Published online May 19, 2026. doi: 10.5498/wjp.v16.i5.116043
Revised: December 18, 2025
Accepted: February 10, 2026
Published online: May 19, 2026
Processing time: 159 Days and 0.5 Hours
Depression in children and adolescents has become a serious public health pro
To compare the short-term efficacy of cognitive behavioral therapy (CBT) plus sertraline vs pharmacological treatment alone (sertraline) in adolescents with de
A single-center randomized controlled study was conducted, and a total of 100 adolescent patients with depression were included who met the diagnostic criteria based on the inclusion and exclusion criteria. The patients were randomly divided into two groups: 50 patients in the study group, who received a comprehensive intervention model (CBT treatment + sertraline treatment + ecological intervention), and 50 patients in the control group, who received only systematic sertraline monotherapy. The Children’s Depression Inventory (CDI) was used to evaluate short-term efficacy in both groups. The Adverse Reaction Symptom Scale (TESS) was used to evaluate treatment safety.
The results showed that there was no significant difference in CDI scores between the two groups before treatment (15.9 ± 6.5 vs 13.6 ± 7.3, P > 0.05). After 3 months of treatment, the median CDI score in the study group was 5 points (interquartile range, 3 points) and in the control group it was 7.5 points (interquartile range, 8 points), with a significant difference between the two groups (Z = -3.052, P < 0.05). After 3 months of treatment, the median TESS score in the study group was 6 points (interquartile range, 3 points) and the median TESS score in the control group was 5 points (interquartile range, 5 points). There was no statistically significant difference between the two groups (P > 0.05); the incidence of various types of side effects (such as extrapyramidal reactions and cholinergic symptoms) was similar between the two groups (all P > 0.05). The main adverse events were mild muscle stiffness (6%) and dry mouth (6%-8%). No serious adverse reactions occurred.
The comprehensive treatment model of CBT combined with sertraline and ecological intervention was significantly better than drug therapy alone in improving depression in children and adolescents in the short term, and de
Core Tip: This study showed that cognitive behavioral therapy based on ecological intervention combined with sertraline had better short-term efficacy than sertraline alone in the treatment of adolescent depression, and the safety profile was comparable. These results provide an empirical basis for the clinical selection of high-efficiency and low-risk adolescent depression treatment regimens. In the future, it is necessary to further verify the long-term effectiveness of the intervention, and explore comprehensive intervention strategies for comorbid factors such as sleep management and metabolic health.
- Citation: Yang LK, Ye Y, Cheng LL, Li X, Ye ZX, Zhu YH, Lin ZY, Chen XL. Short-term efficacy of cognitive behavioral therapy plus sertraline vs sertraline monotherapy for adolescent depression: A randomized controlled study. World J Psychiatry 2026; 16(5): 116043
- URL: https://www.wjgnet.com/2220-3206/full/v16/i5/116043.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i5.116043
Depression is a widespread and increasingly severe mental health issue affecting the normal growth and development of adolescents[1]. In recent years, due to increasing social pressure and lifestyle changes, the incidence of adolescent depression has significantly increased[2]. Research indicates that adolescence is a high-risk period for depression, and the situation has worsened, particularly since the coronavirus disease 2019 pandemic[3]. Depression is a leading cause of global disease burden and ranks as the second most common mental disorder, after ischemic heart disease[4]. As the demands of modern life escalate, there has been an annual increase in psychiatric conditions following depressive disorders[5]. Over the past ten years, depressive symptoms have increased across different adolescent groups[6]. The prevalence of major depressive disorder in adolescents is estimated to be approximately 7.1%, making it a global public health issue[7]. The causes of depression are complex and varied, and include genetic, environmental, and biological factors. Adolescents with a family history of depression have a fourfold increased risk of developing this condition[8]. Furthermore, adolescents face numerous stressors across multiple systems, including family, school, and social media, which can impair cognition, emotional well-being, and academic performance[8].
Currently, the treatment of depression mainly relies on medication and psychological interventions, which are frequently combined in clinical practice to achieve better efficacy. Citalopram (sertraline) is a commonly used selective serotonin reuptake inhibitor (SSRI) that has shown significant efficacy in the treatment of depression. Research has indicated that combining citalopram with other treatment methods can enhance therapeutic outcomes. For instance, one study found that the combination of citalopram and insight therapy based on psychological hotlines was more effective than citalopram alone in reducing depressive and anxiety symptoms in adolescents with depression[9]. In addition, the efficacy of drug therapy is significantly affected by individual differences. The efficacy and safety of sertraline have been specifically evaluated in adolescents. A recent network meta-analysis confirmed the acceptability and comparative efficacy of sertraline among the SSRIs for the acute treatment of depression in children and adolescents[10]. However, optimal treatment often requires combination strategies, as evidenced by studies showing that combining SSRIs with psychotherapy yields superior outcomes compared with monotherapy in this age group[11]. However, the translation of adult treatment paradigms to adolescence requires caution. Although some antidepressants are effective, concerns reg
At the same time, cognitive behavioral therapy (CBT) is a well-established evidence-based psychological intervention technique that is effective in improving cognitive biases and mood disorders in adolescents and improving their ability to cope with negative emotions[13]. In terms of psychological interventions, cognitive-behavioral and interpersonal therapies have shown significant short-term effects in alleviating acute depressive symptoms, although the magnitude of these effects is moderate[14]. Furthermore, social support has been reported to mitigate the impact of negative life events on depressive symptoms, making it crucial to enhance social support systems in schools and communities[15].
In summary, there are still few systematic studies that combine CBT, medication, and ecological interventions. Therefore, this study aims to explore a comprehensive intervention model, including CBT, sertraline and ecological intervention, to evaluate its short-term efficacy in children and adolescents with depression, in order to provide a scien
A total of 100 adolescent patients with depression who met the diagnostic criteria were included in a single-center randomized controlled study following the inclusion criteria. The patients were randomly divided into two groups: 50 patients in the study group, and a comprehensive intervention model (CBT treatment + sertraline treatment + ecological intervention) was implemented, in which 50 patients received only systematic sertraline monotherapy.
The sample size was estimated based on the expected difference in the primary outcome [change in Children’s Depression Inventory (CDI) score] observed in a pilot study at our center (n = 30), which showed a large effect size (Cohen’s d = 0.91) between the combined intervention and medication-only groups. With a two-sided α of 0.05 and power of 0.80, the initial calculation indicated a requirement of 20 participants per group (total n = 40). To ensure robustness and account for a potential attrition rate of 20%, the target sample size was increased to 100 participants (50 per group).
Inclusion criteria: (1) Age between 7 years and 18 years; (2) Gender is not limited; (3) First-time, untreated patients who meet the diagnostic criteria for depressive disorders in the American Diagnostic Statistical Manual of Mental Disorders, 4th edition; (4) The applicant and his/her parents have no obvious difficulties in understanding and expressing them
Exclusion criteria: (1) Presence of other central nervous system or psychiatric disorders, severe physical disorders, history of substance or drug dependence, and mental retardation; (2) Allergy to sertraline; and (3) Those who are using or must use drugs or health products that may affect the 5-hydroxytryptamine system during the study.
The study was approved by the Ethics Committee of Wenzhou Seventh People’s Hospital and was carried out in accordance with the Declaration of Helsinki and its subsequent amendments. Subjects and their guardians provided written informed consent.
Control group: Treated with sertraline, an SSRI antidepressant. In this project, sertraline was procured using Pfizer (trade name: Zoloft, 50 mg/tablet, 14 tablets/box. Oral administration is adopted, with a gradual titration of small doses, starting from 12.5 mg/day in normal-weight children aged 6-12 years, and gradually increasing to 25-50 mg/day within two weeks according to the patient’s response to the drug; normal-weight adolescents aged 12-18 years began at 25 mg/day and gradually increased to 50 mg/day over two weeks depending on the patient’s response to the drug, after which the dose could continue to be adjusted according to efficacy. The maximum dose was not to exceed 200 mg/day.
Study group: A comprehensive treatment group using drug treatment + psychotherapy, i.e., sertraline + CBT treatment, while integrating the concept of ecological intervention.
The ecological intervention was implemented as a structured multilevel supportive protocol encompassing individual, microsystem, and macrosystem components. To ensure consistency and fidelity, all interventions were delivered by a trained multidisciplinary team (including a child psychiatrist, clinical psychologist, school liaison officer, and family counselor) following a detailed manualized intervention protocol. This protocol specified the objectives, content, duration, frequency, and intensity of each intervention. Fidelity was monitored through: (1) Weekly group supervision sessions during which case progress and protocol adherence were reviewed; (2) Completion of standardized checklists for each session by the interveners; and (3) Random audio recording and review of 10% of the sessions using a fidelity rating scale (adapted from the Treatment Fidelity Checklist for Complex Interventions).
For individuals, the interventions included the following: (1) Structured school engagement plans: Individualized academic support sessions (two sessions/week, 45 minutes each) facilitated by a school liaison officer in collaboration with teachers; (2) Nutritional guidance: Two initial consultations (60 minutes each) with a registered dietitian to develop personalized meal plans, followed by brief, biweekly check-ins (15 minutes) for 3 months; (3) Sleep hygiene education: A psychoeducation session (60 minutes) followed by daily sleep diary monitoring for 4 weeks, with a weekly review (15 minutes) by a clinical psychologist; and (4) Supervised physical activity: Group exercise sessions (e.g., aerobic games and yoga) held twice weekly for 60 minutes, led by a certified fitness instructor.
For the micro-system: (1) Family support: Monthly family therapy sessions (90 minutes each) focusing on communication skills and conflict resolution conducted by the family counselor; (2) School-based support: One teacher training workshop (three hours) on recognizing depressive symptoms, followed by the implementation of monthly 45-minute student-led art or game sessions in the classroom to foster expression and peer connections; and (3) Community resource linkage: Assessment of needs and connection to at least one local youth center or peer support group, with follow-up contact after one month to assess engagement.
For the macrosystem: (1) Sociocultural value assessment: Semi-structured interviews (approximately 60 minutes) were conducted separately with adolescents and parents at baseline to identify stressors related to academic pace, living environment, and family expectations; (2) Nature exposure activities: Biweekly, therapist-supervised outings to local parks or green spaces (90-120 minutes each), incorporating mindful observation and light physical activities; and (3) Psychoeducation groups: Weekly group sessions (60 minutes each) for adolescents over 3 months, covering topics such as stress management techniques, emotion regulation strategies, and depression literacy to normalize experiences and reduce self-stigma.
Both groups received routine clinical monitoring and supportive communication from the research team to control for nonspecific attention effects. However, only the study group received the structured, multicomponent ecological intervention, as described above.
It has been pointed out that isolation from nature and disconnection from the pace of modern life can lead to stress, anxiety and depression, and that young people are particularly vulnerable to these stressors. In addition, the integrated treatment method of this project also insists on the importance of psychoeducation, believing that education can help depressed children and adolescents understand that they are not the exception, many people experience this degree of sadness and depression, etc., and the examples of specific depression cases can help them understand that depression is common in society, so as to reverse their distorted cognition and reduce the symptoms of depression to a certain extent.
Short-term efficacy[16]: The CDI is a self-report, symptom-focused scale specifically designed for adolescents and children aged 7-17 years. Comprising 27 assessment items, it systematically measures psychological and behavioral indicators, including depressed affect, anhedonia, vegetative symptoms, self-perception, and interpersonal functioning (Cronbach’s alpha coefficient = 0.82). Each item consists of three declarative statements scored on a 0-2 ordinal scale, with higher values reflecting more severe symptoms. The total score ranges from 0 to 54, with elevated scores indicating a greater depressive symptom burden. The clinical remission threshold for the CDI score is usually set at 11 points[17].
Safety[18]: Vital signs and adverse reactions were tracked post-therapy using the Treatment-Emergent Symptom Scale (TESS) (NIMH, 1973). Safety evaluations primarily focused on the occurrence, frequency, and intensity of adverse events, while also incorporating comprehensive assessment metrics, such as physical examinations, electrocardiograms, and routine laboratory tests. In case of any adverse events deemed necessary, the patients discontinued the study as required.
SPSS 21.0 software was used for data analysis. After testing for normal distribution of the data, those conforming to a normal distribution were expressed as mean ± SD. The independent samples t-test was used for comparison between groups. Non-normally distributed metrics were expressed as median (median) and interquartile range (P25-P75), and the Mann-Whitney U rank sum test was applied. The χ2 test was used to analyze count and percentage data n (%). Statistical significance was set at P < 0.05. For continuous variables assessed for between-group differences at baseline, the choice of descriptive statistics [mean ± SD or median (interquartile range)] was based on the distribution of the entire sample. The corresponding inferential test (independent samples t-test or Mann-Whitney U test) was applied consistently based on the same distributional assessment. In cases where the distribution was approximately normal, both mean ± SD and median (interquartile range) were provided for a comprehensive description, but the t-test was used for hypothesis testing.
Among the 100 patients, 48.0% were male, with a median age of 12 years. There were 26 obese patients, accounting for 26.0%. The median sleep time was 365.2 ± 64.4 minutes, and the rest time was 441.0 ± 56.5 minutes. The results are summarized in Table 1.
| Variables | All (n = 100) |
| Age, years | 12 (10.25,14) |
| Sex | |
| Men | 48 (48.0) |
| Women | 52 (52.0) |
| Obesity | 26 (26.0) |
| Sleep duration, minute, mean ± SD | 365.2 ± 64.4 |
| Time in bed, minute, mean ± SD | 441.0 ± 56.5 |
Among the 50 patients included in the study group, 46.0% were male, with a median age of 12.5 years, and 15 were obese patients, accounting for 30.0%, with a sleep duration of 363.8 ± 68.5 minutes, bed rest time 442.6 ± 56.3 minutes. Among the 50 patients included in the control group, 25.0% were male, with a median age of 11 years, and 11 were obese, accounting for 22.0%, with a sleep duration of 366.5 ± 60.7 minutes, bed rest time 439.3 ± 56.7 minutes. There was no significant difference in baseline characteristics between the two groups (P > 0.05), as shown in Table 2.
| Variables | Study group (n = 50) | Control group (n = 50) | P value |
| Age, years | 12.6 ± 2.3 | 11 (4) | 0.171 |
| 12.5 (11, 14) | |||
| Sex | 0.689 | ||
| Men | 23 (46.0) | 25 (50.0) | |
| Women | 27 (54.0) | 25 (50.0) | |
| Obesity | 15 (30.0) | 11 (22.0) | 0.197 |
| Sleep duration, minute, mean ± SD | 363.8 ± 68.5 | 366.5 ± 60.7 | 0.524 |
| Time in bed, minute, mean ± SD | 442.6 ± 56.3 | 439.3 ± 56.7 | 0.421 |
The median daily maintenance dose of sertraline in the study group was 50.0 mg (interquartile range: 25.0 mg), with a mean dose of 58.5 ± 32.1 mg. In the control group, the median daily maintenance dose was 50.0 mg (interquartile range: 37.5 mg), with a mean dose of 62.0 ± 35.6 mg. There was no statistically significant difference in the maintenance doses between the two groups (Z = -0.521, P = 0.602).
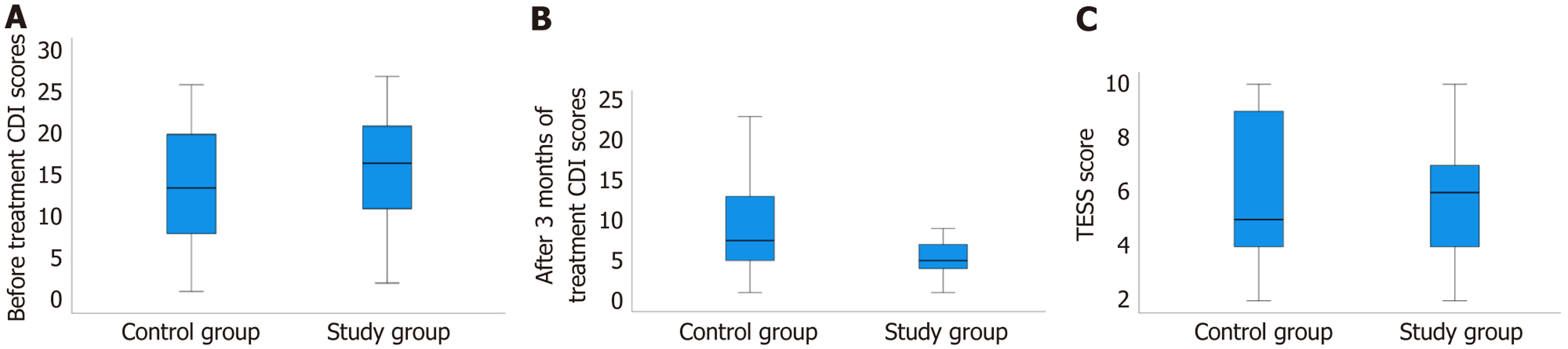
Before treatment, the CDI scores of the study group were 15.9 ± 6.5 and the control group were 13.6 ± 7.3, and there was no significant difference between the two groups (P > 0.05), as shown in Figure 1A. After 3 months of treatment, the median CDI score in the study group was 5 (4, 7.25), and that in the control group was 7.5 (5, 13.25), with a significant difference between the two groups (Z = -3.052, P < 0.05). as shown in Figure 1B.
After 3 months of treatment, the median TESS score in the study group was 6 (4, 7), and the median TESS score in the control group was 5 (4, 9) (Figure 1C). There was no statistically significant difference between the two groups (P > 0.05). There was also no significant difference in the frequency of side effects between the two groups (P > 0.05), as shown in Table 3.
| Variables | Study group (n = 50) | Control group (n = 50) | P value |
| Extrapyramidal side effects | 0.743 | ||
| Muscle stiffness | 3 (6) | 3 (6) | |
| Tremor | 1 (2) | 2 (4) | |
| Twisting movement | 1 (2) | 1 (2) | |
| Immobility | 2 (4) | 1 (2) | |
| Cholinergic side effects | 0.239 | ||
| Dry mouth | 3 (6) | 4 (8) | |
| Blurred vision | 5 (10) | 5 (10) | |
| Stuffy nose | 4 (8) | 3 (6) | |
| Salivation | 3 (6) | 4 (8) | |
| Constipation | 4 (8) | 3 (6) | |
In recent years, methods for treating depression have continuously evolved, particularly in the treatment of adolescent depression. Traditionally, medication has been the primary approach, with second-generation antidepressants, such as SSRIs and norepinephrine reuptake inhibitors, being widely used in clinical settings[19]. However, the effectiveness and safety of these medications in adolescents have been subjects of debate, especially regarding the potentially increased risk of suicide associated with antidepressants[20]. The role of psychotherapy in the treatment of depression has gained considerable attention. CBT and Interpersonal Psychotherapy are both effective interventions for depression[21]. Research indicates that combining psychotherapy with medication can enhance treatment outcomes, particularly in patients with severe depression[22]. Additionally, psychotherapy has shown positive effects in improving overall mental health and life satisfaction[23].
No significant differences in age, sex ratio, obesity rate, or sleep-related indices between the study and control groups (P > 0.05), indicating that the baseline characteristics of the two groups were balanced, which excluded the interference of confounding factors in the evaluation of efficacy and ensured the reliability of the study results. After 3 months of treatment, the CDI score in the intervention group was significantly lower than that in the control group compared with the baseline, and the difference between the groups was statistically significant (P < 0.05). This result suggests that the intervention employed by the study group had significant advantages in alleviating depressive symptoms. This aligns with contemporary meta-analytic evidence demonstrating the superior efficacy of combined CBT and SSRI therapy over either treatment alone for adolescent depression[24,25] and highlights the value of integrated care models[26]. The short-term efficacy of comprehensive interventions can be explained by several synergistic mechanisms. First, by addressing contextual barriers (e.g., academic stress and family conflict) and establishing structured routines, the ecological component likely enhances overall treatment adherence, a known mediator of outcomes in adolescent depression[27]. Second, CBT directly targets maladaptive cognitive patterns, and its combination with rapid neurochemical modulation by sertraline may accelerate the correction of negative cognitive biases and behavioral activation[28]. Third, the multilevel support system (family, school, and community) provided by the ecological intervention may have bolstered perceived social support and reduced environmental stressors, thereby facilitating faster emotional recovery[13]. Future studies should directly assess these potential mediators to confirm their pathways of action.
As the core quantitative indicator of depressive symptoms in children, the clinical remission threshold of CDI score is usually set at ≤ 11 points, and the average score of the study group after treatment was below the cut-off value, indicating that most children had reached the clinical effective standard, while the control group showed only partial improvement, which may be related to the difference in intervention intensity or mechanism of action. Notably, the CDI scores of both groups of patients were below the clinical remission threshold of 11 points after treatment, suggesting that most subjects experienced a significant reduction in symptoms after three months of intervention, reaching clinically meaningful remission. The scores in the intervention group were lower than those in the control group (median, 5 vs 7.5, respectively). Although the difference was statistically significant, whether this difference represents a clear “minimal clinically important difference” still requires further assessment in conjunction with individual functional improvement. Although this study did not directly measure specific functional indicators such as academic performance or social functioning, the CDI scale itself covers multiple dimensions, including emotion, interest, and interpersonal functioning, and a reduction in scores can indirectly reflect an overall trend of functional improvement in patients. Future research should include function-specific scales (such as the Children’s Global Assessment Scale) or quality of life questionnaires to evaluate the impact of treatment on adolescents’ daily functioning more comprehensively.
The median maintenance dose of sertraline was comparable between the two groups (50.0 mg/day in both groups, P = 0.602), indicating that the observed superior efficacy in the combined treatment group was unlikely to be attributable to differences in pharmacological intensity, but rather to the additive or synergistic effects of structured CBT and ecological intervention.
There was no significant difference in the TESS score (P > 0.05) and incidence of various types of side effects (e.g., extrapyramidal reactions and cholinergic symptoms) between the two groups after treatment, indicating that the safety of the two intervention methods was comparable. Specifically, the low incidence of minor side effects such as muscle stiffness (6%) and dry mouth (6%-8%), and no serious adverse events, suggests that the intervention regimen in the study group was well tolerated, which is consistent with recent safety profiles of combined treatment approaches in adolescent depression[29,30]. These results provide evidence supporting the clinical selection of treatment regimens with better efficacy and safety.
Although the ecological intervention was designed as a multicomponent package and delivered using a standardized protocol, we acknowledge that its comprehensive nature could introduce variability. To address the reviewer’s concern regarding whether nonspecific attention rather than CBT per se contributed to the observed effects, it is important to note that both groups received regular clinical assessments and supportive communication, ensuring that attentional bias was minimized. The additional components in the study group - structured CBT, along with systematic ecological support, likely acted synergistically, which may explain the superior outcomes compared with medication alone.
This study has several limitations. First, the sample size was small (50 cases per group), the follow-up period was only 3 months, and there was a lack of long-term efficacy and recurrence rate data. Second, subgroup analyses were not performed for specific components of the intervention (e.g., type of psychotherapy, drug dose), making it difficult to identify the core response factors. Future studies are needed to isolate the specific contributions of CBT, sertraline, and each element of ecological intervention to the overall outcome. Moreover, although we implemented an ecological intervention using a structured checklist and multidisciplinary team approach, it remains a complex, multifaceted intervention without a previously validated manual. This may limit the replicability and generalizability of the results. Third, although the maintenance doses of sertraline were not significantly different between the groups, the dosing was adjusted based on the clinical response, which introduces a potential source of variability. A fixed-dose design in future trials could isolate the specific contributions of the pharmacological components more precisely. In addition, multidimensional outcomes, such as quality of life and family function, were not included, limiting the comprehensive assessment of intervention effects. Future studies need to expand the sample size, extend the follow-up period, and combine multi
This study shows that CBT based on ecological intervention combined with sertraline has better short-term efficacy than sertraline alone in the treatment of adolescent depression, and the safety profile was comparable. These results provide a basis for the clinical selection of highly efficient, low-risk treatment regimens for adolescent depression. In the future, it will be necessary to further verify the long-term effectiveness of the intervention and explore comprehensive intervention strategies for comorbid factors such as sleep management and metabolic health.
| 1. | Song X, Li Y, Wang X, Wang X, Bao Y, Zhang D, Li Z, Meng C, Wang C, Zhang X, Lyu S. Evolution of Core Symptoms of Depression Disorders Among Chinese Adolescents Across Different Grades. Depress Anxiety. 2025;2025:2309327. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 2. | Lukic I, Ivkovic S, Glavonic E, Adzic M, Mitic M. Long-lasting Depressive Behavior of Adolescent Chronically Stressed Mice is Mediated by Gut Microbiota Dysbiosis. Mol Neurobiol. 2025;62:8868-8886. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 3. | Sun Y, Liu X, Li Y, Zhi Q, Xia Y. Effectiveness of individualized rTMS under sMRI guidance in reducing depressive symptoms and suicidal ideation in adolescents with depressive disorders: an open-label study. Front Psychiatry. 2024;15:1485878. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 4. | Arfaie A, Safikhanlou S, Bakhshipour Roodsari A, Farnam A, Shafiee-Kandjani AR. Assessment of Behavioral Approach and Behavioral Inhibition Systems in Mood Disorders. Basic Clin Neurosci. 2018;9:261-268. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 9] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 5. | Zhang Q, Guo F, Fu ZW, Zhang B, Huang CG, Li Y. Timosaponin derivative YY-23 acts as a non-competitive NMDA receptor antagonist and exerts a rapid antidepressant-like effect in mice. Acta Pharmacol Sin. 2016;37:166-176. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 22] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 6. | Krokstad S, Weiss DA, Krokstad MA, Rangul V, Kvaløy K, Ingul JM, Bjerkeset O, Twenge J, Sund ER. Divergent decennial trends in mental health according to age reveal poorer mental health for young people: repeated cross-sectional population-based surveys from the HUNT Study, Norway. BMJ Open. 2022;12:e057654. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 61] [Article Influence: 15.3] [Reference Citation Analysis (0)] |
| 7. | Teng T, Shively CA, Li X, Jiang X, Neigh GN, Yin B, Zhang Y, Fan L, Xiang Y, Wang M, Liu X, Qin M, Zhou X, Xie P. Chronic unpredictable mild stress produces depressive-like behavior, hypercortisolemia, and metabolic dysfunction in adolescent cynomolgus monkeys. Transl Psychiatry. 2021;11:9. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 31] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 8. | Cyrkler M, Czerwiak KZ, Drabik A, Soroka E. A New Pandemic of the XXIst Century: The Growing Crisis of Adolescent Depression in the Digital Age. Med Sci Monit. 2024;30:e944838. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 9. | Zhang Z, He L, Dong P, Tian Y, Ai T, Wang Z, Wang H, Ma C, Mao F, Zhang L. Effect of sertraline combined with psychological hotline-based Naikan therapy in the treatment of adolescents with depressive disorder. Int J Psychiatry Med. 2025;60:517-532. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 10. | Zhou X, Teng T, Zhang Y, Del Giovane C, Furukawa TA, Weisz JR, Li X, Cuijpers P, Coghill D, Xiang Y, Hetrick SE, Leucht S, Qin M, Barth J, Ravindran AV, Yang L, Curry J, Fan L, Silva SG, Cipriani A, Xie P. Comparative efficacy and acceptability of antidepressants, psychotherapies, and their combination for acute treatment of children and adolescents with depressive disorder: a systematic review and network meta-analysis. Lancet Psychiatry. 2020;7:581-601. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 112] [Cited by in RCA: 244] [Article Influence: 40.7] [Reference Citation Analysis (0)] |
| 11. | Robin M, Surjous L, Belbèze J, Bonnardel L, Varlet M, Silva J, Lamothe J, Essadek A, Falissard B, Cohen D, Corcos M. Influence of at-risk family interactions on the course of psychiatric care in adolescence. Eur Child Adolesc Psychiatry. 2024;33:2847-2857. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 12. | Ignaszewski MJ, Waslick B. Update on Randomized Placebo-Controlled Trials in the Past Decade for Treatment of Major Depressive Disorder in Child and Adolescent Patients: A Systematic Review. J Child Adolesc Psychopharmacol. 2018;28:668-675. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 23] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 13. | Okpete UE, Byeon H. Enhancing adolescent mental health through cognitive and social support: Insights from study on depression in Chinese adolescents. World J Psychiatry. 2024;14:1779-1782. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 14. | Zielińska M, Łuszczki E, Michońska I, Dereń K. The Mediterranean Diet and the Western Diet in Adolescent Depression-Current Reports. Nutrients. 2022;14:4390. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 54] [Cited by in RCA: 43] [Article Influence: 10.8] [Reference Citation Analysis (0)] |
| 15. | Myers K, Rockhill C, Cortese S. Editorial: For Adolescents With Subthreshold Depression, Is an Ounce of Prevention Worth a Pound of Cure? J Am Acad Child Adolesc Psychiatry. 2021;60:1056-1058. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 16. | Park S, Kim BN, Park MH. The relationship between parenting attitudes, negative cognition, and the depressive symptoms according to gender in Korean adolescents. Int J Ment Health Syst. 2016;10:35. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 8] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 17. | Davis SK, Nowland R, Qualter P. The Role of Emotional Intelligence in the Maintenance of Depression Symptoms and Loneliness Among Children. Front Psychol. 2019;10:1672. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 18] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 18. | Ren Z, Wang H, Feng B, Gu C, Ma Y, Chen H, Li B, Liu L. An exploratory cross-sectional study on the impact of education on perception of stigma by Chinese patients with schizophrenia. BMC Health Serv Res. 2016;16:210. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 8] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 19. | Kovich H, Kim W, Quaste AM. Pharmacologic Treatment of Depression. Am Fam Physician. 2023;107:173-181. [PubMed] |
| 20. | Masi G. Controversies in the Pharmacotherapy of Adolescent Depression. Curr Pharm Des. 2022;28:1975-1984. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 13] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 21. | Weersing VR, Goger P, Schwartz KTG, Baca SA, Angulo F, Kado-Walton M. Evidence-Base Update of Psychosocial and Combination Treatments for Child and Adolescent Depression. J Clin Child Adolesc Psychol. 2025;54:1-51. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 5] [Article Influence: 5.0] [Reference Citation Analysis (1)] |
| 22. | Ristea S, Schenker RA, Stovicek PO, Pîrlog MC, Marinescu D. Neurobiological and pharmacological arguments for customization of cognitive behavioral psychotherapy in the treatment of major depressive disorder. Rom J Morphol Embryol. 2021;62:807-817. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 23. | Sequeira-Nazaré ER, Schmitz B. Learn to be happy-an experimental study in clinical context with depressive patients in Germany. Front Psychol. 2024;15:1426597. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 24. | Goodyer IM, Reynolds S, Barrett B, Byford S, Dubicka B, Hill J, Holland F, Kelvin R, Midgley N, Roberts C, Senior R, Target M, Widmer B, Wilkinson P, Fonagy P. Cognitive-behavioural therapy and short-term psychoanalytic psychotherapy versus brief psychosocial intervention in adolescents with unipolar major depression (IMPACT): a multicentre, pragmatic, observer-blind, randomised controlled trial. Health Technol Assess. 2017;21:1-94. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 73] [Cited by in RCA: 62] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 25. | Cuijpers P, Karyotaki E, Ciharova M, Miguel C, Noma H, Stikkelbroek Y, Weisz JR, Furukawa TA. The effects of psychological treatments of depression in children and adolescents on response, reliable change, and deterioration: a systematic review and meta-analysis. Eur Child Adolesc Psychiatry. 2023;32:177-192. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 68] [Article Influence: 22.7] [Reference Citation Analysis (0)] |
| 26. | Weersing VR, Brent DA, Rozenman MS, Gonzalez A, Jeffreys M, Dickerson JF, Lynch FL, Porta G, Iyengar S. Brief Behavioral Therapy for Pediatric Anxiety and Depression in Primary Care: A Randomized Clinical Trial. JAMA Psychiatry. 2017;74:571-578. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 65] [Cited by in RCA: 84] [Article Influence: 9.3] [Reference Citation Analysis (0)] |
| 27. | Haynes RB, Ackloo E, Sahota N, McDonald HP, Yao X. Interventions for enhancing medication adherence. Cochrane Database Syst Rev. 2008;CD000011. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 442] [Cited by in RCA: 757] [Article Influence: 42.1] [Reference Citation Analysis (0)] |
| 28. | Schwartz KTG, Kado-Walton M, Dickerson JF, Rozenman M, Brent DA, Porta G, Lynch FL, Gonzalez A, Weersing VR. Brief Behavioral Therapy for Anxiety and Depression in Pediatric Primary Care: Breadth of Intervention Impact. J Am Acad Child Adolesc Psychiatry. 2023;62:230-243. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 29. | Correll CU, Cortese S, Croatto G, Monaco F, Krinitski D, Arrondo G, Ostinelli EG, Zangani C, Fornaro M, Estradé A, Fusar-Poli P, Carvalho AF, Solmi M. Efficacy and acceptability of pharmacological, psychosocial, and brain stimulation interventions in children and adolescents with mental disorders: an umbrella review. World Psychiatry. 2021;20:244-275. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 107] [Article Influence: 21.4] [Reference Citation Analysis (0)] |
| 30. | Walter HJ, Abright AR, Bukstein OG, Diamond J, Keable H, Ripperger-Suhler J, Rockhill C. Clinical Practice Guideline for the Assessment and Treatment of Children and Adolescents With Major and Persistent Depressive Disorders. J Am Acad Child Adolesc Psychiatry. 2023;62:479-502. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 105] [Article Influence: 35.0] [Reference Citation Analysis (0)] |