Published online May 16, 2026. doi: 10.12998/wjcc.v14.i14.120147
Revised: March 9, 2026
Accepted: March 31, 2026
Published online: May 16, 2026
Processing time: 70 Days and 7.4 Hours
Adenosine-sensitive focal atrial tachycardias (AT) arising from the anteroseptal region are uncommon and may be difficult to ablate safely because of their proximity to the atrioventricular (AV) conduction system. Failure of conventional right or left atrial ablation should prompt consideration of alternative anatomical sites.
A 64-year-old caucasian man with no structural heart disease presented with re
The non-coronary cusp is a safe and effective ablation target for anteroseptal focal atrial tachycardia.
Core Tip: Anteroseptal focal atrial tachycardia may originate from tissue adjacent to or within the aortic root. When right and left atrial ablation is ineffective or hazardous, systematic mapping of the non coronary cusp can provide a safe and durable cure while minimizing the risk of atrioventricular block.
- Citation: Porto AG, Zappulla P, Conti S, Sgarito G. When the atrium is not enough, ablation of anteroseptal focal atrial tachycardia from the non-coronary aortic cusp: A case report. World J Clin Cases 2026; 14(14): 120147
- URL: https://www.wjgnet.com/2307-8960/full/v14/i14/120147.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i14.120147
Focal atrial tachycardia (AT) represents a minority of supraventricular tachycardias (SVT), counting for approximately 7% of all cases[1]. AT is most frequently encountered in specific regions of the atria such as the crista terminalis, coronary sinus, pulmonary veins, or atrial appendages[2,3]. AT is often challenging to diagnose based on clinical presentation and surface electrocardiogram (ECG). Different algorithms have been proposed to identify the origin of AT based on the analysis of the 12-lead ECG[2,3]. Tachycardias arising from the anterior or anteroseptal atrium are uncommon and often pose diagnostic and therapeutic challenges because of their proximity to the atrioventricular (AV) node and his bundle[4]. Adenosine sensitivity and the presence of intermittent AV block during tachycardia strongly support a focal atrial mechanism and help distinguish this entity from AV node–dependent reentrant tachycardias.
Several studies have suggested that para-Hisian ATs can be successfully ablated from the right or left atrial septum, or non-coronary cusp (NCC) in the aorta[5]. However, ablation from the right or left atrial septum may be ineffective or associated with an unacceptably high risk of conduction system injury. Previous studies have demonstrated that the NCC may harbor atrial myocardial extensions capable of sustaining atrial tachyarrhythmias[4-7]. For this reason, mapping and ablation in the NCC should be always considered in cases of AT originating from the His bundle region. However, conduction system injury have been also reported in catheter ablation of AT from the NCC[6]. We report a case of adenosine-sensitive anteroseptal focal AT successfully treated by radiofrequency (RF) ablation from the NCC after failed conventional atrial approaches.
Recurrent palpitations associated with general malaise for approximately three months.
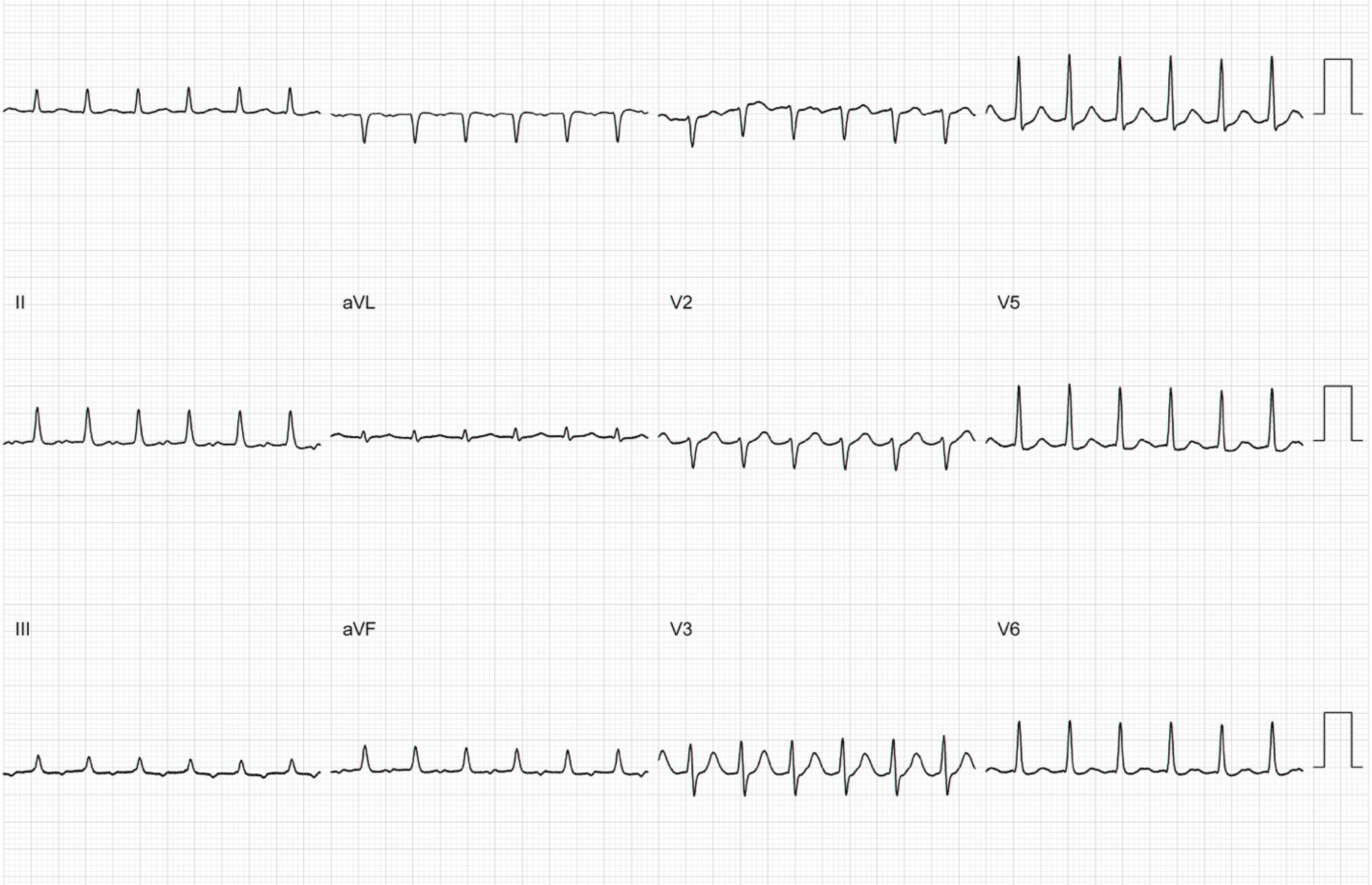
The patient reported sudden-onset, regular palpitations occurring several times per week, often requiring presentation to the emergency department. Episodes were associated with mild dyspnea and fatigue but no syncope, chest pain or hemodynamic instability. Each documented episode was terminated by intravenous adenosine. The 12-lead ECG of the tachycardia is showed in Figure 1.
No history of cardiovascular disease, hypertension, diabetes, or prior arrhythmias.
The patient was a Caucasian, 64-year-old male, normal weight, and non-smoker. There was no family history of arrhythmias or sudden cardiac death.
Blood pressure 125/75 mmHg; heart rate in sinus rhythm 80 beats per minute (bpm); oxygen saturation 98% on room air. Cardiovascular and respiratory examinations were unremarkable.
Routine blood tests, electrolytes, renal, thyroid and hepatic function were within normal limits.
Transthoracic echocardiography showed normal cardiac chamber dimensions, preserved biventricular function, and no structural abnormalities.
Adenosine-sensitive focal AT originating from the anteroseptal region, successfully ablated from the non-coronary aortic cusp.
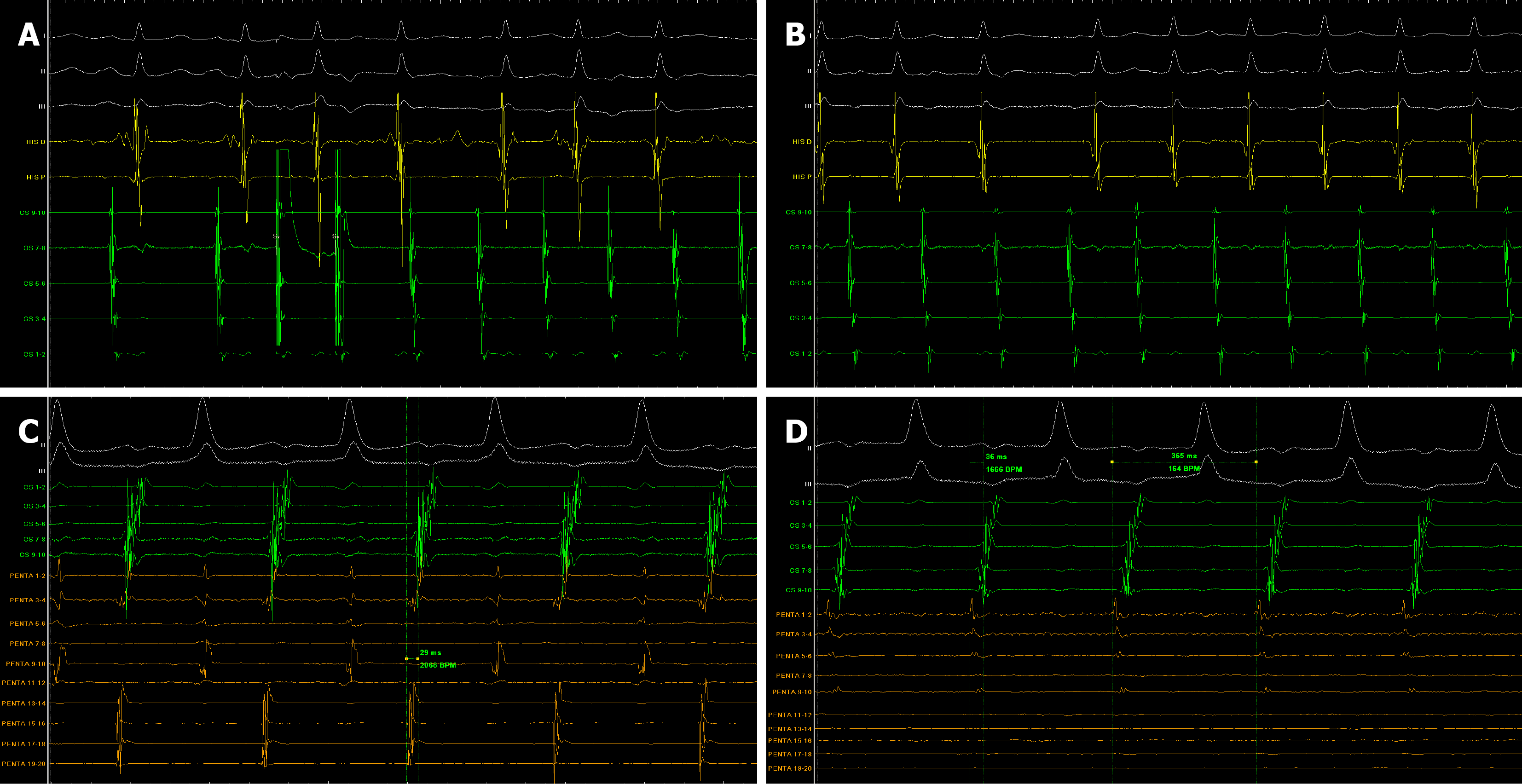
After informed consent, the patient was hence referred for an electrophysiological study and ablation. Baseline rhythm was sinus at 100 bpm with normal AV and infra-Hisian conduction: Atrial-Hisian 80 milliseconds, his-ventricle interval 50 milliseconds. Tachycardia was reproducibly induced with atrial programmed stimulation (Figure 2A). The P wave morphology during tachycardia was positive in lead I and aVL, biphasic in lead II, and predominantly negative in lead III and aVF. It exhibited a variable ventricle-atrial time and a cycle length of 370 milliseconds, with occasional episodes of AV block (Figure 2B). Ventricular overdrive pacing demonstrated AV dissociation without atrial entrainment, confirming a diagnosis of focal AT. The earliest atrial activation was initially recorded in the anterior/anteroseptal right atrium with proximal-to-distal coronary sinus activation. High-density electroanatomical mapping with pentaspline catheter revealed a broad area of early activation on the interatrial septum (max 29 milliseconds, Figure 2C), without a discrete focal point. His bundle electrograms were located approximately 8 mm from the region of earliest atrial activation. Left atrial mapping after transseptal puncture under fluoroscopic guidance did not demonstrate earlier activation. Multiple RF applications at 35 W, 30 seconds each in the right anteroseptal atrium failed to terminate the arrhythmia.
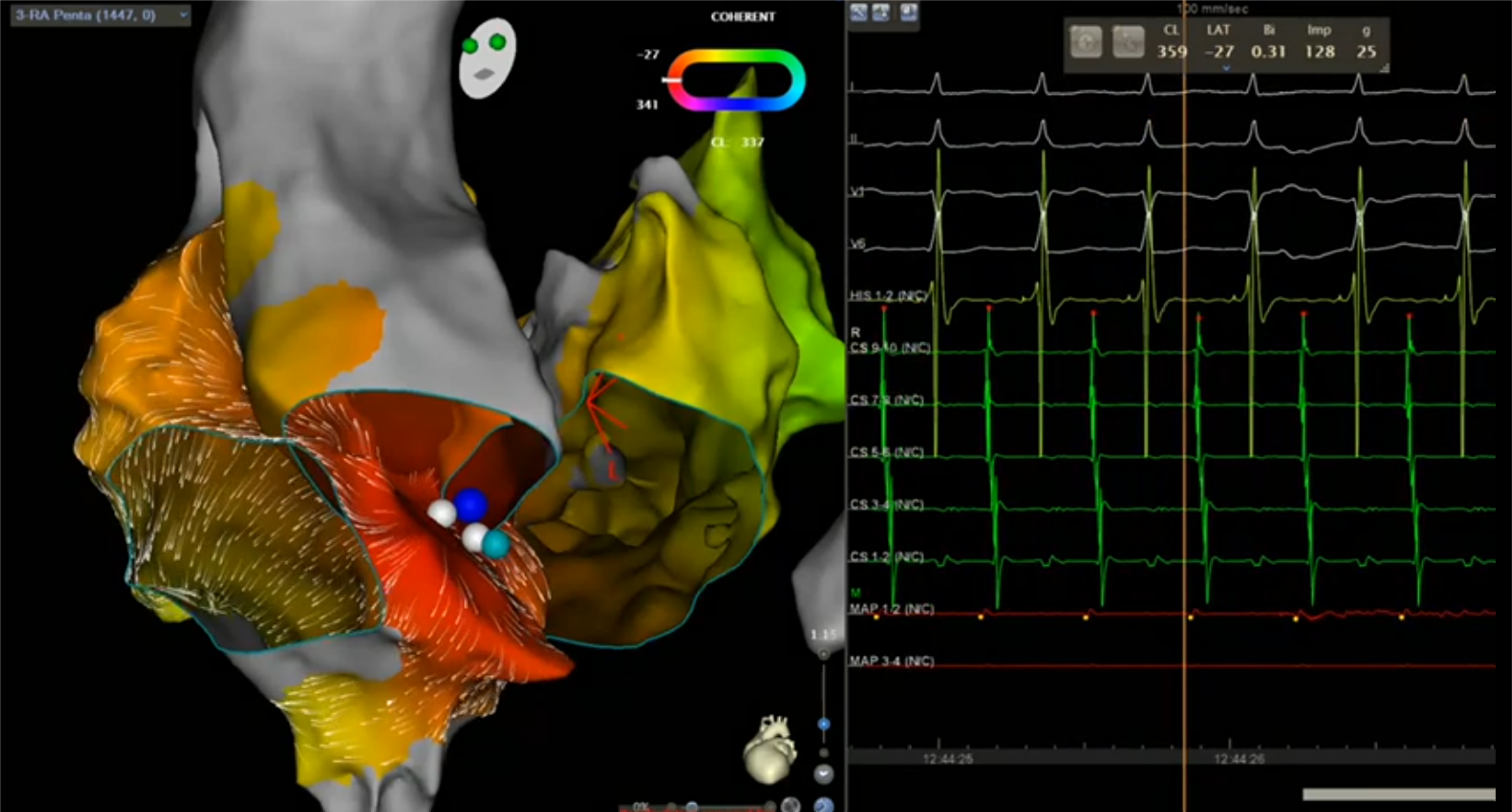
Given the close anatomical relationship between the anteroseptal right atrium and the aortic root, mapping was extended to the aortic bulb via femoral arterial access. The earliest atrial electrogram was identified at the NCC, preceding the surface P wave by 36 milliseconds (Figure 2D). RF energy (35-40 W, 60 seconds) delivered at this site resulted in im
After the final ablation, tachycardia was no longer inducible, even under high-dose isoproterenol infusion. No AV conduction disturbances or vascular complications occurred. The patient was discharged without antiarrhythmic medi
Focal AT is the least common SVT. AT may be difficult to distinguish from other narrow-complex tachycardias. Differential diagnosis is crucial to establishing the proper treatment. AT may have specific characteristics, such as “warm-up” and “cool-down” phases, which are uncommon in other SVT and may help differentiate it. In addition, conducting a thorough electrophysiological study is mandatory to establish the final diagnosis. Recognizing the A-A-V electrogram response following cessation of ventricular overdrive pacing (VAAV response), especially during tachycardia with 1:1 ventricular-atrial conduction. Another characteristic of AT is the variability in tachycardia cycle length, particularly changes of 15 milliseconds or more that predict ventricular cycle length changes, may indicate AT. Finally, AT can be excluded as the underlying mechanism of burst pacing consistently terminates the tachycardia without affecting atrial activation[8].
This case illustrates several important diagnostic and therapeutic aspects of anteroseptal focal AT. First, adenosine sensitivity and intermittent AV block during tachycardia strongly indicated a focal atrial mechanism, excluding typical AV nodal reentry or accessory pathway–mediated tachycardia[9]. Second, although the earliest activation was recorded in the right anteroseptal atrium, ablation at this site was ineffective. This finding supports the concept that some para-hisian tachycardias originate from intramural tissue or from atrial myocardium adjacent to extracardiac structures, particularly the aortic root[4]. Anatomically, the NCC lies in close proximity to the AV septum and the anteroseptal right atrium. Embryologically, remnants of atrial myocardium may persist within this region and serve as an arrhythmogenic substrate. These features explain why the NCC can be a critical site for both mapping and ablation of para-Hisian AT[4]. Several series have reported acute success rates exceeding those of right or left atrial septal approaches, with a low incidence of complications[5,6,10-12]. Ablation from the NCC offers additional advantages, including improved catheter stability and a greater safety margin from the compact AV node and his bundle. In summary, this case confirms that when conventional atrial ablation is unsuccessful or potentially hazardous, systematic mapping of the NCC should be considered early in the management of anteroseptal focal AT.
The NCC should be considered a first-line or early alternative ablation target for adenosine-sensitive anteroseptal focal AT, particularly when atrial septal ablation is ineffective or carries a high risk of AV block.
| 1. | Roberts-Thomson KC, Kistler PM, Kalman JM. Focal atrial tachycardia II: management. Pacing Clin Electrophysiol. 2006;29:769-778. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 24] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 2. | Qian ZY, Hou XF, Xu DJ, Yang B, Chen ML, Chen C, Zhang FX, Shan QJ, Cao KJ, Zou JG. An algorithm to predict the site of origin of focal atrial tachycardia. Pacing Clin Electrophysiol. 2011;34:414-421. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 17] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 3. | Kistler PM, Chieng D, Tonchev IR, Sugumar H, Voskoboinik A, Schwartz LA, McLellan AJ, Prabhu S, Ling LH, Al-Kaisey A, Parameswaran R, Anderson RD, Lee G, Kalman JM. P-Wave Morphology in Focal Atrial Tachycardia: An Updated Algorithm to Predict Site of Origin. JACC Clin Electrophysiol. 2021;7:1547-1556. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 29] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 4. | Markowitz SM. What Is the Optimal Approach to Ablation of Para-Hisian Atrial Tachycardias? JACC Clin Electrophysiol. 2016;2:200-202. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 5. | Lyan E, Toniolo M, Tsyganov A, Rebellato L, Proclemer A, Manfrin M, Nechepurenko A, Morozov A, Abdrahmanov A, Gromyko G, Lyashenko V, Yakovleva M. Comparison of strategies for catheter ablation of focal atrial tachycardia originating near the His bundle region. Heart Rhythm. 2017;14:998-1005. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 24] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 6. | Barkagan M, Michowitz Y, Glick A, Tovia-Brodie O, Rosso R, Belhassen B. Atrial Tachycardia Originating in the Vicinity of the Noncoronary Sinus of Valsalva: Report of a Series Including the First Case of Ablation-Related Complete Atrioventricular Block. Pacing Clin Electrophysiol. 2016;39:1165-1173. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 12] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 7. | Pap R, Makai A, Szilágyi J, Klausz G, Bencsik G, Forster T, Sághy L. Should the Aortic Root Be the Preferred Route for Ablation of Focal Atrial Tachycardia Around the AV Node?: Support From Intracardiac Echocardiography. JACC Clin Electrophysiol. 2016;2:193-199. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 14] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 8. | Knight BP, Zivin A, Souza J, Flemming M, Pelosi F, Goyal R, Man C, Strickberger SA, Morady F. A technique for the rapid diagnosis of atrial tachycardia in the electrophysiology laboratory. J Am Coll Cardiol. 1999;33:775-781. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 224] [Cited by in RCA: 181] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 9. | Liu CF, Cheung JW, Ip JE, Thomas G, Yang H, Sharma S, Markowitz SM, Lerman BB. Unifying Algorithm for Mechanistic Diagnosis of Atrial Tachycardia. Circ Arrhythm Electrophysiol. 2016;9:e004028. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 22] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 10. | Kriatselis C, Roser M, Min T, Evangelidis G, Höher M, Fleck E, Gerds-Li H. Ectopic atrial tachycardias with early activation at His site: radiofrequency ablation through a retrograde approach. Europace. 2008;10:698-704. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 15] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 11. | Das S, Neuzil P, Albert CM, D'Avila A, Mansour M, Mela T, Ellinor PT, Singh J, Patton K, Ruskin JN, Reddy VY. Catheter ablation of peri-AV nodal atrial tachycardia from the noncoronary cusp of the aortic valve. J Cardiovasc Electrophysiol. 2008;19:231-237. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 46] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 12. | Ouyang F, Ma J, Ho SY, Bänsch D, Schmidt B, Ernst S, Kuck KH, Liu S, Huang H, Chen M, Chun J, Xia Y, Satomi K, Chu H, Zhang S, Antz M. Focal atrial tachycardia originating from the non-coronary aortic sinus: electrophysiological characteristics and catheter ablation. J Am Coll Cardiol. 2006;48:122-131. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 131] [Cited by in RCA: 119] [Article Influence: 6.0] [Reference Citation Analysis (0)] |