©Author(s) (or their employer(s)) 2026.
World J Clin Cases. Mar 6, 2026; 14(7): 116694
Published online Mar 6, 2026. doi: 10.12998/wjcc.v14.i7.116694
Published online Mar 6, 2026. doi: 10.12998/wjcc.v14.i7.116694
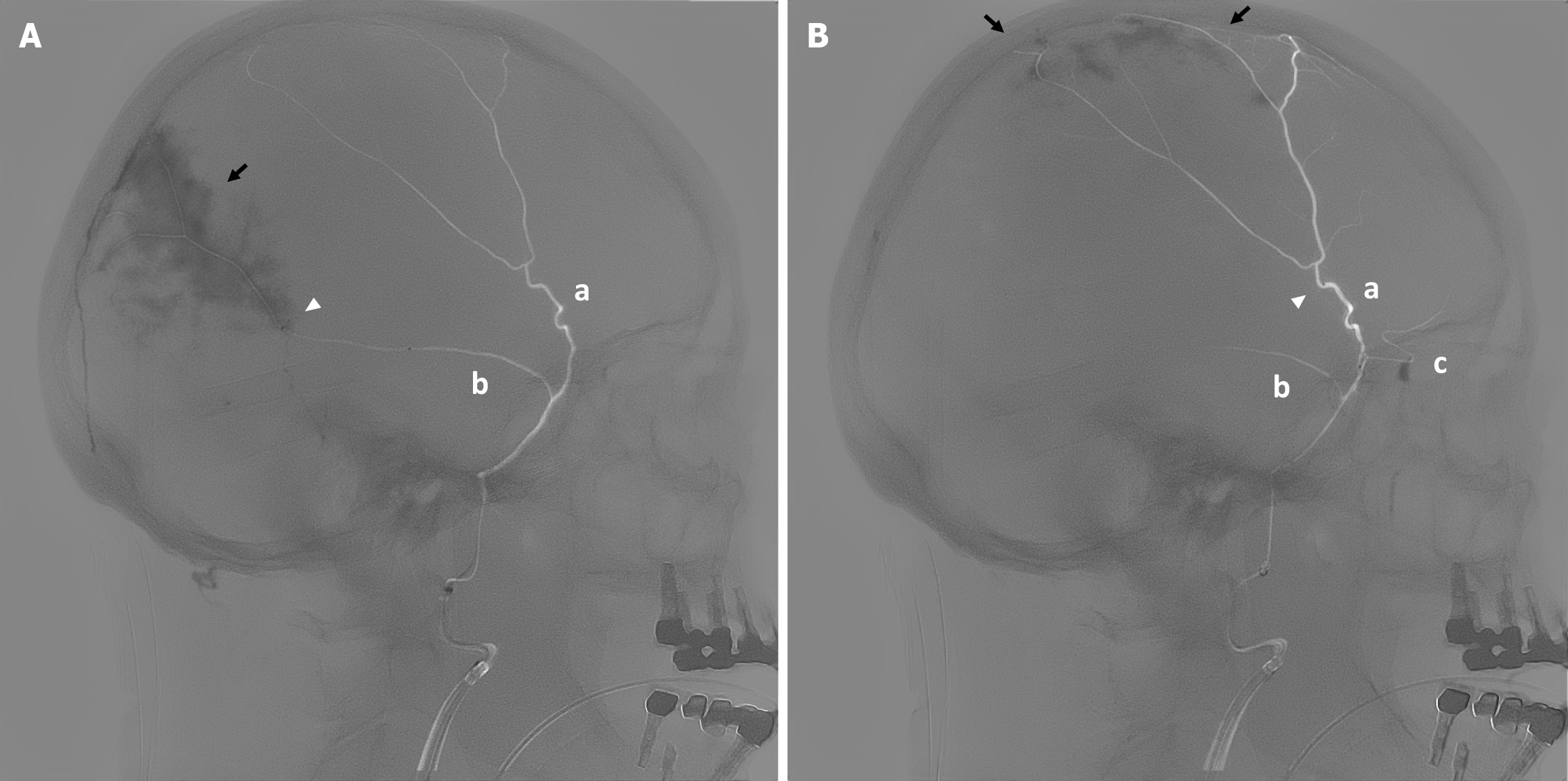
Figure 1 Selective middle meningeal artery angiograms during embolization.
A: Posterior branch angiogram demonstrating the anterior (a) and posterior (b) middle meningeal artery branches. Contrast blush (black arrow) denotes pathological neovascularization of the dural membranes, with the microcatheter tip positioned distally within the posterior branch (white arrowhead); B: Anterior branch angiogram demonstrating the anterior (a) and posterior (b) middle meningeal artery branches and the meningo-ophthalmic artery anastomosis (c), with contrast blush indicating pathological neovascularization (black arrows) and the microcatheter tip advanced beyond the meningo-ophthalmic origin to prevent reflux (white arrowhead).
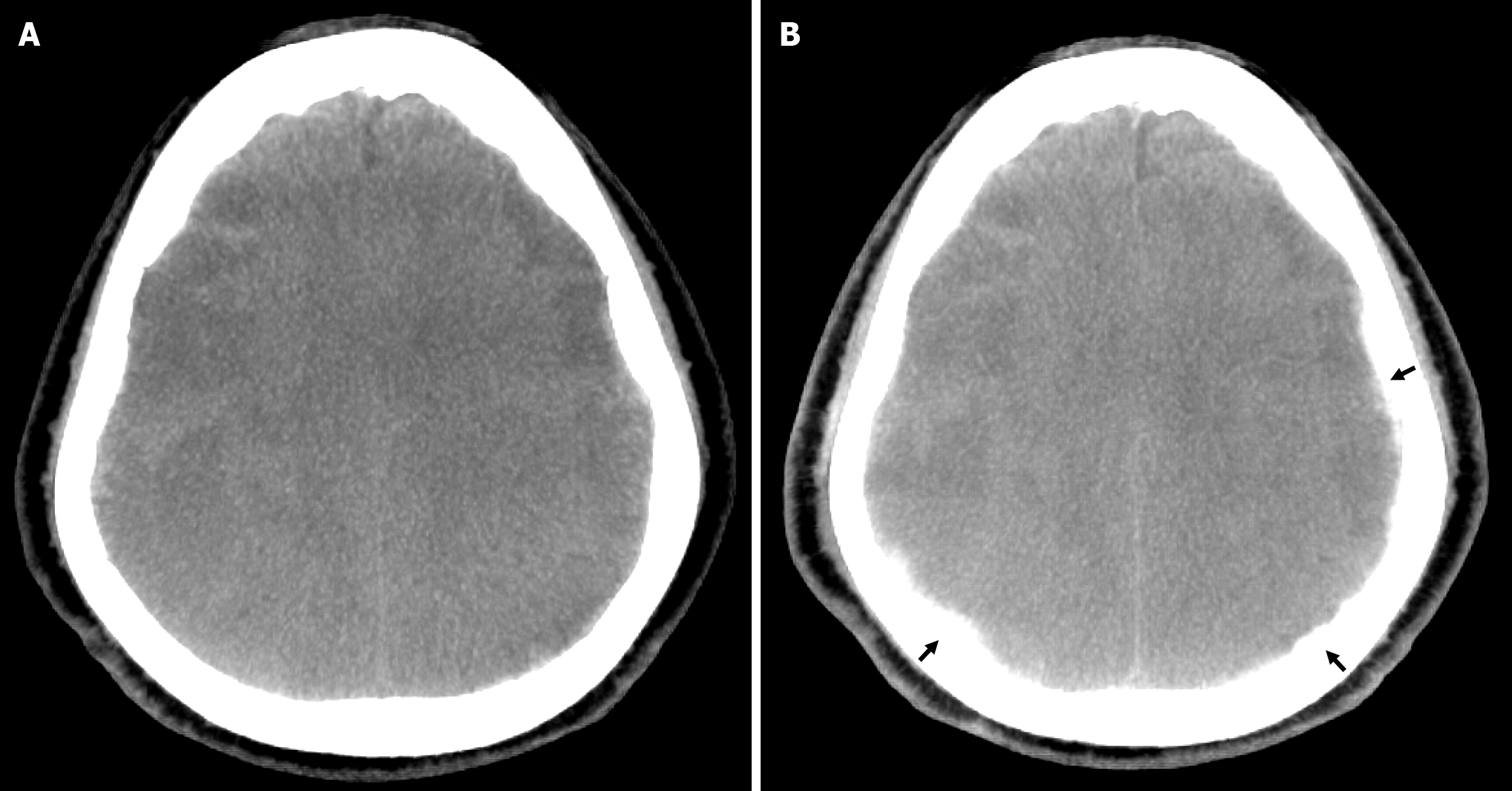
Figure 2 Axial intraprocedural cone-beam computed tomography before and after middle meningeal artery embolization.
A: Pre-embolization computed tomography; B: Post-embolization computed tomography demonstrating contrast penetration into the subdural space (black arrows), indicative of spherical polyvinyl alcohol particle deposition.
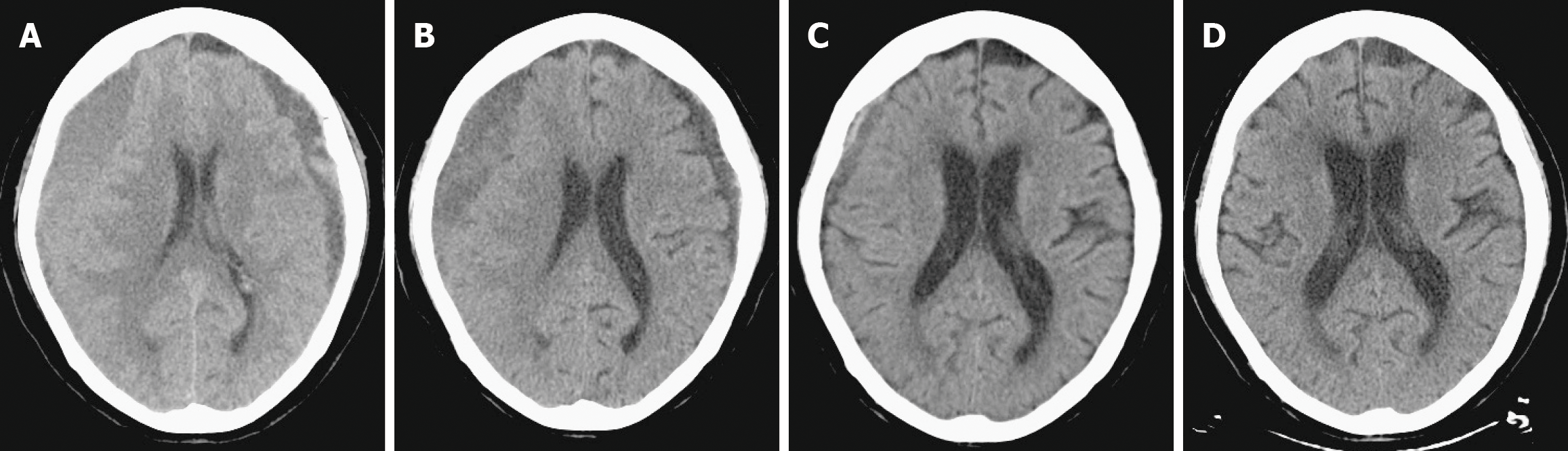
Figure 3 Axial brain computed tomography showing progressive resolution of chronic subdural hematoma following middle meningeal artery embolization.
A: Pre-embolization image illustrating extensive bilateral chronic subdural hematoma; B: One-month post-embolization image showing substantial hematoma reduction; C: Two-month post-embolization image demonstrating continued hematoma clearance; D: Three-month post-embolization image showing complete hematoma resolution and excellent brain re-expansion.
- Citation: Chen CY, Hsu YH. Complete resolution of massive chronic subdural hematoma with refined layered middle meningeal artery embolization: A case report. World J Clin Cases 2026; 14(7): 116694
- URL: https://www.wjgnet.com/2307-8960/full/v14/i7/116694.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v14.i7.116694