Published online Mar 6, 2026. doi: 10.12998/wjcc.v14.i7.117757
Revised: January 25, 2026
Accepted: February 10, 2026
Published online: March 6, 2026
Processing time: 80 Days and 13.5 Hours
Total hip arthroplasty (THA) in young patients with developmental dysplasia of the hip (DDH) is a technically demanding procedure that is associated with a higher incidence of implant-related complications. Transacetabular screw fixation may be required to achieve acetabular stability in these complex reconstructions, but improper screw placement can result in neurovascular injury. Although sy
We report the case of a 28-year-old male who underwent staged bilateral THA via a superior approach for DDH. Following right-sided arthroplasty, the patient developed sciatic-type right leg pain and weakness of foot and ankle dorsiflexion due to a protruding transacetabular screw. Revision surgery included retention of all the well-fixed arthroplasty components, exploration and dissection of the sciatic nerve and trimming of the prominent screw edge. At 3 years postoperatively, the patient was pain-free and had minimal restrictions during daily activities. However, some residual weakness of ankle dorsiflexion remained and an ankle-foot orthosis was used during long-distance walking.
This case underscores the need for careful attention to transacetabular screw placement during THA in DDH and demonstrates a safe and effective extra-acetabular surgical strategy for managing symptomatic screw protrusion avoiding joint dislocation, liner exchange and component revision.
Core Tip: Total hip arthroplasty in developmental dysplasia of the hip carries the risk of transacetabular screw protrusion and neurologic injury. In case of sciatic nerve palsy due to intrapelvic screw penetration, an extra-acetabular approach with exploration of the sciatic nerve and resection of the prominent screw tip can allow immediate pain relief without com
- Citation: Davitis V, Chalidis B. Extra-acetabular resection of a protruding transacetabular screw after total hip arthroplasty for developmental dysplasia: A case report. World J Clin Cases 2026; 14(7): 117757
- URL: https://www.wjgnet.com/2307-8960/full/v14/i7/117757.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i7.117757
Developmental dysplasia of the hip (DDH) is a frequent cause of early degenerative hip disease and may necessitate total hip arthroplasty (THA) at a young age[1]. Epidemiological studies have shown that untreated or severe DDH progresses over time, leading to gait disturbances and early osteoarthritis. Therefore, young patients suffering from DDH have an increased and early need for THA[2]. Moreover, the procedure in dysplastic hips is technically demanding due to the altered acetabular morphology, poor bone stock, shallow acetabular concavity and insufficient acetabular coverage of the femoral head[3].
Acetabular cup fixation in dysplastic hips frequently requires supplemental screw placement to achieve stability when native bone coverage is insufficient. The risks of intrapelvic protrusion of transacetabular screws and injury of the neurovascular structures is generally low, but not negligible[4]. In a study of 3126 consecutive total hip replacements, Schmalzried et al[5] found that the overall incidence of postoperative neuropathy after primary THA was 1.3% but raised to 5.2% after primary arthroplasties that had been done for congenital dislocation or dysplasia of the hip. The likelihood of extraosseous screw placement and injury to neurovascular structures, including the sciatic nerve, is higher in severe DDH due to the inherent difficulty of implanting a cup with a proper size, inclination and anteversion in a deficient acetabulum[6].
We describe a 28-year-old patient with DDH who developed postoperative sciatic pain and paresis of the ipsilateral peroneal nerve due to posterior acetabular screw protrusion after THA. Resection of the prominent screw tip without revising the acetabular component led to immediate pain relief and preservation of initial cup stability.
The patient complained of severe leg pain along the distribution of sciatic nerve, which became worse during standing or walking.
A 28-year-old male with a history of bilateral DDH presented initially with progressive groin pain, stiffness, limping and difficulty in walking. The symptoms had gradually worsened over the preceding 3 years, leading to significant functional limitation and impaired quality of life. Specifically, the patient had severe difficulty in stair climbing, prolonged sitting and putting on his socks and shoes. Conservative management including physiotherapy and intake of regular oral medications such as analgesics and non-steroid anti-inflammatory agents were ineffective to alleviate the symptoms.
The patient underwent staged bilateral THA via a superior approach. Following right-sided arthroplasty, the patient developed sciatic-type right leg pain and weakness of foot and ankle dorsiflexion due to a protruding transacetabular screw.
The patient had no relevant comorbidities or prior surgeries.
The patient had no family history of metabolic or endocrinologic diseases.
Before surgery, clinical examination revealed restricted and painful movements in both hip joints, particularly in flexion and internal rotation, a waddling gait pattern, and a noticeable leg-length discrepancy of 1.2 cm. Firstly, after the left hip arthroplasty the postoperative period was uneventful. But after the right THA, painful hip movements, positive straight leg raise test and weakness of foot and ankle dorsiflexion (2 out of 5 strength) were evident.
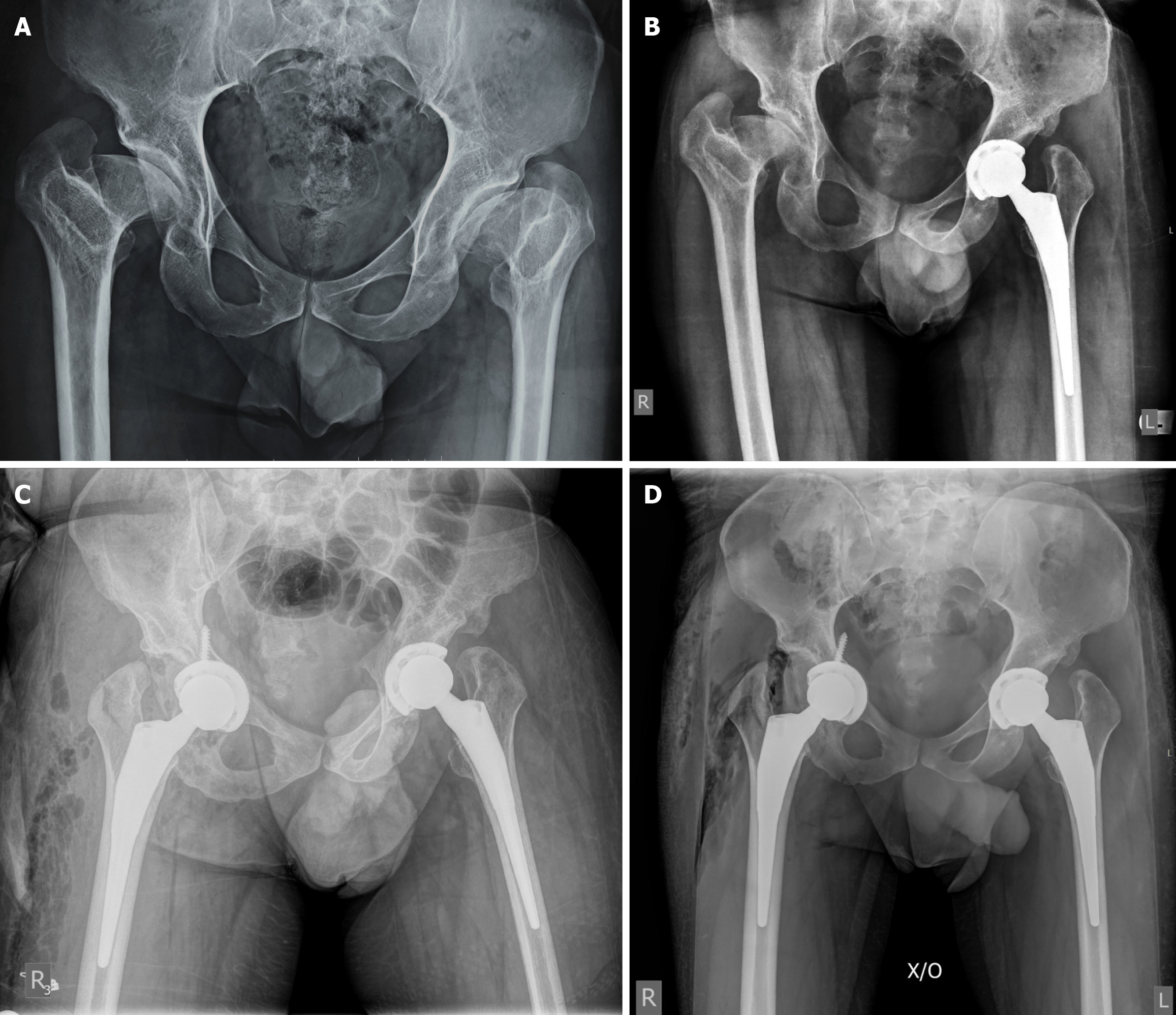
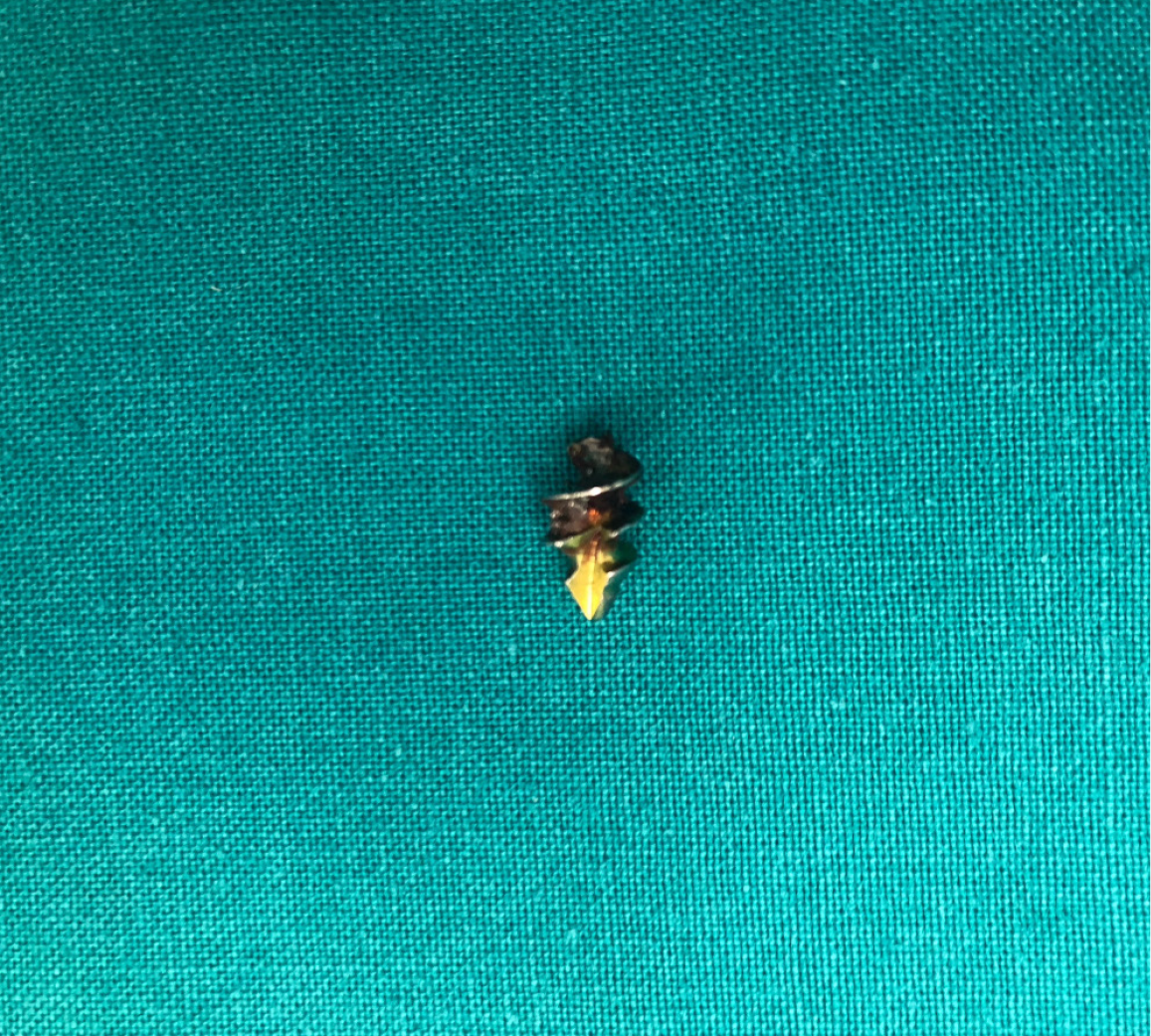
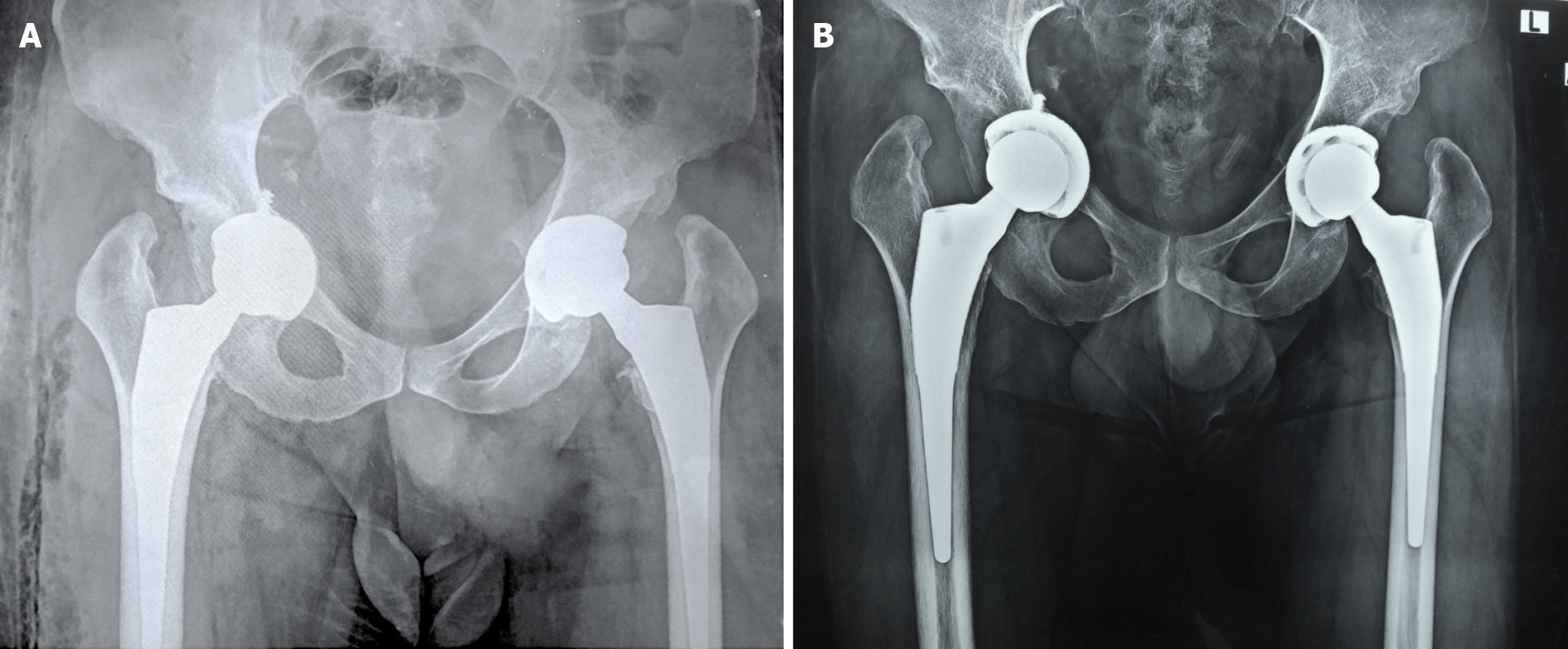
Radiographic evaluation revealed bilateral acetabular dysplasia with a shallow and steep acetabular roof, deficient superolateral coverage, and advanced degenerative changes consistent with secondary osteoarthritis. Severe deformity of the femoral head, joint space narrowing, subchondral sclerosis and osteophyte formation were also evident radiologically (Figure 1A). Postoperative anteroposterior pelvic radiograph after left THA demonstrated satisfactory implant position (Figure 1B). Immediate postoperative pelvic radiograph after right THA demonstrated satisfactory implant position with medialization of the acetabular component and slight intrapelvic penetration of the transacetabular screw (Figure 1C). A higher-quality postoperative radiograph obtained a few hours later revealed protrusion of the transacetabular screw into the greater sciatic notch that caused direct injury of the sciatic nerve (Figure 1D). Post-revision radiographs demonstrated the resected screw tip and trimmed acetabular screw without implant revision (Figures 2 and 3A). At 3 years postoperatively, anteroposterior pelvic radiograph showed stable prosthesis without signs of cup migration or loosening (Figure 3B).
Sciatic-type right leg pain and weakness of foot and ankle dorsiflexion due to a protruding transacetabular screw after THA for DDH.
Although both hips were symptomatic due to DDH, the patient elected to proceed first with the left hip and a cementless THA via a superior approach was performed. A proximal porous coated high-offset femoral stem (Taperloc Complete stem, Zimmer Biomet® Warsaw, IN, United States) and a 46 mm modular dual-mobility acetabular cup (G7 cup, Zimmer Biomet® Warsaw, IN, United States) were implanted without the need for additional transacetabular screw fixation (Figure 1B).
The postoperative period was uneventful and the patient returned 3 months later for the second operation in the contralateral hip. Following the same approach and implant types, a 48 mm cup was inserted using supplemental screw fixation to guarantee adequate cup stability. For that purpose, the screw was firmly tightened with a flexible screwdriver and screw-holding forceps and fully seated within the shell. Elongation of the right limb and equal leg lengths were also achieved.
Due to the postoperative sciatic nerve symptoms and radiographic findings, revision surgery was performed on the same day via the previous superior approach that extended slightly proximally. The sciatic nerve was explored and found to be in close contact with the prominent screw tip. After careful dissection and isolation of the nerve, the protruding portion of the screw was resected with a Gigli saw and a bolt cutter flush with the bone surface. Due to the difficulty in the primary operation to achieve stabilization of the cup, no implant revision or screw removal was taken place (Figures 2 and 3A).
After the procedure, the patient experienced complete resolution of the sciatic pain but continued to report some numbness in the affected leg. At 3 years postoperatively, he regained mobility and had minimal restrictions during the daily activities. However, some residual weakness of ankle dorsiflexion remained and an ankle-foot orthosis was used during long-distance walking (4 out of 5 strengths in ankle dorsiflexion).
Functional outcome, as assessed by the Harris Hip Score, improved from 30 points preoperatively to 93 points postoperatively, reflecting substantial clinical benefit despite the partial neurological deficit at the right lower limb. Pelvic radiograph showed stable prosthesis without signs of cup migration or loosening (Figure 3B).
Neurologic injury following THA remains a rare but serious complication, with a reported incidence of 0.08%-7.6%, depending on whether the procedure is primary or revision[7]. The sciatic nerve is most frequently affected, accounting for nearly 80% of reported nerve palsies, with higher risk in patients undergoing surgery for DDH[8]. The nerve may be injured indirectly due to forceful traction and manipulation or leg lengthening more than 2 cm[9]. In our patient there was direct irritation of the nerve in the greater sciatic notch from a transacetabular screw, which is an uncommon but well-documented mechanism of nerve injury. Late hardware-related neuropathy from screws, cages, or plates has been also described after complex acetabular reconstruction, often requiring surgical exploration and revision surgery[10]. Unfortunately, sciatic nerve injury can result in prolonged or incomplete recovery and development of chronic neurogenic (or neuropathic) pain is not uncommon. Some patients regain full muscle strength within 1-2 years, but in many cases functional deficits may be permanent and not fully reversible requiring long-term use of walking aids or ankle-foot orthoses[11].
The quadrant system emphasizes that the posterior quadrants are relatively safe for acetabular screws fixation, while anterior quadrants should be avoided to prevent injury to major neurovascular structures. However, even screws placed within the posterior quadrants may breach the cortical boundary and extend into the adjacent soft tissues[10]. The risk of sciatic nerve damage is even higher when medialization of the acetabular cup is chosen to ensure optimal coverage and stability of the component, especially in DDH where the available bone stock is often poor and insufficient[6].
Although imaging modalities such as radiographs and computed tomography scans are usually effective to detect screw prominence, poor quality images may not clearly illustrate the protruding screw and delay the diagnosis[12]. This was evident in our case where the immediate pelvic radiograph did not reveal screw misplacement in the sciatic notch due to an improper X-ray beam angle or suboptimal patient positioning. Routinely and despite the presence or not of neurovascular injury symptoms, all the postoperative radiographs should be performed in a standardized and consistent manner in order to identify any implant malposition and avoid a delayed diagnosis and irreversible symptoms. Recent reports have also demonstrated that the musculoskeletal ultrasound could also identify screws impinging on the piriformis tendon or sciatic nerve, offering a dynamic and radiation-free diagnostic option[8].
In the present case, the acute onset of pain and neurologic deficit required immediate exploration of the sciatic nerve throughout its course in the buttock area. Due to the difficulty in stabilizing the acetabular cup during THA procedure and the good grip of the transacetabular screw, we decided not to dislocate the joint and remove the liner and the protruded screw. That approach could have led to implant instability, migration and early failure. The resection of the screw tip with the Gigli saw and bolt cutter did not require additional exposure and did not affect the strength of screw fixation.
The problem of symptomatic transacetabular screw protrusion can be addressed either with intra-acetabular screw exchange or extra-acetabular screw-tip trimming via an endoscopic or open surgical approach. Intra-acetabular screw replacement requires joint dislocation and liner exchange but early cup stability may be compromised. Arthroscopic approaches are less invasive but require specialized equipment and expertise. In contrast, the extra-acetabular approach allows direct sciatic nerve decompression and screw-tip resection while preserving component stability and avoiding revision of the components.
Protrusion of transacetabular screws may be associated with acute iliopsoas tendinitis, persistent groin pain and piriformis impingement[13]. In our case, the direct sciatic nerve irritation represents a more debilitating manifestation of screw malposition. The latter may occur more frequently in DDH where medialization of the acetabular component for facilitating optimal bone coverage along with the deficient bone stock increase the risk of penetration of the acetabular walls[6]. Even in case of symptomatic intrapelvic screw prominence, the presented technique provides a safe and effective extra-acetabular solution to remove the protruding part of a stable transacetabular screw while avoiding joint dislocation, liner exchange and early component revision.
A literature review revealed a variety of different strategies for addressing transacetabular screw protrusion depending on surgeon’s preference, severity of symptoms and stability of the acetabular component. Open surgical removal of protruding screws and exchange of the liner and head without revising the acetabular component have been described in most cases[8,13,14]. In addition, Yoon et al[10] performed a successful minimally invasive hip arthroscopy technique to respect the protruding screw tip. Delayed sciatic nerve neuropathy has also been reported after months or years from the index procedure. In this scenario, osseointegration of the acetabular cup minimizes the risk of implant loosening during surgery and both extra-acetabular and intra-acetabular approaches can be effectively and safely followed. However, and despite nerve exploration and removal of the prominent screws, surgical treatment of delayed neuropathy was associated with only modest pain relief and incomplete recovery of motor and sensory function[15].
This case report has several limitations. Firstly, it is limited only to one patient and any evidence-based recommendations could not be implemented. A larger study including an adequate number of patients and comparing extra-acetabular screw tip removal with intra-acetabular screw exchange and/or cup revision should be performed in order to define the best treatment approach for addressing intrapelvic acetabular screw prominence. Finally, the lack of long-term data could not predict the outcome of THA in dysplastic hips when additional interventions are made in the acetabular socket. Strengths of this case report include timely same-day diagnosis and surgical intervention, comprehensive clinical and radiographic documentation and objective functional evaluation using patient-reported outcome measures throughout the follow-up period confirming the efficacy and safety of the procedure.
Transacetabular screw protrusion after THA for DDH is a rare cause of acute sciatic nerve injury. This case demonstrates that careful preoperative planning, meticulous intraoperative screw placement, and prompt recognition of neurologic symptoms are critical to prevent complications. Extra-acetabular resection of the protruding screw tip allows safe relief of nerve irritation while preserving cup stability, avoiding joint dislocation, liner exchange, or component revision. Surgeons should consider this approach when managing symptomatic screw malposition, and further research is warranted to establish standardized guidelines for intraoperative screw placement and postoperative monitoring in dysplastic hips. In similar case scenarios, this component-preserving strategy eliminates the need for early revision of a stable acetabular construct while performing immediate nerve exploration and decompression through the same surgical approach.
| 1. | Bicanic G, Barbaric K, Bohacek I, Aljinovic A, Delimar D. Current concept in dysplastic hip arthroplasty: Techniques for acetabular and femoral reconstruction. World J Orthop. 2014;5:412-424. [PubMed] [DOI] [Full Text] |
| 2. | Zhang S, Doudoulakis KJ, Khurwal A, Sarraf KM. Developmental dysplasia of the hip. Br J Hosp Med (Lond). 2020;81:1-8. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 20] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 3. | Wang Y. Current concepts in developmental dysplasia of the hip and Total hip arthroplasty. Arthroplasty. 2019;1:2. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 28] [Cited by in RCA: 31] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 4. | Fei C, Wang PF, Wei W, Qu SW, Yang K, Li Z, Zhuang Y, Zhang BF, Zhang K. Relationship between use of screws and acetabular cup stability in total hip arthroplasty: a meta-analysis. J Int Med Res. 2020;48:300060520903649. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 9] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 5. | Schmalzried TP, Amstutz HC, Dorey FJ. Nerve palsy associated with total hip replacement. Risk factors and prognosis. J Bone Joint Surg Am. 1991;73:1074-1080. [PubMed] |
| 6. | Shi XT, Li CF, Han Y, Song Y, Li SX, Liu JG. Total Hip Arthroplasty for Crowe Type IV Hip Dysplasia: Surgical Techniques and Postoperative Complications. Orthop Surg. 2019;11:966-973. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 53] [Cited by in RCA: 60] [Article Influence: 8.6] [Reference Citation Analysis (0)] |
| 7. | Schmalzried TP, Noordin S, Amstutz HC. Update on nerve palsy associated with total hip replacement. Clin Orthop Relat Res. 1997;188-206. [PubMed] |
| 8. | Chen CC, Cheng HY, Shih KS, Hou SM. Ultrasound-diagnosed screw protrusion in total hip arthroplasty: A case report and literature review. Asian J Surg. 2024;47:1403-1405. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 9. | Higuchi Y, Hasegawa Y, Ishiguro N. Leg lengthening of more than 5 cm is a risk factor for sciatic nerve injury after total hip arthroplasty for adult hip dislocation. Nagoya J Med Sci. 2015;77:455-463. [PubMed] |
| 10. | Yoon SJ, Park MS, Matsuda DK, Choi YH. Endoscopic resection of acetabular screw tip to decompress sciatic nerve following total hip arthroplasty. BMC Musculoskelet Disord. 2018;19:184. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 11] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 11. | O'Brien S, Gallagher N, Spence D, Bennett D, Dennison J, Beverland DE. Foot drop following primary total hip arthroplasty. Hip Int. 2020;30:135-140. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 9] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 12. | Lombard C, Gillet P, Germain E, Boubaker F, Blum A, Gondim Teixeira PA, Gillet R. Imaging in Hip Arthroplasty Management Part 2: Postoperative Diagnostic Imaging Strategy. J Clin Med. 2022;11:4416. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 13. | Vargas-Reverón C, Capurro B, Alías AJ, Muñoz-Mahamud E, Pifarré PT, Fernández-Valencia JA. Removal of protruding screws in a painful total hip arthroplasty: A case report. Radiol Case Rep. 2021;16:103-107. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 14. | Stiehl JB, Stewart WA. Late sciatic nerve entrapment following pelvic plate reconstruction in total hip arthroplasty. J Arthroplasty. 1998;13:586-588. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 18] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 15. | Xu LW, Veeravagu A, Azad TD, Harraher C, Ratliff JK. Delayed Presentation of Sciatic Nerve Injury after Total Hip Arthroplasty: Neurosurgical Considerations, Diagnosis, and Management. J Neurol Surg Rep. 2016;77:e134-e138. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 9] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/