Published online Mar 26, 2026. doi: 10.12998/wjcc.v14.i9.118016
Revised: January 31, 2026
Accepted: March 4, 2026
Published online: March 26, 2026
Processing time: 75 Days and 16.8 Hours
A teratoma is a primary germ cell tumor composed of ectodermal, endodermal, and mesodermal layers. The vast majority are mature, benign neoplasms, most commonly found in the sacrococcygeal region or ovaries; mediastinal teratomas are rare in children.
We report a 12-year-old boy who presented with nonspecific left subcostal pain and general malaise for six months. Imaging revealed a giant mediastinal mass, and the patient underwent surgical resection with full recovery. Histopathological examination confirmed a mature mediastinal teratoma.
This case highlights the value of diagnostic imaging in evaluating mediastinal tumors and emphasizes the im
Core Tip: We describe a rare case of a giant mature anterior mediastinal teratoma in a 12-year-old boy presenting with prolonged left subcostal pain without respiratory symptoms. Contrast-enhanced computed tomography revealed a massive mediastinal tumor with significant mass effect. Complete surgical resection resulted in full recovery, and histopathology confirmed a benign mature teratoma. This case highlights the need to consider mediastinal tumors in children with persistent, unexplained thoracoabdominal pain and underscores the key role of imaging and surgery in achieving favorable outcomes.
- Citation: Loor CS, Macias Fernandez PK, Blasco Arriaga EE, Custodio LE, Bombón Caizaluisa MF, Ross Rodriguez EA, Pozo Albán MI, Grochowska A, Gagliardo Cadena EA. Hidden giant - atypical pediatric anterior mediastinal teratoma: A case report. World J Clin Cases 2026; 14(9): 118016
- URL: https://www.wjgnet.com/2307-8960/full/v14/i9/118016.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i9.118016
Mature teratoma is a tumor containing the three germ layers: Ectodermal, endodermal, and mesodermal[1]. The great majority of teratomas are mature, benign neoplasms. The incidence is 1 in 4000 live births worldwide, with both sexes equally affected. The most common sites of presentation are the sacrococcygeal (40%), ovary (25%), testis (12%), brain (5%), and, in fewer cases, other sites such as the neck and mediastinum (18%)[2].
It is most commonly found in children either incidentally or with symptoms of compression due to mass effect, such as chest pain, cough, dysphagia, and respiratory distress[3]. The unusual pain in the chest can also lead to the diagnosis of teratoma. Any atypical chest symptom should prompt further diagnosis. The diagnostic method of choice is contrast-enhanced computed tomography (CT). However, the differential diagnosis includes malignant mediastinal tumors in children, such as thymoma, lymphoma, leukemia, and other germ cell tumors, so it is necessary to confirm the diagnosis through biopsy. Tumor markers like alpha-fetoprotein (AFP) and human chorionic gonadotropin can also be used to confirm a malignant component[4]. This pathology may present complications such as cardiac tamponade, fistulization to the skin, and malignant transformation, so the definitive treatment is surgical resection[5,6]. While mature teratomas are usually benign and often present in the abdominal region, the presence of mediastinum, especially in pediatric patients, is rare. Even more unusual are the prolonged symptoms, left subcostal pain for months, combined with general malaise, with a lack of typical respiratory symptoms associated with the tumor. This case is also unique due to the large size of the tumor itself. This rare clinical presentation highlights the importance of imaging diagnostics and the inclusion of mediastinal tumors as a differential diagnosis of persistent, unexplained thoracoabdominal pain in children. This case was prepared in accordance with the CARE guidelines for case reports.
A 12-year-old boy presented with persistent left subcostal pain associated with general malaise for six months.
The patient reported a six-month history of progressive left subcostal pain, accompanied by intermittent knee pain and generalized fatigue. There were no prominent respiratory symptoms such as cough, dyspnea, or chest tightness. Initial evaluation at an outside hospital revealed an anterior mediastinal mass on imaging studies. The patient received three cycles of chemotherapy (TCG GALOP 2017 protocol) for unclear indications before being referred to our institution for further management.
The patient had no significant past medical history, no previous surgeries, and no known chronic illnesses.
There was no relevant family history of malignancy or genetic disorders. The patient had no known toxic exposures or relevant personal habits.
On admission, vital signs were within normal limits for age. Physical examination revealed markedly decreased breath sounds in the left lung field. No lymphadenopathy, hepatosplenomegaly, or peripheral edema was noted.
Serum tumor markers were within normal limits: AFP: 1.50 UI/mL (normal range: 1.00-7.00 UI/mL); beta-human chorionic gonadotropin (β-HCG): 0.32 mUI/mL (normal range: 0.0-2.00 mUI/mL); biochemical analysis of fluid aspirated from the mediastinal mass showed elevated adenosine deaminase and lactate dehydrogenase levels with very low glucose concentration, suggestive of an inflammatory process but without evidence of malignancy.
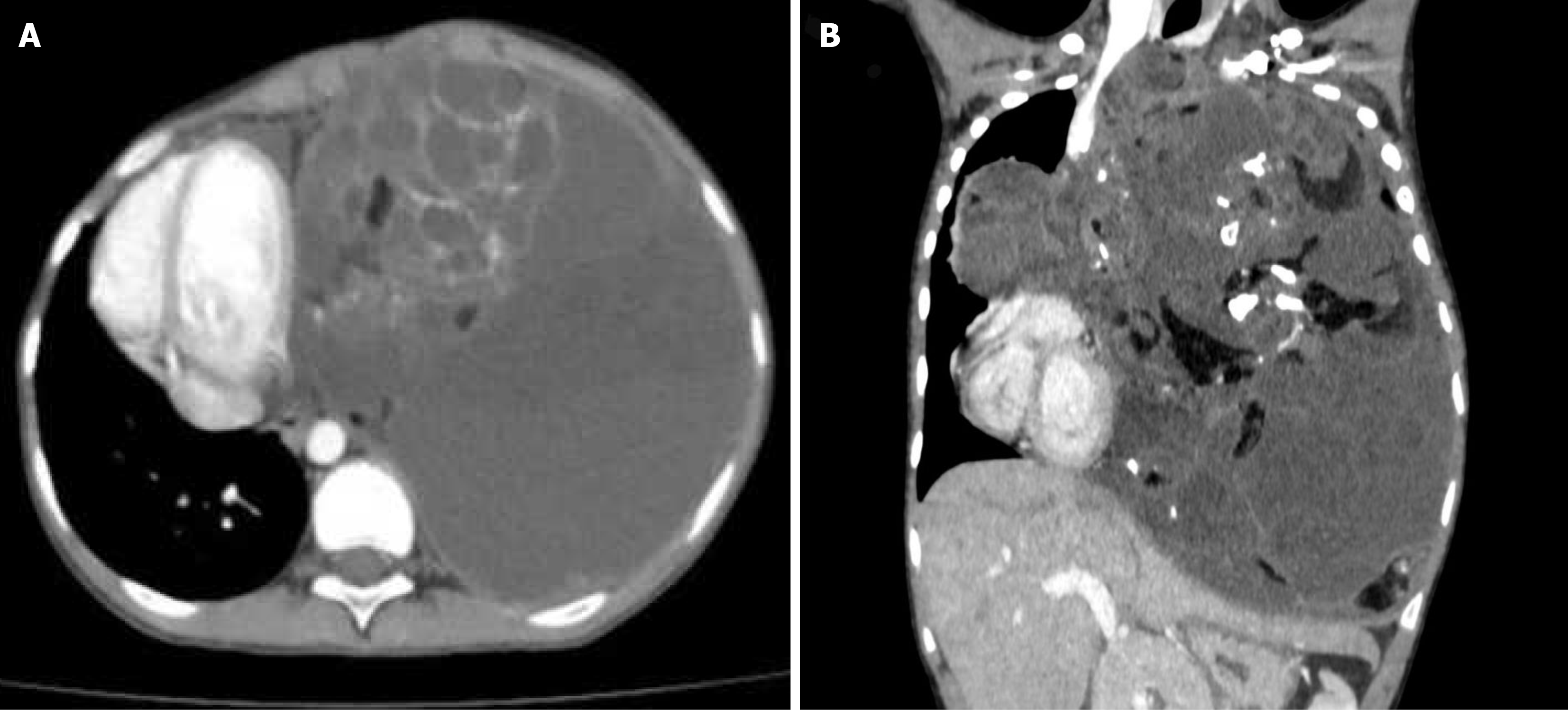
Contrast-enhanced chest CT demonstrated a giant anterior mediastinal mass measuring 24 cm × 16.5 cm × 22 cm, with heterogeneous solid and cystic components, areas of fat density, and multiple calcifications (Figure 1). The mass caused significant displacement of mediastinal structures, including the heart, great vessels, trachea, esophagus, and left lung, with compression of approximately 90% of the left lung parenchyma.
Giant mature anterior mediastinal teratoma.
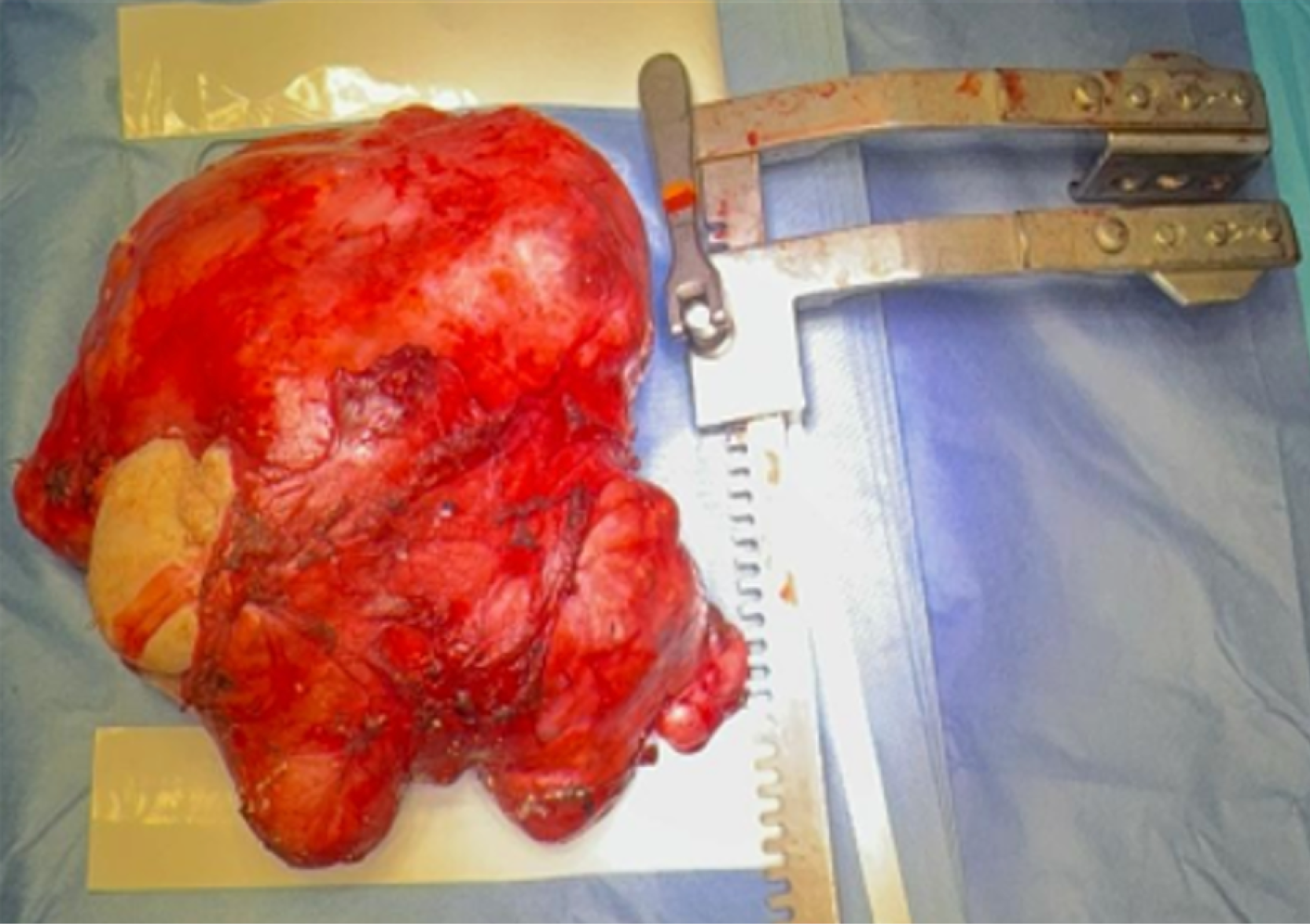
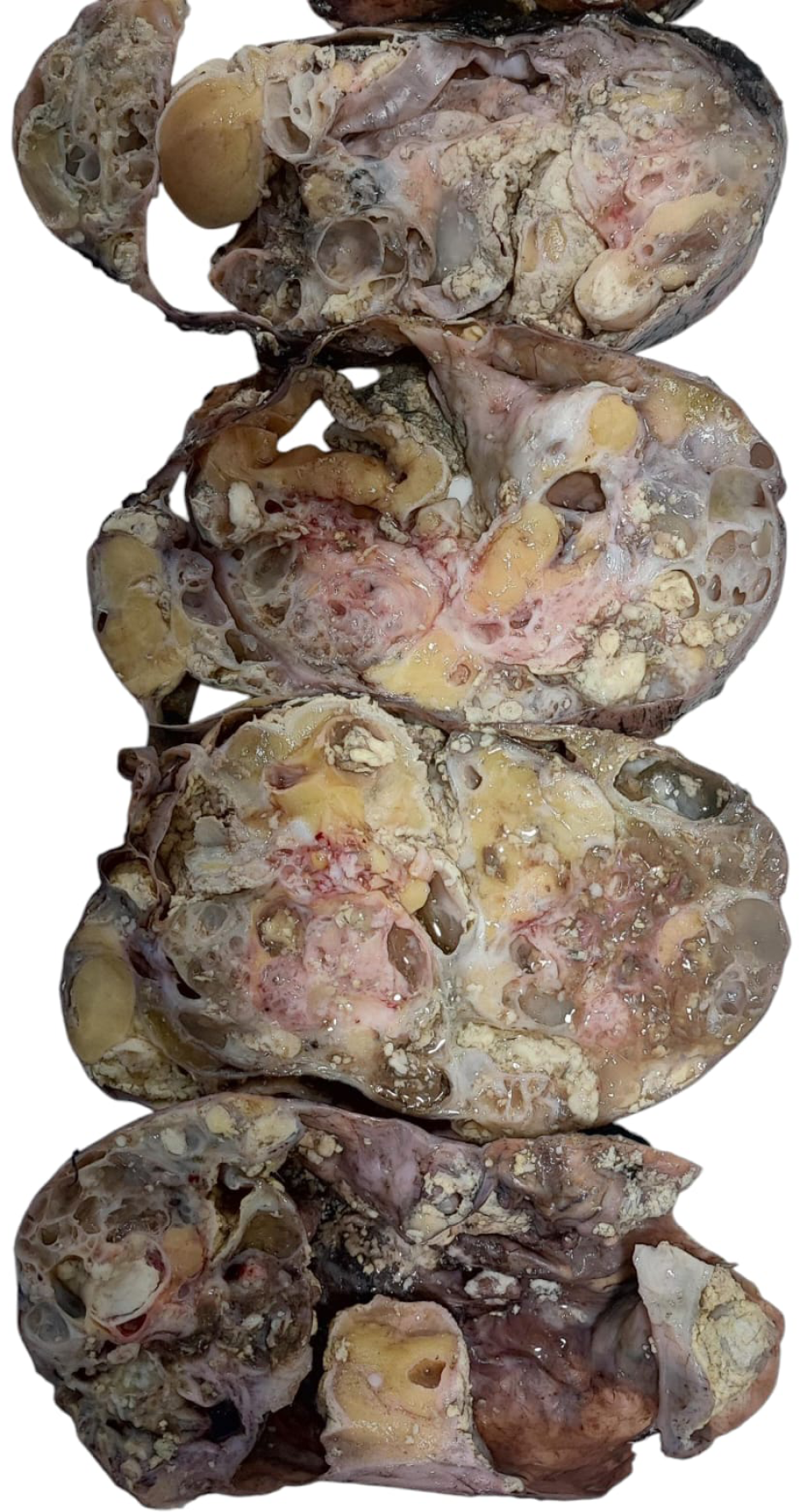
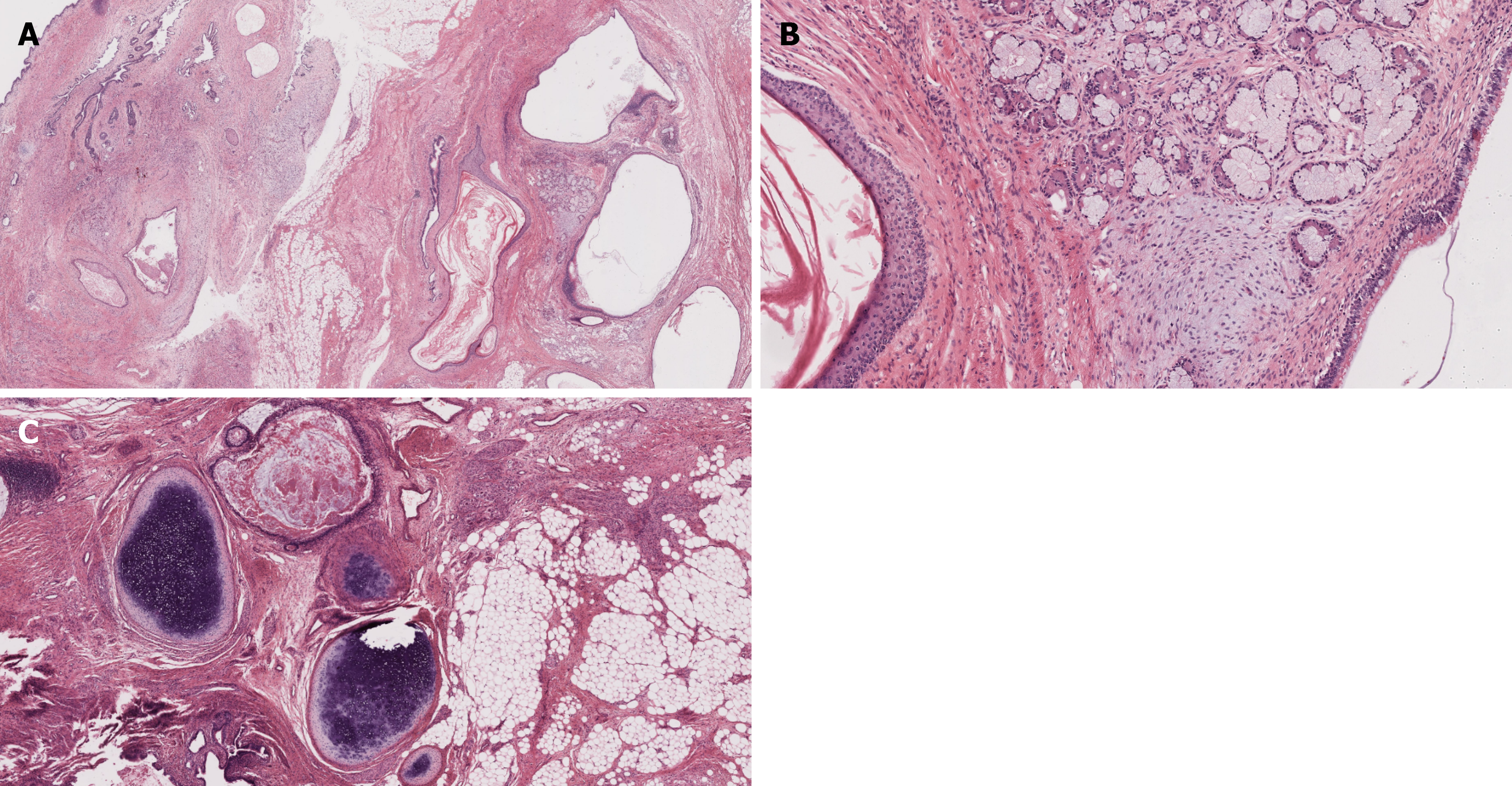
Despite benign histological findings, the patient received two additional cycles of salvage chemotherapy prior to surgery, without radiological response. Definitive management consisted of complete surgical resection via median sternotomy. Intraoperatively, a large multilobulated mass occupying the entire mediastinum and both hemithorax was removed. A minor intraoperative injury to the innominate vein was repaired successfully (Figures 2, 3 and 4).
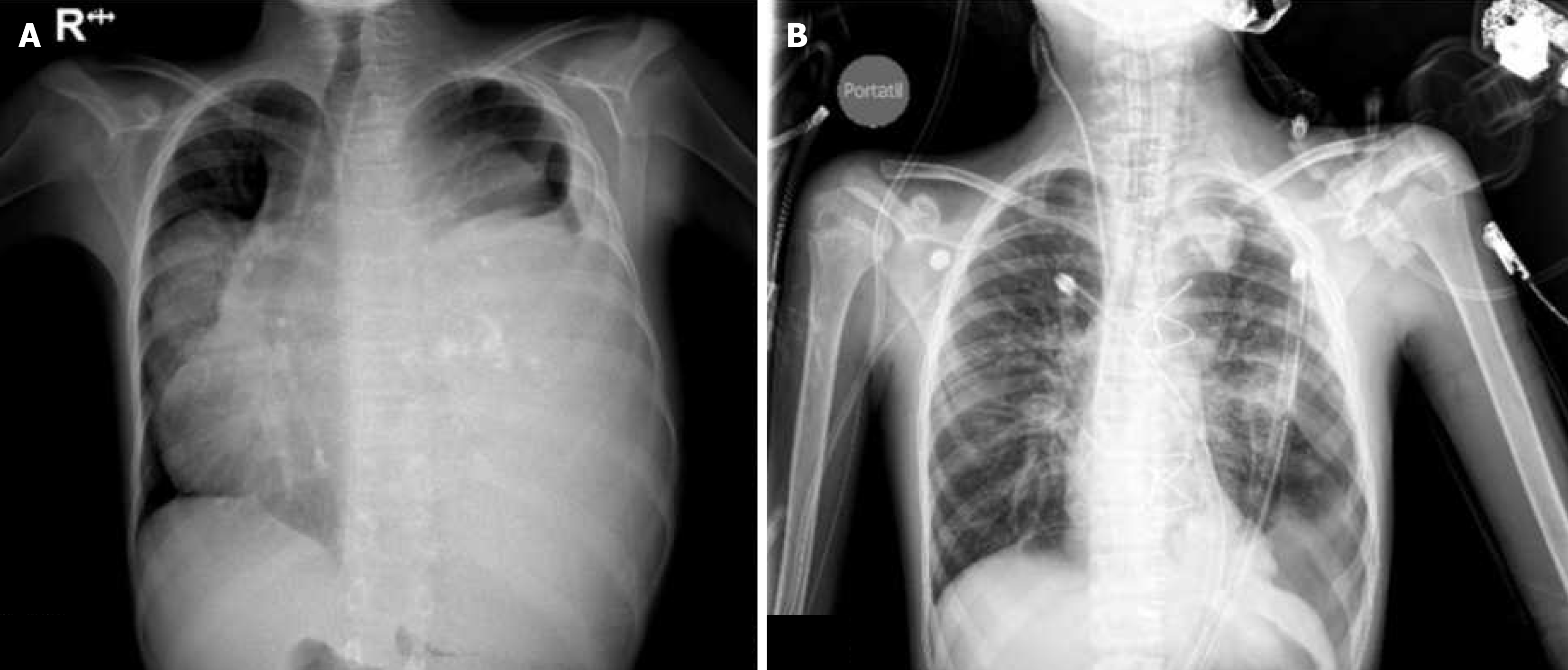
The patient was admitted to the pediatric intensive care unit postoperatively and had an uneventful recovery. Postoperative chest radiographs showed no complications. He was discharged two weeks after surgery in good con
This case highlights an unusual presentation of a giant mediastinal teratoma in a child, presenting with left subcostal pain, a symptom rarely reported in such tumors. While mediastinal teratomas are generally benign and composed of all three germ layers, their location in the anterior mediastinum is uncommon in pediatric patients. Most reported cases describe respiratory symptoms, cough, or chest discomfort rather than localized abdominal or subcostal pain.
Teratoma is a benign tumor composed of all three germ layers. It is divided into benign mature teratoma, malignant immature teratoma, and teratoma with other malignant germ cell tumor components (such as yolk sac tumor, choriocarcinoma, embryonal carcinoma, and seminoma). Its location in the anterior mediastinum is one of the less common sites, most frequently affecting children. A tumor of this size is a rare finding that should be differentiated from other types of malignant pathologies, such as thymoma, leukemia, and lymphoma, as they tend to present in the same location.
The duration of atypical pain in our case was 6 months. Such tumors tend to grow and progressively produce symptoms, mainly from the pressure of the tumor on adjacent organs (mass effect). In the scientific data, Kebalo et al[4] described a case of a 10-year-old girl with persistent chest pain evolving for 16 days, and the cause was also a mature teratoma of the anterior mediastinum. Also, a 13-month-old girl described by Arega et al[7] had a one-month history of dry cough, progressive respiratory distress with rapid breathing, and night sweats and was operated on for mediastinal teratoma. In an older child, mediastinal teratomas as large as 25 cm have been described, often causing significant mediastinal compression[8]. Compared with these reports, our case demonstrates a longer symptomatic period with atypical presentation, emphasizing the variability in clinical manifestations and the need for vigilance.
The diagnosis can be made with chest CT. Magnetic resonance imaging is done when spinal involvement is suspected or to avoid radiation in children, and a positron emission tomography scan should be considered when malignant transformation is suspected. Definitive diagnosis, however, requires histopathological confirmation via biopsy.
A particularly relevant aspect of this case is the administration of systemic chemotherapy despite histopathological findings suggestive of a mature teratoma and benign cytology. Although the biochemical profile of the mediastinal fluid, including markedly elevated adenosine deaminase and lactate dehydrogenase levels, extremely low glucose concentration, and mild β-HCG elevation, may raise concern for an aggressive or malignant process, these findings are non
The histopathological study confirmed the diagnosis of a mature teratoma with no malignant components, correlating with an excellent prognosis of over 96% survival rate[3]. No protocol of post-surgical chemotherapy was implemented, as the nature of the tumor is benign.
In summary, this case adds to the pediatric literature by illustrating a giant anterior mediastinal teratoma with atypical subcostal pain and prolonged symptom duration. Early recognition of such clinical presentations and timely surgical management are crucial for optimal outcomes in this population.
Mature teratomas of the anterior mediastinum are rare tumors in children but should always be considered as a differential diagnosis in thoracoabdominal pain with general malaise. However, early diagnosis and prompt surgical intervention are typically associated with a favorable survival prognosis.
The authors would like to thank the pediatric surgery and radiology teams of Sociedad de Lucha Contra el Cáncer (SOLCA Guayaquil) for their valuable collaboration in the diagnosis and management of this patient.
| 1. | Cong L, Wang S, Yeung SY, Lee JHS, Chung JPW, Chan DYL. Mature Cystic Teratoma: An Integrated Review. Int J Mol Sci. 2023;24:6141. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 62] [Reference Citation Analysis (0)] |
| 2. | Anand S, Longia S, Agarwal N, Maheshwari M, Apte A, Pathak K. Mature mediastinal teratoma: a rare cause of recurrent respiratory distress. Peoples J Sci Res. 2010;3:33-35. |
| 3. | AlHarbi KM, Sairafi MH, Almuzaini SA. Mature cystic teratoma of mediastinum compressing the right atrium in a child: A rare case report. J Taibah Univ Med Sci. 2017;12:555-560. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 4. | Kebalo S, Lamboni D, Guedenon K, Amegbor K, Gnassingbe K. Mature teratoma of the mediastinum in children: A case revealed by persistent chest pain. Pediatr Surg Case Rep. 2022;78:102209. [RCA] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 5. | Al Smady M, Zahari NNB, Mohd Sahid NSB, Saparudin NSB. Anterior mediastinal teratoma with pericardial effusion. Rare presentation. J Surg Case Rep. 2019;2019:rjz136. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 11] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 6. | Ouadnouni Y, Serraj M, El Fatemi H, Ghalimi J, Lakranbi M, Smahi M. Tératomes matures du médiastin. J Afr Cancer. 2014;6:224-227. [DOI] [Full Text] |
| 7. | Arega G, Bekele N, Hailu D, Omer F, Negussie MA, Negussie T. Anterior mediastinal mature teratoma in a 13-month-old girl: A case report. J Pediatr Surg Case Rep. 2025;114:102958. [DOI] [Full Text] |
| 8. | Liew WX, Lam HY, Narasimman S, Navarasi S, Mohd Hamzah K. Mediastinal mature teratoma in a child- A case report. Med J Malaysia. 2016;71:32-34. [PubMed] |
| 9. | Kojima M, Touge R, Kurihara S, Saeki I, Takahashi S. Successful mediastinal teratoma resection in a child by assisted VATS: a case report. J Cardiothorac Surg. 2024;19:511. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 10. | Khanna K, Agarwala S, Bishoi AK, Bakhshi S, Bhatnagar V. Management and long-term outcomes of giant mediastinal germ cell tumors in children. Indian J Med Paediatr Oncol. 2019;40:515-520. [RCA] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 11. | Olanisa O, Westfall J, Stewart B, moldovan T, Topalli X, Kaur J, Shabahang B. Superior Vena Cava Syndrome Due to Mediastinal Teratoma. Am J Resp Crit Care. 2024;209:A4671. [DOI] [Full Text] |
| 12. | Holland AJA. A case of matured mediastinal teratoma complicated by cardiac tamponade: an unusual aetiology. J Pediatr Surg. 2011;46:1676-1677. [DOI] [Full Text] |