Published online Mar 6, 2026. doi: 10.12998/wjcc.v14.i7.118581
Revised: January 22, 2026
Accepted: February 6, 2026
Published online: March 6, 2026
Processing time: 58 Days and 17.6 Hours
Cough assessment is a vital component of clinical management for pulmonary disorders, yet effective tools to execute quantification are insufficient. The do
Core Tip: Evaluating cough for pulmonary conditions relies substantially on acoustic measurement, yet existing quantification tools remain suboptimal. Integrating artificial intelligence (AI), particularly machine learning and deep learning, offers a promising pathway for both therapeutic and preventive applications in cough medicine. Current implementations remain confined to weak AI’s predefined roles, while advances in artificial general intelligence hold the potential to overcome these adaptability constraints. Moreover, harnessing current potential requires resolving key technical, ethical, and legal issues by integrating explainable AI, multimodal hybrid approaches, and robust accountability measures within human-centered frameworks.
- Citation: Thapa R, Paudyal V, Sharma M, Ratnani I, Surani S. Artificial intelligence advancement in addressing cough. World J Clin Cases 2026; 14(7): 118581
- URL: https://www.wjgnet.com/2307-8960/full/v14/i7/118581.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i7.118581
As a defensive mechanism of the respiratory tract, cough is crucial to maintain airway clearance. It is manifested as a sudden, forceful expulsion of air. Although a normal phenomenon, a chronic or persistent cough may signal a potential health threat mandating further evaluation[1,2]. Cough itself is not an autonomous disease; rather, it commonly mirrors an underlying pulmonary pathology. As respiratory disorders are among the principal drivers of the global burden of disease, the study of cough is of paramount significance[3-5]. Nearly 5%-10% adults are affected by chronic cough with its vexing sequelae such as sleep disturbances, dysphonia, syncope, and urinary incontinence, ultimately impairing their quality of life[6,7]. Chronic cough persists beyond 8 weeks in adults and 4 weeks in children[6]. A wide range of diseases with multisystem involvement may present with cough, as shown in Table 1.
| Acute cough (< 3 weeks) |
| Respiratory tract infections (pharyngitis, tonsillitis, bronchitis, pneumonia) |
| Subacute cough (3-8 weeks) |
| Post-infectious cough |
| Chronic cough (> 8 weeks) |
| Upper airway cough syndrome |
| Asthma (cough-variant asthma) |
| Eosinophilic bronchitis |
| Gastro-esophageal reflux disease |
| Drug induced (angiotensin converting enzyme inhibitor) |
| Chronic obstructive pulmonary disease |
| Bronchiectasis |
| Environmental and behavioral factors (smoking, pollution) |
| Neuronal hypersensitivity |
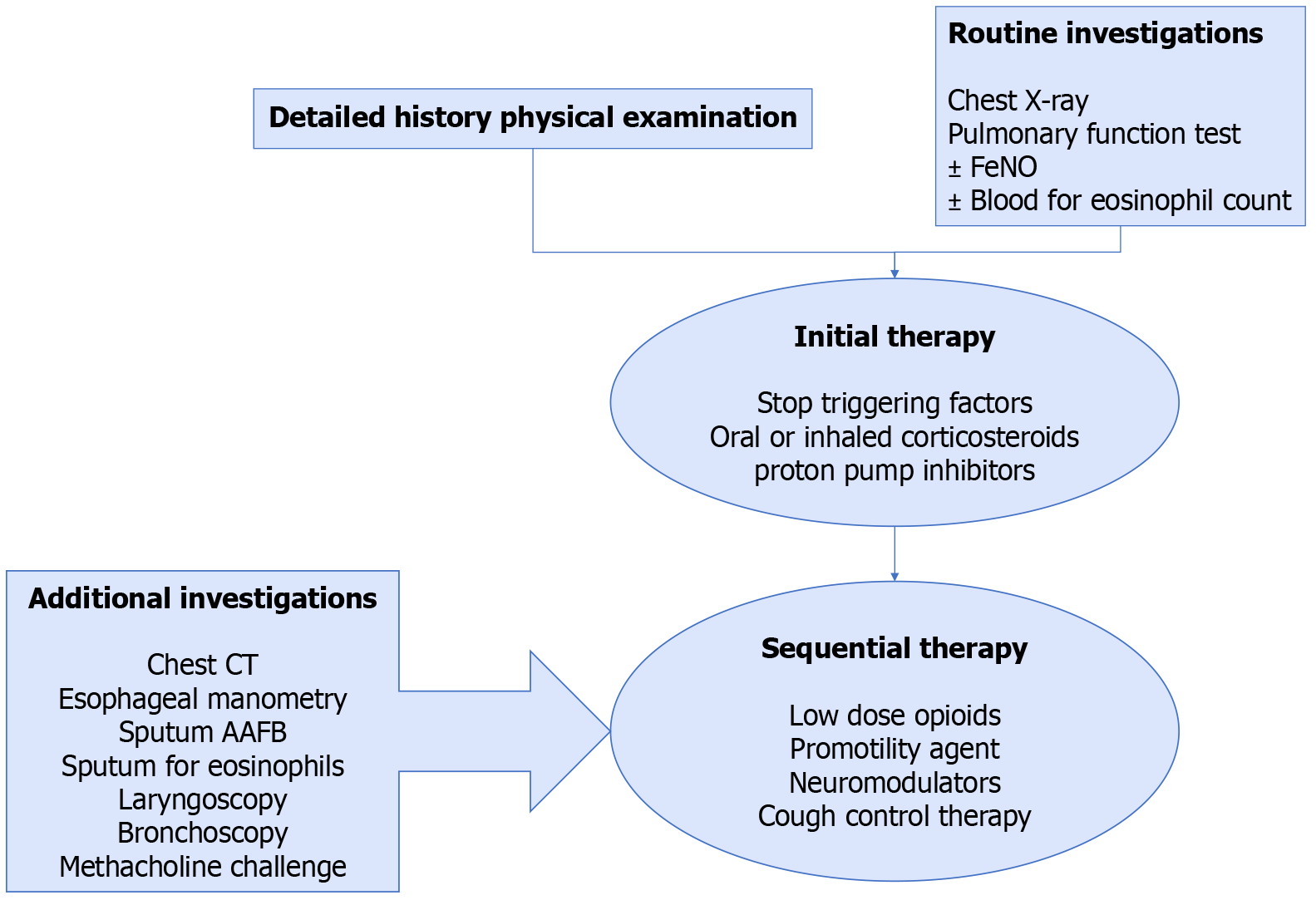
Traditionally, the initial approach to cough begins with a clinical assessment and basic diagnostic investigations, which guide towards empirical therapy followed by sequential trials for non-responders, as depicted in Figure 1[6]. Fueled by the latest technological breakthroughs, cough medicine has evolved from a conventional approach to a modern one that incorporates computational pulmonology. The resource limitations and access challenges highlighted by the coronavirus disease 2019 (COVID-19) pandemic underscored the need for novel diagnostic solutions. Under similar circumstances, innovative technologies such as artificial intelligence (AI) can help overcome these challenges[8,9]. AI serves as a valuable resource in healthcare to strengthen predictive diagnostics, therapeutic efficacy, precision medicine, and predictive prognostics[10,11].
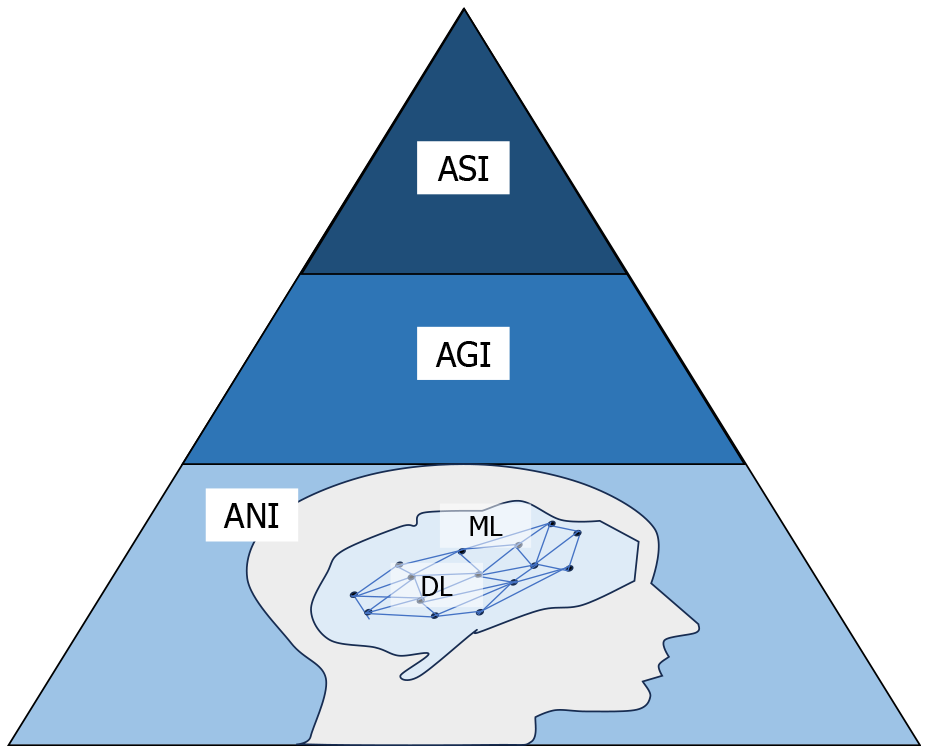
AI refers to the ability of a machine to perform a function that mimics human cognition. It can be categorized into three stages based on intelligence level: Artificial narrow intelligence, artificial general intelligence (AGI), and artificial superintelligence (ASI), as illustrated in Figure 2. Basically, narrow or weak AI is designed for a specific domain, which is intellectually inferior to humans. Likewise, general or strong AI is regarded as functionally analogous to human intelligence, and ASI is seen as surpassing human capabilities. As of today, operational AI is limited to a narrow domain, while AGI and ASI still remain hypothetical. The core application of modern AI, known as machine learning, enables machines to learn autonomously from data and perform pattern recognition for instantaneous decision-making without being explicitly programmed. Based on how algorithms learn from data, they are broadly segmented as supervised and unsupervised learning. The niche functions in machine learning involve deep learning (DL), which relies on multiple deep neural networks, allowing it to handle complex patterns and construct sophisticated predictions. Convolutional neural networks (CNNs) and recurrent neural networks (RNNs) are widely used DL models[10,12-14].
As AI has been revolutionizing various sectors, even healthcare is successfully capitalizing on its rewards. The field of AI officially began in the 1950s, when the term was first coined by John McCarthy[13,14]. During the 1970s, AI was introduced into the healthcare system through the MYCIN program to assist physicians in diagnosing infections and recommending antibiotic therapies[15]. Throughout the foundational era of medical AI and its evolution in the 1980s, INTERNIST-1; its improved version - Quick Medical Reference; and DXplain, were engineered for diagnostic assistance[16-18]. In modern medicine, the transition of AI from a rule-based system to a data-driven system represents a tipping point, particularly since the 2020s, with refinements in DL effectively neutralizing previous challenges[19]. Major advances in healthcare include: IBM Watson, DL-enabled diagnostics, autonomous AI systems, AlphaFold 2, and an automated photoelectrochemical biosensing platform[19-23].
Following these groundbreaking advances in healthcare, AI is driving a massive surge in demand. Its integration into modern healthcare is undeniable because of its potential to handle overwhelming volumes of medical data and mitigate the global shortage of healthcare professionals, which is crucial for expanding personalized medicine. The continuous improvements in AI algorithms and growth in computational power further accelerate its utility. The core assets of the AI system are its capacity to generate economical and accessible solutions through non-invasive, user-friendly modules. It further supports telehealth services, concurrently safeguarding against the spread of infectious diseases. Generally, the applications of AI enhance screening methodologies, diagnostic accuracy, treatment efficacy & effectiveness, prognostic reliability, and operational healthcare management, thereby broadening the availability of comprehensive healthcare[12,19,24-26]. As the modern healthcare landscape inclines toward individualized care, AI’s role in precision or personalized medicine remains crucial. It optimizes clinical outcomes by minimizing adverse effects by analyzing genetic profiles, medical data, and environmental factors. Beyond clinical care, AI plays a vital role in predictive medicine, enabling the anticipation of disease progression and recommending preventive approaches, thereby reinforcing public health preparedness. AI further enhances biomedical innovation by streamlining clinical trials[19,23,27,28]. Advancements have enabled AI penetration across the majority of healthcare domains, where integration with cough medicine is no exception. The COVID-19 pandemic served as a significant catalyst, propelling AI technology into cough medicine[8,29].
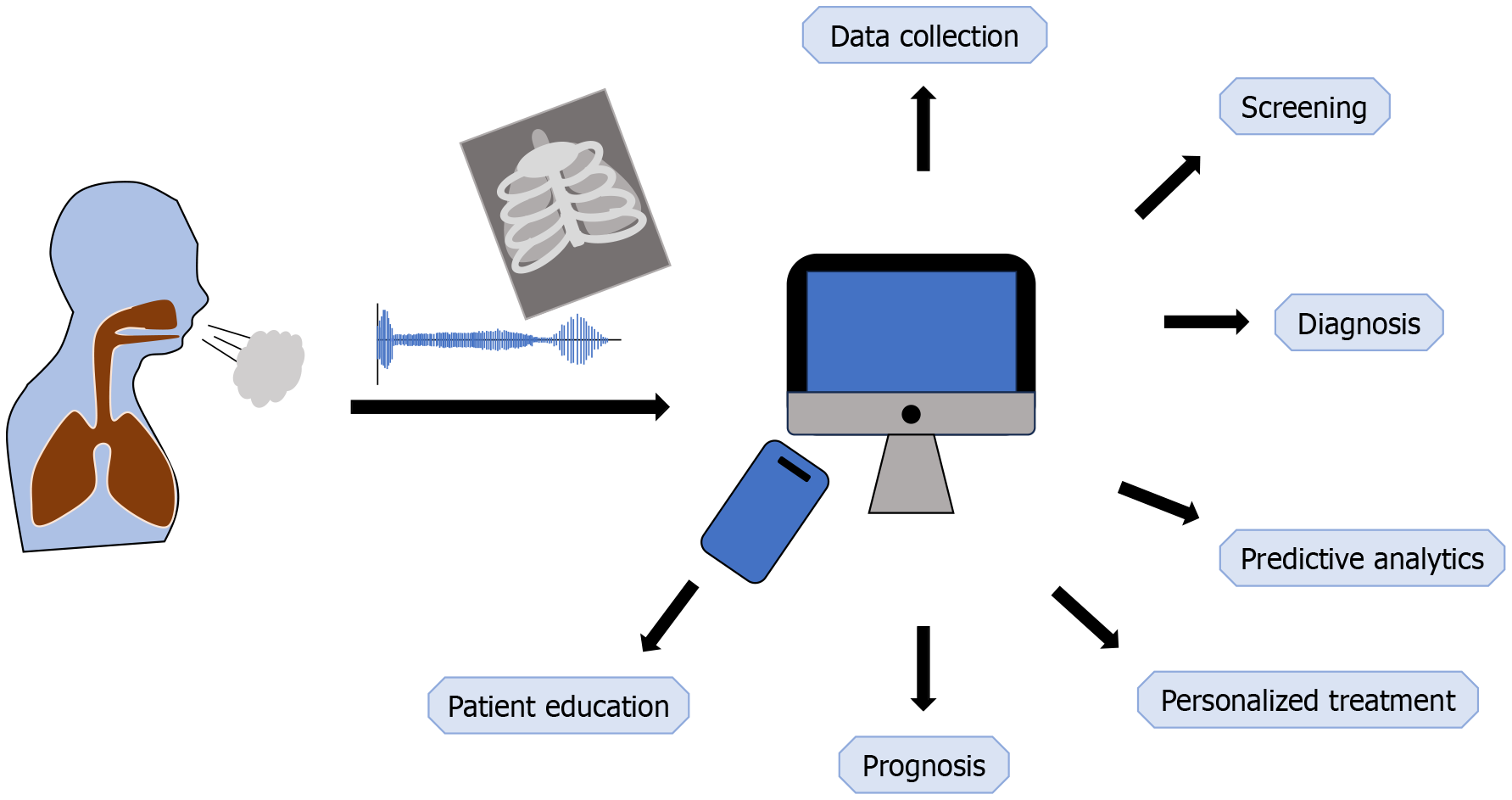
Cough is merely a manifestation of an underlying disease, as shown in Table 1. It often coexists with collateral features, including constitutional symptoms, runny nose, sneezing, nasal & throat irritation, chest tightness, dyspnea, and heartburn, as well as adventitious breath sounds. Further evaluation requires determining the underlying condition, planning therapeutic intervention, and predicting the potential outcome[6,30]. Harnessing electronic health records (EHRs), imaging, and genomics to guide AI enables rapid advances in patient care, as shown in Figure 3. Computer vision (CV), natural language processing (NLP), and reinforcement learning are major domains of DL. CV primarily uses CNN architectures to interpret spatial data, such as images and videos, in medical imaging. Likewise, NLP uses RNN modules to process sequential data, such as text, speech, and time-series data in EHRs[13,24,26,31].
AI enables objective quantification of cough, eliminating the former reliance on subjective assessment, which was limited to questionnaire-based severity scoring[32]. Acoustic cough analysis is the central paradigm of AI driven diagnostic methods[29]. However, to ensure a robust diagnostic framework, a multimodal approach can be adopted, including acoustic features (cough, voice, speech, breath sounds), imaging, and chemical profiles.
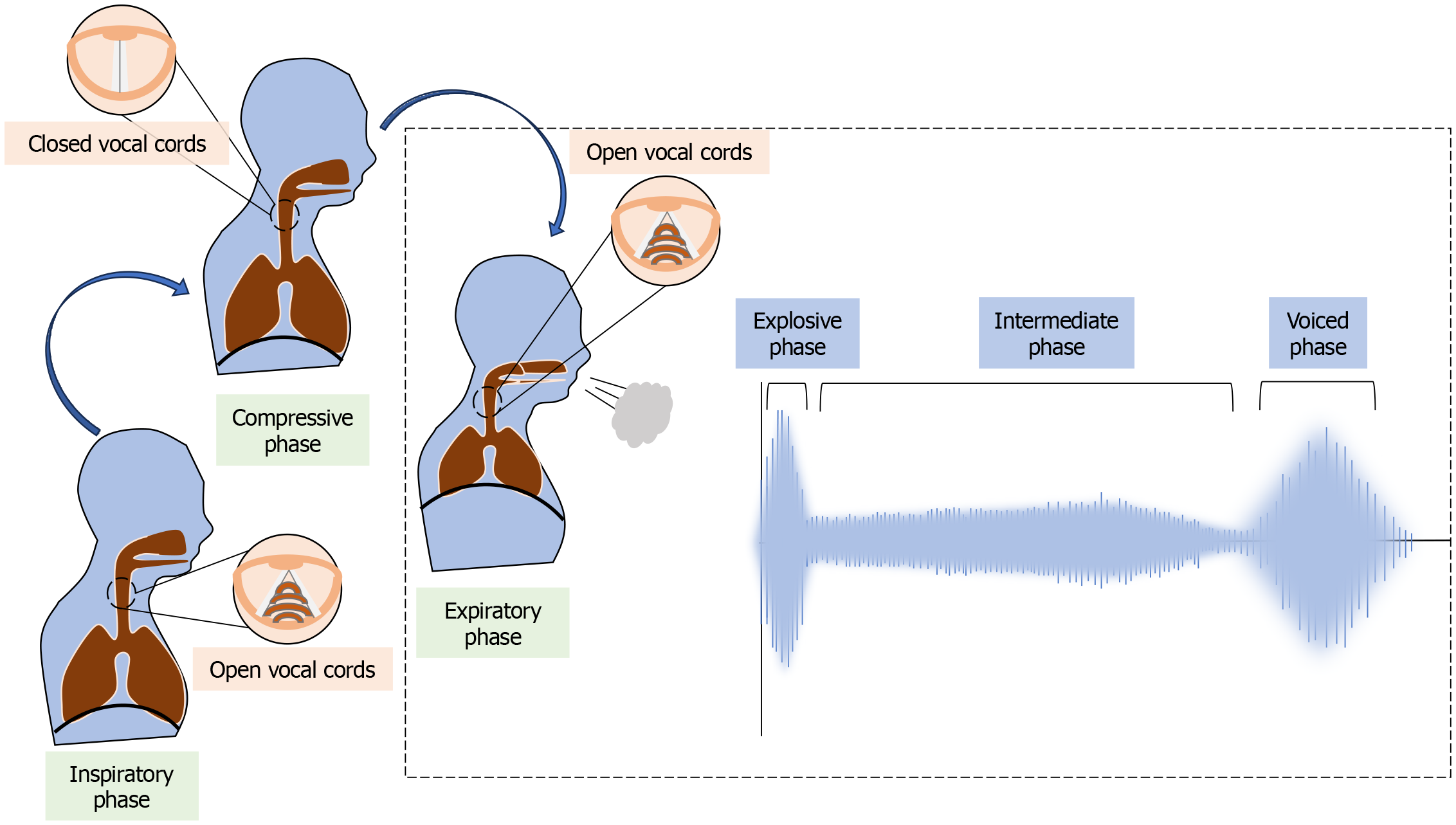
Cough sound analysis: By applying signal processing and machine learning, the acoustic properties of cough sounds can be analyzed in detail to yield clinically relevant information. These properties chiefly rely on their temporal (duration, amplitude) and spectral features (frequency/pitch)[31,33,34]. Physiologically, cough is divided into three sequential phases: Inspiratory phase, compressive phase, and expulsive phase. The central element of cough sound analysis is the expulsive phase, which is further divided into explosive, intermediate, and voiced phases, as shown in Figure 4[1,34,35]. Distinctive acoustic signatures are generated by various diseases, including asthma, pneumonia, bronchitis, chronic obstructive pulmonary disease (COPD), COVID-19, and tuberculosis. Additionally, disease severity can be assessed by monitoring cough counts[36-40].
The outcomes of cough sound analysis may deviate slightly due to the combination of diverse devices (smartphone, sensor, computer) and various ML models (logistic regression, support vector machines, deep neural networks). Furthermore, the scope of cough sound analysis may be tempered by challenges such as: (1) Perceptually identical sounds including non-cough respiratory sound (throat clearing) and non-respiratory environmental noises; (2) Cough triggered by non-pulmonary causes; and (3) Significant disease overlap - obscuring the interpretation. However, these setbacks can be resolved using advanced AI incorporating denoising mechanisms and robust generalizability[41-45].
Standardized acoustic feature extraction from cough excludes the inaudible inspiratory and compressive phases. Nevertheless, these preliminary stages are critical elements in determining cough strength and potential dysfunction. Thus, enabling AI to incorporate these factors to extend diagnostic precision[34,46].
Vocal biomarkers: The application of vocal biomarkers (voice/speech analysis) in pulmonology remains highly specific, focusing mainly on remote monitoring, identifying acute exacerbations, and early intervention for a few conditions (asthma, COPD, COVID-19). However, it holds immense potential beyond its current limitations as AI continues to evolve[47-50].
Breath sound analysis: Acoustic variances in breath sounds (oral, nasal, lung sounds) may serve as a beneficial diagnostic tool. This helps distinguish normal from adventitious breath sounds (stridor, wheeze, crackles)[51,52]. Moreover, it facilitates the identification of subtle breath sounds, primarily observed in children. Currently, breath sound analysis is addressed mainly in pediatrics due to limited cooperation and atypical pulmonary features. Similarly, the studies show overt favoritism towards the analysis of lung sounds. Thus, it is necessary to widen its scope by including adults and incorporating oral and nasal sounds for analysis. Furthermore, to ensure diagnostic accuracy, robust noise-reduction techniques must be implemented to mitigate acoustic contamination[53-57].
Radiography is another area where AI has demonstrated superior performance. It has enhanced medical imaging by improving the detection, characterization, and quantification of abnormalities, particularly in thoracic imaging. It has been boosting efficiency and diagnostic sensitivity. Tools, such as computer-aided detection, also enable scalable screening in resource-limited settings, reducing workload. However, human supervision remains crucial as full automation exceeds current limits. As progress continues, its role in image interpretation is expected to expand[58-62].
Researchers identified distinct metabolic signatures between healthy, acute COVID-19, and post-coronavirus disease (COVID) patients. This metabolomics approach to COVID could be further expanded with AI to significantly enhance diagnostic value for other respiratory illnesses[63-65].
AI provides a holistic approach to address cough, enabling the identification of non-respiratory etiologies that are often overlooked. Furthermore, it should be emphasized that existing AI tools in cough medicine like cough sound classification, disease detection and automated counting, function within the domain of weak AI. Despite their expertise in targeted medical roles, these applications lack the flexibility to function beyond their targeted roles[39,43,66,67]. Nevertheless, we anticipate that technological advancement toward AGI will overcome existing boundaries, empowering systems to generalize their capabilities.
Integrating AI, particularly machine learning and DL, has led to significant improvements in pulmonology. It serves as a core framework in the advancing field of precision medicine, an approach that prioritizes individualized patient care over conventional methods. AI is uniquely capable of integrating and analyzing vast amounts of patient data from multiple sources such as EHRs, medical imaging, and genomics. Moreover, it facilitates prompt intervention through diagnostic accuracy, disease surveillance, and determination of therapeutic effectiveness. Nevertheless, the existing therapeutic capabilities are poised for expansion[10,68-71].
Currently, AI aids prognosis in cough medicine by analyzing cough sounds. However, its future scope is expected to integrate additional biomarkers[72].
Beyond expanding the utilization of AI in curative cough medicine, preventive medicine is newly entering the spotlight. AI - driven technologies optimize respiratory disease management by integrating predictive modeling with real - time monitoring to enhance both preventive and corrective actions. It can further interpret epidemiological trends and datasets, thereby, estimating outbreaks and identifying early warning signs. This facilitates strategic preventive measures and educational initiatives to downregulate disease prevalence. Thus, anticipating to achieve deeper penetration into the clinical framework[72-75]. Some major breakthroughs in AI integration in cough medicine are listed in Table 2.
| Target | Data type | AI technology | Findings | ||
| Screening tool for TB, COVID-19, pneumonia | Cough sound | AudibleHealth AI (RAISONANCE)[86] | Disease | Sensitivity | Specificity |
| Tuberculosis | 90% | 72% | |||
| COVID-19 | 97% | 75.5% | |||
| Pneumonia | 94% | 73% | |||
| Muti-disease smartphone diagnosis | Cough sound | ResAppDx-EU[87] | Respiratory disease | Sensitivity | Specificity |
| Pediatric | 83%-97% | 82-91% | |||
| Adult | 83%-89% | 84%-91% | |||
| Automated cough analysis | Cough sound | Convolutional recurrent neural network[88] | 97.2% accuracy; 92.9% sensitivity; 97.6% specificity | ||
| AI cough classifier | Cough sound | Machine learning (mobile based cough sound classifier)[43] | Detection of respiratory diseases (TB, asthma, COPD) in rural Tanzania | ||
| Chronic cough identification | Cough with electronic health record data | XG boost model[89] | ROC-AUC of 0.916. Best performance when compared with other machine learning algorithms based on logistic regression and neural network approaches | ||
| Lung sound analysis | Lung sound | Feelix smart stethoscope (Sonavi Labs)[90] | Advantages over traditional stethoscope: Quick auscultation since precise positioning is not required; active noise cancellation; automatic abnormality detection | ||
| Bio-acoustic foundation model | Cough, speech & breath sound | Google HeAR (health acoustic representations)[91,92] | HeAR outperformed several audio encoder baselines such as TRILL, FRILL, BigSSL-CAP12, and CLAP by achieving highest overall performance across 33 tasks. Ranked as the top model in health acoustic detection while dominating cough inference and spirometry achieving the highest mean reciprocal rank (0.708) | ||
| Pattern classification and severity mapping | Cough sound | Swaasa platform[66] | 90% accuracy | ||
| Monitoring tool | Cough sound | Hyfe cough monitor[93] | 90.4% sensitivity (supports from initial screening to patient management) | ||
The power of AI is a double-edged sword because its inherent challenges serve as a vital barrier to its advancement. These challenges primarily involve technical aspects and ethical considerations. The primary concern is data quality, which also requires addressing issues of appropriate patient care, data privacy, and security. Furthermore, the lack of transparency, intrinsic to AI - known as the black box phenomenon, compromises generating diagnostic accuracy, effective treatment, and prognostic reliability. The combination of these issues leads to catastrophic consequences in healthcare delivery, thereby prompting legal inquiries and concerns about responsibility and accountability. Beyond that, clinician’s overreliance on AI promotes cognitive offloading, invariably leading to automation bias and professional deskilling. Additionally, amid rising concerns about job security, clinicians may compromise their professional integrity and diminish the standard of care[76-80].
Evolving beyond AI’s limitations demands the adoption of a comprehensive, human-centric strategy that embraces system optimization and resilient ethical governance. Technical refinement should be applied using a hybrid and multimodal approach, as it integrates multiple internal architectures and diverse datasets (clinical records - text, imaging - images/videos, acoustic biomarkers, and chemical biomarkers) to offer optimal generalization, while ensuring data privacy and security[79-81]. Besides, the black box effect of AI mandates the implementation of explainable AI to provide transparent justification, whose strategies facilitate clinical interpretability by revealing the key features, signals, or patterns influencing model outputs. During cough analysis, these techniques are employed to identify acoustically significant patterns while mapping them to underlying respiratory pathophysiology[82,83]. Furthermore, effective legal and policy frameworks to enforce accountability for its output should be formulated. Ultimately, incorporating a human-centric model is a key strategy that leverages technology to strengthen clinicians’ expertise, thereby protecting them against employment fragility. Despite the significant advancements AI has achieved within cough medicine, extensive future research and clinical trials are imperative to operate at its full capacity[79-81,83].
The vast domain of AI covers a spectrum of fields, where cough medicine remains no outlier. Integrating AI remains crucial across the entire clinical framework from initial screening to final prognosis. Though AI poses certain limitations and sparks clinician apprehension about job insecurity, its core value lies in its ability to support clinical judgment and decision-making. With further technological advancement, these limitations are anticipated to be overcome. Thus, AI-human collaboration must be sustained to solidify the transformative potential of AI. Moreover, existing legal obscurities surrounding accountability warrant robust policy prescription. Cough medicine has been yielding promising results so far, though current implications are confined to narrow domain. Nevertheless, future evolution toward AGI holds transformative potential by providing the adaptability required to extend its capabilities beyond predefined roles. Besides, further trials and studies are essential to nurture and strengthen its effectiveness.
| 1. | Chang AB. The physiology of cough. Paediatr Respir Rev. 2006;7:2-8. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 54] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 2. | Widdicombe J, Fontana G. Cough: what's in a name? Eur Respir J. 2006;28:10-15. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 81] [Cited by in RCA: 88] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 3. | Roser M, Ritchie H, Spooner F. Burden of Disease. 2016. [updated February 2024]. Available from: https://ourworldindata.org/burden-of-disease. |
| 4. | Puente-Maestu L, Dávila I, Quirce S, Crespo-Lessmann A, Martínez-Moragón E, Sola J, Nieto ML, González-Barcala FJ, Cea-Calvo L, Sánchez-Jareño M, Rivas-Pardinas C, Domingo C. Burden of refractory and unexplained chronic cough on patients' lives: a cohort study. ERJ Open Res. 2023;9:00425-02023. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 13] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 5. | Yang X, Chung KF, Huang K. Worldwide prevalence, risk factors and burden of chronic cough in the general population: a narrative review. J Thorac Dis. 2023;15:2300-2313. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 23] [Reference Citation Analysis (0)] |
| 6. | Morice AH, Millqvist E, Bieksiene K, Birring SS, Dicpinigaitis P, Domingo Ribas C, Hilton Boon M, Kantar A, Lai K, McGarvey L, Rigau D, Satia I, Smith J, Song WJ, Tonia T, van den Berg JWK, van Manen MJG, Zacharasiewicz A. ERS guidelines on the diagnosis and treatment of chronic cough in adults and children. Eur Respir J. 2020;55:1901136. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 400] [Cited by in RCA: 585] [Article Influence: 97.5] [Reference Citation Analysis (0)] |
| 7. | Chamberlain SA, Garrod R, Douiri A, Masefield S, Powell P, Bücher C, Pandyan A, Morice AH, Birring SS. The impact of chronic cough: a cross-sectional European survey. Lung. 2015;193:401-408. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 108] [Cited by in RCA: 195] [Article Influence: 17.7] [Reference Citation Analysis (0)] |
| 8. | Buonsenso D, Pata D, Chiaretti A. COVID-19 outbreak: less stethoscope, more ultrasound. Lancet Respir Med. 2020;8:e27. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 253] [Cited by in RCA: 227] [Article Influence: 37.8] [Reference Citation Analysis (0)] |
| 9. | Chung Y, Jin J, Jo HI, Lee H, Kim SH, Chung SJ, Yoon HJ, Park J, Jeon JY. Diagnosis of Pneumonia by Cough Sounds Analyzed with Statistical Features and AI. Sensors (Basel). 2021;21:7036. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 8] [Reference Citation Analysis (0)] |
| 10. | Karthika M, Sreedharan JK, Shevade M, Mathew CS, Ray S. Artificial intelligence in respiratory care. Front Digit Health. 2024;6:1502434. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 11. | Drummond D, Adejumo I, Hansen K, Poberezhets V, Slabaugh G, Hui CY. Artificial intelligence in respiratory care: perspectives on critical opportunities and challenges. Breathe (Sheff). 2024;20:230189. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 8] [Reference Citation Analysis (0)] |
| 12. | Xu Y, Liu X, Cao X, Huang C, Liu E, Qian S, Liu X, Wu Y, Dong F, Qiu CW, Qiu J, Hua K, Su W, Wu J, Xu H, Han Y, Fu C, Yin Z, Liu M, Roepman R, Dietmann S, Virta M, Kengara F, Zhang Z, Zhang L, Zhao T, Dai J, Yang J, Lan L, Luo M, Liu Z, An T, Zhang B, He X, Cong S, Liu X, Zhang W, Lewis JP, Tiedje JM, Wang Q, An Z, Wang F, Zhang L, Huang T, Lu C, Cai Z, Wang F, Zhang J. Artificial intelligence: A powerful paradigm for scientific research. Innovation (Camb). 2021;2:100179. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 119] [Cited by in RCA: 291] [Article Influence: 58.2] [Reference Citation Analysis (0)] |
| 13. | Goodfellow I, Bengio Y, Courville A. Machine Learning Basics. In: Deep Learning, MIT Press, 2016: 98-155. Available from: www.deeplearningbook.org. |
| 14. | Liu S, Russo C, Suero Molina E, Di Ieva A. Artificial Intelligence Methods. Adv Exp Med Biol. 2024;1462:21-38. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 15. | van Melle W. MYCIN: a knowledge-based consultation program for infectious disease diagnosis. Int J Man Mach Stud. 1978;10:313-322. [RCA] [DOI] [Full Text] [Cited by in Crossref: 41] [Cited by in RCA: 30] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 16. | Miller RA, McNeil MA, Challinor SM, Masarie FE Jr, Myers JD. The internist-1/quick medical reference project--status report. West J Med. 1986;145:816-822. [PubMed] |
| 17. | Feldman MJ, Barnett GO. An approach to evaluating the accuracy of DXplain. Comput Methods Programs Biomed. 1991;35:261-266. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 21] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 18. | Barnett GO, Cimino JJ, Hupp JA, Hoffer EP. DXplain. An evolving diagnostic decision-support system. JAMA. 1987;258:67-74. [PubMed] [DOI] [Full Text] |
| 19. | Olabiyi W, Akinleye D, Joel E. The Evolution of AI: From Rule-Based Systems to Data-Driven Intelligence. Arch Pharmacal Res. 2025;. |
| 20. | Preethiya T, Subbiah P, Pandiarajan T, Subramanian K, Chelladurai P, Selvalakshmi C. Autonomous System and AI. In: Choudhury T, Mary XA, Chowdhury S, Karthik C, Evangeline CS, editors. Modeling, Simulation, and Control of AI Robotics and Autonomous Systems. IGI Global Scientific Publishing, 2024: 1-14. [DOI] [Full Text] |
| 21. | Abràmoff MD, Lavin PT, Birch M, Shah N, Folk JC. Pivotal trial of an autonomous AI-based diagnostic system for detection of diabetic retinopathy in primary care offices. NPJ Digit Med. 2018;1:39. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1257] [Cited by in RCA: 883] [Article Influence: 110.4] [Reference Citation Analysis (5)] |
| 22. | Skolnick J, Gao M, Zhou H, Singh S. AlphaFold 2: Why It Works and Its Implications for Understanding the Relationships of Protein Sequence, Structure, and Function. J Chem Inf Model. 2021;61:4827-4831. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 172] [Article Influence: 34.4] [Reference Citation Analysis (0)] |
| 23. | Zhang Y, Chen Z, Wei S, Zhang Y, Fu H, Zhang H, Li D, Xie Z. Detection of biological loads in sewage using the automated robot-driven photoelectrochemical biosensing platform. Exploration (Beijing). 2024;4:20230128. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 7] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 24. | Akila K, Gopinathan R, Arunkumar J, Sree Bavai Malar B. The Role of Artificial Intelligence in Modern Healthcare: Advances, Challenges, and Future Prospects. Eur J Cardiovasc Med. 2025;15:615-624. |
| 25. | Alowais SA, Alghamdi SS, Alsuhebany N, Alqahtani T, Alshaya AI, Almohareb SN, Aldairem A, Alrashed M, Bin Saleh K, Badreldin HA, Al Yami MS, Al Harbi S, Albekairy AM. Revolutionizing healthcare: the role of artificial intelligence in clinical practice. BMC Med Educ. 2023;23:689. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2405] [Cited by in RCA: 1215] [Article Influence: 405.0] [Reference Citation Analysis (3)] |
| 26. | Esteva A, Robicquet A, Ramsundar B, Kuleshov V, DePristo M, Chou K, Cui C, Corrado G, Thrun S, Dean J. A guide to deep learning in healthcare. Nat Med. 2019;25:24-29. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3854] [Cited by in RCA: 1900] [Article Influence: 271.4] [Reference Citation Analysis (8)] |
| 27. | Artificial Intelligence in Health Care: The Hope, the Hype, the Promise, the Peril. Washington (DC): National Academies Press (US); 2023-Aug-2 . [PubMed] |
| 28. | Raj GM, Dananjayan S, Gudivada KK. Applications of artificial intelligence and machine learning in clinical medicine: What lies ahead? Med Adv. 2024;2:202-204. [DOI] [Full Text] |
| 29. | Awais M, Bhuva A, Bhuva D, Fatima S, Sadiq T. Optimized DEC: An effective cough detection framework using optimal weighted Features-aided deep Ensemble classifier for COVID-19. Biomed Signal Process Control. 2023;105026. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 30. | Lai K, Tang J, Zhan W, Li H, Yi F, Long L, Zhou J, Chen X, Huang L, Sun Z, Jiang Z, Chen Y, Lu H, Luo W, Chen R, Zhong N. The spectrum, clinical features and diagnosis of chronic cough due to rare causes. J Thorac Dis. 2021;13:2575-2582. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 7] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 31. | Adhi Pramono RX, Anas Imtiaz S, Rodriguez-Villegas E. Automatic Cough Detection in Acoustic Signal using Spectral Features. Annu Int Conf IEEE Eng Med Biol Soc. 2019;2019:7153-7156. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 9] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 32. | Morice AH, Fontana GA, Belvisi MG, Birring SS, Chung KF, Dicpinigaitis PV, Kastelik JA, McGarvey LP, Smith JA, Tatar M, Widdicombe J; European Respiratory Society (ERS). ERS guidelines on the assessment of cough. Eur Respir J. 2007;29:1256-1276. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 535] [Cited by in RCA: 474] [Article Influence: 24.9] [Reference Citation Analysis (0)] |
| 33. | Ansari MS, Singh P, Awasthi R, Sethi TP, Singh V. Spectral pattern of cough sounds as an aid to diagnosis in children with common respiratory diseases. Int J Contemp Pediatr. 2025;12:632-636. [DOI] [Full Text] |
| 34. | Korpás J, Sadlonová J, Vrabec M. Analysis of the cough sound: an overview. Pulm Pharmacol. 1996;9:261-268. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 99] [Cited by in RCA: 87] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 35. | Widodo A, Aisiyah MC. Characterization of Cough Sounds Based on Measured Sound Pressure Levels from Arduino-Based MAX9814 Sound Sensor. J Fis dan Apl. 2023;19:28. [DOI] [Full Text] |
| 36. | Abeyratne UR, Swarnkar V, Triasih R, Setyati A. Cough sound analysis - a new tool for diagnosing pneumonia. Annu Int Conf IEEE Eng Med Biol Soc. 2013;2013:5216-5219. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 37. | Spectral Analysis of Cough Sounds in Patients with Chronic Bronchitis. Int J Biomed. 2025;15:285-290. [DOI] [Full Text] |
| 38. | Modi B, Sharma M, Hemani H, Joshi H, Kumar P, Narayanan S, Shah R. Analysis of Vocal Signatures of COVID-19 in Cough Sounds: A Newer Diagnostic Approach Using Artificial Intelligence. Cureus. 2024;16:e56412. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 39. | Zimmer AJ, Ugarte-Gil C, Pathri R, Dewan P, Jaganath D, Cattamanchi A, Pai M, Grandjean Lapierre S. Making cough count in tuberculosis care. Commun Med (Lond). 2022;2:83. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 27] [Article Influence: 6.8] [Reference Citation Analysis (0)] |
| 40. | Barry SJ, Dane AD, Morice AH, Walmsley AD. The automatic recognition and counting of cough. Cough. 2006;2:8. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 108] [Cited by in RCA: 92] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 41. | Ghrabli S, Elgendi M, Menon C. Identifying unique spectral fingerprints in cough sounds for diagnosing respiratory ailments. Sci Rep. 2024;14:593. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 42. | Ren Z, Chang Y, Bartl-Pokorny KD, Pokorny FB, Schuller BW. The Acoustic Dissection of Cough: Diving Into Machine Listening-based COVID-19 Analysis and Detection. J Voice. 2024;38:1264-1277. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 5] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 43. | Isangula KG, Haule RJ. Leveraging AI and Machine Learning to Develop and Evaluate a Contextualized User-Friendly Cough Audio Classifier for Detecting Respiratory Diseases: Protocol for a Diagnostic Study in Rural Tanzania. JMIR Res Protoc. 2024;13:e54388. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 7] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 44. | Tran V, You T, Tsai W. Acoustic cues for person identification using cough sounds. Comput Meth Prog Bio. 2025;8:100195. [DOI] [Full Text] |
| 45. | Mootassim-Billah S, Schoentgen J, De Bodt M, Roper N, Digonnet A, Le Tensorer M, Van Nuffelen G, Van Gestel D. Acoustic Analysis of Voluntary Coughs, Throat Clearings, and Induced Reflexive Coughs in a Healthy Population. Dysphagia. 2023;38:1467-1486. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 46. | Umayahara Y, Soh Z, Sekikawa K, Kawae T, Otsuka A, Tsuji T. Clinical Significance of Cough Peak Flow and Its Non-Contact Measurement via Cough Sounds: A Narrative Review. Appl Sci. 2020;10:2782. [DOI] [Full Text] |
| 47. | Larsen E, Song X, Joachim D, Ch'en PY, M Green S, Hunt E, Kaur S, Nag R, Pisani O, Thomas S, Adewunmi V, Lutz C, Baghizadeh-Toosi B, Feldman JM, Jariwala S. Respiratory-Responsive Vocal Biomarker for Asthma Exacerbation Monitoring: Prospective Cohort Study. J Med Internet Res. 2025;27:e68741. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 48. | Despotovic V, Ismael M, Cornil M, Call RM, Fagherazzi G. Detection of COVID-19 from voice, cough and breathing patterns: Dataset and preliminary results. Comput Biol Med. 2021;138:104944. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 20] [Cited by in RCA: 30] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 49. | Elbéji A, Zhang L, Higa E, Fischer A, Despotovic V, Nazarov PV, Aguayo G, Fagherazzi G. Vocal biomarker predicts fatigue in people with COVID-19: results from the prospective Predi-COVID cohort study. BMJ Open. 2022;12:e062463. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 16] [Reference Citation Analysis (0)] |
| 50. | Lyu Y, Jiang QC, Yuan S, Hong J, Chen CF, Wu HM, Wang YQ, Shi YJ, Yan HX, Xu J. Non-invasive acoustic classification of adult asthma using an XGBoost model with vocal biomarkers. Sci Rep. 2025;15:28682. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 51. | Reichert S, Gass R, Brandt C, Andrès E. Analysis of respiratory sounds: state of the art. Clin Med Circ Respirat Pulm Med. 2008;2:45-58. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 110] [Cited by in RCA: 73] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 52. | Shokouhmand S, Bhatt S, Faezipour M. Artificial Intelligence in Respiratory Health: A Review of AI-Driven Analysis of Oral and Nasal Breathing Sounds for Pulmonary Assessment. Electronics. 2025;14:1994. [DOI] [Full Text] |
| 53. | Tzeng JT, Li JL, Chen HY, Huang CH, Chen CH, Fan CY, Huang EP, Lee CC. Improving the Robustness and Clinical Applicability of Automatic Respiratory Sound Classification Using Deep Learning-Based Audio Enhancement: Algorithm Development and Validation. JMIR AI. 2025;4:e67239. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 54. | Hafke-Dys H, Kuźnar-Kamińska B, Grzywalski T, Maciaszek A, Szarzyński K, Kociński J. Artificial Intelligence Approach to the Monitoring of Respiratory Sounds in Asthmatic Patients. Front Physiol. 2021;12:745635. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 17] [Reference Citation Analysis (0)] |
| 55. | Moon HJ, Ji H, Kim BS, Kim BJ, Kim K. Machine learning-driven strategies for enhanced pediatric wheezing detection. Front Pediatr. 2025;13:1428862. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 56. | Liu L, Li W, Moxley B. AI-Based Classification of Pediatric Breath Sounds: Toward a Tool for Early Respiratory Screening. Appl Sci. 2025;15:7145. [DOI] [Full Text] |
| 57. | Enseki M, Nukaga M, Tadaki H, Tabata H, Hirai K, Kato M, Mochizuki H. A breath sound analysis in children with cough variant asthma. Allergol Int. 2019;68:33-38. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 15] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 58. | Bennani S, Regnard NE, Ventre J, Lassalle L, Nguyen T, Ducarouge A, Dargent L, Guillo E, Gouhier E, Zaimi SH, Canniff E, Malandrin C, Khafagy P, Koulakian H, Revel MP, Chassagnon G. Using AI to Improve Radiologist Performance in Detection of Abnormalities on Chest Radiographs. Radiology. 2023;309:e230860. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 56] [Article Influence: 18.7] [Reference Citation Analysis (0)] |
| 59. | Kundu S, Elhalawani H, Gichoya JW, Kahn CE Jr. How Might AI and Chest Imaging Help Unravel COVID-19's Mysteries? Radiol Artif Intell. 2020;2:e200053. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 33] [Cited by in RCA: 32] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 60. | Chassagnon G, Vakalopoulou M, Paragios N, Revel MP. Artificial intelligence applications for thoracic imaging. Eur J Radiol. 2020;123:108774. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 120] [Article Influence: 17.1] [Reference Citation Analysis (4)] |
| 61. | Kaplan A, Cao H, FitzGerald JM, Iannotti N, Yang E, Kocks JWH, Kostikas K, Price D, Reddel HK, Tsiligianni I, Vogelmeier CF, Pfister P, Mastoridis P. Artificial Intelligence/Machine Learning in Respiratory Medicine and Potential Role in Asthma and COPD Diagnosis. J Allergy Clin Immunol Pract. 2021;9:2255-2261. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 183] [Cited by in RCA: 102] [Article Influence: 20.4] [Reference Citation Analysis (0)] |
| 62. | Jiang W, Zhang H, Li Z, Jiang X, Shao J, Yang X, Xiong J, Zhou P, Zhang H, Wang H, Yu J, Su X, Wang Y, Liu J, Li Z. AI-Powered Chest X-Ray for Diagnosing Pulmonary Tuberculosis in County and Township Health Care Facilities in Yichang: Retrospective, Real-World Study. J Med Internet Res. 2025;27:e83041. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 63. | Oropeza-Valdez JJ, Padron-Manrique C, Vázquez-Jiménez A, Soberon X, Resendis-Antonio O. Exploring metabolic anomalies in COVID-19 and post-COVID-19: a machine learning approach with explainable artificial intelligence. Front Mol Biosci. 2024;11:1429281. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 64. | Liang S, Cao X, Wang Y, Leng P, Wen X, Xie G, Luo H, Yu R. Metabolomics Analysis and Diagnosis of Lung Cancer: Insights from Diverse Sample Types. Int J Med Sci. 2024;21:234-252. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 19] [Article Influence: 9.5] [Reference Citation Analysis (0)] |
| 65. | Raimundo BS, Leitão PM, Vinhas M, Pires MV, Quintas LB, Carvalheiro C, Barata R, Ip J, Coelho R, Granadeiro S, Simões TS, Gonçalves J, Baião R, Rocha C, Alves S, Fidalgo P, Araújo A, Matos C, Simões S, Alves P, Garrido P, Pantarotto M, Carreiro L, Matos R, Bárbara C, Cruz J, Gil N, Luis-Ferreira F, Vaz PD. Breath Insights: Advancing Lung Cancer Early-Stage Detection Through AI Algorithms in Non-Invasive VOC Profiling Trials. Cancers (Basel). 2025;17:1685. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 66. | Thangakunam B, Chandy ST, Rudraraju G, Sripada NR, Govindaraj J, Gottipulla C, Mamidgi B, Palreddy SD, Reddy Bhoge NK, Reddy Narreddy HV, Prasanna Samuel P, Christopher DJ, Jain M, Yechuri V. Clinical validation of swaasa artificial intelligence platform using cough sounds for screening and diagnosis of respiratory diseases. 2025 Preprint. Available from: medRxiv. [DOI] [Full Text] |
| 67. | Park CW, Seo SW, Kang N, Ko B, Choi BW, Park CM, Chang DK, Kim H, Kim H, Lee H, Jang J, Ye JC, Jeon JH, Seo JB, Kim KJ, Jung KH, Kim N, Paek S, Shin SY, Yoo S, Choi YS, Kim Y, Yoon HJ. Artificial Intelligence in Health Care: Current Applications and Issues. J Korean Med Sci. 2020;35:e379. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 63] [Article Influence: 10.5] [Reference Citation Analysis (0)] |
| 68. | Mesko B. The role of artificial intelligence in precision medicine. Expert Rev Precis Me. 2017;2:239-241. [RCA] [DOI] [Full Text] [Cited by in Crossref: 99] [Cited by in RCA: 99] [Article Influence: 11.0] [Reference Citation Analysis (0)] |
| 69. | Alge M, Kuett L, Duschau-Wicke A, Häberli M, Morice A, Birring S, Elkayam DD. Validity of AI-based long-term cough monitoring for clinical use. 2025 Preprint. Available from: medRxiv. [DOI] [Full Text] |
| 70. | Aslam M. The Role of Artificial Intelligence in Pulmonary Medicine: Transforming Diagnosis, Treatment, and Research. J Adv Lung Health. 2024;4:126-127. [DOI] [Full Text] |
| 71. | Khemasuwan D, Sorensen JS, Colt HG. Artificial intelligence in pulmonary medicine: computer vision, predictive model and COVID-19. Eur Respir Rev. 2020;29:200181. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 74] [Cited by in RCA: 35] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 72. | Alqudaihi KS, Aslam N, Khan IU, Almuhaideb AM, Alsunaidi SJ, Ibrahim NMAR, Alhaidari FA, Shaikh FS, Alsenbel YM, Alalharith DM, Alharthi HM, Alghamdi WM, Alshahrani MS. Cough Sound Detection and Diagnosis Using Artificial Intelligence Techniques: Challenges and Opportunities. IEEE Access. 2021;9:102327-102344. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 39] [Article Influence: 7.8] [Reference Citation Analysis (0)] |
| 73. | Sharan RV, Rahimi-Ardabili H. Detecting acute respiratory diseases in the pediatric population using cough sound features and machine learning: A systematic review. Int J Med Inform. 2023;176:105093. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 12] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 74. | Wang M, Xia C, Huang L, Xu S, Qin C, Liu J, Cao Y, Yu P, Zhu T, Zhu H, Wu C, Zhang R, Chen X, Wang J, Du G, Zhang C, Wang S, Chen K, Liu Z, Xia L, Wang W. Deep learning-based triage and analysis of lesion burden for COVID-19: a retrospective study with external validation. Lancet Digit Health. 2020;2:e506-e515. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 39] [Cited by in RCA: 60] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 75. | Georgakopoulou VE. The Role of Artificial Intelligence in Combatting Respiratory Tract Infections. Cureus. 2024;16:e63635. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 76. | Natali C, Marconi L, Dias Duran LD, Cabitza F. AI-induced Deskilling in Medicine: A Mixed-Method Review and Research Agenda for Healthcare and Beyond. Artif Intell Rev. 2025;58:356. [DOI] [Full Text] |
| 77. | Qiu J, Li L, Sun J, Peng J, Shi P, Zhang R, Dong Y, Lam K, Lo FP, Xiao B, Yuan W, Wang N, Xu D, Lo B. Large AI Models in Health Informatics: Applications, Challenges, and the Future. IEEE J Biomed Health Inform. 2023;27:6074-6087. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 71] [Article Influence: 23.7] [Reference Citation Analysis (0)] |
| 78. | Rahsepar Meadi M, Sillekens T, Metselaar S, van Balkom A, Bernstein J, Batelaan N. Exploring the Ethical Challenges of Conversational AI in Mental Health Care: Scoping Review. JMIR Ment Health. 2025;12:e60432. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 37] [Article Influence: 37.0] [Reference Citation Analysis (0)] |
| 79. | Ibrahim Abdelhalim AA, M Osman HM, Hafez Sadaka SI, Yousif Mohammed MA, Eissa E, Abdalla R, Mohamad Hassan DH. Predictive Ability of Artificial Intelligence Algorithms in Pediatric Respiratory Disease Diagnosis Using Cough Sounds: A Systematic Review. Cureus. 2025;17:e88457. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 80. | Gabaldón-Figueira JC, Keen E, Giménez G, Orrillo V, Blavia I, Doré DH, Armendáriz N, Chaccour J, Fernandez-Montero A, Bartolomé J, Umashankar N, Small P, Grandjean Lapierre S, Chaccour C. Acoustic surveillance of cough for detecting respiratory disease using artificial intelligence. ERJ Open Res. 2022;8:00053-02022. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 18] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 81. | Ribeiro MT, Singh S, Guestrin C. ‘Why Should I Trust You?’: Explaining the Predictions of Any Classifier. KDD '16: Proceedings of the 22nd ACM SIGKDD International Conference on Knowledge Discovery and Data Mining; 2016; 1135-1144. [DOI] [Full Text] |
| 82. | van der Velden BHM, Kuijf HJ, Gilhuijs KGA, Viergever MA. Explainable artificial intelligence (XAI) in deep learning-based medical image analysis. Med Image Anal. 2022;79:102470. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1038] [Cited by in RCA: 458] [Article Influence: 114.5] [Reference Citation Analysis (0)] |
| 83. | Amado-Caballero P, San-José-Revuelta LM, Aguilar-García MD, Garmendia-Leiza JR, Alberola-López C, Casaseca-de-la-Higuera P. XAI-Driven Spectral Analysis of Cough Sounds for Respiratory Disease Characterization. arXiv 2025. Available from: https://arxiv.org/html/2508.14949v1. |
| 84. | Abdullah, Fatima Z, Abdullah J, Rodríguez JLO, Sidorov G. A Multimodal AI Framework for Automated Multiclass Lung Disease Diagnosis from Respiratory Sounds with Simulated Biomarker Fusion and Personalized Medication Recommendation. Int J Mol Sci. 2025;26:7135. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 85. | Foti Randazzese S, Toscano F, Gambadauro A, La Rocca M, Altavilla G, Carlino M, Caminiti L, Ruggeri P, Manti S. Neuromodulators in Acute and Chronic Cough in Children: An Update from the Literature. Int J Mol Sci. 2024;25:11229. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 86. | RAIsonance. RAIsonance Announces New Clinical Validation Results for TB, COVID, Pneumonia. 2025. Available from: https://www.raisonance.ai/. |
| 87. | ResAppDx-EU. The future of respiratory disease diagnosis is digital. 2020. Available from: https://digitalhealth.org.au/wp-content/uploads/2020/06/ResAppDx-EU-flyer.pdf. |
| 88. | Wang Y, Wahab M, Hong T, Molinari K, Gauvreau GM, Cusack RP, Gao Z, Satia I, Fang Q. Automated Cough Analysis with Convolutional Recurrent Neural Network. Bioengineering (Basel). 2024;11:1105. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 89. | Bali V, Turzhitsky V, Schelfhout J, Paudel M, Hulbert E, Peterson-Brandt J, Hertzberg J, Kelly NR, Patel RH. Machine learning to identify chronic cough from administrative claims data. Sci Rep. 2024;14:2449. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 90. | West E, Mclane I, Mclane D, Emmanouilidou D, Elhilali M, West JE, Ward A, Busch-Vishniac I, Mclane J, Dottin-Haley B. Introducing Feelix, a digital stethoscope incorporating active noise control and automatic detection of lung sound abnormalities. J Acoust Soc Am. 2019;145:1923-1923. [DOI] [Full Text] |
| 91. | Shravya Shetty. This AI model is helping researchers detect disease based on coughs. 2024. Available from: https://blog.google/technology/health/ai-model-cough-disease-detection/. |
| 92. | Baur S, Nabulsi Z, Weng WH, Garrison J, Blankemeier L, Fishman S, Chen C, Kakarmath S, Maimbolwa M, Sanjase N, Shuma B, Matias Y, Corrado GS, Patel S, Shetty S, Prabhakara S, Muyoyeta M, Ardila D. HeAR -- Health Acoustic Representations. arXiv 2024. [DOI] [Full Text] |
| 93. | Chaccour C, Sánchez-Olivieri I, Siegel S, Megson G, Winthrop KL, Botella JB, de-Torres JP, Jover L, Brew J, Kafentzis G, Galvosas M, Rudd M, Small P. Validation and accuracy of the Hyfe cough monitoring system: a multicenter clinical study. Sci Rep. 2025;15:880. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/