Published online Apr 19, 2026. doi: 10.5498/wjp.v16.i4.115468
Revised: December 8, 2025
Accepted: January 8, 2026
Published online: April 19, 2026
Processing time: 150 Days and 0.7 Hours
Anxiety and depression are common among patients with inflammatory bowel disease (IBD), negatively affecting their quality of life and disease prognosis. Previous studies have mainly focused on univariate analyses, with limited explo
To construct a structural equation model to examine how various factors influence anxiety and depression in patients with IBD.
An observational study involving 247 patients with IBD was conducted at Changde Hospital, Xiangya School of Medicine, Central South University (The First People’s Hospital of Changde City) from March 2023 to December 2024. Data were collected using a general information questionnaire, the Hospital Anxiety and Depression Scale, the Medical Coping Modes Questionnaire (MCMQ), and the Pittsburgh Sleep Quality Index (PSQI). Spearman correlation was used to assess variable relationships, and SEM was applied to analyze factors influencing anxiety and depression.
PSQI score [11 (10-13)] and MCMQ score [44 (43-45)] were significantly correlated with Hospital Anxiety and De
Poor sleep and maladaptive coping contribute to anxiety and depression in patients with IBD. Targeted psycho
Core Tip: This study applies structural equation modeling to explore factors influencing anxiety and depression in patients with inflammatory bowel disease. It identifies sleep quality and coping modes as key factors influencing anxiety and depression in patients with inflammatory bowel disease. These findings highlight the need for tailored interventions like sleep hygiene education and cognitive-behavioral strategies, could significantly alleviate anxiety and depression, thereby improving overall mental health outcomes and quality of life in this patient population.
- Citation: Zeng Y, Yang X, Zhang XB, Liu Y, Sun J. Risk factors associated with anxiety and depression in patients with inflammatory bowel disease identified using structural equation modeling. World J Psychiatry 2026; 16(4): 115468
- URL: https://www.wjgnet.com/2220-3206/full/v16/i4/115468.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i4.115468
Inflammatory bowel disease (IBD) represents a group of non-specific inflammatory disorders of the gastrointestinal tract, mainly comprising ulcerative colitis and Crohn’s disease. Over the past three decades, the number of IBD patients in China has increased by 911000; it is projected that by 2035 annual new cases will reach 41901 and deaths 6568; thus, the population health burden and societal medical pressure will continue to rise[1,2]. The course of IBD is recurrent and protracted; patients suffer multiple symptoms such as abdominal pain, fatigue, diarrhea, bloody stools and insomnia, and require long-term maintenance therapy. This not only imposes heavy economic costs but also causes combined physical and psychological distress[3,4]. In addition, IBD patients often experience common psychological burdens (e.g., anxiety and depression), impaired quality of life and reduced social functioning[3,5]. Studies have found that anxiety and depression are frequent comorbidities in IBD, with prevalence rates twice or higher than those in the general population[3]. A meta-analysis reported pooled prevalence rates of 32.1% for anxiety and 25.2% for depression in IBD patients[6]. However, the relationship between IBD and depression/anxiety is bidirectional: The mechanisms underlying anxiety and depression are associated with higher inflammatory levels, intestinal dysbiosis and altered brain signaling in IBD patients[3,7], while depression and anxiety can in turn exacerbate IBD symptoms and worsen disease activity[7]. Moreover, patients with poor sleep quality are more prone to fatigue, anxiety and depression, further aggravating symptoms and reducing their quality of life; sleep deprivation may also impair immune function and increase the risk of IBD relapse[8]. Therefore, early identification of such patients and timely provision of appropriate psycho-emotional interventions are of great importance for improving prognosis and quality of life in IBD.
At present, research on anxiety and depression in IBD has mostly focused on single-factor or simple multifactor ana
A total of 23 variables were analyzed in this study. The sample size was calculated as 5 times to 10 times the number of variables, yielding a minimum requirement of 150 participants to 230 participants. Considering 20% of the invalid ques
Inclusion criteria: (1) Meeting diagnostic criteria for IBD; (2) Having at least a primary school education; and (3) Being capable of completing the questionnaire independently.
Exclusion criteria: (1) Presence of other psychiatric disorders (excluding anxiety or depression); (2) History of gastroin
General information of patients (13 items): Demographic and clinical data collected included sex, age, educational level, family income, marital status, parity/number of children, employment status, body-mass index, disease duration, disease classification, place of residence, type of medical insurance, and current use of biological agents.
Hospital Anxiety and Depression Scale: The Hospital Anxiety and Depression Scale (HADS) was used to assess anxiety and depressive symptoms experienced during the past month. The scale comprises two subscales - anxiety and de
Medical Coping Modes Questionnaire: The Medical Coping Modes Questionnaire (MCMQ) evaluated patients’ coping strategies toward illness. It includes three dimensions, avoidance, resignation, and confrontation, across 20 items. Each item is rated on a 4-point scale (1 to 4), with higher scores representing healthier coping strategies[11].
Pittsburgh Sleep Quality Index: The Pittsburgh Sleep Quality Index (PSQI) evaluated sleep quality among patients with IBD over the past month. It contains 19 self-rated and 5 observer-rated items. The 19th self-rated item and the 5 observer-rated items are excluded from scoring. The remaining 18 items are grouped into seven components, each scored 0 to 3, yielding a total score of 0-21. Higher scores indicate poorer sleep quality, with a total score > 7 suggestive of sleep distur
The survey was administered through an electronic questionnaire using a face-to-face interview approach. Participants who met the inclusion criteria were enrolled, excluding those with IBD who were not first-time admissions during the study period. All investigators received standardized training and obtained informed consent from each patient before participation, providing clear explanations of the study’s objectives and essential items. For patients with reading or comprehension difficulties, the investigators verbally clarified the questions and recorded their responses according to their selections. Investigators also monitored the process to ensure that all questionnaires were accurately completed and submitted.
SEM posits causal relationships among latent variables, which are reflected by a set of observed indicators. Drawing on the SEM framework, construction principles, and previous psychiatric research, the following theoretical assumptions were proposed regarding the relationships between PSQI, anxiety, depression, and the related mediating factors: (1) PSQI may directly affect anxiety and depression, and (2) PSQI may also indirectly affect anxiety and depression through coping styles.
Data analysis was conducted using SPSS version 26.0, GraphPad Prism version 8.0, and Amos version 26.0 software. Continuous variables are summarized as mean ± SD or as median (interquartile range), and group comparisons were performed using independent-samples t-tests or non-parametric tests. Categorical variables are expressed as n (%) and analyzed using χ2 tests. Correlation analyses were performed using Pearson or Spearman methods according to data distribution. Linear regression identified anxiety and depression as dependent variables, with influencing factors as predictors. Following prior literature, SEM was constructed in Amos version 26.0 for model fitting, modification, and path analysis, with parameters estimated via maximum likelihood, and mediating effects assessed using bootstrap. Statistical significance was set at P < 0.05.
Among the 247 patients with IBD, there were 122 males (49.4%) and 125 females (50.6%). Seventy-seven patients (31.2%) were aged over 18 years, and 84 had ulcerative colitis (34.0%). Additional demographic and clinical details are presented in Table 1.
| Variable | Classification | n | % |
| Age | ≥ 18 years | 77 | 31.2 |
| ≥ 40 years | 82 | 33.2 | |
| ≥ 60 years | 88 | 35.6 | |
| Sex | Male | 122 | 49.4 |
| Female | 125 | 50.6 | |
| BMI (kg/m2) | < 18.5 | 12 | 83.4 |
| 18.5-23.9 | 206 | 11.7 | |
| ≥ 24.0 | 29 | 4.9 | |
| Course | < 1 year | 109 | 44.1 |
| ≥ 1 year | 138 | 55.9 | |
| Disease classification | Crohn’s disease | 163 | 66.0 |
| Ulcerative colitis | 84 | 34.0 | |
| Working condition | Employed | 114 | 46.2 |
| Unemployed | 133 | 53.8 | |
| Place of abode | Urban | 173 | 70.0 |
| Rural | 74 | 30.0 | |
| Standard of culture | ≤ Junior high | 72 | 29.2 |
| High school/vocational | 85 | 34.4 | |
| ≥ College | 90 | 36.4 | |
| Marital status | Unmarried | 97 | 39.3 |
| Married | 89 | 36.0 | |
| Divorced/widowed | 61 | 24.7 | |
| Average monthly household income | < 3000 yuan | 119 | 48.2 |
| ≥ 3000 yuan | 128 | 51.8 | |
| Use of biological agents | Yes | 185 | 74.9 |
| No | 62 | 25.1 | |
| Disease stage | Remission | 142 | 57.5 |
| Active | 105 | 42.5 | |
| Medical insurance | Yes | 178 | 72.1 |
| No | 69 | 27.9 |
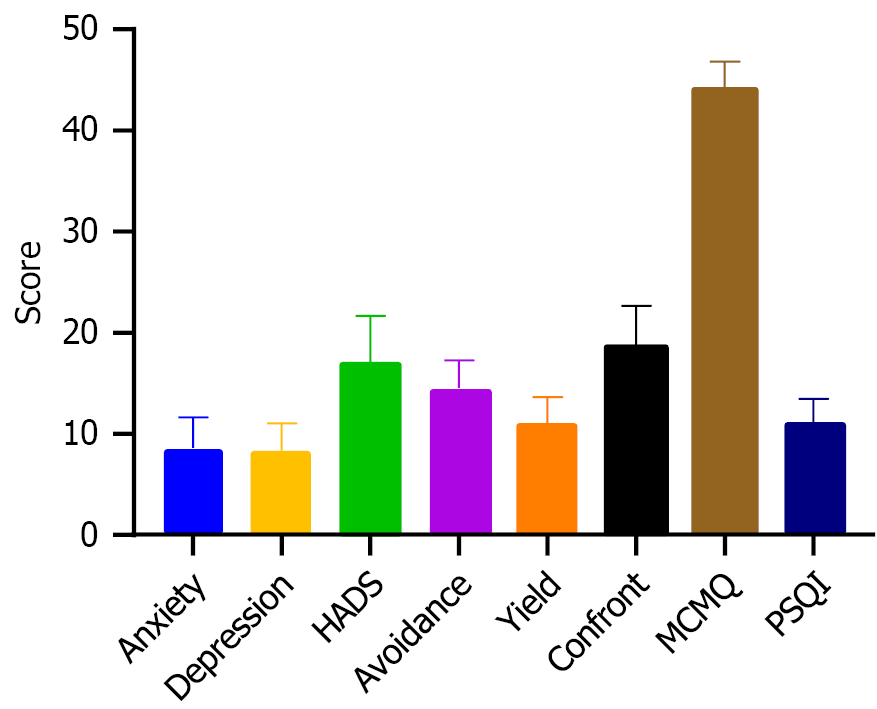
The total PSQI, HADS, and MCMQ scores among participants were 11 (10-13), 15 (13-20), and 44 (43-45), respectively, as shown in Figure 1. Of the 247 patients with IBD, 108 (43.7%) exhibited anxiety and 107 (43.3%) exhibited depression.
Anxiety and depression scores were compared across age groups, sex, employment statuses, per capita monthly family incomes, disease stages, and marital statuses. Statistically significant differences were observed (P < 0.05), as shown in Table 2.
| Variable | n | HADS score | t/F | P value |
| Age | 40.605 | < 0.001 | ||
| ≥ 18 years | 77 | 22.00 (14.00-25.00) | ||
| ≥ 40 years | 82 | 17.00 (14.00-19.00) | ||
| ≥ 60 years | 88 | 14.00 (13.00-16.00) | ||
| Sex | 62.748 | < 0.001 | ||
| Male | 122 | 14.00 (12.75-16.00) | ||
| Female | 125 | 19.00 (15.00-23.00) | ||
| BMI (kg/m2) | 2.184 | 0.336 | ||
| < 18.5 | 12 | 18.50 (14.00-22.00) | ||
| 18.5-23.9 | 206 | 16.00 (13.00-20.00) | ||
| ≥ 24.0 | 29 | 14.00 (13.00-18.50) | ||
| Course | 1.066 | 0.302 | ||
| < 1 year | 109 | 15.00 (13.00-20.00) | ||
| ≥ 1 year | 138 | 16.00 (13.00-20.25) | ||
| Disease classification | 1.345 | 0.246 | ||
| Crohn’s disease | 163 | 15.00 (14.00-21.00) | ||
| Ulcerative colitis | 84 | 15.00 (13.00-19.75) | ||
| Working condition | 183.325 | < 0.001 | ||
| Employed | 114 | 13.00 (12.00-14.00) | ||
| Unemployed | 133 | 20.00 (17.00-24.00) | ||
| Place of abode | 0.089 | 0.766 | ||
| Urban | 173 | 16.00 (13.00-20.00) | ||
| Rural | 74 | 15.00 (14.00-20.00) | ||
| Standard of culture | 3.431 | 0.180 | ||
| ≤ Junior high | 72 | 15.00 (13.00-21.00) | ||
| High school/vocational | 85 | 16.00 (14.00-21.00) | ||
| ≥ College | 90 | 14.00 (13.00-18.00) | ||
| Marital status | 93.130 | < 0.001 | ||
| Married | 89 | 13.00 (12.00-14.00) | ||
| Unmarried | 97 | 18.00 (15.00-20.00) | ||
| Divorced/widowed | 61 | 23.00 (15.00-25.00) | ||
| Average monthly household income | 138.564 | < 0.001 | ||
| < 3000 yuan | 119 | 13.00 (12.00-18.00) | ||
| ≥ 3000 yuan | 128 | 19.00 (16.25-23.75) | ||
| Use of biological agents | 0.245 | 0.620 | ||
| Yes | 185 | 15.00 (13.00-20.00) | ||
| No | 62 | 16.00 (13.00-22.00) | ||
| Disease stage | 144.762 | < 0.001 | ||
| Remission | 142 | 14.00 (12.75-14.00) | ||
| Active | 105 | 21.00 (18.00-24.50) | ||
| Medical insurance | 0.000 | 0.990 | ||
| Yes | 178 | 15.00 (13.00-20.00) | ||
| No | 69 | 15.00 (13.00-21.00) |
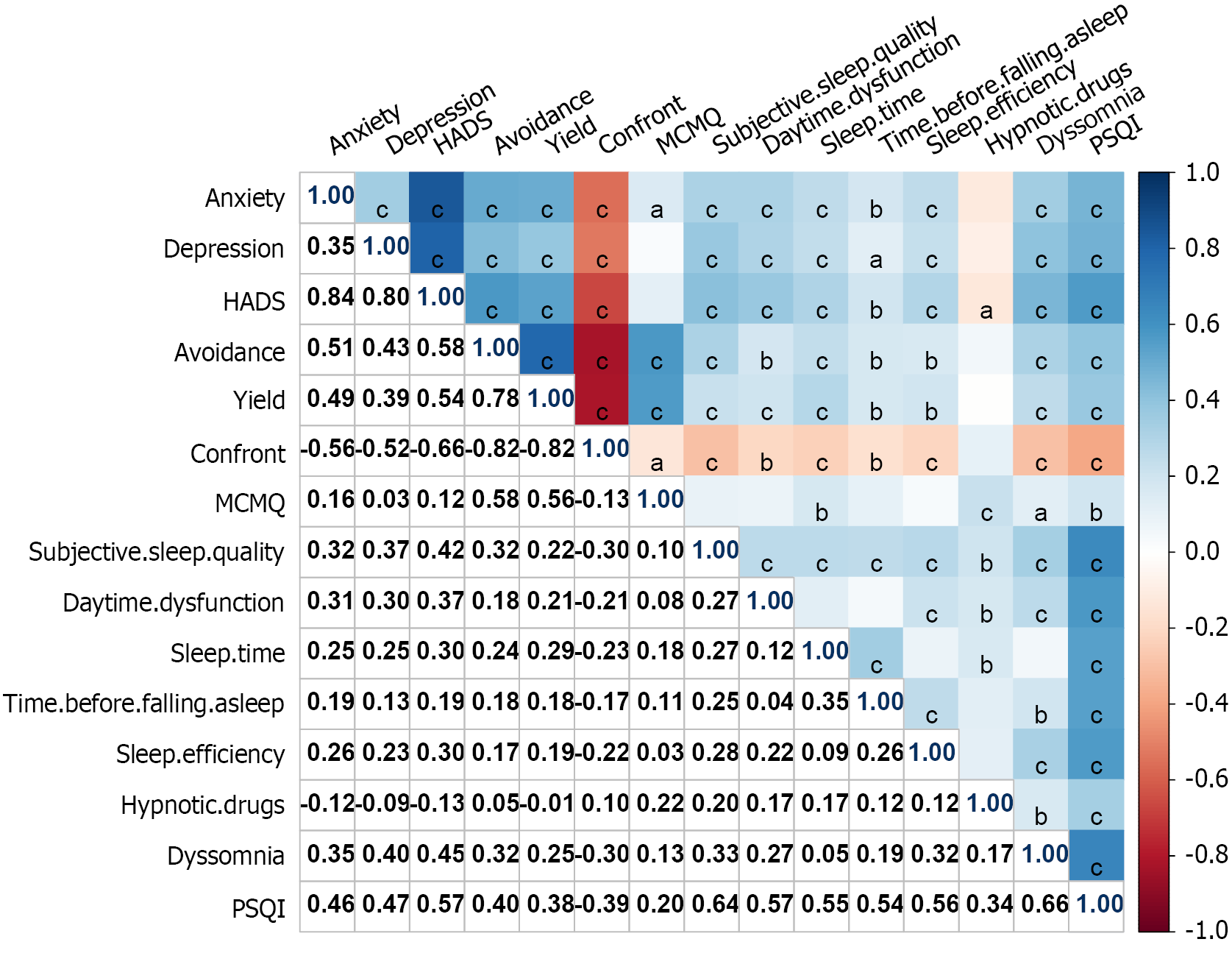
Sleep quality, coping styles, and anxiety and depression scores among patients with IBD were significantly interrelated (P < 0.001), fulfilling the prerequisite for mediation effect testing, as shown in Figure 2.
Using the HADS score in patients with IBD as the dependent variable and age, gender, employment status, per capita monthly family income, disease stage, marital status, PSQI score, and MCMQ score as independent variables (coding shown in Table 3), the model accounted for 86.1% of the variance (Table 4).
| Variable | Coding |
| HADS score | Original value input |
| Age | ≥ 18 years = 2; ≥ 40 years = 1; ≥ 60 years = 0 |
| Sex | Male = 0; female = 1 |
| Working condition | Employed = 0; unemployed = 1 |
| Average monthly household income | < 3000 yuan = 1; ≥ 3000 yuan = 0 |
| Disease stage | Active = 1; remission = 0 |
| Marital status | Married = 0; unmarried = 1; divorced/widowed = 2 |
| PSQI score | Original value input |
| MCMQ score | Original value input |
| Variable | B | SE | β | t | P value | 95%CI |
| Constant | -17.281 | 4.695 | -3.68 | < 0.001 | -26.531 to -8.031 | |
| Age | 1.072 | 0.155 | 0.183 | 6.908 | < 0.001 | 0.766-1.378 |
| Sex | 0.750 | 0.261 | 0.079 | 2.877 | 0.004 | 0.237-1.264 |
| Working condition | 1.118 | 0.556 | 0.117 | 2.009 | 0.046 | 0.022-2.213 |
| Marital status | 0.715 | 0.192 | 0.116 | 3.718 | < 0.001 | 0.336-1.094 |
| Average monthly household income | 0.907 | 0.446 | 0.095 | 2.034 | 0.043 | 0.029-1.786 |
| Disease stage | 1.147 | 0.397 | 0.119 | 2.887 | 0.004 | 0.364-1.929 |
| PSQI score | 1.141 | 0.101 | 0.537 | 11.34 | < 0.001 | 0.943-1.339 |
| MCMQ score | 0.403 | 0.112 | 0.117 | 3.597 | < 0.001 | 0.182-0.624 |
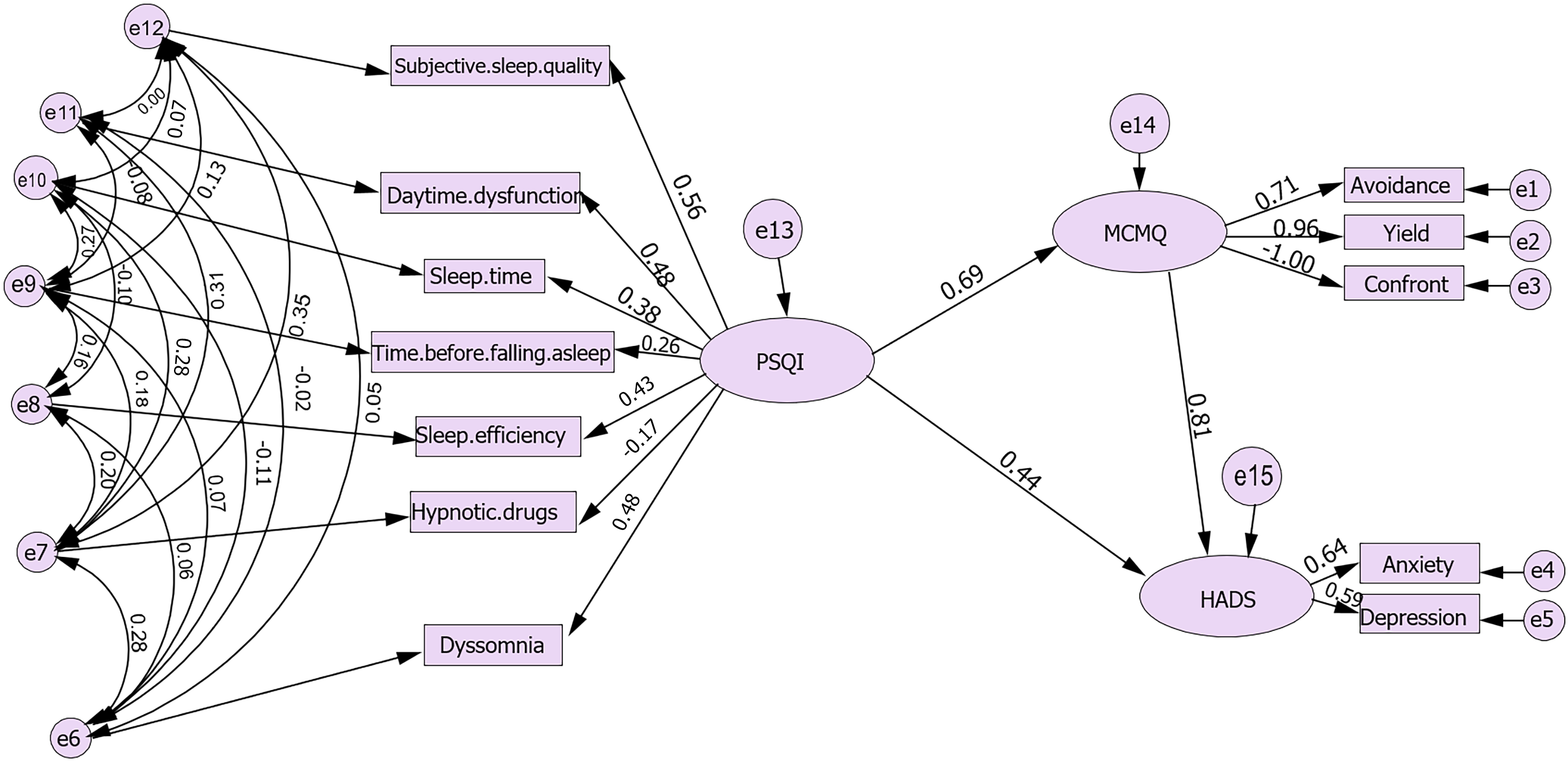
The structural equation model was developed using AMOS 26.0, with anxiety and depression among patients as dependent variables. Control variables that were statistically significant in the hierarchical regression analysis, PSQI as the independent variable, and MCMQ as the mediating variable were included to establish the initial model. Parameters were estimated using the maximum likelihood method. Guided by prior literature and path P values, only statistically meaningful variables and paths were retained to generate the final optimal model (Figure 3). The model demonstrated excellent fit, with χ2/df = 1.039 (Table 5).
| Index | Reference standard | Observed result | Accept |
| χ2/df | < 3.00 | 1.039 | Yes |
| RESEA | < 0.08 | 0.013 | Yes |
| GFI | > 0.90 | 0.978 | Yes |
| AGFI | > 0.90 | 0.949 | Yes |
| NFI | > 0.90 | 0.976 | Yes |
| IFI | > 0.90 | 0.999 | Yes |
| CFI | > 0.90 | 0.999 | Yes |
The bootstrap method was applied to examine mediating effects. Results indicated that PSQI (β = 3.223, P < 0.01) and MCMQ scores (β = 1.859, P < 0.01) exerted direct positive effects on anxiety and depression, whereas MCMQ also demon
| Influence path | Estimate | SE | t | P value |
| PSQI to MCMQ | 3.223 | 0.807 | 3.993 | < 0.001 |
| PSQI to HADS | 1.859 | 0.740 | 2.512 | 0.012 |
| MCMQ to HADS | 0.724 | 0.121 | 6.001 | < 0.001 |
| Avoidance to MCMQ | 1.000 | |||
| Yield to MCMQ | 0.946 | 0.025 | 37.275 | < 0.001 |
| Confront to MCMQ | -1.563 | 0.029 | -53.412 | < 0.001 |
| Anxiety to HADS | 1.000 | |||
| Depression to HADS | 0.833 | 0.085 | 9.787 | < 0.001 |
| Subjective sleep quality to PSQI | 0.592 | 0.115 | 5.141 | < 0.001 |
| Daytime dysfunction to PSQI | 0.726 | 0.158 | 4.589 | < 0.001 |
| Sleep time to PSQI | 0.603 | 0.159 | 3.797 | < 0.001 |
| Time before falling asleep to PSQI | 0.294 | 0.099 | 2.975 | 0.003 |
| Sleep efficiency to PSQI | 0.472 | 0.107 | 4.428 | < 0.001 |
| Hypnotic drugs to PSQI | -0.057 | 0.032 | -1.796 | 0.072 |
| Dyssomnia to PSQI | 1.000 |
| Path | Direct effect (β) | Indirect effect (β) | Total effect (β) |
| PSQI to MCMQ | 3.223 | 0.000 | 3.223 |
| MCMQ to HADS | 1.859 | 2.335 | 4.194 |
| PSQI to HADS | 0.724 | 0.000 | 0.724 |
Compared with the general population, patients with IBD are more prone to developing negative emotional states such as anxiety and depression because of the chronic nature of the disease, which involves persistent symptoms including abdominal pain, diarrhea, and fatigue. These symptoms substantially impair quality of life[13,14]. In addition, psychological stressors can influence the brain through mechanisms involving the brain-gut-microbiota axis and the corticotropin-releasing factor system, thereby altering gut microbiota composition and precipitating gastrointestinal symptoms such as abdominal pain and diarrhea[15,16]. Consequently, early identification of risk factors and timely psychological assessment and intervention are essential for patients with IBD.
Research has identified age as an independent predictor of anxiety and depression[17,18], consistent with the findings of this study. Younger individuals face a higher risk of IBD and are more likely to develop anxiety and depression, largely because of their involvement in crucial life stages such as education, career establishment, and family responsibilities, which often entail considerable financial strain. Moreover, younger patients may lack adequate understanding of IBD, making them more vulnerable to psychological distress. Conversely, older patients generally adapt more effectively to the disease, maintaining a healthier mindset and reducing the likelihood of adverse emotional reactions.
This study also confirmed that women are more susceptible to anxiety and depression than men, consistent with previous research[19]. Women tend to exhibit greater emotional reactivity and may experience heavier psychological burdens, resulting in more pessimistic outlooks when affected by IBD. Liu et al[20] reported that women demonstrated higher disease activity and more severe gastrointestinal symptoms than men, suggesting that differences in physical and psychological resilience contribute to heightened vulnerability. Possible mechanisms underlying this sex difference include hormonal regulation, immune modulation, gut microbiota diversity, and environmental influences[21]. Clinicians should therefore monitor the psychological well-being of female patients with IBD and provide timely education and supportive interventions.
Patients with IBD in the active disease phase exhibit a significantly higher prevalence of anxiety and depression than those in remission, and disease activity serves as an independent predictor of these psychological conditions, consistent with findings by Marrie et al[22]. The link between IBD activity and psychological disorders may reflect the bidirectional interactions of the brain-gut axis[23]. Inflammatory mediators originating in the gut can influence the central nervous system via complex neuroendocrine pathways, while psychological disorders can activate the hypothalamic-pituitary-adrenal axis, thereby worsening intestinal inflammation[24,25]. Continuous monitoring and timely intervention for anxiety and depression in active IBD are therefore crucial to reduce their adverse impact on disease progression.
Bisgaard et al[3] and Shah et al[26] reported that married patients with IBD benefit from ongoing emotional and practical support from their spouses, including daily care and companionship during treatment. Such support alleviates anxiety associated with the unpredictable course of IBD. Spousal involvement also promotes adherence to complex treatment regimens and dietary management, reducing relapse frequency and disease-related distress. Therefore, special attention should be given to unmarried patients with IBD by implementing targeted psychological interventions, such as disease education or peer-support programs, to enhance emotional resilience and reduce illness burden.
Regarding family income, this study found that lower monthly income was associated with a higher risk of anxiety, consistent with previous international research[27]. The chronic, relapsing nature of IBD necessitates long-term care, which can impose substantial financial strain on low-income families, often leading to guilt and heightened anxiety among patients[28]. Furthermore, unemployed patients with IBD are more likely to experience anxiety and depression than employed individuals, and unemployment serves as an independent predictor of these outcomes. Song et al[19] emphasized that employment supports daily functioning and social engagement, which lowers depression risk. Therefore, clinicians should evaluate socioeconomic stressors and offer tailored psychological support for unemployed patients when appropriate.
SEM is a robust analytical approach frequently applied in social and behavioral sciences to examine multiple latent constructs concurrently and clarify intervariable relationships. This study demonstrated that both PSQI and MCMQ scores exerted statistically significant effects on anxiety and depression among patients with IBD. Model fit indices, including the goodness-of-fit index, the adjusted goodness-of-fit index, the root mean square error of approximation, the incremental fit index, the comparative fit index, and the normed fit index, indicated excellent fit, supporting the reliability and validity of the proposed SEM model. Findings revealed that sleep quality and coping strategies significantly affected anxiety and depression, with coping strategies showing a greater total influence than sleep quality.
Previous studies have shown that sleep disturbances not only exacerbate fatigue in patients with IBD but also elevate levels of pro-inflammatory cytokines and inflammatory markers, thereby increasing disease activity[29]. This underscores the need for clinicians to carefully monitor sleep quality in patients with IBD. According to Robbins’ stress theory, patients with IBD frequently experience prolonged sleep onset and reduced sleep efficiency because of recurrent diarrhea and repeated hospitalizations. These sleep difficulties, if unaddressed, can precipitate anxiety and depression. Evidence suggests that cultivating positive psychological traits such as resilience and post-traumatic growth enables patients with IBD to accept their illness, strengthen self-management, and enhance quality of life[30]. Consequently, clinicians may implement positive psychological interventions, including mindfulness therapy, positive cognitive-behavioral therapy, and expressive writing focused on positive emotion, to reduce distress and foster adaptive emotional states, thereby improving overall well-being. Nevertheless, research on these interventions remains limited, and standardized measures for assessing their effectiveness are lacking, warranting further investigation.
This study successfully identified several risk factors associated with anxiety and depression among patients with IBD, although certain limitations should be acknowledged. The sample was obtained from a single hospital, which may have restricted the representativeness of the findings. Patients from various regions may differ in living environments, dietary patterns, and healthcare accessibility, all of which can affect the development of anxiety and depression and their associated risk factors. For instance, individuals in economically developed regions often have greater access to psychological care and specialized mental health services, lowering their risk of emotional distress. Conversely, those in remote areas may face heightened vulnerability because of limited healthcare resources and insufficient disease awareness. Future research should therefore include larger, multicenter samples to improve the external validity and generalizability of the results.
This study identified both direct and indirect determinants of anxiety and depression among patients with IBD, offering a theoretical foundation for clinicians to design targeted intervention strategies. Although the examined variables contri
| 1. | Shao B, Yang W, Cao Q. Landscape and predictions of inflammatory bowel disease in China: China will enter the Compounding Prevalence stage around 2030. Front Public Health. 2022;10:1032679. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 34] [Cited by in RCA: 33] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 2. | Yu Z, Ruan G, Bai X, Sun Y, Yang H, Qian J. Growing burden of inflammatory bowel disease in China: Findings from the Global Burden of Disease Study 2021 and predictions to 2035. Chin Med J (Engl). 2024;137:2851-2859. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 26] [Article Influence: 13.0] [Reference Citation Analysis (0)] |
| 3. | Bisgaard TH, Allin KH, Keefer L, Ananthakrishnan AN, Jess T. Depression and anxiety in inflammatory bowel disease: epidemiology, mechanisms and treatment. Nat Rev Gastroenterol Hepatol. 2022;19:717-726. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 477] [Cited by in RCA: 393] [Article Influence: 98.3] [Reference Citation Analysis (5)] |
| 4. | Yu Q, Zhu C, Feng S, Xu L, Hu S, Chen H, Chen H, Yao S, Wang X, Chen Y. Economic Burden and Health Care Access for Patients With Inflammatory Bowel Diseases in China: Web-Based Survey Study. J Med Internet Res. 2021;23:e20629. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 56] [Cited by in RCA: 49] [Article Influence: 9.8] [Reference Citation Analysis (0)] |
| 5. | Luo J, Xu Z, Noordam R, van Heemst D, Li-Gao R. Depression and Inflammatory Bowel Disease: A Bidirectional Two-sample Mendelian Randomization Study. J Crohns Colitis. 2022;16:633-642. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 133] [Cited by in RCA: 111] [Article Influence: 27.8] [Reference Citation Analysis (1)] |
| 6. | Barberio B, Zamani M, Black CJ, Savarino EV, Ford AC. Prevalence of symptoms of anxiety and depression in patients with inflammatory bowel disease: a systematic review and meta-analysis. Lancet Gastroenterol Hepatol. 2021;6:359-370. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 614] [Cited by in RCA: 520] [Article Influence: 104.0] [Reference Citation Analysis (1)] |
| 7. | Chen DL, Dai YC, Zheng L, Chen YL, Zhang YL, Tang ZP. Features of the gut microbiota in ulcerative colitis patients with depression: A pilot study. Medicine (Baltimore). 2021;100:e24845. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 29] [Article Influence: 5.8] [Reference Citation Analysis (1)] |
| 8. | Gîlc-Blanariu GE, Ștefnescu G, Trifan AV, Moscalu M, Dimofte MG, Ștefnescu C, Drug VL, Afrsnie VA, Ciocoiu M. Sleep Impairment and Psychological Distress among Patients with Inflammatory Bowel Disease-beyond the Obvious. J Clin Med. 2020;9:2304. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 33] [Cited by in RCA: 27] [Article Influence: 4.5] [Reference Citation Analysis (1)] |
| 9. | Philippou A, Sehgal P, Ungaro RC, Wang K, Bagiella E, Dubinsky MC, Keefer L. High Levels of Psychological Resilience Are Associated With Decreased Anxiety in Inflammatory Bowel Disease. Inflamm Bowel Dis. 2022;28:888-894. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 33] [Cited by in RCA: 24] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 10. | Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand. 1983;67:361-370. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36742] [Cited by in RCA: 32349] [Article Influence: 752.3] [Reference Citation Analysis (4)] |
| 11. | Liu Y, Jiang TT, Shi TY. The Relationship Among Rumination, Coping Strategies, and Subjective Well-being in Chinese Patients With Breast Cancer: A Cross-sectional study. Asian Nurs Res (Korean Soc Nurs Sci). 2020;14:206-211. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 21] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 12. | Sancho-Domingo C, Carballo JL, Coloma-Carmona A, Buysse DJ. Brief version of the Pittsburgh Sleep Quality Index (B-PSQI) and measurement invariance across gender and age in a population-based sample. Psychol Assess. 2021;33:111-121. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 141] [Cited by in RCA: 113] [Article Influence: 22.6] [Reference Citation Analysis (0)] |
| 13. | Zhao E, Yu Q, Ali AI, Mu Y, Shi Y, Zhu L. Effects of standard treatments on depressive/anxiety symptoms in patients with inflammatory bowel disease: A systematic review and meta-analysis. Gen Hosp Psychiatry. 2022;74:118-125. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 4] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 14. | Neuendorf R, Harding A, Stello N, Hanes D, Wahbeh H. Depression and anxiety in patients with Inflammatory Bowel Disease: A systematic review. J Psychosom Res. 2016;87:70-80. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 486] [Cited by in RCA: 427] [Article Influence: 42.7] [Reference Citation Analysis (1)] |
| 15. | Triantafillidis JK, Merikas E, Gikas A. Psychological factors and stress in inflammatory bowel disease. Expert Rev Gastroenterol Hepatol. 2013;7:225-238. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 31] [Article Influence: 2.4] [Reference Citation Analysis (1)] |
| 16. | Balestrieri P, Cicala M, Ribolsi M. Psychological distress in inflammatory bowel disease. Expert Rev Gastroenterol Hepatol. 2023;17:539-553. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 21] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 17. | Kim MC, Jung YS, Song YS, Lee JI, Park JH, Sohn CI, Choi KY, Park DI. Factors Associated with Anxiety and Depression in Korean Patients with Inactive Inflammatory Bowel Disease. Gut Liver. 2016;10:399-405. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 20] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 18. | Choi K, Chun J, Han K, Park S, Soh H, Kim J, Lee J, Lee HJ, Im JP, Kim JS. Risk of Anxiety and Depression in Patients with Inflammatory Bowel Disease: A Nationwide, Population-Based Study. J Clin Med. 2019;8:654. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 100] [Cited by in RCA: 89] [Article Influence: 12.7] [Reference Citation Analysis (1)] |
| 19. | Song JH, Kim JW, Oh CH, Kim HJ, Lee CK, Kang WS. Depression, Anxiety, Related Risk Factors and Cognitive Distortion in Korean Patients with Inflammatory Bowel Disease. Psychiatry Investig. 2020;17:1126-1136. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 13] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 20. | Liu C, Zhang J, Chen M, An P, Xiang J, Yu R, Zeng S, Wei S, Deng B, Liu Z, Jiang C, Shi J, Wu K, Dong W. Gender Differences in Psychological Symptoms and Quality of Life in Patients with Inflammatory Bowel Disease in China: A Multicenter Study. J Clin Med. 2023;12:1791. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 14] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 21. | Pace F, Watnick PI. The Interplay of Sex Steroids, the Immune Response, and the Intestinal Microbiota. Trends Microbiol. 2021;29:849-859. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 57] [Cited by in RCA: 46] [Article Influence: 9.2] [Reference Citation Analysis (0)] |
| 22. | Marrie RA, Graff LA, Fisk JD, Patten SB, Bernstein CN. The Relationship Between Symptoms of Depression and Anxiety and Disease Activity in IBD Over Time. Inflamm Bowel Dis. 2021;27:1285-1293. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 111] [Cited by in RCA: 99] [Article Influence: 19.8] [Reference Citation Analysis (1)] |
| 23. | Fairbrass KM, Lovatt J, Barberio B, Yuan Y, Gracie DJ, Ford AC. Bidirectional brain-gut axis effects influence mood and prognosis in IBD: a systematic review and meta-analysis. Gut. 2022;71:1773-1780. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 179] [Cited by in RCA: 162] [Article Influence: 40.5] [Reference Citation Analysis (0)] |
| 24. | Bennebroek Evertsz' F, Sprangers MAG, de Vries LM, Sanderman R, Stokkers PCF, Verdam MGE, Burger H, Bockting CLH. I am a total failure: associations between beliefs and anxiety and depression in patients with inflammatory bowel disease with poor mental quality of life. Behav Cogn Psychother. 2020;48:91-102. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 9] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 25. | Yu R, Liu C, Zhang J, Li J, Tian S, Ding F, Liu Z, Wang T, Liu Z, Jiang C, Shi J, Wu K, Dong W. Correlation Analysis Between Disease Activity and Anxiety, Depression, Sleep Disturbance, and Quality of Life in Patients with Inflammatory Bowel Disease. Nat Sci Sleep. 2023;15:407-421. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 26. | Shah SC, Itzkowitz SH. Colorectal Cancer in Inflammatory Bowel Disease: Mechanisms and Management. Gastroenterology. 2022;162:715-730.e3. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 666] [Cited by in RCA: 609] [Article Influence: 152.3] [Reference Citation Analysis (6)] |
| 27. | Sceats LA, Dehghan MS, Rumer KK, Trickey A, Morris AM, Kin C. Surgery, stomas, and anxiety and depression in inflammatory bowel disease: a retrospective cohort analysis of privately insured patients. Colorectal Dis. 2020;22:544-553. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 18] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 28. | Eugenicos MP, Ferreira NB. Psychological factors associated with inflammatory bowel disease. Br Med Bull. 2021;138:16-28. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 43] [Cited by in RCA: 36] [Article Influence: 7.2] [Reference Citation Analysis (0)] |
| 29. | Rozich JJ, Holmer A, Singh S. Effect of Lifestyle Factors on Outcomes in Patients With Inflammatory Bowel Diseases. Am J Gastroenterol. 2020;115:832-840. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 173] [Cited by in RCA: 151] [Article Influence: 25.2] [Reference Citation Analysis (0)] |
| 30. | Hamama-Raz Y, Nativ S, Hamama L. Post-traumatic Growth in Inflammatory Bowel Disease Patients: The Role of Illness Cognitions and Physical Quality of Life. J Crohns Colitis. 2021;15:1060-1067. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 12] [Article Influence: 2.4] [Reference Citation Analysis (0)] |