Published online May 14, 2026. doi: 10.3748/wjg.v32.i18.117264
Revised: January 13, 2026
Accepted: February 13, 2026
Published online: May 14, 2026
Processing time: 154 Days and 19 Hours
Small bowel angiodysplasia (SBA) are an increasingly recognised cause of chronic anaemia and gastrointestinal bleeding. Gastrointestinal angiodysplasia have been independently associated with clinically significant impairments in health-related quality of life (QoL) and fatigue. Balloon assisted enteroscopy (BAE) and argon plasma coagulation (APC) along with general supportive measures are the stan
To assess the impact of BAE and APC on the QoL of patients with SBA and ex
Symptomatic SBA patients referred for BAE were prospectively recruited from December 2023 to December 2024. Subjects completed a short form-36 health survey (SF-36) and Fatigue Severity Scale (FSS) and provided bloods prior to treatment. Repeat SF-36 and FSS assessments were completed a minimum of 6 months post treatment. Scores pre and post intervention were compared for each subject. Results were controlled for age, gender, haemoglobin level and angiogenic factors.
Of 40 enrolled subjects, 31/36 (86%) who underwent enteroscopy with APC have completed both assessments. There was a statistically significant improvement in both FSS and disease appropriate SF-36 domains over time that was independent of age, gender and haemoglobin level. Of interest, higher endostatin levels were associated with better improvement in fatigue scores.
BAE with APC for SBA is beneficial and results in a significant improvement in both patients reported heath related QoL and fatigue severity irrespective of baseline demographics.
Core Tip: This prospective study in subjects with small bowel angiodysplasia has demonstrated that endoscopic intervention with balloon assisted enteroscopy and argon plasma coagulation has a positive impact on both patients reported quality of life and fatigue severity. The beneficial affect is independent of age, gender and baseline haemoglobin levels. The study supports the use of balloon assisted enteroscopy and argon plasma coagulation as a cornerstone of small bowel angiodysplasia treatment, particularly for those with multiple lesions and those amenable to intervention, as benefit was demonstrated without adjunctive medical therapy. Endostatin would appear to be a potential biomarker for response and warrants additional investigation.
- Citation: Butler T, O’Hara F, Costigan C, Sihag S, Kripakaran D, McNamara D. Enteroscopy and ablation of small bowel angiodysplasia improves quality-of-life and fatigue: A prospective study including biomarker assessment. World J Gastroenterol 2026; 32(18): 117264
- URL: https://www.wjgnet.com/1007-9327/full/v32/i18/117264.htm
- DOI: https://dx.doi.org/10.3748/wjg.v32.i18.117264
Balloon assisted enteroscopy (BAE) and argon plasma coagulation (APC) along with general supportive measures are the standard of care, albeit with high anaemia and bleeding recurrence rates for small bowel angiodysplasia (SBA)[1,2]. In general, there is a recognition that patient reported outcomes are an important assessment of quality in all endoscopy including BAE[3]. Similarly, quality of life (QoL) is an important outcome measure to assess the utility of any given treatment strategy particularly in patients with chronic or relapsing gastrointestinal conditions and should be assessed in addition to biochemical and clinical outcomes[4]. Previous research has shown gastrointestinal angiodysplasia are independently associated with fatigue and clinically significant impairments in health-related QoL, which can improve with medical therapy[5,6]. The effect of endoscopic therapy on fatigue and health related QoL in patients with SBA is unclear.
Several angiogenic factors have been linked with symptomatic sporadic angiodysplasia and associated overt and occult bleeding[7-9]. Their role in disease evolution and progression is not fully understood, nor has their utility in clinical practice as biomarkers been fully explored. This study aims to prospectively assess the impact of BAE with APC on the health related QoL and fatigue in a cohort of patients with capsule endoscopy confirmed SBA and to explore potential predictors of response.
Ethical approval was granted by the St James’s Hospital/Tallaght University Hospital Research Ethics Committee, No. 2020-10 Chairman’s Action (37). Adult patients referred to our centre for device assisted enteroscopy and APC of symptomatic (anaemia or gastrointestinal bleeding) capsule endoscopy confirmed significant (P2 lesions) SBA, were prospectively recruited from June 2023 to December 2024. Patients were invited to participate on the day of their procedure. Following informed consent, subjects completed both validated short form-36 health survey (SF-36) and Fatigue Severity Scale (FSS) questionnaires and provided serum for angiogenic factor analysis before undergoing endoscopy and treatment[10,11]. Patient demographics, base line bloods and endoscopy findings were documented.
Patients with multifocal gastrointestinal angiodysplasia, those with previous device-assisted enteroscopy (DAE) treatments for SBA, those who underwent DAE without intervention (lesion not identified or reached), those who failed endoscopic therapy requiring alternative intervention to control bleeding, those on maintenance medical therapy in
All procedures were performed with a balloon assisted enteroscope in accordance with our unit’s protocol and international guidance, the majority under conscious sedation. Findings and intervention including APC watts and pulses, adjunctive therapy (clips) were recorded as normal in the procedure report. Patients and the referring clinician were appraised of the results of the BAE. Specific instructions on maintenance or supportive care was not given. Both moni
Serum was collected on the day of the procedure as standard and stored for batch analysis. Quantification of angiogenic factors including angiopoietin 1 (Ang-1), angiopoietin 2, vascular endothelial growth factor, endostatin, and tissue inhi
SF-36 domain and FSS scores pre and post BAE and intervention (APC) were compared for each subject over time. A FSS of ≥ 4 was considered to represent significant fatigue, while each SF-36 domain was valued from 0-100, with higher scores associated with a more favourable health state. Results were controlled for age, gender, angiogenic factors and haemoglobin level. Initial analysis was conducted with the assistance of artificial intelligence (Microsoft Copilot, WA, United States) with findings confirmed by univariate and multivariate analysis with SPSS V.30 using standard statistical methods, including a paired t-test, Mann-Whitney U, Spearman correlations, ANOVA and linear regression. To determine the required sample size to detect a clinically significant change in QoL parameters (scores 0-100) and FSS (scores 0-7), we performed a standard power calculation to detect a change of 25 points and 2 points prospectively, with the following assumptions, significance level of 0.05, power of 80%, and standard deviations of 20 and 1.5. The estimated sample size was 22 and 16 respectively.
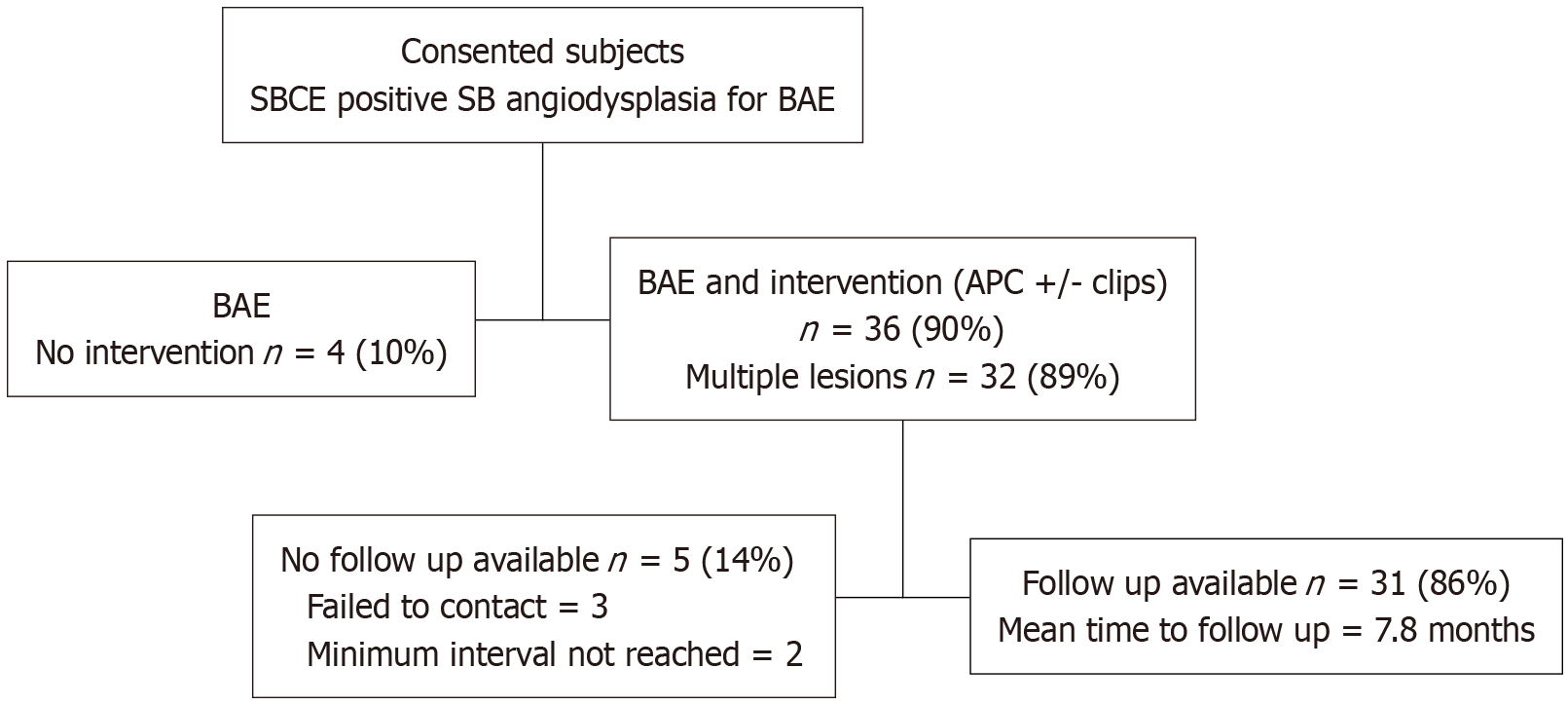
To date 40 patients have been enrolled and completed baseline SF-36 and FSS questionnaires and provided serum for angiogenic factor analysis. BAE, all but one via an anterograde approach, was complete in all cases, with identification and treatment with APC of angiodysplasia in 36 (90%). Multiple angiodysplasia were treated in the majority 32/36 (89%). APC treatment was provided at 25-30 watts at a flow rate of 0.8 L/minute, the median pulses reported was 12, clips were also applied in three cases. There were no procedural associated complications and no subject required repeat BAE during the study period. To date 31/36 (86%) who underwent enteroscopy and APC have been contacted and supplied repeat questionnaires, three individuals could not be reached and were lost to follow up and 2 had not reached the follow up requirement of 6 months. The median interval to follow up was 7.8 months. For this cohort 19 (61%) were male, the mean age was 72 ± 8.6 years (range 49-84) and mean haemoglobin was 11.1 ± 2.4, range 4-14.6 g/dL (Figure 1).
Baseline and follow up SF-36 domain scores are shown in Table 1. In summary, there was a statistically significant improvement in SF-36 scores from baseline to follow up post BAE and APC in all domains except for role limitation due to emotional difficulties and pain. Similarly, there was a significant reduction in fatigue scores over time from a mean of 4.7 (median 4.9) at base line to 2.5 (median 2) on follow up, with a mean change of -2.2, 95% confidence interval (CI): -2.8 to 1.6, P < 0.001. Age, gender and haemoglobin level did not significantly affect the changes in FSS or SF-36 domains (Table 2).
| Domain | PF | RL-P | RL-E | E/F | MH | SF | Pain | GH |
| Baseline | 44.8/40 | 23.6/0 | 50.5/33 | 34.8/45 | 65.2/68 | 63.1/63 | 55.6/65 | 45.3/46 |
| Follow up | 62.4/65 | 54.8/50 | 66.7/100 | 54/50 | 84.1/92 | 90.7/100 | 61.2/60 | 63.4/65 |
| Δ Mean (95%CI) | 17.5 (8-27) | 31.2 (6-57) | 16.2 (-8 to 40) | 19.2 (8-31) | 18.7 (9-29) | 27.7 (16-40) | 5.6 (-11 to 23) | 18 (10-26) |
| P value | 0.003 | 0.017 | 0.178 | 0.002 | 0.001 | 0.0001 | 0.52 | 0.0001 |
| Domain | Predictor | Coefficient | P value | CI lower | CI upper | R2d |
| PF change1 | Age | 0.496799029 | 0.5493559 | -1.1865686 | 2.18016665 | 0.048581685 |
| PF change | Gender | 7.609259284 | 0.5615835 | -18.989681 | 34.2082 | 0.048581685 |
| PF change | Hb | 1.963534859 | 0.4963046 | -3.8858508 | 7.81292048 | 0.048581685 |
| RLP change | Age | -0.144349859 | 0.9149046 | -2.894301 | 2.60560127 | 0.246642284 |
| RLP change | Gender | 36.69853355 | 0.0943931 | -6.7535241 | 80.1505912 | 0.246642284 |
| RLP change | Hb | 7.170977096 | 0.1350192 | -2.3845854 | 16.7265396 | 0.246642284 |
| EF change | Age | 0.946169468 | 0.2363515 | -0.6583037 | 2.55064259 | 0.059013684 |
| EF change | Gender | -5.636567085 | 0.6514632 | -30.988894 | 19.7157594 | 0.059013684 |
| EF change | Hb | 1.086581889 | 0.6919798 | -4.4886602 | 6.66182399 | 0.059013684 |
| GH change | Age | -0.894963168 | 0.1269223 | -2.0616117 | 0.27168537 | 0.101928309 |
| GH change | Gender | 5.985909667 | 0.5103566 | -12.448338 | 24.420157 | 0.101928309 |
| GH change | Hb | -2.06762978 | 0.3041048 | -6.1215138 | 1.98625427 | 0.101928309 |
| MH change | Age | -0.607081002 | 0.3391156 | -1.8884905 | 0.67432848 | 0.212102758 |
| MH change | Gender | 21.07520033 | 0.0419478 | 0.82761193 | 41.3227887 | 0.212102758 |
| MH change | Hb | 0.489064312 | 0.823144 | -3.9635924 | 4.94172105 | 0.212102758 |
| SF change | Age | -0.390959905 | 0.6266197 | -2.0232674 | 1.24134754 | 0.135090432 |
| SF change | Gender | 20.2213016 | 0.1191332 | -5.5708357 | 46.0134389 | 0.135090432 |
| SF change | Hb | 1.068574657 | 0.7017204 | -4.6033865 | 6.74053578 | 0.135090432 |
| FSS change | Age | 0.312632 | 0.531044 | -0.70421 | 1.329473 | 0.158169 |
| FSS change | Gender | 7.96919 | 0.30262 | -7.66476 | 23.60314 | 0.158169 |
| FSS change | Hb | 2.272987 | 0.188219 | -1.19423 | 5.740201 | 0.158169 |
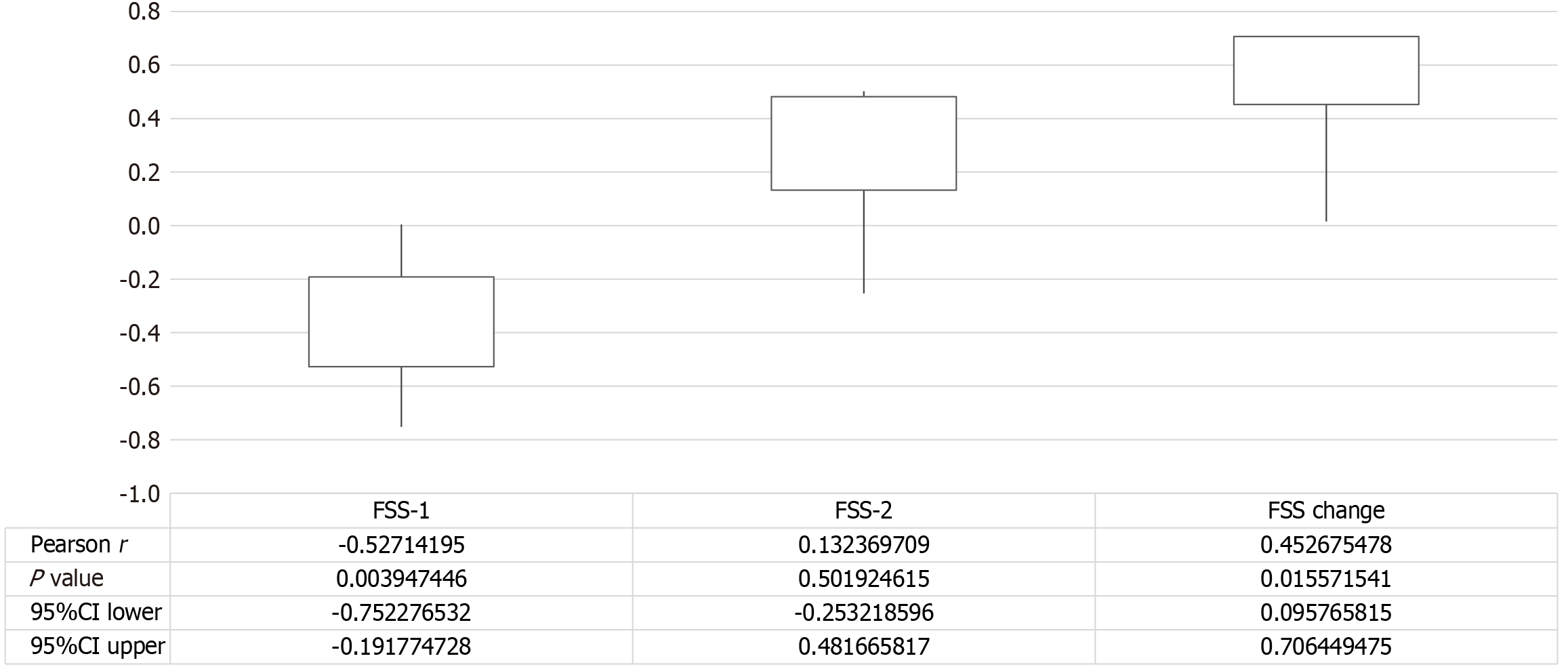
The median/mean values, SD and CIs for each of the five angiogenic factors for the whole cohort are shown in Table 3. There was no statistical association between any of the angiogenic factors and patient characteristics, part from an inverse relationship between haemoglobin level and Ang-1 values (Table 4). Of interest endostatin levels were negatively associated with baseline fatigue scores (r = -0.53, P = 0.004, 95%CI: -0.75 to -0.19) and positively affected the degree of change in FSS scores over time (r = 0.45, P = 0.016, 95%CI: 0.1-0.71; Figure 2). While a higher baseline Ang-1 was associated with less improvement in the role limitation physical domain, r = -0.051, P = 0.005, 95%CI: -0.74 to -0.21, this association did not persist when controlled for haemoglobin.
| Factor (dilution), pg/mL | Mean | Median | SD | 95%CI |
| Endostatin (1/5) | 2773.3 | 2763.9 | 417.3 | 2620-2926 |
| Ang-1 (1/2) | 598.8 | 497.9 | 394.8 | 435.9-743.64 |
| Ang-2 (1/50) | 15231.7 | 11514.5 | 11285.32 | 11092.3-19371.3 |
| VEGF (1/2) | 233.8 | 108.4 | 349.3 | 105.7-362.02 |
| Timp-1 (1/500) | 107269.3 | 78567.1 | 69069.6 | 81934.4-132604.2 |
| Angiogenic factor (dilution), pg/mL | Predictor | Coefficient | P value | R2 |
| Ang-1 (1/2) | Age | -3.9091 | 0.6688 | 0.2064 |
| Ang-1 (1/2) | Gender | 170.7615 | 0.2425 | 0.2064 |
| Ang-1 (1/2) | Hb | -79.3965 | 0.0178 | 0.2064 |
| Ang-2 (1/50) | Age | 45.1366 | 0.8759 | 0.0428 |
| Ang-2 (1/50) | Gender | 3435.2961 | 0.4542 | 0.0428 |
| Ang-2 (1/50) | Hb | 480.0491 | 0.6333 | 0.0428 |
| VEGF (1/2) | Age | 3.3534 | 0.6846 | 0.1569 |
| VEGF (1/2) | Gender | 98.5417 | 0.4517 | 0.1569 |
| VEGF (1/2) | Hb | 48.1964 | 0.1012 | 0.1569 |
| Endostatin (1/5) | Age | -2.7524 | 0.8002 | 0.0332 |
| Endostatin (1/5) | Gender | 66.3708 | 0.6996 | 0.0332 |
| Endostatin (1/5) | Hb | 20.2682 | 0.5926 | 0.0332 |
| Timp1 (1/500) | Age | 2216.3375 | 0.217 | 0.0677 |
| Timp1 (1/500) | Gender | -17153.681 | 0.5408 | 0.0677 |
| Timp1 (1/500) | Hb | 3417.3353 | 0.5793 | 0.0677 |
Our prospective study is the first to show BAE and intervention with APC for symptomatic SBA has a positive impact on patient reported fatigue and QoL domains relating to general health, physical functioning and role limitation associated with physical problems, as well as mental health and social functioning. Domains relating to pain and role limitation due to emotional problems were not affected, which is in keeping with the nature of the condition. The improvement in QoL parameters post BAE and APC remained significant on controlling for age, gender and baseline haemoglobin levels. Our findings are similar to previous studies assessing medical therapy[6].
The majority of patients included in our study had multiple lesions detected and treated on BAE, which may bias our study in favour of a good response to intervention. However, in our experience most patients presenting with sporadic SBA have multiple lesions in keeping with this cohort and as such our study reflects clinical practice[11]. In addition, we assessed the impact of therapy on QoL and fatigue in patients referred for BAE and intervention only. It is assumed that some patients with isolated, difficult to reach, or less significant, P1 lesions or those with significant comorbidity precluding enteroscopy were not included. As such, our data cannot be extrapolated to suggest all SBA patients would benefit from BAE and APC.
As patients included were referred after a positive capsule endoscopy with known SBA, it is assumed all were already on supportive care, which accounts for the finding of a median baseline haemoglobin level of 11.1 g/dL. Similarly, there was no specific instruction given post BAE and intervention regarding monitoring or ongoing supportive care. As such, the impact of ongoing iron supplements, or transfusions and degree of local monitoring cannot be assessed. Unlike other studies of medical therapy, which allowed endoscopic intervention as required, adjuvant medical treatment including somatostatin anlogues were excluded in our cohort, to allow us to specifically assess the effect of enteroscopy and APC on QoL and FSS. The impact of combined endoscopic and medical therapy is therefore beyond the scope of our paper. Of note haemoglobin level alone should not be taken as a reason to defer BAE and APC, as the majority of patients in our study benefited from endoscopic ablation, irrespective of haemoglobin.
In general, the majority of angiogenic factors previously associated with sporadic SBA did not correlate with changes in either SF-36 scores or FSS scale[12-15]. While the relatively small sample size and lack of control group could account for this, our findings may simply reflect the fact that these factors are altered in response to a systemic driver, linked to SBA pathogenesis, such as hypoperfusion or hypoxia, which is not altered by endoscopic intervention. In addition, ongoing angiogenic abnormalities likely account for the high rate of recurrent disease and need for re-intervention. As such, targeted interventions against these factors should remain an ongoing focus of investigation, in an attempt to alter the natural history of the disease. In contrast to other factors, endostatin, a protein known to have anti-angiogenic effects, and under investigation as a cancer therapy, had a statistically significant effect on fatigue. Our preliminary data suggests higher endostatin levels may be linked with lower baseline and greater improvements in FSS scores, suggesting a possible protective role in our SBA cohort. Our findings suggest endostatin warrants further examination and validation as an independent biomarker of disease and potential treatment target, in larger multicenter translational as well as basic science studies.
The virtual nature of our follow up, a telephone call rather than physical appointment, to accommodate patients re
The median time to follow up in our cohort was only 7.8 months which is likely to be too short to evaluate both the long term impact of treatment on QoL as well as disease recurrence. Reported recurrence rates are significant, 80% with a mean time to representation of 10.7 months in a previous cohort of ours[11]. Of note, no one in our cohort needed re-intervention over the study period. It would be of interest to reassess the impact of retreatment with BAE and APC on this cohort.
Our study has shown BAE and ablation of SBA significantly improves fatigue and related QoL, independently of demo
| 1. | Becq A, Sidhu R, Goltstein LCMJ, Dray X. Recent advances in the treatment of refractory gastrointestinal angiodysplasia. United European Gastroenterol J. 2024;12:1128-1135. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 10] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 2. | García-Compeán D, Del Cueto-Aguilera ÁN, Jiménez-Rodríguez AR, González-González JA, Maldonado-Garza HJ. Diagnostic and therapeutic challenges of gastrointestinal angiodysplasias: A critical review and view points. World J Gastroenterol. 2019;25:2549-2564. [PubMed] [DOI] [Full Text] |
| 3. | Sidhu R, Shiha MG, Carretero C, Koulaouzidis A, Dray X, Mussetto A, Keuchel M, Spada C, Despott EJ, Chetcuti Zammit S, McNamara D, Rondonotti E, Sabino J, Ferlitsch M; External Voting Panel. Performance measures for small-bowel endoscopy: a European Society of Gastrointestinal Endoscopy (ESGE) Quality Improvement Initiative - Update 2025. Endoscopy. 2025;57:366-389. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 15] [Article Influence: 15.0] [Reference Citation Analysis (1)] |
| 4. | Borgaonkar MR, Irvine EJ. Quality of life measurement in gastrointestinal and liver disorders. Gut. 2000;47:444-454. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 162] [Cited by in RCA: 142] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 5. | Grooteman KV, Matheeuwsen M, van Geenen EJM, Drenth JPH. Decreased health-related quality of life in angiodysplasia patients: A cross-sectional cohort. PLoS One. 2017;12:e0177522. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 7] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 6. | Goltstein LCMJ, Grooteman KV, Bernts LHP, Scheffer RCH, Laheij RJF, Gilissen LPL, Schrauwen RWM, Talstra NC, Zuur AT, Braat H, Hadithi M, Brouwer JT, Nagengast WB, Oort FA, Tenthof van Noorden J, Kievit W, van Geenen EJM, Drenth JPH. Standard of Care Versus Octreotide in Angiodysplasia-Related Bleeding (the OCEAN Study): A Multicenter Randomized Controlled Trial. Gastroenterology. 2024;166:690-703. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 22] [Article Influence: 11.0] [Reference Citation Analysis (2)] |
| 7. | Holleran G, Hall B, O'Regan M, Smith S, McNamara D. Expression of Angiogenic Factors in Patients With Sporadic Small Bowel Angiodysplasia. J Clin Gastroenterol. 2015;49:831-836. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 37] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 8. | Holleran G, Hussey M, Smith S, McNamara D. Assessment of serum angiogenic factors as a diagnostic aid for small bowel angiodysplasia in patients with obscure gastrointestinal bleeding and anaemia. World J Gastrointest Pathophysiol. 2017;8:127-132. [PubMed] [DOI] [Full Text] |
| 9. | Holleran G, Smith S, Mcnamara D. Identification of novel circulating angiogenic factors in small bowel angiodysplasia: a further step towards delineating the pathophysiology and defining treatment targets. 2019 Preprint. [DOI] [Full Text] |
| 10. | McHorney CA, Ware JE Jr, Raczek AE. The MOS 36-Item Short-Form Health Survey (SF-36): II. Psychometric and clinical tests of validity in measuring physical and mental health constructs. Med Care. 1993;31:247-263. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5083] [Cited by in RCA: 4574] [Article Influence: 138.6] [Reference Citation Analysis (3)] |
| 11. | Valko PO, Bassetti CL, Bloch KE, Held U, Baumann CR. Validation of the fatigue severity scale in a Swiss cohort. Sleep. 2008;31:1601-1607. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 560] [Cited by in RCA: 469] [Article Influence: 26.1] [Reference Citation Analysis (1)] |
| 12. | Schreiner P, Rossel JB, Biedermann L, Valko PO, Baumann CR, Greuter T, Scharl M, Vavricka SR, Pittet V, Juillerat P, Rogler G, von Känel R, Misselwitz B; Swiss IBD Cohort Study Group. Fatigue in inflammatory bowel disease and its impact on daily activities. Aliment Pharmacol Ther. 2021;53:138-149. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 44] [Article Influence: 8.8] [Reference Citation Analysis (0)] |
| 13. | Holleran G, Hall B, Zgaga L, Breslin N, McNamara D. The natural history of small bowel angiodysplasia. Scand J Gastroenterol. 2016;51:393-399. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 30] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 14. | Albitar HAH, Almodallal Y, Papadakis KA, Rajan E, Kamath PS, Iyer VN. Intravenous Bevacizumab Reduces Transfusion Requirements and Endoscopic Interventions in Patients With Gastric Antral Vascular Ectasia and Small Bowel Angioectasia. Gastroenterology. 2020;158:1162-1163.e4. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 26] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 15. | Chen H, Wu S, Tang M, Zhao R, Zhang Q, Dai Z, Gao Y, Yang S, Li Z, Du Y, Yang A, Zhong L, Lu L, Xu L, Shen X, Liu S, Zhong J, Li X, Lu H, Xiong H, Shen Y, Chen H, Gong S, Xue H, Ge Z. Thalidomide for Recurrent Bleeding Due to Small-Intestinal Angiodysplasia. N Engl J Med. 2023;389:1649-1659. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 44] [Article Influence: 14.7] [Reference Citation Analysis (1)] |