Published online Mar 16, 2026. doi: 10.12998/wjcc.v14.i8.117957
Revised: January 9, 2026
Accepted: February 27, 2026
Published online: March 16, 2026
Processing time: 84 Days and 6.9 Hours
Ectopic pregnancy (EP) is rarely associated with congenital Müllerian anomalies, such as unicornuate uterus and undescended fallopian tube pregnancy. When EP occurs in extra-pelvic locations like the subhepatic space, diagnosis is often chall
We report a rare case of a 28-year-old woman presenting with subhepatic EP. Symptoms included amenorrhea, intermittent right upper abdominal pain, and elevated serum beta human chorionic gonadotropin (β-hCG) level (4087.42 mIU/mL). Transvaginal ultrasound was non-diagnostic, failing to locate the gestational sac or right adnexa. Crucially, large-field-of-view (LFOV) magnetic resonance imaging (MRI) localized the ectopic sac between the inferior hepatic edge and right iliac fossa. Laparoscopy confirmed tubal EP within an undescend
This case underscores the critical diagnostic utility of LFOV MRI in accurately pinpointing extra-pelvic EP when pelvic ultrasound is negative and β-hCG is high, particularly essential in complex cases involving congenital Müllerian ano
Core Tip: Large-field-of-view magnetic resonance imaging (MRI) is a necessary problem-solving tool for rare extra-pelvic ectopic pregnancy (e.g., subhepatic) when transvaginal ultrasound is inconclusive in patients with Müllerian anomalies. MRI’s comprehensive anatomical coverage is crucial for early and accurate localization.
- Citation: Huang WJ, Zhao XR, Cao YQ, Huang XZ, Lai WL, Xi Y, Wu HY. Subhepatic ectopic pregnancy in Müllerian anomaly localized by large-field-of-view magnetic resonance imaging: A case report. World J Clin Cases 2026; 14(8): 117957
- URL: https://www.wjgnet.com/2307-8960/full/v14/i8/117957.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i8.117957
Müllerian duct anomalies represent the most common congenital female genital tract malformations, with an incidence of 3.4%-5%. The unicornuate uterus comprises 2.5%-13.2% of these anomalies and is associated with an approximate 4% ectopic pregnancy (EP) rate. Contrary, EP in an undescended fallopian tube is exceedingly rare. This report details an exceptional case of EP occurring within an undescended fallopian tube located subhepatically, emphasizing the value of large-field-of-view (LFOV) magnetic resonance imaging (MRI) in this diagnostic challenge.
A 28-year-old female presented with amenorrhea > 7 weeks, intermittent right upper abdominal pain (0.5 month), and subsequent vaginal bleeding/tissue discharge (3 days).
The patient denied any symptoms such as fever, vomiting, or acute, severe abdominal pain prior to the presentation of vaginal bleeding and tissue discharge. Her symptoms of right upper abdominal discomfort had been persistent for two weeks, escalating the clinical suspicion of an ectopic event.
There was no past illness.
There was no significant personal and family history.
At admission, physical examination revealed moderate vaginal discharge with a small amount of retained blood. There was no tenderness on lifting or rocking the cervix, and no tenderness was noted in the uterine body or bilateral adnexa.
Upon admission, continuous monitoring of laboratory tests significantly confirmed elevated serum beta human chorionic gonadotropin (β-hCG) levels at 4087.42 mIU/mL. The progesterone level was 6.09 ng/mL.
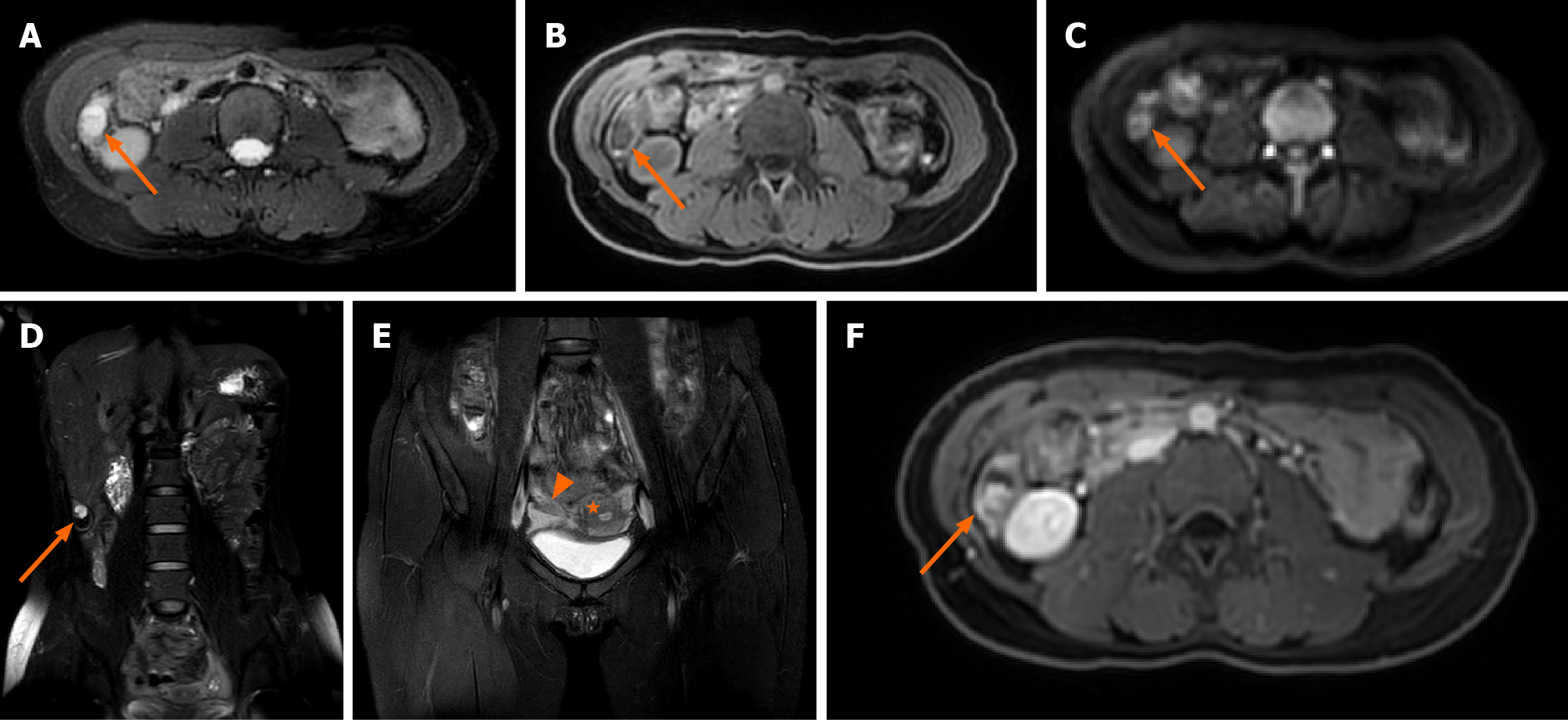
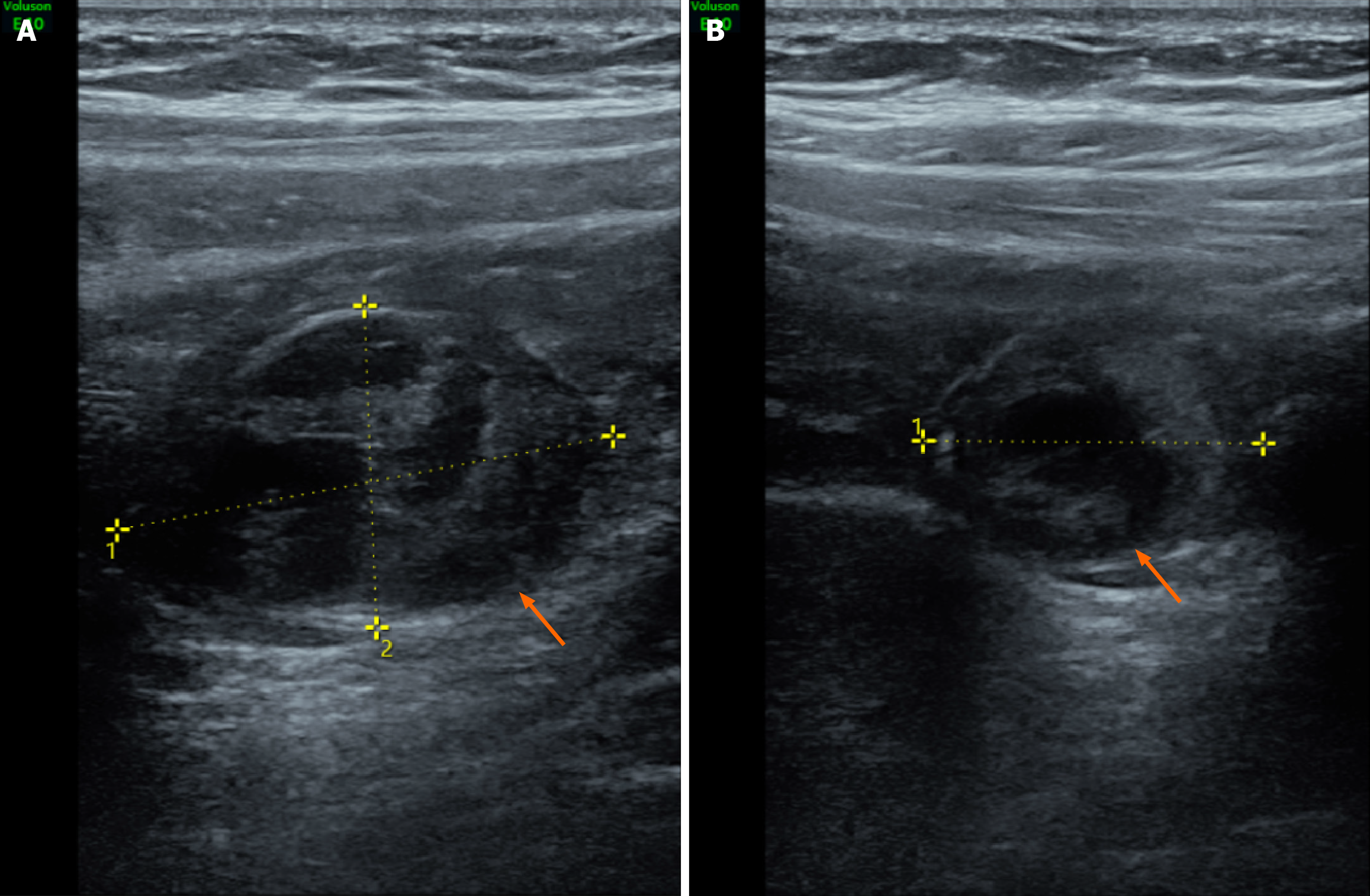
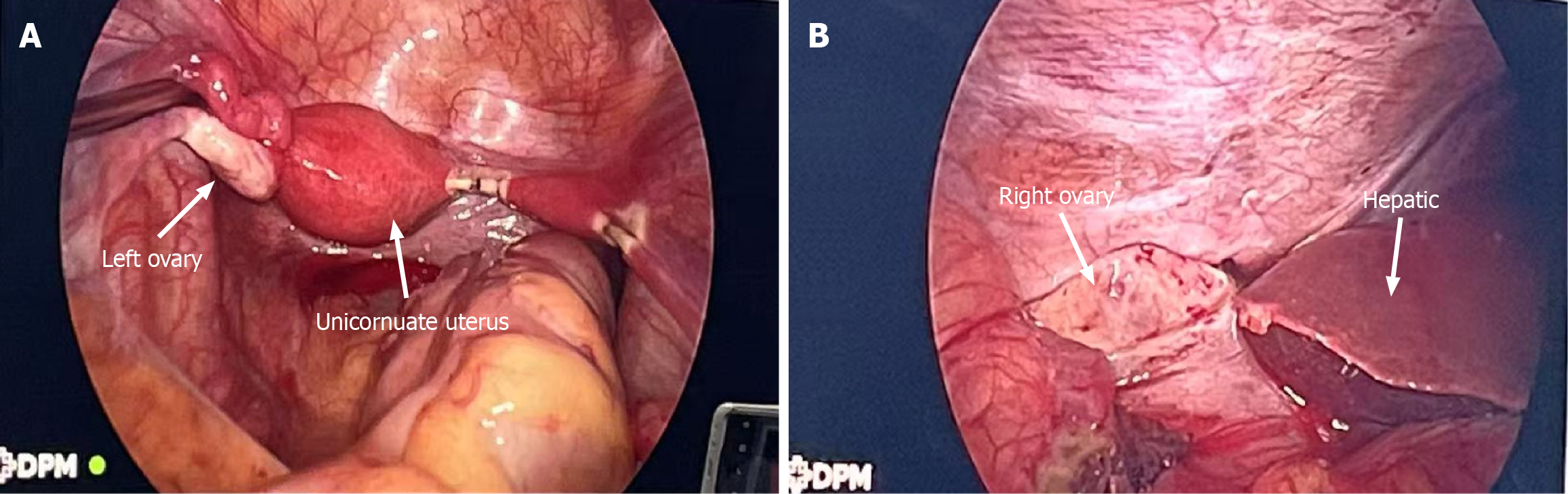
MRI of a 28-year-old pregnant woman with surgically and pathologically confirmed unruptured tubal ectopic pregnancy (Figure 1). Axial T2-weighted fat-suppressed image shows a small nodular hyperintense focus (arrow) within the gestational sac. Axial T1-weighted image demonstrates the nodule with isointense signal relative to muscle. Diffusion-weighted image (b-value = 800 s/mm²) shows no restricted diffusion within the lesion. The coronal magnetic resonance image of the entire abdomen shows that the gestational sac is located between the lower edge of the right lobe of the liver and the right iliac fossa. Coronal T2-weighted image confirms uterine morphology consistent with a left unicornuate uterus and a right rudimentary horn. The uterus is deviated toward the left pelvic sidewall. Axial contrast-enhanced T1-weighted fat-suppressed image reveals vivid enhancement of the nodule and mild enhancement of the cyst wall. Targeted transabdominal ultrasound, performed with MRI guidance, identifies the ectopic gestational sac in the right upper abdomen, within the subhepatic region (Figure 2). Intraoperative and histopathological correlation (Figure 3). Laparoscopic view showing a left unicornuate uterus and normal left ovary within the pelvic cavity. Intraoperative photograph shows the ectopic fallopian tube and ovary (arrow) displaced to the right upper abdomen, firmly adherent to the inferior hepatic surface and capsule.
Tubal ectopic pregnancy within an undescended right fallopian tube, associated with a left unicornuate uterus and a contralateral rudimentary horn.
Laparoscopic right salpingectomy and excision of gestational tissue were performed. Intraoperative findings included hemoperitoneum, and the right fallopian tube/ovary were adhered to the inferior liver surface/abdominal wall. The sac was in the ampullary portion of the undescended tube. Histopathology confirmed tubal pregnancy (chorionic villi present).
The patient’s surgical course was uneventful, and she experienced a complete resolution of her symptoms. Her serum β-hCG levels normalized (became negative) within two weeks of the surgery.
The developmental complexity of Müllerian duct anomalies, such as the unicornuate uterus, frequently poses significant diagnostic challenges. A unicornuate uterus results from the developmental failure or arrested growth of one paramesonephric duct, often accompanied by ipsilateral renal agenesis in approximately 28% of cases[1,2]. The rare phenomenon of an undescended ovary and fallopian tube is hypothesized to stem from a failure of the gubernaculum to guide the descent of the urogenital ridge, leading to ectopic adnexal structures located far above the pelvic brim. In the present case, the subhepatic location of the EP underscores the possibility of transperitoneal gamete migration into an undescended tube[3,4]. While transvaginal ultrasound remains the first-line diagnostic tool for EP, its diagnostic efficacy is strictly limited by its field of view (FOV). In cases of undescended adnexa, the gestational sac typically lies beyond the reach of a standard vaginal probe, which often leads to a false-negative pelvic scan despite significantly elevated β-hCG levels.
When ultrasound is inconclusive, the choice of cross-sectional imaging becomes critical. Computed tomography (CT) is a widely accessible alternative in many emergency departments and holds significant value in identifying hemoperitoneum or clarifying gross anatomy when MRI is unavailable. However, CT’s utility in early pregnancy is limited by concerns regarding ionizing radiation and its relatively inferior soft-tissue contrast compared to MRI. MRI is superior in characterizing the internal components of a gestational sac and its precise relationship to complex Müllerian malformations, providing a safer and more detailed preoperative map[5].
The success of the diagnosis in this case was specifically attributed to the application of LFOV MRI. Standard pelvic MRI protocols focus on the true pelvis to achieve high spatial resolution of the uterine morphology; however, this narrow focus carries the risk of missing extra-pelvic pathologies. As demonstrated in this patient, a conventional pelvic FOV would likely have failed to capture the subhepatic gestational sac, potentially leading to catastrophic delays in treatment. However, LFOV imaging is not without technical trade-offs. Expanding the FOV generally requires a compromise in spatial resolution or an increase in acquisition time to maintain an adequate signal-to-noise ratio. To balance these factors, we suggest a clinical protocol wherein high-resolution pelvic sequences are first used to define uterine anomalies, followed immediately by a rapid LFOV “scout” or coronal sequence if the adnexa are not visualized within the pelvis.
Consequently, for patients with known or suspected Müllerian duct anomalies presenting with suspected EP and inconclusive ultrasound findings, LFOV MRI should be considered a vital component of the diagnostic workup rather than a mere secondary option. This approach ensures that undescended adnexal secretions are not overlooked due to anatomical preconceptions. By integrating LFOV imaging into the clinical protocol, radiologists and clinicians can achieve more accurate localization of extra-pelvic gestations, thereby facilitating timely surgical intervention and improving patient outcomes in these rare but life-threatening scenarios[4,5].
This case, a rare subhepatic EP with unicornuate uterus/undescended adnexa, highlights the critical role of LFOV MRI. When pelvic ultrasound is inconclusive in the setting of suspected EP with complex congenital anomalies, LFOV MRI is essential for accurate, life-saving extra-pelvic localization.
We sincerely thank all the authors for their valuable contributions to this research.
| 1. | Akar ME, Bayar D, Yildiz S, Ozel M, Yilmaz Z. Reproductive outcome of women with unicornuate uterus. Aust N Z J Obstet Gynaecol. 2005;45:148-150. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 38] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 2. | Reichman D, Laufer MR, Robinson BK. Pregnancy outcomes in unicornuate uteri: a review. Fertil Steril. 2009;91:1886-1894. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 138] [Cited by in RCA: 125] [Article Influence: 7.4] [Reference Citation Analysis (0)] |
| 3. | Pardal C, Braga L, Vides B. Ectopic pregnancy in an undescended fallopian tube: a diagnostic challenge. BMJ Case Rep. 2016;2016:bcr2015213058. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 4] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 4. | Woolnough B, Ballermann C. An Atypical Presentation of Ectopic Pregnancy With Unicornuate Uterus and Undescended Fallopian Tube. J Obstet Gynaecol Can. 2019;41:214-216. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 5. | Pan J, Wang S, Wang H, Fan Z. A Rare Ectopic Ovary Mimicking Colon Sigmoideum Mesenchymoma Presenting as an Intestinal Mesenchymoma. Front Oncol. 2019;9:580. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.4] [Reference Citation Analysis (0)] |