Published online May 6, 2026. doi: 10.12998/wjcc.v14.i13.118772
Revised: February 15, 2026
Accepted: March 30, 2026
Published online: May 6, 2026
Processing time: 94 Days and 14.1 Hours
Severe maxillary atrophy complicates implant-supported full-mouth rehabilitation and often precludes conventional implant placement. Although zygomatic implants provide a graftless posterior anchorage option, limited anteroposterior spread may compromise prosthetic biomechanics. This case report highlights a prosthetically driven approach combining zygomatic and nasalis implants to en
A 55-year-old woman presented with partial edentulism of the maxilla and the mandible, seeking fixed dental rehabilitation. Clinical and radiographic evalu
Strategic integration of zygomatic and nasalis implants enables predictable, biomechanically stable full-mouth rehabilitation in severe maxillary atrophy.
Core Tip: Severe maxillary atrophy limits the predictability of conventional implant-supported full-mouth rehabilitation. This case report demonstrates a prosthetically driven strategy integrating zygomatic and nasalis implants to overcome the biomechanical limitations of posterior-only anchorage. Enhanced anteroposterior spread enables immediate loading while reducing cantilever forces and improving prosthetic stability, function, and esthetics. The digitally guided workflow and stepwise clinical protocol presented offer a reliable graftless solution for managing complex maxillary atrophy and improving patient comfort and quality of life.
- Citation: Sarkar D, Srivastava SK, Srivastava S, Shekhar A, Sikdar C, Rana A. Immediate loading full-mouth rehabilitation using zygomatic and nasalis implants with conventional mandibular implants: A case report. World J Clin Cases 2026; 14(13): 118772
- URL: https://www.wjgnet.com/2307-8960/full/v14/i13/118772.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i13.118772
Severe maxillary atrophy represents a complex clinical challenge in implant-supported prosthodontic rehabilitation, frequently compromising both functional and esthetic outcomes. Progressive alveolar bone resorption, maxillary sinus pneumatization, and reduced bone density often preclude the placement of conventional implants by limiting primary stability and long-term osseointegration[1]. Although augmentation procedures such as sinus floor elevation, onlay grafting, or extensive bone grafting have been advocated to restore bone volume, these approaches are associated with increased surgical morbidity, prolonged treatment duration, higher financial burden, and variable predictability, particularly in elderly or medically compromised patients[2].
Zygomatic implants, first introduced as a graftless solution for the rehabilitation of the severely atrophic maxilla, achieve anchorage in the dense zygomatic bone and have demonstrated high survival rates and favorable long-term outcomes[3]. Subsequent refinements, including anatomy-guided placement concepts such as the zygoma anatomy-guided approach, have further enhanced surgical precision and prosthetic outcomes by adapting implant trajectories to patient-specific anatomical variations[4]. Despite these advantages, rehabilitation strategies relying predominantly on posterior zygomatic anchorage may result in a reduced anteroposterior spread and increased prosthetic cantilever forces, potentially affecting long-term biomechanical stability[5].
To address this limitation, recent treatment concepts have emphasized the importance of combining posterior zygo
Compared with pterygoid implants, which require complex posterior anatomical navigation and present a steep learning curve, anterior nasalis implants allow more straightforward access and prosthetically driven positioning. When combined with zygomatic implants, this approach enhances anteroposterior spread, reduces cantilever length, and facilitates immediate loading protocols without the need for bone grafting[6,8].
This technical case report describes a prosthodontically driven full-mouth rehabilitation using a combined approach of zygomatic and anterior nasalis implants in a patient with severe maxillary atrophy. By integrating available evidence with a step-by-step clinical workflow, this report highlights the clinical rationale and potential advantages of this combined graftless strategy as an alternative to augmentation-based or posterior-only anchorage techniques.
A focused literature review was conducted using PubMed and Google Scholar databases with the search terms “severe maxillary atrophy”, “zygomatic implants”, “nasalis implants”, “immediate loading”, and “full-arch implant rehabilitation”. By integrating current evidence with a step-by-step clinical workflow, this report highlights the clinical merit, novelty, and rationale of a combined implant approach and introduces the successful management of a patient requiring fixed full-mouth rehabilitation.
A 55-year-old woman presented to the Department of Prosthodontics with missing teeth in both the maxillary and mandibular arches, resulting in difficulty with mastication, compromised speech, and dissatisfaction with facial esthetics. The patient expressed a desire for fixed dental rehabilitation.
The patient reported progressive tooth loss over several years, primarily due to advanced dental caries and periodontal disease. She had intermittently used removable dental prostheses, which she found uncomfortable and functionally inadequate. The condition progressively worsened, resulting in impaired masticatory efficiency, reduced lower facial height, and loss of lip support, which prompted her to seek definitive fixed implant-supported rehabilitation.
The patient reported no history of systemic diseases, including diabetes mellitus, cardiovascular disorders, osteoporosis, or autoimmune conditions. There was no history of maxillofacial trauma, radiation therapy, bisphosphonate use, prior implant therapy, or maxillofacial surgery.
The patient was a non-smoker and reported no consumption of alcohol or tobacco in any form. There was no relevant family history of systemic disease, craniofacial anomalies, or hereditary bone disorders. Dietary history revealed a preference for a soft diet due to compromised mastication. No parafunctional habits were reported.
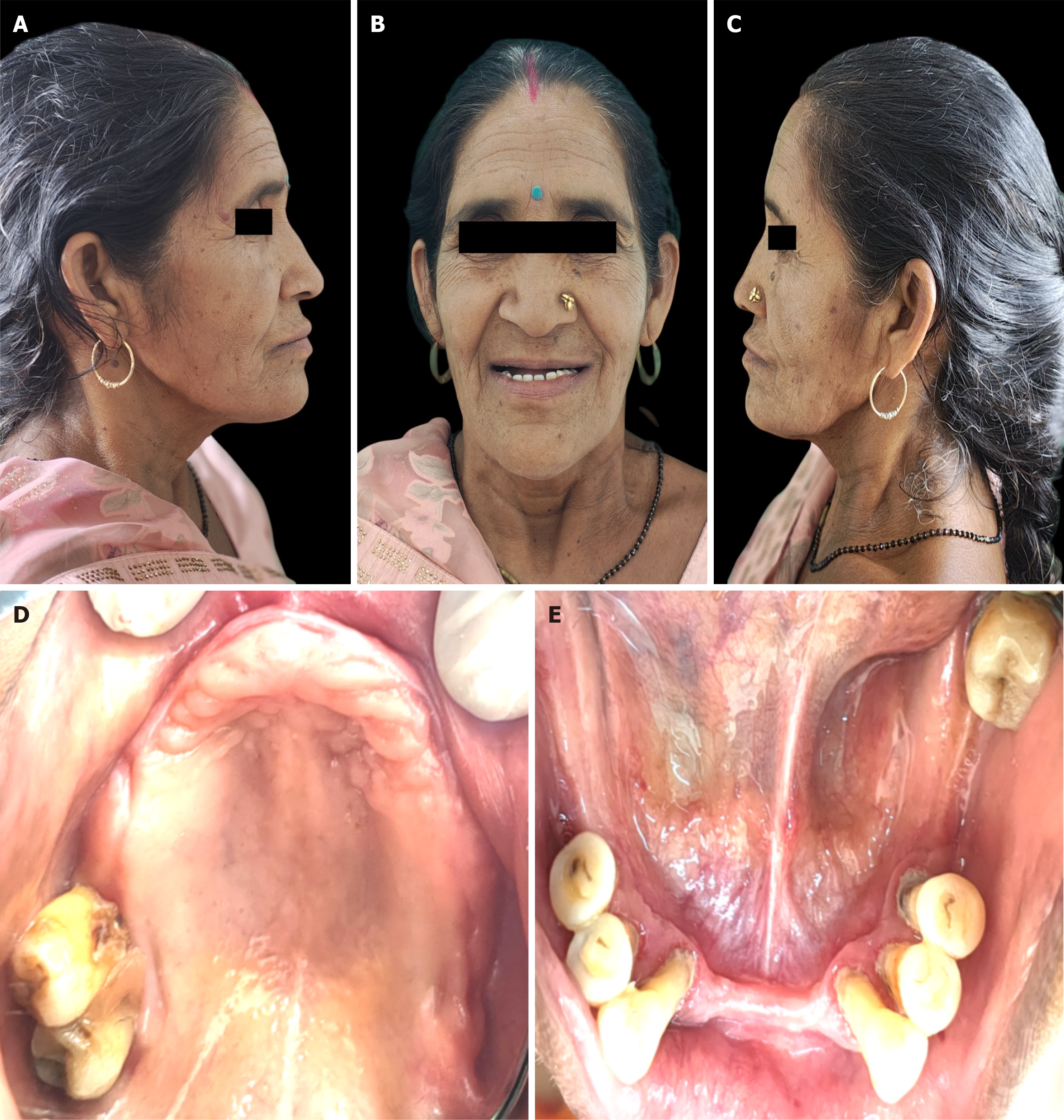
Extraoral examination revealed reduced lower facial height, mild perioral wrinkling, and diminished lip support, consistent with long-standing edentulism. Facial symmetry was preserved, and no abnormalities of the temporomandibular joints were detected (Figure 1A-C).
Intraoral examination demonstrated partial edentulism of the maxillary arch with moderate-to-severe alveolar ridge resorption, most pronounced in the posterior regions (Figure 1D). The mandibular arch exhibited multiple remaining teeth with extensive coronal destruction, increased mobility, and advanced periodontal compromise, indicating a poor long-term prognosis. An ill-fitting removable prosthesis was present in the mandibular anterior region and was planned for removal as part of the definitive treatment (Figure 1E).
Routine hematological and biochemical investigations, including complete blood count, renal and hepatic function tests, and infection markers, were within normal physiological limits. These findings confirmed the patient’s suitability for surgical intervention under local anesthesia. The patient reported no known drug allergies and demonstrated good compliance with prescribed medications.
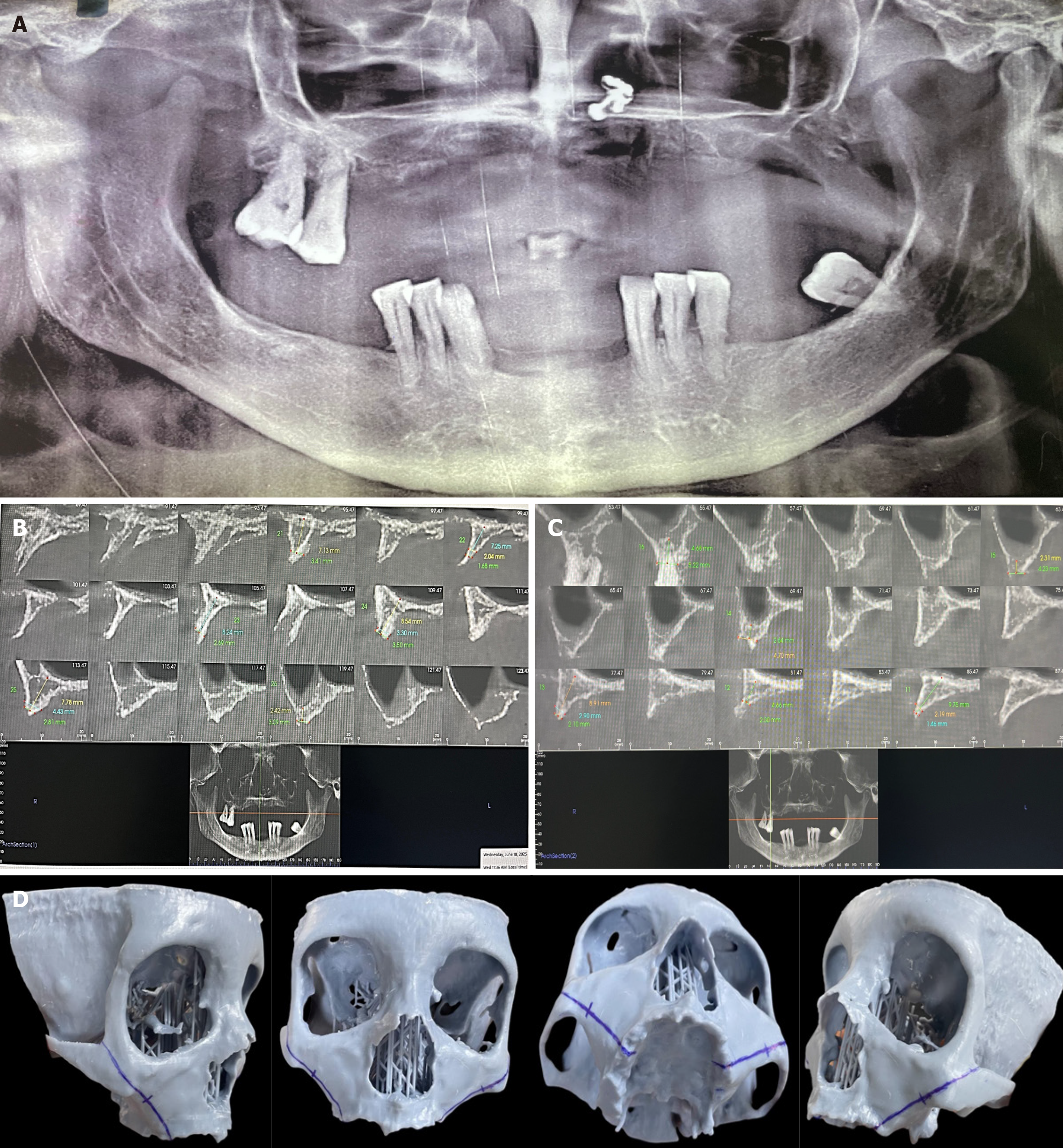
Preoperative panoramic radiography demonstrated partial edentulism with advanced alveolar ridge resorption in the posterior maxilla and marked pneumatization of the maxillary sinuses, rendering conventional implant placement unfavorable. The mandible exhibited an irregular alveolar crest morphology with reduced periodontal support around the remaining teeth (Figure 2A).
Cone-beam computed tomography (CBCT) confirmed severe maxillary atrophy, with residual vertical bone height measuring less than 4 mm in multiple posterior regions (Figure 2B and C). To facilitate precise surgical planning, a stereolithographic three-dimensional printed model was fabricated from the CBCT dataset. This model enabled detailed assessment of zygomatic bone volume, implant angulation, and proposed implant trajectories, while allowing identification of critical anatomical landmarks (Figure 2D). Based on these radiographic findings, a graftless rehabilitation strategy using posterior zygomatic implants combined with anterior nasalis implants in the maxilla, supplemented by conventional implants in the mandible, was planned.
Severe maxillary alveolar ridge atrophy with posterior maxillary sinus pneumatization, associated with partial edentulism of the maxilla and compromised mandibular dentition with a poor periodontal prognosis, requiring full-arch implant-supported prosthodontic rehabilitation.
Following standard aseptic protocols, local anesthesia was administered using 2% lignocaine with 1:80000 adrenaline (Xylocaine® with Adrenaline, AstraZeneca, Södertälje, Sweden) via bilateral posterior superior alveolar, infraorbital, and greater palatine nerve blocks, supplemented by buccal and palatal infiltrations. Adequate anesthesia and hemostasis were confirmed before flap reflection. A prophylactic single oral dose of amoxicillin (35 mg/kg) was administered one hour prior to surgery.
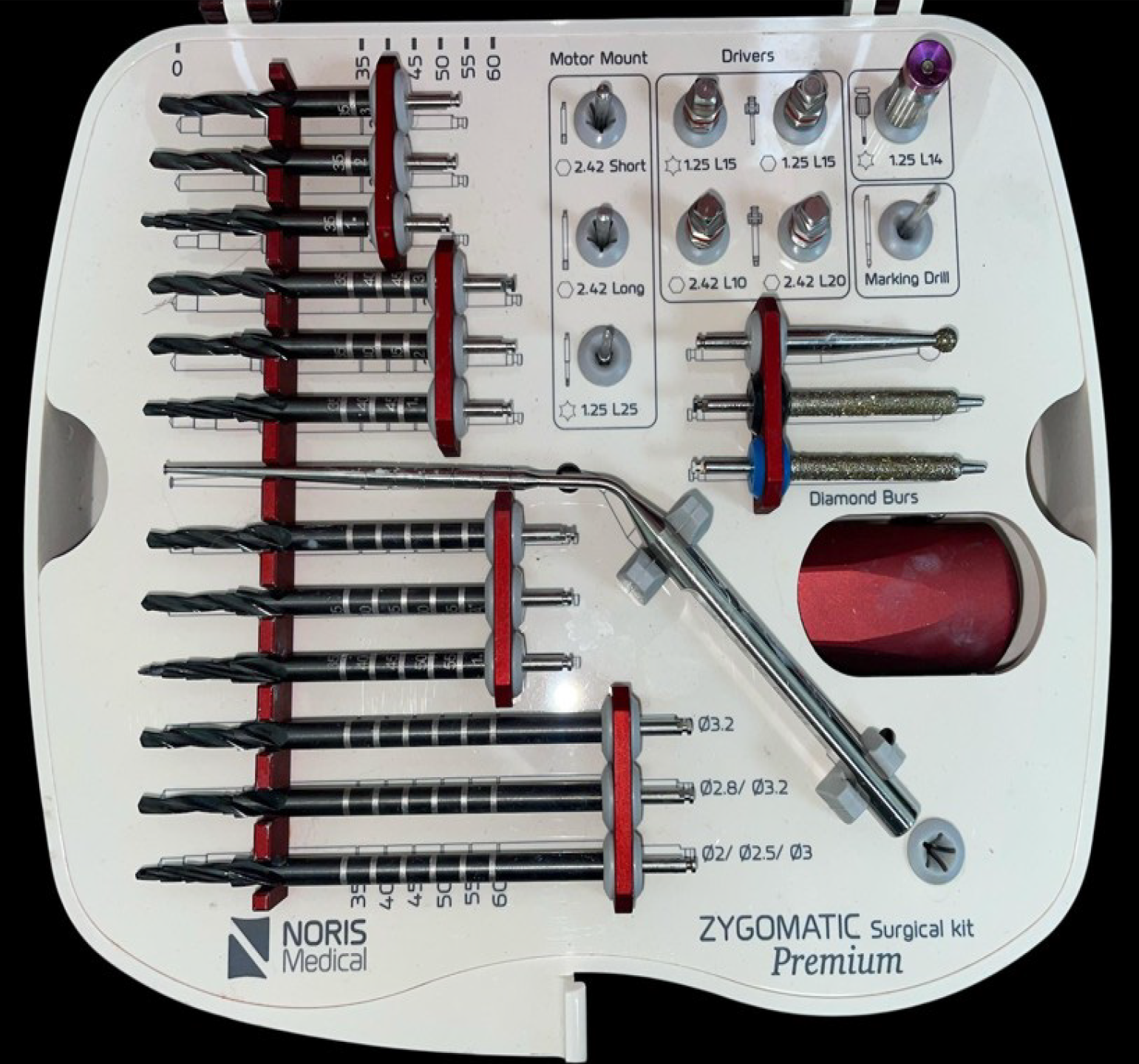
A dedicated zygomatic surgical kit (Noris Medical, Nesher, Israel) was used for implant placement. The kit includes long and short precision drills, diamond burs for controlled bone contouring, depth-calibrated drills, motor mounts, and prosthetic drivers, facilitating accurate control of angulation and depth in anatomically complex regions adjacent to the maxillary sinus and orbit (Figure 3).
A slightly palatalized crestal incision was initiated from the posterior buccal aspect of the maxillary tuberosity and extended anteriorly toward the midline. Vertical vestibular-releasing incisions were performed bilaterally up to the level of the anterior nasal spine. This incision design allowed mobilization of palatal connective tissue toward the buccal aspect, reducing the risk of soft-tissue dehiscence in the coronal implant region.
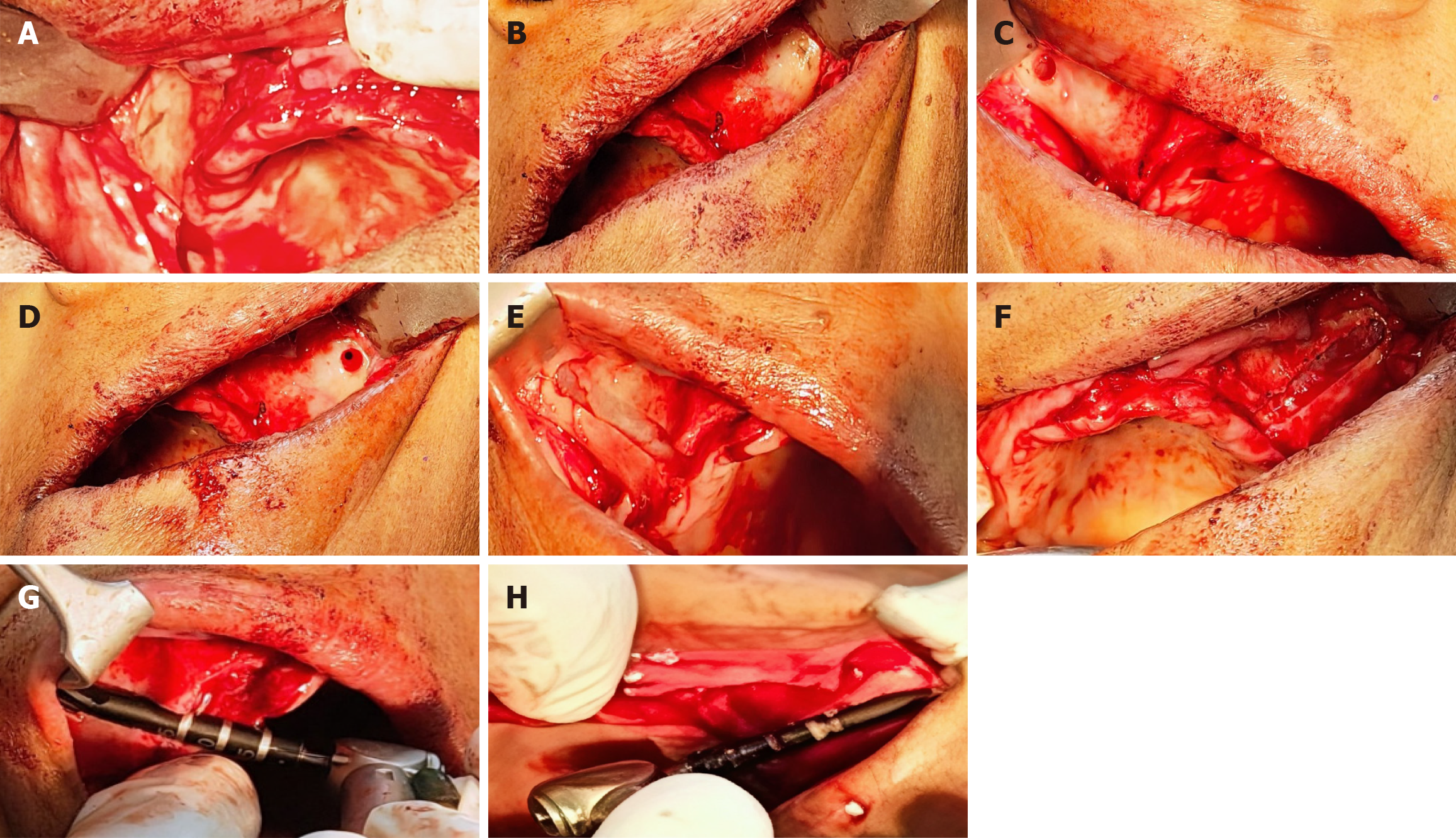
Bilateral full-thickness mucoperiosteal flaps were elevated to expose the lateral maxillary wall and zygomatic buttress regions. Adequate visualization of anatomical landmarks in both quadrants facilitated accurate determination of implant trajectories and safe osteotomy preparation (Figure 4A and B).
Within the zygoma anatomy-guided approach, three functional zones along the zygomatic implant pathway were identified[4]. The zygomatic implant critical zone represents the coronal region where the implant initially engages the maxillary bone; preservation of residual alveolar bone and peri-implant soft tissues in this region is essential to minimize long-term biological complications. The zygomatic antrostomy zone corresponds to the segment where the osteotomy traverses the maxillary sinus or lateral sinus wall, with its position determined by maxillary morphology. The zygomatic anchorage zone refers to the portion of the zygomatic bone where the implant achieves maximal primary stability through engagement of dense cortical bone.
Initial osteotomy preparation was performed using a round diamond bur to define the entry point on the lateral maxillary wall at the level of the zygomatic buttress (Figure 4C and D). This step ensured controlled positioning and prevented bur slippage in proximity to vital anatomical structures. The osteotomy was subsequently refined using a diamond bur to establish a smooth and accurately contoured implant pathway (Figure 4E and F).
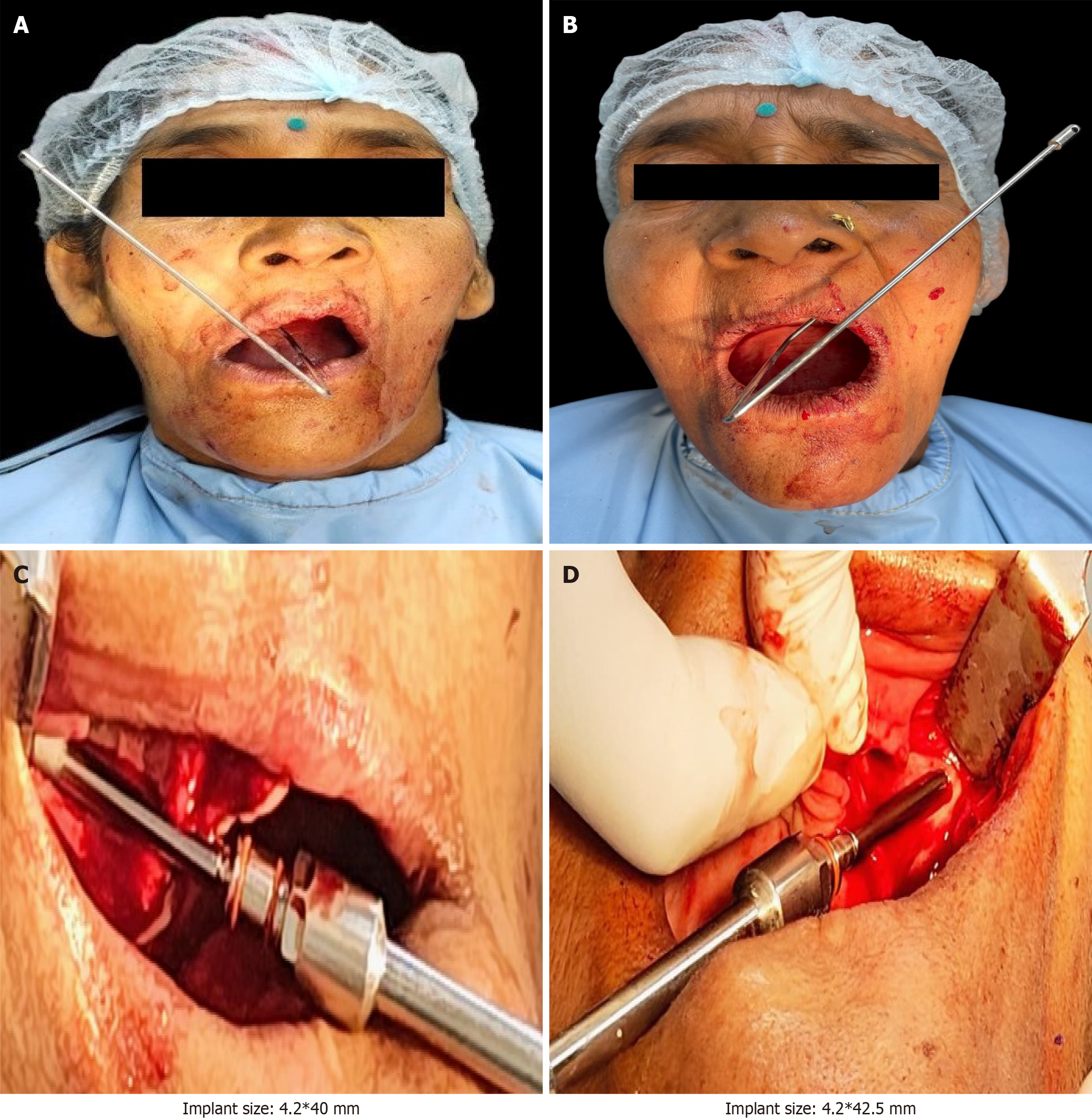
An extrasinus trajectory was adopted, directing the osteotomy along the lateral maxillary wall toward the body of the zygomatic bone while avoiding sinus penetration. Depth-calibrated drills were then used in a stepwise manner to extend the osteotomy to the planned length, with continuous copious irrigation to prevent thermal injury (Figure 4G and H).
A zygomatic pathfinder was inserted to confirm the intended implant trajectory and verify emergence at the lateral surface of the zygomatic bone. Both tactile and visual assessment of the exit point ensured correspondence with the planned extrasinus path prior to definitive implant placement (Figure 5A and B).
Following osteotomy preparation, two zygomatic implants were placed bilaterally (one per side) to achieve anchorage within the dense cortical bone of the zygomatic body (Figure 5C and D). Primary stability adequate for immediate loading was achieved for all zygomatic implants, after which 52° multiunit abutments (Noris Medical, Nesher, Israel) were connected to optimize prosthetic emergence and parallelism.
In the anterior maxilla, three nasalis implants were placed bilaterally in the canine-incisor region, anchored in the anterior nasal floor and adjacent basal bone. The implants were positioned medial to the canine eminence and lateral to the nasal septum, based on available cortical bone and prosthetically driven requirements. Primary implant stability was clinically assessed and considered adequate to permit prosthetic loading. In the mandible, conventional endosseous implants were placed in sites with adequate bone volume. All anterior maxillary and mandibular implants were restored with 0° multiunit abutments to establish a uniform restorative platform.
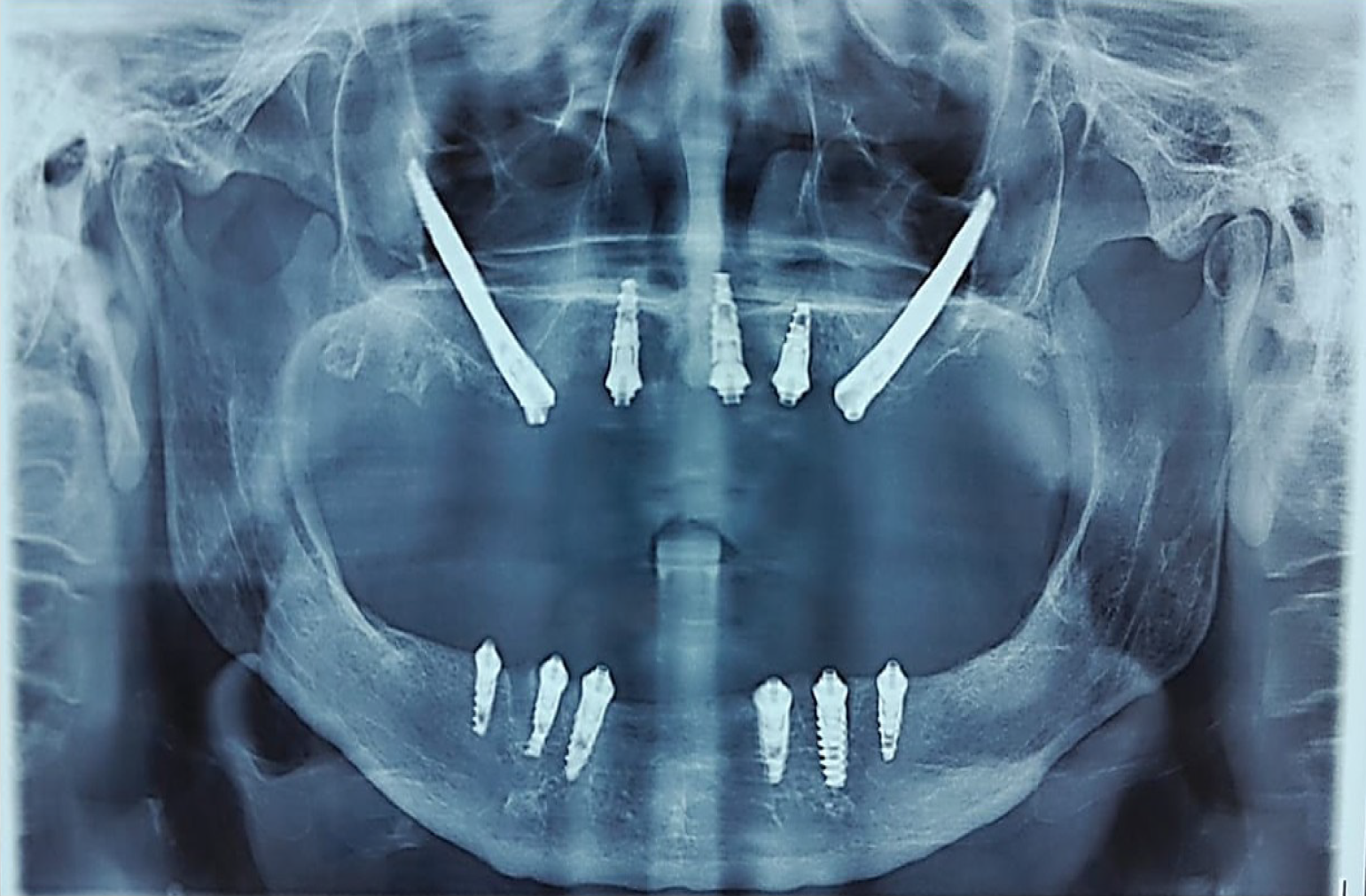
This combined implant configuration enabled immediate functional loading by improving load distribution and minimizing cantilever forces. A postoperative panoramic radiograph confirmed accurate bilateral placement of the zygomatic implants, visualization of nasalis implants in the anterior nasal floor region, and stable positioning of conventional mandibular implants (Figure 6).
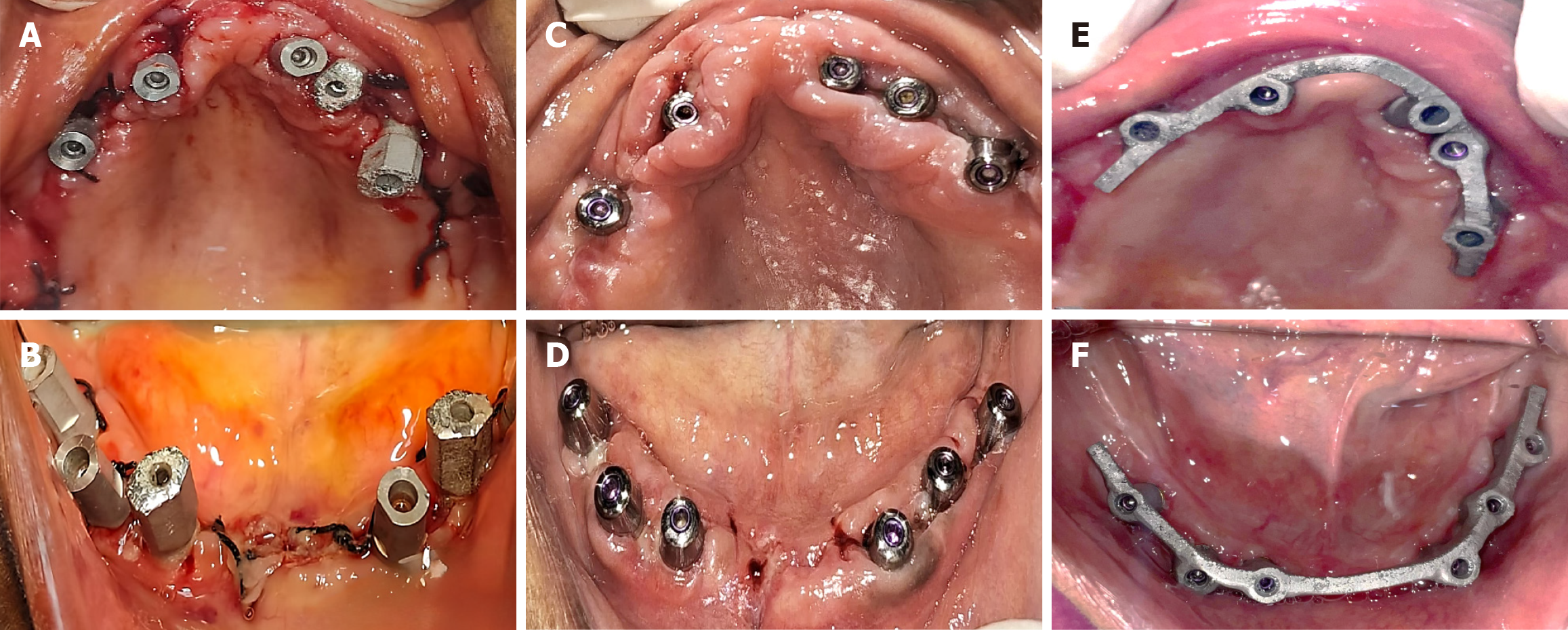
Regarding the prosthetic workflow and immediate loading timeline, no interim removable prosthesis was used. On the operative day, a digital intraoral scan was performed using scan bodies attached to the implants in both arches, enabling precise capture of three-dimensional implant positions for prosthetic fabrication (Figure 7A and B). Multiunit comfort caps were then placed to protect implant platforms, facilitate peri-implant soft-tissue contouring, and maintain the transmucosal corridor during healing (Figure 7C and D).
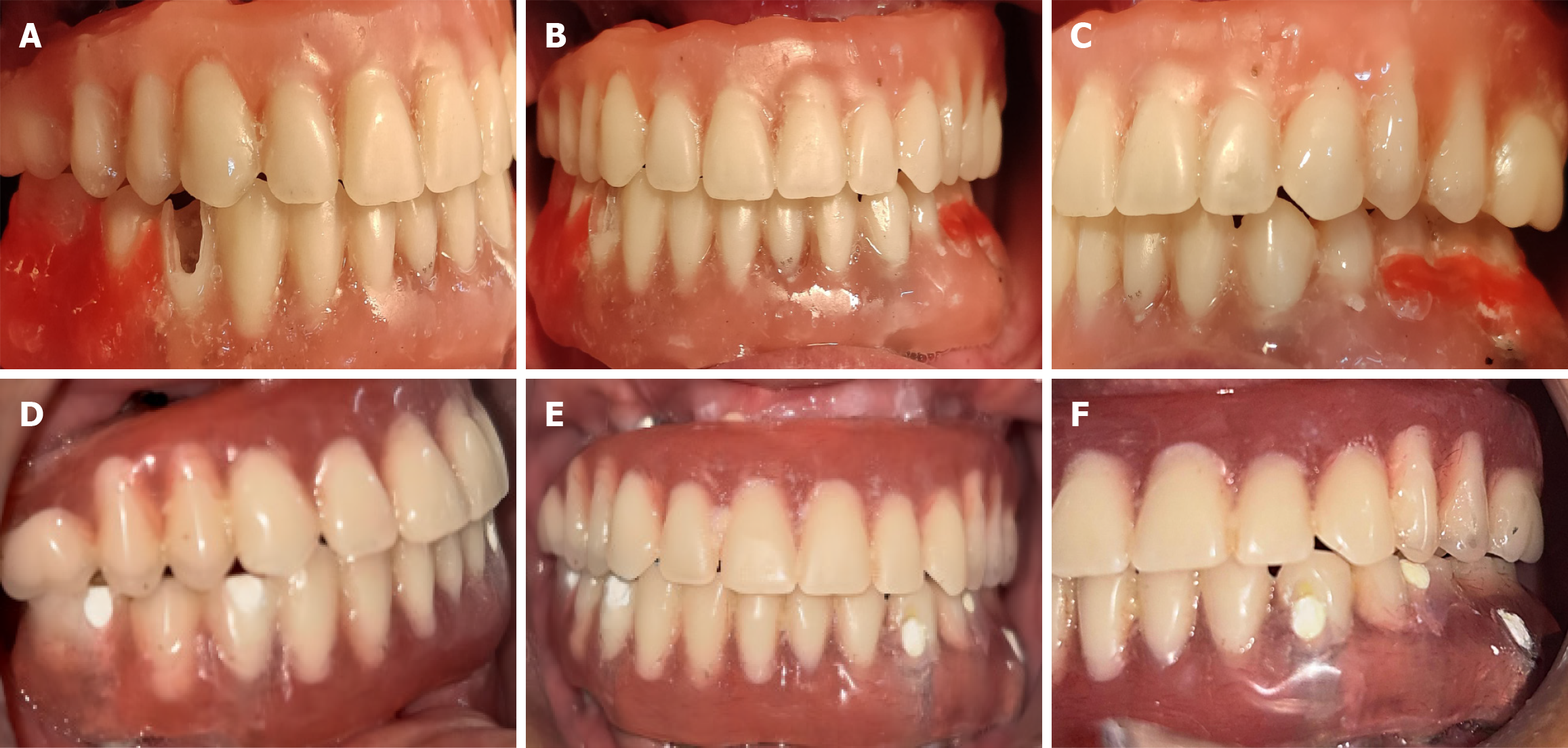
Definitive metal frameworks were fabricated using a digital workflow and evaluated intraorally to verify passive fit and accuracy on the first postoperative day (Figure 7E and F). Following successful framework verification, a hybrid prosthesis try-in was performed to assess occlusion, phonetics, esthetics, and patient comfort on the first postoperative day (Figure 8A-C). Necessary adjustments were made before final prosthesis delivery.
The definitive hybrid prosthesis was immediately loaded without the use of a provisional restoration on the second postoperative day. The prosthesis consisted of a rigid metal framework veneered with acrylic resin and denture teeth, providing a favorable balance between mechanical strength and esthetics. Immediate loading restored function and facial esthetics while allowing early patient adaptation (Figure 8D-F).
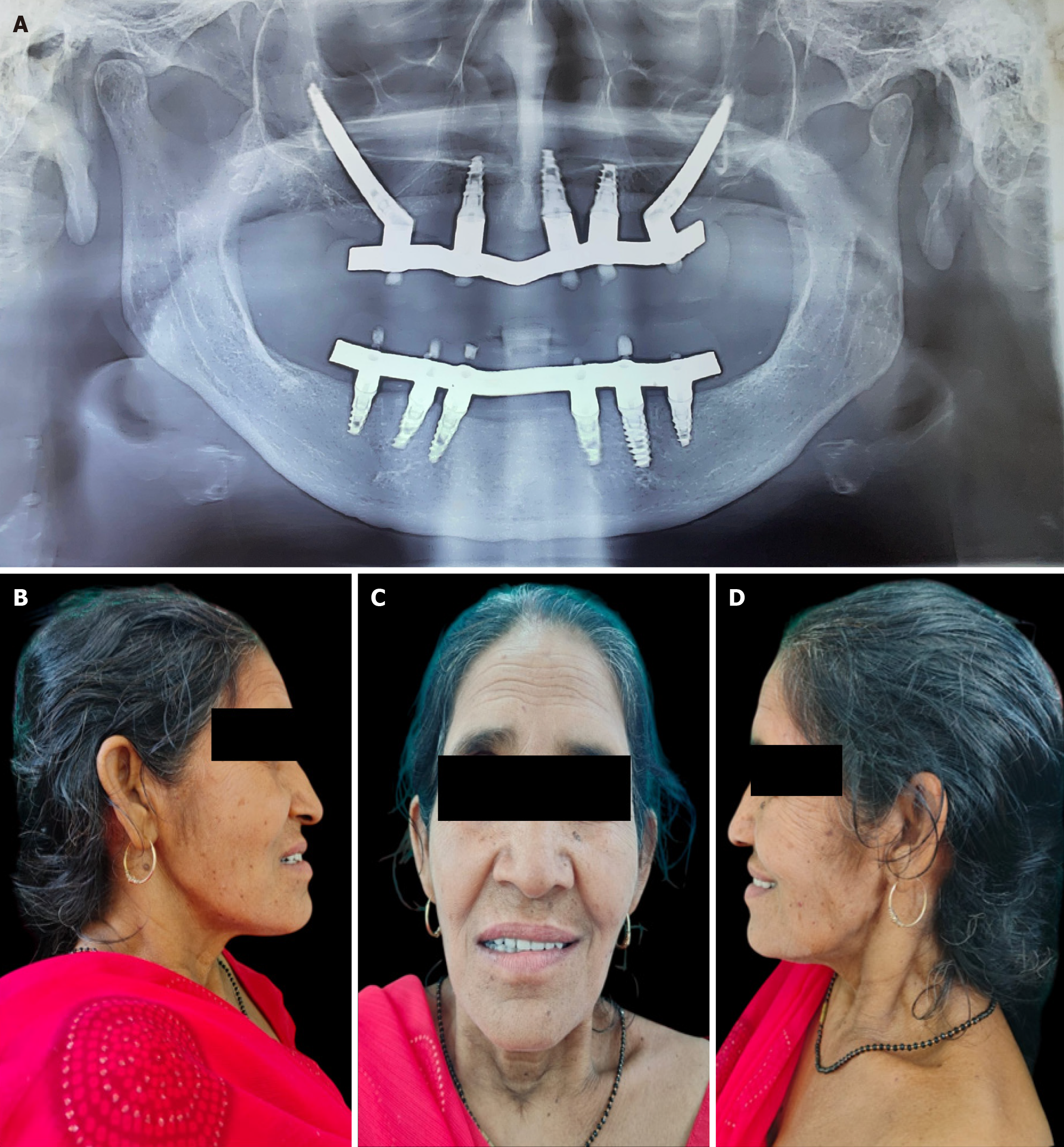
The post-prosthetic panoramic radiograph confirmed stable fixation of the hybrid prosthesis to the supporting implants, demonstrating accurate seating of the metal framework and appropriate implant-abutment connections (Figure 9A). Radiographic evaluation showed maintained peri-implant bone levels, with no evidence of early marginal bone loss, framework misfit, or mechanical complications. Comparative radiographic assessment between immediate postoperative and 6-month follow-up images revealed no clinically significant crestal bone level changes around the zygomatic or nasalis implants. Marginal bone levels were evaluated using panoramic radiographs and CBCT images by measuring the distance from the implant platform to the first bone-implant contact.
Postoperative extraoral profile photographs demonstrated a marked improvement in facial balance and soft-tissue support. Rehabilitation of the maxilla using zygomatic and nasalis implants, in conjunction with mandibular implants, restored lip support and lower facial height, resulting in improved facial harmony and profile (Figure 9B-D). These changes were consistent with the correction of maxillary deficiency and the restoration of appropriate occlusal relationships.
The timeline of care was aligned with the CARE guidelines. The patient initially presented with severe maxillary atrophy and functional impairment. Surgical placement of zygomatic and nasalis implants with immediate loading was performed following comprehensive clinical and radiographic planning. Post-prosthetic evaluations were conducted at 24 hours, 1 week, 1 month, 3 months, and 6 months following prosthesis delivery.
At each follow-up visit, all implants exhibited clinical stability, with healthy peri-implant soft tissues and no signs of inflammation, infection, or soft-tissue dehiscence. Radiographic assessments during follow-up revealed stable peri-implant bone levels without pathological changes.
At the 6-month follow-up, the hybrid prosthesis remained functionally and esthetically stable. No biological or mechanical complications were observed. Occlusion, phonetics, and masticatory function were satisfactory. Patient-reported outcome assessment indicated a high level of satisfaction with comfort, chewing efficiency, speech, and facial appearance.
The patient reported improved confidence during social interactions and expressed satisfaction with the immediate restoration of function and facial esthetics, particularly noting enhanced comfort compared with previous removable prostheses.
Cawood and Howell[9] proposed a widely accepted classification system for edentulous jaws that remains a valuable tool in treatment planning for maxillofacial rehabilitation. This classification describes six stages of residual ridge resorption, ranging from dentate conditions (class I) to advanced basal bone loss with minimal residual alveolar bone (class VI). It provides a standardized framework for assessing anatomical limitations, anticipating surgical challenges, and selecting appropriate reconstructive or implant-based treatment strategies. In advanced stages of maxillary atrophy, this classification highlights the limitations of conventional implant placement and underscores the need for alternative approaches that bypass compromised alveolar bone.
Zygomatic implants have emerged as a predictable graftless solution for rehabilitation of the severely atrophic maxilla, with reported survival rates ranging from 90% to 100%. Brånemark et al[3] reported a 94% survival rate in a long-term follow-up of 52 implants placed in 28 patients, while Kahnberg et al[10] demonstrated a 96.3% success rate in a three-year evaluation of 145 zygomatic implants. Similarly, Peñarrocha et al[11] reported a 100% survival rate for 40 zygomatic implants placed in 21 patients over a mean follow-up of 29 months. These outcomes support the clinical reliability of zygomatic implants as an alternative to extensive bone grafting procedures.
Despite their advantages, zygomatic implants are technically demanding and require advanced surgical expertise due to their proximity to critical anatomical structures. Reported complications include postoperative sinusitis, oroantral fistula formation, periorbital hematoma, epistaxis, transient sensory disturbances, and, rarely, orbital injury[3,12]. The incidence of sinusitis has been reported to range from 2.3% to 13.6%[13]. However, endoscopic evaluation by Petruson[14] demonstrated a normal sinus mucosa without evidence of inflammation or increased secretion surrounding zygomatic implants, suggesting that sinus-related complications may not be inevitable when appropriate surgical protocols are followed.
From a prosthodontic perspective, the long-term success of full-arch rehabilitation is strongly influenced by the volume, quality, and distribution of supporting tissues[15]. In cases of severe maxillary atrophy, posterior anchorage provided solely by zygomatic implants may be insufficient to achieve an optimal anteroposterior spread, potentially increasing cantilever length and biomechanical loading on the prosthesis. To overcome this limitation, several hybrid anchorage strategies have been described in the literature, including quad-zygoma configurations, pterygoid implants, and trans-nasal or anterior anchorage techniques[16].
Trans-nasal and anterior anchorage concepts have been reported primarily as adjuncts to improve anterior support in cases where the premaxilla is severely resorbed; however, standardized descriptions and long-term outcome data for these approaches remain limited. Accordingly, the present report does not claim the invention of anterior nasal anchorage but rather illustrates a reproducible integration of anterior nasalis implants with posterior zygomatic implants within a prosthodontically driven treatment framework.
Quad-zygoma concepts provide enhanced posterior support but may increase surgical complexity, operative time, and anatomical risk, particularly in patients with limited zygomatic bone volume or unfavorable orbital anatomy. Pterygoid implants offer posterior anchorage but require precise angulation and present prosthetic access challenges, especially during immediate loading protocols. In contrast, the incorporation of anterior nasalis implants—anchored in the dense cortical bone of the anterior nasal floor—provides an additional anterior support point, improving anteroposterior distribution without extending posterior cantilevers or increasing surgical morbidity. This approach may be particularly advantageous when posterior-only solutions are biomechanically unfavorable or when grafting and quad-zygoma strategies are contraindicated or declined by the patient.
In the present case, the combination of posterior zygomatic implants with anterior nasalis implants improved load distribution and prosthetic stability, facilitating immediate loading with a fixed hybrid prosthesis. This implant configuration was selected based on individual anatomical constraints and prosthetic requirements rather than as a universal solution, underscoring the importance of case-specific planning. Strategic implant placement was guided by the planned prosthetic design and available bone morphology, consistent with established prosthodontic principles[17-20]. The use of multiunit abutments and a digital workflow further contributed to accurate prosthesis fabrication and passive fit.
Prosthetic rehabilitation supported by zygomatic implants also presents unique restorative considerations. The inclined neck geometry of zygomatic implants necessitates the use of dedicated prosthetic components, including reduced-length abutment screws, to ensure accurate seating and secure engagement. The distopalatal emergence of these implants may complicate prosthetic access and hygiene maintenance, emphasizing the importance of meticulous restorative planning and patient education.
Overall, this case demonstrates that a combined zygomatic-anterior nasalis implant strategy can serve as a viable graftless alternative to posterior-only anchorage, quad-zygoma configurations, or extensive augmentation procedures in selected patients with severe maxillary atrophy. While long-term comparative studies are required, this report contributes clinical insight into the biomechanical and prosthetic rationale of a hybrid anchorage approach, highlighting the importance of individualized treatment planning, precise surgical execution, and prosthodontically driven rehabilitation to achieve predictable functional and esthetic outcomes.
Rehabilitation of the severely atrophic maxilla remains one of the most complex challenges in implant-supported prosthodontics, particularly when conventional implant placement is precluded by limited bone volume and unfavorable anatomical conditions. This case report demonstrates that a combined approach using zygomatic implants with anterior nasalis and conventional implants can provide a predictable, graftless solution for comprehensive maxillary rehabilitation.
Integration of the zygoma anatomy-guided approach with a prosthetically driven digital workflow allowed optimized implant positioning, improved biomechanical load distribution, and immediate functional loading, resulting in favorable functional and esthetic outcomes.
Within the limitations of a single case report, these findings suggest that hybrid zygomatic-anterior implant strategies may represent a viable alternative to extensive bone grafting procedures in selected patients with severe maxillary atrophy. This approach has the potential to reduce surgical morbidity and overall treatment duration while maintaining prosthetic stability and patient satisfaction. Nevertheless, successful application requires advanced surgical expertise and meticulous prosthetic planning. Further long-term, prospective clinical studies are needed to establish standardized protocols and to evaluate the broader applicability of this treatment concept.
| 1. | Bedrossian E, Stumpel L 3rd, Beckely ML, Indresano T. The zygomatic implant: preliminary data on treatment of severely resorbed maxillae. A clinical report. Int J Oral Maxillofac Implants. 2002;17:861-865. [PubMed] |
| 2. | Esposito M, Grusovin MG, Felice P, Karatzopoulos G, Worthington HV, Coulthard P. The efficacy of horizontal and vertical bone augmentation procedures for dental implants - a Cochrane systematic review. Eur J Oral Implantol. 2009;2:167-184. [PubMed] |
| 3. | Brånemark PI, Gröndahl K, Ohrnell LO, Nilsson P, Petruson B, Svensson B, Engstrand P, Nannmark U. Zygoma fixture in the management of advanced atrophy of the maxilla: technique and long-term results. Scand J Plast Reconstr Surg Hand Surg. 2004;38:70-85. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 166] [Cited by in RCA: 190] [Article Influence: 8.6] [Reference Citation Analysis (0)] |
| 4. | Aparicio C, Olivo A, de Paz V, Kraus D, Luque MM, Crooke E, Simon P, Simon M, Ferreira J, Serrano AS, Ilg JP, Bilbao A, Fernandez A, Guitián P, Neugarten J. The zygoma anatomy-guided approach (ZAGA) for rehabilitation of the atrophic maxilla. Clin Dent Rev. 2022;6:2. [DOI] [Full Text] |
| 5. | Vrielinck L, Blok J, Politis C. Survival of conventional dental implants in the edentulous atrophic maxilla in combination with zygomatic implants: a 20-year retrospective study. Int J Implant Dent. 2022;8:27. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 14] [Reference Citation Analysis (0)] |
| 6. | Chrcanovic BR, Albrektsson T, Wennerberg A. Survival and Complications of Zygomatic Implants: An Updated Systematic Review. J Oral Maxillofac Surg. 2016;74:1949-1964. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 162] [Cited by in RCA: 154] [Article Influence: 15.4] [Reference Citation Analysis (0)] |
| 7. | Davó R, Felice P, Pistilli R, Barausse C, Marti-Pages C, Ferrer-Fuertes A, Ippolito DR, Esposito M. Immediately loaded zygomatic implants vs conventional dental implants in augmented atrophic maxillae: 1-year post-loading results from a multicentre randomised controlled trial. Eur J Oral Implantol. 2018;11:145-161. [PubMed] |
| 8. | Aparicio C, Ouazzani W, Aparicio A, Fortes V, Muela R, Pascual A, Codesal M, Barluenga N, Franch M. Immediate/Early loading of zygomatic implants: clinical experiences after 2 to 5 years of follow-up. Clin Implant Dent Relat Res. 2010;12 Suppl 1:e77-e82. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 32] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 9. | Cawood JI, Howell RA. A classification of the edentulous jaws. Int J Oral Maxillofac Surg. 1988;17:232-236. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 850] [Cited by in RCA: 844] [Article Influence: 22.2] [Reference Citation Analysis (0)] |
| 10. | Kahnberg KE, Henry PJ, Hirsch JM, Ohrnell LO, Andreasson L, Brånemark PI, Chiapasco M, Gynther G, Finne K, Higuchi KW, Isaksson S, Malevez C, Neukam FW, Sevetz E Jr, Urgell JP, Widmark G, Bolind P. Clinical evaluation of the zygoma implant: 3-year follow-up at 16 clinics. J Oral Maxillofac Surg. 2007;65:2033-2038. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 52] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 11. | Peñarrocha M, García B, Martí E, Boronat A. Rehabilitation of severely atrophic maxillae with fixed implant-supported prostheses using zygomatic implants placed using the sinus slot technique: clinical report on a series of 21 patients. Int J Oral Maxillofac Implants. 2007;22:645-650. [PubMed] |
| 12. | Ferrara ED, Stella JP. Restoration of the edentulous maxilla: the case for the zygomatic implants. J Oral Maxillofac Surg. 2004;62:1418-1422. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 27] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 13. | Block MS, Haggerty CJ, Fisher GR. Nongrafting implant options for restoration of the edentulous maxilla. J Oral Maxillofac Surg. 2009;67:872-881. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 28] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 14. | Petruson B. Sinuscopy in patients with titanium implants in the nose and sinuses. Scand J Plast Reconstr Surg Hand Surg. 2004;38:86-93. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 38] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 15. | Tallgren A. The continuing reduction of the residual alveolar ridges in complete denture wearers: a mixed-longitudinal study covering 25 years. J Prosthet Dent. 1972;27:120-132. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 626] [Cited by in RCA: 548] [Article Influence: 10.1] [Reference Citation Analysis (0)] |
| 16. | Haraldson T, Carlsson GE. Chewing efficiency in patients with osseointegrated oral implant bridges. Swed Dent J. 1979;3:183-191. [PubMed] |
| 17. | Leblebicioglu B, Rawal S, Mariotti A. A review of the functional and esthetic requirements for dental implants. J Am Dent Assoc. 2007;138:321-329. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 26] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 18. | Rosén A, Gynther G. Implant treatment without bone grafting in edentulous severely resorbed maxillas: a long-term follow-up study. J Oral Maxillofac Surg. 2007;65:1010-1016. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 44] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 19. | Weinberg LA. The biomechanics of force distribution in implant-supported prostheses. Int J Oral Maxillofac Implants. 1993;8:19-31. [PubMed] |
| 20. | Lin CL, Wang JC, Ramp LC, Liu PR. Biomechanical response of implant systems placed in the maxillary posterior region under various conditions of angulation, bone density, and loading. Int J Oral Maxillofac Implants. 2008;23:57-64. [PubMed] |