Published online May 16, 2026. doi: 10.12998/wjcc.v14.i14.119832
Revised: February 16, 2026
Accepted: March 23, 2026
Published online: May 16, 2026
Processing time: 79 Days and 20.3 Hours
Spinal trauma is a major cause of morbidity, with cervical injuries being the most common type. Desert safari dune bashing, a popular tourist activity, poses a sig
A case series of five patients involved in a single sand dune vehicle rollover. Clinical, radiological, and management data were retrieved from hospital elec
Sand dune rollover vehicle crashes can cause complex, multi-level spinal fractures even if the patients are neurologically intact. Awareness of these mechanisms can aid in preventing these injuries, ensuring appropriate immobilization, rapid diagnosis, and timely management to prevent secondary neurological injuries.
Core Tip: Traumatic spinal injury is a major cause of morbidity, with cervical injuries being the most common type. Desert safari dune bashing, a popular tourist activity, poses a significant risk due to various maneuvers and exposes occupants to flexion-extension, axial loading, and rotational injuries of the spine. Rollover crashes on dunes exert unique forces on occupants, often leading to spinal injuries. Mixed forces analysis and understanding injury patterns assist in prognosis and prevention. Awareness of these mechanisms can aid in preventing these injuries, ensuring appropriate immobilization, rapid diagnosis, and timely management to prevent secondary neurological injuries.
- Citation: Dar PMUD, Arumugam SK, Hakim S, Peralta R, El-Menyar A, Rizoli S, Al-Thani H. Force analysis of mechanism and pattern of spinal trauma in sand dune vehicle crash: Five case reports. World J Clin Cases 2026; 14(14): 119832
- URL: https://www.wjgnet.com/2307-8960/full/v14/i14/119832.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i14.119832
Worldwide, 5.37 million people were living with spinal fractures in 2021, with approximately 7.5 million new cases reported that year[1,2]. The age-standardized prevalence rate is about 65 per 100000 population[3]. Motor vehicle accidents are the leading cause of spinal injuries, with males accounting for 80% of cases[4]. Spine injuries contribute to emergency department visits by tourists, highlighting the specific risks associated with popular desert safari activities. The primary external forces that cause spinal injuries include flexion, extension, compression, rotation, and shear[5]. Most spinal cord injuries occur in the cervical spine (60%), and mortality is mainly due to respiratory failure[6,7]. The ASIA scoring system is commonly used to assess the management and neurological outcomes of spinal injuries[8]. Patients may present with paraplegia or quadriplegia, depending on the injury level.
Rollover car crashes on sand dunes expose occupants to unique biomechanical forces, often resulting in diverse spinal injuries. Force analysis of these injuries’ mechanisms is crucial for predicting prognosis and developing preventive strategies. The main aim of this study is to analyze the mechanisms and patterns of spinal injuries sustained during rollover car crashes on sand dunes.
The following five patients were brought to the Trauma Resuscitation Unit by emergency medical services (Table 1). We have named the patients as cases 1-5 to maintain patient data confidentiality.
| Patient parameters | Case 1 | Case 2 | Case 3 | Case 4 | Case 5 |
| Age (years) | 52 | 39 | 26 | 37 | 48 |
| Sex | Male | Female | Female | Male | Female |
| Sitting row in car | Driver seat | Back seat | Back seat | Front seat | Back seat |
| Chief complaints | Neck and back pain | Neck and back pain | Neck and back pain | Neck and back pain | Back and pelvic pain |
| Neurological exam (motor and sensory) | Intact | Intact | Intact | Intact | Intact |
| Spinal injuries level | Cervical | Cervical | Cervical and thoracic | Cervical and thoracic | Thoracic |
| Associated injuries | No | Yes | No | No | Yes |
| History of present illness | Sand dune vehicle rollover | Sand dune vehicle rollover | Sand dune vehicle rollover | Sand dune vehicle rollover | Sand dune vehicle rollover |
| History of past illness | None | None | None | None | Hypertension |
| Personal and family history | Nothing significant | Nothing significant | Nothing significant | Nothing significant | Nothing significant |
| Laboratory results | Unremarkable | Unremarkable | Unremarkable | Unremarkable | Unremarkable |
| Management | Conservative | Surgery | Surgery | Conservative | Conservative |
| Hospital stay (days) | 5 | 10 | 10 | 5 | 5 |
| Outcome | Improved and neurologically intact | Improved and neurologically intact | Improved and neurologically intact | Improved and neurologically intact | Improved and neurologically intact |
Case 1: A 52-year-old male was brought in by Emergency Medical Services via air ambulance after being an unrestrained driver in a motor vehicle accident. On arrival, he was alert and hemodynamically stable, with a Glasgow Coma Scale (GCS) score of 15. He reported neck and upper back pain.
Case 2: A 39-year-old female, an unrestrained back seat passenger, was ejected from a vehicle and presented with neck and back pain.
Case 3: She was a 26-year-old unrestrained female who presented conscious, oriented to time, place, and person, and hemodynamically stable. She reported neck and upper back pain. Power and sensation were intact in all four limbs.
Case 4: He was a 37-year-old male patient who was hemodynamically stable, with preserved power and sensation in all four limbs.
Case 5: A 48-year-old female back seat passenger was found lying face down on the dunes with shallow breathing and a low GCS of 8/15. She was intubated at the scene and brought to the Trauma Resuscitation Unit. On arrival, she was hemodynamically stable with a GCS of 3/15.
As detailed in Table 1.
As detailed in Table 1.
As detailed in Table 1.
As detailed in Table 1.
As detailed in Table 1.
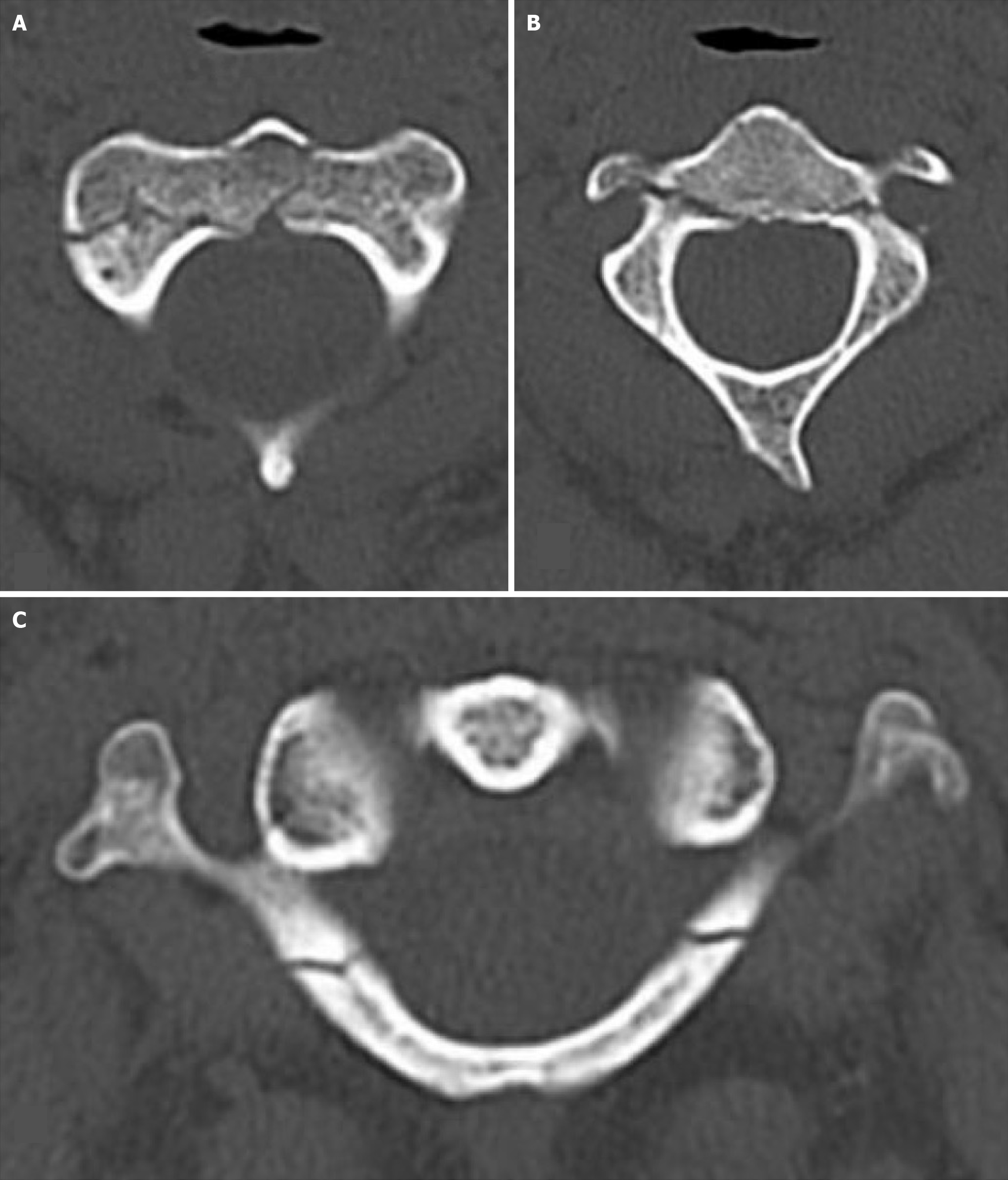
Case 1: Chest and pelvic X-rays were normal, and the Extended-Focused Assessment with Sonography for Trauma (e-FAST) examination was negative. Motor strength and sensation were intact in all four limbs. Pan-computed tomography (CT) revealed a fracture at the base of the odontoid process of the axis (C2) vertebra, with extension into the vertebral body (type III) and right lateral mass (Figure 1). Cervical spine magnetic resonance imaging (MRI) showed intact spinal ligaments and no spinal cord injury. Magnetic resonance angiography demonstrated normal opacification of bilateral vertebral arteries without dissection or aneurysm. This type III odontoid fracture likely resulted from combined flexion and axial loading, a mechanism common in unrestrained drivers during rollovers.
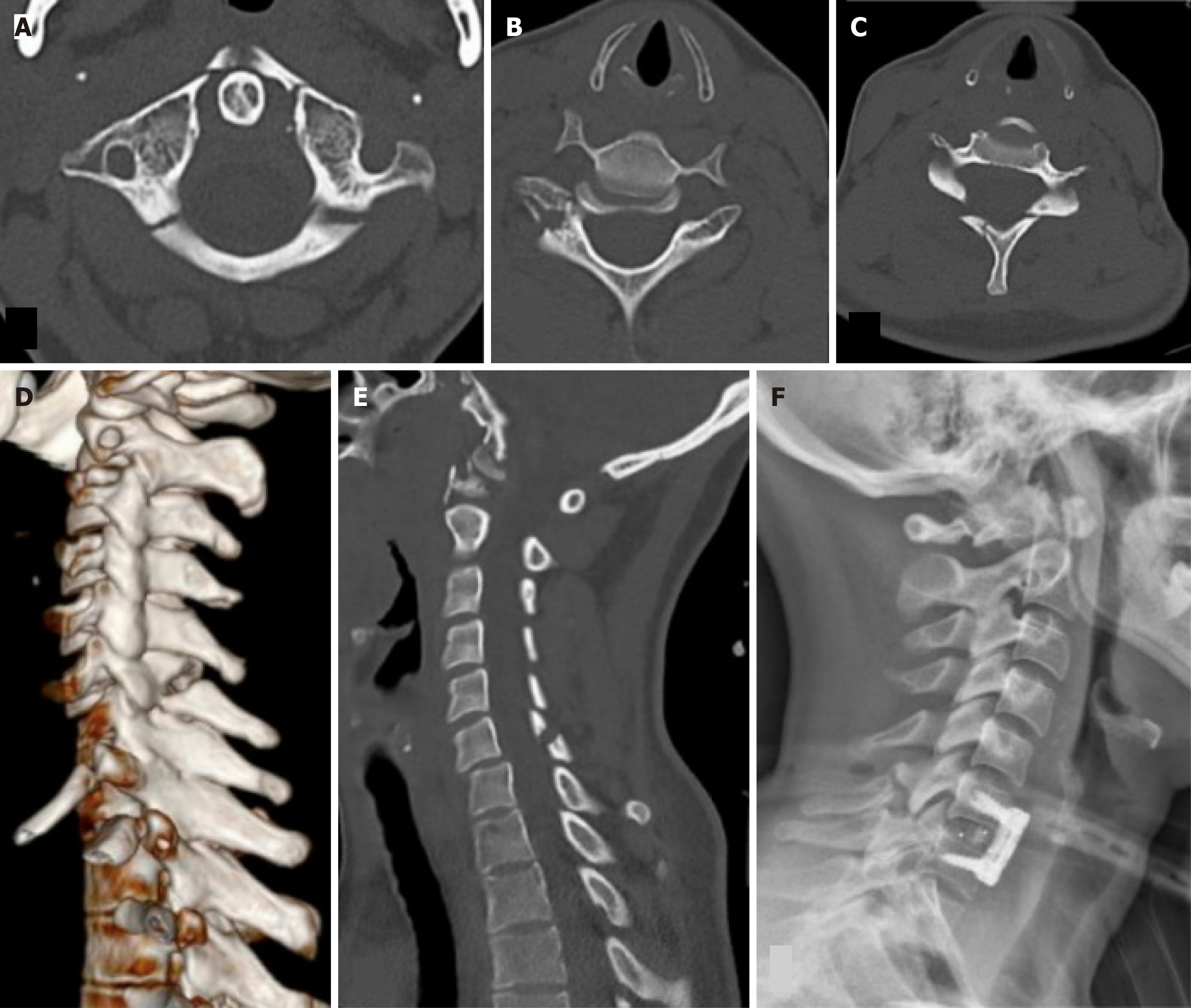
Case 2: Pan CT scan revealed a complex, multi-level injury pattern consistent with a high-energy rollover ejection. She sustained a Jefferson fracture (type III) of the Atlas (C1), bilateral facet joint fractures at C6-C7 with grade 1 spon
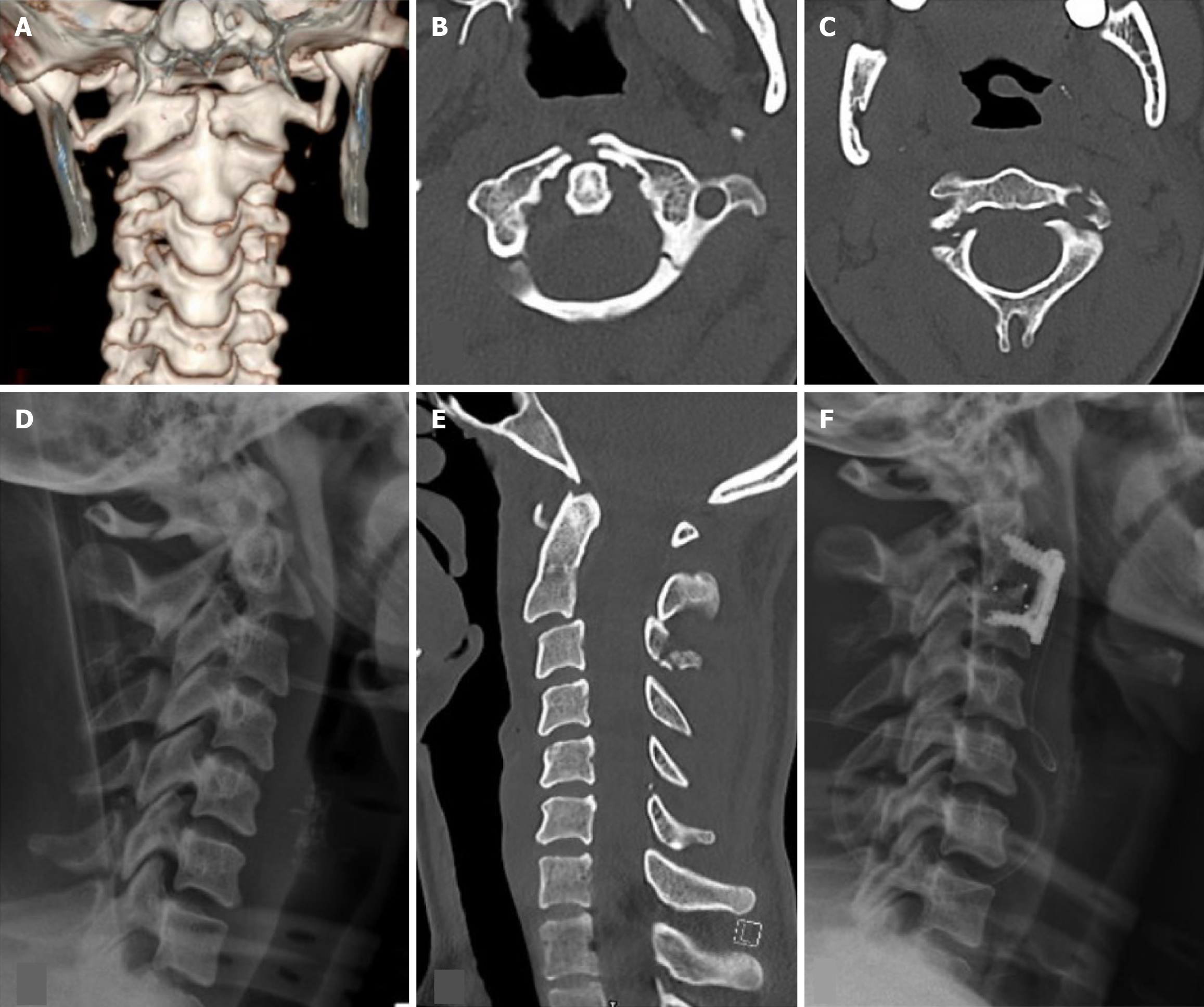
Case 3: The e-FAST was negative, and chest and pelvic X-rays were normal. A pan-CT scan revealed a Jefferson fracture (Figure 3A and B) of the first cervical vertebra (C1), a Hangman fracture (Figure 3C) of the second cervical vertebra (C2) with grade I spondylolisthesis of C2 over C3 (Figure 3D and E), a right facet joint fracture at C6-C7, and a fracture of the anterosuperior endplate of the fourth thoracic vertebra (T4). MRI confirmed these spinal injuries, along with disruption of the anterior Atlanto-occipital membrane on the right, injuries to the apical, transverse, and anterior longitudinal ligaments. Additional injuries included bilateral lung contusions.
Case 4: The e-FAST was negative, and both chest and pelvic X-rays were normal. Pan-CT scan revealed a C4 spinous process fracture, an anterior compression fracture of the vertebral body, and a fracture of the left superior articular process of the 7th thoracic vertebra (T7). MRI of the spine confirmed these findings and additionally showed interspinous and supraspinous ligament injuries at C3-C4 and C4-C5, intervertebral disc protrusion at C6-C7, causing spinal canal narrowing and abutting the cervical cord without significant compression, anterior wedging and mild compression with retropulsion of T7, and a compression fracture of T8.
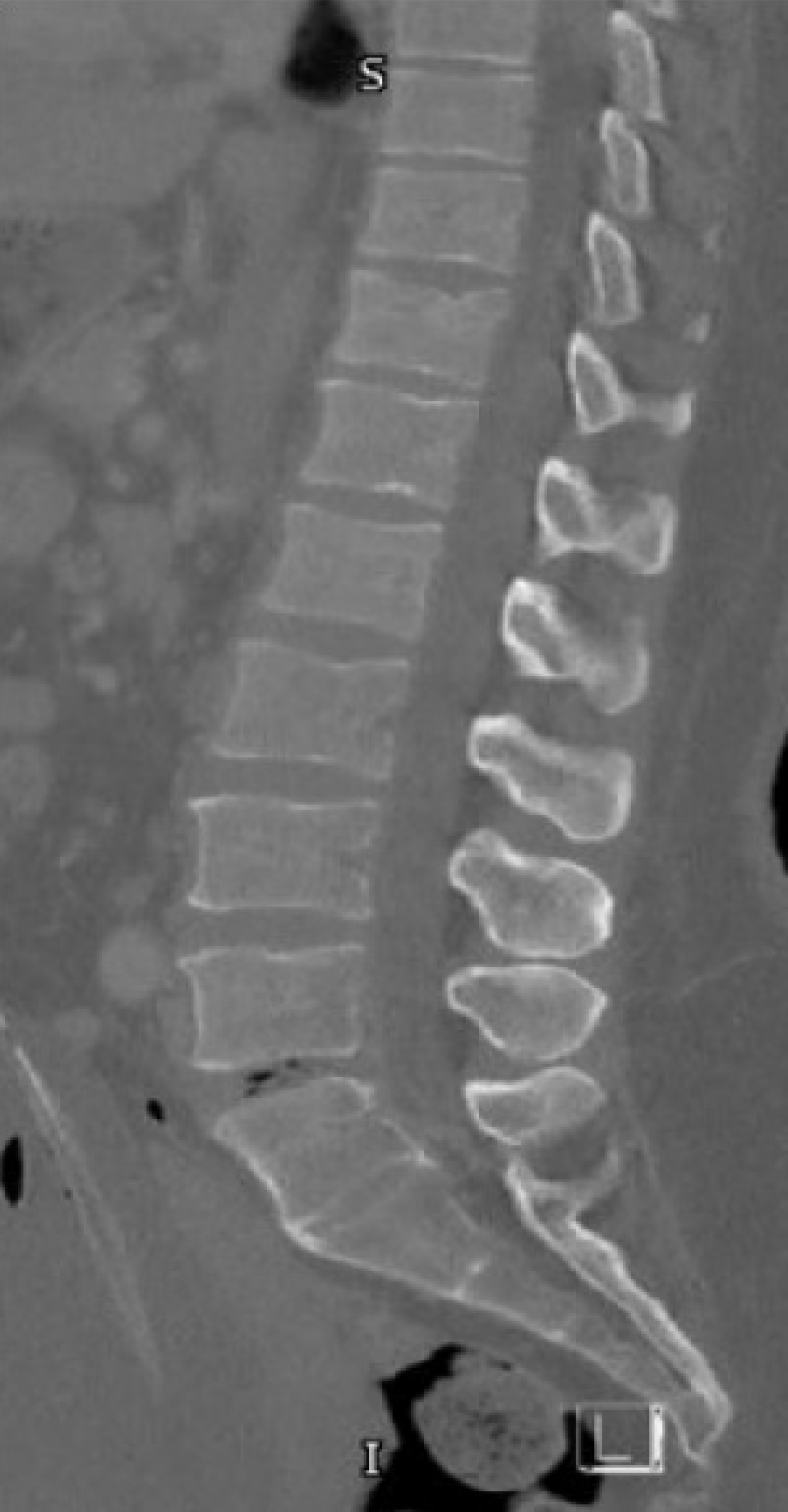
Case 5: e-FAST was negative, and a pan-CT revealed a T12 vertebral fracture. Additional injuries included an epidural hematoma in the basal cisterns, pituitary fossa, and parasellar areas, ethmoid sinus fracture, nasal bone fracture, right lung contusions, and fractures of the left acetabulum and iliac bone.
Trauma, neurosurgery, orthopedic, and radiology teams.
All cases were diagnosed as blunt traumatic spinal injuries.
The patient was admitted to the Trauma Intensive Care Unit for observation, managed conservatively with pain medications and a cervical collar, and discharged successfully on the fifth day.
Initially, she was managed with a halo vest for the Jefferson fracture and subsequently underwent anterior cervical discectomy and fusion (ACDF) at C6-C7 (Figure 2) ten days after admission. This combination of biomechanical mechanisms explains the instability and the need for surgical stabilization, unlike the relatively stable Jefferson fracture, which is managed conservatively with a halo vest.
She was admitted to the Trauma Intensive Care Unit, initially managed with a halo vest, and underwent C2-C3 ACDF three days later (Figure 3F). She was discharged ten days after admission. The pattern of injuries reflects a combined high-energy axial and hyperextension-flexion mechanism. The Jefferson fracture resulted from axial loading via the occipital condyles. The Hangman fracture with grade I spondylolisthesis reflects a classic hyperextension-distraction mechanism involving posterior tension and anterior shear forces on the pars interarticularis. The C6-C7 facet fracture may have resulted from hyperflexion with shear, while the T4 endplate fracture likely resulted from localized axial compression. The ligamentous injuries confirmed the multi-directional nature of the forces involved, with both tensile and compressive components acting across different cervical levels. This biomechanical complexity justified the staged management: Initial halo vest immobilization, followed by definitive C2-C3 ACDF.
He was managed conservatively with a thoracolumbar brace and was successfully discharged after five days. This injury pattern reflects a combined flexion-compression mechanism with associated ligamentous failure. The C4 spinous process fracture and cervical interspinous/supraspinous ligament injury suggest a flexion-distraction component, while the disc protrusion at C6-C7 is likely due to shear forces during flexion. The T7 anterior compression with retropulsion and the T8 compression fracture are consistent with axial compressive loading, resulting in a wedge deformity of the thoracic spine. The combination of bony fractures and posterior ligamentous disruption highlights the mixed forces sustained during the rollover.
She received conservative management for the T12 fracture and other injuries and underwent surgical fixation for her pelvic fracture. Her GCS improved; she was extubated and later transferred to the ward, where she was discharged after 5 days. The thoracolumbar junction marks the transition between the rigid thoracic and flexible lumbar spine, making it vulnerable to injury. The T12 vertebral body fracture resulted from axial compression. The rollover accident caused vertical loading and flexion forces, leading to a wedge-shaped T12 fracture. Associated craniofacial injuries suggest a high-energy deceleration mechanism, while the pelvic ring fracture reflects secondary axial load transmission during ejection and ground impact.
The patient experienced clinical improvement with preserved neurological status. At the four-month follow-up, the patient’s pain had subsided, there was no neurological deficit, and power was preserved in all limbs.
The patient experienced clinical improvement with preserved neurological status. At the one-month follow-up, she was on a halo vest brace to stabilize the head and cervical spine. Neck pain was improving, and power in the limbs was preserved.
The patient experienced clinical improvement with preserved neurological status. The patient was discharged in stable condition and subsequently returned to her home country, where she continues follow-up care and is no longer followed at our hospital.
The patient experienced clinical improvement with preserved neurological status. At six-month follow-up, he reported resumed active participation in outdoor activities, marking a successful recovery trajectory.
The patient experienced clinical improvement with preserved neurological status. The patient was discharged in stable condition and later returned to her home country. She is now receiving follow-up care there and is no longer being followed up at our hospital.
Spine injuries usually result from a sudden traumatic impact on the spine that fractures or dislocates the vertebrae. Awareness of the anatomy of the spine is important for understanding normal biomechanics, and there are four main mechanisms of primary spinal injury: Impact with persistent pressure, Impact with transient pressure, distraction injury, and transection or laceration[9,10].
The atlas (C1) has no vertebral body and is composed of the anterior arch, posterior arch, and lateral masses. It articulates superiorly with the occipital condyles and inferiorly with the axis (C2) and plays a vital role in flexion, extension, and rotation of the cervical spine. The axis (C2) is composed of the odontoid process, which extends superiorly from the vertebral body of C2. The shape of C3-C7, thoracic and lumbar spinal vertebrae, is similar and resembles more classic vertebrae with a body, pedicle, spinous processes, and facet joints. The C1-C7 vertebrae have transverse foramina, and the vertebral arteries pass through them from C6-C1.
Ligaments play an essential role in maintaining the spine’s stability. The transverse ligament holds the odontoid process firmly against the anterior arch and prevents the anterior translation of C1 on C2[11]. The alar ligaments running bilaterally from the odontoid process form a confluence to the medial occipital condyles and the anterior arch of the atlas and prevent the excessive lateral and rotational motion. The alar ligament, along with the apical ligament, is the secondary stabilizer of the head and spine. The anterior longitudinal ligament and the posterior longitudinal ligament (PLL) stabilize the intervertebral discs. The anterior longitudinal ligament prevents hyperextension, and the PLL prevents hyperflexion[11]. The posterior ligamentous complex (supraspinous ligament, interspinous ligament, and ligamentum flavum) plays a vital role in the stability of the cervical spine.
The range of motion in the cervical spine comprises flexion 80%-90%, extension 70%, lateral flexion 20%-40%, and rotation on either side up to 90%. The whole cervical spine is divided into four units, including the cradle (atlas/C1), axis (C2), root (C2-C3 junction), and the column (C3-C7)[11]. The spinal injuries are classified according to the predominant force applied. The main primary external forces that can lead to cervical spine injury include flexion, extension, com
Anterior atlantoaxial subluxation: It occurs due to a flexion/shear force that disrupts the transverse ligament of the atlas[12] and is an infrequent injury. Such injuries can occur in motor vehicle crashes and tackling during football play. The second case in our series sustained the C1 and C2 fracture and grade 1 spondylolisthesis. He has a disruption of the anterior atlantooccipital membrane and anterior longitudinal ligament with injury to the nuchal and interspinous ligaments. Another patient (case 3) in our series has a Jefferson fracture (Figure 3) and a Hangman fracture (Figure 3). MRI of the spine showed disruption of the anterior atlantooccipital membrane on the right, injury to the apical ligament, transverse ligament, and anterior longitudinal ligament.
Odontoid process fracture: The odontoid process fracture is one of the most common fractures of the cervical spine and accounts for about 10% of all cervical spine injuries[13]. Both extension and flexion forces can cause this fracture. When the flexion/shear force is the cause of an odontoid fracture, there is anterior displacement of C1 on C2. The forward flexion of the cervical spine transmits shear forces to the base of the odontoid process, while axial load contributes to extension into the vertebral body and lateral mass. This type of injury pattern reflects the vulnerability of the craniovertebral junction to high-speed rollover trauma. The absence of ligamentous or vascular injury explains the patient’s stability and favorable prognosis with conservative management.
These injuries are usually asymptomatic unless they cause compression of the spinal cord. Odontoid process fractures are classified into three types, and management depends on the fracture level. A type 1 fracture of the odontoid process occurs at its tip and is usually managed nonoperatively. Type 2 fracture occurs at the base of the odontoid process. This type has a high rate of nonunion due to compromise in vascularity after fracture. These fractures are managed surgically, with either a halo or a C1-C2 fusion. In type 3, the fracture extends through the body of the atlas. These can be managed conservatively[13]. If there is injury to the surrounding ligaments along with the fracture on MRI, it indicates an unstable C1-C2 complex and necessitates surgery. In our series, one patient (case two) had a fracture at the base of the dens (odontoid process) with extension into the vertebral body and the right lateral mass (Figure 1). He was successfully managed conservatively.
Facet dislocation: The dislocation of the facet occurs when the flexion/distraction force, along with the rotatory force, is applied to the cervical spine. The inferior articular facet of the upper cervical level moves over the superior articular facet of the lower cervical level. It can be unilateral or bilateral and usually affects the C4-C5 or C5-C6 levels. The patient often presents with radiculopathy of an existing nerve root. Unilateral injuries are more stable than bilateral facet injuries. Bilateral facet dislocation is usually associated with spinal cord injury because of the anterolisthesis of the vertebral body. These injuries can be managed with axial in-line traction and some cervical spine flexion. Close reduction should be abandoned if neurological symptoms worsen. In the present series, case two had a bilateral facet joint fracture at the C6-C7 level with grade 1 spondylolisthesis of C6 over C7, with a fracture extending to the posterior elements of C6. This patient was managed with ACDF (Figure 2). Another patient (case three) had a right C6-C7 facet joint fracture and was managed conservatively with a stiff collar.
Flexion teardrop fracture: These fractures occur when combined flexion and compression forces act simultaneously on the spinal column. Usually, these injuries can occur in head-first shallow pool dives and are associated with a higher chance of quadriplegia. These are unstable injuries and require decompression and surgical stabilization.
Whiplash injury: This type of injury occurs due to rapid upper cervical spine flexion coupled with lower cervical spine extension relative to the spine’s normal resting position after impact. Usually occurs in rear-end impact during motor vehicle accidents. The possible injuries include injury to the intervertebral disc and/or zygapophyseal joints.
Traumatic spondylolisthesis: This type of injury results from the extension and distraction of the cervical spine and occurs when there is a hyperextension force centered on the chin or during judicial hanging. The hyperextension caused a fracture of the pars interarticularis of C2. This type of injury can also lead to PLL disruption, C2-C3 intervertebral disc damage, and bilateral facet fractures/dislocations[14]. It is also called a Hangman’s fracture; however, the most common cause is motor vehicle accidents. One patient (case two) in our series had grade 1 spondylolisthesis of C6 over C7, along with Hangman fracture and other spinal injuries. This patient was neurologically intact and was managed with a halo vest application and C2-C3 ACDF.
Axial compression injuries: The axial compression injury of the spine is the type of spinal trauma that occurs when a vertical force is transmitted along the axis of the spine. It can result from a load applied caudally via the head or torso. The former can result from superior-inferior head impact, and the latter results from the inertia of the torso loading the neck when the head stops relative to the body. In a rollover crash, occupants interact with the vehicle roof, and caudal impact loading may result when the roof intrudes vertically against the occupant’s head. In our series, all patients experienced axial loading as they struck the vehicle’s roof during the rollover. To contextualize the intensity of such vertical loading, it is estimated that the peak force exerted in these scenarios can reach a force considerable enough to cause significant spinal injuries.
C1 fracture: The fracture of the atlas constitutes about 2%-13% of all cervical spine injuries and is typically associated with the traumatic axial loading of the head on the lateral masses of C1[15]. This type of injury causes Jefferson fractures, a burst-type fracture of C1 with bilateral fractures of the anterior and posterior arches of the atlas. Other external forces can be applied during this type of fracture, which includes flexion, extension, and rotatory forces. Sometimes, the isolated anterior or posterior arch fractures or a unilateral lateral mass fracture can occur, depending on the combination of forces applied concomitantly with the axial compression[16]. The treatment of this fracture depends on the mechanical stability and neurological status. If the transverse ligament is intact, the injury can be managed with a stiff collar or halo immobilization. If the ligament is injured, treatment will include a C1-C2 fusion or an occipito-cervical fusion. Two of our patients (cases two and three), who were unrestrained back-seat passengers, sustained a Jefferson fracture along with other cervical spine injuries (Figures 2 and 4). Both patients had no neurological deficit and were managed with a halo vest application.
Compression/burst fracture: The axial loading of the cervical spine with the neck in neutral position can cause compression or burst fractures of the vertebral body. As the force is transmitted through the vertebral body, an anterior wedge deformity of the vertebral body occurs. If the force persists, the posterior part of the vertebral body can be retro-pulsed into the canal, potentially resulting in spinal cord injury[16]. Compression fractures of the cervical spine are typically treated with a cervical collar, unless there is injury to the posterior ligamentous complex. Burst fractures are unstable and usually require decompression and fixation[17]. In our series, the mechanism of injury was a vehicle rollover, and all patients sustained axial loading injuries.
Three patients in our series sustained thoracic spine injuries. One had T7 anterior wedging, mild compression with retropulsion, and a T8 compression fracture. Another had a T12 anterior superior endplate fracture (Figure 4). The third patient had a fracture of the anterosuperior endplates of T4.
The spectrum of spinal injuries in our series illustrates the complex coupling effect of multiple forces encountered during high-energy collisions. Axial compression was the predominant loading mechanism, accounting for Jefferson fractures and thoracolumbar compression fractures. Hyperflexion and flexion-distraction forces resulted in disruption of the posterior elements, spondylolisthesis, and spinous process fractures. Hyperextension and shear mechanisms led to Hangman fractures and ligamentous injuries. Notably, the coexistence of tensile and compressive forces across adjacent levels caused multi-level instability, particularly at C6-C7. These combined loading patterns demonstrate that rollover crashes generate simultaneous axial, flexion-extension, and shear forces, resulting in various spinal injuries. Radiological imaging is essential for confirming injuries, assessing spinal stability, and determining appropriate management, whether surgical or conservative.
This case series highlights the severity and complexity of spinal injuries that occur during recreational desert safari rollovers. The main injury mechanism, axial loading combined with flexion-extension, resulted in multi-level cervical and thoracic spine fractures. Prompt spinal immobilization, thorough radiological evaluation, and timely intervention are essential for optimal outcomes. Our findings stress the importance of preventive strategies, such as strict seatbelt use and public awareness, to reduce such injuries. We suggest that operators should verify seat-belt compliance before each dune run to enhance tourist safety. Moreover, a call for tour-operator certification could further extend the reach of these insights beyond the academic realm, ensuring that certified operators uphold safety standards. This study adds to the limited literature on spinal trauma patterns in desert dune rollovers and provides biomechanical insights valuable to trauma physicians in high-risk environments.
| 1. | Dong Y, Peng R, Kang H, Song K, Guo Q, Zhao H, Zhu M, Zhang Y, Guan H, Li F. Global incidence, prevalence, and disability of vertebral fractures: a systematic analysis of the global burden of disease study 2019. Spine J. 2022;22:857-868. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 83] [Article Influence: 20.8] [Reference Citation Analysis (0)] |
| 2. | Lan Y, Chen S, Lan G, Li C, Wei J. Global, regional, and national burden of fracture of vertebral column, 1990-2021: analysis of data from the global burden of disease study 2021. Front Public Health. 2025;13:1573888. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 3. | Bae Y, Kim M, Jeong W, Jang S, Lee SW. Epidemiology and Future Burden of Vertebral Fractures: Insights from the Global Burden of Disease 1990-2021. Healthcare (Basel). 2025;13:1774. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 4. | Lee BB, Cripps RA, Fitzharris M, Wing PC. The global map for traumatic spinal cord injury epidemiology: update 2011, global incidence rate. Spinal Cord. 2014;52:110-116. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 682] [Cited by in RCA: 561] [Article Influence: 46.8] [Reference Citation Analysis (0)] |
| 5. | Cusick JF, Yoganandan N. Biomechanics of the cervical spine 4: major injuries. Clin Biomech (Bristol). 2002;17:1-20. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 58] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 6. | Varma A, Hill EG, Nicholas J, Selassie A. Predictors of early mortality after traumatic spinal cord injury: a population-based study. Spine (Phila Pa 1976). 2010;35:778-783. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 64] [Cited by in RCA: 83] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 7. | Bilello JF, Davis JW, Cunningham MA, Groom TF, Lemaster D, Sue LP. Cervical spinal cord injury and the need for cardiovascular intervention. Arch Surg. 2003;138:1127-1129. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 79] [Cited by in RCA: 75] [Article Influence: 3.3] [Reference Citation Analysis (1)] |
| 8. | Wilson JR, Hashimoto RE, Dettori JR, Fehlings MG. Spinal cord injury and quality of life: a systematic review of outcome measures. Evid Based Spine Care J. 2011;2:37-44. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 59] [Cited by in RCA: 70] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 9. | Dumont RJ, Okonkwo DO, Verma S, Hurlbert RJ, Boulos PT, Ellegala DB, Dumont AS. Acute spinal cord injury, part I: pathophysiologic mechanisms. Clin Neuropharmacol. 2001;24:254-264. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 510] [Cited by in RCA: 527] [Article Influence: 21.1] [Reference Citation Analysis (0)] |
| 10. | Rowland JW, Hawryluk GW, Kwon B, Fehlings MG. Current status of acute spinal cord injury pathophysiology and emerging therapies: promise on the horizon. Neurosurg Focus. 2008;25:E2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 485] [Cited by in RCA: 561] [Article Influence: 33.0] [Reference Citation Analysis (2)] |
| 11. | Bogduk N, Yoganandan N. Biomechanics of the cervical spine Part 3: minor injuries. Clin Biomech (Bristol). 2001;16:267-275. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 118] [Cited by in RCA: 95] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 12. | Yang SY, Boniello AJ, Poorman CE, Chang AL, Wang S, Passias PG. A review of the diagnosis and treatment of atlantoaxial dislocations. Global Spine J. 2014;4:197-210. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 167] [Cited by in RCA: 150] [Article Influence: 12.5] [Reference Citation Analysis (0)] |
| 13. | Boughton OR, Bernard J, Szarko M. Odontoid process fractures: the role of the ligaments in maintaining stability. A biomechanical, cadaveric study. SICOT J. 2015;1:11. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 7] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 14. | Li XF, Dai LY, Lu H, Chen XD. A systematic review of the management of hangman's fractures. Eur Spine J. 2006;15:257-269. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 114] [Cited by in RCA: 125] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 15. | Hadley MN, Dickman CA, Browner CM, Sonntag VK. Acute traumatic atlas fractures: management and long term outcome. Neurosurgery. 1988;23:31-35. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 143] [Cited by in RCA: 109] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 16. | Mead LB 2nd, Millhouse PW, Krystal J, Vaccaro AR. C1 fractures: a review of diagnoses, management options, and outcomes. Curr Rev Musculoskelet Med. 2016;9:255-262. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 50] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 17. | Feuchtbaum E, Buchowski J, Zebala L. Subaxial cervical spine trauma. Curr Rev Musculoskelet Med. 2016;9:496-504. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 36] [Article Influence: 3.6] [Reference Citation Analysis (0)] |