Published online Apr 16, 2026. doi: 10.12998/wjcc.v14.i11.119572
Revised: February 20, 2026
Accepted: March 10, 2026
Published online: April 16, 2026
Processing time: 68 Days and 20.6 Hours
Rectal foreign bodies (RFBs), mostly due to self-insertion for sexual pleasure, are occasionally encountered in emergency departments. They are more common in young male patients, and because patients often delay seeking medical attention due to embarrassment, complications such as perforation and peritonitis may be present at diagnosis. Emergency physicians must remain mindful of potential RFB insertion and conduct history-taking and physical examinations with sensitivity to patient embarrassment. Reports of penetrating peritonitis caused by long-term RFB retention are rare.
A 16-year-old male experienced persistent fever of approximately 38 °C for 35 days. Although antipyretics and antibiotics were prescribed at a local clinic, his symptoms did not improve. Later, he disclosed that his condition had worsened after inserting a smartphone stand into his rectum 35 days before for sexual gratification, and he was referred to our hospital. Upon arrival, his vital signs were stable, and mild tenderness was noted in the left lower abdomen. Laboratory tests revealed leukocytosis and elevated C-reactive protein levels (5.21 mg/dL). Abdominal computed tomography revealed a spring-like foreign body and a large amount of fecal material in the rectum. Endoscopic removal was unsuccessful; therefore, laparotomy was performed for object extraction. Intraoperatively, the rectum was found to have perforated into the retroperitoneal cavity. The postoperative course was uneventful, and the patient was discharged 11 days after admission.
We report a case of penetrating peritonitis after long-term RFB retention, without an acute abdomen, because the perforation was retroperitoneal.
Core Tip: Rectal foreign bodies (RFBs) are occasionally encountered, and most cases involve self-insertion for sexual pleasure. They are common in young male patients, and because patients often delay seeking medical attention due to embarrassment, complications such as perforation and peritonitis may already be present at diagnosis. Physicians must remain mindful of the possibility of RFB insertion and conduct history-taking and physical examinations with sensitivity to patient embarrassment. We report the first case of penetrating peritonitis caused by long-term RFB retention, which did not present as an acute abdomen because the perforation was confined to the retroperitoneal space.
- Citation: Usuda D, Furukawa D, Imaizumi R, Ono R, Kaneoka Y, Nakajima E, Kato M, Sugawara Y, Shimizu R, Inami T, Sakurai R, Kawai K, Matsubara S, Tanaka R, Suzuki M, Shimozawa S, Hotchi Y, Osugi I, Katou R, Ito S, Mishima K, Kondo A, Mizuno K, Takami H, Komatsu T, Nomura T, Sugita M. Perforative peritonitis caused by long-term retention of a rectal foreign body: A case report. World J Clin Cases 2026; 14(11): 119572
- URL: https://www.wjgnet.com/2307-8960/full/v14/i11/119572.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i11.119572
Rectal foreign bodies (RFBs) are common and should be recognized as a potentially serious condition that may require urgent proctological surgical intervention[1-5]. Most patients with RFBs present to the emergency room usually after exhausting efforts to remove the object at home[2,6]. Retained RFBs, although common, can pose a unique problem to the acute care surgeon or emergency room physician, due to the variety of objects and difficulty of their extraction[7-10]. There is no limit to the types of objects inserted into the anal canal, and reports have documented various foreign objects. Unusual objects contribute to the growing list of reported occurrences due to their unusual location, presenting clinicians with diagnostic and therapeutic dilemmas that are characterized by severe possible complications and different therapeutic opportunities[4,8,11-13]. Due to their rarity, treating physicians rarely have a standard approach to diagnosis, extraction techniques, and post-extraction care assessment[13].
There is little epidemiologic information on these cases[14]. The incidence of RFB cases has been increasing in recent years, primarily attributable to auto-erotic acts, sexual behaviors, sexual assaults, behavioral disorders, or ingestion, with rare instances of accidental causes. This rising trend is predominantly observed in young patients[1,2,10,14,15]. Anorectal auto-eroticism is a paraphilic involving self-insertion of various objects into the anal canal and rectal cavity to increase or enhance sexual pleasure[4,16,17]. Based on a meta-analysis, the motivation of RFB insertion is mostly sexual stimulation (36%)[7]. Occasionally, a foreign object may be ingested and successfully pass through the entire gastrointestinal tract, being retained in the rectum[16]. Occasionally, the objects are inserted by children themselves[15,18]. In extremely rare cases, foreign bodies in adjacent tissues or organs can penetrate the rectal wall and enter the rectal lumen[16].
Here, we report the first case of penetrating peritonitis caused by long-term RFB retention (35 days). In this case, the patient did not present with an acute abdomen because the perforation was confined to the retroperitoneal space. These findings are novel and are reported in this study.
A 16-year-old male patient was referred to our hospital due to persistent fever of approximately 38 °C for 35 days and a 5 kg weight loss in 1 month.
Although antipyretics and antibiotics were prescribed at a local clinic, his symptoms did not improve. Later, he disclosed that his condition had worsened after inserting a smartphone stand into his rectum as part of an autoerotic paraphilic activity for sexual gratification 35 days before, and he was referred to our hospital.
The patient had no significant medical history, including mental illness.
He was a high school student and did not require assistance with daily activities. He had no allergies, underwent annual health checkups, and no abnormalities were noted during his most recent examination 6 months prior. He lived with his parents, twin brother, and sister; there was no family history of hereditary or malignant diseases.
The patient was 170 cm tall and weighed 53 kg, with a body mass index of 18.3 kg/m². At the outpatient department, his vital signs were normal: Blood pressure of 114/60 mmHg, a regular heart rate of 96 beats per minute, body temperature of 36.0 °C, oxygen saturation of 98% on room air, respiratory rate of 18 breaths per minute, and Glasgow Coma Scale score of 15 points (E4V5M6). Physical examination revealed mild tenderness in the left lower abdomen.
Routine serum laboratory examinations performed upon arrival at the outpatient department revealed an increased white blood cell count, neutrophil proportion, C-reactive protein level, and total bilirubin level (Table 1). Urinalysis was not performed because the patient did not complain of lower urinary tract symptoms. Negative test results were returned for a rapid BinaxNOW™ coronavirus disease 2019/Flu A&B Combo Self Test.
| Parameter (unit) | Measured value | Normal value |
| White blood cells (103/µL) | 12.2 | 3.9-9.7 |
| Neu (%) | 82 | 37-72 |
| Lym (%) | 12 | 25-48 |
| Mon (%) | 5 | 2-12 |
| Eos (%) | 1 | 1-9 |
| Bas (%) | 0 | 0-2 |
| Hemoglobin (g/dL) | 13.6 | 13.4-17.1 |
| Platelets (103/µL) | 232 | 153-346 |
| Aspartate transaminase (IU/L) | 19 | 5-37 |
| Alanine aminotransferase (IU/L) | 22 | 6-43 |
| Lactic acid dehydrogenase (U/L) | 143 | 124-222 |
| Alkaline phosphatase (U/L) | 97 | 38-113 |
| Gamma-glutamyl transpeptidase (IU/L) | 33 | 0-75 |
| Total bilirubin (mg/dL) | 1.9 | 0.4-1.2 |
| Total protein (g/dL) | 7 | 6.5-8.5 |
| Albumin (g/dL) | 3.9 | 3.8-5.2 |
| Creatine kinase (U/L) | 102 | 57-240 |
| Blood urea nitrogen (mg/dL) | 13 | 9-21 |
| Creatinine (mg/dL) | 0.81 | 0.6-1 |
| Amylase (IU/L) | 110 | 43-124 |
| Sodium (mEq/L) | 137 | 135-145 |
| Potassium (mEq/L) | 3.9 | 3.5-5 |
| Chloride (mEq/L) | 101 | 96-107 |
| C-reactive protein (mg/dL) | 5.21 | 0-0.29 |
| Plasma glucose (mg/dL) | 84 | 65-109 |
| Procalcitonin (ng/mL) | 0.2 | 0-0.5 |
| Lactate (mmol/L) | 1.1 | 1-1.5 |
| Hepatitis B virus surface antigen | Negative | |
| Hepatitis C virus antibody | Negative | |
| Rapid plasma reagin qualitative test | Negative | |
| Treponema pallidum hemagglutination test qualitative test | Negative |
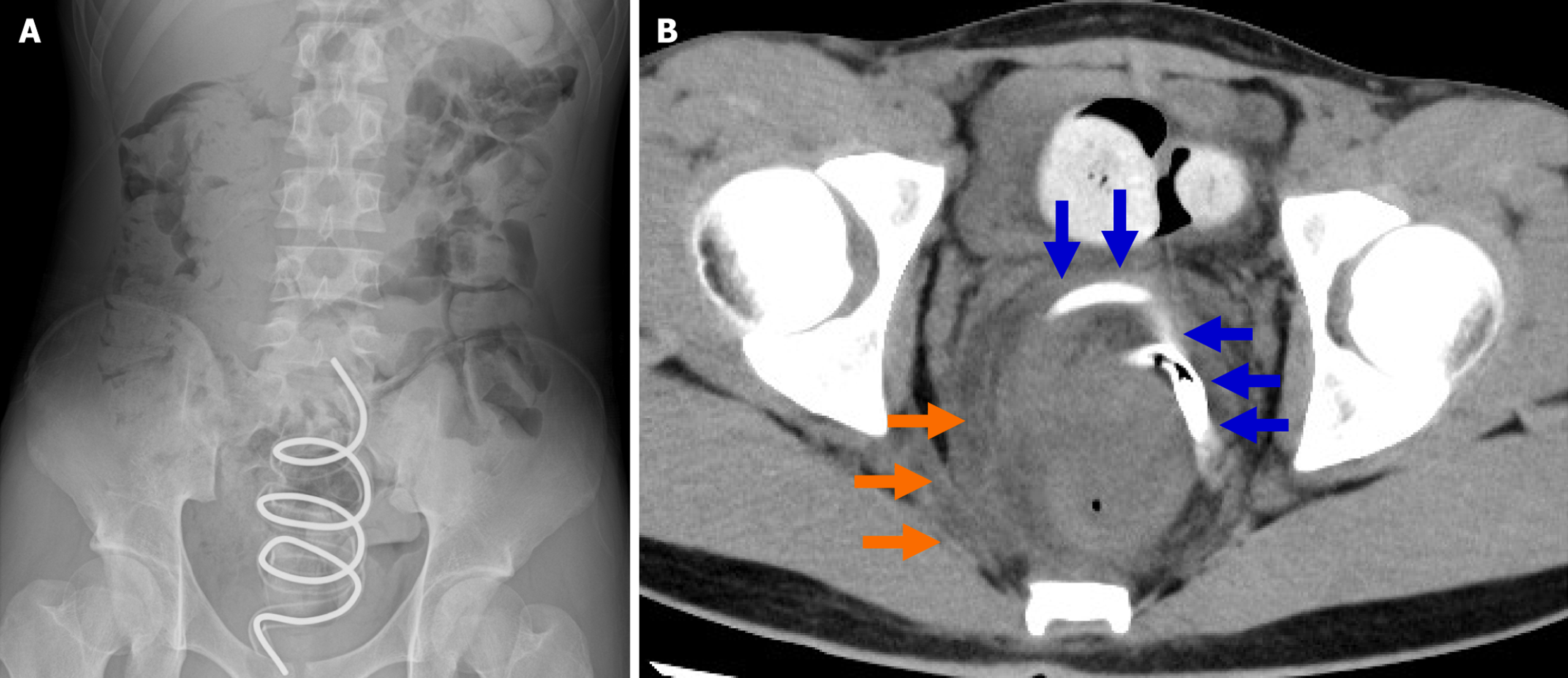
Supine abdominal radiography showed a low-radiolucent spiral-shaped foreign body measuring 17.5 cm long and 6.3 cm wide in the pelvic cavity, along with gas and a large amount of fecal material in the colon (Figure 1A). Plain abdominal computed tomography (CT) revealed the presence of a foreign body in the rectum (blue arrows), with edema of the rectal wall and increased density of the surrounding fat tissue (orange arrows). In addition, marked fecal retention was obs
The suspected diagnosis was an RFB caused by a smartphone stand, resulting in perforative peritonitis.
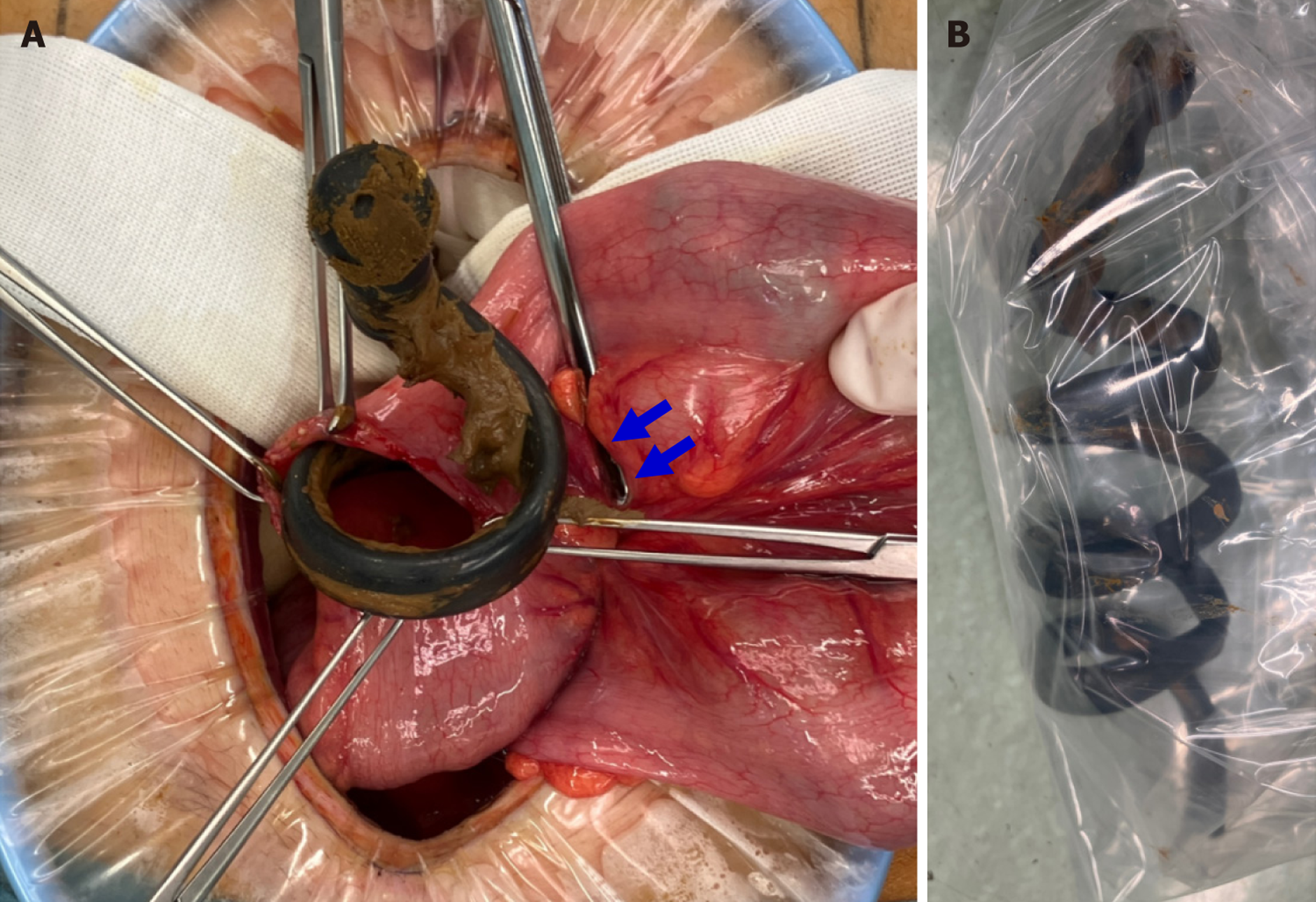
Endoscopic removal was unsuccessful; therefore, a laparotomy was performed to extract the object. It was approximately 70 cm in length. Intraoperatively, the rectum was perforated into the retroperitoneal cavity (Figure 2A). Images of the removed foreign body are presented in Figure 2B.
The postoperative course was uneventful. Antibiotic therapy was discontinued on postoperative day 5, and oral intake of a liquid diet was initiated on the same day. His recovery remained favorable; the intra-abdominal drain was removed on postoperative day 6, and he was discharged on postoperative day 11.
We report the first known case of penetrating peritonitis caused by long-term RFB retention (35 days), which did not present as an acute abdomen because the perforation was confined to the retroperitoneal space. This is new knowledge, and consequently, there is value in reporting this case. In addition, the diagnosis was delayed because of an atypical course, including young age, mild abdominal findings, and prolonged fever. This case offers an important clinical insight.
In an epidemiological study between 2012 and 2021 in the United States, patients were typically young (the average age was 43 years) and predominantly male, with a male-to-female ratio of 6:1 from 20 years to 90 years of age, and a bimodal age distribution[7,8,14]. Males exhibited a bimodal age distribution, with peaks in the fifth decade, whereas females showed a right-skewed distribution that peaked in the second decade. The types of RFBs are classified into the following categories: Everyday items, food, and sexual articles[19]. Sexual devices (55%) and glass objects (18%) were the most commonly self-inserted RFBs, and remedies for constipation were present in 0.4% of patients[7,14]. In this case, the patient was male and had inserted a foreign body through his anus to obtain sexual gratification, which was consistent with previous reports[4,16]. In contrast, the patient was 16 years old, which was younger than those described in previous cases[14].
The timing of presentation varies widely. Some individuals seek immediate emergency care due to significant discomfort or inability to retrieve the object, while others delay for several days to weeks[7,20]. Patient management includes a detailed history and examination, followed by necessary tests, as careful assessment is essential for accurate diagnosis of RFBs[8,21]. Early diagnosis and timely intervention are important to prevent complications in RFBs[22]. Proper imaging to assess the object’s shape, size, nature, and location is essential[22]. However, diagnosis is often delayed due to patient embarrassment and reluctance to seek medical help, which may increase the likelihood of complications[3,23]. Therefore, patient histories should be taken with the appropriate sensitivity after diagnostic evaluation and identification of the object[7]. Additionally, clinicians should be aware of this condition, as it could indicate underlying psychiatric issues, drug trafficking, or sexual assault[3]. Reports of penetrating peritonitis caused by prolonged foreign body retention are rare. However, its occurrence is a well-established fact. In this case, gradual weight loss in one of the twins raised concerns about his health among family members, leading to medical consultation and ultimately to the diagnosis of an RFB. The severity of rectal injury was determined using the Rectal Organ Injury Scale (ROIS) as follows: Grade I - contusion or hematoma without devascularization or partial thickness laceration; Grade II - laceration involving 50% of the rectal wall circumference; Grade III - laceration involving > 50% of the rectal wall circumference; Grade IV - full-thickness laceration extending into the perineum; and Grade V - devascularized segment[4].
Treating RFBs presents a complex challenge for surgeons because of various factors, including the type of object, the patient's anatomy, how long it has been inserted, possible associated injuries, and the level of local contamination[5,10,24]. To date, there is no standardized management protocol for RFBs that aids in the avoidance of serious complications[5,12]. However, there are currently studies that precisely indicate strategies for the diagnosis and treatment of rectal injuries caused by foreign bodies[25]. While most cases are effectively managed with conservative treatment, surgical intervention might sometimes be needed[10]. When extracting a foreign object, the primary consideration is choosing the least invasive and safest method for the patient. Usually, removal under anesthesia is a safe approach, though laparotomy carries the standard surgical risks[6,18,21]. Extraction, when possible, allows the avoidance of surgery that might be necessary in the case of failure or complications[11]. Most of the time, these can be removed trans-anally at the bedside using anesthesia, along with manipulation techniques involving specialized devices or endoscopy for challenging objects, with only a small proportion of patients requiring hospitalization for > 24 hours[1,8]. Absolute contraindications to the transanal approach include peritonitis secondary to rectal or bowel perforation, clinical signs of sepsis or hemodynamic instability, and radiologic evidence of perforation, such as intra-abdominal free air on plain radiographs or CT, or the presence of free fluid[4,26]. Surgical interventions have been reported to be necessary in the following cases: Cases with acute abdomens due to intestinal perforations, pelvic abscesses, obstruction, and bleeding; when the object is fragile and poses a high-risk during removal; and when the object is too large to be removed manually, has migrated proximally, or when the object is deeply impacted at the rectal valves[7,21]. Specifically, if the patient does not have peritonitis or per
RFBs inserted into the anus constitute one of the most important problems needing emergency surgery due to their potential complications[21]. While most RFBs typically do not cause major injury, inserting certain objects into the rectum can lead to unpredictable and potentially deadly consequences[17]. According to a meta-analysis, the total complication rate of RFBs was described to be 30%, and rectal perforation or peritonitis caused by foreign bodies has been reported[7,12,28]. Rectal injury was more severe in patients with self-inserted RFBs, such as rectal laceration, rectal mucosal ulcers, and bleeding[13]. Occurrence of retained RFBs with bowel perforation resulting from auto-eroticism is rare among males[23].
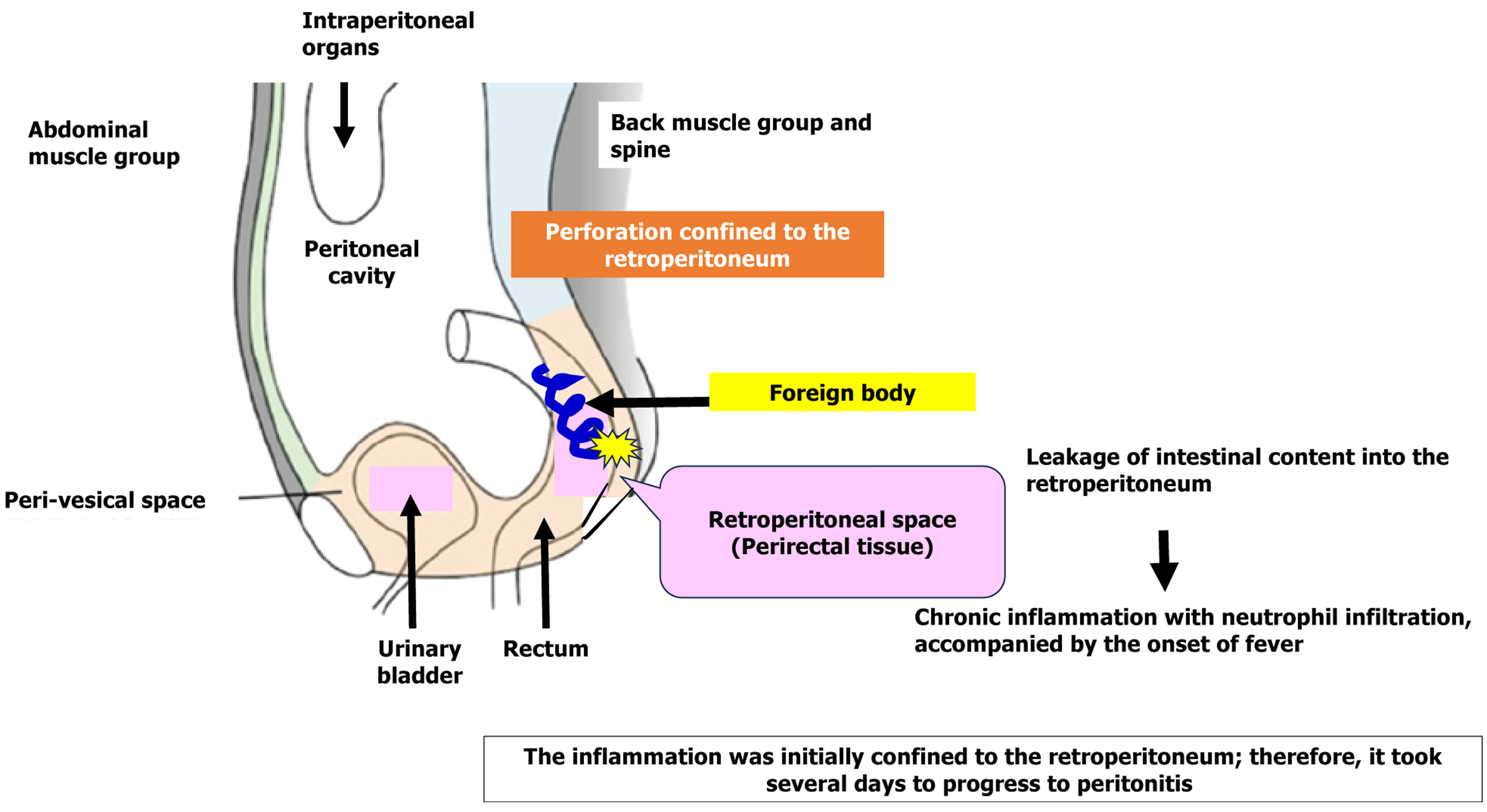
We discuss the pathophysiology of rectal perforations with retroperitoneal penetration, as observed in this case. Typical rectal perforation can have a fatal course. In the present case, the sharp, pointed shape of the object and pro
This case report is limited since it only reports a single case. Therefore, the actual condition and characteristics of the disease may deviate from the findings of the literature review due to reporting bias. Further studies are necessary to better assess the effects of clinical presentation, laboratory and imaging tests, treatment approaches, and outcomes.
Herein, we report the first known case of penetrating peritonitis caused by long-term RFB retention (35 days). A high index of suspicion, a systematic approach, and a low threshold for imaging studies are essential for the successful management and positive outcomes of patients with RFBs. Emergency physicians should conduct history-taking and physical examinations with sensitivity to the patient’s embarrassment while always considering the possibility of foreign body insertion. In addition, in cases of RFBs, objects with certain shapes are more likely to cause intestinal perforation and may require surgical intervention for removal; therefore, careful management is essential.
| 1. | Bhasin S, Williams JG. Rectal foreign body removal: increasing incidence and cost to the NHS. Ann R Coll Surg Engl. 2021;103:734-737. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 9] [Reference Citation Analysis (0)] |
| 2. | Gentile M, Cestaro G, Di Filippo G, Amato B, Sivero L. Successful transanal removal of unusual foreign body self-inserted in the rectum A case report and review of literature. Ann Ital Chir. 2019;90:88-92. [PubMed] |
| 3. | Ebrahim M, Perdawood SK. [Rectal foreign bodies]. Ugeskr Laeger. 2018;180:V11170866. [PubMed] |
| 4. | Kumar P, Rehman S, Rana AKS. Approach to rectal foreign body: an unusual presentation. BMJ Case Rep. 2018;2018:bcr2018224253. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (1)] |
| 5. | Fritz S, Killguss H, Schaudt A, Sommer CM, Richter GM, Belle S, Reissfelder C, Loff S, Köninger J. Proposal of an algorithm for the management of rectally inserted foreign bodies: a surgical single-center experience with review of the literature. Langenbecks Arch Surg. 2022;407:2499-2508. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 6. | Son MY, Park SJ, Moon W, Oh GM, Park MI, Kim SE, Kim JH, Jung K. Endoscopy-assisted Removal of a Large Rectal Foreign Body by the Valsalva Maneuver. Korean J Gastroenterol. 2020;76:42-45. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.5] [Reference Citation Analysis (1)] |
| 7. | Ploner M, Gardetto A, Ploner F, Scharl M, Shoap S, Bäcker HC. Foreign rectal body - Systematic review and meta-analysis. Acta Gastroenterol Belg. 2020;83:61-65. [PubMed] |
| 8. | Ikram S, Singh S, Kallam R, Dabra A. A play that went wrong: Unique presentation of bowel perforation from an unusually large per-rectal foreign body. BMJ Case Rep. 2017;2017:bcr2017222959. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 4] [Article Influence: 0.4] [Reference Citation Analysis (2)] |
| 9. | Liu C, Li Y. Rectal foreign body of a cosmetic bottle treated successfully by transanal retrieval: A case report. Medicine (Baltimore). 2024;103:e40651. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 10. | Hassine HB, Chaka A, Ouertani F, Jabra SB, Korbi I, Noomen F. Management of a rectal entrapped foreign body: a case report. Pan Afr Med J. 2024;48:162. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 11. | Slaiki S, El Bouhaddouti H, Mouaqit O, Ousadden A, Taleb KA, Benjelloun EB. [Voluminous colorectal foreign bodies inserted voluntarily: about a case]. Pan Afr Med J. 2019;34:142. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.1] [Reference Citation Analysis (2)] |
| 12. | van Steenhoven J, van der Sluis P, Davids PHP, Verleisdonk EJMM. [A step-up approach for dealing with rectal foreign bodies]. Ned Tijdschr Geneeskd. 2018;162:D2891. [PubMed] |
| 13. | Zhang Y, Han Y, Xu H, Chen D, Gao H, Yuan H, Zeng X. A retrospective analysis of transanal surgical management of 291 cases with rectal foreign bodies. Int J Colorectal Dis. 2022;37:2167-2172. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (1)] |
| 14. | Loria A, Marianetti I, Cook CA, Melucci AD, Ghaffar A, Juviler P, Temple LK, Jones CMC, Fleming FJ. Epidemiology and healthcare utilization for rectal foreign bodies in United States adults, 2012-2021. Am J Emerg Med. 2023;69:76-82. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 9] [Reference Citation Analysis (1)] |
| 15. | Schellenberg M, Brown CVR, Trust MD, Sharpe JP, Musonza T, Holcomb J, Bui E, Bruns B, Hopper HA, Truitt MS, Burlew CC, Inaba K, Sava J, Vanhorn J, Eastridge B, Cross AM, Vasak R, Vercuysse G, Curtis EE, Haan J, Coimbra R, Bohan P, Gale S, Bendix PG; AAST Contemporary Management of Rectal Injuries Study Group. Rectal Injury After Foreign Body Insertion: Secondary Analysis From the AAST Contemporary Management of Rectal Injuries Study Group. J Surg Res. 2020;247:541-546. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 17] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 16. | Ye H, Huang S, Zhou Q, Yu J, Xi C, Cao L, Wang P, Gong Z. Migration of a foreign body to the rectum: A case report and literature review. Medicine (Baltimore). 2018;97:e11512. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 19] [Article Influence: 2.4] [Reference Citation Analysis (1)] |
| 17. | Hejna P, Zátopková L, Janík M. Rectal explosion: a strange case of autoerotic death. Int J Legal Med. 2021;135:307-312. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 6] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 18. | Brungardt JG, O'Dell RJ, Eaton SR, Bennett AW. Rectal foreign bodies: national outcomes after the operating room. Int J Colorectal Dis. 2021;36:265-269. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 6] [Article Influence: 1.2] [Reference Citation Analysis (1)] |
| 19. | Yang Z, Xin P, Zhou S, Zhou C, He X, Bao G. Systematic review of rectal foreign bodies in older men: humanistic care and a novel challenge for society. Ann Transl Med. 2022;10:164. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 5] [Article Influence: 1.3] [Reference Citation Analysis (1)] |
| 20. | Lake JP, Essani R, Petrone P, Kaiser AM, Asensio J, Beart RW Jr. Management of retained colorectal foreign bodies: predictors of operative intervention. Dis Colon Rectum. 2004;47:1694-1698. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 131] [Cited by in RCA: 102] [Article Influence: 4.6] [Reference Citation Analysis (2)] |
| 21. | Cinar H, Berkesoglu M, Derebey M, Karadeniz E, Yildirim C, Karabulut K, Kesicioglu T, Erzurumlu K. Surgical management of anorectal foreign bodies. Niger J Clin Pract. 2018;21:721-725. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 7] [Article Influence: 0.9] [Reference Citation Analysis (1)] |
| 22. | Nepal A, Maharjan S, Chalise A, Rajbhandari AP. Rectal Foreign Body: A Case Report. JNMA J Nepal Med Assoc. 2022;60:1049-1051. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (1)] |
| 23. | Simbila AN, Suphian A, Ngowi NJ, Mfinanga RJ, Kilindimo S, Sawe HR. Colon perforation by foreign body insertion for sexual gratification: a case report. Pan Afr Med J. 2021;40:188. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 24. | Lian C, Hou JG, Wang J, Liu XJ, Li XL. An unusual rectal foreign body: A sundried corn-stick. Trop Doct. 2023;53:307-308. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 25. | Easton-Carr R, Paish LM. Rectum Foreign Body Removal. 2025 Jul 7. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan. [PubMed] |
| 26. | Pokharel A, Singh JK, Khadka BR, Adhikari S, Dhakal S. Rectal foreign body and its association with social stigma and mental health: A case report. Int J Surg Case Rep. 2024;124:110236. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 27. | Bisgin T, Sogucak S, Manoğlu B, Derici ZS, Atila K, Sokmen S. Surgical management of rectal foreign bodies: A single-center experience. Ulus Travma Acil Cerrahi Derg. 2023;29:304-309. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 28. | Bains L, Gupta A, Kori R, Kumar V, Kaur D. Transanal high pressure barotrauma causing colorectal injuries: a case series. J Med Case Rep. 2019;13:133. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 9] [Article Influence: 1.3] [Reference Citation Analysis (1)] |