Published online May 6, 2026. doi: 10.12998/wjcc.v14.i13.119644
Revised: March 9, 2026
Accepted: April 1, 2026
Published online: May 6, 2026
Processing time: 80 Days and 16.9 Hours
Thoracic trauma is a major cause of trauma-related morbidity and mortality, often resulting from blunt mechanisms. While advances in acute management have improved short-term outcomes, long-term results-particularly health-related quality of life (QoL) after chest wall surgery-remain poorly defined. Identifying factors influencing long-term QoL is essential to optimize patient care.
To investigate long-term QoL and identify clinical factors influencing outcomes.
Forty-one consecutive patients underwent chest wall surgery for thoracic trauma between November 2016 and November 2024 at our Hospital. Data collected for this retrospective cohort study included demographics, trauma characteristics, surgical details, postoperative complications, hospital and intensive care unit stay, and long-term patient-reported outcomes [EuroQol 5-Dimension 3-Level Questionnaire (EQ-5D-3 L), Numerical Rating Scale (NRS) for pain, and dyspnea scores]. Univariable and multivariable linear regression analyses were performed to identify predictors of QoL and pain.
At a median follow-up of 14 months (range 1-72), the median EQ-5D-3 L score was 0.68 (range 0.027-1), with no significant correlation with follow-up duration (Spearman’s rho = -0.05, P = 0.78). Pain was the only independent predictor of lower QoL (β = -0.079 per NRS unit, P = 0.016). Age, male gender, and comorbidities showed non-significant negative trends with QoL. For pain, a greater number of comorbidities was significantly associated with lower pain scores (β = -0.810, P = 0.041), while male sex was non-significantly associated with less pain. Dyspnea and perioperative variables were not significantly related to either outcome.
Long-term QoL after chest wall surgery is lower than the general population; pain is the main determinant. Effective pain control and comorbidity management are essential for personalized postoperative care.
Core Tip: Long-term outcomes after surgical stabilization of thoracic trauma are poorly characterized. This study shows that health-related quality of life (QoL) remains lower than in the general population even months after surgery. Pain emerged as the only independent predictor of worse long-term QoL, whereas perioperative and trauma-related variables were not significantly associated. Comorbidities influenced pain perception, underscoring their role in recovery. These findings emphasize the need for tailored long-term follow-up strategies focused on pain control and comprehensive management of comorbidities to improve patient outcomes after thoracic trauma surgery.
- Citation: Raveglia F, Degiovanni S, Bertolaccini L, Cara A, Cassina EM, Danuzzo F, Libretti L, Pirondini E, Sibilia MC, Spinelli F, Tuoro A, De Simone M, Chiarelli M, Cioffi U, Petrella F. Beyond survival: Pain as the main determinant of long-term quality of life after thoracic trauma surgery. World J Clin Cases 2026; 14(13): 119644
- URL: https://www.wjgnet.com/2307-8960/full/v14/i13/119644.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i13.119644
Polytrauma is a major global health concern, responsible for approximately 5.8 million deaths annually and remains the leading cause of death, hospitalization, and long-term disability among young adults[1,2]. Thoracic trauma accounts for 20%-25% of all trauma cases. It ranks as the third leading cause of trauma-related mortality after abdominal and head injuries[3,4], being directly or indirectly involved in nearly 50% of trauma-related deaths[5]. Blunt trauma is the most common mechanism[6], often associated with chest wall fractures[7]. Due to its high morbidity and mortality, thoracic trauma has been extensively studied, resulting in evidence-based guidelines that help identify high-risk patients and guide surgical decisions[8,9]. Nonetheless, most available data focus predominantly on short-term postoperative outcomes, such as early morbidity and mortality. While these endpoints are essential, it is crucial to recognize that mortality rates have significantly improved in recent years, primarily due to advances in therapeutic strategies[10]. Consequently, greater attention should be directed toward identifying prognostic factors influencing long-term outcomes [particularly health-related quality of life (QoL), which remains an under-investigated yet critical aspect of patient recovery] and optimizing care pathways. Therefore, the endpoints of the present study are to evaluate the long-term QoL in patients who have undergone chest wall surgery following thoracic trauma, and secondarily, the variables influencing it.
This study specifically included patients who underwent chest wall surgery following thoracic trauma, independent of whether a flail chest was present. It was conducted in accordance with the Declaration of Helsinki, as revised in 2013[11].
This is a single-center, retrospective cohort study conducted at our academic institution. Inclusion criteria were: > 18 years old and presented with one or more rib fractures identified on computed tomography scans that required surgical intervention. Informed consent was obtained from all participants; however, given the emergency setting, written consent for both the surgical procedure and the use of clinical and imaging data for scientific and/or educational purposes was obtained in some cases only after patients were able to clearly express their will. This study is based on data collected within the framework of a research project approved by the Medical Ethics Committee of our institution (No. 4594).
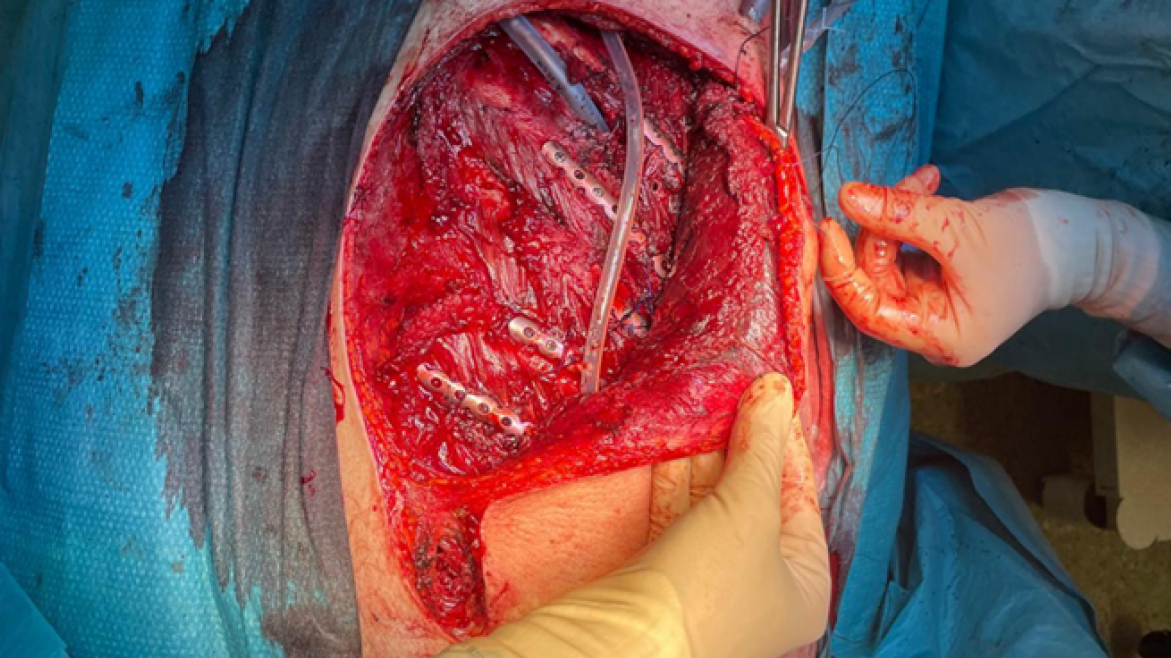
Surgical indication has always been confirmed in accordance with the ongoing guidelines[9]. Rib fixation was always performed by a senior and a junior thoracic surgeon from the same team in our department. Three-dimensional chest reconstruction was always required to determine the surgical strategy. Prophylactic 2 g of Cefazolin i.v. preoperative antibiotic therapy was always administered. Surgical approaches were performed to achieve better chest wall stability and minimal muscle dissection. Therefore, not all fractured ribs were stabilized. To fix the ribs after reduction we used the MatrixRIB system (Depuy Synthes) with at least three bicortical screws on each side of the fracture (Figure 1). However, other techniques have been adopted in some cases.
For each enrolled patients, the following data has been collected from a review of medical records: Demographics (age, sex and comorbidities); trauma characteristics [location, mechanism, Injury Severity Score (ISS), Abbreviated Injury Scale (AIS) and Organ Injury Scale (OIS) scores, and concomitant thoracic or extra thoracic injuries]; number of fractured ribs; days from admission to surgery, type of surgery, surgical technique and duration.
The outcomes evaluated included postoperative in-hospital complications, reoperation rate, pneumonia rate, and mortality rate, as well as hospital and intensive care unit (ICU) length of stay. Long-term outcomes were evaluated using patient-reported parameters, including pain assessed with the Numerical Rating Scale (NRS), QoL assessed with the EuroQol 5-Dimension 3-Level Questionnaire (EQ-5D-3 L) questionnaire, and dyspnea severity assessed with the modified Medical Research Council scale. Postoperative data were obtained from medical records, while long-term patient-related information was collected through telephone interviews.
The primary endpoint of the study was to assess the long-term QoL in patients who underwent thoracic cage surgery for blunt trauma. The secondary endpoint was to investigate the variables that influence QoL.
The EQ-5D-3 L questionnaire, developed by the EuroQol group, is a standardized instrument widely used for measuring health-related QoL. It is commonly used in clinical evaluations of healthcare interventions and in population health surveys. The questionnaire includes five health dimensions: Mobility; self-care; usual activities (e.g., work, study, housework, family or leisure activities); pain/discomfort; and anxiety/depression. For each dimension, respondents indicate their health status by selecting one of three levels of severity: ‘no problems’, ‘some problems’, or ‘extreme problems’. The answers for the five dimensions are then converted into a summary score that indicates overall utility.
Descriptive statistics were used to summarize demographic, clinical, and surgical characteristics. Continuous variables were expressed as median (range) and compared between groups using unpaired Student’s t-tests when normally distributed, or the Mann–Whitney U test when non-normally distributed. Normality was assessed using the Kolmogorov-Smirnov test. Categorical variables were reported as absolute n (%), and differences in their distribution were analyzed using χ2 or Fisher’s exact tests, as appropriate.
Associations between continuous variables (e.g., EQ-5D-3 L scores, pain scores, age, follow-up duration) were evaluated using Spearman’s rank correlation coefficients (rho) when the data were not normally distributed, and Pearson’s correlation coefficients when normality assumptions were met. For each correlation, both the coefficient and the corresponding P value were reported.
Variables showing a P value ≤ 0.10 in univariable analyses, or deemed clinically relevant, were included in multivariable linear regression models to identify independent predictors of EQ-5D-3 L scores and pain levels (NRS). Regression results were expressed as β coefficients, standard errors (SE), 95%CI, and P values.
All tests were two-sided, and statistical significance was defined as P ≤ 0.05. Graphical exploration of associations included scatter plots with regression lines for continuous predictors and kernel density estimates for distributional analysis. Data were analyzed using RStudio (R version 4.4.2, Pile of Leaves).
Between November 2016 and November 2024, 41 consecutive patients underwent chest wall surgery for thoracic trauma. They were predominantly male (70.7%), with a median age of 56.3 years (range: 24-80 years). Comorbidities were present in 48.7% of patients: 24.4% had major comorbidities (such as ischemic heart disease, decompensated diabetes mellitus, epilepsy, and renal failure), and 24.4% had minor comorbidities (including dyslipidemia, hypertension, and depressive disorder). Traumatic mechanisms included vehicle vs non-vehicle collisions (32.1%), vehicle vs vehicle collisions (25.0%), falls from a height less than 2 meters (17.8%) or more than 2 meters (7.1%), and other trauma dynamics (17.8%), such as vehicle-wall collision; no cases involved assault or penetrating injuries. At admission, 17.1% of patients were already intubated or required immediate intubation. Before surgery, 53.65% of patients underwent chest drainage, and 7.31% required intercostal artery embolization.
Patients sustained a median of 9.5 rib fractures (range: 2-20), with sternal fractures observed in 14.6% of cases and flail chest in 65.9%. The overall trauma severity was reflected by a median ISS of 24.3 (range: 4-75), a median AIS of 2.73 (range: 2-4), and a median OIS of 2 (range: 1-5). Among the thoracic injuries observed, pulmonary contusion was the most frequent (78.0%), followed by isolated pneumothorax (53.5%) and pneumothorax associated with other intrathoracic injuries, such as diaphragm or vascular involvement (10.7%). Isolated diaphragmatic injury was reported in 3.5% of cases. Additionally, concurrent extrathoracic trauma was present in 80.4% of patients, involving orthopedic injuries (46.4%), central nervous system trauma (22.0%), visceral injuries (39.0%), and vascular injuries.
All 41 patients underwent rib fixation, including 27 with flail chest and 2 with sternal stabilization. Fixation techniques included plates and screws in 35 cases, sutured cerclages in 2 cases, and a combined approach in 4 cases, one of which involved a polymeric prosthesis. Additionally, 2 diaphragm repairs were performed.
The median length of hospital stay was 23.9 days (range 2-86), with a mean ICU stay of 9.9 days (range 0-43). The median time from admission to thoracic surgery was 5 days (range 0-15).
In-hospital complications included pneumonia (34.0%), cardiac arrhythmia (7.3%), cerebrovascular accident (2.4%), chest wall hematoma (7.1%), and bleeding requiring reoperation (7.3%). One patient died due to concomitant severe brain injury; one additional post-discharge death unrelated to trauma was recorded. Two patients required a new surgical intervention for the displacement of plates that were removed 5 and 24 months after the initial procedure.
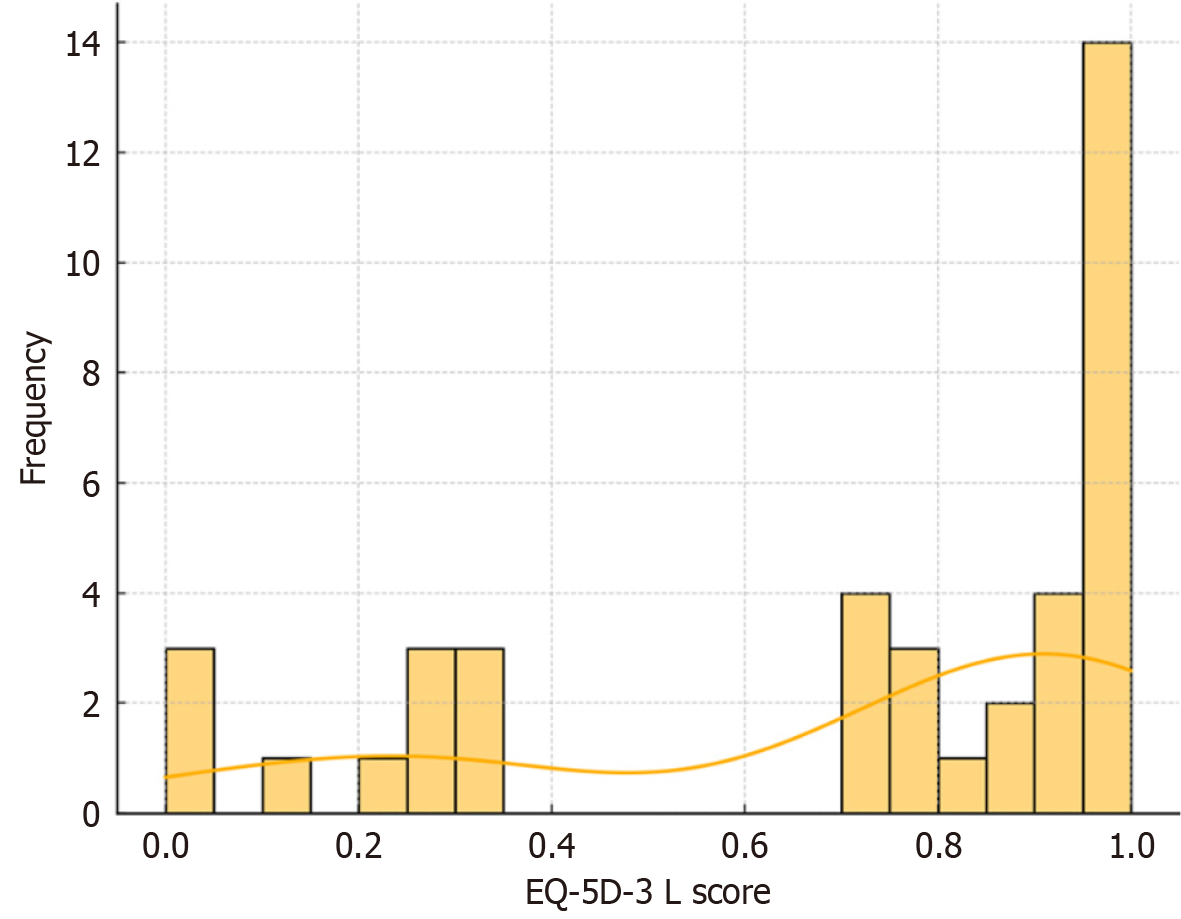
At a median follow-up of 14 months (range 1-72), the median EQ-5D-3 L quality-of-life score was 0.68 (range 0.027-1), with no significant correlation with follow-up duration (Spearman’s rho = -0.05, P = 0.78). The median Numerical Rating Pain Score was 3 (range 1-6), and no meaningful association between follow-up duration and pain scores was observed. None of the patients reported dyspnea at rest, while eight patients (28.5%) reported exertional dyspnea, which was not significantly associated with EQ-5D-3 L scores (P = 0.74).
The EQ-5D-3 L distribution plot effectively highlights the variation in patient scores, potentially revealing clusters that reflect shared characteristics (Figure 2).
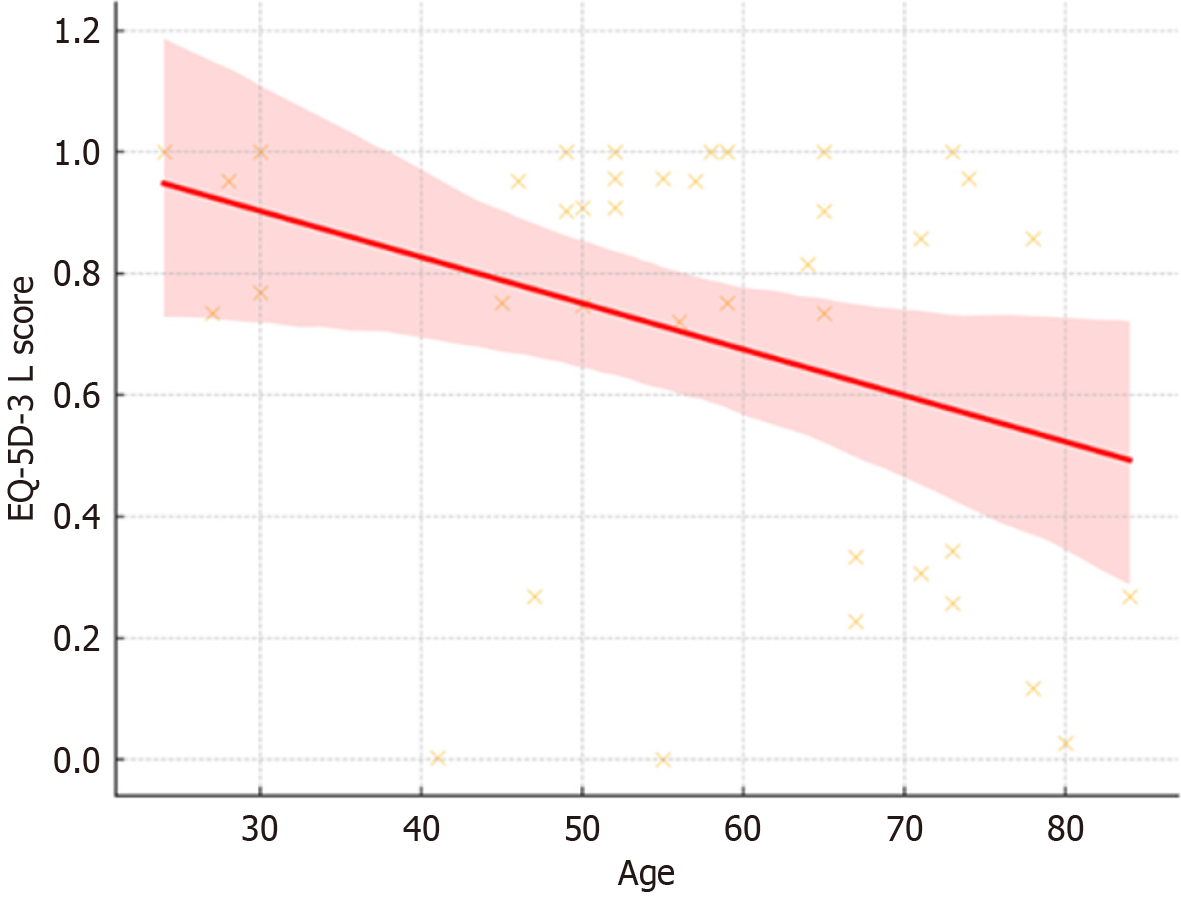
Correlation analysis revealed a moderate negative relationship between EQ-5D-3 L scores and age (Spearman’s rho =
Univariable analysis of predictors of EQ-5D-3 L score and univariable analysis of predictors of pain score (NRS) are reported in Tables 1 and 2.
| Variable | β coefficient (estimate) | SE | 95%CI | P value |
| Age (per year) | -0.006 | 0.003 | -0.012 to 0.000 | 0.072 |
| Sex (male vs female) | -0.105 | 0.120 | -0.348 to 0.138 | 0.380 |
| Number of comorbidities | -0.095 | 0.060 | -0.216 to 0.026 | 0.118 |
| Pain score (NRS) | -0.082 | 0.032 | -0.147 to -0.017 | 0.015 |
| Exertional dyspnea (yes vs no) | -0.045 | 0.140 | -0.326 to 0.236 | 0.745 |
| Total hospital stay (days) | -0.002 | 0.002 | -0.006 to 0.002 | 0.288 |
| ICU stay (days) | -0.003 | 0.004 | -0.011 to 0.005 | 0.430 |
| Variable | β coefficient (estimate) | SE | 95%CI | P value |
| Age (per year) | -0.014 | 0.025 | -0.064 to 0.036 | 0.580 |
| Sex (male vs female) | -0.280 | 0.570 | -1.439 to 0.879 | 0.640 |
| Number of comorbidities | -0.785 | 0.366 | -1.535 to -0.035 | 0.041 |
| EQ-5D-3 L score | -2.190 | 0.840 | -3.890 to -0.490 | 0.013 |
| Exertional dyspnea (yes vs no) | 0.190 | 0.560 | -0.940 to 1.320 | 0.745 |
| Total hospital stay (days) | 0.010 | 0.020 | -0.030 to 0.050 | 0.520 |
| ICU stay (days) | 0.020 | 0.030 | -0.040 to 0.080 | 0.480 |
In the multivariable regression analysis (Table 3), age was negatively associated with EQ-5D-3 L scores (β = -0.007 per year, P = 0.086), approaching statistical significance. Sex (P = 0.37) and comorbidities (P = 0.17) were not significant independent predictors. Pain was significantly and negatively associated with EQ-5D-3 L scores (β = -0.079 per unit increase, P =0.016), indicating that higher pain levels were linked to worse QoL. Dyspnea and length of hospital or ICU stay were not significantly associated with EQ-5D-3 L scores (all P > 0.5).
| Variable | β coefficient | SE | 95%CI | P value |
| Age (per year) | -0.007 | 0.004 | -0.015 to 0.001 | 0.086 |
| Sex (male vs female) | -0.109 | 0.120 | -0.355 to 0.137 | 0.370 |
| Number of comorbidities | -0.111 | 0.080 | -0.274 to 0.052 | 0.170 |
| Pain score (NRS) | -0.079 | 0.031 | -0.143 to -0.015 | 0.016 |
| Exertional dyspnea (yes vs no) | -0.030 | 0.150 | -0.338 to 0.278 | 0.850 |
| Total hospital stay (days) | -0.001 | 0.002 | -0.005 to 0.003 | 0.720 |
| ICU stay (days) | -0.002 | 0.004 | -0.010 to 0.006 | 0.590 |
In the regression analysis of pain levels (Table 4), age was not significantly associated with pain (P = 0.59), and sex showed no significant difference in pain perception (P = 0.64). Comorbidities were significantly associated with lower reported pain levels (β = -0.810, P = 0.041). EQ-5D-3 L scores were inversely and significantly correlated with pain levels (β = -2.189, P = 0.013), indicating that patients with poorer QoL tended to report higher pain levels.
| Variable | β coefficient | SE | 95%CI | P value |
| Age (per year) | -0.012 | 0.023 | -0.058 to 0.034 | 0.590 |
| Sex (male vs female) | -0.291 | 0.605 | -1.517 to 0.935 | 0.640 |
| Number of comorbidities | -0.810 | 0.380 | -1.584 to -0.036 | 0.041 |
| EQ-5D-3 L score | -2.189 | 0.865 | -3.919 to -0.459 | 0.013 |
The role of rib fixation and chest cage surgery in the treatment of blunt chest trauma has been extensively explored over the past decade, with robust evidence supporting the current clinical guidelines. These guidelines primarily focus on identifying optimal indications for surgical referral, based on predictive factors for perioperative mortality and morbidity. However, few studies have investigated long-term outcomes, particularly health-related QoL. This area deserves greater attention because improving postoperative outcomes requires a shift in focus from perioperative management to long-term recovery and functional reintegration.
In our series, mortality was very low (1/41), due to a neurological complication in a multiply injured patient, confirming, together with previous literature, that rib fixation is a safe procedure[12-14]. Complication rates were also low. More importantly, the median EQ-5D-3 L score at a median follow-up of 14 months was 0.68 (range 0.027-1), which, although slightly lower than reported in some studies[15], is consistent with the expected range of 0.60-0.80[16]. Compared to the general Italian population, where EQ-5D-3 L scores typically exceed 0.80[17], our findings indicate a fair, though suboptimal, health status. This suggests that, despite the benefits of surgical treatment, some residual limitations persist that influence patients’ perceived QoL.
Previous studies evaluating have generally documented favorable long-term QoL after rib fixation. A systematic review[18] reported an overall satisfactory long-term QoL following surgical stabilization, with a mean EQ-5D-3 L score of 0.80. Similarly, earlier studies[19] evaluating rib fixation with titanium devices highlighted good QoL outcomes and low levels of residual pain.
When examining determinants of long-term QoL, pain emerged as the only independent factor significantly associated with lower EQ-5D-3 L scores. In the multivariable analysis, each one-point increase in pain score (NRS) was associated with a reduction of 0.079 points in EQ-5D-3 L utility. Previous studies suggest that the minimal clinically important difference for EQ-5D utility values generally ranges between approximately 0.05 and 0.10. Therefore, the magnitude of the observed association suggests that the impact of pain on QoL is not only statistically significant but also potentially clinically meaningful. This aligns with the concept that chronic or persistent pain remains a major driver of post-traumatic morbidity, even when chest wall stability is restored. Age and the number of comorbidities showed a negative, non-significant trend in their relationship with QoL, while male gender also tended toward lower scores without reaching statistical significance. These trends suggest possible underlying biological or psychosocial mechanisms that warrant further exploration in larger datasets.
Regarding pain, our data revealed an inverse association between the number of comorbidities and reported pain levels, which was statistically significant. This finding is not intuitively expected from a clinical standpoint and should therefore be interpreted with caution. One possible explanation is that patients with multiple comorbidities may receive more intensive ongoing medical management, including regular pharmacological treatments that could indirectly improve pain control. However, detailed information on regular analgesic use, chronic pain treatment, psychiatric medications, or structured pain-management programs was not systematically collected and could not be included in the analysis. Therefore, unmeasured differences in medication use or baseline pain perception may have influenced this result. Male sex was also associated with lower pain scores, although this did not reach statistical significance and may reflect differences in pain perception or reporting.
Regarding perioperative variables, our findings differ slightly from those of Peek et al[20], who identified ICU length of stay as a significant determinant of poorer QoL. In our cohort, ICU stay was not significantly related to QoL or pain outcomes. In a previous, smaller study from our group[21], the ISS was found to be a strong predictor of long-term QoL. However, in the current larger dataset, this association did not remain significant in the multivariable model, possibly due to the inclusion of additional variables and the modest sample size.
This study has several limitations, including its small sample size and retrospective, single-center design, which may limit generalizability. Data heterogeneity and the absence of a control group restrict direct comparisons and may introduce bias. In addition, follow-up duration varied widely (1-72 months), which may have introduced heterogeneity in long-term outcomes, particularly because pain perception and functional recovery after thoracic trauma surgery may evolve. Although no significant correlation was observed between follow-up duration and EQ-5D-3 L scores in our cohort, residual temporal effects cannot be excluded. Detailed information regarding regular analgesic use, chronic pain treatment, psychiatric medications, and structured pain-management programs was not systematically available and therefore could not be included in the analysis. These unmeasured factors may have influenced pain perception and could partly explain the unexpected inverse association observed between comorbidities and reported pain levels. Despite these limitations, the study’s strength lies in its long-term follow-up and the integration of patient-reported outcomes with detailed clinical variables.
In our cohort, long-term QoL after surgical stabilization for blunt chest trauma remained lower than that of the general population. Pain emerged as the only independent predictor of poorer EQ-5D-3 L scores, underscoring the importance of effective pain prevention and management strategies in this setting. Male sex and a higher number of comorbidities showed a non-significant trend toward lower EQ-5D-3 L scores, suggesting a possible negative influence on perceived QoL. Conversely, male sex and, in particular, a higher number of comorbidities were associated with lower reported pain scores, with the latter reaching statistical significance. These findings highlight the need for a tailored, multidimensional approach to postoperative care that integrates pain control and comorbidity management to optimize recovery.
| 1. | Chrysou K, Halat G, Hoksch B, Schmid RA, Kocher GJ. Lessons from a large trauma center: impact of blunt chest trauma in polytrauma patients-still a relevant problem? Scand J Trauma Resusc Emerg Med. 2017;25:42. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 134] [Cited by in RCA: 109] [Article Influence: 12.1] [Reference Citation Analysis (0)] |
| 2. | Ziegler DW, Agarwal NN. The morbidity and mortality of rib fractures. J Trauma. 1994;37:975-979. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 546] [Cited by in RCA: 441] [Article Influence: 13.8] [Reference Citation Analysis (0)] |
| 3. | Baker E, Xyrichis A, Norton C, Hopkins P, Lee G. The long-term outcomes and health-related quality of life of patients following blunt thoracic injury: a narrative literature review. Scand J Trauma Resusc Emerg Med. 2018;26:67. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 28] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 4. | Flagel BT, Luchette FA, Reed RL, Esposito TJ, Davis KA, Santaniello JM, Gamelli RL. Half-a-dozen ribs: the breakpoint for mortality. Surgery. 2005;138:717-23; discussion 723. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 438] [Cited by in RCA: 346] [Article Influence: 16.5] [Reference Citation Analysis (0)] |
| 5. | Lundin A, Akram SK, Berg L, Göransson KE, Enocson A. Thoracic injuries in trauma patients: epidemiology and its influence on mortality. Scand J Trauma Resusc Emerg Med. 2022;30:69. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 32] [Reference Citation Analysis (0)] |
| 6. | Singh AK, Prasad G, Mishra P. The Impact of Thoracic Trauma on Morbidity and Outcomes: A Six-Year Experience From a Tertiary Care Level 1 Center. Cureus. 2024;16:e73580. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 7. | Dogrul BN, Kiliccalan I, Asci ES, Peker SC. Blunt trauma related chest wall and pulmonary injuries: An overview. Chin J Traumatol. 2020;23:125-138. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 42] [Cited by in RCA: 143] [Article Influence: 23.8] [Reference Citation Analysis (0)] |
| 8. | Franssen AJPM, Daemen JHT, Luyten JA, Meesters B, Pijnenburg AM, Reisinger KW, van Vugt R, Hulsewé KWE, Vissers YLJ, de Loos ER. Treatment of traumatic rib fractures: an overview of current evidence and future perspectives. J Thorac Dis. 2024;16:5399-5408. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 9. | Sermonesi G, Bertelli R, Pieracci FM, Balogh ZJ, Coimbra R, Galante JM, Hecker A, Weber D, Bauman ZM, Kartiko S, Patel B, Whitbeck SS, White TW, Harrell KN, Perrina D, Rampini A, Tian B, Amico F, Beka SG, Bonavina L, Ceresoli M, Cobianchi L, Coccolini F, Cui Y, Dal Mas F, De Simone B, Di Carlo I, Di Saverio S, Dogjani A, Fette A, Fraga GP, Gomes CA, Khan JS, Kirkpatrick AW, Kruger VF, Leppäniemi A, Litvin A, Mingoli A, Navarro DC, Passera E, Pisano M, Podda M, Russo E, Sakakushev B, Santonastaso D, Sartelli M, Shelat VG, Tan E, Wani I, Abu-Zidan FM, Biffl WL, Civil I, Latifi R, Marzi I, Picetti E, Pikoulis M, Agnoletti V, Bravi F, Vallicelli C, Ansaloni L, Moore EE, Catena F. Surgical stabilization of rib fractures (SSRF): the WSES and CWIS position paper. World J Emerg Surg. 2024;19:33. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 24] [Cited by in RCA: 34] [Article Influence: 17.0] [Reference Citation Analysis (0)] |
| 10. | Hardy BM, Enninghorst N, King KL, Balogh ZJ. The most critically injured polytrauma patient mortality: should it be a measurement of trauma system performance? Eur J Trauma Emerg Surg. 2024;50:115-119. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 11. | World Medical Association. World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA. 2013;310:2191-2194. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24525] [Cited by in RCA: 20922] [Article Influence: 1609.4] [Reference Citation Analysis (16)] |
| 12. | Apampa AA, Ali A, Kadir B, Ahmed Z. Safety and effectiveness of surgical fixation versus non-surgical methods for the treatment of flail chest in adult populations: a systematic review and meta-analysis. Eur J Trauma Emerg Surg. 2022;48:1025-1034. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 7] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 13. | Peek J, Beks RB, Kremo V, van Veelen N, Leiser A, Houwert RM, Link BC, Knobe M, Babst RH, Beeres FJP. The evaluation of pulmonary function after rib fixation for multiple rib fractures and flail chest: a retrospective study and systematic review of the current evidence. Eur J Trauma Emerg Surg. 2021;47:1105-1114. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 16] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 14. | Hisamune R, Kobayashi M, Nakasato K, Yamazaki T, Ushio N, Mochizuki K, Takasu A, Yamakawa K. A meta-analysis and trial sequential analysis of randomised controlled trials comparing nonoperative and operative management of chest trauma with multiple rib fractures. World J Emerg Surg. 2024;19:11. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 15] [Article Influence: 7.5] [Reference Citation Analysis (0)] |
| 15. | Hoepelman RJ, Minervini F, Beeres FJP, van Wageningen B, IJpma FF, van Veelen NM, Lansink KWW, Hoogendoorn JM, van Baal MCP, Groenwold RHH, Houwert RM; NEXT study group. Quality of life and clinical outcomes of operatively treated patients with flail chest injuries: A multicentre prospective cohort study. Front Surg. 2023;10:1156489. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 16. | Beks RB, de Jong MB, Houwert RM, Sweet AAR, De Bruin IGJM, Govaert GAM, Wessem KJP, Simmermacher RKJ, Hietbrink F, Groenwold RHH, Leenen LPH. Long-term follow-up after rib fixation for flail chest and multiple rib fractures. Eur J Trauma Emerg Surg. 2019;45:645-654. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 51] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 17. | Scalone L, Cortesi PA, Mantovani LG, Ciampichini R, Cesana G. Reference Eq-5d-3l and Eq-5d-5l Data From the Italian General Population. Value Health. 2014;17:A514-A515. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 18. | Peek J, Beks RB, Hietbrink F, Heng M, De Jong MB, Beeres FJP, Leenen LPH, Groenwold RHH, Houwert RM. Complications and outcome after rib fracture fixation: A systematic review. J Trauma Acute Care Surg. 2020;89:411-418. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 60] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 19. | Billè A, Okiror L, Campbell A, Simons J, Routledge T. Evaluation of long-term results and quality of life in patients who underwent rib fixation with titanium devices after trauma. Gen Thorac Cardiovasc Surg. 2013;61:345-349. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 27] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 20. | Peek J, Kremo V, Beks R, van Veelen N, Leiser A, Link BC, Houwert RM, Minervini F, Knobe M, Babst RH, Beeres FJP. Long-term quality of life and functional outcome after rib fracture fixation. Eur J Trauma Emerg Surg. 2022;48:255-264. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 17] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 21. | Sibilia MC, Danuzzo F, Spinelli F, Cassina EM, Libretti L, Pirondini E, Raveglia F, Tuoro A, Bertolaccini L, Isgro’ S, Perrone S, Rizzo S, Petrella F. Prognostic Factors and Clinical Outcomes of Surgical Treatment of Major Thoracic Trauma. Healthcare (Basel). 2024;12:1147. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |