Copyright: ©Author(s) 2026.
World J Gastrointest Oncol. Apr 15, 2026; 18(4): 115614
Published online Apr 15, 2026. doi: 10.4251/wjgo.v18.i4.115614
Published online Apr 15, 2026. doi: 10.4251/wjgo.v18.i4.115614
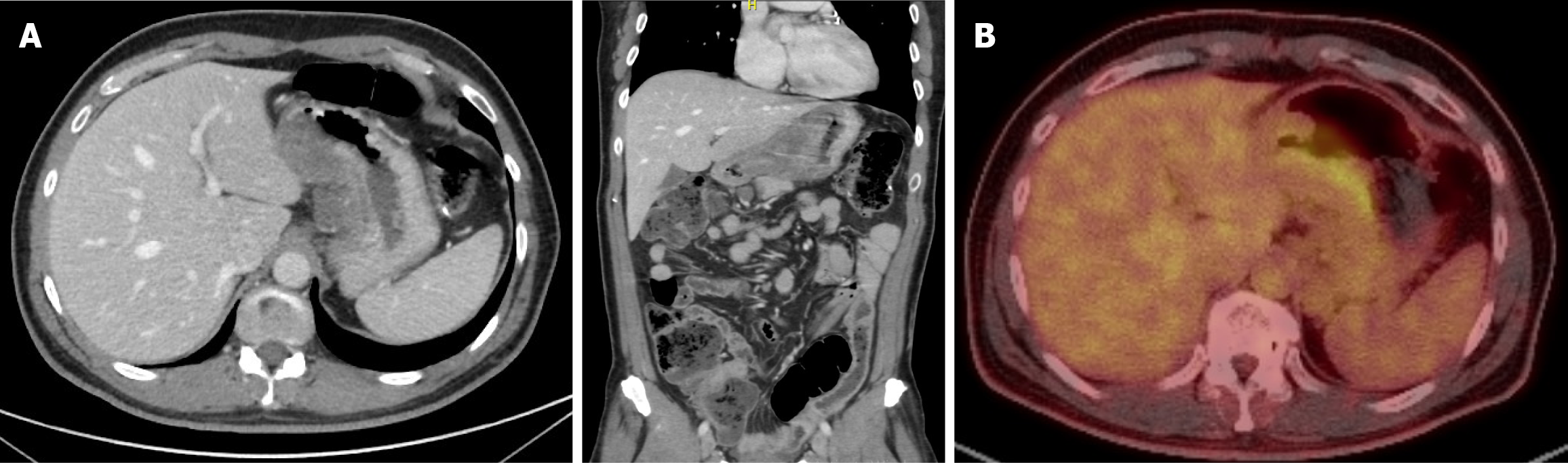
Figure 1 Initial radiological staging.
A: Computed tomography (CT) scan of the chest, abdomen and pelvis scan showing a mural thickening of the lesser curvature of stomach reaching the antrum, associated with locoregional lymphadenopathy; B: Whole positron emission tomography/CT scan showing FDG avid gastric thinking.
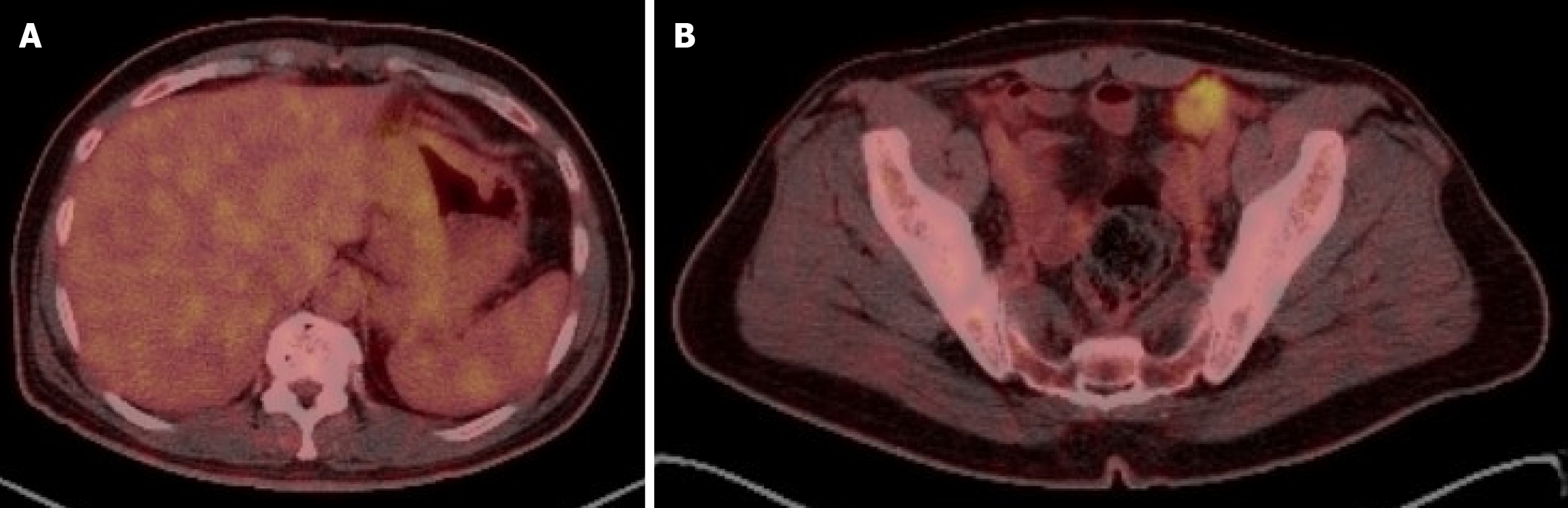
Figure 2 Post-neoadjuvant chemotherapy whole body positron emission tomography/computed tomography scan showing significant interval metabolic activity regression of the previously noted gastric lesser curvature FDG avid thickening and complete metabolic remission of the previously noted locoregional lymphadenopathy.
A: Whole body positron emission tomography/computed tomography scan post-neoadjuvant chemotherapy showing A-significant interval metabolic activity regression of the previously noted gastric lesser curvature FDG avid thickening and complete metabolic remission of the previously noted locoregional lymphadenopathy; B: New FDG uptake in an ileal bowel loop that was reported as inflammatory/infectious.
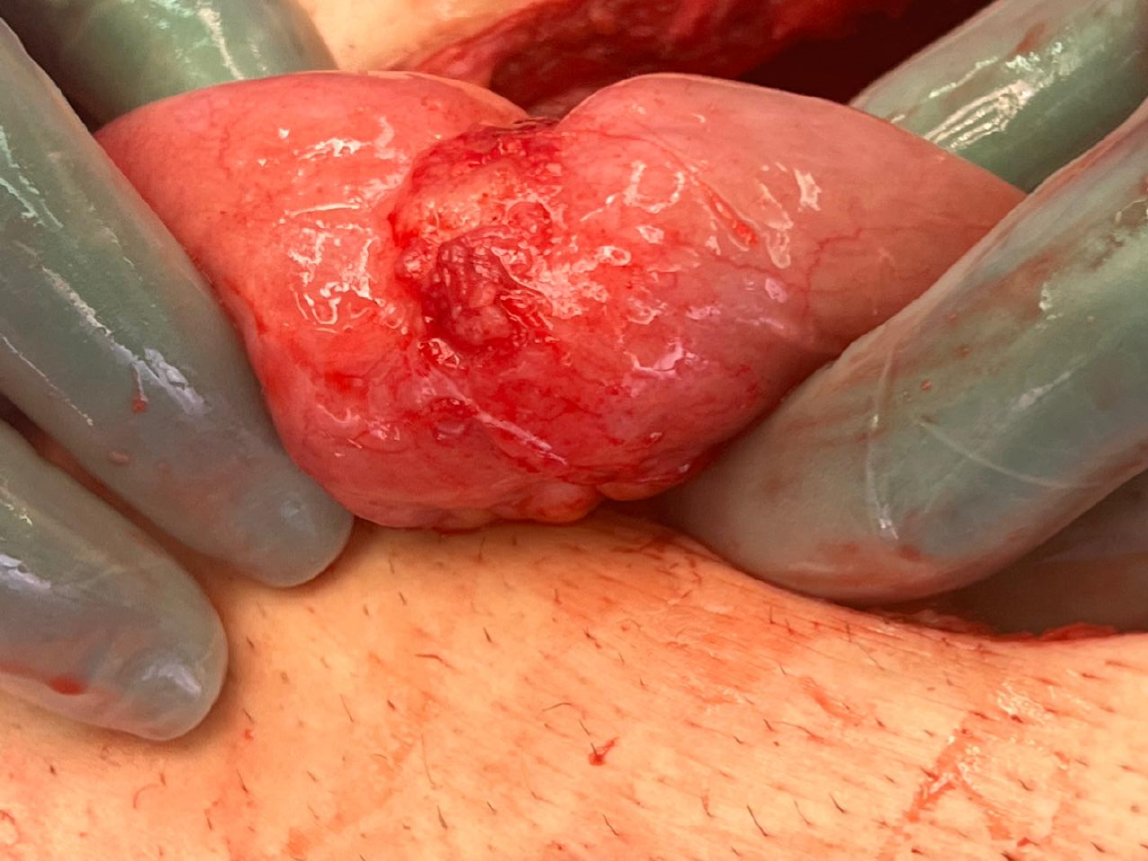
Figure 3
Intraoperative picture during the first exploration showing a small bowel mass at 40 cm proximal to the ileocecal valve.
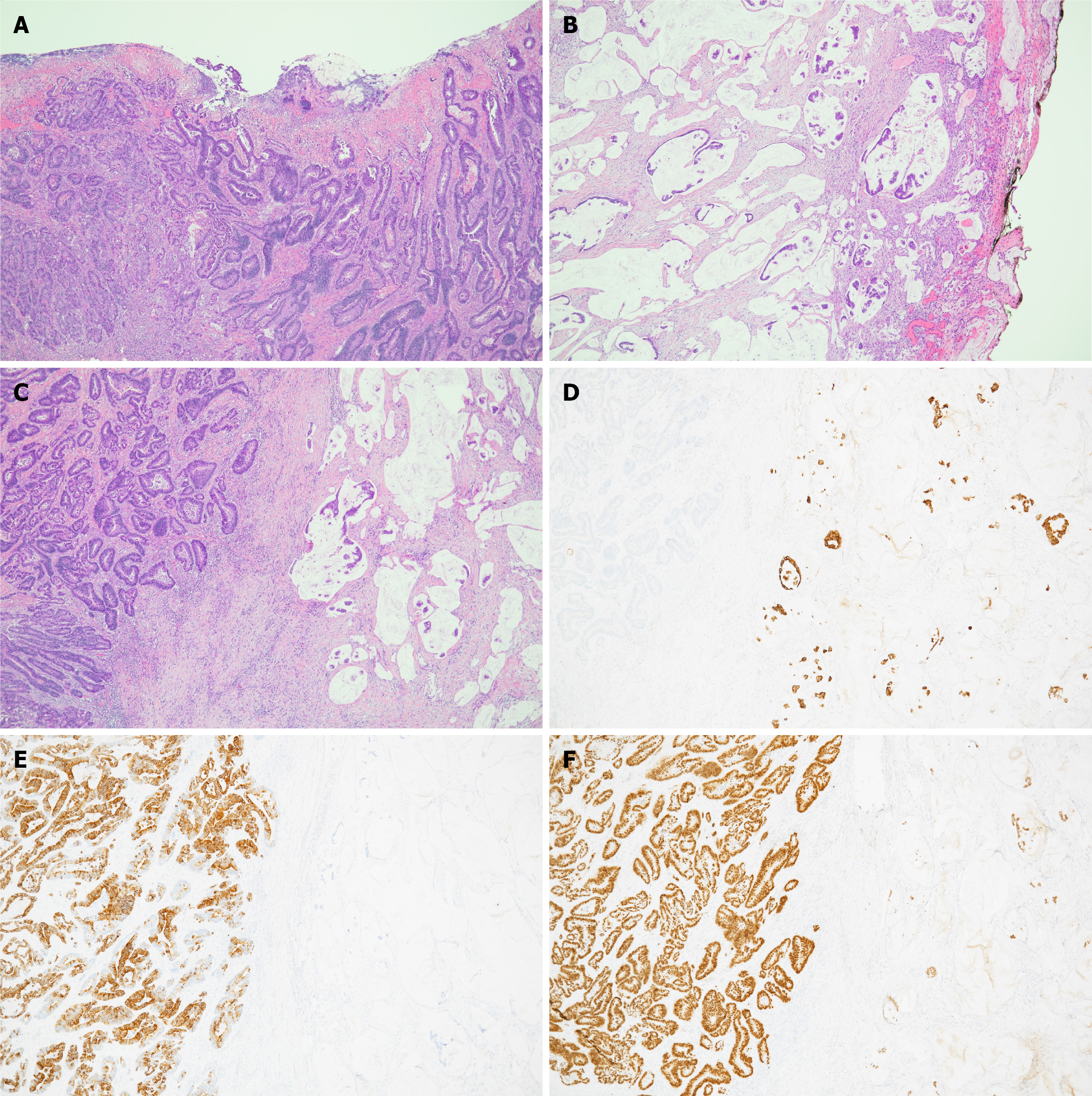
Figure 4 Histopathological examination of the resected small bowel mass showed.
A: A primary small bowel moderately differentiated adenocarcinoma; B: A metastatic Gastric mucinous adenocarcinoma; C: Co-existing primary small bowel adenocarcinoma (left) and metastatic gastric mucinous adenocarcinoma (right); D: Cytokeratin 7 immunohistochemical stain highlights the gastric adenocarcinoma; E and F: Cytokeratin 20 and CDX-2 immunohistochemical stains highlight the small bowel adenocarcinoma.
- Citation: AlQattan AS, Binkhamis L, Foula MS, Alsalim A, Alselwi WM, Alzahir AA. Triple gastrointestinal malignancies with tumor-to-tumor metastasis from gastric adenocarcinoma to small bowel adenocarcinoma: A case report. World J Gastrointest Oncol 2026; 18(4): 115614
- URL: https://www.wjgnet.com/1948-5204/full/v18/i4/115614.htm
- DOI: https://dx.doi.org/10.4251/wjgo.v18.i4.115614