Published online Apr 16, 2026. doi: 10.12998/wjcc.v14.i11.119670
Revised: February 25, 2026
Accepted: March 16, 2026
Published online: April 16, 2026
Processing time: 65 Days and 17.8 Hours
Glaucoma, being a chronic disease requires regular follow-up for intraocular pressure (IOP) monitoring and assessment of disease progression, was adversely affected by mobility restrictions such as those imposed during the coronavirus disease 2019 (COVID-19) pandemic. With shutdowns and lockdowns in multiple areas, patients either missed follow-up dates or presented late, affecting the management of various ophthalmic disorders, including glaucoma. Given the diverse etiologies of secondary glaucoma, delay and loss to follow-up during the COVID-19 pandemic were likely to have a substantial impact on clinical out
To assess the clinical profile and management outcomes of secondary glaucoma during the COVID-19 pandemic.
This prospective observational study was conducted at a tertiary care institute from July 2020 to December 2021. The findings were compared with those of a similar cohort evaluated between January 2022 and June 2023.
Out of 62 patients, 46 (74.2%) were males and 25 (40.3%) were aged > 60 years. The aetiologies included pseudoexfoliation (PXF) (26.8%), neovascular glaucoma (NVG) (17.1%), trauma (13.4%), steroid-induced glaucoma (12.2%), miscellaneous causes (11.0%), developmental glaucoma (6.1%) and, uveitic glaucoma (4.9%). Delays in surgery and frequent dropouts contributed to cases of lens-induced glaucoma (8.5%). At presentation, best-corrected visual acuity was < 3/60 in 41.4% of eyes, IOP was > 30 mmHg in 57.4 % of eyes, and severe optic disc damage was noted in 42.7% of eyes. Target IOP was achieved in 65.9% of eyes after six months of treatment. While the mean cup to disc ratio and mean deviation on Humphrey visual field did not show statistically significant difference, the mean retinal nerve fiber layer thickness showed a statistically significant increase. All variables were compared with those of a similar post-pandemic cohort over the same duration. An increase in cases of NVG (27.3%) and other forms of secondary glaucoma was observed in the post-pandemic period, except for lens-induced glaucoma.
PXF glaucoma was the most common cause of secondary glaucoma during the pandemic. Target IOP was achieved mostly with surgical therapy. COVID-19 posed challenges in treatment and played a pivotal role in the deve
Core Tip: This study aimed to assess the clinical course of secondary glaucoma during the coronavirus disease 2019 (COVID-19) pandemic in a tertiary care institute in eastern India and compare them with that of a similar cohort in the post-pandemic period. The majority patients were male, of elderly age group and had pseudoexfoliation as the most common etiology. Target intraocular pressure was achieved in 65.9% of eyes after six months of treatment. There was an increase in mean retinal nerve fiber layer thickness post treatment which was statistically significant. After the pandemic, there was an increase in neovascular (27%) and other forms of secondary glaucoma, except lens-induced glaucoma.
- Citation: Nayak B, Bhatt B, Parija S, Chakraborty K, Sahoo DP, Nanda J, Panda BB. Clinical profile and outcome of secondary glaucoma managed during the COVID-19 pandemic in a tertiary care institute. World J Clin Cases 2026; 14(11): 119670
- URL: https://www.wjgnet.com/2307-8960/full/v14/i11/119670.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i11.119670
Glaucoma is a progressive optic neuropathy characterized by degeneration of retinal ganglion cells and thinning of the retinal nerve fiber layer (RNFL), resulting in structural changes in the optic nerve head[1]. Globally, an estimated 79.6 million individuals were affected by glaucoma in 2020, and this number is projected to reach 118.6 million by 2040, largely due to population aging, notably in China and India[2,3]. Established risk factors include age, gender, race, genetic predisposition, family history, smoking, systemic hypertension, vasospasm, steroid use, and others[4-6].
Secondary glaucoma may develop due to various ocular and systemic conditions such as trauma, retinal ischemia, uveitis, diabetes mellitus, and hypertension[7]. Management varies depending on the underlying cause, with some cases requiring surgical intervention. Steroid-induced glaucoma may improve with discontinuation of the steroids, whereas glaucoma following penetrating keratoplasty, vireo-retinal surgery, and neovascular glaucoma (NVG) often require primary surgical intervention as first-line treatment as they respond poorly to medical therapy alone[8]. Pseudoexfoliation (PXF) and pigment dispersion glaucoma typically present with high baseline intraocular pressure (IOP) and significant fluctuation frequently necessitating surgical management[9]. Similarly, glaucoma secondary to angle dysgenesis, such as in Sturge Weber syndrome and iridocorneal endothelial syndrome, often responds inadequately to medical management alone and requires surgery. Timely diagnosis and appropriate intervention are crucial to prevent visual loss, as secondary glaucoma remains a significant cause of visual morbidity[10].
Glaucoma, being a chronic disease requiring regular follow-up for IOP monitoring and assessment of disease pro
Given the diverse etiologies of secondary glaucoma, delay and loss to follow-up during the COVID-19 pandemic were likely to have a substantial impact on clinical outcomes. However, comprehensive studies evaluating the clinical profile and outcomes of various types of secondary glaucoma, particularly from the eastern region of India, remains limited. This study aims to highlight the challenges and outcomes associated with the management of secondary glaucoma during the COVID-19 pandemic.
This prospective observational study was conducted in the Department of Ophthalmology at a tertiary care institute in eastern India from July 1, 2020 to December 31, 2021. The study was approved by the Institutional Ethics Committee, and all procedures adhered to the tenets of the Declaration of Helsinki guidelines.
For comparative analysis, a post-pandemic cohort was prospectively enrolled between January 1, 2022, and June 30, 2023, using identical inclusion criteria, diagnostic protocols, management strategies, and follow-up schedules.
Pandemic cohort: A total of 62 patients (82 eyes) aged > 5 years diagnosed with secondary glaucoma were enrolled during the pandemic period. Both newly diagnosed and previously treated (old) cases were included.
Post-pandemic cohort: During the post-pandemic period, consecutive patients fulfilling the same eligibility criteria were enrolled. Demographic characteristics, etiological profile, severity at presentation, treatment modality, and six-month outcomes were recorded using the same standardized methodology to ensure comparability between the two cohorts.
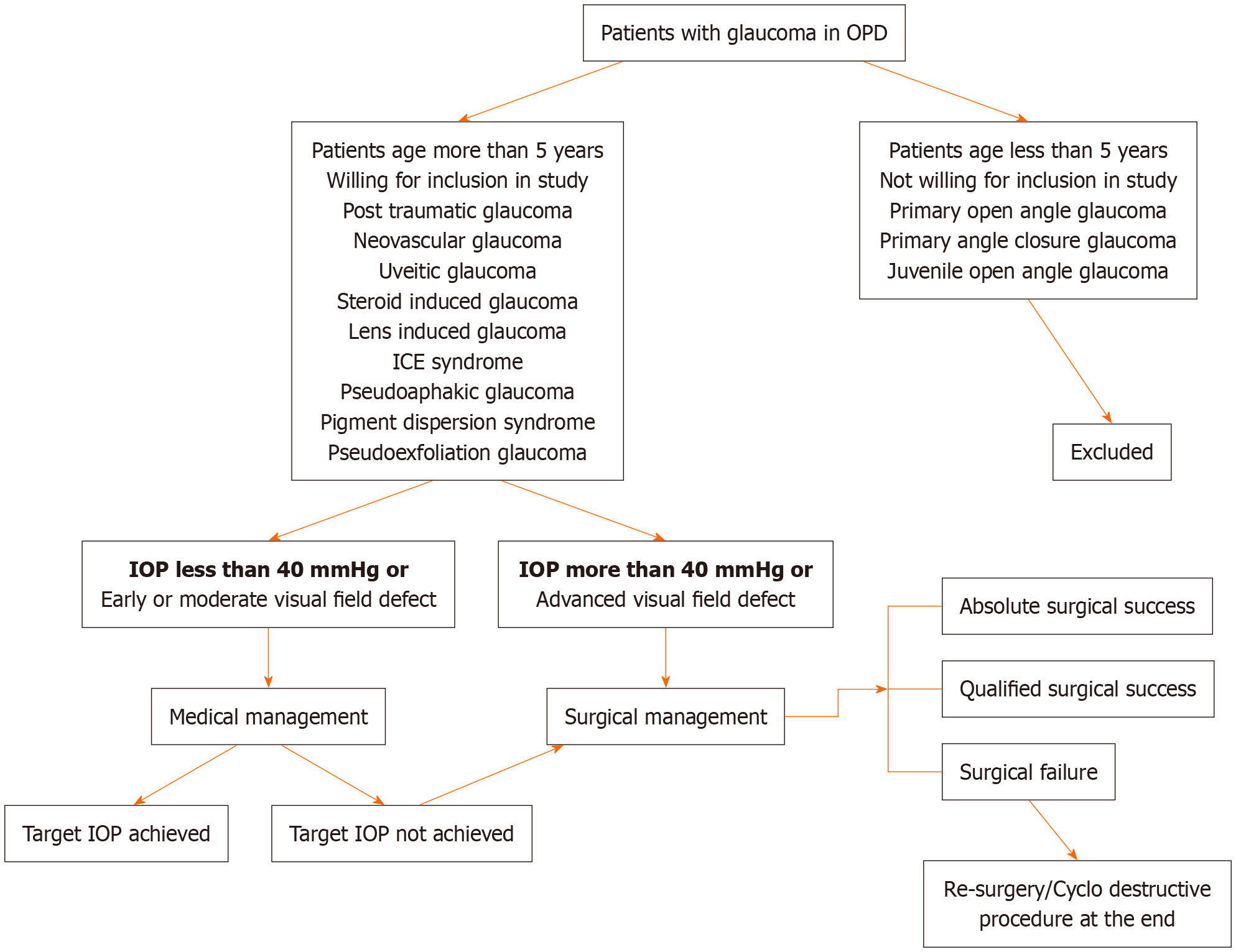
Patients aged > 5 years who provided informed consent and assent forms (as applicable) and fulfilled the following criteria were included (Figure 1): (1) Clinical history and examination findings suggestive of secondary glaucoma due to trauma, neovascularisation, uveitis, previous intraocular surgeries, lens-induced glaucoma, steroid-induced glaucoma, uveitic glaucoma; (2) Glaucoma secondary to malformation of the iridocorneal endothelial junction; and (3) IOP > 21 mmHg with a vertical cup to disc (C:D) ratio ≥ 0.6:1 with thinning of the neuroretinal rim and corresponding glaucomatous visual field defect. Patients already receiving treatment for secondary glaucoma were categorized as old cases. Exclusion criteria included age < 5 years, primary glaucoma, and refusal to provide consent.
A semi-structured questionnaire was administered to assess the impact of the pandemic on healthcare access, including missed follow-up visits, delay in surgical intervention, and difficulty in procuring medications, and travel restrictions due to lockdown (Supplementary Table 1). All patients were managed in accordance with the preferred practice guidelines of the All India Ophthalmological society and relevant World health Organisation (WHO) recommendations[11].
The following variables were recorded for all participants: Age, sex, socioeconomic status (assessed using the modified Kuppuswamy scale), COVID-19 status, laterality of the affected eye, etiology of secondary glaucoma, best-corrected visual acuity (BCVA), slit lamp examination, IOP, fundus examination findings, and gonioscopic features.
IOP was measured by Goldman applanation tonometry. Optical coherence tomography (OCT) was performed to document the RNFL thickness using Cirrus HD-OCT (Carl Zeiss Meditec Inc. Hacienda Drive, Dublin, CA, United States). The signal strength above six were included in the analysis. Visual field assessment was performed in patients with BCVA ≥ 6/60 using the Humphrey field analyzer II (HFA) (Carl Zeiss 720 HFA-II, Carl Zeiss Meditec Inc. Hacienda Drive, Dublin, CA, United States).
Glaucoma severity was classified as early, moderate, and severe based on visual field defects according to the Hodapp-Parrish-Anderson classification[12]. In cases in whom visual field testing could not be performed due to poor visual acuity, severity was determined based on optic disc findings according to established Canadian guidelines[13].
Medical management included topical and/or systemic anti-glaucoma medications, with documentation of drug type, dosage, frequency, and duration. Surgical intervention was indicated in cases with: (1) Baseline IOP > 40 mmHg at presentation with advanced glaucomatous optic disc cupping and visual field defect; (2) Intolerance to or inability to afford anti-glaucoma medications; (3) Failure to achieve target IOP (12 mmHg for advanced glaucoma, 15 mmHg for moderate glaucoma, 18 mmHg for mild glaucoma); or (4) Documented progression despite achieving target[7].
All patients were screened for COVID infection prior to surgical intervention. The primary surgical procedure was trabeculectomy augmented with mitomycin C (MMC) 0.04% with or without an Ologen implant. In case of NVG, intra
Early bleb failure was managed with needling and MMC augmentation. Refractory cases following bleb needling were managed with topical anti-glaucoma medications, and in case of persistently uncontrolled IOP, re-trabeculectomy was performed. Absolute and qualified success were defined as achieving the target IOP of < 12 mmHg in advanced glaucoma, < 15 mmHg in moderate glaucoma, and < 18 mmHg in mild glaucoma, with a minimum IOP > 5 mmHg in all groups, without or with anti-glaucoma medications, respectively[14]. Additional surgical procedures, such as cataract surgery by phacoemulsification in lens-induced glaucoma and hyphema drainage in post-traumatic glaucoma, were performed when indicated.
Patients were followed up at 1 week, 1 month, 3 months, and 6 months for assessment of IOP and progression of optic disc changes. Visual field progression was evaluated at 3 months and 6 months after initiation of medical or surgical treatment. The clinical profile and treatment outcome were documented and IOP, optic disc changes, and visual field parameters were compared across different types of secondary glaucoma.
Assuming a 75% success rate for IOP reduction at six months, with a 95% confidence interval and 20% precision, the minimum required sample size was calculated to be 62 patients (82 eyes).
Data were analysed using SPSS version 20.0 (IBM Corp., Armonk, NY, United States). Categorical variables were represented as n (%), and continuous variables as mean ± SD. Repeated measures Analysis of Variance (ANOVA) test was used to compare quantitative parametric data over time. A P value < 0.05 was considered statistically significant.
A total of 62 patients diagnosed with secondary glaucoma were recruited in this study. Among them, 20 patients had bilateral involvement, resulting in a total of 82 eyes included in the analysis. The common causes of secondary glaucoma were pseudoexfoliaton glaucoma (26.8%), NVG (17.1%), traumatic glaucoma (13.4 %), steroid-induced glaucoma (12.2%), miscellaneous causes (11.0%), lens-induced glaucoma (LIG) (8.5%), developmental glaucoma (6.1%) and uveitic glaucoma (4.9%). Miscellaneous causes included pseudophakic glaucoma, post vitrectomy glaucoma, pigment dispersion syn
Thirty-six eyes (43.9%) were from patients aged > 60 years. Steroid-induced glaucoma, was the most common etiology in patients aged < 20 years (55.5%) and 21-40 years (41.6%). Neovascular glaucoma was most frequently observed in the 41-60 years age group, (36.0%), while PXF glaucoma predominated in patients aged > 60 years of age (55.5%). Among the study participants, 22 (33.8%) patients had associated systemic comorbidities, diabetes mellitus was present in 13 (16.1%) patients, hypertension in 6 (9.7%), and both conditions in 3 (3.2%) patients.
The BCVA was categorized according to WHO classification for visual impairment. The mean BCVA at the presentation was 3/60 on Snellen’s chart. A total of 41.4% of eyes had BCVA < 3/60 meeting the WHO definition of blindness. Among specific etiologies, 50% of eyes with NVG and 36.4% eyes with traumatic glaucoma had BCVA < 3/60. In lens-induced glaucoma, 71.4% of eyes had BCVA < 1/60 likely due to the presence of mature cataract. In contrast, up to 80.0% of eyes with steroid-induced glaucoma presented with relatively good BCVA, falling in the category of 6/18-6/6. Most eyes with uveitic glaucoma, developmental glaucoma, and miscellaneous causes had BCVA > 6/60.
The mean IOP at presentation was 34.7 ± 10.46 mmHg and the distribution across various etiologies is presented in Table 1. Overall, 44.7% of eyes presented with severe glaucoma PXF glaucoma was the most common cause among eyes in the severe category.
| Type of secondary glaucoma | Total | |||||||||
| PXF | Trauma | NVG | LIG | SIG | Uveitic | Developmental | Others | |||
| IOP at presentation in mmHg, % | ≤ 20 | 2 | 0 | 0 | 0 | 4 | 0 | 0 | 0 | 6 |
| 9.1 | 0.0 | 0.0 | 0.0 | 40.0 | 0.0 | 0.0 | 0.0 | 7.3 | ||
| 21-30 | 8 | 5 | 3 | 3 | 2 | 2 | 2 | 4 | 29 | |
| 36.4 | 45.5 | 21.4 | 42.9 | 20.0 | 50.0 | 40.0 | 44.4 | 35.4 | ||
| 31-40 | 9 | 3 | 8 | 1 | 2 | 1 | 2 | 3 | 29 | |
| 40.9 | 27.3 | 57.1 | 14.3 | 20.0 | 25.0 | 40.0 | 33.3 | 35.4 | ||
| > 40 | 3 | 3 | 3 | 3 | 2 | 1 | 1 | 2 | 18 | |
| 13.6 | 27.3 | 21.4 | 42.9 | 20.0 | 25.0 | 20.0 | 22.2 | 22.0 | ||
| Total | 22 | 11 | 14 | 7 | 10 | 4 | 5 | 9 | 82 | |
| 100.0 | 100.0 | 100.0 | 100.0 | 100.0 | 100.0 | 100.0 | 100.0 | 100.0 | ||
Out of 82 eyes, 59 were treated medically with anti-glaucoma medications, and 23 were treated surgically. Patients were followed up at 1 week, 1 month, 3 months, and 6 months after treatment initiation. There was a statistically significant improvement in mean BCVA at subsequent follow-ups (P = 0.0001, repeated measures ANOVA).
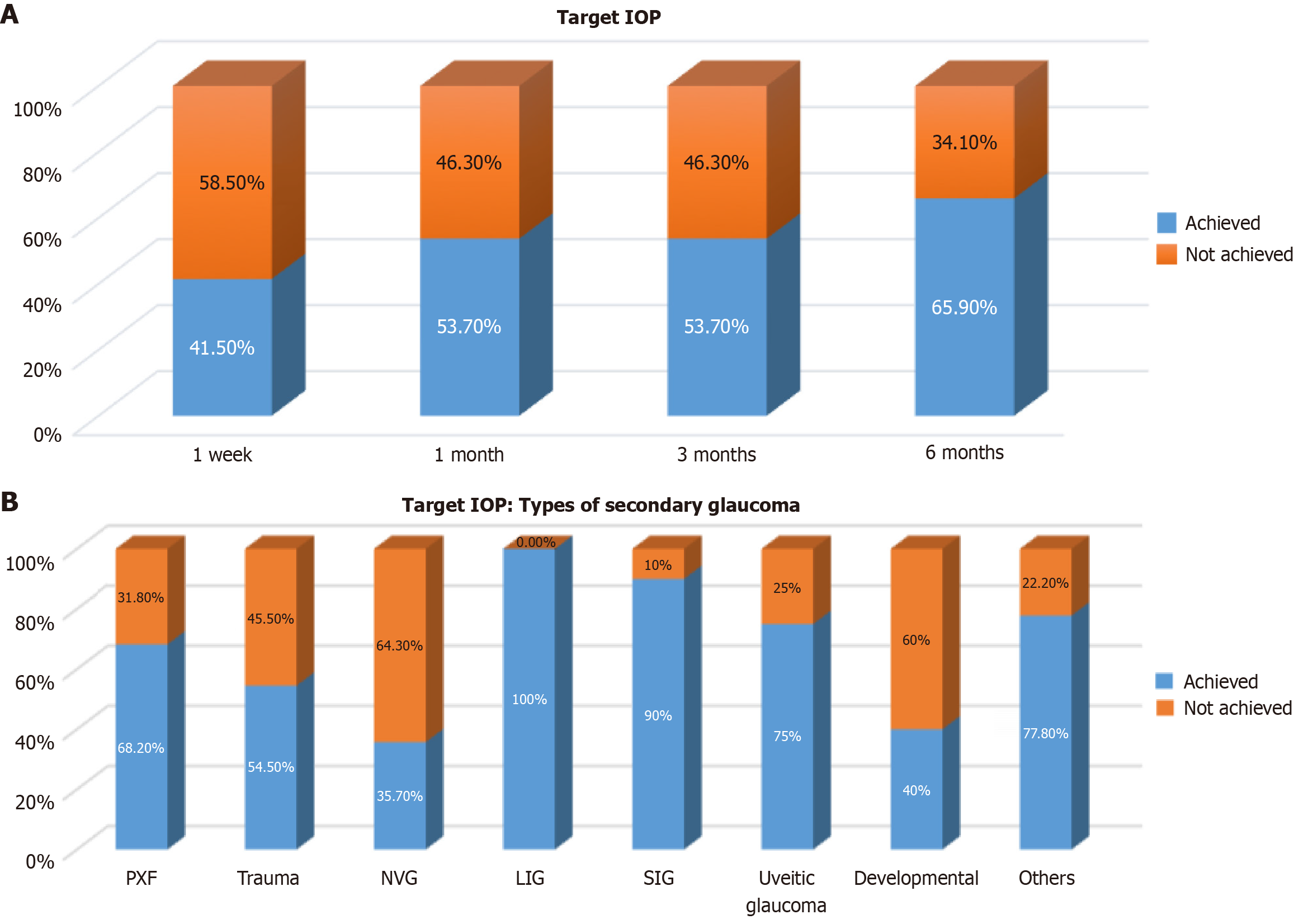
A significant reduction in mean IOP was observed at all follow-up visits compared to baseline (P = 0.0001, repeated measures ANOVA). Detailed IOP trends are summarized in Table 2. At 1 week, 41.5% of eyes achieved target IOP, which increased to 65.9% at 6 months. The proportion of eyes achieving target IOP at different follow-up intervals is shown in Figure 2A, and across different types of secondary glaucoma in Figure 2B.
| mean ± SD | n | F value | P value | |
| IOP in mmHg at presentation | 34.72 ± 10.46 | 82 | 201.64 | 0.0001 |
| At 1 week | 18.65 ± 7.27 | 82 | ||
| At 1 month | 16.71 ± 6.42 | 82 | ||
| At 3 months | 16.63 ± 5.39 | 82 | ||
| At 6 months | 16.65 ± 7.22 | 82 |
The mean cup-to-disc (C:D) ratio at presentation was 0.795 ± 0.121. At follow-up visits (1-week, 1 month, 3 months, and 6 months), the mean C:D ratios were 0.780, 0.785, 0.787, and 0.795, respectively. Pairwise comparison showed no statistically significant change over time (P = 1.000).
The mean RNFL thickness at presentation was 50.08 ± 31.20 μm. Post-treatment mean RNFL thickness values at 1 week, 1 month, 3 months, and 6 months were 65.07 μm, 63.82 μm, 63.29 μm, and 62.44 μm, respectively. This improvement was statistically significant (P = 0.0001).
Visual field analysis was performed in 41 eyes. The mean deviation (MD) at presentation was -11.766 ± 9.164 dB. The mean MD at 3 months and 6 months was -12.16 dB and -12.22 dB, respectively. The change in MD over time was not statistically significant (P = 0.337).
Among the 62 patients, 30 had been diagnosed with glaucoma prior to COVID-19 pandemic. Approximately 64.6% reported disruption in regular follow-up due to repeated shutdowns and lockdown & mobility restrictions. Additionally, 45.1% of the patients reported poor treatment compliance due to difficulty in accessing medications. Delays in surgical care were also noted, with 10.9% of patients experiencing postponement of cataract surgery and 15.9% experiencing delay in glaucoma surgery. Overall, 47.6% of patients reported a history of COVID-19 infection during the study period (Supplementary Table 1).
During the post-pandemic period (18 months), 80 patients (110 eyes) with secondary glaucoma were enrolled. Neovascular glaucoma (27.3%) was the most common etiology, followed by PXF glaucoma (18.2%), steroid-induced glaucoma (14.5%), miscellaneous causes (11.8%), traumatic glaucoma (10.9%), uveitic glaucoma (9.1%), and developmental glaucoma (8.2%) respectively. Out of 110 eyes, 66 (60.0%) were treated medically, and 44 (40.0%) surgically. The mean IOP at presentation (35.2 ± 9.46 mmHg), and treatment success rates at follow-ups were comparable to those observed during the pandemic period. A comparative summary of clinical presentation and etiological distribution between the pandemic and post-pandemic periods is provided in Table 3.
| COVID-19 | Post COVID-19 | P value | |
| Number of patients | 62 | 82 | |
| Number of eyes affected | 82 | 110 | 0.86 |
| Male:female ratio | 2.8:1 | 1.8:1 | 0.79 |
| PXF | 22 (26.8) | 20 (18.2) | 0.04 |
| NVG | 14 (17.1) | 30 (27.3) | |
| Traumatic | 11 (13.4) | 12 (10.9) | |
| SIG | 10 (12.2) | 16 (14.5) | |
| LIG | 7 (8.5) | 0 (0.00) | |
| Developmental | 5 (6.1) | 9 (8.2) | |
| Uveitic | 4 (4.9) | 10 (9.1) | |
| Miscellaneous | 9 (11.0) | 13 (11.8) | |
| Medical management in percentage | 59 (71.9) | 66 (60.0) | 0.07 |
| Surgical management in percentage | 23 (28.1) | 44 (40.00) | |
| Mean IOP at presentation in mmHg | 34.7 ± 10.46 | 35.2 ± 9.46 | 0.73 |
| Mean IOP at 6 months in mmHg | 16.65 ± 7.22 | 14.95 ± 6.45 | 0.087 |
The purpose of the study was to evaluate and present the demographic and clinical profile of various types of secondary glaucoma during the COVID-19 pandemic and analyse the management outcomes in a tertiary care institute in eastern India. The management outcomes were primarily assessed in terms of intraocular pressure, optic disc changes, and visual field changes in eyes with clear media.
According to this study, PXF glaucoma was the most common cause of secondary glaucoma, comprising 26.8% of the total cases. Studies conducted in Western population in the 1990s also reported PXF glaucoma as the leading cause of secondary glaucoma[15,16]. Most studies in the Indian population have reported a lower prevalence[10,17-19]. Similarly, recent studies from Asia have reported a lower prevalence[20-22]. However, a study by Al Obeidan et al[23] reported in as many as 54% of cases, and a study by Sherpa and Pokhrel[24] in Nepal (2014-2016), reported PXF (6.7%) as a significant cause of secondary glaucoma. These differences may be attributed to numerous factors such as demographic profile, educational status, health awareness among the patients, and availability of quality diagnostic and treatment facilities. The incidence of aphakic glaucoma, which was the most common cause of secondary glaucoma 40 years ago[17], has declined significantly due to advancements in cataract surgeries.
The prevalence of secondary glaucoma was highest in individuals aged > 60 years (40.3%). Steroid-induced glaucoma was the most common cause in patients younger than 40 years, which is a matter of concern for the over-the-counter availability of steroids for conditions like allergic conjunctivitis and vernal keratoconjunctivitis. A majority of PXF cases were found in individuals above 60 years, consistent with Ramanarao and Jain[19].
Most cases in this study were unilateral (67.7%), reinforcing the importance of excluding secondary causes in all cases of unilateral glaucoma.
In this study, males were more frequently affected which may be attributed to cultural differences, resulting in a male predominance in seeking treatment, and this has been found in all leading studies done in the last two decades[18-22,24]. The study revealed that the predominant cause of secondary glaucoma in male eyes was PXF, whereas in females, it was lens-induced glaucoma. Analysis of sex distribution across different types of secondary glaucoma indicated a higher prevalence in male eyes compared to female eyes in all types, except for lens-induced glaucoma, where females constituted a higher proportion (28.6%). Similar findings have been reported in other prominent studies as well[18-20]. The higher prevalence of LIG in females may be attributed to anatomical factors such as smaller eyes, rendering them more susceptible to phacomorphic glaucoma[25,26]. Additionally, in our study, delayed presentation of mature cataracts for surgery was identified as important contributing factor for LIG. This delay was largely influenced by challenges in accessing medical care during the COVID-19 pandemic, marked by repeated shutdowns and lockdowns, with the majority of hospitals halting routine elective procedures, including cataract surgeries. Consequently, many patients presented with phacomorphic and phacolytic glaucoma as ophthalmic emergencies during this period.
We observed statistically significant improvement in BCVA at follow-up visits compared with baseline. This im
An IOP of ≥ 30 mmHg was observed in nearly 50% or more of eyes across all types of secondary glaucoma except steroid-induced glaucoma (40%). A statistically significant reduction was noted at all follow-up visits compared to baselines for all 82 eyes (P value < 0.05). This holds true for patients treated both medically and surgically treated groups.
Target IOP was achieved in 41.5% at one week, which increased to 65.9% at six months of follow-up. However, 34.1% of eyes overall (39% of 59 eyes treated medically and 21.7% of 23 eyes treated surgically) did not achieve the predefined target IOP at six-months. This may be attributed to various factors such as, different pathologies as the cause, poor compliance with medications, early post-operative bleb fibrosis, and the stringent target IOP criteria applied in the study. Consequently, a few eyes with clinically acceptable IOP control were categorised as not having achieved target IOP. The mean IOP at follow-up visits were consistently lower in the surgical group compared to the medical group, indicating greater effectiveness of surgical intervention in achieving IOP reduction.
Among specific etiologies, only 35.7% of NVG and 40% of developmental causes had achieved target IOP at six months, reflecting the refractory nature of these conditions. In contrast, the majorities of eyes with lens-induced glaucoma (85.7%) and steroid-induced glaucoma (90%) achieved the target IOP. There were no cases in the medical group that were considered for surgery during the follow-up period of 1 week, 1 month, and 3 months. Because, in many cases, the achieved IOP was close to the predefined target IOP without evidence of progressive visual field deterioration. In other cases, surgical intervention was not pursued due to poor visual prognosis secondary to the underlying primary pathology. However, there were two cases from the medical management group (one in the PXF group and one in the NVG group) failed to achieve the target IOP at the end of six months and demonstrated progressive visual field loss; these eyes subsequently underwent filtration surgery (trabeculectomy with MMC).
Among all eyes with NVG, 85.8% of eyes presented late with moderate-to-severe glaucoma, which may be attributed to the aggressive nature of NVG. The effect of COVID-19 likely contributed to this delayed presentation due to the reduced hospital visits and disrupted follow-up care. As most NVG cases were secondary to diabetic retinopathy, optimal glycemic control and timely management with retinal laser photocoagulation and anti-VEGF therapy were suboptimal during repeated lockdowns and healthcare service disruptions.
A study by Das and Senthil[27] from India reported a 6.6-fold increase of NVG and a 2.7-fold lens induced glaucoma one year after the onset of COVID-19 pandemic. Another study from south India by Krishna et al[28] also observed that lens induced glaucoma (phacomorphic and phacolytic) was the most common glaucoma emergency during first lockdown and second lockdown periods followed by NVG.
The analysis of the C:D ratio of all 82 eyes inferred that there was no statistically significant change in the mean C:D ratio in the subsequent post-treatment follow-up compared with baseline. This stability may indicate effective disease control and prevention of further structural progression. Evaluation of the average RNFL thickness in 55 eyes revealed a statistically significant increase in average RNFL thickness during post-treatment follow-up compared to baseline values. A study by Raghu et al[29] reported similar finding of a statistically significant increase in average RNFL thickness following trabeculectomy. A plausible clarification proposed for the immediate increase in RNFL thickness post-treatment is the reversal of the physical compressive effect on the RNFL by the elevated pre-treatment intraocular pressure, allowing restoration of the normal contour and configuration of retinal ganglion cell axons[30]. Another proposed mechanism is transient retinal swelling secondary to acute reduction in IOP following treatment[31].
The change in mean deviation index in the visual field was not statistically significant at three and six months compared with the baseline. This suggests adequate IOP control during the follow up periods, preventing further functional progression of visual field changes over six months.
When compared with the post-pandemic cohort evaluated over a similar duration, the overall clinical profile of secondary glaucoma showed some differences, although the severity at presentation remained largely comparable. The male-to-female ratio (1.8:1) demonstrated relative improvement in the post-pandemic period, possibly reflecting improved access to hospital services for both genders following restoration of routine healthcare facilities.
In the post-pandemic cohort, neovascular glaucoma emerged as the most common etiology, followed by PXF glaucoma. The increased proportion of NVG may be attributed to reduced access to routine healthcare services during COVID-19 restrictions, particularly for systemic conditions such as diabetes and hypertension. Inadequate control of these systemic diseases, along with delayed management of retinal pathologies, likely contributed to the development of late complications, including NVG, in the post-pandemic period. Neovascular glaucoma was reported as the most common emergency glaucoma presentation during the unlock period between first and second lock down of COVID-19 in the study conducted by Krishna et al[28] from south India.
In this study, PXF continued to show a significant prevalence in the post-pandemic period, underscoring the importance of this condition in the studied geographical area. There was no significant difference in presentation in other types of glaucoma between the post-pandemic and the pandemic period except for lens-induced glaucoma. Notably, no cases of lens-induced glaucoma were observed in the post-pandemic cohort. This may be explained by improved healthcare access to cataract surgical services after the pandemic, preventing progression to mature or hypermature cataracts and their associated complications.
In the post-pandemic period, 60% of eyes were managed medically and 40% surgically. In contrast, during the COVID-19 period, only 28% of eyes underwent surgical intervention. This difference is expected, as surgical procedures were limited during the pandemic due to restrictions in operation theatre functioning and challenges in postoperative follow-up[32,33]. However, overall management outcomes in terms of visual acuity and IOP control were comparable between the two periods.
This prospective observational study provides valuable region-specific data on the demographic and clinical profile of secondary glaucoma in eastern India, where limited published evidence exists. It comprehensively evaluates both medical and surgical management strategies and six-month outcomes, including IOP control, structural parameters (cup-to-disc ratio and RNFL thickness), and functional assessment through visual field analysis, thereby reflecting real-world tertiary care practice. The study uniquely documents the impact of the COVID-19 pandemic on glaucoma care, highlighting disruptions in follow-up, medication access, and surgical services that contributed to advanced presentations, particularly increased lens-induced glaucoma due to delayed cataract surgery and advanced NVG associated with poor systemic disease control. Additionally, comparison with a post-pandemic cohort using identical protocols strengthens temporal analysis and enhances methodological rigor through standardized target IOP and surgical success criteria.
Due to the COVID-19 pandemic, there was a delay in treating cases requiring elective surgery. The follow-up period in this study was restricted to six months, although follow-up for a longer time would be required to comment on the clinical course of each type of secondary glaucoma. In OCT evaluation, ganglion cell complex was not studied; only RNFL was assessed. Due to poor vision, not all patients could undergo visual field and OCT examination during follow-up. The direct effect of COVID-19 infection on eyes and treatment was not mentioned in the manuscript as our objective was to see the profile and treatment outcome of secondary glaucoma in COVID-19 period.
In this study, PXF glaucoma emerged as the most common cause of secondary glaucoma, particularly among the elderly, with an overall male predominance. Steroid-induced glaucoma was more frequent in younger patients. Secondary glaucoma was predominantly unilateral and often presented with markedly elevated IOP (> 30 mmHg) and significant visual impairment, with many cases showing severe optic disc and visual field damages. While medical management was effective in most cases, surgical intervention was necessary for advanced disease or extremely high IOP. The COVID-19 pandemic posed substantial challenges in the timely management of secondary glaucoma, highlighting the importance of maintaining healthcare access and preparedness during public health emergencies to prevent disease progression and visual loss.
| 1. | Harasymowycz P, Birt C, Gooi P, Heckler L, Hutnik C, Jinapriya D, Shuba L, Yan D, Day R. Medical Management of Glaucoma in the 21st Century from a Canadian Perspective. J Ophthalmol. 2016;2016:6509809. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 58] [Cited by in RCA: 81] [Article Influence: 8.1] [Reference Citation Analysis (1)] |
| 2. | Foster PJ, Buhrmann R, Quigley HA, Johnson GJ. The definition and classification of glaucoma in prevalence surveys. Br J Ophthalmol. 2002;86:238-242. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1354] [Cited by in RCA: 1657] [Article Influence: 69.0] [Reference Citation Analysis (1)] |
| 3. | Tham YC, Li X, Wong TY, Quigley HA, Aung T, Cheng CY. Global prevalence of glaucoma and projections of glaucoma burden through 2040: a systematic review and meta-analysis. Ophthalmology. 2014;121:2081-2090. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6080] [Cited by in RCA: 4983] [Article Influence: 415.3] [Reference Citation Analysis (2)] |
| 4. | Imrie C, Tatham AJ. Glaucoma: the patient's perspective. Br J Gen Pract. 2016;66:e371-e373. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 15] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 5. | Hashemi H, Mohammadi M, Zandvakil N, Khabazkhoob M, Emamian MH, Shariati M, Fotouhi A. Prevalence and risk factors of glaucoma in an adult population from Shahroud, Iran. J Curr Ophthalmol. 2019;31:366-372. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 29] [Article Influence: 3.6] [Reference Citation Analysis (1)] |
| 6. | McMonnies CW. Glaucoma history and risk factors. J Optom. 2017;10:71-78. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 322] [Cited by in RCA: 251] [Article Influence: 27.9] [Reference Citation Analysis (1)] |
| 7. | Sihota R, Shakrawal J, Sidhu T, Sharma AK, Dada T, Pandey V. Does TRABECULECTOMY meet the 10-10-10 challenge in PACG, POAG, JOAG and Secondary glaucomas? Int Ophthalmol. 2020;40:1233-1243. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 6] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 8. | Sun Y, Liang Y, Zhou P, Wu H, Hou X, Ren Z, Li X, Zhao M. Anti-VEGF treatment is the key strategy for neovascular glaucoma management in the short term. BMC Ophthalmol. 2016;16:150. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 29] [Cited by in RCA: 46] [Article Influence: 4.6] [Reference Citation Analysis (1)] |
| 9. | Ritch R, Schlötzer-Schrehardt U. Exfoliation syndrome. Surv Ophthalmol. 2001;45:265-315. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 536] [Cited by in RCA: 612] [Article Influence: 24.5] [Reference Citation Analysis (1)] |
| 10. | Dubey S, Jain K, Mukherjee S, Sharma N, Pegu J, Gandhi M, Bhoot M. Current profile of secondary glaucoma in a Northern India tertiary eye care hospital. Ophthalmic Epidemiol. 2019;26:200-207. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 11] [Article Influence: 1.6] [Reference Citation Analysis (1)] |
| 11. | Tejwani S, Angmo D, Nayak BK, Sharma N, Sachdev MS, Dada T, Sinha R. Response to comments on: Preferred practice guidelines for glaucoma management during COVID-19 pandemic. Indian J Ophthalmol. 2020;68:2312-2313. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 12. | Hodapp E, Parrish RK II Anderson DR. Clinical decisions in glaucoma. St. Louis: Mosby, 1993: 52-61. |
| 13. | Sihota R, Angmo D, Ramaswamy D, Dada T. Simplifying "target" intraocular pressure for different stages of primary open-angle glaucoma and primary angle-closure glaucoma. Indian J Ophthalmol. 2018;66:495-505. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 89] [Cited by in RCA: 125] [Article Influence: 15.6] [Reference Citation Analysis (1)] |
| 14. | Casson RJ, Chidlow G, Wood JP, Crowston JG, Goldberg I. Definition of glaucoma: clinical and experimental concepts. Clin Exp Ophthalmol. 2012;40:341-349. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 245] [Cited by in RCA: 330] [Article Influence: 23.6] [Reference Citation Analysis (1)] |
| 15. | Strohl A, Pozzi S, Wattiez R, Roesen B, Miño de Kaspar H, Klauss V. [Secondary glaucoma in Paraguay. Etiology and incidence]. Ophthalmologe. 1999;96:359-363. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 9] [Article Influence: 0.3] [Reference Citation Analysis (1)] |
| 16. | Schwartz EC, Mutumba RN, Schaal ST, Spiegel D, Klauss V. [Etiology of secondary glaucoma at university clinics in Munich and Nairobi]. Ophthalmologe. 1995;92:577-580. [PubMed] |
| 17. | Agarwal HC, Sood NN, Kalra BR, Ghosh B. Secondary Glaucoma. Indian J Ophthalmol. 1982;30:121-124. [PubMed] |
| 18. | Gadia R, Sihota R, Dada T, Gupta V. Current profile of secondary glaucomas. Indian J Ophthalmol. 2008;56:285-289. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 32] [Article Influence: 1.8] [Reference Citation Analysis (1)] |
| 19. | Ramanarao S, Jain D. A clinical study of secondary glaucoma. Indian J Clin Exp Ophthalmol. 2020;6:5-8. [DOI] [Full Text] |
| 20. | Gurung J, Sitoula RP, Singh AK. Profile of Secondary Glaucoma in a Tertiary Eye Hospital of Eastern Nepal. Nepal J Ophthalmol. 2021;13:98-103. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (1)] |
| 21. | Komaratih E, Rindiastuti Y, Primitasari Y. Profile of Secondary Glaucoma at a Tertiary Hospital in East Java. Folia Med Indones. 2020;56:56. [DOI] [Full Text] |
| 22. | Gong H, Ren J, Zheng B, Huang X, Liao Y, Zhou Y, Lin M. The Profile of Secondary Glaucoma in China: A Study of Over 10,000 Patients. J Glaucoma. 2021;30:895-901. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 9] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 23. | Al Obeidan SA, Dewedar A, Osman EA, Mousa A. The profile of glaucoma in a Tertiary Ophthalmic University Center in Riyadh, Saudi Arabia. Saudi J Ophthalmol. 2011;25:373-379. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 52] [Article Influence: 3.5] [Reference Citation Analysis (1)] |
| 24. | Sherpa D, Pokhrel S. Current pattern of secondary glaucoma. J Chitwan Med Coll. 2017;7:21-24. [DOI] [Full Text] |
| 25. | Lee JW, Lai JS, Lam RF, Wong BK, Yick DW, Tse RK. Retrospective analysis of the risk factors for developing phacomorphic glaucoma. Indian J Ophthalmol. 2011;59:471-474. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 10] [Article Influence: 0.7] [Reference Citation Analysis (1)] |
| 26. | Zhumageldiyeva FE, Dzhumataeva Z, Dauletbekov D, Suleymenov M, Utelbayeva Z, Meyermanova Z, Teleuova T. A-Scan Parameters and the Risk of Phacomorphic Glaucoma in the Kazakh Population. Medicina (Kaunas). 2022;58:1544. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 27. | Das AV, Senthil S. Year One of COVID-19 Pandemic: Effect on Presentation of Patients With Glaucoma in a Multi-Tier Ophthalmology Network in India. Front Ophthalmol (Lausanne). 2022;2:900988. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 28. | Krishna U, Odayappan A, Venkatesh R, Kavitha S. Changes in emergency glaucoma care during the COVID-19 pandemic in South India. Indian J Ophthalmol. 2023;71:864-868. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 29. | Raghu N, Pandav SS, Kaushik S, Ichhpujani P, Gupta A. Effect of trabeculectomy on RNFL thickness and optic disc parameters using optical coherence tomography. Eye (Lond). 2012;26:1131-1137. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 34] [Article Influence: 2.4] [Reference Citation Analysis (1)] |
| 30. | Quigley HA, Addicks EM, Green WR, Maumenee AE. Optic nerve damage in human glaucoma. II. The site of injury and susceptibility to damage. Arch Ophthalmol. 1981;99:635-649. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 763] [Cited by in RCA: 862] [Article Influence: 19.2] [Reference Citation Analysis (1)] |
| 31. | Emery JM, Landis D, Paton D, Boniuk M, Craig JM. The lamina cribrosa in normal and glaucomatous human eyes. Trans Am Acad Ophthalmol Otolaryngol. 1974;78:OP290-OP297. [PubMed] |
| 32. | Rao A, Senthil S. Effect of COVID-19 on glaucoma surgical practice in India: The challenges faced and the outcomes. J Clin Ophthalmol Res. 2023;11:114-118. [DOI] [Full Text] |
| 33. | Ayub G, de Vasconcelos JPC, Costa VP. The Impact of Covid-19 in the Follow-Up of Glaucoma Patients in a Tertiary Center: A Comparison Between Pre-Pandemic and Pandemic Periods. Clin Ophthalmol. 2021;15:4381-4387. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 21] [Article Influence: 4.2] [Reference Citation Analysis (1)] |