Published online May 26, 2026. doi: 10.12998/wjcc.v14.i15.120269
Revised: March 9, 2026
Accepted: April 10, 2026
Published online: May 26, 2026
Processing time: 79 Days and 22.4 Hours
Angiolipoma is a rare benign tumor composed of mature adipocytes and proliferative capillary networks, most frequently found in the extremities. Occurrence in the nasal region, particularly at the alar base, is exceedingly rare, with no prior cases documented in the English-language literature.
A 59-year-old Korean lady presented with painless, progressive swelling of the right nostril of the right nasal alar base. Radiologic evaluation revealed a well-circumscribed, enhancing 10 mm mass without bony erosion or intranasal exten
This is the first published case to widen the morphological spectrum of nasal angiolipomas and underscores the relevance of including angiolipoma in the dif
Core Tip: This is the first published case to widen the morphological spectrum of nasal angiolipomas, particularly at the nasal alar base and underscores the relevance of including angiolipoma in the differential diagnosis of vascular-appearing nasal tumors. Complete surgical excision provides good cosmetic and functional benefits with a low chance of recurrence. It also provides an overview of the surgical technique for reconstruction of alar base defects. This case adds valuable insight to the literature and encourages heightened clinical suspicion for accurate diagnosis and optimal surgical management.
- Citation: Choi JY, Aldosari AM, Lim SC. Angiolipoma of the nasal alar base: A case report. World J Clin Cases 2026; 14(15): 120269
- URL: https://www.wjgnet.com/2307-8960/full/v14/i15/120269.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i15.120269
Angiolipoma is a benign mesenchymal tumor considered a vascular variant of a lipoma. It is composed of mature adipocytes scattered among a noticeable capillary-type vascular network, which often contains fibrin microthrombi[1]. Due to its vascularity, it usually develops in the trunk or extremities, where it frequently manifests as a sore subcu
Nasal angiolipomas remain extremely uncommon, with the majority occurring on the nasal dorsum and tip, according to a thorough analysis of previously published cases[5]. To the best of our knowledge, this is the first recorded instance of an angiolipoma developing exclusively from the nasal alar base, a place not previously reported in the available English-language literature. This report describes the clinical features, radiologic findings, operative details, and histopathologic characteristics of the patient, and highlights important diagnostic points clinicians should consider when evaluating vascular-appearing lesions in the nasal region.
A 59-year-old Korean female patient presented to a local otolaryngology clinic with persistent swelling of the right nasal base and a palpable mass in the alar region.
She reported having undergone rhinoplasty ten years earlier, 2 years back, she gradually noticed a small lump that slowly increased in size. Despite the cosmetic concern, she denied pain, obstruction, bleeding, or any other nasal symptoms. After that, she was referred to our tertiary hospital for further management.
Her medical and surgical and histories were unremarkable.
Her family history was otherwise unremarkable, and there was no history of trauma.
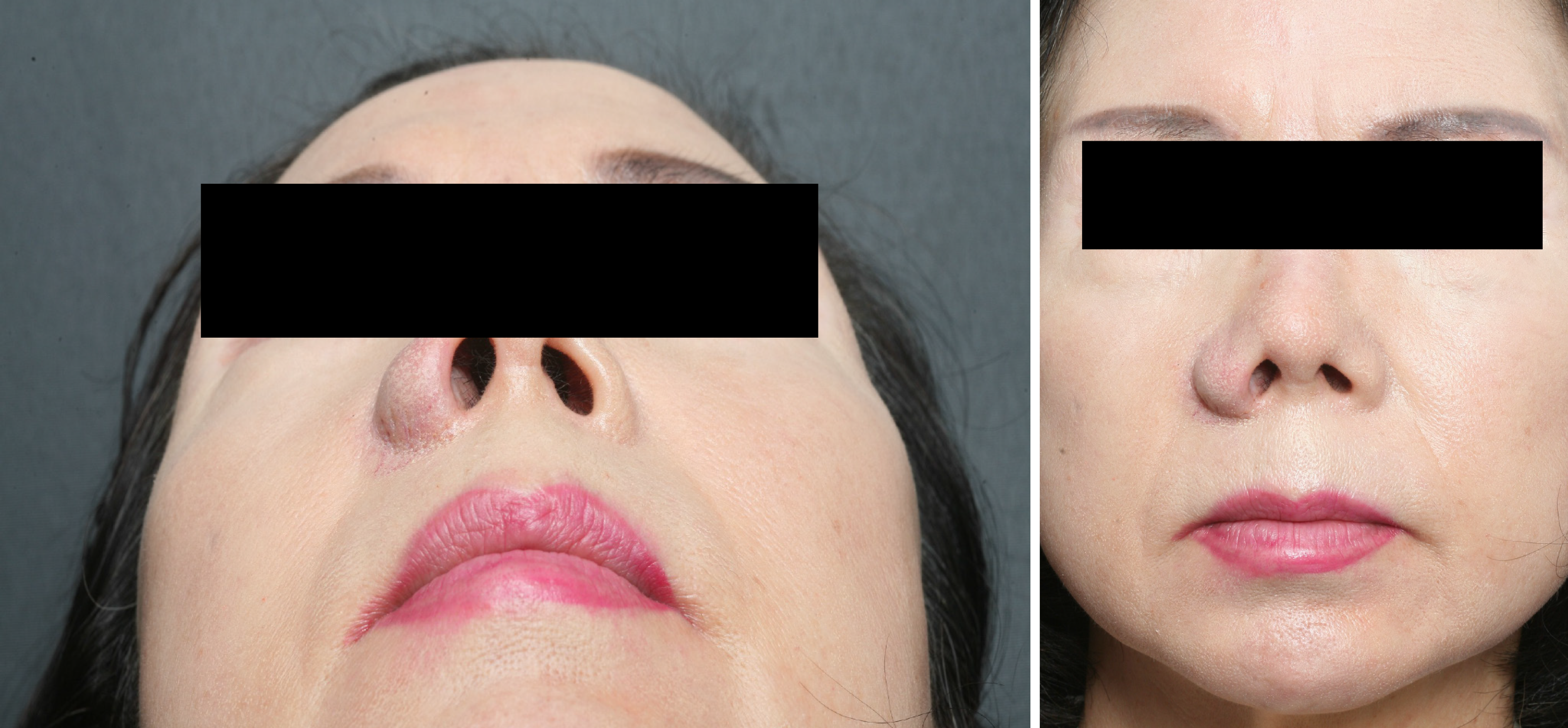
On physical examination, a well-circumscribed, slightly compressible nodule measuring approximately 1 cm was detected at the right alar base. The overlying skin was intact and showed only faint superficial vascular markings. The lesion was mobile, non-tender, and there was no associated cervical lymphadenopathy as shown in Figure 1.
All labs were within normal range, including complete blood count, coagulation profile, liver function test, and kidney function test.
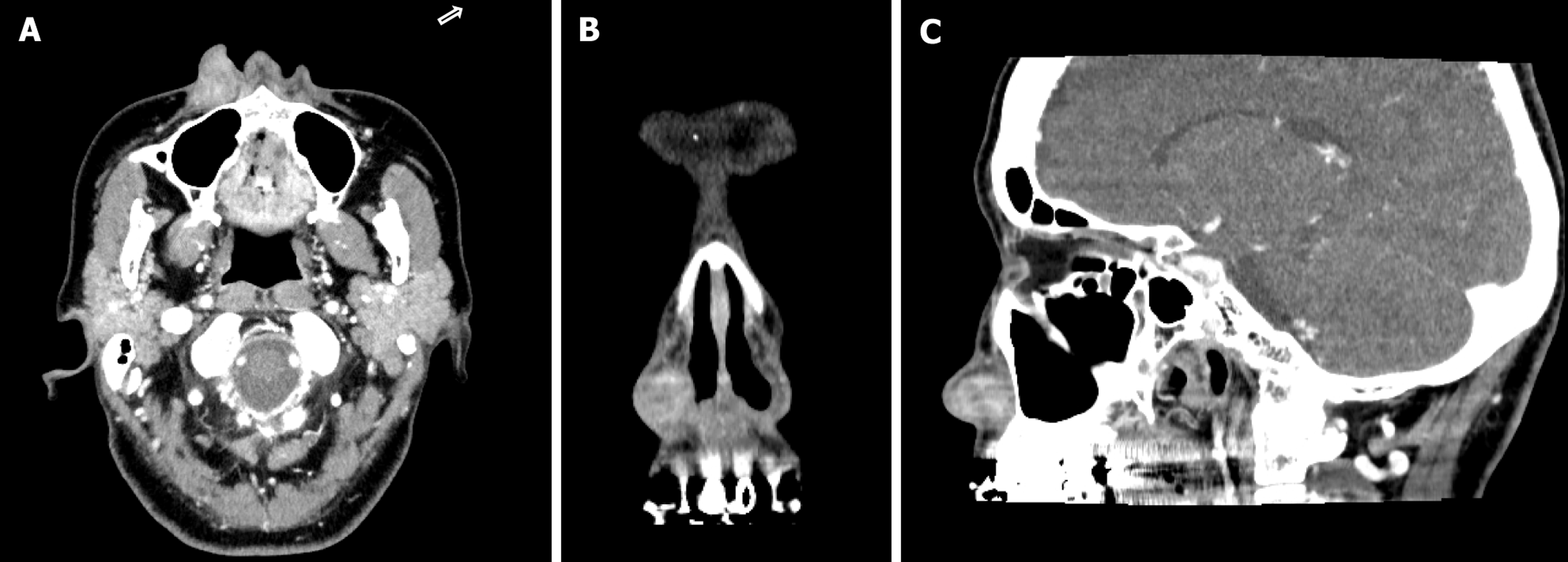
A contrast-enhanced computed tomography scan demonstrated a 10 mm × 10 mm, well-defined, avidly enhancing soft-tissue mass consistent with a vascular lesion. No bony erosion or intranasal extension was observed as shown in Figure 2. Based on these findings, surgical excision under local anesthesia was recommended for both diagnosis and treatment.
Non-infiltrative angiolipoma.
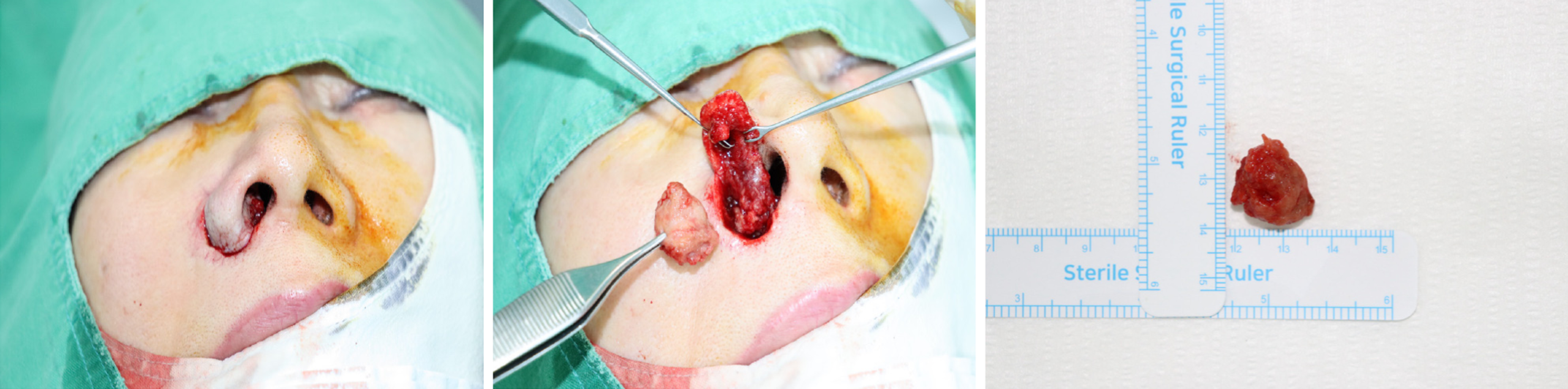
Complete surgical removal with alar base reconstruction (Figure 3).
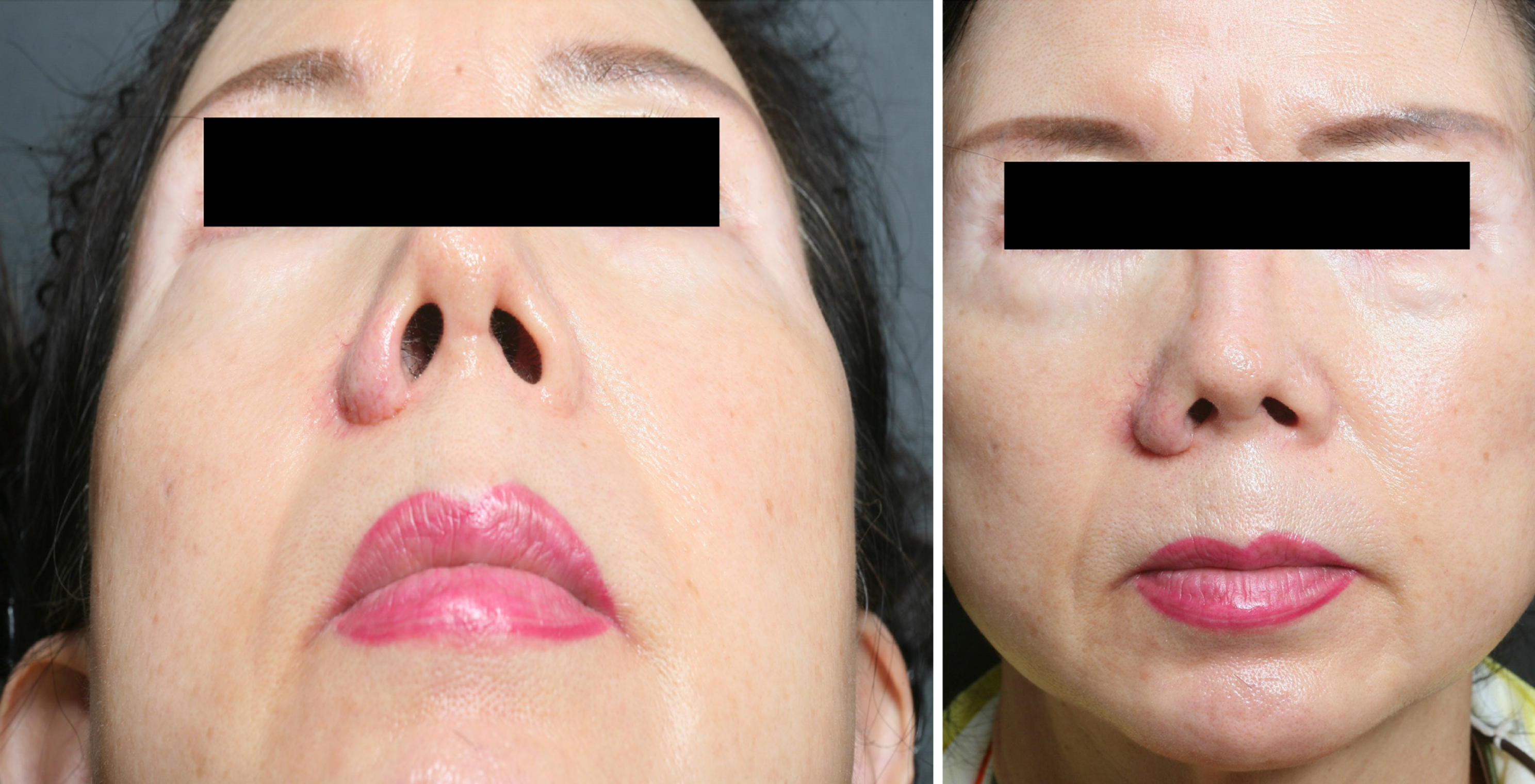
The surgical site healed uneventfully with a satisfactory cosmetic outcome, and the patient continues to be followed up in our clinic with no sign of recurrence (Figure 4).
Angiolipomas of the head and neck are infrequently encountered, and nasal involvement is even more uncommon. It most usually occurs in the limbs, whereas involvement of the head and neck is unusual and nasal presentation is ext
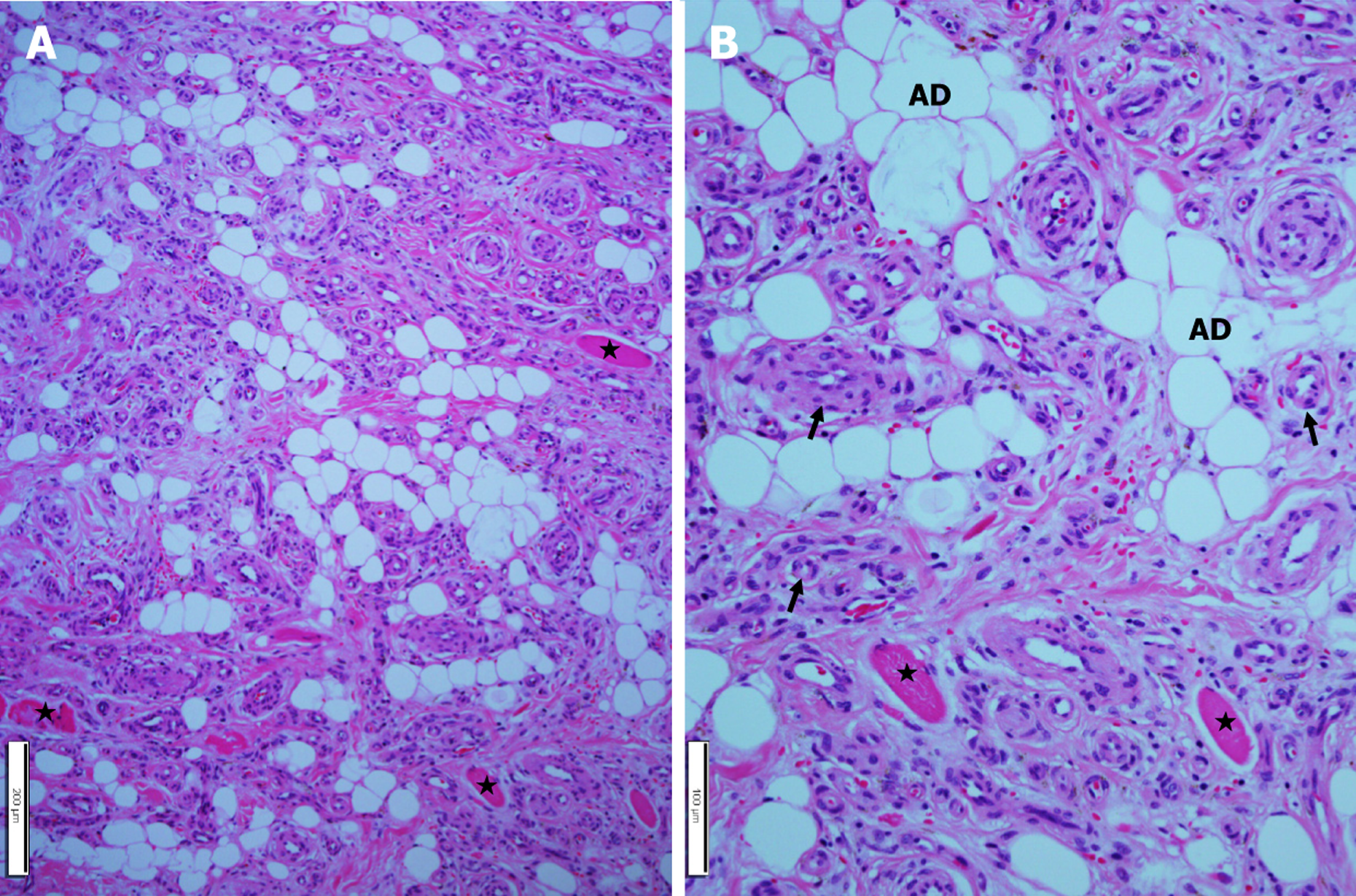
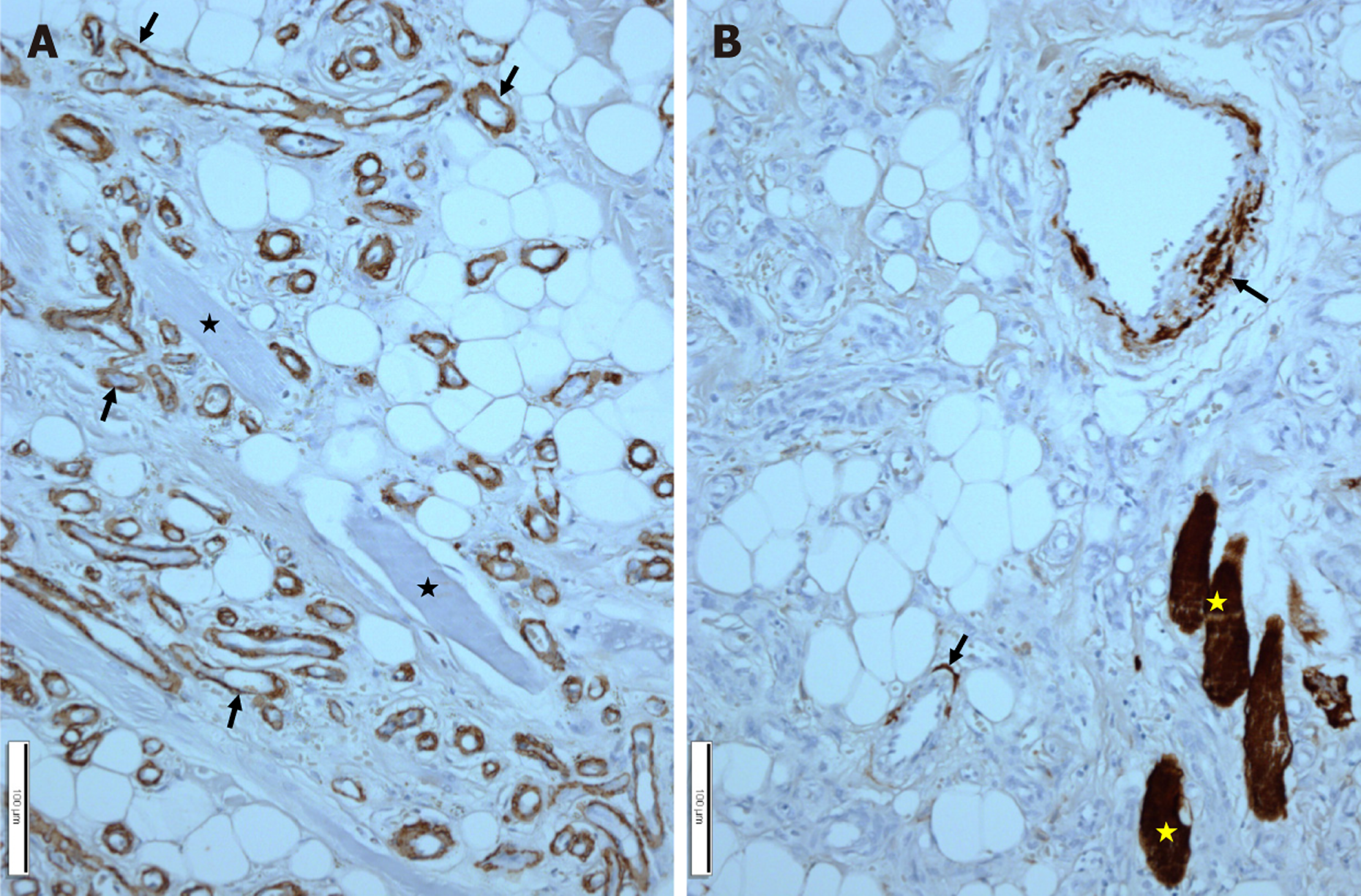
Radiologically, angiolipomas often present as well-defined enhancing lesions due to their vascular component; imaging findings are nonspecific and overlap with those of lipoma, hemangioma, and other vascular lesions[2,11]. Therefore, the diagnosis is based on histopathologic examination. Histology in this instance showed mature adipocytes with intermixed vascular channels and α-smooth muscle actin positivity limited to the vascular walls, consistent with a non-infiltrating angiolipoma (Figures 5 and 6).
According to Dionne and Seemayer[12], angiolipomas are categorized as either non-infiltrating or infiltrating, with the latter exhibiting muscle invasion and a greater risk of recurrence. The lesion in this case was non-infiltrating, which is why surgical removal was simple and the result was favorable. Complete local excision is considered curative, and recurrence is rare when the entire tumor is removed[6]. In this case, the histologic identification of mature adipocytes with intermixed vascular channels, supported by alpha-smooth muscle actin staining, confirmed the diagnosis. Imp
The clinical, radiologic, and histopathologic findings emphasize the importance of considering angiolipoma in the differential diagnosis of well-defined vascular-appearing nasal lesions. Continued reporting of such rare presentations will enhance our understanding and support more accurate diagnosis of these unusual lesions.
| 1. | Kransdorf MJ, Larsen BT, Goulding KA, Cumsky JL, Hwang S, Long JR. Angiolipoma: a review of 778 lesions in 344 patients. Skeletal Radiol. 2023;52:541-552. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 11] [Reference Citation Analysis (0)] |
| 2. | Reiser V, Haj Yahya B, Chaushu G, Kaplan I, Hamzani Y. Angiolipoma in the Head and Neck: Imaging, Diagnosis and Management. Medicina (Kaunas). 2020;56:283. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 3. | Shohet JA, Simpson B, Coleman JR, Geiger XJ. Angiolipoma presenting as a nasal mass. Otolaryngol Head Neck Surg. 1998;118:848-849. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 4] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 4. | Gupta SC, Jain S, Singh HP, Sachan A, Dey S. Lymphangiomatous polyp of the nasal cavity: a rare presentation. Ear Nose Throat J. 2012;91:E10-E12. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 5. | Han HH, Choi JY, Seo BF, Mun SH, Rhie JW, Ahn ST, Oh DY. Radiologic misunderstanding of cutaneous angiomyolipoma in the alar base. J Craniofac Surg. 2014;25:e343-e344. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 6. | Arenaz Búa J, Luáces R, Lorenzo Franco F, García-Rozado A, Crespo Escudero JL, Fonseca Capdevila E, López-Cedrún JL. Angiolipoma in head and neck: report of two cases and review of the literature. Int J Oral Maxillofac Surg. 2010;39:610-615. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 22] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 7. | Rao SS, Panda NK, Saikia UN, Saravanan K. Angiolipoma presenting as a nasal mass: how rare a presentation? Ear Nose Throat J. 2008;87:384-385. [PubMed] [DOI] [Full Text] |
| 8. | Ali MH, el-Zuebi F. Angiolipoma of the cheek: report of a case. J Oral Maxillofac Surg. 1996;54:213-215. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 14] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 9. | de Bree E, Karatzanis A, Hunt JL, Strojan P, Rinaldo A, Takes RP, Ferlito A, de Bree R. Lipomatous tumours of the head and neck: a spectrum of biological behaviour. Eur Arch Otorhinolaryngol. 2015;272:1061-1077. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 27] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 10. | Alvi A, Garner C, Thomas W. Angiolipoma of the head and neck. J Otolaryngol. 1998;27:100-103. [PubMed] |
| 11. | Burt AM, Huang BK. Imaging review of lipomatous musculoskeletal lesions. SICOT J. 2017;3:34. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 34] [Cited by in RCA: 54] [Article Influence: 6.0] [Reference Citation Analysis (0)] |