Published online May 19, 2026. doi: 10.5498/wjp.v16.i5.116272
Revised: January 1, 2026
Accepted: February 6, 2026
Published online: May 19, 2026
Processing time: 162 Days and 23 Hours
Endoscopic submucosal dissection (ESD) has become the preferred treatment for early gastric cancer due to its minimal invasiveness and organ preservation. However, the cancer diagnosis and treatment process may serve as a traumatic source triggering post-traumatic stress disorder (PTSD) in patients. The incidence and risk factors of PTSD in early gastric cancer patients following ESD remain poorly characterized.
To investigate the incidence and risk factors of PTSD in patients with early gastric cancer after ESD, and to provide scientific evidence for clinical psychological in
A retrospective analysis was conducted on clinical data of 216 patients with early gastric cancer who underwent ESD treatment at the First Affiliated Hospital of Chongqing Medical University (a tertiary medical center performing approximately 800-1000 ESD procedures annually) from March 2023 to March 2024. All patients had complete data with no missing values. Preoperative psychological assessments (Self-Rating Anxiety Scale, Self-Rating Depression Scale, Social Sup
Among 216 patients, 56 developed PTSD, with an incidence rate of 25.9%. Multivariate logistic regression analysis showed that age [odds ratio (OR) = 1.060, 95% confidence interval (CI): 1.013-1.109, P = 0.012], unmarried/di
The prediction model based on multiple factors has good predictive performance and may facilitate identification of high-risk patients preoperatively, providing preliminary evidence for early psychological screening. However, prospective multicenter validation is required before clinical implementation.
Core Tip: We quantified post-traumatic stress disorder 3 months after endoscopic submucosal dissection for early gastric cancer and identified six independent preoperative factors - age, marital status, lesion size, ulcer, depression level, and social support. A pragmatic 6-factor model showed good discrimination (area under the curve = 0.856) and allows risk stratification before treatment. This approach supports routine preoperative screening and targeted psychological intervention to improve adherence and recovery.
- Citation: Liu J, Wang Y, Wang RH. Incidence and risk factors of post-traumatic stress disorder in patients after endoscopic submucosal dissection for early gastric cancer. World J Psychiatry 2026; 16(5): 116272
- URL: https://www.wjgnet.com/2220-3206/full/v16/i5/116272.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i5.116272
Gastric cancer is one of the most common malignant tumors worldwide, with both incidence and mortality rates ranking among the highest[1]. With the continuous development of endoscopic techniques and the popularization of early screening, the detection rate of early gastric cancer has been increasing year by year. Endoscopic submucosal dissection (ESD), as an important treatment method for early gastric cancer, has become the preferred treatment for patients meeting the indications due to its advantages of minimal trauma, rapid recovery, and preservation of organ function[2]. Although ESD is minimally invasive, several factors contribute to significant post-traumatic stress disorder (PTSD) risk: (1) The psychological impact of a “cancer” diagnosis itself - the existential threat and vulnerability associated with malignancy represents the primary traumatic stressor, independent of procedural invasiveness (diagnostic trauma); (2) Despite minimal invasiveness, the procedure duration (typically 1-3 hours) and the patient’s conscious or lightly sedated state during the operation may contribute to procedural distress (procedural trauma); and (3) Post-procedure concerns about potential complications (bleeding, perforation) and fear of recurrence or metastasis perpetuate the stress response. The cancer diagnosis likely constitutes the predominant PTSD trigger rather than the surgical procedure itself.
PTSD refers to a delayed and persistent mental disorder that occurs after an individual experiences, witnesses, or encounters a traumatic event, mainly manifested as traumatic re-experience, avoidance symptoms, and hyperarousal state[3]. Recent studies have found that cancer diagnosis and treatment can serve as a traumatic source leading to PTSD symptoms in patients, seriously affecting their quality of life and treatment compliance[4]. Foreign studies have reported that the incidence of PTSD in cancer patients ranges from 3% to 35%, with large variations possibly related to differences in cancer types, treatment methods, assessment tools, and assessment time points[5]. However, current domestic and international research on PTSD in patients after ESD for early gastric cancer is relatively limited, and its incidence and related risk factors have not been clearly established.
Identifying high-risk factors for PTSD development in patients after ESD has important clinical significance for early screening and timely intervention. Based on this, this study retrospectively analyzed clinical data of patients after ESD for early gastric cancer to explore the incidence of PTSD and its risk factors, aiming to provide scientific evidence for developing targeted psychological intervention strategies in clinical practice, thereby improving patient prognosis and enhancing their quality of life[6].
A retrospective study method was employed, selecting 216 early gastric cancer patients who underwent ESD treatment at the First Affiliated Hospital of Chongqing Medical University from March 2023 to March 2024 as study subjects. Sample demographics were consistent with other Chinese tertiary centers. All patients underwent routine follow-up after surgery, with the final follow-up completed in July 2025. This study was approved by the hospital ethics committee and granted exemption from informed consent.
Inclusion criteria: (1) Preoperatively diagnosed with early gastric cancer (including high-grade intraepithelial neoplasia) by gastroscopy and pathological biopsy; (2) Met ESD treatment indications and successfully completed ESD surgery; (3) Age ≥ 18 years; (4) Complete postoperative follow-up data, completed PTSD assessment at 3 months postoperatively; (5) Clear consciousness with normal comprehension and expression abilities; and (6) Complete clinical medical records.
Exclusion criteria: (1) Combined with other malignant tumors; (2) Pre-existing mental illness or cognitive dysfunction before surgery; (3) Experienced major traumatic events within 6 months before surgery (including but not limited to: Death of first-degree relatives, serious traffic accidents, natural disasters, violent injuries, and other stressful life events); (4) Long-term use of antipsychotic or antidepressant medications; (5) Severe complications during or after surgery requiring surgical treatment; (6) Incomplete clinical data or loss to follow-up; and (7) Combined with severe dysfunction of important organs such as heart, lungs, liver, or kidneys.
Data collection: All 216 patients had complete data with no missing values. Clinical data of patients were retrospectively collected through the hospital’s electronic medical record system and follow-up records, including: (1) General demographic data: Gender, age, education level (illiterate/primary school, junior high school, high school/technical secondary school, college and above), marital status (married/unmarried or divorced/widowed), occupation (employed, retired, unemployed); (2) Disease-related data: Lesion location, lesion size (maximum diameter, cm), pathological type (differentiated adenocarcinoma, undifferentiated adenocarcinoma), depth of invasion (according to Japanese Gastric Cancer Treatment Guidelines: Mucosal layer M, submucosal layer SM1/SM2), presence of ulcer [defined as pre-existing peptic ulcers identified at pre-operative endoscopy using Sydney System criteria: Mucosal defect ≥ 5 mm extending to muscularis mucosae or deeper with white coating/bleeding; only ulcers within/at tumor margin were included; ESD-induced ulcers were excluded; independent assessment by two endoscopists; distribution: PTSD group 37.5% (21/56) vs non-PTSD group 24.4% (39/160)], lymphovascular invasion, etc.; (3) Surgery-related data: En bloc resection rate (lesion removed as one piece), complete resection rate (en bloc resection with negative margins); and (4) Past medical history, family tumor history.
PTSD assessment: The PTSD Checklist-Civilian Version (PCL-C) was used to assess PTSD in all patients at 3 months postoperatively through outpatient or telephone follow-up. This scale contains 17 items divided into three dimensions: Re-experiencing symptoms (5 items, including recurrent intrusive traumatic memories, nightmares, flashbacks, etc.), avoidance/numbing symptoms (7 items, including avoidance of trauma-related stimuli, emotional numbing, decreased interest, etc.), and hyperarousal symptoms (5 items, including sleep disturbances, irritability, hypervigilance, etc.). A score ≥ 38 is a validated Chinese screening threshold (sensitivity 0.82, specificity 0.83) for identifying at-risk individuals. A score ≥ 50 corresponds to Diagnostic and Statistical Manual of Mental Disorders-IV criteria (specificity 0.94) for clinically significant PTSD. Primary analysis used ≥ 38; subgroup analysis compared moderate (38-49) vs severe (≥ 50) symptoms. A PCL-C total score ≥ 38 was used as the diagnostic threshold for positive PTSD screening, and ≥ 50 as the clinical threshold for PTSD diagnosis. This study primarily used ≥ 38 as the criterion for PTSD occurrence and conducted subgroup analysis for clinical PTSD patients with scores ≥ 50.
By retrospectively reviewing medical records, routine psychological assessment data from patients before surgery and at 3 months postoperatively were collected.
Self-Rating Anxiety Scale: This scale contains 20 items, of which 15 are negative statement items, and 5 are positive statement items. Each item uses a 4-point rating scale (1 = none or very little of the time, 2 = a small part of the time, 3 = a considerable amount of time, 4 = most or all of the time). The raw score is the sum of all item scores, standard score = raw score × 1.25 rounded to the nearest integer, with a standard score range of 25-100 points; higher scores indicate more severe anxiety.
Self-Rating Depression Scale: This scale contains 20 items, of which 10 are negative statement items, and 10 are positive statement items. Each item uses a 4-point rating scale (1 = none or very little of the time, 2 = a small part of the time, 3 = a considerable amount of time, 4 = most or all of the time). The raw score is the sum of all item scores, standard score = raw score × 1.25 rounded to the nearest integer, with a standard score range of 25-100 points; higher scores indicate more severe depression.
Social Support Rating Scale: This scale contains 10 items divided into three dimensions: Objective support (3 items, assessing actual support received), subjective support (4 items, assessing emotional support experienced by the individual), and utilization of social support (3 items, assessing the individual's utilization of social support). The total score is the sum of all item scores, ranging from 12 points to 66 points; higher scores indicate better social support levels.
SPSS 26.0 statistical software was used for data analysis. Complete case analysis was employed, excluding cases with missing key variables. For continuous variables, normality was first tested using the Shapiro-Wilk test; those following normal distribution were expressed as mean ± SD, and independent samples t-test was used for comparison between groups; those not following normal distribution were expressed as median (interquartile range) [M (P25, P75)], and Mann-Whitney U test was used for comparison between groups; categorical variables were expressed as number (percentage) [n (%)], and χ2 test or Fisher’s exact test (when theoretical frequency < 5) was used for comparison between groups. Univariate analysis was used to screen possible influencing factors of PTSD occurrence, and variables with P < 0.10 in univariate analysis were included in multivariate Logistic regression analysis, using the stepwise backward elimination method (elimination criterion P > 0.10) to screen independent risk factors for PTSD occurrence. Multicollinearity was diagnosed using the variance inflation factor (VIF), with VIF > 10 indicating the presence of collinearity. The receiver operating characteristic (ROC) curve was used to evaluate the discrimination of the prediction model, calculating the area under the curve (AUC) and 95% confidence interval. P < 0.05 was considered statistically significant. Model calibration was assessed using the Hosmer-Lemeshow test and calibration plot. Bootstrap validation (1000 iterations) was performed to calculate the optimism-corrected C-index and assess overfitting risk.
This study included 216 patients after ESD for early gastric cancer, including 138 males (63.9%) and 78 females (36.1%), aged 39-78 years, with an average age of (60.3 ± 9.7) years. At 3-month follow-up after surgery, using the PCL-C scale for assessment, a total of 56 patients had PCL-C total scores ≥ 38, with a PTSD incidence of 25.9%. Among them, 18 patients had PCL-C total scores ≥ 50, accounting for 8.3% of the total. There were statistically significant differences between the two groups in age, education level, marital status, occupation, lesion size, presence of ulcer, lymphovascular invasion, and family tumor history (P < 0.10), while other indicators showed no statistically significant differences (P > 0.10) (Table 1).
| Item | Category/unit | PTSD group (n = 56) | Non-PTSD group (n = 160) | Test statistic | P value |
| Gender | Male | 33 (58.9) | 105 (65.6) | χ2 = 0.838 | 0.36 |
| Female | 23 (41.1) | 55 (34.4) | |||
| Age (years)1 | M (P25, P75) | 63.0 (58.0, 68.0) | 59.0 (54.0, 65.0) | Z = -2.456 | 0.014 |
| Education level | Illiterate/primary | 18 (32.1) | 28 (17.5) | χ2 = 7.624 | 0.054 |
| Junior high | 22 (39.3) | 58 (36.3) | |||
| High school/technical | 12 (21.4) | 48 (30.0) | |||
| College and above | 4 (7.1) | 26 (16.3) | |||
| Marital status | Married | 42 (75.0) | 142 (88.8) | χ2 = 6.589 | 0.01 |
| Unmarried/divorced/widowed | 14 (25.0) | 18 (11.3) | |||
| Occupation | Employed | 18 (32.1) | 72 (45.0) | χ2 = 5.893 | 0.053 |
| Retired | 28 (50.0) | 68 (42.5) | |||
| Unemployed | 10 (17.9) | 20 (12.5) | |||
| Lesion location | Fundus/body | 12 (21.4) | 42 (26.3) | χ2 = 0.556 | 0.456 |
| Antrum/angle | 44 (78.6) | 118 (73.8) | |||
| Lesion size (cm) | M (P25, P75) | 2.2 (1.5, 3.0) | 1.8 (1.2, 2.5) | Z = -2.867 | 0.004 |
| Pathological type | Differentiated adenocarcinoma | 48 (85.7) | 143 (89.4) | χ2 = 0.581 | 0.446 |
| Undifferentiated adenocarcinoma | 8 (14.3) | 17 (10.6) | |||
| Depth of invasion | Mucosal layer M | 38 (67.9) | 118 (73.8) | χ2 = 0.748 | 0.387 |
| Submucosal layer SM | 18 (32.1) | 42 (26.3) | |||
| Combined with ulcer | Yes | 26 (46.4) | 48 (30.0) | χ2 = 5.312 | 0.021 |
| No | 30 (53.6) | 112 (70.0) | |||
| Lymphovascular invasion | Yes | 12 (21.4) | 18 (11.3) | χ2 = 3.611 | 0.057 |
| No | 44 (78.6) | 142 (88.8) | |||
| En bloc resection | Yes | 52 (92.9) | 152 (95.0) | Fisher | 0.719 |
| No | 4 (7.1) | 8 (5.0) | |||
| Complete resection | Yes | 48 (85.7) | 144 (90.0) | χ2 = 0.753 | 0.386 |
| No | 8 (14.3) | 16 (10.0) | |||
| Past medical history | Yes | 34 (60.7) | 88 (55.0) | χ2 = 0.580 | 0.446 |
| No | 22 (39.3) | 72 (45.0) | |||
| Family tumor history | Yes | 22 (39.3) | 42 (26.3) | χ2 = 3.578 | 0.059 |
| No | 34 (60.7) | 118 (73.8) |
Preoperative Self-Rating Anxiety Scale (SAS) and Self-Rating Depression Scale (SDS) scores in the PTSD group were higher than those in the non-PTSD group (P < 0.05), while preoperative Social Support Rating Scale (SSRS) scores were lower than those in the non-PTSD group (P < 0.05). At 3 months postoperatively, SAS and SDS scores in the PTSD group remained higher than those in the non-PTSD group (P < 0.001), while SSRS scores were lower than those in the non-PTSD group (P < 0.001) (Table 2). Further analysis of each dimension of the SSRS scale showed that patients in the PTSD group scored lower than those in the non-PTSD group in all three dimensions: Objective support, subjective support, and utilization of social support, with all differences being statistically significant (P < 0.001) (Table 3).
| Scale | Time point | PTSD group (n = 56) | Non-PTSD group (n = 160) | t value | P value |
| SAS | Preoperative | 48.6 ± 8.2 | 42.3 ± 7.5 | 5.198 | < 0.001 |
| 3 months postoperative | 51.2 ± 9.4 | 38.5 ± 6.8 | 10.632 | < 0.001 | |
| SDS | Preoperative | 52.3 ± 9.6 | 45.8 ± 8.2 | 4.751 | < 0.001 |
| 3 months postoperative | 56.8 ± 10.5 | 40.2 ± 7.3 | 12.486 | < 0.001 | |
| SSRS | Preoperative | 32.4 ± 5.8 | 38.6 ± 6.2 | -6.563 | < 0.001 |
| 3 months postoperative | 28.7 ± 6.3 | 40.1 ± 5.9 | -11.982 | < 0.001 |
| Dimension | Time point | PTSD group | Non-PTSD group (n = 160) | t value | P value |
| Objective support1 | Preoperative | 7.8 ± 1.9 | 8.9 ± 2.0 | -3.565 | < 0.001 |
| 3 months postoperative | 6.9 ± 2.1 | 9.2 ± 1.9 | -7.323 | < 0.001 | |
| Subjective support2 | Preoperative | 13.5 ± 2.6 | 16.2 ± 2.8 | -6.304 | < 0.001 |
| 3 months postoperative | 11.8 ± 2.8 | 17.3 ± 2.7 | -12.739 | < 0.001 | |
| Utilization of social support3 | Preoperative | 11.1 ± 2.1 | 13.5 ± 2.2 | -7.094 | < 0.001 |
| 3 months postoperative | 10.0 ± 2.3 | 13.6 ± 2.1 | -10.489 | < 0.001 |
The total PCL-C scale score for the 56 patients in the PTSD group was (45.6 ± 6.8) points, of which the re-experiencing symptoms dimension score was (14.2 ± 3.1) points, the avoidance/numbing symptoms dimension score was (18.5 ± 3.6) points, and the hyperarousal symptoms dimension score was (12.9 ± 2.8) points. The avoidance/numbing symptoms dimension had the highest score, accounting for 40.5% of the total score.
Variables with P < 0.10 in univariate analysis were included in multivariate Logistic regression analysis, including age, education level, marital status, occupation, lesion size, combined with ulcer, lymphovascular invasion, family tumor history, preoperative SAS score, preoperative SDS score, and preoperative SSRS score. Multicollinearity diagnosis showed that VIF values for all variables were < 3, indicating no collinearity problem. Although the preoperative SAS score showed significance in univariate analysis (P < 0.001), it was eliminated during the stepwise backward selection process due to high correlation with SDS score (r = 0.72) and weaker independent predictive efficacy (P = 0.156 at elimination). Using stepwise backward elimination for multivariate Logistic regression analysis, results showed that age, unmarried/divorced/widowed status, lesion size, combined with ulcer, preoperative SDS score, and preoperative SSRS score were independent risk factors for PTSD occurrence in patients after ESD for early gastric cancer (P < 0.05) (Table 4).
| Variable | B | SE | Wald χ2 | P value | OR | 95%CI |
| Age (per 1-year increase) | 0.058 | 0.023 | 6.281 | 0.012 | 1.06 | 1.013-1.109 |
| Marital status (unmarried/divorced/widowed vs married) | 1.124 | 0.456 | 6.079 | 0.014 | 3.077 | 1.259-7.516 |
| Lesion size (per 1-cm increase) | 0.485 | 0.186 | 6.796 | 0.009 | 1.624 | 1.129-2.336 |
| Combined with ulcer (yes vs no) | 0.892 | 0.382 | 5.455 | 0.02 | 2.44 | 1.154-5.161 |
| Preoperative SDS score (per 1-point increase) | 0.062 | 0.021 | 8.722 | 0.003 | 1.064 | 1.021-1.109 |
| Preoperative SSRS score (per 1-point increase) | -0.098 | 0.034 | 8.291 | 0.004 | 0.907 | 0.848-0.970 |
| Constant | -9.824 | 2.145 | 20.963 | < 0.001 | < 0.001 | - |
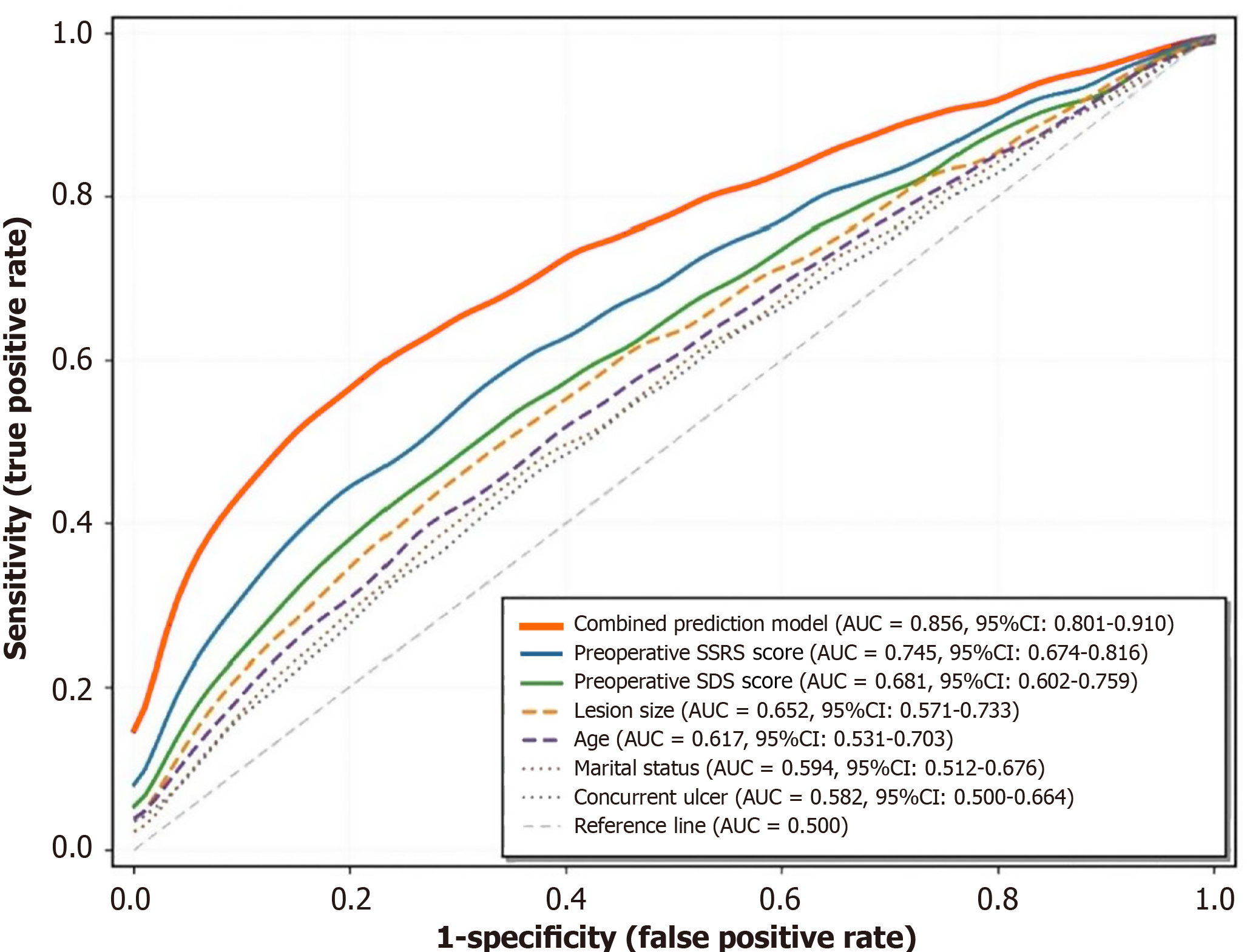
A prediction model was established using the 6 independent risk factors from multivariate Logistic regression analysis. ROC curve analysis showed that the model’s AUC for predicting PTSD occurrence in patients after ESD for early gastric cancer was 0.856 (95% confidence interval: 0.801-0.910), with a sensitivity of 78.6%, a specificity of 85.0%, and a Youden index of 0.636 (Figure 1, Table 5). The predictive efficacy of every single factor was lower than that of the combined model (P < 0.05).
| Predictive factor | AUC | 95%CI | Sensitivity (%) | Specificity (%) | Youden index | Cut-off value1 |
| Combined prediction model | 0.856 | 0.801-0.910 | 78.6 | 85 | 0.636 | Predicted probability ≥ 0.31 |
| Age | 0.617 | 0.531-0.703 | 64.3 | 60.6 | 0.249 | 62 years |
| Marital status | 0.594 | 0.512-0.676 | 25 | 88.8 | 0.138 | Unmarried/divorced/widowed |
| Lesion size | 0.652 | 0.571-0.733 | 58.9 | 68.8 | 0.277 | 2.0 cm |
| Combined with ulcer | 0.582 | 0.500-0.664 | 46.4 | 70 | 0.164 | Yes |
| Preoperative SDS score | 0.681 | 0.602-0.759 | 62.5 | 70 | 0.325 | 50 points |
| Preoperative SSRS score | 0.745 | 0.674-0.816 | 71.4 | 71.3 | 0.427 | 35 points |
Among the 56 patients in the PTSD group, 18 had PCL-C total scores ≥ 50, and 38 had scores of 38-49. The clinical PTSD group (PCL-C ≥ 50) showed statistically significant differences compared with the mild-to-moderate PTSD group (PCL-C: 38-49) in age, 3-month postoperative SAS score, SDS score, SSRS score, and proportion of combined ulcer (P < 0.05) (Table 6).
| Item | Category/unit | Clinical PTSD group | Mild-to-moderate PTSD group (n = 38) | Test statistic | P value |
| Gender | Male | 10 (55.6) | 23 (60.5) | χ2 = 0.137 | 0.711 |
| Female | 8 (44.4) | 15 (39.5) | |||
| Age (years) | 64.8 ± 7.3 | 59.6 ± 8.5 | t = 2.239 | 0.029 | |
| 3-month postoperative SAS score (points) | 58.3 ± 8.6 | 48.2 ± 7.9 | t = 4.392 | < 0.001 | |
| 3-month postoperative SDS score (points) | 64.7 ± 9.2 | 53.5 ± 8.4 | t = 4.635 | < 0.001 | |
| 3-month postoperative SSRS score (points) | 24.1 ± 5.2 | 30.8 ± 5.7 | t = -4.242 | < 0.001 | |
| Combined with ulcer | Yes | 11 (61.1) | 15 (39.5) | χ2 = 2.546 | 0.111 |
| No | 7 (38.9) | 23 (60.5) |
This study found that the incidence of PTSD in patients after ESD for early gastric cancer was 25.9%, which is basically consistent with previous studies on cancer-related PTSD[7]. The overall prevalence of PTSD in cancer patients is 22.1%, while another study on gastrointestinal tumor patients reported a PTSD incidence of 18%-32%[8]. The results of this study fall within this range, suggesting that cancer diagnosis and treatment as a traumatic source can indeed lead to stress disorder symptoms in a considerable proportion of patients. It is noteworthy that despite ESD being a minimally invasive treatment method, its PTSD incidence should not be overlooked, which may be related to the psychological impact of the cancer diagnosis itself, concerns about disease recurrence and metastasis, and postoperative lifestyle changes[9]. This study explicitly distinguishes between diagnostic trauma and procedural trauma in the context of PTSD development. The psychological impact of the cancer diagnosis itself, representing an existential threat, likely serves as the primary traumatic stressor, independent of the procedural invasiveness of ESD. This aligns with the stress-diathesis model of PTSD, where the perceived threat to one’s existence constitutes the predominant trigger for post-traumatic stress res
In this study, clinical PTSD patients with PCL-C ≥ 50 accounted for 8.3%. Although this proportion is lower than the screening positive rate, it still suggests that a certain proportion of patients require professional psychological intervention. Studies have pointed out that PTSD patients reaching the clinical diagnosis level usually have more severe anxiety and depression symptoms and lower quality of life; without timely intervention, this may affect treatment compliance and prognosis[10]. The subgroup analysis of this study also confirmed this, showing that patients in the clinical PTSD group had significantly higher postoperative anxiety and depression scores than the mild-to-moderate PTSD group, with lower social support levels, suggesting that these high-risk patients need focused attention.
This study found that age is an independent risk factor for PTSD occurrence, with the risk of PTSD increasing by 6.0% for each additional year of age. This differs somewhat from previous research results; some studies believe that younger patients are more prone to PTSD[11], while other studies support a higher risk in elderly patients[12]. The results of this study lean more toward the latter, with possible reasons including: Elderly patients have relatively weaker cognitive abilities and psychological coping abilities regarding disease, and are more prone to fear of death and worry about family members; elderly patients’ physical functions decline, postoperative recovery is slower, which may increase psychological burden[13]. Additionally, elderly patients have reduced social activities, which may lead to insufficient social support, further increasing PTSD risk.
Marital status is also an important influencing factor. This study showed that the risk of PTSD in unmarried/divorced/widowed patients was 3.077 times that of married patients. Marital relationships are considered one of the most im
Lesion size, as an important indicator of tumor burden, showed in this study that the risk of PTSD increased by 62.4% for each 1-cm increase in lesion size. Larger lesions usually mean relatively later disease stage, increased treatment dif
The risk of PTSD in patients with a combined ulcer was 2.440 times that of patients without an ulcer. The presence of ulcers not only increases the technical difficulty of ESD surgery and the risk of complications, such as perforation and bleeding[18], but may also prolong postoperative recovery time. Patients may be informed preoperatively that ulcers increase surgical risk, and this information itself may trigger anxiety and worry. Additionally, studies have pointed out that patients with combined ulcers are more prone to postoperative symptoms such as abdominal pain and bleeding, and these physical discomforts may intensify psychological stress reactions[19]. Ulcer healing requires a longer time, and patients need stricter dietary control and medication treatment, with quality of life being more greatly affected, poten
Preoperative depression level is a strong predictor of PTSD occurrence, with the risk of PTSD increasing by 6.4% for each 1-point increase in preoperative SDS score. This finding emphasizes the importance of preoperative psychological assessment. There is a complex bidirectional relationship between depressive symptoms and PTSD; depression may reduce an individual’s psychological coping ability and stress resistance, making them more susceptible to developing PTSD after traumatic events[20]. At the same time, depressed patients often have negative cognitive biases, tending toward catastrophic thinking and pessimistic expectations, and this cognitive pattern may amplify the negative impact of cancer diagnosis and treatment[21]. The high correlation between preoperative SAS scores and SDS scores (r = 0.72) indicates substantial overlap between anxiety and depressive symptoms, which is clinically expected in cancer patients. In our stepwise multivariate analysis, SDS was retained while SAS was excluded, suggesting that depressive symptoms may have stronger independent predictive validity for PTSD in this context. This finding aligns with existing literature indicating that depression, as a core feature of negative affectivity, exerts more persistent and profound effects on post-traumatic stress responses. However, the high correlation precludes the complete separation of anxiety and depression effects. Future studies employing factor analysis or structural equation modeling may better elucidate the distinct contributions of these constructs to PTSD development.
Social support plays a protective role in the occurrence and development of PTSD. This study showed that the risk of PTSD decreased by 9.3% for each 1-point increase in preoperative SSRS score. Social support is an important resource for individuals to cope with stressful events, including emotional support, informational support, and practical help[22]. Good social support can help patients establish positive coping methods, reduce psychological pressure, and enhance confidence in overcoming disease. Further analysis in this study found that patients in the PTSD group scored significantly lower than the non-PTSD group in all three dimensions: Objective support, subjective support, and utilization of social support, suggesting that insufficient social support is multidimensional. Studies have shown that the subjective support perceived by cancer patients has a greater impact on mental health than objective support, because subjective support reflects an individual’s feeling of being cared for and valued[23]. Therefore, clinical work should not only encourage family members to provide practical help but also emphasize emotional support and psychological companionship, helping patients establish positive support networks.
This study analyzed the dimension scores of the PCL-C scale for patients in the PTSD group, and results showed that avoidance/numbing symptoms scored highest, accounting for 40.5% of the total score. This finding is consistent with the characteristics of cancer-related PTSD, where patients often adopt avoidance strategies to cope with cancer-related traumatic memories and negative emotions, such as avoiding hospital environments, avoiding discussions about the disease, and emotional numbing[24]. However, excessive avoidance may hinder patients’ correct understanding of the disease and positive coping, affecting treatment compliance and follow-up compliance. Therefore, psychological intervention should particularly focus on helping patients gradually face traumatic experiences and establish adaptive coping methods.
The prediction model established based on 6 independent risk factors in this study showed good predictive efficacy, with an AUC of 0.856, sensitivity of 78.6%, and specificity of 85.0%. The advantage of this model is that all included indicators are clinically easily obtainable, objective indicators, facilitating promotion and application in clinical practice. Through this model, high-risk PTSD patients can be identified preoperatively, providing scientific evidence for implementing early psychological screening and preventive intervention[25]. ROC curve analysis showed that the predictive efficacy of the combined prediction model was significantly superior to any single factor, with an AUC of 0.856, while the AUC range for single factors was 0.582-0.745. This suggests that PTSD occurrence is the result of multiple factors acting together, and the predictive value of single factors is limited. Among them, the independent predictive efficacy of preoperative SSRS score was relatively good (AUC = 0.745), further confirming the important role of social support in PTSD prevention. In clinical practice, multidimensional assessment methods should be adopted, comprehensively considering patients’ demographic characteristics, disease characteristics, and psychosocial factors to improve the accuracy of PTSD prediction[26].
Based on the results of this study, it is recommended to establish a three-level prevention system during the perioperative period of ESD for early gastric cancer: For primary prevention, comprehensive psychological assessment should be conducted preoperatively for all patients to identify high-risk populations; patients who are older, living alone, have preoperative depressive symptoms, and insufficient social support should be given focused attention[27]. For secondary prevention, early psychological intervention should be implemented for screened high-risk patients, including cognitive behavioral therapy, relaxation training, mindfulness therapy, etc., to help patients establish positive coping methods. For tertiary prevention, patients who have already developed PTSD symptoms should be referred to psychological specialists in a timely manner for standardized treatment, including psychotherapy and pharmacotherapy when necessary[28]. Additionally, family education and the establishment of social support networks should be emphasized. Medical staff should guide family members on how to provide effective emotional support and practical help, encourage patients to participate in cancer rehabilitation groups or support groups, and reduce psychological burden through peer support. For patients living alone or lacking family support, consideration should be given to introducing social workers or volunteer services to provide continuous care and assistance[29].
Several cultural factors may influence PTSD prevalence and expression in Chinese cancer patients: (1) Cancer stigma remains prevalent in Chinese culture, potentially intensifying psychological distress; (2) “Protective disclosure” practices, where families may withhold or filter information about diagnosis and prognosis, can affect information processing and coping mechanisms; (3) Cultural stoicism and reluctance to express emotional distress may lead to symptom underreporting, suggesting that actual PTSD prevalence could be higher than detected; and (4) The central role of social support in Chinese society, consistent with the strong protective effect of SSRS in our model, underscores the importance of family-centered care approaches in this population.
Several limitations warrant consideration: (1) The inherent constraints of the retrospective design preclude causal inference and may introduce recall bias in psychological assessments, though we acknowledge that routine preoperative assessments minimize this concern; (2) Single-center recruitment at a tertiary medical center may limit generalizability to community hospitals or different healthcare settings; (3) Single-timepoint PTSD assessment at 3 months post-procedure fails to capture symptom trajectory and may miss early-onset or delayed-onset PTSD cases; and (4) Absence of baseline pre-operative PTSD assessment precludes exclusion of pre-existing trauma effects.
The prediction model may facilitate identification of high-risk patients and provide preliminary evidence for pre-operative psychological screening, rather than representing immediate clinical utility. We explicitly recommend prospective multicenter validation studies and interventional trials to confirm model performance and assess the actual impact of early psychological intervention on patient outcomes before widespread clinical implementation.
| 1. | Lin JL, Lin JX, Lin GT, Huang CM, Zheng CH, Xie JW, Wang JB, Lu J, Chen QY, Li P. Global incidence and mortality trends of gastric cancer and predicted mortality of gastric cancer by 2035. BMC Public Health. 2024;24:1763. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 88] [Cited by in RCA: 83] [Article Influence: 41.5] [Reference Citation Analysis (0)] |
| 2. | Kim GH. Endoscopic submucosal dissection for early gastric cancer: It is time to consider the quality of its outcomes. World J Gastroenterol. 2023;29:5800-5803. [PubMed] [DOI] [Full Text] |
| 3. | Bryant RA. Post-traumatic stress disorder: a state-of-the-art review of evidence and challenges. World Psychiatry. 2019;18:259-269. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 162] [Cited by in RCA: 301] [Article Influence: 43.0] [Reference Citation Analysis (0)] |
| 4. | Anderson D, Jones V. Psychological interventions for cancer-related post-traumatic stress disorder: narrative review. BJPsych Bull. 2024;48:100-109. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 5. | Sabah A, Hammadi F, Lee CH, Aljaberi MA, van Dijk M, Lin CY, Griffiths MD. Post-Traumatic Stress Disorder (PTSD) Among Algerian Cancer Patients: Validity of the Arabic DSM-5 PTSD Checklist (PCL-5) and Associated Factors. Psychooncology. 2025;34:e70109. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 5] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 6. | Bognár SA, Teutsch B, Bunduc S, Veres DS, Szabó B, Fogarasi B, Zahariev OJ, Vörhendi N, Almog O, Hadani Y, Gergő D, Mihály E, Erőss B, Bunduc S, Márta K, Hegyi P. Psychological intervention improves quality of life in patients with early-stage cancer: a systematic review and meta-analysis of randomized clinical trials. Sci Rep. 2024;14:13233. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 31] [Article Influence: 15.5] [Reference Citation Analysis (0)] |
| 7. | Zhang L, Liu X, Tong F, Zhou R, Peng W, Yang H, Liu F, Yang D, Huang X, Wen M, Jiang L, Yi L. The prevalence of psychological disorders among cancer patients during the COVID-19 pandemic: A meta-analysis. Psychooncology. 2022;31:1972-1987. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 26] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 8. | van de Wal D, den Hollander D, Desar IME, Gelderblom H, Oosten AW, Reyners AKL, Steeghs N, Husson O, van der Graaf WTA. Fear, anxiety and depression in gastrointestinal stromal tumor (GIST) patients in the Netherlands: Data from a cross-sectional multicenter study. Int J Clin Health Psychol. 2024;24:100434. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 9. | Li Y, Xiao T, Liao H, Qu H, Ren P, Chen X. Fear of progression, loneliness, and hope in patients with gastrointestinal cancer: a cross-sectional relational study. Front Psychol. 2023;14:1279561. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 10. | Al Jowf GI, Ahmed ZT, Reijnders RA, de Nijs L, Eijssen LMT. To Predict, Prevent, and Manage Post-Traumatic Stress Disorder (PTSD): A Review of Pathophysiology, Treatment, and Biomarkers. Int J Mol Sci. 2023;24:5238. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 57] [Reference Citation Analysis (0)] |
| 11. | Al-Saadi LS, Chan MF, Al-Azri M. Prevalence of Anxiety, Depression, and Post-Traumatic Stress Disorder among Children and Adolescents with Cancer: A Systematic Review and Meta-Analysis. J Pediatr Hematol Oncol Nurs. 2022;39:114-131. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 18] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 12. | Lee ARYB, Leong I, Lau G, Tan AW, Ho RCM, Ho CSH, Chen MZ. Depression and anxiety in older adults with cancer: Systematic review and meta-summary of risk, protective and exacerbating factors. Gen Hosp Psychiatry. 2023;81:32-42. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 39] [Article Influence: 13.0] [Reference Citation Analysis (0)] |
| 13. | Kadambi S, Loh KP, Dunne R, Magnuson A, Maggiore R, Zittel J, Flannery M, Inglis J, Gilmore N, Mohamed M, Ramsdale E, Mohile S. Older adults with cancer and their caregivers - current landscape and future directions for clinical care. Nat Rev Clin Oncol. 2020;17:742-755. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 116] [Cited by in RCA: 112] [Article Influence: 18.7] [Reference Citation Analysis (0)] |
| 14. | Krajc K, Miroševič Š, Sajovic J, Klemenc Ketiš Z, Spiegel D, Drevenšek G, Drevenšek M. Marital status and survival in cancer patients: A systematic review and meta-analysis. Cancer Med. 2023;12:1685-1708. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 32] [Cited by in RCA: 92] [Article Influence: 30.7] [Reference Citation Analysis (0)] |
| 15. | Wheldon CW, Shahsavar Y, Choudhury A, McCormick BP, Albertorio-Díaz JR. Loneliness among adult cancer survivors in the United States: prevalence and correlates. Sci Rep. 2025;15:3914. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 12] [Article Influence: 12.0] [Reference Citation Analysis (0)] |
| 16. | Yang Y, Qian X, Tang X, Shen C, Zhou Y, Pan X, Li Y. The links between symptom burden, illness perception, psychological resilience, social support, coping modes, and cancer-related worry in Chinese early-stage lung cancer patients after surgery: a cross-sectional study. BMC Psychol. 2024;12:463. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 19] [Reference Citation Analysis (0)] |
| 17. | Antoni MH, Moreno PI, Penedo FJ. Stress Management Interventions to Facilitate Psychological and Physiological Adaptation and Optimal Health Outcomes in Cancer Patients and Survivors. Annu Rev Psychol. 2023;74:423-455. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 97] [Cited by in RCA: 73] [Article Influence: 24.3] [Reference Citation Analysis (4)] |
| 18. | Chen DY, Chen HD, Lv XD, Huang Z, Jiang D, Li Y, Han B, Han LC, Xu XF, Li SQ, Lin GF, Huang ZX, Lin JN, Lv XP. Outcome and risk factors of ulcer healing after gastric endoscopic submucosal dissection: A systematic review and meta-analysis. World J Gastrointest Surg. 2024;16:3568-3577. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 19. | Liu Q, Li L, Wei J, Xie Y. Correlation and influencing factors of preoperative anxiety, postoperative pain, and delirium in elderly patients undergoing gastrointestinal cancer surgery. BMC Anesthesiol. 2023;23:78. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 32] [Reference Citation Analysis (0)] |
| 20. | Zhang C, Wang J, He Y, Wang K, Wang C, Zhang L, Wu X, Liang S, Wu X, Wei Y, Zhang M, Wang W. Depression impact on PTSD in Cancer patients through serial mediation of hope and perceived social support. Sci Rep. 2025;15:24727. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 21. | Quan L, Wang X, Lu W, Zhao X, Sun J, Sang Q. The relationship between fear of recurrence and depression in patients with cancer: The role of invasive rumination and catastrophizing. Front Psychiatry. 2022;13:920315. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 14] [Reference Citation Analysis (0)] |
| 22. | Chirico A, Palombi T, Alivernini F, Lucidi F, Merluzzi TV. Emotional Distress Symptoms, Coping Efficacy, and Social Support: A Network Analysis of Distress and Resources in Persons With Cancer. Ann Behav Med. 2024;58:679-691. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 9] [Reference Citation Analysis (0)] |
| 23. | Brajković L, Milat-Panža K, Kopilaš V. Subjective Well-Being in Cancer Patients: The Roles of Social Support, Purpose in Life, Resilience, and Informativeness. Healthcare (Basel). 2023;11:3181. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 24. | Malgaroli M, Szuhany KL, Riley G, Miron CD, Park JH, Rosenthal J, Chachoua A, Meyers M, Simon NM. Heterogeneity of posttraumatic stress, depression, and fear of cancer recurrence in breast cancer survivors: a latent class analysis. J Cancer Surviv. 2023;17:1510-1521. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 13] [Reference Citation Analysis (0)] |
| 25. | Yang J, Jiang W. A meta-analysis of the association between post-traumatic stress disorder and cancer risk. Front Psychiatry. 2023;14:1281606. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 26. | Öztürk FÖ, Gür GC. The Impact of Core Belief Disruption on PTSD Symptoms in Cancer Patients: The Mediating and Moderating Roles of Intrusion and Avoidance Behavior. Psychiatr Q. 2025;96:497-513. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 27. | Schultz KS, Linhares SM, Park EY, Godfrey EL, Dhanda U, Epstein EJ, Blake KBT, Huang Y, Zaheer H, Leeds IL. Insult to Injury: Cross-Sectional Analysis of Preoperative Psychosocial Vulnerabilities in Adult Patients Undergoing Major Elective Cancer Surgery. Cancers (Basel). 2025;17:2859. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 28. | Hobart M, Chang D, Hefting N, Davis LL. Brexpiprazole in Combination With Sertraline and as Monotherapy in Posttraumatic Stress Disorder: A Full-Factorial Randomized Clinical Trial. J Clin Psychiatry. 2025;86:24m15577. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 29. | Thomas TH, Campbell G, Tan KR, Murray PJ, Loughlin K, Roberge MC, Wang Y, Lee YJ, DiLello R, Donovan HS. Integrating Family Caregivers Into Cancer Care: Implementation of Evidence-Based Caregiver Protocols Into Gynecologic Oncology Practice. JCO Oncol Pract. 2025;21:476-484. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |