Published online Mar 26, 2026. doi: 10.12998/wjcc.v14.i9.118553
Revised: February 5, 2026
Accepted: March 3, 2026
Published online: March 26, 2026
Processing time: 78 Days and 4.7 Hours
Esophageal injuries are rare but potentially life-threatening conditions, particularly in the pediatric population. These injuries can be classified as blunt or penetrating, with penetrating trauma being more common overall, though blunt mechanisms predominate in certain contexts such as road traffic accidents. Pe
A 7-year-old girl presented to the outpatient department following a motorcycle accident. A large, open wound was noted on the left side of the face, and the patient was taken to the operating theater for wound washout and closure. Upon further inspection, the patient was noted to have a perforation of the cervical esophagus. The injury was closed primarily, and the skin was then closed in layers. The patient’s diet was advanced as tolerated, and she was discharged home on postoperative day 2 without any complications.
Blunt traumatic esophageal injuries are rare in children. Early repair is necessary to achieve favorable outcomes.
Core Tip: Traumatic esophageal injuries are rare, accounting for less than 1% of all traumatic injuries. Esophageal injuries are even more rare in the pediatric population. While penetrating esophageal injuries are more common in adults, children are more likely to have blunt esophageal injuries, particularly from transportation-related accidents. Here, we report the successful management of a cervical esophageal perforation in a pediatric patient.
- Citation: Kakooza J, Akankwasa P, Mugabe S, Kiadii BK, Lewis CR. Blunt esophageal injury in a pediatric patient: A case report. World J Clin Cases 2026; 14(9): 118553
- URL: https://www.wjgnet.com/2307-8960/full/v14/i9/118553.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i9.118553
Esophageal injuries can be broadly categorized into blunt and penetrating types, each with distinct epidemiological patterns and clinical implications. Penetrating esophageal trauma, often resulting from gunshot or stab wounds, is more prevalent than blunt injury and typically affects the cervical region more frequently than thoracic or abdominal segments[1]. Blunt esophageal injuries, in contrast, are rarer and usually occur due to high-impact mechanisms such as motor vehicle accidents, leading to shear forces or barotrauma that cause perforation. These injuries carry high morbidity and mortality rates if not diagnosed promptly, with challenges in detection due to nonspecific symptoms[2]. Noniatrogenic esophageal trauma, excluding procedural causes, shows a predominance of penetrating mechanisms in adults (approximately 50% penetrating, mostly gunshot and stab wounds), but its overall incidence among trauma admissions is well below 1%, underscoring the need for multimodal diagnostic approaches including computed tomography, endoscopy, and fluoroscopy[3].
In the pediatric population, esophageal injuries exhibit notable differences compared to adults. Children are more likely to sustain blunt trauma, particularly from transportation-related accidents, with lower overall injury severity scores and fewer associated complications. For instance, pediatric traumatic esophageal injuries are associated with a median injury severity score of 14, compared to 22 in adults, and result in shorter hospital stays and higher rates of discharge to home. Mortality rates, while not significantly different, trend lower in children at approximately 10% vs 19% in adults[4]. These disparities may stem from greater tissue elasticity in children, reducing the extent of damage, but also highlight the importance of age-specific considerations in management protocols.
Management of esophageal injuries varies based on factors such as injury location, timing of diagnosis, and patient stability. Guidelines recommend prompt evaluation using tools like computed tomography angiography, esophagoscopy, or esophagography, with operative repair preferred for most cases, though nonoperative approaches may be suitable for small, contained perforations. In pediatric cases, a systematic review suggests that non-surgical management is viable for stable patients with early-diagnosed, contained leaks, while primary repair is indicated for unstable patients or those with larger defects[5]. Algorithms from trauma associations emphasize individualized treatment, incorporating drainage, decompression, and nutrition support[6]. We present a case of successful surgical management of a blunt esophageal injury in a pediatric patient, demonstrating the efficacy of primary repair in achieving uncomplicated recovery.
A 7-year-old girl presented to the outpatient department following a boda motorcycle accident.
The patient presented immediately after the accident. The patient noted a wound to her left face and scratches to both upper extremities. There were no other specific complaints.
The patient had no significant past medical history.
There was no relevant personal or family history.
Vital signs were within normal limits, and the airway was intact.
Laboratory examinations were significant for mild anemia.
No preoperative imaging was performed.
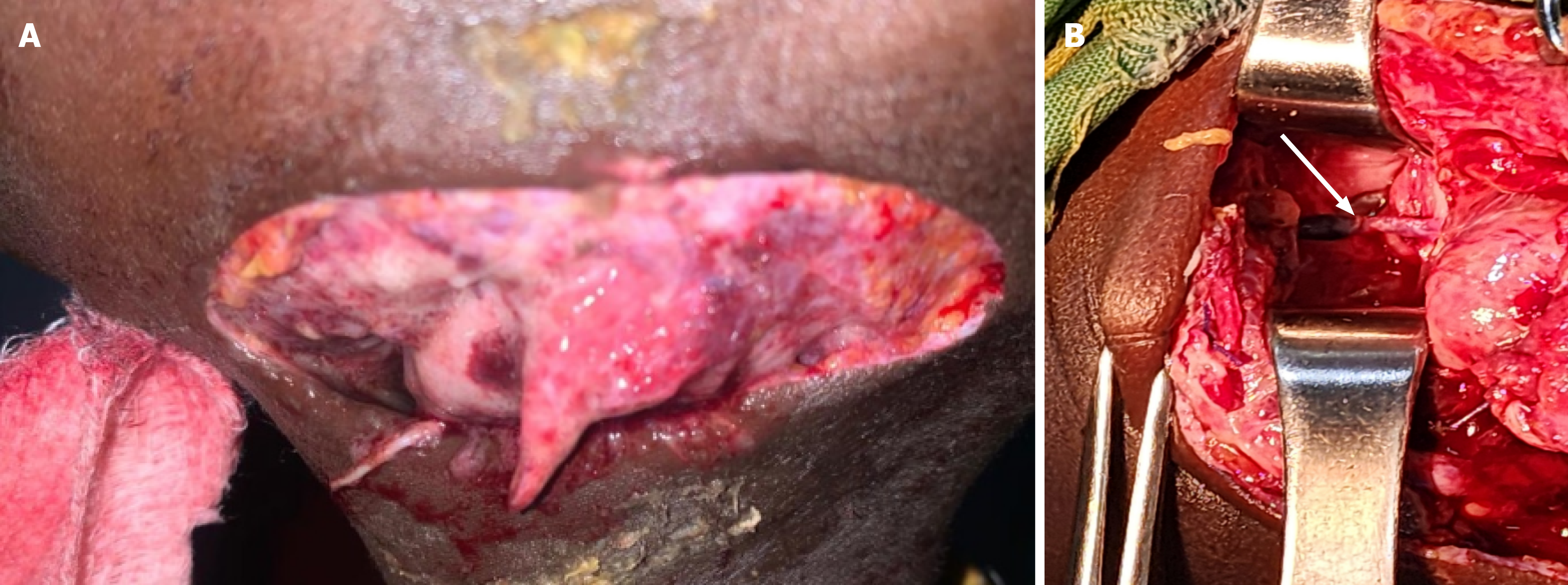
On physical examination, a large open wound was noted on the left side of the face (Figure 1A). There were no signs of penetrating trauma, and the only other injuries identified were superficial abrasions to the bilateral upper extremities. The patient was prepared for the operating room for wound washout and closure.
In the operating room, general anesthesia was induced, and a nasogastric tube was placed. Perioperative antibiotics were administered. The wound was prepared in the standard sterile fashion and irrigated thoroughly with normal saline and diluted povidone-iodine. Upon further exploration, an approximately 2 cm perforation of the cervical esophagus (Figure 1B) was identified, through which the nasogastric tube was visualized. The esophageal defect was closed in an interrupted fashion using 2-0 Vicryl sutures. The subcutaneous tissues were closed in layers, and the skin was approximated with interrupted Prolene sutures.
The nasogastric tube was left in place and removed on postoperative day 2. A liquid diet was initiated and advanced as tolerated. The patient was discharged on postoperative day 2 with no reported complications on follow-up.
Traumatic esophageal injuries are exceedingly rare entities in clinical practice, accounting for a minuscule fraction of overall trauma presentations, with reported incidences less than 0.01% among large cohorts of over 1.4 million adult trauma patients[7]. This rarity extends to pediatric populations, where such injuries represent an even smaller proportion, often linked to unique etiological factors. Penetrating mechanisms dominate the landscape of traumatic esophageal injuries, occurring approximately 10 times more frequently than blunt injuries. Overall, the relative risk indicates that penetrating trauma is 34% more likely to occur[1]. Regarding location, the cervical esophagus is the most affected segment, comprising 69% to over 80% of cases, followed by thoracic involvement at around 31%, while abdominal perforations are the least frequent, often comprising less than 10%[8]. This distribution is influenced by the anatomical accessibility and protective structures. Cervical injuries benefit from easier surgical access and lower mortality rates (approximately 7.9%), whereas thoracic perforations carry higher risks due to proximity to vital mediastinal structures, resulting in elevated morbidity and mortality up to 13.5% or more[1,3]. In children, blunt traumatic esophageal injuries pre
Road traffic accidents serve as a primary mechanism for blunt esophageal trauma, particularly in pediatric patients, where high-speed collisions account for a significant proportion of cases[4]. The pathophysiology involves multiple forces: Rapid deceleration leading to compression of the esophagus between the sternum and vertebral bodies, shear stress at fixed points like the gastroesophageal junction, and barotrauma from sudden increases in intraluminal pressure against a closed glottis, often exacerbated by a full stomach[10]. In motor vehicle crashes, blunt forces to the abdomen or chest can stretch the esophageal wall against the diaphragmatic crura, resulting in longitudinal tears or perforations, with the distal esophagus being particularly vulnerable due to its lack of serosal covering and relatively poor blood supply[10]. Pediatric cases, as in our report involving a motorcycle accident, highlight how even seemingly minor external injuries can mask severe internal damage from these mechanisms, with transportation-related incidents contributing to 63% of blunt esophageal injuries in children compared to lower rates in adults[4]. Associated high-energy transfers often coincide with polytrauma, such as rib fractures or diaphragmatic injuries, amplifying the diagnostic challenge and underscoring the role of road traffic accidents in global trauma epidemiology[11,12].
Management of traumatic esophageal injuries is multifaceted, tailored to injury location, extent, timing of presentation, and patient stability, with a shift toward individualized approaches incorporating both operative and non-operative strategies. Primary surgical repair remains the cornerstone for accessible, large defects, often reinforced with muscle flaps, and is employed in approximately 53%-61% of cases, particularly for cervical and thoracic perforations[1,8]. Adjuncts include broad-spectrum antibiotics, esophageal decompression via nasogastric tube, enteral or parenteral nutrition, and drainage to prevent sepsis. In pediatric populations, non-operative management is increasingly favored for stable patients with contained leaks, demonstrating high success rates. For instance, 11 out of 13 childhood perforations were managed conservatively with antibiotics and drainage, yielding favorable outcomes except in delayed cases[13]. Aggressive conservative protocols, including nil per os, intravenous fluids, proton pump inhibitors, and gastrostomy for nutrition, have enabled spontaneous closure even in delayed presentations complicated by esophagocutaneous fistulas, as evidenced by the case of an 11-year-old patient with penetrating trauma healing without surgery[14]. Early in
Blunt esophageal injuries in children, though rare, require vigilant diagnosis and tailored management to prevent complications. This case illustrates the success of primary surgical repair in a cervical perforation following blunt trauma, resulting in rapid recovery without sequelae. Early exploration and adherence to established protocols can optimize outcomes in such challenging scenarios.
| 1. | Papaconstantinou D, Kapetanakis EI, Mylonakis A, Davakis S, Kotidis E, Tagkalos E, Rouvelas I, Schizas D. Current aspects in the management of esophageal trauma: a systematic review and proportional meta-analysis. Dis Esophagus. 2024;37:doae007. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 2. | Schraufnagel DP, Mubashir M, Raymond DP. Non-iatrogenic esophageal trauma: a narrative review. Mediastinum. 2022;6:23. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 6] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 3. | Aiolfi A, Inaba K, Recinos G, Khor D, Benjamin ER, Lam L, Strumwasser A, Asti E, Bonavina L, Demetriades D. Non-iatrogenic esophageal injury: a retrospective analysis from the National Trauma Data Bank. World J Emerg Surg. 2017;12:19. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 29] [Cited by in RCA: 14] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 4. | Xu AA, Breeze JL, Jackson CA, Paulus JK, Bugaev N. Comparative analysis of traumatic esophageal injury in pediatric and adult populations. Pediatr Surg Int. 2019;35:793-801. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 3] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 5. | Al Jubab A, Jafarli IA, Al Tokhais T. Surgical Versus Non-Surgical Treatment for Traumatic Esophageal Perforation in Children: A Systematic Review. J Curr Surg. 2016;6:41-45. [DOI] [Full Text] |
| 6. | Biffl WL, Moore EE, Feliciano DV, Albrecht RA, Croce M, Karmy-Jones R, Namias N, Rowell S, Schreiber M, Shatz DV, Brasel K. Western Trauma Association Critical Decisions in Trauma: Diagnosis and management of esophageal injuries. J Trauma Acute Care Surg. 2015;79:1089-1095. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 35] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 7. | Gambhir S, Grigorian A, Swentek L, Maithel S, Sheehan BM, Daly S, Lekawa M, Nahmias J. Esophageal Trauma: Analysis of Incidence, Morbidity, and Mortality. Am Surg. 2019;85:1134-1138. [DOI] [Full Text] |
| 8. | Raff LA, Schinnerer EA, Maine RG, Jansen J, Noorbakhsh MR, Spigel Z, Campion E, Coleman J, Saquib S, Carroll JT, Jacobson LE, Williams J, Young AJ, Pascual J, Burruss S, Gordon D, Robinson BRH, Nahmias J, Kutcher ME, Bugaev N, Jeyamurugan K, Bosarge P. Contemporary management of traumatic cervical and thoracic esophageal perforation: The results of an Eastern Association for the Surgery of Trauma multi-institutional study. J Trauma Acute Care Surg. 2020;89:691-697. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 10] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 9. | Melmer PD, Chaconas CE, McCrae AL, Sciarretta JD. Conservative Therapy for Cervical Esophageal Perforation Following Blunt Trauma. Am Surg. 2021;87:1518-1520. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 10. | Tanoto EA, Wahyuni S, Soedjatmiko H. Delayed distal thoracic esophageal perforation secondary to blunt trauma: a case report. J EMS Med. 2024;3:55-59. [DOI] [Full Text] |
| 11. | Schuster A, Klute L, Kerschbaum M, Kunkel J, Schaible J, Straub J, Weber J, Alt V, Popp D. Injury Pattern and Current Early Clinical Care of Pediatric Polytrauma Comparing Different Age Groups in a Level I Trauma Center. J Clin Med. 2024;13:639. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 12. | Lai S, Wilhelm S, Morden R, Akay B, Novotny N, Stallion A, Brahmamdam P. Blunt Trauma and Diaphragm Injury in Children: An Analysis of the National Trauma Data Bank. Children (Basel). 2025;12:168. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 13. | van der Zee D, Festen C, Severijnen R, van der Staak F. Management of pediatric esophageal perforation. J Thorac Cardiovasc Surg. 1988;95:692-695. [RCA] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 20] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 14. | Mishra B, Singhal S, Aggarwal D, Kumar N, Kumar S. Non operative management of traumatic esophageal perforation leading to esophagocutaneous fistula in pediatric age group: review and case report. World J Emerg Surg. 2015;10:19. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 8] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 15. | Sudarshan M, Cassivi SD. Management of traumatic esophageal injuries. J Thorac Dis. 2019;11:S172-S176. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 41] [Cited by in RCA: 27] [Article Influence: 3.9] [Reference Citation Analysis (0)] |