Published online May 19, 2026. doi: 10.5498/wjp.v16.i5.116997
Revised: December 29, 2025
Accepted: February 10, 2026
Published online: May 19, 2026
Processing time: 155 Days and 0.2 Hours
Chronic kidney disease (CKD) and the maintenance hemodialysis (MHD) it necessitates impose significant physical and psychological burdens on patients, including high rates of anxiety, depression, and various physiological complications, which severely impair their quality of life.
To investigate the effects of a collaborative care model combined with mental health education on the psychological status and complications in patients with CKD undergoing MHD.
A total of 128 patients who underwent hemodialysis at the Hemodialysis Center of the Second Affiliated Hospital of Chongqing Medical University between April 2023 and March 2025 were enrolled and randomly assigned to a control group (n = 64) or study group (n = 64). The control group received routine hemodialysis management plus mental health education, whereas the study group also rec
The SAS and SDS scores in the intervention group were significantly lower than those in the control group (both P < 0.05). Post-intervention WHOQOL-BREF scores in the physical health, psychological health, social relationships, and environmental domains increased in both groups, with significantly higher scores in the intervention group (P < 0.05). Similarly, both the general health status and kidney disease-specific domain scores of the KDQOL improved in both groups, with greater imp
The collaborative care model combined with mental health education had significant positive effects on the psychological well-being and complication control in patients with CKD undergoing MHD. This approach may be widely used in clinical practice to improve nursing care for patients undergoing MHD.
Core Tip: This study demonstrates that a collaborative care model combined with structured mental health education significantly improves psychological well-being, quality of life, and complication management in patients with chronic kidney disease undergoing maintenance hemodialysis. The findings highlight the importance of integrating family invo
- Citation: Li YJ, Zhang Y, Peng XL, Mei YJ, Yang XJ, Luo YJ. Collaborative mental health care improves well-being and reduces complications in hemodialysis patients. World J Psychiatry 2026; 16(5): 116997
- URL: https://www.wjgnet.com/2220-3206/full/v16/i5/116997.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i5.116997
Chronic kidney disease (CKD) is a long-term progressive illness that has a profound impact on patients’ quality of life. As the disease progresses, a considerable proportion of patients eventually develop end-stage renal disease (ESRD), for which maintenance hemodialysis (MHD) is the primary renal replacement therapies[1]. However, patients undergoing long-term hemodialysis face multiple complications and physical and psychological burdens that markedly reduce their quality of life and impose a heavy medical load. MHD patients frequently report significant psychological distress such as anxiety and depression[2]. Studies have shown that the prevalence of anxiety and depression is high in this population and is closely linked to poor sleep quality[3]. A survey of Chinese patients undergoing MHD found an association between CKD duration and suicide risk[4]. In addition, symptoms such as fatigue and pain further decrease the quality of life[3]. Owing to the chronic nature of the disease, dietary restrictions, functional limitations, accompanying complications, and fear of death, patients with CKD are especially prone to emotional disorders.
In addition to psychological problems, MHD patients often develop numerous physiological complications, including hypertension, hypotension, anemia, infection, protein-energy wasting, and fluid-related problems such as heart failure and pulmonary edema, resulting from poor adherence to fluid restriction[5,6]. These complications not only increase suffering but also lead to high rehospitalization rates and substantial economic costs. Given the serious physical and mental challenges confronting patients undergoing MHD, it is essential to improve nursing quality and life satisfaction. Health education, as a key intervention, helps patients acquire disease-related knowledge and improve their self-management skills, thereby enhancing their psychological well-being and treatment outcomes[7]. However, the current health education is mostly hospital-based and lacks family involvement and support. The family is the primary setting in which patients live, and family members play a vital role in patient recovery. As an interdisciplinary approach, the collaborative care model emphasizes cooperation and communication between healthcare providers, patients, and family members to deliver comprehensive and continuous care[8]. Therefore, this study aimed to explore the effects of a collaborative care model combined with mental health education on the psychological well-being and complication mana
From April 2023 to March 2025, 128 patients undergoing hemodialysis at the Blood Purification Center of the Second Affiliated Hospital of Chongqing Medical University were enrolled and randomly divided into two groups. The control group included 64 patients (38 males and 26 females), aged 52-65 years, with a mean age of 53.4 ± 4.5 years. The study group consisted of 64 patients (36 males and 28 females) aged 50-67 years, with a mean age of 53.8 ± 5.2 years. No statistically significant differences were observed in baseline demographic and clinical characteristics between the two groups (Table 1).
| Item | Control (n = 64) | Study (n = 64) | Statistic | P value |
| Sex (male/female) | 38/26 | 36/28 | χ2 = 0.127 | 0.722 |
| Age (years) | 53.4 ± 4.5 | 53.8 ± 5.2 | t = -0.478 | 0.633 |
| Dry weight (kg) | 58.3 ± 6.9 | 57.8 ± 7.2 | t = 0.408 | 0.684 |
| Dialysis vintage (months) | 38.2 ± 12.6 | 36.9 ± 11.8 | t = 0.598 | 0.551 |
| Residual urine volume (mL/24 hours) | 245.6 ± 85.3 | 238.4 ± 79.7 | t = 0.502 | 0.616 |
Inclusion criteria: (1) All patients met the diagnostic criteria for CKD as outlined in the Chinese Expert Consensus on the Diagnosis and Treatment of Chronic Kidney Disease in the Elderly[9] and were undergoing hemodialysis; and (2) Family members were informed of the study and voluntarily agreed to participate; written informed consent was obtained.
Exclusion criteria: (1) Severe dysfunction of other vital organs; (2) Patients with abnormal mental status who were unable to communicate effectively; or (3) Residing outside local areas.
The control group received routine hemodialysis management combined with mental health education, which included instructing patients to follow medical advice, addressing patient inquiries, providing health education, and regularly assisting with relevant examinations.
Based on routine hemodialysis management, the study group received a collaborative care model combined with mental health education. The intervention process was as follows.
Establishment of a multidisciplinary team: A professional team was formed comprising nephrologists, nurses, psychological counselors, and dietitians. Physicians were responsible for the diagnosis, treatment planning, and condition assessment. Nurses with extensive hemodialysis experience guided family caregivers in home-based care. Psychological counselors assessed and intervened in patients’ psychological issues, whereas dietitians developed individualized dietary plans according to patients’ nutritional status. Team members worked in close cooperation to provide comprehensive care services.
Needs assessment: Before initiating the collaborative care and mental health education program, patients underwent comprehensive evaluations through questionnaires, face-to-face interviews, and psychological assessments, which informed the development of targeted intervention measures.
Individualized care planning: Based on the assessment results, personalized intervention plans were developed for each patient. These plans included disease education, psychological intervention, family caregiving skills training, and dietary guidance. For patients with high psychological stress, the frequency and intensity of psychological counseling were increased, whereas for those with weaker family caregiving capacity, focused training in caregiving skills was provided.
Family caregiving guidance: Nurses conducted regular home visits to train family members on appropriate caregiving practices.
Dietary management: Family members should be instructed to master the patient’s dietary principles and adjust their meal plans according to renal function, urine output, and blood pressure. Emphasize high-quality protein (lean meat, fish, eggs, etc.) while restricting salt and phosphate and discourage pickled products and high-phosphorus foods.
Fluid control: Families were educated on the importance of fluid in preventing sodium and water retention. They were trained to record daily fluid intake and urine output, adjust intake according to dialysis schedules, encourage small and frequent water consumption, and monitor for edema, with instructions to seek medical help if symptoms worsened.
Vascular access care: Instruct caregivers to monitor the arteriovenous fistula or central venous catheter for redness, swelling, oozing, pain, or other adverse signs, and keep the access site clean and dry. Do not measure blood pressure, draw blood, or infuse fluids into the fistula arm, and avoid any pressure or trauma to the fistula. The patients were ins
Symptom monitoring: Train family members to monitor common complications such as hypertension, hypotension, disequilibrium syndrome, and infection and record vital signs such as blood pressure and temperature.
Mental health education - relieving anxiety and stress: Educational lectures, pamphlets, and counseling were provided to patients and families to explain the etiology, pathogenesis, treatment methods, and prognosis of CKD. Knowledge of MHD principles and precautions improved understanding of the disease and self-management. Emotional support and cognitive restructuring techniques were emphasized to alleviate negative emotions and foster a positive treatment outlook.
Enhancing treatment information and self-management: Psychological counseling and support groups were organized to reduce anxiety and depression. Transparent treatment information helped patients understand the therapeutic processes and expected outcomes, thereby improving confidence, adherence, and active participation in decision-making. Family members were encouraged to provide care and emotional support to foster a positive home environment.
Exercise guidance: Develop an individualized exercise plan based on the patient’s physical condition and interests. Encourage moderate activities, such as walking or tai chi, to improve fitness and immunity.
Medication guidance: Instruct patients to take medicines on time and at the correct dose to avoid missed or incorrect doses. Tell patients and caregivers to seek medical help promptly if any adverse symptoms occur during treatment.
Follow-up, evaluation, and adjustment: During the intervention, regular assessments of the patients’ psychological status and health behaviors were performed. Intervention plans were adjusted based on the assessment outcomes to ensure effectiveness and relevance. Patient and family feedback were encouraged to continuously improve service quality. Both groups received their respective interventions for eight weeks.
Assessment of depressive status: Patients’ depressive status was assessed before and after the 8-week intervention using the Self-Rating Depression Scale (SDS)[10]. A standardized score of 53 was considered the cut-off value for depression: 53-62 indicated mild depression, 63-72 indicated moderate depression, and > 72 indicated severe depression. Higher scores indicated more severe depressive symptoms.
Assessment of anxiety status: Patients’ anxiety status was assessed before and after the 8-week intervention using the Self-Rating Anxiety Scale (SAS)[10]. The normal cut-off value was 40, with a standardized score of 50 set as the threshold for anxiety. Scores of 50-59 indicated mild anxiety, 60-69 indicated moderate anxiety, and ≥ 70 indicated severe anxiety. Higher scores indicated more severe anxiety symptoms.
Assessment of 1uality of life: Patients’ quality of life was evaluated before and after the 8-week intervention using the World Health Organization Quality of Life-BREF (WHOQOL-BREF) questionnaire[11]. The scale consists of 26 items scored on a 5-point Likert scale covering four domains: Physical health, psychological health, social relationships, and environment. Raw scores were transformed to a range of 4-20, with higher scores indicating a better quality of life.
Assessment of symptom improvement: Symptom improvement was assessed before and after the 8-week intervention using the Kidney Disease Quality of Life (KDQOL) questionnaire[12]. The assessment included two domains: General health status and kidney disease specificity. Scores in each domain were transformed to a range of 0-100, with higher scores indicating a better health status.
Incidence of complications: After eight weeks of intervention, the incidence of complications such as infection, hyper
All data were analyzed using SPSS software (version 22.0; IBM Corp., Armonk, NY, United States). Data with a normal distribution were expressed as mean ± SD, and comparisons between groups were performed using the t-test. A P value < 0.05 was considered statistically significant.
Before the nursing intervention, no statistically significant differences were shown in the SAS and SDS scores between the two groups (P > 0.05). After eight weeks of different nursing interventions, both SAS and SDS scores in the study group were significantly lower than those in the control group and significantly lower than their baseline values (P < 0.05; Table 2).
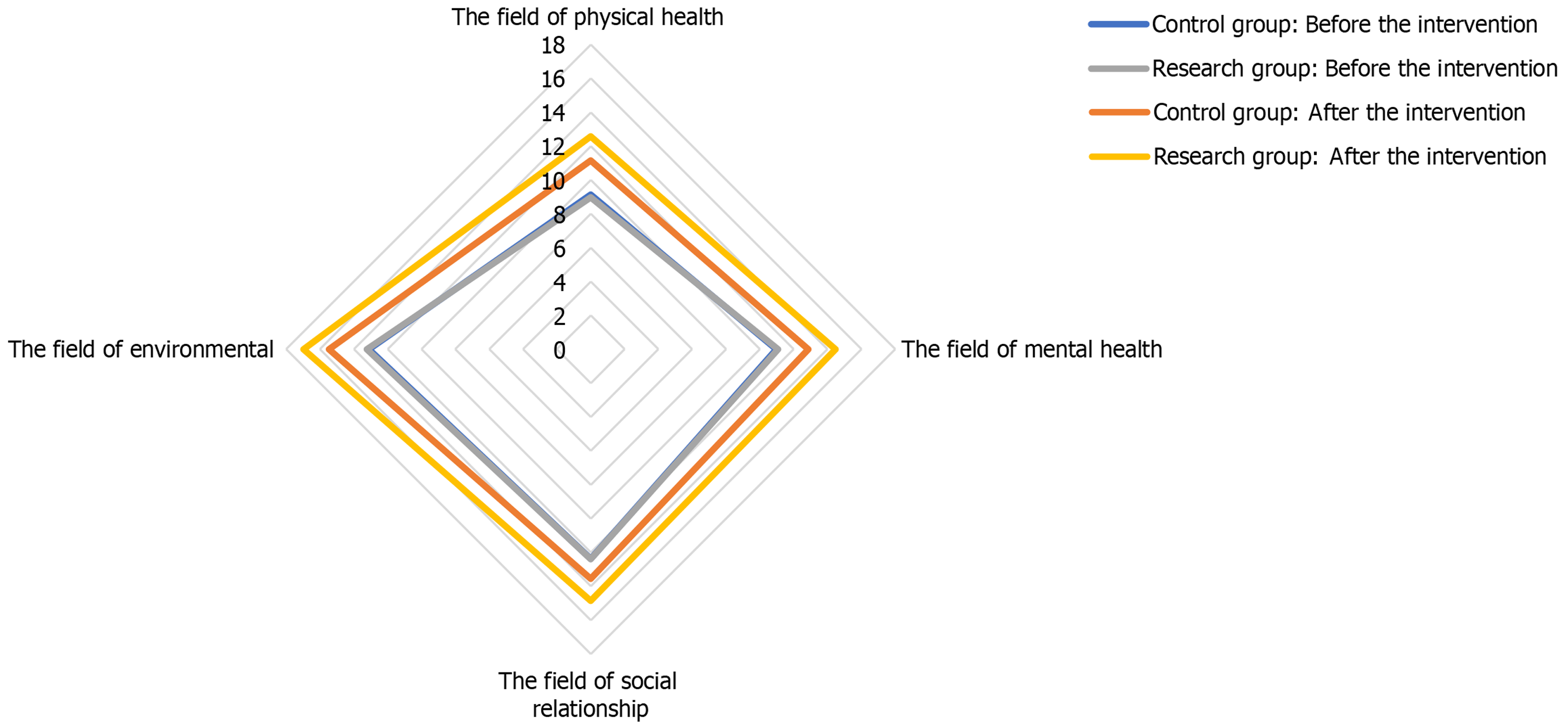
Before the intervention no statistically significant differences showed between the two groups in physical health, psychological health, social relationships, or environment domains of the WHOQOL-BREF (P > 0.05). After the intervention, scores in all domains increased in both groups, with significantly higher scores in the intervention group than in the control group (P < 0.05; Table 3 and Figure 1).
| Group | n | Physical health | Mental health | Social relations | Environment | ||||
| Before the intervention | After the intervention | Before the intervention | After the intervention | Before the intervention | After the intervention | Before the intervention | After the intervention | ||
| Control group | 64 | 9.13 ± 2.10 | 11.16 ± 2.18a | 10.96 ± 2.44 | 12.87 ± 2.27a | 12.37 ± 2.37 | 13.56 ± 2.41a | 13.10 ± 2.19 | 15.46 ± 2.15a |
| Study group | 64 | 8.98 ± 2.31 | 12.57 ± 3.02a | 11.07 ± 2.53 | 14.46 ± 2.32a | 12.40 ± 3.05 | 14.85 ± 2.33a | 13.22 ± 2.44 | 16.97 ± 1.88a |
| t value | 0.285 | 3.812 | 0.43 | 4.768 | 0.645 | 3.078 | 0.898 | 5.837 | |
| P value | 0.768 | < 0.001 | 0.658 | < 0.001 | 0.521 | 0.001 | 0.38 | < 0.001 | |
Before the intervention no statistically significant differences showed between the two groups in general health status or kidney disease-specific domain scores (P > 0.05). After the intervention, both domains showed significant improvements in both groups, with the study group scoring significantly higher than the control group (P < 0.05; Table 4).
| Group | n | General health conditions | Specific areas of kidney diseases | ||||||
| Before the intervention | After the intervention | t value | P value | Before the intervention | After the intervention | t value | P value | ||
| Control group | 64 | 65.47 ± 10.21 | 68.23 ± 9.68 | 4.497 | < 0.001 | 60.27 ± 9.74 | 63.59 ± 10.37 | 14.034 | < 0.001 |
| Study group | 64 | 66.21 ± 9.56 | 1.25 ± 10.10 | 10.657 | < 0.001 | 60.30 ± 10.32 | 68.35 ± 9.87 | 29.152 | < 0.001 |
| t value | 0.495 | 3.214 | 0.495 | 3.214 | |||||
| P value | 0.632 | 0.023 | 0.632 | 0.023 | |||||
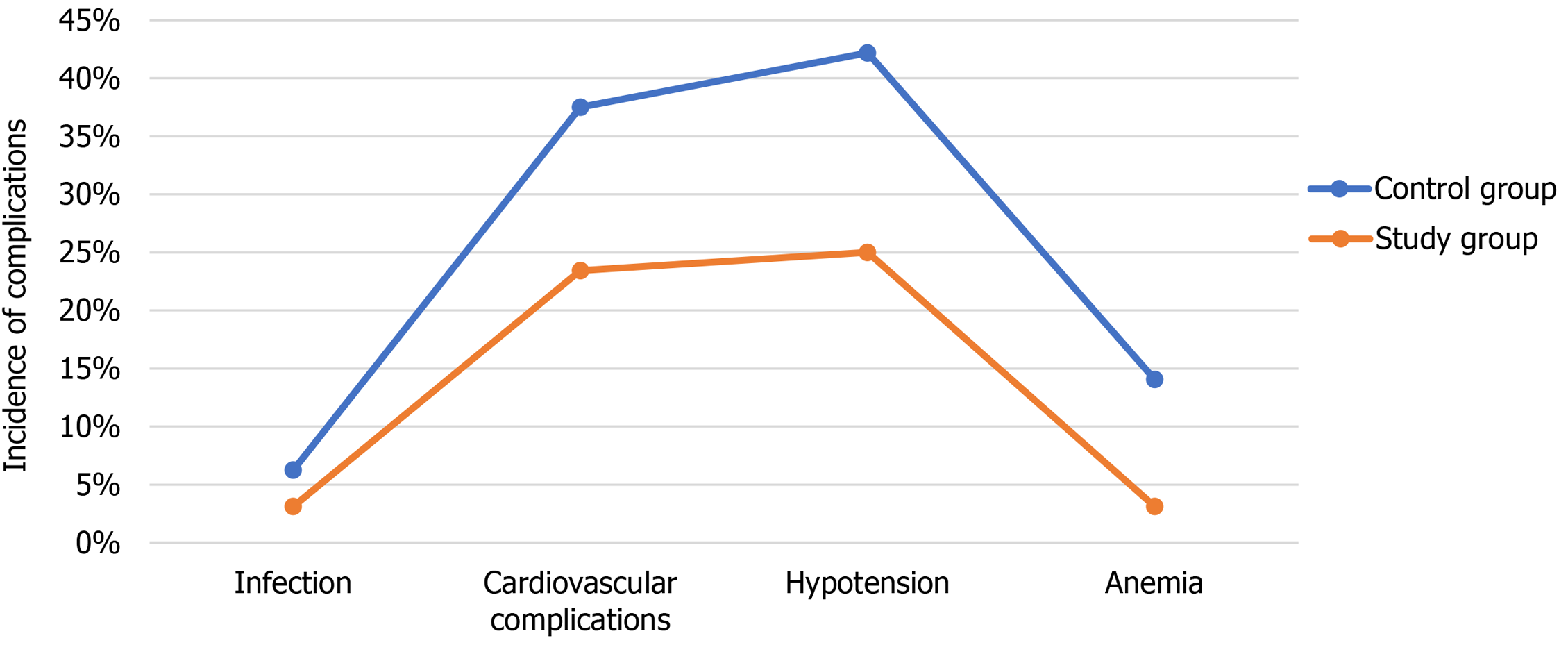
The incidence rates of hypertension (P = 0.047), hypotension (P = 0.042), and anemia (P = 0.028) were significantly lower in the study group compared with the control group. Although the incidence of infection showed a decreasing trend in the study group, the difference was not statistically significant (P > 0.05; Table 5 and Figure 2).
| Group | n | Infection | Hypertension | Hypotension complications | Anemia |
| Control group | 64 | 4 (6.25) | 24 (37.5) | 27 (42.18) | 9 (14.06) |
| Study group | 64 | 2 (3.13) | 15 (23.44) | 16 (25.00) | 2 (3.12) |
| χ2 value | 0.174 | 3.125 | 4.126 | 4.873 | |
| P value | 0.405 | 0.047 | 0.042 | 0.028 |
CKD has become a major global public health issue[13,14]. MHD, the primary renal replacement therapy for patients with ESRD, not only fulfills the mission of sustaining life, but also exerts profound effects on patients’ physiological, psychological, and social functioning. The collaborative care model, which involves the joint participation of professional healthcare providers and family members, targets the specific needs of patients with MHD[15,16]. This model, when combined with structured health education, not only emphasizes physical health, but also focuses on improving psychological well-being and social adaptability. Knowledge dissemination, behavioral interventions, and skill training enable patients and their families to establish scientific health concepts, strengthen self-management and coping abilities, enhance health literacy, and ultimately improve quality of life[17,18].
Patients undergoing long-term MHD often experience both the disease burden and financial stress, leading to widespread negative emotions such as anxiety and depression[19,20]. Traditional hospital-centered nursing care tends to focus on disease management, while neglecting patients’ psychological needs. In this study, the collaborative care model combined with mental health education was used to extend nursing services to patients’ homes, providing systematic health education and family support. Family involvement plays a pivotal role in dialysis treatment. Emotional support from family members significantly enhances patients’ sense of self-worth and belonging, reduces loneliness and depressive symptoms[9], and helps divert attention away from pain, thereby alleviating anxiety and fear[21]. Family based psychological interventions, such as emotional reassurance and counseling, further assist patients in developing a positive mindset and enhancing disease-coping abilities. Evidence suggests that patients with higher levels of family support experience lower rates of anxiety and depression, and improved quality of life and survival outcomes[22]. By enhancing disease knowledge and self-management capacity, mental health education also improves patients’ confidence[23]. Consistent with these findings, the present study demonstrated significantly lower SAS and SDS scores in the intervention group than in the control group (P < 0.05), indicating that the intervention effectively alleviated psychological distress and improved psychological health.
With regard to complications, the collaborative care model combined with mental health education yielded favorable outcomes. MHD patients are prone to multiple complications, including hypertension, anemia, and infections, which not only reduce their quality of life but may also pose life-threatening risks[24,25]. The intervention program in this study strengthened dietary guidance, medication supervision, and regular follow-ups, thereby improving treatment adherence[26]. Family caregivers play an important role in assisting patients with strict dietary control of fluid, salt, and protein intake, ensuring medication compliance and adherence to dialysis schedules. Mental health education enhanced patients’ awareness of complication prevention and management[27]. The results showed that the incidences of hypertension (P = 0.047), hypotension (P = 0.042), and anemia (P = 0.028) were significantly lower in the study group than in the control group, whereas the incidence of infection showed a decreasing trend without statistical significance (P > 0.05). These findings suggest that the intervention was particularly effective in controlling common complications such as hypo
Although this study provides encouraging evidence for the combined application of collaborative nursing and health education in MHD patients, it has several limitations: (1) Single-center design with a relatively small sample (n = 128) and all participants recruited from one hospital may introduce selection bias. Nursing resources, case-mix, and cultural backgrounds differ across regions and levels of care, thus future studies should verify the findings in multicenter, larger samples; (2) The main psychological outcomes (SAS and SDS) and quality-of-life indices (WHOQOL-BREF and KDQOL) were self-reported scales. Although they are valid and reliable, they are susceptible to social desirability and recall bias. Objective indicators, such as interdialytic weight-gain adherence and achievement rates for serum phosphorus/potassium targets, should be included in future research; and (3) No cost-effectiveness analysis was performed (e.g., whether additional staffing costs were offset by reduced rehospitalizations or complication-related expenses). Multi
In summary, the collaborative care model combined with mental health education exerted significant positive effects on psychological well-being and complication control in patients with CKD undergoing MHD. This nursing approach can be widely promoted in future clinical practice to provide higher-quality, patient-centered care and improve both the quality of life and survival outcomes in MHD patients.
| 1. | Liu F, Wu H, Zhang YY, Cheng L. [Application of incremental resistance exercise training combined with WeChat health education platform in the nursing of patients with chronic renal failure after maintenance hemodialysis]. Zhongguo Yiyao Daobao. 2022;19:162-165, 181. |
| 2. | Villanego F, Naranjo J, Vigara LA, Cazorla JM, Montero ME, García T, Torrado J, Mazuecos A. Impact of physical exercise in patients with chronic kidney disease: Sistematic review and meta-analysis. Nefrologia (Engl Ed). 2020;40:237-252. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 42] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 3. | Jhamb M, Steel JL, Yabes JG, Roumelioti ME, Erickson S, Devaraj SM, Vowles KE, Vodovotz Y, Beach S, Weisbord SD, Rollman BL, Unruh M. Effects of Technology Assisted Stepped Collaborative Care Intervention to Improve Symptoms in Patients Undergoing Hemodialysis: The TĀCcare Randomized Clinical Trial. JAMA Intern Med. 2023;183:795-805. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 33] [Article Influence: 11.0] [Reference Citation Analysis (0)] |
| 4. | Wang X, Hao X, Ma M, Jiang W, Li B, Xu Y, Sun P. Chronic kidney disease duration and suicide risk among maintenance hemodialysis patients in China. Clin Kidney J. 2024;17:sfae055. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 5. | Goel A, Grewal H, Dua A. Intradialytic complications in patients of end-stage renal disease on maintenance hemodialysis. Int J Curr Pharm Sci. 2024;16:92-95. [DOI] [Full Text] |
| 6. | Du Z, Chu T, Dai F, Mao H, Zhao J. Correlation analysis of anxiety, depression, and sleep quality in end-stage renal disease patients undergoing maintenance hemodialysis. Medicine (Baltimore). 2025;104:e44433. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 5] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 7. | Ren QY, Yang JH, Yang L. [Effect of health education based on the feedback method on psychological status and complications in maintenance hemodialysis patients with chronic kidney disease]. Zhongguo Linchuang Yisheng Zazhi. 2025;53:437-440. [DOI] [Full Text] |
| 8. | Zhang L, Zou L, Zhou L. Effectiveness of psychoeducational interventions on psychological distress and health-related quality of life among patients with maintenance hemodialysis: a systematic review and meta-analysis. Ren Fail. 2024;46:2331613. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 18] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 9. | Nephrology Group of Geriatrics Branch of Chinese Medical Association; National Clinical Research Center for Geriatric Disease. [Expert Consensus Report on the Diagnosis and Treatment of Chronic Kidney Disease in the Chinese Elderly]. Zhongguo Laonianbing Yanjiu Dianzi Zazhi. 2018;5:1-8. [DOI] [Full Text] |
| 10. | American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition. Washington: American Psychiatric Association Publishing, 2013. [RCA] [DOI] [Full Text] [Cited by in Crossref: 98503] [Cited by in RCA: 60214] [Article Influence: 3542.0] [Reference Citation Analysis (11)] |
| 11. | Ali HT, Helal A, Ismail SM, Hamdi NM, Mohamed NL, Essa AM, Mohammed M; QOL Collaborator Group, Ebada MA. Exploring the Quality of Life of University Students in Egypt: A Cross-Sectional Survey Using the World Health Organization Quality of Life-BREF (WHOQOL-BREF) Assessment. Am J Health Promot. 2025;39:263-273. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 9] [Reference Citation Analysis (0)] |
| 12. | Tasnim T, Karim KMR, Rahman T, Rashid HU. Health-related quality of life and its predictors among chronic kidney disease patients: A hospital-based cross-sectional study. PLoS One. 2025;20:e0319100. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 8] [Reference Citation Analysis (0)] |
| 13. | Karim SI, Sattar K, Ahmad T, Memon MK, Alqahtani AS, Alsubiheen AM, Alrashed FA. Cardiovascular and renal comorbidities among saudi patients with type 2 diabetes: A cross-sectional observational study. PLoS One. 2025;20:e0324233. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 14. | Raina M, Shah R, Hu J, Pember B, Cahill T, Bunchman T, Yap HK, McCulloch M. The global health burden of pediatric chronic kidney disease: An analysis of the Global Burden of Disease database from 1990 to 2021. PLoS One. 2025;20:e0323257. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 15. | Zhang Z, Wang S, Xu Z, Sun Y, Zhou X, Zhou R, Li Q, Wang G. Frailty risk prediction models in maintenance hemodialysis patients: a systematic review and meta-analysis of studies from China. Ren Fail. 2025;47:2500663. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 16. | Cui CL, Li L, Liu H. [The Impact of Family Follow-up Care on the Quality of Life of Maintenance Hemodialysis Patients]. Guoji Yizhi Yu Xueye Jinghua Zazhi. 2023;21:43-45. [DOI] [Full Text] |
| 17. | Hoffmann M, Ben Henda A, Mazouz O, Amaria R. Effects of Replacing Intradialytic Parenteral Nutrition by Oral Nutritional Supplements and Polyester-Polyarylate Membrane on Nutritional Status in Maintenance Hemodialysis Patients with End-Stage Kidney Disease. Biomed Hub. 2025;10:98-104. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 18. | Liu Y, Luo X, Ru X, Wen C, Ding N, Zhang J. Impact of a multimodal health education combined with teach-back method on self-management in hemodialysis patients: A randomized controlled trial. Medicine (Baltimore). 2024;103:e39971. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 19. | Lnu A, Rathee G, Sharma R, Dahiya S, Vaibhav F, Kumar P. Treatment Adherence and Factors Influencing It in End-Stage Renal Disease Patients on Maintenance Hemodialysis: A Study From a Tertiary Care Hospital in North India. Cureus. 2024;16:e73335. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 20. | Han XX, Zhang HY, Kong JW, Liu YX, Zhang KR, Ren WY. Systemic immune inflammation index is a valuable marker for predicting hemodialysis patients with depression: a cross-sectional study. Front Psychiatry. 2024;15:1423200. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 21. | Chen HX, Zhang XY, Ji YL. [The Impact of Family-Patient Collaborative Empowerment Nursing Intervention on Maintenance Hemodialysis Patients]. Qilu Huli Zazhi. 2020;63-65. |
| 22. | Wang G, Yi X, Fan H. Care preparedness of family caregivers of maintenance hemodialysis patients: a cross-sectional study. Sci Rep. 2024;14:18369. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 23. | Zhang H, Xia L. Clinical effect of nursing methods integrating health belief models on self-care of maintenance hemodialysis patients: A retrospective study. Medicine (Baltimore). 2024;103:e38703. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 24. | Chen S, Cao Q, Bu S, Xu L, Zhou Z, Wu Y, Zheng H. The value of triglyceride glucose-body mass index, fasting blood glucose to HDL-C ratio, and platelet to HDL-C ratio in predicting abdominal aortic calcification in maintenance hemodialysis patients. Ren Fail. 2025;47:2505699. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 25. | Shi Y, Wang T, Ding Z, Yan L, Yao C, Qian H. Frequent hypoglycemia during hemodialysis in ESRD patients leads to higher risk of death. Ren Fail. 2025;47:2484471. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 26. | Kohler M, Thaqi Q, Kuske S, Schwalbach T, Riguzzi M, Naef R. Evidence adaptation and tailored implementation of family bereavement support in specialised palliative care: A multi-method study. Int J Nurs Stud Adv. 2025;8:100305. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 27. | Xu Y, Chen Z, Tang X, Xia X, Zhao N, Zou S. Latent profile analysis of nutrition knowledge, attitudes, and practices and their influencing factors in maintenance hemodialysis patients. Sci Rep. 2025;15:17246. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |