Published online Apr 16, 2026. doi: 10.12998/wjcc.v14.i11.119232
Revised: February 12, 2026
Accepted: March 3, 2026
Published online: April 16, 2026
Processing time: 77 Days and 13.7 Hours
Primary adrenal insufficiency [Addison’s disease (AD)] is a rare but potentially life-threatening endocrine disorder caused by impaired cortisol and aldosterone production. While autoimmune adrenalitis is the most common etiology in adults, genetic causes account for a substantial proportion of childhood-onset cases and should be actively investigated. Among inherited etiologies, X-linked adrenoleukodystrophy (X-ALD) is one of the most important genetic causes of primary adrenal insufficiency in males. X-ALD is a peroxisomal disorder caused by pathogenic variants in the ABCD1 gene, leading to impaired degradation of very long-chain fatty acids. Its clinical spectrum ranges from isolated adrenal insufficiency to progressive cerebral demyelination or adrenomyeloneuropathy.
We report a 27-year-old male diagnosed with AD in early childhood who re
This case illustrates that childhood-onset AD in males may represent the earliest manifestation of X-ALD and that the “Addison-only” phenotype does not confer long-term neurological protection. The late emergence of psy
Core Tip: Adrenoleukodystrophies are a heterogeneous neurological occurrence and sometimes their differential diagnosis might be difficult. Addison disease among other background conditions might be related to such a progressive disorder that could lead to severe neurological injury. We present a case where the nervous symptomatology was delayed vis-à-vis the initial and main disease, and whose psychiatric signs preceded gait instability, impaired balance, and dysarthria. Imaging and genetic studies are of particular diagnostic importance in this setting.
- Citation: Djamandi P, Gorica H, Kyriakou O, Xhukellari E, Rroji A, Vyshka G. Late-onset neurological manifestations of X-linked adrenoleukodystrophy in a male with childhood-onset Addison’s disease: A case report. World J Clin Cases 2026; 14(11): 119232
- URL: https://www.wjgnet.com/2307-8960/full/v14/i11/119232.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i11.119232
Primary adrenal insufficiency (PAI) also known as Addison’s disease (AD) is a rare but potentially life-threatening endocrine disorder resulting from impaired cortisol and aldosterone production due to dysfunction or destruction of the adrenal cortex. In adults, the most common etiology is autoimmune adrenalitis; however, in childhood-onset cases, genetic causes account for a substantial proportion and should be actively investigated[1].
Among inherited causes, X-linked adrenoleukodystrophy (X-ALD) is among the most critical genetic etiologies of primary adrenal insufficiency in males[2]. X-ALD is a peroxisomal disorder caused by pathogenic variants in the ABCD1 gene located on chromosome Xq28, leading to defective transport and degradation of very long-chain fatty acids (VLCFAs)[3].
The clinical spectrum of X-ALD is highly heterogeneous, ranging from isolated adrenal insufficiency to progressive inflammatory cerebral demyelination or adrenomyeloneuropathy (AMN). In many affected boys, adrenal insufficiency is the first manifestation and may remain the only clinical feature for years or even decades, a presentation commonly referred to as the “Addison-only” phenotype[2].
Despite an initial endocrine-only presentation, studies have demonstrated that a significant proportion of patients eventually develop neurological involvement later in life, including adult-onset cerebral adrenoleukodystrophy (ALD) or AMN, even after prolonged periods of apparent clinical stability[2].
Furthermore, psychiatric and behavioral symptoms are increasingly recognized as early manifestations of cerebral disease in adolescents and adults and may precede overt neurological decline, frequently leading to diagnostic delay[2].
We report the case of a young man diagnosed with AD in early childhood who developed psychiatric and neurological manifestations more than two decades later, ultimately leading to the diagnosis of X-ALD. This case underscores the importance of considering X-ALD in males with early-onset primary adrenal insufficiency and highlights the need for systematic screening and lifelong neurological surveillance, even in patients with long-standing endocrine-only disease.
A 27-year-old male, diagnosed with AD at age five and maintained on fludrocortisone therapy, remained in good health until presentation to our neurological facility.
At this age, he developed prominent psychiatric and behavioral changes, including marked disinhibition; aggressive and irritable behavior toward family members, friends, and colleagues; and socially inappropriate conduct in professional settings.
These symptoms were accompanied by intrusive and recurrent sexual thoughts and impaired impulse control, including the expression of sexually inappropriate comments in the workplace. The behavioral disturbances led to sig
Approximately one year prior to presentation, the patient developed insidious psychiatric and behavioral changes. Family members reported progressive disinhibition, irritability, and reduced emotional regulation, with episodes of verbal aggressiveness toward relatives, friends, and colleagues. These behavioral changes were accompanied by impaired impulse control and hypersexual behavior, characterized by intrusive sexual thoughts and socially inappropriate comments, including inappropriate remarks in the workplace. The patient demonstrated limited insight into these behaviors, leading to significant interpersonal conflict and occupational difficulties. Psychiatric evaluation led to initiation of risperidone therapy (titrated to 2 mg/day) for behavioral dysregulation and impulse control symptoms. Although mild reduction in irritability was reported, hypersexual behavior and the other symptoms persisted.
Nothing worth to mention was reported.
Notably, his younger brother had been diagnosed with AD at the age of 22 and was receiving similar treatment, raising suspicion of a familial disorder. Genetic testing confirmed the presence of a hemizygous pathogenic variant [c.1415_1416del p. (Gln472ArgfsTer83)] in the ABCD1 gene, thereby establishing the diagnosis of X-ALD.
Two years after the onset of psychiatric symptoms, the patient experienced progressive gait instability, impaired balance, and dysarthria.
On neurological examination, the patient was alert and oriented but exhibited mild executive dysfunction and reduced verbal fluency. Speech was dysarthric with a scanning quality. Cranial nerve examination was normal. Motor exami
Endocrine evaluation confirmed persistent primary adrenal insufficiency. Baseline morning serum cortisol levels were markedly reduced, with inappropriately elevated plasma adrenocorticotropic hormone concentrations, consistent with long-standing primary adrenal failure. Electrolyte levels were within normal limits under chronic replacement therapy. There was no clinical or biochemical evidence of adrenal crisis at presentation.
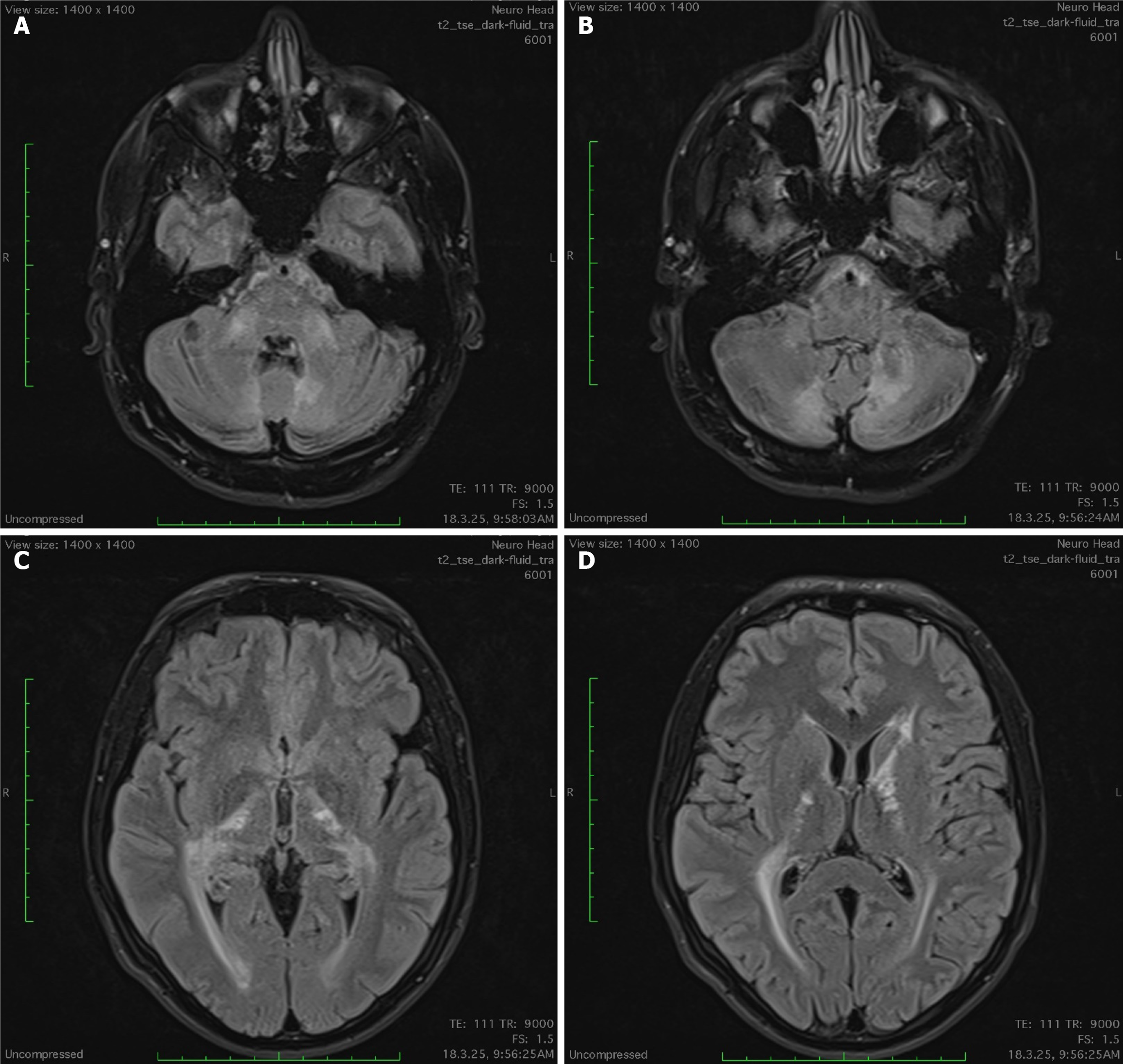
Brain magnetic resonance imaging (MRI) revealed bilateral, nearly symmetrical white matter hyperintensities on T2-weighted, fluid-attenuated inversion recovery (FLAIR) sequences, while spinal MRI was unremarkable. These radiologic findings suggested ALD (Figure 1).
Given the clinical suspicion of X-ALD, plasma VLCFA analysis was performed and revealed elevated concentrations of hexacosanoic acid (C26:0) and increased C24:0/C22:0 and C26:0/C22:0 ratios, consistent with a peroxisomal β-oxidation defect.
With no definitive curative genetic treatment at hand, the patient was referred for continuous psychiatric monitoring and was suggested yearly imaging control of the brain.
The next imaging examination still to be scheduled; while the patient is under antipsychotic therapy.
This case illustrates the clinically challenging association between childhood-onset AD and X-ALD, highlighting the potential for very late neurological manifestations after a prolonged “Addison-only” phenotype[2]. The patient developed neuropsychiatric and motor symptoms more than two decades after the diagnosis of PAI, underscoring the importance of lifelong neurological surveillance in male patients with early-onset AD of unknown etiology.
X-ALD is caused by pathogenic variants in the ABCD1 gene, located on Xq28[4]. This gene encodes the ALD protein, a peroxisomal membrane transporter responsible for the import of VLCFAs into peroxisomes for β-oxidation[2,4]. Dysfunction of this transporter leads to the accumulation of VLCFAs in the adrenal cortex, white matter, and spinal cord, resulting in adrenal insufficiency and progressive neurodegeneration. Adrenal involvement often precedes neurological disease and may represent the earliest or sole manifestation for years, particularly in boys[2,5].
The so-called “Addison-only” phenotype is well described. Approximately 80% of boys with X-ALD experience adrenal insufficiency in childhood, typically before the onset of neurological symptoms[2,6,7]. However, studies have demonstrated that neurological manifestations often emerge later in life, including adult-onset cerebral ALD or AMN, even after decades of apparent clinical stability[2]. This case exemplifies such delayed neurological progression, with symptom onset more than 20 years after initial endocrine presentation.
A notable feature of this case is the psychiatric prodrome, characterized by behavioral disinhibition and intrusive thoughts, which preceded overt neurological decline by approximately two years. Psychiatric and behavioral changes are increasingly recognized as manifestations of cerebral ALD, particularly in adults, and may mimic primary psychiatric disorders, leading to diagnostic delay[8,9]. Involvement of the frontal white matter is thought to underlie these symptoms[2,3,10].
Neuroimaging findings were essential in raising suspicion for X-ALD[11]. The presence of bilateral, nearly symmetrical white matter hyperintensities on T2-weighted and FLAIR sequences is characteristic of cerebral ALD and should prompt metabolic and genetic evaluation, particularly in patients with a history of adrenal insufficiency. Approximately 80% of patients initially develop demyelination in the splenium of the corpus callosum, with subsequent spread to the adjacent parieto-occipital white matter[2]. The most frequent presentation of the cerebral form is a lesion in the parieto-occipital white matter[11,12]. Although spinal MRI was unremarkable in this case, this does not exclude early AMN or evolving central nervous system involvement, as spinal cord pathology may develop later or remain clinically silent for prolonged periods.
The familial history of AD in the patient’s younger brother further supported a genetic etiology. Identification of a hemizygous pathogenic ABCD1 variant confirmed the diagnosis. Genetic testing revealed the ABCD1 variant c.1415_1416del p. (Gln472ArgfsTer83), which results in a shift in the reading frame starting at codon 472 in exon(s) no. 5 (of 10). According to HGMD professional 2024.4, this variant has previously been reported as disease-causing in ALD[12-14]. These findings highlight the importance of family screening, as male relatives may be at risk of developing neurological disease, and female carriers may develop late-onset symptoms.
From a clinical standpoint, this case reinforces several critical principles. First, all males with idiopathic AD, particularly those diagnosed in childhood, should be screened for X-ALD using VLCFA analysis and/or genetic testing[2]. Second, the emergence of psychiatric symptoms in such patients should prompt consideration of cerebral involvement[8,9,12,15]. Finally, lifelong neurological follow-up is essential, even in patients with long-standing endocrine-only disease, as early detection of neurological progression may allow timely referral to specialized centers and consideration of disease-modifying strategies in selected cases.
This case illustrates how X-ALD may remain clinically silent from a neurological standpoint for more than two decades after childhood-onset adrenal insufficiency, presenting initially with isolated psychiatric and behavioral changes before overt motor symptoms emerge. In this patient, progressive disinhibition, hypersexual behavior, and impaired executive function preceded cerebellar and pyramidal signs by approximately two years, leading to an initial psychiatric diagnosis and delayed neurological evaluation.
The case underscores that new-onset behavioral or psychiatric symptoms in adults with a history of childhood-onset AD should raise suspicion for cerebral involvement, even in the absence of early motor deficits. Characteristic symmetric white matter abnormalities on MRI can be a decisive diagnostic clue when psychiatric symptoms obscure the underlying neurological disorder. Rather than representing a purely endocrine disorder, the “Addison-only” phenotype may be a temporally limited stage of a multisystem disease. Recognition of subtle neuropsychiatric changes in such patients is critical to avoid misattribution to primary psychiatric illness and to facilitate timely neurological assessment.
Systematic screening for X-ALD should be considered in all males with idiopathic primary adrenal insufficiency, particularly when diagnosed in childhood, and lifelong neurological surveillance is essential even in clinically stable patients. Early recognition of neurological progression has critical implications for patient management, family counseling, and genetic screening, underscoring the need for close collaboration between endocrinologists, neurologists, and genetic specialists.
| 1. | Bancos I, Hahner S, Tomlinson J, Arlt W. Diagnosis and management of adrenal insufficiency. Lancet Diabetes Endocrinol. 2015;3:216-226. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 358] [Cited by in RCA: 280] [Article Influence: 25.5] [Reference Citation Analysis (1)] |
| 2. | Engelen M, Kemp S, de Visser M, van Geel BM, Wanders RJ, Aubourg P, Poll-The BT. X-linked adrenoleukodystrophy (X-ALD): clinical presentation and guidelines for diagnosis, follow-up and management. Orphanet J Rare Dis. 2012;7:51. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 471] [Cited by in RCA: 384] [Article Influence: 27.4] [Reference Citation Analysis (1)] |
| 3. | Jain CK, Maurya S, Tripathi PK. Adrenoleukodystrophy: Current understanding of disease mechanisms, diagnosis, and therapeutic advances-a recent review. Brain Dev. 2025;47:104476. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 4. | Kemp S, Berger J, Aubourg P. X-linked adrenoleukodystrophy: clinical, metabolic, genetic and pathophysiological aspects. Biochim Biophys Acta. 2012;1822:1465-1474. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 228] [Cited by in RCA: 200] [Article Influence: 14.3] [Reference Citation Analysis (1)] |
| 5. | van Geel BM, Bezman L, Loes DJ, Moser HW, Raymond GV. Evolution of phenotypes in adult male patients with X-linked adrenoleukodystrophy. Ann Neurol. 2001;49:186-194. [PubMed] [DOI] [Full Text] |
| 6. | Dubey P, Raymond GV, Moser AB, Kharkar S, Bezman L, Moser HW. Adrenal insufficiency in asymptomatic adrenoleukodystrophy patients identified by very long-chain fatty acid screening. J Pediatr. 2005;146:528-532. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 116] [Cited by in RCA: 100] [Article Influence: 4.8] [Reference Citation Analysis (1)] |
| 7. | Cappa M, Todisco T, Bizzarri C. X-linked adrenoleukodystrophy and primary adrenal insufficiency. Front Endocrinol (Lausanne). 2023;14:1309053. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 19] [Article Influence: 6.3] [Reference Citation Analysis (1)] |
| 8. | Rosebush PI, Garside S, Levinson AJ, Mazurek MF. The neuropsychiatry of adult-onset adrenoleukodystrophy. J Neuropsychiatry Clin Neurosci. 1999;11:315-327. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 40] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 9. | Kitchin W, Cohen-Cole SA, Mickel SF. Adrenoleukodystrophy: frequency of presentation as a psychiatric disorder. Biol Psychiatry. 1987;22:1375-1387. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 29] [Article Influence: 0.7] [Reference Citation Analysis (1)] |
| 10. | Hayashida M, Horiguchi J. Adult-onset adrenoleukodystrophy with frontal lobe symptoms: a case report. Open J Psychiatry. 2015;5:180-185. [DOI] [Full Text] |
| 11. | Schiffmann R, van der Knaap MS. Invited article: an MRI-based approach to the diagnosis of white matter disorders. Neurology. 2009;72:750-759. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 474] [Cited by in RCA: 398] [Article Influence: 23.4] [Reference Citation Analysis (1)] |
| 12. | Shamim D, Alleyne K. X-linked adult-onset adrenoleukodystrophy: Psychiatric and neurological manifestations. SAGE Open Med Case Rep. 2017;5:2050313X17741009. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 11] [Article Influence: 1.2] [Reference Citation Analysis (1)] |
| 13. | Kemp S, Ligtenberg MJ, van Geel BM, Barth PG, Wolterman RA, Schoute F, Sarde CO, Mandel JL, van Oost BA, Bolhuis PA. Identification of a two base pair deletion in five unrelated families with adrenoleukodystrophy: a possible hot spot for mutations. Biochem Biophys Res Commun. 1994;202:647-653. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 53] [Article Influence: 1.7] [Reference Citation Analysis (1)] |
| 14. | Brownstone E, Voigtländer T, Baumhackl U, Finsterer J. Epilepsy in adult X-linked adrenoleucodystrophy due to the deletion c.1415-1416delAG in exon 5 of the ABCD1-gene. Gene. 2013;513:71-74. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 5] [Article Influence: 0.4] [Reference Citation Analysis (1)] |
| 15. | Galvão ACR, Machado-Porto GCL, Porto FHG, Lucato LT, Nitrini R. Adult-onset adrenoleukodystrophy presenting as a psychiatric disorder: MRI findings. Dement Neuropsychol. 2012;6:290-295. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 0.4] [Reference Citation Analysis (1)] |