This editorial refers to "Clinical study on the efficacy of laparoscopic hepatectomy via the retroperitoneal approach for treating liver tumors" by Fei et al, 2025; https://dx.doi.org/10.4254/wjh.v17.i12.110764.
INTRODUCTION
Hepatocellular carcinoma (HCC) is the third leading cause of cancer-related death, underscoring its substantial impact on public health. Surgical resection remains the cornerstone of treatment for patients with early-stage HCC, using various approaches including open surgery, laparoscopic hepatectomy (LH), and robotic LH[1]. Most laparoscopic hepatectomies are performed via a transperitoneal approach; however, recent studies have indicated that retroperitoneal laparoscopic partial hepatectomy (RLPH) can be utilized for tumors located in the posterosuperior segments of the right liver, specifically segments S6, S7, and S8[1,2]. Therefore, a thorough understanding of hepatic segmentation[3-6] and retroperitoneal anatomy[7,8] is crucial for performing RLPH and for recognizing the indications, limitations, and complications of this promising approach[1].
SURGICAL ANATOMY OF HEPATIC SEGMENTS AND RIGHT RETROPERITONEUM
The liver is divided into eight functionally independent segments (S1-S8) based on the distribution of third-order portal vein branches and the hepatic veins. The left lobe is divided into the medial segment (S4) and the lateral segments (S2 and S3), while the right lobe is divided into the anterior segments (S5 and S8) and the posterior segments (S6 and S7) by the right hepatic vein. The caudate lobe (S1) is located posteriorly between the fissure for the ligamentum venosum and inferior vena cava (IVC)[3,4]. The accuracy of this hepatic segmentation has been confirmed by ultrasound (US)[4,5] and further supported by real-time fluorescent imaging techniques using indocyanine green[6]. The retroperitoneum lies between the parietal peritoneum and the transversalis fascia. The perirenal space, bounded by Gerota’s and Zuckerkandl’s fasciae, contains the kidneys, adrenal glands, fat, and vessels, and at the upper right pole it communicates with the retrohepatic space at the liver’s bare area (Figure 1)[7,8].
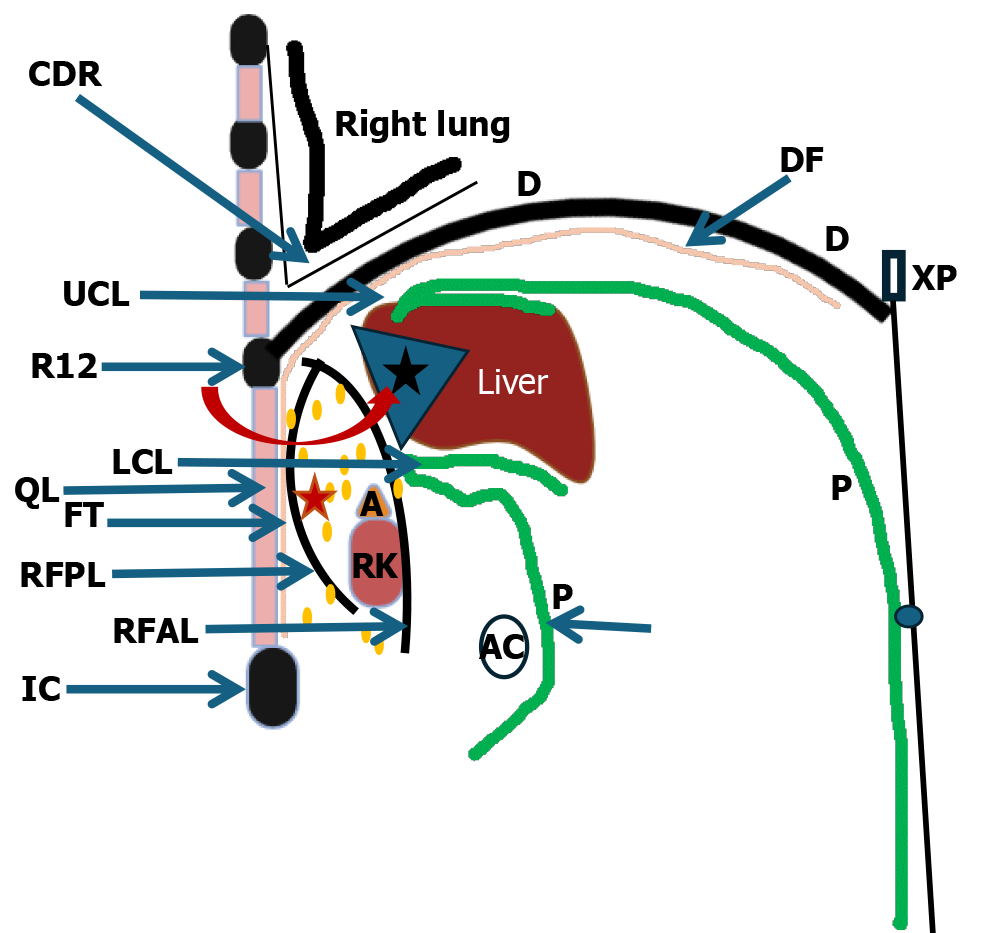
Figure 1 A schematic sagittal section of the right extraperitoneal space, showing the perirenal space (red star) and the bare area of the liver (black star, blue triangle).
The curved red arrow indicates access to the bare area in retroperitoneal laparoscopic partial hepatectomy. A: Adrenal gland; AC: Ascending colon; ALRF: Anterior layer of renal fascia; CDR: Costodiaphragmatic recess; D: Diaphragm; DF: Diaphragmatic fascia; FT: Fascia transversalis; IC: Iliac crest; LCL: Lower coronary ligament; P: Parietal peritoneum; PLRF: Posterior layer of renal fascia; QL: Quadratus lumborum; RK: Right kidney; R12: Rib12; UCL: Upper coronary ligament; XP: Xiphoid process.
LAPAROSCOPIC PROCEDURES FOR DIFFICULT RIGHT HEPATIC SEGMENTS
Various approaches have been described for accessing the posterosuperior liver segments (S6, S7, and S8), which are difficult to reach using the transabdominal laparoscopic approach. These segments are obscured during laparoscopy because they lie behind the right hepatic lobe and are further concealed by the limited working space beneath the diaphragm. Therefore, to adequately expose these segments, the right lobe of the liver must be fully mobilized, including division of the round ligament and dissection of the retroperitoneal attachments, which may injure the IVC and right adrenal gland[9-11].
According to most reports, lateral approaches – such as the transdiaphragmatic, transthoracic, or intercostal routes – alongside the classic transabdominal approach, are useful for laparoscopic visualization and resection of these segments in patients with hepatic tumors[9]. Additionally, robotic laparoscopy for resection of hepatic tumors has been reported using the transabdominal approach[1,12]. More recently, retroperitoneal resection of hepatic tumors has also been described[2,13-16].
RETROPERITONEAL LH FOR TUMORS IN THE RIGHT LIVER
A recent retrospective study by Fei et al[17] recently published in World Journal of Hepatology investigated the safety and efficacy of RLPH for lesions in segments S6, S7, and S8 in 72 patients, with a mean tumor diameter of 7.5 ± 3.4 cm. All surgeries were completed successfully, with conversion to an open approach required in 10 patients, and all patients ultimately receiving effective treatment. The authors make an important and timely contribution to minimally invasive liver surgery by applying a retroperitoneal access route – traditionally used in urologic surgery[13] – to the resection of right posterior hepatic lesions in these difficult-to-access segments. Their findings are consistent with previous studies[14-16]. The reported operative outcomes are encouraging, particularly the acceptable operative time, modest blood loss, and restoration of liver function within two weeks.
Importantly, the approach described by Fei et al[17] provides access to the liver’s bare area – which contains the difficult hepatic segments mentioned above – through the retroperitoneal space without requiring extensive transperitoneal mobilization (Figure 1). This represents a noteworthy anatomical and technical advantage that has been highlighted in prior reports[15], but was not detailed in the study by Fei et al[17]. One of the main indications for RLPH is to overcome the well-recognized challenges and risks associated with conventional transperitoneal laparoscopic resection of deep-seated right-lobe tumors, while avoiding injury to intraperitoneal structures[9-11].
Technically, potential limitations of the RLPH approach include limited familiarity of hepatic surgeons in different centers with retroperitoneal anatomy and difficulty in performing the Pringle maneuver to control accidental intraoperative bleeding; however, IVC bleeding can be effectively managed using this retroperitoneal approach[18]. The use of preoperative imaging modalities such as magnetic resonance imaging and intraoperative techniques including US and indocyanine green fluorescence imaging may reduce the rate of conversion to open hepatectomy. In addition, the relatively high conversion rate in the study of Fei et al[17] deserves further exploration, especially in relation to tumor characteristics and anatomical constraints such as proximity to major blood vessels. Postoperative histopathological examination of the resected tumor is important for follow-up and further treatment, as hepatic tumors exhibit heterogeneous pathological types[2].
However, several methodological limitations in the study by Fei et al[17] warrant further attention. The absence of a control group precludes definitive comparisons with standard transperitoneal LH. In addition, the retrospective, single-center design introduces potential selection bias. The statistical analysis lacks comparative tests such as t-tests or analysis of variance; this is likely due to the absence of a control group, resulting in a purely descriptive summary of the 72 patients. Although the authors suggest superiority over historical controls – such as reduced intraoperative blood loss and shorter operative time – the analysis does not provide P values or confidence intervals to support these claims.
For malignant cases, survival analysis was not performed because of missing follow-up data; however, a partial analysis, such as Kaplan-Meier curves or Cox regression, could have been presented.
Despite these limitations, the work by Fei et al[17] broadens the discussion on how alternative anatomical approaches can be strategically utilized to improve access to difficult hepatic segments. Their experience offers a valuable reference for centers aiming to expand their minimally invasive capabilities and lays the groundwork for future prospective, comparative, and multicenter studies to clarify indications, technical refinements, and long-term oncologic safety. Notably, recent studies suggest that robotic surgery and artificial intelligence (AI) technologies may reduce complication rates in laparoscopic partial hepatectomy.
ROBOTIC SURGERY AND AI IN PARTIAL HEPATECTOMY
Robotic retroperitoneal hepatectomy (RRH)[1,13,19] is a promising, albeit sparsely studied, technique for tumors located in the posterosuperior hepatic segments. Although the current literature consists mostly of case reports, the approach appears feasible, particularly for S7 lesions at the liver dome. RRH combines the direct access provided by the retroperitoneal route with the technical advantages of robotic surgery. It helps overcome the limitations of standard laparoscopy in deep, narrow operative fields and in patients with cirrhotic livers, allowing for enhanced dexterity during critical maneuvers such as suturing and dissection near major vascular structures. This is supported by a recent study which reports that robotic hepatectomy offers higher safety and efficacy for treating BCLC stage 0-A HCC in segments 7 and 8 compared with laparoscopic or open hepatectomy[1].
AI and machine learning are emerging as advanced technologies for optimizing RLPH, offering innovative solutions to enhance surgical precision, efficiency, and safety. AI algorithms can analyze live laparoscopic video feeds to identify anatomical landmarks, highlight critical structures, and track the movement of surgical instruments. Preoperatively, AI-driven surgical planning platforms also integrate advanced imaging modalities, such as US, magnetic resonance imaging, and computed tomography, to generate three-dimensional reconstructions of patient anatomy. Intraoperatively, AI can provide real-time tracking and guidance, enabling surgeons to navigate complex anatomical planes and manipulate instruments with greater accuracy during RLPH and related robotic procedures[1,20,21]. Vascular variations relevant to transperitoneal and extraperitoneal LH can be identified preoperatively or intraoperatively using US imaging supported by AI-based analysis[22-25], thereby helping to prevent unexpected intraoperative bleeding and facilitating the Pringle maneuver during LH[26-30].
CONCLUSION
RLPH is a safe and effective method for removing hepatic cancers located in difficult-to-access segments S6, S7, and S8 that cannot be adequately reached via the transperitoneal approach. Further clinical trials – particularly prospective, comparative, and multicenter studies – are required to clarify the indications, technical refinements, and long-term oncologic safety of RLPH. RRH is also a promising, though still sparsely studied, technique for tumors in these posterosuperior hepatic segments. In addition, AI may enhance the safety, efficiency, and outcomes of both RLPH and RRH.
Peer review: Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Gastroenterology and hepatology
Country of origin: Malaysia
Peer-review report’s classification
Scientific quality: Grade B
Novelty: Grade B
Creativity or innovation: Grade B
Scientific significance: Grade B
P-Reviewer: Mohamed DA, PhD, Professor, Egypt S-Editor: Luo ML L-Editor: A P-Editor: Xu J