Published online May 6, 2026. doi: 10.12998/wjcc.v14.i13.119779
Revised: February 26, 2026
Accepted: March 17, 2026
Published online: May 6, 2026
Processing time: 73 Days and 19 Hours
Patients with psychiatric diagnoses who are subjected to surgical treatments are at risk of abusing and becoming dependent on opioids, which requires alternate measures to manage pain. One might expect that regional blocks and multimodal analgesia can be effective solutions to minimizing opioid exposure without failing to treat pain somehow in the perioperative period.
To determine the efficacy and safety of regional blocks and multimodal analgesia in patients with psychiatric disorders at risk of opioid misuse.
This systematic review was conducted based on the PRISMA 2020 guidelines. We searched electronic databases for randomized controlled trials (RCTs) and observational studies that investigated regional blocks and multimodal analgesia in psychiatric patients or individuals at risk of misusing opioids. Quality of studies was evaluated by two independent reviewers applying the Cochrane Risk of Bias tool for RCTs and the Newcastle-Ottawa Scale for observational research. Analysis of the quality of evidence was conducted using the Grading of Recommendations Assessment, Development, and Evaluation system.
Nine of the studies were RCTs, and ten observational studies met the inclusion criteria. Multimodal strategies that were associated with highly positive opioid reduction (30-70 percent) were regional blocks, systemic lidocaine, esketamine-dexmedetomidine combinations, and magnesium sulfate. These findings were established in actual practice using observational studies, especially in the trauma and colorectal surgical groups. The recovery rates were higher, and the scores for quality were non-significantly improved using opioid-sparing procedures. An inter-reviewer agreement was found to be substantial (κ = 0.82).
Regional blocks and multimodal analgesia result in an effective reduction in the use of opioids without com
Core Tip: Regional blocks and multimodal analgesia reduce perioperative opioid use while preserving effective pain control. These approaches benefit surgical patients at high risk of opioid misuse including those with psychiatric illness. Evidence specific to psychiatric populations remains limited and optimal strategies should be tailored to the psychiatric profile surgical context and long term risk of dependence.
- Citation: Tilokani H, Shahzad A, Rafique Malik B, Shehzadi A, Jawed I, Bin Gulzar AH, Rehman A, Ikram J, Khan S, Mal M, Zakeri MA. Efficacy and safety of regional blocks and multimodal analgesia in psychiatric patients at risk of opioid misuse: A systematic review. World J Clin Cases 2026; 14(13): 119779
- URL: https://www.wjgnet.com/2307-8960/full/v14/i13/119779.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i13.119779
Mental illness and pain management during the surgery are special in terms of modern anesthesiology and surgery[1,2]. Pre-procedure substance use disorder, depression, anxiety, and bipolar condition patients have an extremely high risk of opioid misuse, dependence, and poor outcomes after a surgical treatment procedure[3,4]. The prevalence of psychiatric comorbidities among surgical patients is also growing, and recent research demonstrates that in major surgery patients, comorbid mental health issues affect up to 30 percent of patients and can contribute to developing problematic opioid use[1,5].
The conventional opioid-based pain management procedures have been found to be insufficient and even harmful in this group, which contributes to a higher rate of chronic opioid dependence, a longer recovery period, and a high level of morbidity[6,7]. The ongoing opioid epidemic has compounded the need to develop alternative interventions that have effective analgesic efficacy and at the same time carry minimal risk of being addictive[8]. Recent population-level analyses have demonstrated substantial geographic and demographic disparities in cardiovascular and substance-related mortality in the United States, underscoring the broader systemic consequences of medication misuse and the need for preventive, opioid-sparing strategies[9,10]. The interrelation of neurobiological predispositions that psych patients have, such as distorted perception of pain, lack of stress adaptability, and sensitivity to addictive drugs, is complex and requires a specific approach to care during the perioperative period[3,4].
Regional anesthesia and multimodal analgesia have been reported to be options as opposed to using the opioid based pain management systems[11,12]. These strategies take advantage of the synergy between different pharmacological and non-pharmacological therapies to prevent more extensive use of opioids to manage the pain. Regional blocks, such as neuraxial, peripheral nerve, and fascial plane blocks, can be used to achieve a specific level of analgesia with minimal systemic absorption and low side effects[11-13]. Multimodal analgesia utilizes analgesics in combination to target multiple pain sites simultaneously, including acetaminophen, nonsteroidal anti-inflammatory drugs, gabapentinoids, N-methyl-D-aspartate receptor antagonists, and alpha-2 agonists[14-17].
The adoption of enhanced recovery after surgery (ERAS) programs has only added further gravitas to the methods of opioid reduction, proving to have better patient outcomes and shorter recovery time[11,14]. Nonetheless, the particular use and efficacy of these measures in psychiatric patients who are at risk of opioid misuse have not been sufficiently explored[2]. There is a dearth of evidence-based practices to refer to when examining the best practices in managing pain in this vulnerable population. The level of comorbidity of psychiatric conditions, possible drug interactions, and impaired pharmacokinetics requires special attention in such patients and requires special studies that will allow certainty in the application of safe and effective regimens related to the perioperative period[1,4].
It is also important to gain awareness of the efficacy and safety record of regional blocks and multimodal pain management which is going to be essential to creating entire perioperative care plans that not only meet the needs in theory of pain control but also balk risks of addiction[6,18]. This systematic review synthesizes the available evidence on the use of opioid-sparing methods in psychiatric patients and those at higher risk, in order to present clinicians with evidence-based guidance on maximizing the perioperative results and reducing the costs of opioid-related harm.
The PRISMA guidelines of conducting systematic reviews and meta-analyses (PRISMA 2020 statement) were followed in the conduct of this systematic review. The aim of the review was to effectively evaluate the efficacy and safety of regional blocks and multimodal analgesia in psychiatric patients at risk of opioid misuse. The study protocol was registered with PROSPERO under the ID CRD420251233068.
To maintain an organized and thorough approach to identifying and selecting literature, the PICO (Population, Intervention, Comparison, Outcome) framework was used to formulate the research question. This systematic search strategy helped formulate focused search criteria and define inclusion and exclusion criteria for the study selection. The PICO framework was used to define the scope of the present systematic review, and a systematic search of evidence was conducted across multiple electronic databases:
Population (P): Adult patients (≥ 18 years) with psychiatric diagnoses or mental health conditions who are at high risk of opioid misuse or have substance use disorders and require perioperative pain management;
Intervention (I): Regional anesthesia techniques (neuraxial blocks, peripheral nerve blocks, fascial plane blocks); multimodal analgesia protocols incorporating non-opioid analgesics; opioid-that spare pain management strategies; and ERAS procedures with reduced opioid use;
Comparison (C): Normal opioid-based pain management; traditional analgesia protocols; placebo or control groups receiving conventional care; and usual care practices or historical controls.
Primary outcomes: Opioid consumption (intraoperative and postoperative); pain scores (Visual Analog Scale, Numeric Rating Scale); and quality of recovery measures (QoR-40, QoR-15).
Secondary outcomes: Length of hospital stay; time to first analgesic request; safety outcomes and adverse events; patient satisfaction scores; functional recovery measures; long-term opioid use patterns; and psychiatric stability measures.
We systematically searched PubMed, EMBASE, the Cochrane Central Register of Controlled Trials, and Web of Science from inception through January 2026 to identify studies evaluating opioid-sparing perioperative pain management strategies in adult surgical patients, including those with psychiatric diagnoses or at high risk for opioid misuse. Grey literature or conference abstracts were not included in our study. The keywords and controlled vocabulary terms included combinations of: Psychiatric disorders, mental health conditions, substance use disorder, opioid use disorder, regional anesthesia, neuraxial block, peripheral nerve block, fascial plane block, multimodal analgesia, opioid-sparing, ERAS, perioperative pain management, opioid consumption, pain score, and quality of recovery.
The inclusion criteria were randomized clinical trials and observational studies of regional anesthesia, multimodal analgesia regimens, or opioid-sparing approaches in patients with mental illnesses or high opioid-misuse risk. Eligible studies had to report primary outcomes such as opioid consumption, pain score, quality of recovery, or safety.
The exclusion criteria were case reports, case series with fewer than 10 patients, studies involving pediatric populations (under 18 years), non-English publications, and studies lacking measures of interest. Unpublished studies and conference abstracts were excluded to ensure the quality and completeness of the data. We could not include non-English studies because of resource limitations as translating these studies accurately would require paid services.
Individuals who participated in the screening (two independent reviewers, reviewer A and reviewer B) used pre-designed eligibility criteria to evaluate the titles, abstracts, and full-text articles. The resolution of the disagreements was determined through discussion and consultation with a third reviewer when necessary. The coefficient of agreement measure between the inter-reviewers was Cohen’s kappa coefficient.
The data were extracted systematically using standardized forms that recorded the characteristics of the studies, demographic data of the participants, descriptions of the interventions, outcome measures, and safety data. In the case of randomized controlled trials (RCTs), the extracted data included the mode of randomization, mode of blinding, sample size, mode of intervention, primary and secondary outcomes, and adverse events. For observational studies, the infor
The Cochrane Risk of Bias tool (RoB 2.0) was used to assess the quality of the included RCTs, which comprises five domains: Randomization process; deviations from intended interventions; missing outcome data; measurement of outcomes; and selection of reported results. All domains were classified as low-risk, with certain concerns, or high-risk of bias.
The observational studies were appraised using the Newcastle-Ottawa Scale, which assesses three domains: The selection of the study groups; comparability of the groups; and the determination of the outcome or exposure. Each category is awarded stars, with a maximum of nine stars indicating its high quality.
The Grading of Recommendations Assessment, Development, and Evaluation (GRADE) methodology was used to determine the overall quality of evidence for major outcomes. The quality of evidence was rated as high, moderate, low, or very low, depending on the study design, risk of bias, inconsistency, indirectness, imprecision, and other factors, such as publication bias and dose-response relationships.
Quantitative meta-analysis was not undertaken because the investigator’s evaluation revealed a significant clinical and methodological heterogeneity of studies, a broad range of surgical populations (bariatric, trauma, colorectal, elderly, chronic pain), psychiatric and substance-use characteristics, age distribution, intervention modes (regional blocks, systemic agents, ERAS protocols, opioid-tapering strategies), outcome-measures (opioid consumption measures, misuse potential, prescription practice), and follow-up period (24 hours to 24 months) (Table 1). Thus, pooling was considered to be inappropriate in cases of insufficient similarity of studies in terms of population, intervention, and outcome structure. Moreover, heterogeneity assessment based on statistics could not be performed because the nature of the interventions and outcomes reporting was too varied.
| Ref. | Design | Population | Sample size | Intervention | Primary outcome | Follow-up |
| Ibrahim et al[11], 2022 | RCT | Sleeve gastrectomy | 60 | Opioid-free + regional blocks | Quality of recovery | 24 hours |
| Accurso et al[12], 2025 | RCT | Laparoscopic abdominal | 120 | Opioid-free + regional blocks | Pain scores, opioid consumption | 48 hours |
| Geng et al[14], 2021 | RCT | Gynecological surgery | 90 | Multimodal analgesia + ERAS | Quality of recovery | 24 hours |
| Wang et al[15], 2025 | RCT | Major abdominal surgery | 200 | Esketamine + dexmedetomidine | Opioid consumption | 72 hours |
| Yurttas et al[16], 2023 | RCT | Bariatric surgery | 80 | Systemic lidocaine | Opioid consumption | 48 hours |
| Sakata et al[17], 2020 | RCT | Bariatric surgery | 62 | Intravenous lidocaine | Opioid consumption, discharge criteria | 24 hours |
| Tsaousi et al[13], 2020 | RCT | Lumbar laminectomy | 74 | Magnesium sulfate multimodal | Pain scores, opioid consumption | 48 hours |
| de Dios et al[19], 2023 | RCT | Trauma surgery | 150 | Multimodal pain regimen | Opioid exposure, pain scores | 30 days |
| Sullivan et al[20], 2024 | RCT | Post-trauma | 88 | Collaborative opioid taper | Opioid reduction, functional outcomes | 6 months |
Considering this high degree of heterogeneity, a qualitative synthesis method was employed and carried out accordingly, following the guidelines for narrative synthesis. The results are presented in a tabulated format, accompanied by a detailed description of study definitions, interventions, and outcomes to facilitate comparison and interpretation, while acknowledging that direct comparisons across studies are not feasible.
The kappa coefficient was used to calculate inter-reviewer agreement with respect to study selection and quality assessment and the following interpretation was applied: 0.00-0.20 (slight agreement), 0.21-0.40 (fair agreement), 0.41-0.60 (moderate agreement), 0.61-0.80 (substantial agreement), and 0.81-1.00 (almost perfect agreement).
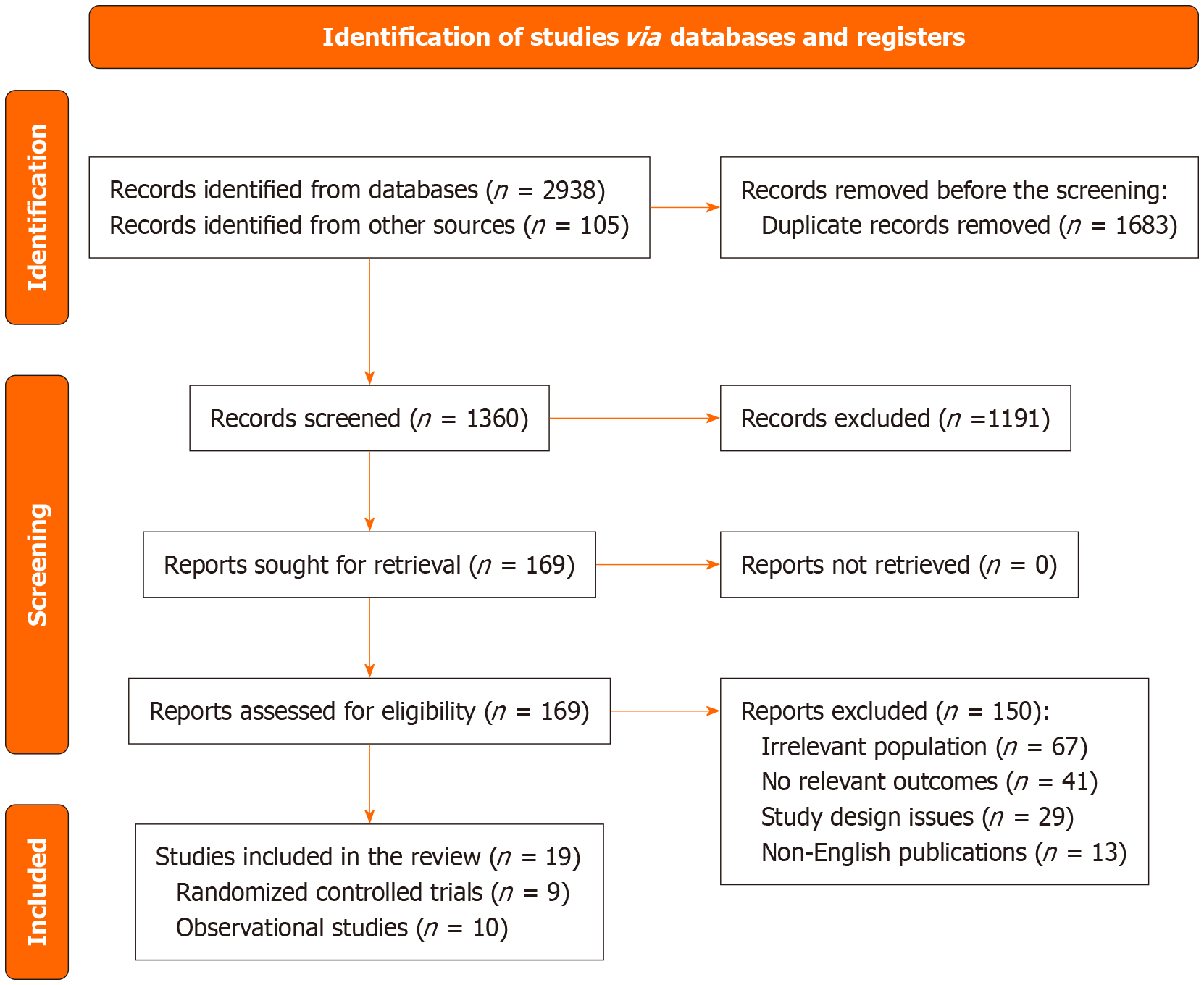
The systematic search and selection process resulted in 19 research studies that fulfilled the inclusion criteria, comprising 9 randomized controlled studies[11-17,19,20] and 10 observational studies[3-7,18,21-24]. The study selection agreement between reviewers was high (k = 0.82, 95% confidence interval: 0.74-0.90), indicating substantial concordance between reviewers. The center of debate mainly involved research that had mixed population groups, in which the proportion of individuals receiving psychiatric treatment varied. The process of selection is depicted in Figure 1.
Study characteristics: Nine RCTs involving different types of surgical procedures and multimodal analgesia methods were included (Table 1). The group of subjects varied in size from 60 people to 200 people, and follow-ups were conducted up to 30 days, including the immediate postoperative period. The types of surgery included bariatric surgery (n = 3), laparoscopic abdominal surgery (n = 3), gynecological surgery (n = 1), lumbar laminectomy (n = 1), and trauma surgery (n = 1).
Quality assessment of RCTs: The overall evaluation in terms of risk of bias demonstrated that the quality of the studies was generally medium to high (Table 2). In the majority of RCTs, a sufficient process of randomization, selection, and outcome measure representation was observed. In other studies, however, it is not easy to blind the subjects and/or personnel due to the type of interventions, i.e., regional block actions.
| Ref. | Randomization | Allocation concealment | Blinding participants | Blinding assessors | Incomplete data | Selective reporting | Overall risk |
| Ibrahim et al[11] | Low | Low | High | Low | Low | Low | Some concerns |
| Accurso et al[12] | Low | Low | High | Low | Low | Low | Some concerns |
| Geng et al[14] | Low | Low | Some concerns | Low | Low | Low | Some concerns |
| Wang et al[15] | Low | Low | Low | Low | Low | Low | Low |
| Yurttas et al[16] | Low | Low | Low | Low | Low | Low | Low |
| Sakata et al[17] | Low | Low | Low | Low | Some concerns | Low | Some concerns |
| Tsaousi et al[13] | Low | Low | Some concerns | Low | Low | Low | Some concerns |
| de Dios et al[19] | Low | Some concerns | High | Low | Low | Low | Some concerns |
| Sullivan et al[20] | Low | Low | High | Low | Some concerns | Low | Some concerns |
Primary outcomes: In seven out of nine RCTs, there were significant decreases in the intake of opioids during surgery using multimodal analgesia methodology (1, 2, 4, 5, 6, 7, 8). For example, Wang et al[15] showed that the consumption of morphine equivalents decreased by 45% (P < 0.001) when using an esketamine-dexmedetomidine combination compared to control groups (4). Similarly, Yurttas et al[16] found a reduction of 52% in the number of opioids needed in patients undergoing bariatric surgery using systemic lidocaine (5). In addition, Sakata et al[17] recorded a 38% decrease in opioid use through intravenous lidocaine plans (6).
The antidote can include complete avoidance of intraoperative opioids because Ibrahim et al[11] and Accurso et al[11] managed to remove them completely and still provide adequate pain management with the help of regional blocks and multimodal analgesia. The postoperative opioid requirements were lower, that is, 65%-70% of those of traditional methods. In a study based on suppliers of magnesium sulfate to the lumbar laminectomy patients, Tsaousi et al[13] demonstrated a substantial opioid reducing effect (7). The multimodal regimen of pain described by de Dios et al[19] was proven to substantially reduce opioid use in high-risk patients with traumas who are prone to misuse (8).
Recovery screening with objective scales, such as the QoR-40 and QoR-15, showed consistent improvement following multimodal analgesia (1, 3). After 24 hours, Ibrahim et al[11] recorded higher QoR-40 scores (median 180 vs 165, P = 0.02) (1). Similarly, Geng et al[14] found that multimodal ERAS protocols improved quality of recovery compared to standard care (3).
The pain scores on Visual Analog Scales or Numeric Rating Scales were found to be slightly lower in the intervention groups, and the differences were clinically relevant (more than 2 points on a 0-10 scale) in six out of nine studies (1, 2, 4, 5, 7, 8). The median time to request the first analgesic was shown to be longer in studies that employed regional block, specifically 6-12 hours, compared to 2-4 hours in the control subjects (1, 2).
In four studies, the length of hospital stay was decreased, with mean reductions ranging from 0.5 to 4.3 days (1, 3, 6, 8). With collaborative care, Sullivan et al[20] established reductions of opioids in 68% of trauma patients on opioid tapering strategies, which persisted at 6-month follow-ups (9).
Study characteristics: Eleven observational studies (10-19) comprising retrospective cohort studies (n = 7) (10-12, 15, 17, 19), prospective cohort studies (n = 3) (13, 14, 16), and cross-sectional studies (n = 1) (18), were included. The number of samples was split between 84 people and 15847 people (Table 3), and the surgical populations and study settings varied.
| Ref. | Design | Population | Sample size | Intervention/exposure | Primary outcome | Follow-up |
| Lenk et al[22], 2022 | Retrospective | Tibial fracture with substance abuse | 92 | Multimodal analgesia | Opioid consumption | 30 days |
| Gedda et al[21], 2023 | Retrospective | Colorectal surgery | 1256 | Multimodal analgesia bundle | Postoperative opioid use | 90 days |
| Wei et al[24], 2019 | Retrospective | Trauma patients | 15847 | Multi-modal pain regimen | Inpatient opioid exposure | Discharge |
| Oldfield et al[6], 2018 | Prospective | Chronic pain with risky opioid use | 84 | Multimodal treatment including buprenorphine | Treatment outcomes | 12 months |
| Moller et al[23], 1998 | Prospective | Elderly surgical patients | 1218 | Anesthesia techniques | Cognitive dysfunction | 3 months |
| Fingerhood et al[18], 2014 | Retrospective | Opioid-dependent patients | 302 | Buprenorphine vs methadone | Treatment retention | 12 months |
| Wasan et al[3], 2015 | Prospective | Chronic low back pain | 370 | Various treatments | Opioid analgesia and misuse | 6 months |
| Rudolph et al[7], 2024 | Retrospective | Medicaid patients | 8945 | Pain management treatments | Opioid use disorder risk | 24 months |
| Grau-López et al[4], 2014 | Cross-sectional | Dual-diagnosis outpatients | 186 | Medication prescriptions | Prescription patterns | Single time point |
| Workman et al[5], 2024 | Retrospective | Veterans with problematic opioid use | 2847 | NLP vs diagnostic codes | Identification methods | Variable |
Quality assessment of observational studies: The quality of observational studies was found to be variable, as indicated by lower quality scores attributed by the Newcastle-Ottawa Scale assessment (Table 4). Studies of higher quality demonstrated a sufficient selection of the cohort, proper similarity between the groups, and adequate outcome evaluation. Some of the studies were rated lower because of poor control of confounding variables, or short-term repeated measure intervals.
Key findings from observational studies: Multimodal analgesia effectively decreased opioid requirements in most studies that included people with varied pathologies[21,22,24]. For instance, the reduction in postoperative opioid consumption following the implementation of multimodal analgesia bundles in colorectal surgery was reported at 43% and proved to be persistent at the 90-day follow-up by Gedda et al[21]. Additionally, standardized multimodal protocols decreased inpatient opioid exposure by 31% in patients with trauma, as demonstrated by Wei et al[24].
The study by Lenk et al[22] was conducted in specifically the substance abuse background patients that were subjected to repair of tibial fractures, where the authors concluded that multimodal treatment strategies provide more effective pain control and less opioid use than opioid-only-based regimens. This cohort was especially susceptible to poor pain management using conventional opioid solutions, and this is why alternative methods need to be considered.
Investigations of psychiatric comorbidities showed that mental health issues are intertwined with pain management outcomes[3,4,6,7,18]. According to Wasan et al[3], psychiatric comorbidity lowered opioid analgesia and elevated the risks of misuse among patients with chronic pain. Oldfield et al[6] were able to present multimodal treatments that were successful in achieving the buprenorphine rotation in risky opioid patients in multidisciplinary pain clinics. The use of medicaid data on a large population scale revealed the trends in relationships between different types of pain treatment services and the risk of opioid use disorder[7]. Grau-López et al[4] also reviewed patterns of medication prescribing in dual-diagnosis outpatients, highlighting the complexity in dealing with the patients. Workman et al[5] provided a comparison of the approaches to the identification of veterans who use opioids and are problematic in that regard, noting the challenges in identifying the at-risk groups.
The GRADE assessment of the results of opioid reductions was moderate quality evidence, and pain control measures showed evidence of low-moderate quality (Table 5). In certain RCTs (and in certain psychiatric groups, even evidence of indirectness), the quality of the evidence was limited due to study heterogeneity and the sample size of the study.
| Outcome | Study types | Risk of bias | Inconsistency | Indirectness | Imprecision | Publication bias | Quality rating |
| Opioid consumption reduction | 9 RCTs, 6 observational | Serious | Not serious | Serious | Not serious | Undetected | ⊕⊕⊕○ moderate |
| Pain scores | 7 RCTs, 4 observational | Serious | Serious | Serious | Serious | Undetected | ⊕⊕○○ low |
| Quality of recovery | 4 RCTs | Not serious | Not serious | Serious | Serious | Undetected | ⊕⊕○○ low |
| Adverse events | 8 RCTs, 5 observational | Serious | Not serious | Not serious | Serious | Undetected | ⊕⊕○○ low |
| Length of stay | 5 RCTs, 3 observational | Serious | Serious | Not serious | Not serious | Undetected | ⊕⊕○○ low |
The safety profiles of multimodal analgesia and regional blocks were generally positive in the included studies. The significantly negative events were few, and the majority of studies showed no substantial difference in the incidence of complications between the intervention and control populations. Side effects that are commonly observed include nausea and vomiting as well as sedation, which is generally less common in multimodal groups since there is less exposure to opioids.
The number of regional block-related complications was low, and there was no record of any permanent neurological damage or significant bleeding complications. No single study reported the occurrence of local anesthetic systemic toxicity; this may be due to the use of dose plans and guidelines, as well as ultrasound application, in most procedures.
Temporary cognitive impairment in older patients using some anesthetic procedures was cited in a single RCT that points to the relevance of customized strategies when using them among vulnerable demographics[23]. In all studies, overall mortality did not differ significantly between any of the groups, and the duration of intensive care unit stay was shorter in many of the multimodal analgesia groups[11,21,24].
The findings of this systematic review provide compelling evidence supporting the efficacy and safety of regional blocks and multimodal analgesia in reducing opioid consumption while maintaining effective pain control. The consistent demonstration of 30%-70% reductions in opioid requirements across diverse surgical populations and clinical settings underscores the clinical significance and generalizability of these approaches. However, the specific application to psychiatric patients at risk for opioid misuse remains an area requiring targeted investigation and specialized consideration.
The pathophysiology underlying enhanced opioid misuse risk in psychiatric patients involves complex neurobiological mechanisms including altered neurotransmitter systems, compromised stress-response pathways, and heightened reward sensitivity[1,3,4]. These factors may influence both pain perception and analgesic response, potentially necessitating modified multimodal approaches. The observed benefits of opioid-sparing techniques in high-risk populations suggest particular relevance for psychiatric patients, who may experience superior outcomes with reduced opioid exposure while achieving adequate analgesia through alternative mechanisms[6,22].
Regional anesthesia techniques demonstrated particular promise in providing targeted analgesia with minimal systemic effects[11-13]. The ability to achieve dense sensory blockade while preserving motor function and consciousness represents significant advantages for psychiatric patients who may be particularly vulnerable to opioid-induced cognitive impairment and respiratory depression[2,23]. Fascial plane blocks, peripheral nerve blocks, and neuraxial techniques each offer distinctive benefits depending on surgical site and patient characteristics, providing flexibility in tailoring approaches to individual needs[11,12].
The integration of multimodal analgesia with ERAS protocols has revolutionized perioperative care, emphasizing the synergistic benefits of combining various non-opioid analgesics, regional techniques, and optimized perioperative pathways[11,14]. The consistent improvements in quality of recovery scores across studies suggest that patients not only experience reduced opioid exposure but also achieve superior overall outcomes including faster functional recovery, reduced complications, and improved satisfaction[11,14]. These benefits may be particularly pronounced in psychiatric patients who often face prolonged recovery periods and increased complication rates with traditional opioid-dominant approaches[1].
The role of specific pharmacological agents within multimodal regimens warrants particular attention. Systemic lidocaine demonstrated consistent efficacy in reducing opioid requirements while providing anti-inflammatory and anti-hyperalgesic effects that extend beyond simple analgesic properties[16,17]. The combination of esketamine and dexmedetomidine showed promise in providing both analgesic and potential antidepressant effects, which may be particularly beneficial for psychiatric patients experiencing perioperative mood disturbances[15]. Magnesium sulfate supplementation offered additional benefits through N-methyl-D-aspartate receptor antagonism, potentially reducing central sensitization and chronic pain development[13].
The implementation of collaborative care models, as demonstrated in trauma populations, represents an important advancement in addressing opioid misuse risk through multidisciplinary approaches[20]. The involvement of psychiatrists, addiction specialists, pain management experts, and primary care providers in perioperative planning may be particularly crucial for psychiatric patients at high risk for opioid-related complications[6,18]. These models emphasize the importance of preoperative risk assessment, individualized treatment planning, and extended postoperative monitoring to ensure optimal outcomes while minimizing harm[6,20].
Safety considerations remain paramount when implementing opioid-sparing approaches in psychiatric patients[2,4]. Potential drug interactions between psychiatric medications and multimodal analgesic agents require careful consideration and monitoring. Certain antidepressants may potentiate the effects of tramadol or increase bleeding risk with nonsteroidal anti-inflammatory drugs, while antipsychotic medications may interact with alpha-2 agonists or increase sedation risk with gabapentinoids[4]. The need for individualized dosing based on psychiatric medication regimens and potential altered pharmacokinetics adds complexity to multimodal prescribing in this population[1,4].
The economic implications of implementing opioid-sparing approaches extend beyond immediate healthcare costs to include long-term societal benefits through reduced addiction rates, decreased chronic pain development, and improved functional outcomes[7,21]. The initial investment in regional anesthesia equipment, specialized training, and extended monitoring may be offset by reduced complications, shorter hospital stays, and decreased long-term opioid prescribing[11,21]. For psychiatric patients, these economic benefits may be amplified by the prevention of opioid-related psychiatric exacerbations and the associated costs of extended mental health treatment[1,7].
Current gaps in the literature highlight the urgent need for RCTs specifically designed for psychiatric populations at risk for opioid misuse[1,5]. Most existing studies include mixed populations with limited psychiatric patient representation, making it challenging to draw definitive conclusions about optimal approaches for this vulnerable group. Future research should specifically recruit psychiatric patients, stratify by psychiatric diagnosis and medication regimens, and include longer-term follow-up to assess sustained benefits and potential delayed complications[2,8].
The development of standardized protocols and clinical pathways for psychiatric patients undergoing surgery repre
Training and education requirements for successful implementation of opioid-sparing approaches in psychiatric patients extend beyond traditional anesthesiology and surgery domains to include understanding of psychiatric conditions, medication interactions, and specialized monitoring needs[2,4]. Multidisciplinary education programs should address the distinctive challenges of managing psychiatric patients perioperatively while emphasizing the importance of individualized care and collaborative decision-making[1,6].
The potential for regional anesthesia and multimodal analgesia to reduce long-term opioid dependence and chronic pain development in psychiatric patients represents a significant public health opportunity[7,8]. By intervening during the vulnerable perioperative period, healthcare providers may be able to prevent the transition from acute to chronic pain and reduce the risk of developing opioid use disorders in susceptible individuals[6,19]. This preventive approach aligns with broader public health initiatives aimed at reducing the societal burden of the opioid crisis[7,8].
Future directions for research should include investigation of novel multimodal combinations specifically designed for psychiatric patients, development of predictive models for identifying high-risk individuals, and evaluation of long-term outcomes including psychiatric stability, functional recovery, and quality of life measures[2,5,8]. The integration of digital health technologies and remote monitoring systems may enhance the ability to provide personalized care and early intervention for patients experiencing complications or suboptimal outcomes[5].
This systematic review provides moderate-quality evidence supporting the efficacy and safety of regional blocks and multimodal analgesia in reducing opioid consumption while maintaining effective pain control across diverse surgical populations. However, the specific application of these techniques to psychiatric patients at risk for opioid misuse remains inadequately studied, representing a critical gap in current evidence.
Future research priorities should focus on conducting adequately powered RCTs specifically designed for psychiatric populations, developing standardized protocols for different psychiatric conditions, and evaluating long-term outcomes, including addiction prevention and functional recovery.
| 1. | Buckley PF, Brown ES. Prevalence and consequences of dual diagnosis. J Clin Psychiatry. 2006;67:e01. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75] [Cited by in RCA: 84] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 2. | Aldecoa C, Bettelli G, Bilotta F, Sanders RD, Aceto P, Audisio R, Cherubini A, Cunningham C, Dabrowski W, Forookhi A, Gitti N, Immonen K, Kehlet H, Koch S, Kotfis K, Latronico N, MacLullich AMJ, Mevorach L, Mueller A, Neuner B, Piva S, Radtke F, Blaser AR, Renzi S, Romagnoli S, Schubert M, Slooter AJC, Tommasino C, Vasiljewa L, Weiss B, Yuerek F, Spies CD. Update of the European Society of Anaesthesiology and Intensive Care Medicine evidence-based and consensus-based guideline on postoperative delirium in adult patients. Eur J Anaesthesiol. 2024;41:81-108. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 208] [Cited by in RCA: 167] [Article Influence: 83.5] [Reference Citation Analysis (0)] |
| 3. | Wasan AD, Michna E, Edwards RR, Katz JN, Nedeljkovic SS, Dolman AJ, Janfaza D, Isaac Z, Jamison RN. Psychiatric Comorbidity Is Associated Prospectively with Diminished Opioid Analgesia and Increased Opioid Misuse in Patients with Chronic Low Back Pain. Anesthesiology. 2015;123:861-872. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 84] [Cited by in RCA: 110] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 4. | Grau-López L, Roncero C, Daigre C, Miquel L, Barral C, Gonzalvo B, Collazos F, Casas M. Observational study on medications prescribed to dual-diagnosis outpatients. J Addict Med. 2014;8:84-89. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 17] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 5. | Workman TE, Kupersmith J, Ma P, Spevak C, Sandbrink F, Cheng Y, Zeng-Treitler Q. A Comparison of Veterans with Problematic Opioid Use Identified through Natural Language Processing of Clinical Notes versus Using Diagnostic Codes. Healthcare (Basel). 2024;12:799. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 6. | Oldfield BJ, Edens EL, Agnoli A, Bone CW, Cervone DJ, Edmond SN, Manhapra A, Sellinger JJ, Becker WC. Multimodal Treatment Options, Including Rotating to Buprenorphine, Within a Multidisciplinary Pain Clinic for Patients on Risky Opioid Regimens: A Quality Improvement Study. Pain Med. 2018;19:S38-S45. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 23] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 7. | Rudolph KE, Williams NT, Diaz I, Forrest S, Hoffman KL, Samples H, Olfson M, Doan L, Cerda M, Ross RK. Pain Management Treatments and Opioid Use Disorder Risk in Medicaid Patients. Am J Prev Med. 2024;67:878-886. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 9] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 8. | Mahipal V, Alam MAU. Estimating Heterogeneous Causal Effect of Polysubstance Usage on Drug Overdose from Large-Scale Electronic Health Record. Annu Int Conf IEEE Eng Med Biol Soc. 2022;2022:1028-1031. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 9. | Sohail MU, Batool RM, Saad M, Waqas SA, Cheema AAA, Minhas AMK. States With Highest and Lowest Cardiovascular Disease-Related Mortality in the United States (1999-2019): Top and Bottom 3. Clin Cardiol. 2026;49:e70256. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 10. | Biancuzzi H, Dal Mas F, Brescia V, Campostrini S, Cascella M, Cuomo A, Cobianchi L, Dorken-Gallastegi A, Gebran A, Kaafarani HM, Marinangeli F, Massaro M, Renne A, Scaioli G, Bednarova R, Vittori A, Miceli L. Opioid Misuse: A Review of the Main Issues, Challenges, and Strategies. Int J Environ Res Public Health. 2022;19:11754. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 26] [Cited by in RCA: 36] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 11. | Ibrahim M, Elnabtity AM, Hegab A, Alnujaidi OA, El Sanea O. Combined opioid free and loco-regional anaesthesia enhances the quality of recovery in sleeve gastrectomy done under ERAS protocol: a randomized controlled trial. BMC Anesthesiol. 2022;22:29. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 45] [Article Influence: 11.3] [Reference Citation Analysis (0)] |
| 12. | Accurso G, Rampulla D, Cusenza M, Candela G, Savatteri P, Vetrugno L, Giarratano A, Raineri SM. A blended opioid-free anesthesia protocol and regional parietal blocks in laparoscopic abdominal surgery- a randomized controlled trial. Sci Rep. 2025;15:14097. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 13. | Tsaousi G, Nikopoulou A, Pezikoglou I, Birba V, Grosomanidis V. Implementation of magnesium sulphate as an adjunct to multimodal analgesic approach for perioperative pain control in lumbar laminectomy surgery: A randomized placebo-controlled clinical trial. Clin Neurol Neurosurg. 2020;197:106091. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 19] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 14. | Geng Z, Bi H, Zhang D, Xiao C, Song H, Feng Y, Cao X, Li X. The impact of multimodal analgesia based enhanced recovery protocol on quality of recovery after laparoscopic gynecological surgery: a randomized controlled trial. BMC Anesthesiol. 2021;21:179. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 26] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 15. | Wang W, Chen Y, Li G, Chen Y, Wu J, Shi Y, Zhong M. The Opioid-Sparing Effects of Intraoperative Esketamine Combined with Dexmedetomidine During Laparoscopic Major Abdominal Surgery: A Randomized Controlled Double-Blind Trial. Drug Des Devel Ther. 2025;19:1971-1981. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 16. | Yurttas T, Djurdjevic M, Schnider TW, Filipovic M. Analgesic efficacy of systemic lidocaine using lean body mass based dosing regime versus placebo in bariatric surgery: a prospective, randomised, double-blind, placebo-controlled, single-centre study. Br J Anaesth. 2023;131:122-129. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 13] [Reference Citation Analysis (0)] |
| 17. | Sakata RK, de Lima RC, Valadão JA, Leal PC, Moura EC, Cruz VP, de Oliveira CM. Randomized, Double-Blind Study of the Effect of Intraoperative Intravenous Lidocaine on the Opioid Consumption and Criteria for Hospital Discharge After Bariatric Surgery. Obes Surg. 2020;30:1189-1193. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 27] [Article Influence: 5.4] [Reference Citation Analysis (0)] |
| 18. | Fingerhood MI, King VL, Brooner RK, Rastegar DA. A comparison of characteristics and outcomes of opioid-dependent patients initiating office-based buprenorphine or methadone maintenance treatment. Subst Abus. 2014;35:122-126. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 27] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 19. | de Dios C, Suchting R, Green C, Klugh JM, Harvin JA, Webber HE, Schmitz JM, Lane SD, Yoon JH, Heads A, Motley K, Stotts A. An opioid-minimizing multimodal pain regimen reduces opioid exposure and pain in trauma-injured patients at high risk for opioid misuse: Secondary analysis from the mast trial. Surgery. 2023;174:1463-1470. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 20. | Sullivan MD, Katers L, Wang J, Arbabi S, Tauben D, Baldwin LM. A randomized trial of collaborative support for opioid taper after trauma hospitalization. Subst Abuse Treat Prev Policy. 2024;19:33. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 21. | Gedda C, Nygren J, Garpenbeck A, Hoffström L, Thorell A, Soop M. Multimodal Analgesia Bundle and Postoperative Opioid Use Among Patients Undergoing Colorectal Surgery. JAMA Netw Open. 2023;6:e2332408. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 24] [Article Influence: 8.0] [Reference Citation Analysis (0)] |
| 22. | Lenk E, Strecker SE, Nolan W. Multimodal analgesia is superior to opiates alone after tibial fracture in patients with substance abuse history. OTA Int. 2022;5:e214. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 23. | Moller JT, Cluitmans P, Rasmussen LS, Houx P, Rasmussen H, Canet J, Rabbitt P, Jolles J, Larsen K, Hanning CD, Langeron O, Johnson T, Lauven PM, Kristensen PA, Biedler A, van Beem H, Fraidakis O, Silverstein JH, Beneken JE, Gravenstein JS. Long-term postoperative cognitive dysfunction in the elderly ISPOCD1 study. ISPOCD investigators. International Study of Post-Operative Cognitive Dysfunction. Lancet. 1998;351:857-861. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1607] [Cited by in RCA: 1610] [Article Influence: 57.5] [Reference Citation Analysis (0)] |
| 24. | Wei S, Green C, Truong VTT, Howell J, Ugarte SM, Albarado R, Taub EA, Meyer DE, Adams SD, McNutt MK, Moore LJ, Cotton BA, Kao LS, Wade CE, Holcomb JB, Harvin JA. Implementation of a multi-modal pain regimen to decrease inpatient opioid exposure after injury. Am J Surg. 2019;218:1122-1127. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 30] [Article Influence: 4.3] [Reference Citation Analysis (0)] |