Published online Apr 19, 2026. doi: 10.5498/wjp.v16.i4.115520
Revised: December 8, 2025
Accepted: January 20, 2026
Published online: April 19, 2026
Processing time: 142 Days and 24 Hours
The increasing prevalence of adolescent depression has led to widespread antidepressant use, with associated risks of intentional and accidental poisoning. Family dysfunction, parental mental health problems, and poor family psychological environment are known risk factors for adolescent self-harm behaviors, but their specific role in antidepressant poisoning has not been systematically investigated.
To analyze the incidence characteristics of adolescent antidepressant poisoning in emergency departments, explore the influence of family psychological envi
A retrospective study design was employed, collecting data from 250 adolescent patients aged 12-18 years admitted to the emergency department of a hospital from January 2020 to January 2025, including 28 cases of antidepressant poisoning (poisoning group) and 222 cases of non-drug poisoning adolescent patients (nor
The incidence of adolescent antidepressant poisoning in emergency departments was 11.2% [95% confidence interval (CI): 7.8%-15.8%]. Multivariate logistic regression analysis showed that female gender [odds ratio (OR) = 2.847, 95%CI: 1.024-7.913], high Center for Epidemiologic Studies Depression Scale scores (OR = 1.124, 95%CI: 1.062-1.190), low Family Structure Characteristics Questionnaire total scores (OR = 0.934, 95%CI: 0.891-0.979), high parental Symptom Checklist-90 total scores (OR = 1.018, 95%CI: 1.005-1.031), and low Social Support Rating Scale total scores (OR = 0.895, 95%CI: 0.839-0.955) were independent influencing factors for adolescent antidepressant poisoning (all P < 0.05).
The incidence of adolescent antidepressant poisoning is relatively high, with female gender, depression severity, family structure instability, parental mental health problems, and lack of social support being important in
Core Tip: Among adolescents presenting to the emergency department, antidepressant poisoning comprised 11.2% of visits and was predominantly intentional. Multivariable analysis showed higher depressive symptoms (Center for Epidemiologic Studies Depression Scale), greater parental psychological distress (Symptom Checklist-90), lower social support (Social Support Rating Scale), and unstable family structure (Family Structure Characteristics Questionnaire) independently correlated with antidepressant poisoning, especially in females. These findings support a family-centered, bio-psycho-social prevention strategy that couples rapid emergency department screening with targeted interventions for parental mental health and adolescent social-support strengthening.
- Citation: Yu W, Wang F. Analysis of emergency adolescent antidepressant poisoning incidence and family psychological environment influencing factors. World J Psychiatry 2026; 16(4): 115520
- URL: https://www.wjgnet.com/2220-3206/full/v16/i4/115520.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i4.115520
Adolescence is a critical stage of individual physical and mental development, and also a high-incidence period for various mental health problems. In recent years, with increasing social competitive pressure and accelerated pace of life, adolescent mental health problems such as depression and anxiety have become increasingly prominent, becoming a global public health challenge[1]. World Health Organization data shows that depression is one of the main causes of disability among adolescents, seriously affecting their learning, life, and social functioning. To address this problem, the use of antidepressant medications in adolescent populations has shown a rapid upward trend[2].
However, the widespread application of antidepressant medications in adolescents has also brought new safety hazards. Due to the specificity of their physiological and psychological development, adolescents have significantly different sensitivity to medications compared to adults, making them more prone to adverse drug reactions[3]. Particularly under the influence of emotional impulse or self-harm behaviors, adolescents may experience antidepressant overdose, leading to acute poisoning events. Such events not only directly threaten adolescents' lives but also impose heavy burdens on families and society[4].
Family, as an important environment for adolescent growth, has a decisive impact on adolescent mental health development through its psychological atmosphere. Studies have shown that family dysfunction, inappropriate parental rearing patterns, and family stress events are closely related to adolescent depression and self-harm behaviors[5]. Poor family psychological environment may increase the risk of adolescents engaging in dangerous behaviors, including drug poisoning events, through various mechanisms. However, current systematic research on the impact of family psychological environment on adolescent antidepressant poisoning is relatively lacking[6].
Given the complexity and severity of adolescent antidepressant poisoning events, understanding their incidence characteristics and related influencing factors in depth, particularly the mechanism of family psychological environment, is of great significance for developing effective prevention strategies. This study adopts a descriptive cross-sectional design to systematically analyze the clinical characteristics of adolescent antidepressant poisoning patients admitted to emergency departments, and assess the impact of family psychological environment from multiple dimensions including family structure, family function, parental mental health, rearing patterns, and social support, aiming to provide scientific evidence for clinical medical staff to identify high-risk adolescents and improve prevention strategies[7].
This study adopted a retrospective study design, collecting clinical data of adolescent patients admitted to our hospital's emergency department from January 2020 to January 2025.
Inclusion criteria: (1) Age criteria: Adolescent patients aged 12-18 years, conforming to the World Health Organization’s definition of adolescent age; (2) Diagnostic criteria: Clearly diagnosed by clinical physicians, including antidepressant poisoning patients and non-drug poisoning adolescent patients seeking emergency care; (3) Informed consent: Patient guardians signed informed consent forms, agreeing to participate in this study; (4) Cooperation criteria: Patients with clear consciousness, able to understand and cooperate in completing relevant scale assessments; and (5) Data com
Exclusion criteria: (1) Cognitive dysfunction: Presence of intellectual developmental delay, severe cognitive dysfunction, or mental developmental delay, unable to accurately understand scale content or cooperate in completing assessments; (2) Consciousness state: Presence of severe consciousness disorder, coma state, or severely abnormal mental state at presentation, unable to conduct effective communication and assessment; (3) Comorbid diseases: Comorbidity with severe physical diseases (such as malignant tumors, severe cardiovascular and cerebrovascular diseases, end-stage renal disease, etc.) that may affect the accuracy of psychological state assessment; (4) Drug effects: Currently using medications that may significantly affect cognitive function and psychological state (such as sedatives, antipsychotic drugs, etc.), and unable to discontinue or adjust dosage; and (5) Compliance issues: Patients or guardians refusing to participate in the study, or voluntarily withdrawing during the study process.
Basic demographic data: Collected basic demographic information of patients, including: (1) Age: Recording patients’ exact age (in years), stratified by age groups 12-14 years, 15-16 years, 17-18 years; (2) Gender: Male or female; and (3) Educational level: Current school stage (middle school, high school) and specific grade.
Clinical data: Systematically collected patient-related clinical data: (1) Poisoning-related data, including antidepressant drug types [selective serotonin reuptake inhibitors (SSRIs), serotonin-norepinephrine reuptake inhibitors, tricyclics, etc.], dosage taken, poisoning severity grading (mild, moderate, severe), presentation time, clinical symptoms and signs, relevant laboratory examination results, treatment regimens, and length of hospital stay; (2) Past medical history data, covering psychiatric disease history, antidepressant medication use history, previous suicide attempt history, other chronic disease history, etc.; and (3) Analysis of specific causes of poisoning occurrence, distinguishing different situations such as accidental poisoning, suicidal intent, drug abuse, etc.
Family psychological environment assessment data: Standardized scales were used to comprehensively assess family psychological environment: (1) Family structure characteristics: The self-designed Family Structure Characteristics Questionnaire (FSCQ) was used to systematically assess patients’ family structure conditions. This questionnaire includes 5 dimensions with 25 items covering family integrity, family size, economic status, living environment, and care patterns, using a combination of multiple choice questions and graded scoring. The family integrity dimension has 5 items (5-15 points), assessing family member composition, classified as intact family (both parents present, 3 points), single-parent family (one parent absent, 2 points), and reconstituted family (step-parents or other guardians, 1 point); family size dimension has 4 items (4-12 points), assessing family population and generational structure; economic status dimension has 6 items (6-18 points), classified by family monthly income as high income (> 8000 yuan, 3 points), middle income (3000-8000 yuan, 2 points), low income (< 3000 yuan, 1 point); living environment dimension has 5 items (5-15 points), assessing residential area, housing conditions, and stability; care pattern dimension has 5 items (5-15 points), assessing primary caregiver identity, care quality, and stability. Total score 25-75 points, higher scores indicate more stable family structure; (2) Family function assessment using the Family Adaptability and Cohesion Evaluation Scales-II (FACES-II): The second version of FACES-II was used to comprehensively assess family function status. This scale includes 2 core dimensions of cohesion and adaptability with 30 items total, using a 5-point Likert scoring method (1 = never, 2 = rarely, 3 = sometimes, 4 = frequently, 5 = always). The cohesion dimension has 15 items (15-75 points), assessing emotional connections among family members; the adaptability dimension has 15 items (15-75 points), assessing the family’s ability to change in response to problems arising from family circumstances and different family developmental stages. For each item, respondents need to answer twice, once for their actual feelings about their current family situation, and once for their desired ideal family situation; (3) Parental mental health assessment using the Symptom Checklist-90 (SCL-90): The SCL-90 was used to assess patients’ parents’ mental health status. This scale includes 9 symptom dimensions with 90 items total: Somatization, obsessive-compulsive symptoms, interpersonal sensitivity, depression, anxiety, hostility, phobia, paranoia, and psychoticism, using a 5-point Likert scoring method (1 = none, 2 = mild, 3 = moderate, 4 = severe, 5 = extremely severe). The somatization dimension has 12 items (12-60 points), assessing physical discomfort; obsessive-compulsive symptoms dimension has 10 items (10-50 points), assessing obsessive thoughts and behaviors; interpersonal sensitivity dimension has 9 items (9-45 points), assessing discomfort in interpersonal interactions; depression dimension has 13 items (13-65 points), assessing depressive mood and cognition; anxiety dimension has 10 items (10-50 points), assessing anxiety symptoms; hostility dimension has 6 items (6-30 points), assessing anger and aggression; phobia dimension has 7 items (7-35 points), assessing fear responses; paranoia dimension has 6 items (6-30 points), assessing suspicion and persecutory thoughts; psychoticism dimension has 10 items (10-50 points), assessing psychotic symptoms. Total score 90-450 points, any factor score ≥ 2 points or total score ≥ 160 points or positive items ≥ 43 items suggests significant mental health problems; (4) Analysis of parental rearing attitudes using the Egna Minnen Betraffande Uppfostran (EMBU): The Chinese revised version of EMBU was used to analyze parents’ rearing attitudes and behavioral patterns. The father version scale includes 6 dimensions with 58 items: Emotional warmth and understanding, punishment and strictness, excessive interference, favoring subjects, rejection and denial, and overprotection. The mother version scale includes 5 dimensions with 57 items: Emotional warmth and understanding, excessive interference and overprotection, rejection and denial, punishment and strictness, and favoring subjects, using a 4-point Likert scoring method (1 = never, 2 = rarely, 3 = frequently, 4 = always). Father version: Emotional warmth and understanding dimension has 19 items (19-76 points), assessing father’s care and understanding of children; punishment and strictness dimension has 12 items (12-48 points), assessing harsh punishment and rough treatment; excessive interference dimension has 14 items (14-56 points), assessing excessive control and intervention of children; favoring subjects dimension has 6 items (6-24 points), assessing degree of favoritism toward children; rejection and denial dimension has 12 items (12-48 points), assessing rejection and negative attitudes toward children; overprotection dimension has 18 items (18-72 points), assessing excessive protection and indulgence behaviors. Mother version: Emotional warmth and understanding dimension has 19 items (19-76 points); excessive interference and overprotection dimension has 19 items (19-76 points); rejection and denial dimension has 14 items (14-56 points); punishment and strictness dimension has 12 items (12-48 points); favoring subjects’ dimension has 6 items (6-24 points). Higher scores indicate more pronounced rearing patterns; (5) Survey of major family stress events in the past year: The Life Events Scale (LES) was used to assess major stress events experienced by patients’ families in the past year. This scale includes 3 dimensions with 48 items covering family life, work and study, and social and other aspects, using weighted scoring. Each event is assigned different weight scores according to its impact on individuals, with total scores reflecting the cumulative stress intensity of life events experienced by individuals in the past year. Scoring is weighted according to event frequency and impact degree, with total scores ≥ 20 points suggesting significant life stress. This scale can effectively identify family stress levels; and (6) Assessment of family social support using the Social Support Rating Scale (SSRS): The SSRS was used to assess the status of patients’ families in obtaining and utilizing social support. This scale includes 3 dimensions with 10 items: Objective support, subjective support, and utilization of support, using a combination of multiple scoring methods. The objective support dimension has 3 items (0-22 points), assessing actually received support, including number of economic support sources, number of help-seeking targets, and number of group relationships; subjective support dimension has 4 items (4-28 points), assessing subjective feelings about support, using a 7-point scoring method; utilization of support dimension has 3 items (3-12 points), assessing actual utilization of support, including confiding methods, help-seeking methods, and degree of activity participation. Total score 7-62 points, higher scores indicate better social support levels, total scores ≤ 22 points suggest insufficient social support, 23-44 points indicate moderate level, ≥ 45 points indicate good level.
Adolescent psychosocial factors: Comprehensive assessment of patients’ psychosocial conditions: (1) Mental health status assessment: The Center for Epidemiologic Studies Depression Scale (CES-D) was used to measure depression levels. This scale includes 20 items using 4-point scoring (0 = rarely, 3 = most of the time), total score 0-60 points, ≥ 16 points suggests presence of depressive symptoms, ≥ 25 points suggests obvious depressive symptoms; the Self-Rating Anxiety Scale (SAS) was used to assess anxiety levels. This scale includes 20 items using 4-point scoring (1 = rarely, 4 = persistent), standard score = raw score × 1.25, standard score ≥ 50 points suggests presence of anxiety symptoms, ≥ 60 points suggests obvious anxiety symptoms; (2) Academic stress factors: The Adolescent LES (ALES) was used to assess patients’ academic stress conditions. This scale includes 6 dimensions with 27 items covering academic stress, interpersonal relationships, punishment, loss, health adaptation, and others, using 5-point scoring (1 = no impact, 5 = extremely severe impact). Total score 27-135 points, higher scores indicate greater life event stress; (3) Empathy ability assessment: The Chinese version of the Interpersonal Reactivity Index (IRI) was used to assess adolescents’ empathic ability. This scale includes 4 dimensions with 28 items: Perspective taking, fantasy, empathic concern, and personal distress, using 5-point Likert scoring (0 = completely inconsistent, 4 = completely consistent). The perspective taking dimension has 7 items (0-28 points), assessing individuals’ tendency to spontaneously adopt others’ perspectives; fantasy dimension has 7 items (0-28 points), assessing individuals’ empathic responses to fictional characters; empathic concern dimension has 7 items (0-28 points), assessing individuals’ sympathy and concern response tendencies toward those in misfortune; personal distress dimension has 7 items (0-28 points), assessing anxiety and discomfort feelings in tense interpersonal situations. Perspective taking and fantasy dimensions belong to cognitive empathy, empathic concern and personal distress belong to emotional empathy, total score 0-112 points, higher scores indicate stronger empathic ability in corresponding dimensions; and (4) Stress coping ability analysis: The Coping Style Questionnaire (CSQ) was used to measure coping strategies adopted by patients when facing stress and difficulties. This scale includes 6 dimensions with 62 items: Problem solving, self-blame, help-seeking, fantasy, withdrawal, and rationalization, using “yes/no” binary choice format rather than multiple choice. The problem solving dimension includes 12 items, reflecting mature coping styles, demonstrating individuals’ ability to adopt active coping and rational thinking when facing difficulties; self-blame and fantasy dimensions reflect immature coping styles, manifesting as excessive self-blame and unrealistic fantasy escape; withdrawal dimension reflects negative coping, demonstrating tendencies to avoid and escape problems; rationalization and help-seeking dimensions belong to mixed coping styles, containing both positive components and certain limitations. Scoring principle: Each item selected as “yes” scores 1 point, “no” scores 0 points, but item 19 in the problem solving dimension and items 36, 39, 42 in the help-seeking dimension are reverse scored. Scoring method uses factor scoring, i.e., subscale factor score = subscale item total score/number of items in that subscale. Assessment timing: To minimize the potential impact of acute distress on self-report measures, all psychological assessments were conducted after medical stabilization, typically 24-48 hours post-admission when patients demonstrated clear consciousness and ability to communicate effectively. Clinical staff confirmed patient readiness for assessment based on their physical and mental state. This timing was chosen to balance the need for accurate psychological evaluation with the practical constraints of emergency department care.
Incidence statistical data: Collected total number of adolescent emergency department visits during the same period to calculate antidepressant poisoning incidence.
SPSS version 26.0 statistical software was used for data analysis. First, normality tests were conducted for all continuous variables. For analysis of variance, Levene’s test was used to assess homogeneity of variance between groups. Continuous data were expressed as mean ± SD for normally distributed data, and median (interquartile range) for non-normally distributed data; categorical data were expressed as n (%). Emergency department adolescent antidepressant poisoning incidence = number of adolescent antidepressant poisoning patients during study period/total number of adolescent emergency department visits during same period × 100%, with 95% confidence intervals (CIs) calculated. For group comparisons, normally distributed continuous data with homogeneous variance used independent samples t-tests or one-way ANOVA, non-normally distributed or heterogeneous variance data used Mann-Whitney U tests or Kruskal-Wallis H tests; categorical data used χ2 tests or Fisher’s exact test. To identify influencing factors for adolescent antidepressant poisoning, variables with P < 0.10 in univariate analysis were included in multivariate logistic regression analysis, using forward method to establish prediction models, calculating odds ratios (ORs) and 95%CI. Collinearity diagnosis was performed for continuous variables, with variance inflation factor < 5 as acceptable level. Model goodness of fit was assessed using Hosmer-Lemeshow test, discrimination ability was evaluated using area under receiver operating characteristic (ROC) curve. All statistical tests used two-sided tests, with P < 0.05 considered statistically significant.
This retrospective study was approved by the Ethics Committee of the Affiliated Hangzhou First People’s Hospital (Approval No. 2025ZN372-1), strictly protecting patient privacy, with all data used only for scientific research, not involving disclosure of patients’ personal identity information.
From January 2020 to January 2025, our hospital’s emergency department received 250 adolescent patients meeting study criteria. Among these, 28 cases had antidepressant poisoning, with an incidence of 11.2% (95%CI: 7.8%-15.8%). The 28 antidepressant poisoning patients were designated as the poisoning group, and 222 non-drug poisoning adolescent patients as the normal group.
Comparison of basic demographic characteristics between the two groups showed significant differences. In age distribution, the proportion of 17-18 years old in the poisoning group was significantly higher than the normal group (60.7% vs 38.7%), while the proportion of 12-14 years old was relatively lower (17.9% vs 32.4%), with statistically significant differences (P = 0.024). In gender composition, female patients comprised the vast majority in the poisoning group (78.6%), significantly higher than the normal group (48.6%), with obvious gender ratio differences (P = 0.002). Educational level analysis showed that the proportion of high school students in the poisoning group (67.9%) was significantly higher than the normal group (47.7%), while the proportion of middle school students was relatively lower (32.1% vs 52.3%), with statistically significant differences (P = 0.045). Specific grade distribution also showed significant differences (P = 0.015), indicating obvious differences in distribution characteristics of antidepressant poisoning among adolescents of different age groups, genders, and educational stages (Table 1).
| Characteristic | Poisoning group (n = 28) | Normal group (n = 222) | χ2 value | P value |
| Age group | 7.452 | 0.024 | ||
| 12-14 years | 5 (17.9) | 72 (32.4) | ||
| 15-16 years | 6 (21.4) | 64 (28.8) | ||
| 17-18 years | 17 (60.7) | 86 (38.7) | ||
| Gender | 9.127 | 0.002 | ||
| Male | 6 (21.4) | 114 (51.4) | ||
| Female | 22 (78.6) | 108 (48.6) | ||
| Educational level | 4.006 | 0.045 | ||
| Middle school | 9 (32.1) | 116 (52.3) | ||
| High school | 19 (67.9) | 106 (47.7) | ||
| Specific grade distribution | 12.384 | 0.015 | ||
| 7th grade | 2 (7.1) | 38 (17.1) | ||
| 8th grade | 3 (10.7) | 42 (18.9) | ||
| 9th grade | 4 (14.3) | 36 (16.2) | ||
| 10th grade | 6 (21.4) | 38 (17.1) | ||
| 11th grade | 8 (28.6) | 36 (16.2) | ||
| 12th grade | 5 (17.9) | 32 (14.4) |
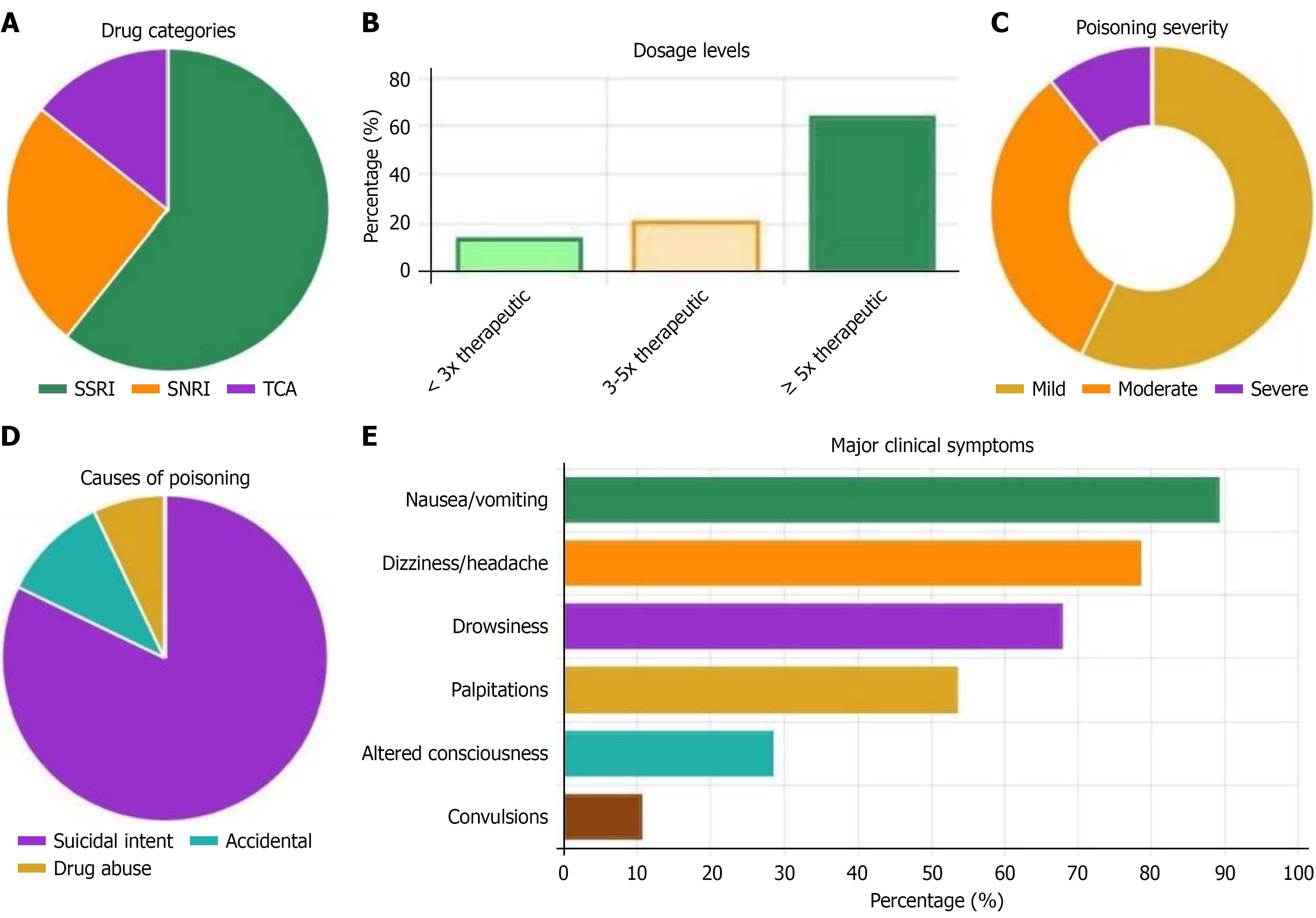
Clinical characteristic analysis of the poisoning group showed that SSRI class poisoning was most common, accounting for 60.7%, followed by serotonin-norepinephrine reuptake inhibitor class (25.0%) and tricyclic class (14.3%). Regarding dosage taken, 64.3% of patients took doses ≥ 5 times the therapeutic dose, suggesting severe poisoning. Most patients (71.4%) presented within 2-6 hours after drug ingestion, with mild poisoning severity being predominant (57.1%). Clinical symptoms were most commonly nausea and vomiting (89.3%), followed by dizziness and headache (78.6%) and somnolence (67.9%). Notably, 82.1% of poisoning events had suicidal intent, reflecting serious psychological crisis. Past history showed 71.4% of patients had psychiatric disease history, 64.3% had antidepressant medication use history, 25.0% had previous suicide attempt history, with average hospital stay of 4.3 ± 2.2 days (Figure 1; Table 2).
| Clinical characteristic | Poisoning group (n = 28) |
| Drug type | |
| SSRI class | 17 (60.7) |
| SNRI class | 7 (25.0) |
| Tricyclic class | 4 (14.3) |
| Dosage taken | |
| < 3 times therapeutic dose | 4 (14.3) |
| 3-5 times therapeutic dose | 6 (21.4) |
| ≥ 5 times therapeutic dose | 18 (64.3) |
| Presentation time | |
| < 2 hours | 5 (17.9) |
| 2-6 hours | 20 (71.4) |
| > 6 hours | 3 (10.7) |
| Poisoning severity | |
| Mild | 16 (57.1) |
| Moderate | 9 (32.1) |
| Severe | 3 (10.7) |
| Main clinical symptoms | |
| Nausea and vomiting | 25 (89.3) |
| Dizziness and headache | 22 (78.6) |
| Somnolence | 19 (67.9) |
| Palpitations | 15 (53.6) |
| Consciousness disorder | 8 (28.6) |
| Convulsions | 3 (10.7) |
| Treatment regimen | |
| Gastric lavage + activated charcoal | 24 (85.7) |
| Symptomatic supportive treatment | 28 (100.0) |
| Blood purification | 3 (10.7) |
| Mechanical ventilation | 2 (7.1) |
| Cause of poisoning | |
| Suicidal intent | 23 (82.1) |
| Accidental poisoning | 3 (10.7) |
| Drug abuse | 2 (7.1) |
| Past history | |
| Psychiatric disease history | 20 (71.4) |
| Antidepressant medication use history | 18 (64.3) |
| Previous suicide attempt history | 7 (25.0) |
| Other chronic disease history | 5 (17.9) |
| Abnormal laboratory findings | |
| Liver function abnormalities | 12 (42.9) |
| ECG abnormalities | 16 (57.1) |
| Electrolyte disorders | 8 (28.6) |
| Hospital stays (days) | 4.3 ± 2.2 |
Family structure characteristics comparison: The poisoning group scored significantly lower than the normal group in all FSCQ dimensions and total score (all P < 0.05). Family integrity dimension score was 8.4 ± 2.8 points in the poisoning group vs 10.4 ± 2.3 points in the normal group (P = 0.002); economic status dimension was 9.8 ± 3.2 points in the poisoning group vs 12.6 ± 2.8 points in the normal group (P < 0.001); FSCQ total score was 44.6 ± 8.6 points in the poisoning group vs 55.3 ± 7.4 points in the normal group (P < 0.001; Table 3).
| FSCQ dimension | Poisoning group (n = 28) | Normal group (n = 222) | 95%CI | t value | P value |
| Family integrity | 8.4 ± 2.8 | 10.4 ± 2.3 | -3.3 to -0.7 | -3.942 | 0.002 |
| Family size | 7.1 ± 2.2 | 8.2 ± 1.7 | -1.9 to -0.3 | -2.891 | 0.004 |
| Economic status | 9.8 ± 3.2 | 12.6 ± 2.8 | -4.2 to -1.4 | -4.862 | < 0.001 |
| Living environment | 8.9 ± 2.6 | 11.5 ± 2.2 | -3.6 to -1.6 | -5.521 | < 0.001 |
| Care pattern | 10.4 ± 2.9 | 12.6 ± 2.4 | -3.4 to -1.0 | -4.289 | < 0.001 |
| FSCQ total score | 44.6 ± 8.6 | 55.3 ± 7.4 | -14.1 to -7.3 | -5.874 | < 0.001 |
Family function status comparison: FACES-II assessment results showed that the poisoning group’s family cohesion score was 36.7 ± 10.2 points, significantly lower than the normal group’s 49.2 ± 8.6 points (P < 0.001); family adaptability score was 39.4 ± 9.1 points in the poisoning group vs 46.7 ± 7.9 points in the normal group (P < 0.001). Further analysis of the difference between actual feelings and ideal conditions showed that the poisoning group’s ideal-actual difference in cohesion dimension was significantly greater than the normal group (P < 0.001), and the ideal-actual difference in adaptability dimension was also greater than the normal group (P < 0.001), suggesting a larger gap between current family function status and expectations in the poisoning group (Table 4).
| FACES-II dimension | Poisoning group (n = 28) | Normal group (n = 222) | 95%CI | t value | P value |
| Cohesion | |||||
| Actual feelings | 36.7 ± 10.2 | 49.2 ± 8.6 | -16.4 to -8.6 | -6.784 | < 0.001 |
| Ideal condition | 58.7 ± 8.2 | 62.4 ± 7.8 | -7.3 to -0.1 | -2.359 | 0.019 |
| Ideal-actual difference | 22.0 ± 8.1 | 13.2 ± 5.4 | 4.9-12.7 | 6.195 | < 0.001 |
| Adaptability | |||||
| Actual feelings | 39.4 ± 9.1 | 46.7 ± 7.9 | -10.8 to -3.8 | -4.462 | < 0.001 |
| Ideal condition | 56.2 ± 7.9 | 58.9 ± 8.1 | -5.8 to 0.4 | -1.735 | 0.084 |
| Ideal-actual difference | 16.8 ± 7.2 | 12.2 ± 4.7 | 2.4-6.8 | 3.742 | < 0.001 |
Parental mental health status comparison: SCL-90 assessment showed that parents in the poisoning group scored significantly higher than the normal group in all symptom dimensions. Depression dimension score was 25.4 ± 7.6 points in the poisoning group vs 18.6 ± 5.4 points in the normal group (P < 0.001); anxiety dimension score was 21.8 ± 6.9 points in the poisoning group vs 15.4 ± 4.6 points in the normal group (P < 0.001); SCL-90 total score was 172.5 ± 38.2 points in the poisoning group vs 132.7 ± 30.2 points in the normal group (P < 0.001; Table 5).
| SCL-90 dimension | Poisoning group (n = 28) | Normal group (n = 222) | 95%CI | t value | P value |
| Somatization | 20.1 ± 5.9 | 16.2 ± 4.5 | 1.8-6.0 | -3.724 | < 0.001 |
| Obsessive-compulsive | 17.2 ± 5.2 | 13.6 ± 3.9 | 1.8-5.4 | -3.892 | < 0.001 |
| Interpersonal sensitivity | 15.1 ± 4.6 | 11.9 ± 3.4 | 1.6-4.8 | -3.921 | < 0.001 |
| Depression | 25.4 ± 7.6 | 18.6 ± 5.4 | 4.2-9.4 | -5.082 | < 0.001 |
| Anxiety | 21.8 ± 6.9 | 15.4 ± 4.6 | 4.1-8.7 | -5.421 | < 0.001 |
| Hostility | 12.4 ± 4.1 | 9.1 ± 3.1 | 1.8-4.8 | -4.523 | < 0.001 |
| Phobia | 13.6 ± 4.8 | 10.6 ± 3.3 | 1.4-4.6 | -3.582 | < 0.001 |
| Paranoia | 11.2 ± 3.7 | 8.7 ± 2.8 | 1.3-3.7 | -3.841 | < 0.001 |
| Psychoticism | 16.1 ± 5.4 | 13.1 ± 4.2 | 1.1-4.9 | -3.167 | 0.002 |
| SCL-90 total score | 172.5 ± 38.2 | 132.7 ± 30.2 | 26.5-53.1 | -6.021 | < 0.001 |
Parental rearing patterns comparison: EMBU assessment results showed that fathers in the poisoning group scored significantly lower than the normal group in emotional warmth and understanding dimension (42.3 ± 9.8 points vs 53.1 ± 8.4 points, P < 0.001), while scoring significantly higher in punishment and strictness, excessive interference, and rejection and denial dimensions. Maternal rearing patterns showed similar trends, with the poisoning group scoring lower in emotional warmth and understanding dimension (46.7 ± 10.1 points vs 55.3 ± 8.8 points, P < 0.001), and higher in excessive interference and overprotection, rejection and denial, and punishment and strictness dimensions (Table 6).
| EMBU dimension | Poisoning group (n = 28) | Normal group (n = 222) | 95%CI | t value | P value |
| Father version | |||||
| Emotional warmth and understanding | 42.3 ± 9.8 | 53.1 ± 8.4 | -14.4 to -7.2 | -6.142 | < 0.001 |
| Punishment and strictness | 24.8 ± 6.7 | 18.6 ± 5.4 | 3.8-8.6 | 5.128 | < 0.001 |
| Excessive interference | 28.4 ± 7.2 | 21.8 ± 6.7 | 3.9-9.3 | 4.829 | < 0.001 |
| Favoring subjects | 14.1 ± 3.9 | 12.6 ± 3.4 | 0.1-2.9 | 2.126 | 0.035 |
| Rejection and denial | 22.7 ± 6.1 | 16.9 ± 4.9 | 3.6-8.0 | 5.284 | < 0.001 |
| Overprotection | 32.8 ± 7.9 | 28.4 ± 7.2 | 1.5-7.3 | 3.018 | 0.003 |
| Mother version | |||||
| Emotional warmth and understanding | 46.7 ± 10.1 | 55.3 ± 8.8 | -12.4 to -4.8 | -4.721 | < 0.001 |
| Excessive interference and overprotection | 37.2 ± 8.4 | 31.6 ± 7.4 | 2.7-8.5 | 3.728 | < 0.001 |
| Rejection and denial | 24.3 ± 6.5 | 19.2 ± 5.6 | 2.7-7.5 | 4.382 | < 0.001 |
| Punishment and strictness | 20.9 ± 5.8 | 16.8 ± 4.7 | 2.0-6.2 | 3.951 | < 0.001 |
| Favoring subjects | 13.7 ± 3.8 | 11.9 ± 3.2 | 0.7-2.9 | 2.634 | 0.009 |
Family stress events and social support comparison: The poisoning group scored significantly higher than the normal group on LES total score (35.6 ± 11.8 points vs 18.9 ± 8.6 points, P < 0.001), suggesting the poisoning group families experienced more stress events. Dimensional analysis showed the poisoning group scored significantly higher than the normal group in family life, work and study, and social and other dimensions. SSRS assessment showed the poisoning group scored significantly lower than the normal group in objective support, subjective support, and utilization of support dimensions, with SSRS total score of 29.4 ± 7.2 points in the poisoning group vs 41.2 ± 7.9 points in the normal group (P < 0.001; Table 7).
| Scale and dimension | Poisoning group (n = 28) | Normal group (n = 222) | 95%CI | t value | P value |
| LES total score | 35.6 ± 11.8 | 18.9 ± 8.6 | 12.5-20.9 | 7.962 | < 0.001 |
| LES dimensions | |||||
| Family life | 13.2 ± 4.2 | 7.2 ± 3.2 | 4.5-7.5 | 8.094 | < 0.001 |
| Work and study | 12.8 ± 3.9 | 6.8 ± 2.9 | 4.6-7.4 | 8.752 | < 0.001 |
| Social and others | 9.6 ± 3.5 | 4.9 ± 2.8 | 3.4-6.0 | 7.428 | < 0.001 |
| SSRS total score | 29.4 ± 7.2 | 41.2 ± 7.9 | -15.2 to -8.4 | -7.924 | < 0.001 |
| SSRS dimensions | |||||
| Objective support | 9.1 ± 3.1 | 12.6 ± 3.2 | -4.7 to -2.3 | -5.712 | < 0.001 |
| Subjective support | 12.4 ± 3.8 | 16.9 ± 4.1 | -6.2 to -2.8 | -5.831 | < 0.001 |
| Utilization of support | 7.9 ± 2.3 | 11.7 ± 2.6 | -4.8 to -2.8 | -7.841 | < 0.001 |
Mental health status comparison: The poisoning group CES-D score was 29.8 ± 8.4 points, significantly higher than the normal group’s 12.8 ± 6.2 points (P < 0.001); SAS standard score was 56.3 ± 9.1 points in the poisoning group vs 38.2 ± 7.6 points in the normal group (P < 0.001). The poisoning group depressive symptom prevalence was 96.4% (27/28), obvious depressive symptom prevalence was 89.3% (25/28); anxiety symptom prevalence was 92.9% (26/28), obvious anxiety symptom prevalence was 78.6% (22/28; Table 8).
| Indicator | Poisoning group (n = 28) | Normal group (n = 222) | 95%CI | Statistical value | P value |
| CES-D score (points) | 29.8 ± 8.4 | 12.8 ± 6.2 | 13.8-20.2 | t = 11.246 | < 0.001 |
| SAS standard score (points) | 56.3 ± 9.1 | 38.2 ± 7.6 | 14.8-21.4 | t = 10.928 | < 0.001 |
| Depressive symptoms detection | 27 (96.4) | 32 (14.4) | χ2 = 76.842 | < 0.001 | |
| Obvious depressive symptoms detection | 25 (89.3) | 18 (8.1) | χ2 = 103.672 | < 0.001 | |
| Anxiety symptoms detection | 26 (92.9) | 28 (12.6) | χ2 = 87.461 | < 0.001 | |
| Obvious anxiety symptoms detection | 22 (78.6) | 15 (6.8) | χ2 = 89.527 | < 0.001 |
Academic stress and life events comparison: ALES total score showed that academic and life stress score in the poi
| ALES dimension | Poisoning group (n = 28) | Normal group (n = 222) | 95%CI | t value | P value |
| Academic stress | 15.9 ± 4.2 | 11.2 ± 3.8 | 3.2-6.2 | 6.184 | < 0.001 |
| Interpersonal relationships | 13.8 ± 3.9 | 9.6 ± 3.2 | 2.8-5.6 | 6.024 | < 0.001 |
| Punishment | 12.1 ± 3.5 | 8.7 ± 2.9 | 2.2-4.6 | 5.428 | < 0.001 |
| Loss | 10.4 ± 3.0 | 7.4 ± 2.8 | 1.9-4.1 | 5.291 | < 0.001 |
| Health adaptation | 11.8 ± 3.4 | 8.2 ± 3.1 | 2.4-4.8 | 5.682 | < 0.001 |
| Others | 12.8 ± 3.8 | 7.2 ± 2.9 | 4.2-7.0 | 8.264 | < 0.001 |
| ALES total score | 76.8 ± 16.4 | 52.3 ± 14.6 | 18.4-30.6 | 8.129 | < 0.001 |
Empathy ability comparison: IRI assessment results showed that the poisoning group scored lower than the normal group in perspective taking dimension (16.8 ± 4.6 points vs 19.6 ± 4.2 points, P = 0.005), and higher in personal distress dimension (19.2 ± 4.8 points vs 13.7 ± 4.6 points, P < 0.001). Fantasy and empathic concern dimensions showed no significant differences between groups (both P > 0.05). Analysis by empathy type showed that the poisoning group scored significantly lower in cognitive empathy (perspective taking + fantasy) than the normal group (35.4 ± 7.2 points vs 38.5 ± 6.9 points, P = 0.043), and significantly higher in emotional empathy (empathic concern + personal distress) than the normal group (36.8 ± 7.9 points vs 33.1 ± 7.2 points, P = 0.021; Table 10).
| IRI dimension | Poisoning group (n = 28) | Normal group (n = 222) | 95%CI | t value | P value |
| Cognitive empathy | |||||
| Perspective taking | 16.8 ± 4.6 | 19.6 ± 4.2 | -4.6 to -1.0 | -3.369 | 0.005 |
| Fantasy | 18.6 ± 4.4 | 18.9 ± 4.3 | -1.9 to 1.3 | -0.362 | 0.718 |
| Cognitive empathy total | 35.4 ± 7.2 | 38.5 ± 6.9 | -6.1 to -0.1 | -2.298 | 0.043 |
| Emotional empathy | |||||
| Empathic concern | 17.6 ± 4.7 | 19.4 ± 4.5 | -3.7 to 0.1 | -2.029 | 0.103 |
| Personal distress | 19.2 ± 4.8 | 13.7 ± 4.6 | 3.7-7.3 | 6.129 | < 0.001 |
| Emotional empathy total | 36.8 ± 7.9 | 33.1 ± 7.2 | 1.6-5.8 | 2.627 | 0.021 |
| IRI total score | 72.2 ± 11.4 | 71.6 ± 10.2 | -4.0 to 5.2 | 0.295 | 0.768 |
Stress coping patterns comparison: CSQ assessment showed that the poisoning group scored significantly lower than the normal group in problem solving dimension (0.52 ± 0.19 vs 0.68 ± 0.22, P = 0.001), while scoring significantly higher in self-blame, fantasy, and withdrawal dimensions. Help-seeking and rationalization dimensions showed no statistically significant differences between groups (both P > 0.05). Analysis by coping style type showed that the poisoning group had significantly lower mature coping (problem solving) scores, significantly higher immature coping (self-blame + fantasy) and negative coping (withdrawal) scores, with no significant difference in mixed coping (help-seeking + rationalization) between groups (Table 11).
| CSQ dimension | Poisoning group (n = 28) | Normal group (n = 222) | 95%CI | t value | P value |
| Mature coping | |||||
| Problem solving1 | 0.52 ± 0.19 | 0.68 ± 0.22 | -0.24 to -0.08 | -3.942 | 0.001 |
| Immature coping | |||||
| Self-blame | 0.61 ± 0.22 | 0.31 ± 0.19 | 0.22-0.38 | 7.584 | < 0.001 |
| Fantasy | 0.58 ± 0.21 | 0.34 ± 0.20 | 0.16-0.32 | 6.124 | < 0.001 |
| Immature coping total | 1.19 ± 0.32 | 0.65 ± 0.28 | 0.43-0.65 | 9.284 | < 0.001 |
| Negative coping | |||||
| Withdrawal | 0.59 ± 0.24 | 0.28 ± 0.17 | 0.23-0.39 | 7.418 | < 0.001 |
| Mixed coping | |||||
| Help-seeking1 | 0.39 ± 0.20 | 0.42 ± 0.18 | -0.10 to 0.04 | -0.812 | 0.418 |
| Rationalization | 0.46 ± 0.18 | 0.48 ± 0.21 | -0.08 to 0.04 | -0.511 | 0.610 |
| Mixed coping total | 0.85 ± 0.27 | 0.90 ± 0.26 | -0.15 to 0.05 | -0.993 | 0.322 |
Variables with P < 0.10 in univariate analysis were included in multivariate logistic regression analysis. Univariate analysis results showed that gender (P < 0.01), age group (P < 0.05), CES-D score (P < 0.001), SAS score (P < 0.001), FSCQ total score (P < 0.001), FACES-II cohesion (P < 0.001), FACES-II adaptability (P < 0.001), parental SCL-90 total score (P < 0.001), father EMBU emotional warmth and understanding (P < 0.001), mother EMBU emotional warmth and understanding (P < 0.001), SSRS total score (P < 0.001), ALES total score (P < 0.001), IRI perspective taking (P = 0.005), CSQ problem solving (P = 0.001), and other 14 variables had P < 0.10, and were included in multivariate analysis.
A multivariate logistic regression model was established using the forward method. Collinearity diagnosis showed all variables had variance inflation factors < 3.0, with no serious multicollinearity detected. The final model showed that female gender (OR = 2.847, 95%CI: 1.024-7.913, P = 0.045), high CES-D scores (OR = 1.124, 95%CI: 1.062-1.190, P < 0.001), low FSCQ total scores (OR = 0.934, 95%CI: 0.891-0.979, P = 0.005), high parental SCL-90 total scores (OR = 1.018, 95%CI: 1.005-1.031, P = 0.006), and low SSRS total scores (OR = 0.895, 95%CI: 0.839-0.955, P = 0.001) were independent influencing factors for adolescent antidepressant poisoning. Model goodness of fit was good (Hosmer-Lemeshow test: χ2 = 7.346, P = 0.500), with area under ROC curve of 0.823 (95%CI: 0.745-0.901), showing good predictive efficacy (Table 12).
| Influencing factor | B value | SE | Wald value | P value | OR value | 95%CI |
| Gender (female) | 1.046 | 0.522 | 4.021 | 0.045 | 2.847 | 1.024-7.913 |
| CES-D score | 0.117 | 0.029 | 16.284 | < 0.001 | 1.124 | 1.062-1.190 |
| FSCQ total score | -0.068 | 0.024 | 7.951 | 0.005 | 0.934 | 0.891-0.979 |
| Parental SCL-90 total score | 0.018 | 0.007 | 7.442 | 0.006 | 1.018 | 1.005-1.031 |
| SSRS total score | -0.111 | 0.033 | 11.285 | 0.001 | 0.895 | 0.839-0.955 |
This study’s results show that the incidence of adolescent antidepressant poisoning in emergency departments was 11.2%, reflecting the severity of current adolescent antidepressant poisoning problems. Compared with international research reports, this study’s results are at a moderate to high level[8]. The rising incidence may be related to multiple factors: First, the continuous increase in adolescent mental health problem incidence in recent years has correspondingly increased antidepressant prescription rates; second, increased convenience for adolescents to obtain medications, including family member medications and online drug purchases; third, increased psychosocial stress factors such as academic pressure and interpersonal relationship problems have increased the risk of drug abuse[9].
From gender distribution, female adolescents accounted for 78.6%, consistent with previous research results[10]. The reasons why female adolescents are more prone to antidepressant poisoning may include: (1) Female adolescents have higher depression prevalence rates themselves, with more opportunities to access antidepressant medications; (2) Females tend to adopt internalized coping methods when facing psychological distress, including self-harm behaviors; and (3) Hormonal level changes have more significant effects on female adolescent emotional regulation[11]. Age distribution showed that the 17-18 years age group had the highest proportion (60.7%), suggesting that high school stage is a high-risk period for antidepressant poisoning, possibly closely related to developmental tasks faced during this stage such as academic pressure, identity crisis, and independence development[12].
Regarding drug types, SSRI class poisoning was most common (60.7%), consistent with the widespread clinical use of SSRI class medications. Although SSRI class medications have relatively high safety, large doses can still produce serious adverse reactions[13]. Notably, 64.3% of patients took doses exceeding 5 times the therapeutic dose, and 82.1% of poisoning events had suicidal intent, indicating that most poisoning events were not accidental but deliberate self-harm behaviors by adolescents, reflecting their serious psychological crisis state[14].
This study found that the poisoning group scored significantly lower than the normal group in all family structure characteristic dimensions, with family integrity and economic status showing the most obvious differences. Family structure instability, such as single-parent families and reconstituted families, may increase the risk of adolescents engaging in dangerous behaviors through various mechanisms[15]. Lack of family integrity is often accompanied by defective guardianship, insufficient emotional support, and role confusion, which may collectively lead to adolescent behavioral problems and emotional distress. Families with poor economic conditions often face more life stress, and parents may neglect psychological care for adolescents due to economic pressure, while economic difficulties themselves are important sources of adolescent psychological stress[16].
Family function assessment results showed that the poisoning group had significantly lower family cohesion and adaptability scores, with larger ideal-actual differences, suggesting these families not only had poor functional levels but also higher dissatisfaction with current conditions among family members. Low family cohesion reflects lack of effective emotional connection and communication among family members, making it difficult for adolescents to obtain sufficient emotional support and sense of belonging in such environments[17]. Poor family adaptability indicates families lack flexible ability to cope with stress and change; when facing difficulties, family systems cannot effectively adjust to maintain members’ mental health. Such functionally defective family environments may prompt adolescents to seek inappropriate coping methods, including drug abuse and other self-harm behaviors[18].
Study results showed that parents in the poisoning group scored significantly higher than the normal group in all SCL-90 symptom dimensions, particularly in depression and anxiety dimensions. The negative impact of parental mental health problems on adolescent psychological development has been widely recognized[19]. Depressed or anxious parents often exhibit emotional instability, inconsistent parenting behaviors, and delayed responses to adolescent needs, directly affecting parent-child relationship quality and family atmosphere. Additionally, parental mental health problems may affect adolescents through both genetic and environmental dual pathways, not only increasing adolescents’ biological susceptibility to mental illness but also increasing environmental risk factors through poor parenting environments[20].
EMBU assessment results showed that parents in the poisoning group scored significantly lower in emotional warmth and understanding dimension, while scoring higher in negative parenting patterns such as punishment and strictness, excessive interference, and rejection and denial. This result is consistent with numerous studies confirming the impact of parenting patterns on adolescent mental health[21]. Lack of emotional warmth in parenting may lead adolescents to form insecure attachment patterns, affecting their self-worth and interpersonal relationship development. Excessively harsh punishment and rejection-denial attitudes may damage adolescents’ self-esteem and increase the risk of internalized problem behaviors. Excessive interference in parenting, while superficially showing parental concern, actually limits adolescent autonomy development and may lead adolescents to seek control through extreme behaviors[22].
The poisoning group scored significantly lower than the normal group in all social support dimensions, suggesting lack of social support is an important risk factor for adolescent antidepressant poisoning. As an important protective factor, social support can promote individual mental health through various mechanisms[23]. Lack of objective support means adolescents lack actual help resources when facing difficulties; insufficient subjective support reflects adolescents’ poor perception of available support, and this cognitive bias may exacerbate feelings of helplessness; decreased utilization of support indicates that even when support resources exist, adolescents lack effective ability or willingness to use these resources. Multiple deficits in social support form vicious cycles, further deteriorating adolescents’ psychological state[24].
Adolescents in the poisoning group scored significantly higher than the normal group in depression and anxiety assessments, with depressive symptom prevalence as high as 96.4% and obvious depressive symptom prevalence of 89.3%. This result indicates that depressive mood is a core risk factor for adolescent antidepressant poisoning. Depressive symptoms may increase drug poisoning risk through multiple pathways: (1) Cognitive distortion leads to decreased coping ability for difficulties, making extreme methods more likely; (2) Emotional regulation difficulties make it hard for adolescents to effectively manage negative emotions when facing stress; and (3) Low self-worth and hopelessness increase the possibility of self-harm behaviors[25]. Anxiety symptoms also play important roles; high anxiety levels may lead to increased impulsivity in adolescents, resulting in dangerous behaviors during emotional excitement.
Study results showed that the poisoning group scored significantly higher than the normal group in all academic stress and life event dimensions, reflecting the important role of stress accumulation effects in adolescent antidepressant poisoning. Academic stress, as one of the main stressors during adolescence, may exceed adolescents’ coping ability range when excessively accumulated. When stress exists long-term without effective relief, it may lead to depletion of adaptive resources, increasing the risk of mental illness and dangerous behaviors[26]. The cumulative effect of life events indicates that simultaneous action of multiple stressors may produce super-additive negative impacts; even if individual event impact levels are limited, multiple event accumulation may produce serious consequences.
The poisoning group was significantly lower than the normal group in cognitive empathy ability, while scoring higher in emotional empathy, particularly in personal distress dimension. This result suggests unbalanced empathy development may be a risk factor. Cognitive empathy deficits may affect adolescents’ understanding and prediction of others’ emotional states, leading to interpersonal difficulties; while excessive personal distress scores indicate adolescents experience excessive personal discomfort when facing others’ pain, and this emotional burden may increase their psychological stress[27].
In coping patterns, the poisoning group showed typical maladaptive patterns: Insufficient mature coping ability, over-reliance on immature coping methods like self-blame and fantasy, while showing obvious avoidance tendencies. These coping pattern deficits prevent adolescents from effectively solving problems when facing stress, potentially exacerbating difficulty severity and persistence.
Multivariate logistic regression analysis identified 5 independent influencing factors: Female gender, depression severity, family structure stability, parental mental health status, and social support level. This result has important theoretical and practical significance. First, it confirms that adolescent antidepressant poisoning results from multiple factors working together, with single factors unable to fully explain occurrence mechanisms. Second, the model’s good predictive efficacy (area under ROC curve = 0.823) provides scientific tools for clinical screening and risk assessment.
Gender as an unchangeable biological factor reminds clinical medical staff to pay special attention to female adolescents. Depression severity as an interventional psychological factor emphasizes the importance of early identification and treatment of depressive symptoms. Family structure stability and parental mental health status as environmental factors suggest the key position of family intervention in prevention strategies. Social support level as a protective factor provides direction for constructing comprehensive prevention systems.
Temporal relationships and bidirectional causality: While our findings demonstrate strong associations between family psychological environment and adolescent antidepressant poisoning, the cross-sectional design precludes definitive establishment of temporal sequence and causal direction. Although it is conceptually logical that pre-existing family dysfunction contributes to adolescent poisoning risk, bidirectional causality remains plausible. Specifically, an adolescent’s acute poisoning event may retrospectively traumatize the family system, leading to deterioration in parental mental health, disruption of family function, and breakdown of previously stable family structures. The acute crisis of a child’s suicide attempt can trigger parental depression and anxiety, strain marital relationships, and fundamentally alter family dynamics. Our data collection included inquiries about the duration of family problems and parental symptoms, which in the majority of cases predated the poisoning event. However, recall bias and the difficulty in precisely dating the onset of family dysfunction limit our ability to definitively establish temporal precedence. This limitation underscores the critical need for prospective longitudinal studies that can track families from baseline through adolescence to establish true temporal sequence and identify critical developmental periods when family interventions may be most effective in preventing adverse outcomes.
This study’s innovation is mainly reflected in: (1) Using multi-dimensional, systematic assessment methods to comprehensively analyze family psychological environment impacts; (2) Establishing multi-factor prediction models with good predictive efficacy; and (3) In-depth exploration of interactions between adolescent individual psychosocial factors and family environmental factors.
However, this study also has certain limitations: First, the study design limits causal inference. Family dysfunction may precede poisoning, but poisoning events can also retrospectively impact family functioning and parental mental health, creating temporal ambiguity. Prospective longitudinal studies are needed to establish temporal precedence and identify critical intervention periods. Second, the small sample size (n = 28 in poisoning group) may affect generalizability and statistical power. Third, exclusive reliance on self-report scales introduces reporting bias. Despite conducting assessments 24-48 hours post-admission, adolescents may distort family perceptions (exaggerating dysfunction or minimizing due to shame), while parents may exhibit guilt-driven bias. Future studies should incorporate multi-informant reports, clinician-rated interviews, observational family interaction assessments, and objective biomarkers. Finally, deeper mechanisms such as gene-environment interactions and neurobiological pathways were not explored.
Based on study results, we recommend establishing multi-level prevention intervention systems: (1) Individual level: Strengthen adolescent mental health screening, early identification and treatment of psychological problems like depression and anxiety, while conducting coping skill training and empathy ability cultivation; (2) Family level: Provide family therapy and parent education services, improve family function and parenting patterns, while paying attention to parental mental health status; (3) Social level: Construct adolescent social support networks, reduce environmental stress factors, create social environments conducive to healthy adolescent growth; and (4) Medical system level: Establish standardized antidepressant medication management systems, strengthen medication safety education, and improve emergency treatment procedures.
In summary, adolescent antidepressant poisoning results from interactions of individual, family, and social multiple factors, requiring comprehensive intervention models using bio-psycho-social approaches. Through multidisciplinary collaboration and systematic prevention measures, we can effectively reduce occurrence rates and protect adolescent physical and mental health.
| 1. | Kieling C, Buchweitz C, Caye A, Silvani J, Ameis SH, Brunoni AR, Cost KT, Courtney DB, Georgiades K, Merikangas KR, Henderson JL, Polanczyk GV, Rohde LA, Salum GA, Szatmari P. Worldwide Prevalence and Disability From Mental Disorders Across Childhood and Adolescence: Evidence From the Global Burden of Disease Study. JAMA Psychiatry. 2024;81:347-356. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 490] [Cited by in RCA: 371] [Article Influence: 185.5] [Reference Citation Analysis (0)] |
| 2. | Chua KP, Volerman A, Zhang J, Hua J, Conti RM. Antidepressant Dispensing to US Adolescents and Young Adults: 2016-2022. Pediatrics. 2024;153:e2023064245. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 45] [Cited by in RCA: 36] [Article Influence: 18.0] [Reference Citation Analysis (0)] |
| 3. | Ramos SF, Araújo-Neto FC, Aires-Moreno GT, de Araújo DCSA, Lima EDC, de Lyra DP Jr. Causality and avoidability of adverse drug reactions of antibiotics in hospitalized children: a cohort study. Int J Clin Pharm. 2021;43:1293-1301. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 6] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 4. | Anderson KN, Johns D, Holland KM, Chen Y, Vivolo-Kantor AM, Trinh E, Bitsko RH, Leeb RT, Radhakrishnan L, Bacon S, Jones CM. Emergency Department Visits Involving Mental Health Conditions, Suicide-Related Behaviors, and Drug Overdoses Among Adolescents - United States, January 2019-February 2023. MMWR Morb Mortal Wkly Rep. 2023;72:502-512. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 38] [Cited by in RCA: 28] [Article Influence: 9.3] [Reference Citation Analysis (0)] |
| 5. | Li M, Wang J, Ma P, Sun W, Gong H, Gao Y. The relationship between harsh parenting and adolescent depression. Sci Rep. 2023;13:20647. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 19] [Cited by in RCA: 12] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
| 6. | Nawi AM, Ismail R, Ibrahim F, Hassan MR, Manaf MRA, Amit N, Ibrahim N, Shafurdin NS. Risk and protective factors of drug abuse among adolescents: a systematic review. BMC Public Health. 2021;21:2088. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 353] [Cited by in RCA: 189] [Article Influence: 37.8] [Reference Citation Analysis (0)] |
| 7. | Shen J, Zhou S, Du M, Xia B, Jiang Y. Cluster analysis of family resilience in adolescents with emotional disorders: a cross-sectional study. BMC Psychiatry. 2025;25:804. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Reference Citation Analysis (0)] |
| 8. | Garnett MF, Miniño AM. Drug Overdose Deaths in the United States, 2003-2023. NCHS Data Brief. 2024;1. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 132] [Cited by in RCA: 129] [Article Influence: 64.5] [Reference Citation Analysis (0)] |
| 9. | Anderson TL, Valiauga R, Tallo C, Hong CB, Manoranjithan S, Domingo C, Paudel M, Untaroiu A, Barr S, Goldhaber K. Contributing Factors to the Rise in Adolescent Anxiety and Associated Mental Health Disorders: A Narrative Review of Current Literature. J Child Adolesc Psychiatr Nurs. 2025;38:e70009. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 43] [Cited by in RCA: 18] [Article Influence: 18.0] [Reference Citation Analysis (0)] |
| 10. | Daly M. Prevalence of Depression Among Adolescents in the U.S. From 2009 to 2019: Analysis of Trends by Sex, Race/Ethnicity, and Income. J Adolesc Health. 2022;70:496-499. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 311] [Cited by in RCA: 240] [Article Influence: 60.0] [Reference Citation Analysis (1)] |
| 11. | Luo D, Dashti SG, Sawyer SM, Vijayakumar N. Pubertal hormones and mental health problems in children and adolescents: a systematic review of population-based studies. EClinicalMedicine. 2024;76:102828. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 35] [Cited by in RCA: 26] [Article Influence: 13.0] [Reference Citation Analysis (0)] |
| 12. | Verlenden JV, Fodeman A, Wilkins N, Jones SE, Moore S, Cornett K, Sims V, Saelee R, Brener ND. Mental Health and Suicide Risk Among High School Students and Protective Factors - Youth Risk Behavior Survey, United States, 2023. MMWR Suppl. 2024;73:79-86. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 64] [Cited by in RCA: 40] [Article Influence: 20.0] [Reference Citation Analysis (0)] |
| 13. | Zhou Y, Lu Y, Wu Y, Kong W, Zhou L, Guo X, Wei H, Wang H, Xie F, Yan S, Yang F, Liu C, Li Q, Li N, Zou Y, Chen J. Safety of antidepressants commonly used in 6-17-year-old children and adolescents: A disproportionality analysis from 2014-2023 on the basis of the FAERS database. PLoS One. 2025;20:e0330025. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 14. | Ruge MJ, Hays HL, Kistamgari S, Rine NI, Zhu M, Ding K, Smith GA. Poison Center Calls About Self-Harm or Suicidal Intent and Other Exposure Reasons in 6- to 12-Year-Old Children. Pediatrics. 2025;156:e2024069753. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Reference Citation Analysis (0)] |
| 15. | Hoffmann JP. Family Structure, Unstructured Socializing, and Heavy Substance Use among Adolescents. Int J Environ Res Public Health. 2022;19:8818. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 7] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 16. | Prime H, Wade M, Browne DT. Risk and resilience in family well-being during the COVID-19 pandemic. Am Psychol. 2020;75:631-643. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1674] [Cited by in RCA: 970] [Article Influence: 161.7] [Reference Citation Analysis (0)] |
| 17. | van Eickels RL, Tsarpalis-Fragkoulidis A, Zemp M. Family cohesion, shame-proneness, expressive suppression, and adolescent mental health-A path model approach. Front Psychol. 2022;13:921250. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 37] [Cited by in RCA: 19] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 18. | Gao Y, Wang Y, Wang Z, Ma M, Li H, Wang J, Liu J, Qian H, Zhu P, Xu X. Family intimacy and adaptability and non-suicidal self-injury: a mediation analysis. BMC Psychiatry. 2024;24:210. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 18] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 19. | Mace K, Sifaki M, Midouhas E, Flouri E, Papachristou E. The Course of Parental Psychological Distress in Childhood and Adolescent Depression. JAACAP Open. 2025;3:634-644. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Reference Citation Analysis (0)] |
| 20. | Zhou S, Kwan CK, Ai Y, Ma Y. Parent-adolescent intergenerational transmission of distress: the roles of family climate, adolescents' self-compassion and mindfulness. Front Psychol. 2025;16:1595515. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 21. | Wang L, Tian J, Rozelle S. Parenting style and child mental health at preschool age: evidence from rural China. BMC Psychiatry. 2024;24:314. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 24] [Cited by in RCA: 10] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 22. | Shah EN, Szwedo DE, Allen JP. Parental Autonomy Restricting Behaviors During Adolescence as Predictors of Dependency on Parents in Emerging Adulthood. Emerg Adulthood. 2023;11:15-31. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 24] [Cited by in RCA: 12] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 23. | Cherewick M, Lama R, Rai RP, Dukpa C, Mukhia D, Giri P, Matergia M. Social support and self-efficacy during early adolescence: Dual impact of protective and promotive links to mental health and wellbeing. PLOS Glob Public Health. 2024;4:e0003904. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 4] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 24. | Bauer A, Stevens M, Purtscheller D, Knapp M, Fonagy P, Evans-Lacko S, Paul J. Mobilising social support to improve mental health for children and adolescents: A systematic review using principles of realist synthesis. PLoS One. 2021;16:e0251750. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 83] [Cited by in RCA: 44] [Article Influence: 8.8] [Reference Citation Analysis (0)] |
| 25. | Mittermeier S, Seidel A, Scheiner C, Kleindienst N, Romanos M, Buerger A. Emotional dysregulation and its pathways to suicidality in a community-based sample of adolescents. Child Adolesc Psychiatry Ment Health. 2024;18:15. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 11] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 26. | Deng Y, Cherian J, Khan NUN, Kumari K, Sial MS, Comite U, Gavurova B, Popp J. Family and Academic Stress and Their Impact on Students' Depression Level and Academic Performance. Front Psychiatry. 2022;13:869337. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 240] [Cited by in RCA: 93] [Article Influence: 23.3] [Reference Citation Analysis (0)] |
| 27. | Gaspar A, Esteves F. Empathy development from adolescence to adulthood and its consistency across targets. Front Psychol. 2022;13:936053. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 6] [Article Influence: 1.5] [Reference Citation Analysis (0)] |