reported pulmonary A. sydowii infections, most described as isolated case reports[8,9]. Similar to the present case, reported cases have involved both immunocompromised and immunocompetent individuals, with ages ranging from young adults to the elderly[2,5,10]. Pulmonary involvement typically presents with nonspecific respiratory symptoms, and radiological findings often include nodules or ground-glass opacities. Diagnosis in most cases relied on fungal culture with advanced identification methods such as molecular techniques or MALDI-TOF mass spectrometry. Triazole antifungal therapy, particularly voriconazole, has been the most commonly used treatment, and favorable clinical outcomes have been reported in the majority of cases. The present case aligns with these observations, further supporting the pathogenic potential of A. sydowii in immunocompetent hosts.
There are currently no species-specific treatment guidelines for A. sydowii infection, and management is extrapolated from established recommendations for invasive aspergillosis. The Infectious Diseases Society of America guidelines recommend voriconazole as the first-line agent for the treatment of invasive aspergillosis[11]. Voriconazole has de
An important feature of this case is the absence of traditional immunosuppressive risk factors. Here patient had no comorbidities or immune dysfunction. Occupational exposure may have contributed, as healthcare workers are repeatedly exposed to airborne fungal spores in clinical environments. This observation supports the need for heightened clinical suspicion of fungal infections even in immunocompetent individuals when symptoms persist despite conventional therapy.
Although this report is limited by the lack of long-term radiological follow-up and absence of serial biomarker monitoring, it provides valuable insight into the clinical spectrum, diagnostic challenges, and successful management of pulmonary A. sydowii infection in an immunocompetent host.
Pulmonary infection caused by A. sydowii is rare and can occur in immunocompetent individuals, presenting with nonspecific respiratory symptoms and radiological findings that mimic more common pulmonary conditions. This case underscores the importance of considering uncommon fungal pathogens in patients with persistent respiratory symptoms, particularly in those with potential occupational or environmental exposure. Early diagnosis using a combination of direct microscopy, fungal culture, advanced identification techniques such as MALDI-TOF mass spectrometry, and supportive fungal biomarkers is crucial for timely and accurate diagnosis. Prompt initiation of appropriate antifungal therapy can result in favorable outcomes and prevent unnecessary diagnostic delays or inappropriate treatments.
| 1. | Nagashima A, Nagato T, Kobori T, Nagi M, Okochi Y. Uncommon Occurrence of Pulmonary Aspergillosis Caused by Aspergillus sydowii: A Case Report. Cureus. 2023;15:e51353. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 2. | Yang Y, Zhao Y, Xi X, Ding R, Yang L. Coinfection of Cedecea lapagei and Aspergillus sydowii detected in bronchoalveolar lavage fluid of a patient with pulmonary infection using metagenomic next-generation sequencing: A case report. Heliyon. 2024;10:e33130. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 3. | Janani RS, Xess I, Das BK, Cs S, Bordoloi T, Pandey M, Ahmed J, Singh G. Invasive aspergillosis due to cryptic Aspergillus species: A prospective study from a single centre in India. Indian J Med Microbiol. 2024;51:100708. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 4. | Buonafina-Paz MD, Santos FA, Leite-Andrade MC, Alves AI, Bezerra JD, Leal MC, Robert E, Pape PL, Lima-Neto RG, Neves RP. Otomycosis caused by the cryptic and emerging species Aspergillus sydowii: two case reports. Future Microbiol. 2022;17:1437-1443. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 7] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 5. | R L, Ninan MM, Kurien R, N A F, Sahni RD, Michael JS. Cryptic aspergillosis: a rare entity and a diagnostic challenge. Access Microbiol. 2022;4:000344. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 12] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 6. | Morena R, Morrone HL, Serapide F, Russo A. Invasive Pulmonary Aspergillosis in Non-Neutropenic Patients: An Evolving Clinical Paradigm. Diagnostics (Basel). 2025;16:34. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 7. | Lass-Florl C, Alastruey-Izquierdo A, Gupta R, Chakroborti A. Interpretation, pitfalls of biomarkers in diagnosis of invasive fungal diseases. Indian J Med Microbiol. 2022;40:480-484. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 14] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 8. | Vera-Cabrera L, Cardenas-de la Garza JA, Cuellar-Barboza A, Gallardo-Rocha A, Molina-Torres CA, Escalante-Fuentes W, Ocampo-Candiani J. Case Report: Coral Reef Pathogen Aspergillus sydowii Causing Black Grain Mycetoma. Am J Trop Med Hyg. 2021;104:871-873. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 8] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 9. | Zhang Y, Wang S, Zhou C, Zhang Y, Pan J, Pan B, Wang B, Hu B, Guo W. Epidemiology of Clinically Significant Aspergillus Species from a Large Tertiary Hospital in Shanghai, China, for the Period of Two Years. Infect Drug Resist. 2023;16:4645-4657. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 10. | Nagarajan C, Thayanidhi P, Kindo AJ, Ramaraj V, Mohanty S, Arunachalam R. Fungal Rhinosinusitis: Report of uncommon Aspergillus species as etiological agents. Int J Case Rep Images. 2014;5:13. [DOI] [Full Text] |
| 11. | Patterson TF, Thompson GR 3rd, Denning DW, Fishman JA, Hadley S, Herbrecht R, Kontoyiannis DP, Marr KA, Morrison VA, Nguyen MH, Segal BH, Steinbach WJ, Stevens DA, Walsh TJ, Wingard JR, Young JA, Bennett JE. Practice Guidelines for the Diagnosis and Management of Aspergillosis: 2016 Update by the Infectious Diseases Society of America. Clin Infect Dis. 2016;63:e1-e60. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2370] [Cited by in RCA: 2071] [Article Influence: 207.1] [Reference Citation Analysis (5)] |
| 12. | AlShaheen H, Abuzied Y, Aldalbahi H, AlSheef M. Aspergilloma in an Immunocompetent Host: A Case Report. Cureus. 2023;15:e40727. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 1.3] [Reference Citation Analysis (0)] |