Published online Apr 19, 2026. doi: 10.5498/wjp.v16.i4.114419
Revised: November 20, 2025
Accepted: January 5, 2026
Published online: April 19, 2026
Processing time: 157 Days and 2.1 Hours
Survivors of acute respiratory distress syndrome (ARDS) frequently suffer from long-term physical and psychological sequelae, including impaired lung function and posttraumatic stress disorder (PTSD), highlighting the need for comprehensive rehabilitation strategies.
To evaluate the impact of staged pulmonary rehabilitation nursing combined with cognitive psychological intervention (SPRNCPI) on PTSD in patients with ARDS.
A retrospective analysis was conducted on the data of 230 patients with ARDS admitted from April 2020 to April 2024. The patients were divided into two groups: A routine care (RC) group (n = 125) and a SPRNCPI group (n = 105). The SPRNCPI group received mechanical ventilation support, RC, and additional staged pulmonary rehabilitation nursing combines with cognitive psychological interventions including psychological support, emotional management training, and regular follow-ups. Baseline demographic information, respiratory function parameters, oxygenation index, serum cortisol levels, PTSD symptoms, emotional status, and quality of life were assessed.
After nursing, forced expiratory volume in one second (P < 0.001), forced vital capacity (P = 0.009), and PaO2/FiO2 (P = 0.005) were significantly higher in the SPRNCPI group than in the RC group. Serum cortisol levels (P = 0.002), Impact of Event Scale-Revised overall score (P < 0.001), Self-Rating Anxiety Scale (P = 0.002), and Self-Rating Depression Scale (P < 0.001) scores were significantly lower in the SPRNCPI group. Physiological field scores (P = 0.033), psychological field scores (P = 0.015), social field scores (P = 0.043), and environmental field scores (P = 0.010) were significantly higher in the SPRNCPI group.
SPRNCPI significantly improves respiratory function, reduced PTSD symptoms, lowered anxiety and depression levels, and enhanced overall quality of life in patients with ARDS. This integrated approach offers a promising strategy for enhancing patient outcomes in critical care settings.
Core Tip: This study demonstrates that a novel, integrated protocol combining staged pulmonary rehabilitation nursing with cognitive psychological intervention offers a holistic approach for survivors of acute respiratory distress syndrome. Unlike routine care, this combined strategy significantly improved not only respiratory function and oxygenation but also mitigated psychological trauma, effectively reducing symptoms of posttraumatic stress disorder, anxiety, and depression. This underscores the critical need to address both physical and mental health in acute respiratory distress syndrome recovery to enhance overall patient outcomes.
- Citation: Liu X, Zhao J, Wang YX, Pei YJ, Shi XP, Peng SW. Effect of combined pulmonary-psychological nursing on posttraumatic stress disorder in patients with acute respiratory distress syndrome. World J Psychiatry 2026; 16(4): 114419
- URL: https://www.wjgnet.com/2220-3206/full/v16/i4/114419.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i4.114419
Acute respiratory distress syndrome (ARDS) is a life-threatening condition characterized by the acute onset of hypoxemia and bilateral pulmonary infiltrates. Despite advancements in critical care medicine, ARDS remains a challenging condition with high rates of complications and prolonged hospital stay[1]. Patients suffering from ARDS often experience severe physical and psychological distress, including posttraumatic stress disorder (PTSD), which can persist long after the acute phase of illness has resolved[2]. The prevalence of PTSD among ARDS survivors is estimated to be as high as 23.9%, underscoring the need for comprehensive interventions that address physical recovery and mental health[3].
The pathophysiology of ARDS involves complex interactions between inflammatory mediators, endothelial dysfunc
Pulmonary rehabilitation has emerged as a promising adjunctive therapy for various respiratory conditions, including chronic obstructive pulmonary disease (COPD) and interstitial lung disease[7]. This multidisciplinary approach aims to improve physical function, reduce symptoms, and enhance overall quality of life[8]. However, its application in ARDS is poorly established. Staged pulmonary rehabilitation, tailored to the different phases of ARDS - from the acute phase through recovery - offers a potential pathway to optimize patient outcomes. By incorporating targeted exercises, brea
Despite the recognized benefits of pulmonary rehabilitation and cognitive psychological interventions, their integra
This study retrospectively analyzed the medical records of 230 patients with ARDS admitted to Henan Provincial People’s Hospital from April 2020 to April 2024. Collect demographic information of patients through the case system. All executed procedures comply with the ethical standards of the responsible committees for human experiments (institutions and countries) and the 1964 Declaration of Helsinki and subsequent versions. This study was approved by the Institutional Review Board of Henan Provincial People’s Hospital. Informed consent was waived by the Institutional Review Board and Ethics Committee of Henan Provincial People’s Hospital for this retrospective study because of the exclusive use of de-identified patient data, which posed no potential harm or impact on patient care.
The inclusion criteria were as follows: (1) Patients over 18 years old; (2) Clinically diagnosed with ARDS[12]; (3) They have received mechanical ventilation greater than 12 hours or noninvasive ventilation greater than 4 hours; and (4) They have complete medical records. The exclusion criteria were as follows: (1) Combined with severe cognitive impairment, unable to cooperate with rehabilitation training and nursing evaluation; (2) Seriou’s chest deformities, spinal deformities, and other diseases that affect respiratory movement; (3) History of chest surgery or trauma within 3 months; (4) Com
A total of 261 patients with ARDS were initially identified during the study period. After the inclusion and exclusion criteria were applied, 31 patients were excluded: 5 for severe cognitive impairment, 12 for preexisting spinal or chest deformities, 8 with a recent history of chest surgery or trauma, and 6 with advanced malignancies. Finally, 230 patients were enrolled in this study.
Grouping criteria: According to the type of care received, the patients were divided into two groups: The routine care (RC) group and the staged pulmonary rehabilitation nursing combined with cognitive psychological intervention (SPRNCPI) group. A total of 125 patients with ARDS who only received routine medical care and standard treatment were included in the RC group, and 105 patients who received SPRNCPI in addition to RC were included in the SPRNCPI group. The disparity in group sizes arose from the retrospective assignment based on the standard care protocols available at different phases of the study period and patient eligibility for the combined intervention, rather than from randomized allocation.
Nursing methods: The patients were first rapidly initiated on mechanical ventilation support: Once ARDS was diag
RC: The patients were assisted in turning over and performing back tapping every 2 hours to promote sputum clearance and prevent atelectasis pneumonia; the oxygen flow rate was adjusted reasonably according to the patient’s condition and medical orders to ensure adequate oxygen supply; the patient’s vital signs, respiratory rate, rhythm, and depth were closely monitored, and abnormalities were promptly identified and reported to the doctor; nebulization inhalation therapy was performed on patients 2-3 times a day as per medical orders.
SPRNCPI: The SPRNCPI included the following: (1) First stage (acute phase, within 48 hours of mechanical ventilation); (2) Second stage (relief phase, from 48 hours of mechanical ventilation up to before weaning); and (3) Third stage (rehabilitation phase, from after weaning until discharge). The cognitive psychological interventions, which were integrated throughout these stages, included the following: (1) Psychological support: Providing counseling services to patients and their families to help them cope with the anxiety and fear brought about by the illness; (2) Emotional management training: Teaching patients’ emotional regulation skills under the guidance of professional psychological consultants to reduce the risk of developing PTSD; and (3) regular follow-ups: Continuously tracking the patient’s recovery status after discharge and providing further psychological support and rehabilitation training when necessary.
Baseline data collection: For all enrolled patients, baseline demographic information, including severity grading, causes, and length of hospital stay, was collected from the medical record system.
Respiratory function parameters: Forced vital capacity (FVC) and forced expiratory volume in one second (FEV1) were recorded before nursing care and 1 week after nursing care, and the FEV1/FVC ratio was then calculated. FVC was measured using a spirometer (V508368, Jiangsu Yuanyan Medical Equipment Co., Ltd., China) to record the patient’s thoracic gas volume. FEV1 was measured using a pulmonary function testing device (AS-407, MINATO Medical Science, Japan).
Optimal PEEP: Before and 1 week after nursing care, the “PEEP incremental-decremental method” was used to determine the optimal PEEP. PEEP was incrementally increased from 5 cm H2O with a gradient of 2 cm H2O per step (not exceeding 20 cm H2O). Each adjustment was maintained for 30 minutes of ventilation until respiratory mechanics stabilized, followed by the measurement of arterial blood gases (PaO2 and PaCO2), oxygenation index (PaO2/FiO2), plateau pressure, and static lung compliance [Cstat, calculated as: Cstat = tidal volume/(plateau pressure-PEEP)]. If plateau pressure exceeded 30 cm H2O or if circulatory indicators (heart rate, mean arterial pressure) fluctuated more than 15% from baseline values, then the increase was stopped and the decrement phase began. Starting from the highest safe PEEP value, the value was decreased in the same gradient down to 5 cm H2O, with each gradient also maintained for 30 minutes and the parameters recorded accordingly. The optimal PEEP was determined based on the principle of “optimal oxygenation and minimal risk of lung injury”. Preference was given to the PEEP value where PaO2/FiO2 was maximized (≥ 200 mmHg, or ≥ 150 mmHg if FiO2 ≤ 0.6) and SpO2 ≥ 92% while also meeting plateau pressure ≤ 30 cm H2O, Cstat ≥ 30 mL/cm H2O, and stable circulation (heart rate, mean arterial pressure fluctuation < 15%, no signs of inadequate tissue perfusion).
Oxygenation index: Before and 1 week after nursing care, the oxygenation index was calculated using the relevant lung ventilation parameters displayed on the ventilator as = PaO2/FiO2, where PaO2 is the arterial oxygen partial pressure, and FiO2 is the fraction of inspired oxygen. A high oxygenation index indicates a good respiratory status.
Serum cortisol: Before nursing care and 1 week after nursing care at 8:00, 6 mL of fasting venous blood was collected from the patient into a tube without anticoagulant and kept completely still until serum separation. Centrifugation was performed to separate the serum by spinning at 4000 rpm for 10 minutes at 4 °C. The supernatant was carefully with
PTSD symptoms: The Impact of Event Scale-Revised (IES-R) questionnaire was used to measure PTSD symptoms before and 1 week after care. The IES-R encompasses three dimensions: Overall intrusion, overall avoidance, and overall hype
Emotion and hope level evaluation: The patient’s mood and hope level were evaluated before and after patient care using the Self-Rating Scale for Depression (SDS), Self-Rating Anxiety Scale (SAS), and Herth Hope Scale. SDS and SAS both contain 20 questions and are rated on a 4-point scale, with low scores indicating weak depression and anxiety. The Herth Hope Scale consists of 12 questions, with scores of 12-23 being low, 24-35 being moderate, and 36-48 being high; high scores indicate a high level of hope. The Cronbach’s alpha values for SDS and SAS are 0.92 and 0.81, respectively[14,15]. The Cronbach’s alpha for the Herth Hope Scale is 0.88[16].
Survival quality evaluation: The World Health Organization Quality of Life-BREF Scale was used to assess the quality of life before and after patient care. This scale consists of 26 questions, each rated on a 5-point Likert scale (1-5 points), and is divided into four domains: Physical, psychological, social relationships, and environment. The raw scores for the items within each domain are summed and then converted to a standardized score using the formula: Standardized score = [(raw score - minimum possible score)/(maximum possible score - minimum possible score)] × 100, resulting in a score range of 0-100. High scores indicate good quality of life in that domain. The Cronbach’s alpha for the World Health Organization Quality of Life-BREF Scale is 0.90[17].
The χ2 test or Fisher exact probability method was used for the comparison of classified variables between two groups. t-test or Mann-Whitney U test was used for the analysis of differences in the numerical variables between two groups. SPSS version 20.0 and GraphPad Prism version 5 statistical software were used for data analysis. All P values were bilaterally distributed, and P < 0.05 indicated that the difference was statistically significant.
In the comparison of general information between the RC (n = 125) and SPRNCPI (n = 105) groups, no significant differences were observed in age (P = 0.064), gender distribution (P = 0.508), body mass index (P = 0.090), education level (P = 0.534), combined diabetes (P = 0.785), combined hypertension (P = 0.247), combined hyperlipidemia (P = 0.347), smoking status (P = 0.611), or drinking status (P = 0.825; Table 1). These results indicate that the two groups were compa
| Parameters | RC group (n = 125) | SPRNCPI group (n = 105) | t/χ2 | P value |
| Age (years) | 56.74 ± 5.65 | 58.86 ± 10.44 | 1.868 | 0.064 |
| Gender | 0.439 | 0.508 | ||
| Male | 72 (57.60) | 65 (61.90) | ||
| Female | 53 (42.40) | 40 (38.10) | ||
| BMI (kg/m2) | 23.02 ± 3.00 | 23.73 ± 3.30 | 1.704 | 0.090 |
| Education level (years) | 1.255 | 0.534 | ||
| Primary or below | 37 (29.60) | 30 (28.57) | ||
| Secondary school | 44 (35.20) | 44 (41.90) | ||
| College or above | 44 (35.20) | 31 (29.52) | ||
| Combined diabetes | 17 (13.60) | 13 (12.38) | 0.075 | 0.785 |
| Combined hypertension | 21 (16.80) | 12 (11.43) | 1.340 | 0.247 |
| Combined hyperlipidemia | 25 (20.00) | 16 (15.24) | 0.883 | 0.347 |
| Smoking | 0.985 | 0.611 | ||
| Never | 30 (24.00) | 20 (19.05) | ||
| Former | 19 (15.20) | 15 (14.28) | ||
| Current | 76 (60.80) | 70 (66.67) | ||
| Drinking | 0.384 | 0.825 | ||
| Never | 27 (21.60) | 22 (20.95) | ||
| Former | 20 (16.00) | 14 (13.33) | ||
| Current | 78 (62.40) | 69 (65.72) |
In the comparison of clinical characteristics between the RC and SPRNCPI groups, no significant differences were observed in lung injury score (P = 0.089), severity grading (P = 0.506), causes of illness (P = 0.813), Acute Physiology and Chronic Health Evaluation II score (P = 0.153), Sequential Organ Failure Assessment score (P = 0.766), length of hospital stay (P = 0.661), length of ICU stay (P = 0.712), ventilation duration (P = 0.634), or duration of respiratory failure (P = 0.220; Table 2). These results indicate that the two groups were comparable in terms of clinical characteristics.
| Parameters | RC group (n = 125) | SPRNCPI group (n = 105) | t/χ2 | P value |
| Lung injury score | 2.65 ± 0.35 | 2.74 ± 0.44 | 1.708 | 0.089 |
| Severity grading | 0.442 | 0.506 | ||
| Moderate | 93 (74.40) | 74 (70.48) | ||
| Severe | 32 (25.60) | 31 (29.52) | ||
| Causes | 0.952 | 0.813 | ||
| Trauma | 30 (24.00) | 31 (29.52) | ||
| Sepsis | 39 (31.20) | 31 (29.52) | ||
| Pneumonia | 44 (35.20) | 33 (31.43) | ||
| Other or unknown | 12 (9.60) | 10 (9.52) | ||
| APACHE II score | 14.47 ± 2.35 | 14.12 ± 1.26 | 1.434 | 0.153 |
| SOFA score | 7.25 ± 1.58 | 7.19 ± 1.63 | 0.298 | 0.766 |
| Length of hospital stay (days) | 28.53 ± 5.77 | 28.28 ± 2.72 | 0.440 | 0.661 |
| Length of ICU stay (days) | 15.02 ± 1.06 | 14.97 ± 1.08 | 0.370 | 0.712 |
| Ventilation duration (days) | 9.53 ± 2.68 | 9.39 ± 1.71 | 0.477 | 0.634 |
| Duration of respiratory failure (days) | 8.93 ± 1.12 | 9.11 ± 1.16 | 1.230 | 0.220 |
In the comparison of lung function between the RC and SPRNCPI groups, no significant differences were observed in FEV1 before nursing (P = 0.792), FVC before nursing (P = 0.481), or FEV1/FVC ratio before nursing (P = 0.919; Table 3). After nursing, FEV1 (2.02 ± 0.16 vs 1.92 ± 0.25, t = 3.620, P < 0.001) and FVC (2.41 ± 0.31 vs 2.32 ± 0.25, t = 2.641, P = 0.009) were significantly higher in the SPRNCPI group. Although the FEV1/FVC ratio showed a trend toward improvement in the SPRNCPI group, the difference did not reach statistical significance (P = 0.063).
| Parameters | RC group (n = 125) | SPRNCPI group (n = 105) | t | P value |
| FEV1 (L) | ||||
| Before nursing | 1.32 ± 0.24 | 1.33 ± 0.21 | 0.264 | 0.792 |
| After nursing | 1.92 ± 0.25 | 2.02 ± 0.16 | 3.620 | < 0.001 |
| FVC (L) | ||||
| Before nursing | 1.97 ± 0.22 | 1.99 ± 0.19 | 0.706 | 0.481 |
| After nursing | 2.32 ± 0.25 | 2.41 ± 0.31 | 2.641 | 0.009 |
| FEV1/FVC (%) | ||||
| Before nursing | 66.14 ± 5.62 | 66.21 ± 5.49 | 0.102 | 0.919 |
| After nursing | 82.61 ± 4.91 | 83.84 ± 5.04 | 1.867 | 0.063 |
In the comparison of blood gas parameters between the RC and SPRNCPI groups, no significant differences were observed in optimal PEEP before nursing (P = 0.748), FiO2 before nursing (P = 0.066), and PaO2/FiO2 before nursing (P = 0.232; Table 4). After nursing, significant differences were noted: Optimal PEEP (8.93 ± 1.02 vs 9.26 ± 1.14, t = 2.265, P = 0.024) and FiO2 (0.45 ± 0.05 vs 0.47 ± 0.06, t = 2.509, P = 0.013) were significantly lower in the SPRNCPI group, whereas PaO2/FiO2 was significantly higher in the SPRNCPI group (285.43 ± 24.76 vs 276.67 ± 22.15, t = 2.830, P = 0.005).
| Parameters | RC group (n = 125) | SPRNCPI group (n = 105) | t | P value |
| Optimal PEEP (cm H2O) | ||||
| Before nursing | 10.25 ± 1.35 | 10.31 ± 1.27 | 0.322 | 0.748 |
| After nursing | 9.26 ± 1.14 | 8.93 ± 1.02 | 2.265 | 0.024 |
| FiO2 | ||||
| Before nursing | 0.65 ± 0.08 | 0.64 ± 0.07 | 1.847 | 0.066 |
| After nursing | 0.47 ± 0.06 | 0.45 ± 0.05 | 2.509 | 0.013 |
| PaO2/FiO2 (mmHg) | ||||
| Before nursing | 152.36 ± 18.74 | 155.28 ± 17.92 | 1.199 | 0.232 |
| After nursing | 276.67 ± 22.15 | 285.43 ± 24.76 | 2.830 | 0.005 |
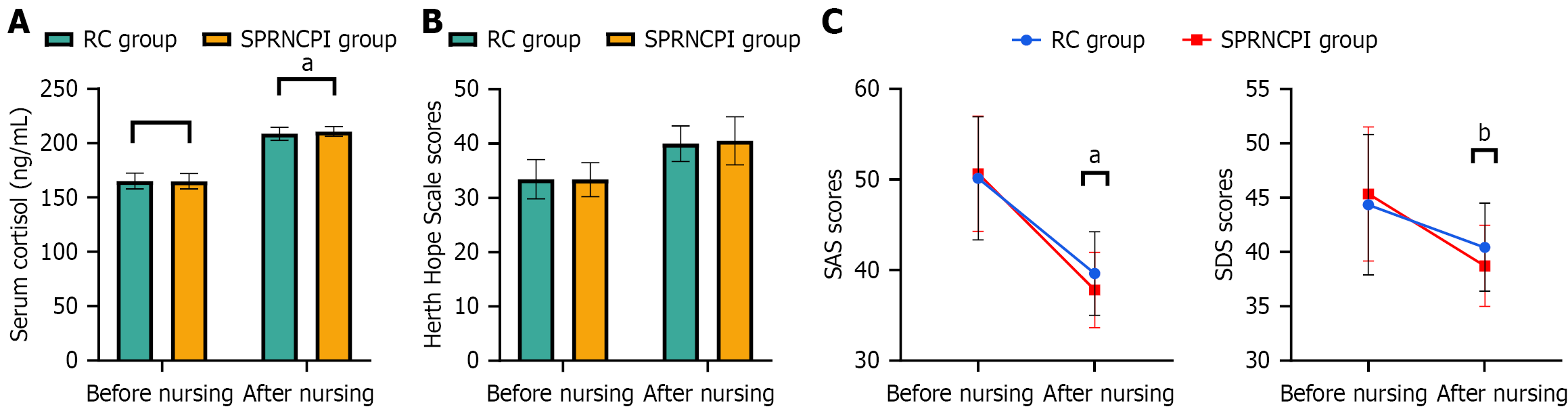
In the comparison of serum cortisol levels between the RC and SPRNCPI groups, no significant differences were observed before nursing (P = 0.4809; Figure 1A). After nursing, serum cortisol levels were significantly lower in the SPRNCPI group (20.65 ± 1.04 vs 21.26 ± 1.91, t = 3.064, P < 0.01).
In the comparison of IES-R scores between the RC and SPRNCPI groups, no significant differences were observed in overall intrusion before nursing (P = 0.774), overall avoidance before nursing (P = 0.901), overall hyperarousal before nursing (P = 0.698), or IES-R overall score before nursing (P = 0.828; Table 5). After nursing, overall intrusion (5.91 ± 1.42 vs 6.63 ± 2.32, t = 2.896, P = 0.004) and overall avoidance (6.84 ± 0.27 vs 7.15 ± 1.02, t = 3.259, P = 0.001) were significantly lower in the SPRNCPI group. Overall hyperarousal showed a more pronounced decrease in the SPRNCPI group (4.52 ± 0.75 vs 5.14 ± 1.85, t = 4.545, P < 0.001). The IES-R overall score after nursing was significantly lower in the SPRNCPI group (17.27 ± 1.41 vs 18.92 ± 1.91, t = 7.502, P < 0.001).
| Parameters | RC group (n = 125) | SPRNCPI group (n = 105) | t | P value |
| Overall intrusion (score) | ||||
| Before nursing | 8.43 ± 1.68 | 8.37 ± 1.71 | 0.287 | 0.774 |
| After nursing | 6.63 ± 2.32 | 5.91 ± 1.42 | 2.896 | 0.004 |
| Overall avoidance (score) | ||||
| Before nursing | 9.45 ± 2.73 | 9.42 ± 0.76 | 0.125 | 0.901 |
| After nursing | 7.15 ± 1.02 | 6.84 ± 0.27 | 3.259 | 0.001 |
| Overall hyperarousal (score) | ||||
| Before nursing | 6.73 ± 2.23 | 6.66 ± 0.17 | 0.389 | 0.698 |
| After nursing | 5.14 ± 1.85 | 4.52 ± 0.75 | 4.545 | < 0.001 |
| IES-R overall (score) | ||||
| Before nursing | 24.61 ± 5.63 | 24.45 ± 5.53 | 0.217 | 0.828 |
| After nursing | 18.92 ± 1.91 | 17.27 ± 1.41 | 7.502 | < 0.001 |
In the comparison of Herth Hope Scale scores between the RC and SPRNCPI groups, no significant differences were observed before nursing (P = 0.868) or after nursing (P = 0.295; Figure 1B). In the comparison of SAS and SDS scores between the RC and SPRNCPI groups, no significant differences were observed in SAS (P = 0.558) or SDS (P = 0.241) scores before nursing (Figure 1C). After nursing, SAS and SDS scores were significantly lower in the SPRNCPI group (37.79 ± 4.14 vs 39.62 ± 4.62, t = 3.147, P = 0.002; 38.71 ± 3.73 vs 40.43 ± 4.05, t = 3.336, P < 0.001).
In the comparison of quality of survival scores between the RC and SPRNCPI groups, no significant differences were observed in physiological field scores, psychological field scores, social field scores, and environmental field scores (all P > 0.05; Table 6). After nursing, physiological field scores (P = 0.033), psychological field scores (P = 0.015), social field scores (P = 0.043), and environmental field scores (P = 0.010) were significantly higher in the SPRNCPI group.
| Parameters | RC group (n = 125) | SPRNCPI group (n = 105) | t | P value |
| Physiological field (score) | ||||
| Before nursing | 42.36 ± 8.25 | 42.15 ± 8.17 | 0.193 | 0.847 |
| After nursing | 63.24 ± 9.32 | 65.83 ± 8.91 | 2.145 | 0.033 |
| Psychological field (score) | ||||
| Before nursing | 39.82 ± 7.64 | 40.05 ± 7.58 | 0.228 | 0.820 |
| After nursing | 66.26 ± 8.45 | 68.92 ± 7.83 | 2.455 | 0.015 |
| Social field (score) | ||||
| Before nursing | 45.23 ± 8.91 | 45.17 ± 8.87 | 0.044 | 0.965 |
| After nursing | 69.95 ± 9.24 | 72.36 ± 8.65 | 2.032 | 0.043 |
| Environmental field (score) | ||||
| Before nursing | 48.75 ± 9.13 | 48.82 ± 9.05 | 0.058 | 0.954 |
| After nursing | 72.14 ± 9.57 | 75.28 ± 8.74 | 2.583 | 0.010 |
This study aimed to evaluate the impact of SPRNCPI on patients with ARDS. Results indicate that this integrated approach led to improvements in several key areas, including lung function, oxygenation index, serum cortisol levels, PTSD symptoms, anxiety, depression, and quality of life. Post nursing assessments revealed that FEV1 and FVC were higher in the SPRNCPI group than in the RC group. This finding suggests that the combination of staged pulmonary rehabilitation and cognitive psychological interventions may enhance lung function recovery in patients with ARDS. Pulmonary rehabilitation typically involves targeted exercises, breathing techniques, and education, which can improve muscle strength and endurance, thereby enhancing overall respiratory function[18,19]. Cognitive psychological inter
After nursing, the SPRNCPI group demonstrated better oxygenation index, lower FiO2, and lower levels of optimal PEEP than the RC group. These changes suggest that SPRCPCI can reduce the demand for the “respiratory support intensity” of mechanical ventilation in patients while improving gas exchange efficiency, reducing their dependence on high-concentration oxygen, and lowering the risk of lung injury (such as barotrauma and volutrauma) potentially caused by prolonged high PEEP and the likelihood of complications such as oxygen toxicity and pulmonary fibrosis due to high-concentration oxygen inhalation. This approach aligns closely with the core principles of “protective lung ventilation strategies” in ARDS treatment. From a mechanistic perspective, the staged pulmonary rehabilitation has likely contri
Serum cortisol levels were reduced in the SPRNCPI group after nursing. Cortisol is a biomarker of stress, and its decrease in this context could indicate a weakened stress response[26]. This finding indicates that the integrated inter
After nursing, overall intrusion, avoidance, hyperarousal, and IES-R scores were lower in the SPRNCPI group than in the RC group. This finding indicates that the integrated approach effectively reduced PTSD symptoms in ARDS survivors. Cognitive psychological interventions, including psychological support and emotional management training, may have directly mitigated the psychological burden by providing structured coping strategies and reducing stress levels. These interventions can help patients process traumatic experiences and develop resilience, thereby decreasing intrusive thoughts and avoidance behaviors[29,30]. Our findings suggest that the integrated approach of staged pul
After nursing, anxiety and depression scores were lower in the SPRNCPI group than in the RC group, indicating that the integrated approach also has positive effects on mental health. Psychological distress is a significant issue among patients with ARDS, often persisting long after hospital discharge. The reduction in anxiety and depression scores suggests that the staged pulmonary rehabilitation and cognitive psychological interventions improve physical function and provides substantial psychological benefits. The inclusion of regular follow-ups and emotional management training might have played a critical role in achieving these improvements[31,32]. While the intervention significantly reduced anxiety and depression scores, no significant improvement was observed in the Herth Hope Scale. A possible explanation is that hope is a stable and multidimensional construct, influenced by factors beyond the scope of our short-term psychological intervention, such as personal resilience, social support, and long-term outlook. As directly responsive to emotional regulation and coping strategies, anxiety and depression may have been immediately alleviated by the cognitive psychological components.
After nursing, physiological, psychological, social, and environmental field scores were higher in the SPRNCPI group than in the RC group. This finding indicates that the integrated approach positively impacts multiple dimensions of quality of life. Comprehensive rehabilitation programs that address physical and psychological needs are essential for improving long-term outcomes in patients with ARDS[30]. Our findings suggest that the combined approach of staged pulmonary rehabilitation and cognitive psychological interventions can provide a holistic framework for improving the overall quality of life of ARDS survivors.
Despite the promising results, this study has several limitations. The nonrandomized, retrospective design is a principal limitation. Group allocation was determined by the care modality received, which may have introduced selection bias and confounded the observed outcomes. Although baseline characteristics were comparable between the groups, unmeasured factors could have influenced the assignment to the intervention group and the prognosis. The retrospective design limits the ability to establish causality between the intervention and the observed outcomes. Prospective randomized controlled trials are needed to validate these findings. The study population was relatively homogeneous, potentially limiting the generalizability of the results to other populations. Future research should aim to include diverse patient groups to assess the broad applicability of the integrated approach. Psychological outcomes such as PTSD, anxiety, and depression were assessed only 1 week after the intervention. Given that PTSD often develops or persists over a longer period, the absence of long-term follow-up (e.g., at 3 months, 6 months, or 12 months) limits the ability to fully capture the trajectory of psychological recovery. Future studies should include extended follow-ups to further evaluate the sustainability of the intervention effects.
The integration of SPRNCPI demonstrated substantial benefits for patients with ARDS. This approach improved lung function, oxygenation, serum cortisol levels, PTSD symptoms, anxiety, depression, and overall quality of life. By add
| 1. | Yang P, Sjoding MW. Acute Respiratory Distress Syndrome: Definition, Diagnosis, and Routine Management. Crit Care Clin. 2024;40:309-327. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 10] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 2. | Kentish-Barnes N, Resche-Rigon M, Lafarge A, Souppart V, Renet A, Pochard F, Azoulay E. PTSD Symptoms Among Family Members of Patients With ARDS Caused by COVID-19 After 12 Months. JAMA. 2023;330:1383-1385. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 3. | Miori S, Sanna A, Lassola S, Cicolini E, Zanella R, Magnoni S, De Rosa S, Bellani G, Umbrello M. Incidence, Risk Factors, and Consequences of Post-Traumatic Stress Disorder Symptoms in Survivors of COVID-19-Related ARDS. Int J Environ Res Public Health. 2023;20:5504. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 4] [Article Influence: 1.3] [Reference Citation Analysis (1)] |
| 4. | Wick KD, Ware LB, Matthay MA. Acute respiratory distress syndrome. BMJ. 2024;387:e076612. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 90] [Cited by in RCA: 76] [Article Influence: 38.0] [Reference Citation Analysis (1)] |
| 5. | Cave C, Samano D, Sharma AM, Dickinson J, Salomon J, Mahapatra S. Acute respiratory distress syndrome: A review of ARDS across the life course. J Investig Med. 2024;72:798-818. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 11] [Article Influence: 5.5] [Reference Citation Analysis (1)] |
| 6. | Chommeloux J, Valentin S, Winiszewski H, Adda M, Pineton de Chambrun M, Moyon Q, Mathian A, Capellier G, Guervilly C, Levy B, Jaquet P, Sonneville R, Voiriot G, Demoule A, Boussouar S, Painvin B, Lebreton G, Combes A, Schmidt M. One-Year Mental and Physical Health Assessment in Survivors after Extracorporeal Membrane Oxygenation for COVID-19-related Acute Respiratory Distress Syndrome. Am J Respir Crit Care Med. 2023;207:150-159. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 37] [Article Influence: 12.3] [Reference Citation Analysis (1)] |
| 7. | He W, Wang J, Feng Z, Li J, Xie Y. Effects of exercise-based pulmonary rehabilitation on severe/very severe COPD: a systematic review and meta-analysis. Ther Adv Respir Dis. 2023;17:17534666231162250. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 35] [Cited by in RCA: 31] [Article Influence: 10.3] [Reference Citation Analysis (0)] |
| 8. | Troosters T, Janssens W, Demeyer H, Rabinovich RA. Pulmonary rehabilitation and physical interventions. Eur Respir Rev. 2023;32:220222. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 110] [Cited by in RCA: 88] [Article Influence: 29.3] [Reference Citation Analysis (1)] |
| 9. | Da L, Zhang K. Early pulmonary rehabilitation in ARDS patients: Effects on respiratory function and long-term outcomes: A retrospective study. Medicine (Baltimore). 2024;103:e41023. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 10. | Dinse H, Skoda EM, Schweda A, Jansen C, Schmidt K, Konik M, Rohn H, Witzke O, Stettner M, Kleinschnitz C, Bäuerle A, Teufel M. Respiratory biofeedback and psycho-education for patients with post COVID- 19 symptoms and bodily distress: study protocol of the randomized, controlled explorative intervention trial POSITIV. Trials. 2025;26:140. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 11. | Cheng SWM, McKeough ZJ, McNamara RJ, Alison JA. Pulmonary Rehabilitation Using Minimal Equipment for People With Chronic Obstructive Pulmonary Disease: A Systematic Review and Meta-Analysis. Phys Ther. 2023;103:pzad013. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 16] [Article Influence: 5.3] [Reference Citation Analysis (1)] |
| 12. | Gorman EA, O'Kane CM, McAuley DF. Acute respiratory distress syndrome in adults: diagnosis, outcomes, long-term sequelae, and management. Lancet. 2022;400:1157-1170. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 330] [Cited by in RCA: 291] [Article Influence: 72.8] [Reference Citation Analysis (1)] |
| 13. | Krupelnytska L, Yatsenko N, Keller V, Morozova-Larina O. The impact of events scale-revised (IES-R): Validation of the Ukrainian version. Compr Psychiatry. 2025;139:152593. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 5] [Article Influence: 5.0] [Reference Citation Analysis (1)] |
| 14. | Deluca P, Foley M, Dunne J, Kimergård A. The Severity of Dependence Scale (SDS) for Codeine: Preliminary Investigation of the Psychometric Properties of the SDS in an Online Sample of Codeine Users From the UK. Front Psychiatry. 2021;12:595706. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 4] [Article Influence: 0.8] [Reference Citation Analysis (1)] |
| 15. | Olatunji BO, Deacon BJ, Abramowitz JS, Tolin DF. Dimensionality of somatic complaints: factor structure and psychometric properties of the Self-Rating Anxiety Scale. J Anxiety Disord. 2006;20:543-561. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 159] [Cited by in RCA: 128] [Article Influence: 6.1] [Reference Citation Analysis (3)] |
| 16. | Benzein E, Berg A. The Swedish version of Herth Hope Index--an instrument for palliative care. Scand J Caring Sci. 2003;17:409-415. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 73] [Cited by in RCA: 55] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 17. | Ilić I, Šipetić S, Grujičić J, Mačužić IŽ, Kocić S, Ilić M. Psychometric Properties of the World Health Organization's Quality of Life (WHOQOL-BREF) Questionnaire in Medical Students. Medicina (Kaunas). 2019;55:772. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 78] [Cited by in RCA: 47] [Article Influence: 6.7] [Reference Citation Analysis (1)] |
| 18. | Wang J, Deng N, Qi F, Li Q, Jin X, Hu H. The effectiveness of postoperative rehabilitation interventions that include breathing exercises to prevent pulmonary atelectasis in lung cancer resection patients: a systematic review and meta-analysis. BMC Pulm Med. 2023;23:276. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 16] [Article Influence: 5.3] [Reference Citation Analysis (1)] |
| 19. | Tao W, Huang J, Jin Y, Peng K, Zhou J. Effect of Pulmonary Rehabilitation Exercise on Lung Volume and Respiratory Muscle Recovery in Lung Cancer Patients Undergoing Lobectomy. Altern Ther Health Med. 2024;30:90-96. [PubMed] |
| 20. | Taylor SJC, Sohanpal R, Steed L, Marshall K, Chan C, Yaziji N, Barradell AC, Font-Gilabert P, Healey A, Hooper R, Kelly MJ, Mammoliti KM, Priebe S, Rajasekaran A, Roberts CM, Rowland V, Singh SJ, Smuk M, Underwood M, Waseem S, White P, Wileman V, Pinnock H. Tailored psychological intervention for anxiety or depression in COPD (TANDEM): a randomised controlled trial. Eur Respir J. 2023;62:2300432. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 23] [Article Influence: 7.7] [Reference Citation Analysis (1)] |
| 21. | Lamberton CE, Mosher CL. Review of the Evidence for Pulmonary Rehabilitation in COPD: Clinical Benefits and Cost-Effectiveness. Respir Care. 2024;69:686-696. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 19] [Article Influence: 9.5] [Reference Citation Analysis (1)] |
| 22. | Sohanpal R, Pinnock H, Steed L, Heslop-Marshall K, Kelly MJ, Chan C, Wileman V, Barradell A, Dibao-Dina C, Font Gilabert P, Healey A, Hooper R, Mammoliti KM, Priebe S, Roberts M, Rowland V, Waseem S, Singh S, Smuk M, Underwood M, White P, Yaziji N, Taylor SJ. A tailored psychological intervention for anxiety and depression management in people with chronic obstructive pulmonary disease: TANDEM RCT and process evaluation. Health Technol Assess. 2024;28:1-129. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 8] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
| 23. | Yohannes AM. Psychosocial Support in Pulmonary Rehabilitation. Respir Care. 2024;69:664-677. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 5] [Article Influence: 2.5] [Reference Citation Analysis (1)] |
| 24. | Ryzer D, Bhatti B, Streicher A, Weinberg P, Hanna F, Moretto J, Brooks D, Quach S, Oliveira A. Cognitive Interventions in Individuals With Chronic Respiratory Diseases: Protocol for a Systematic Review. JMIR Res Protoc. 2023;12:e48235. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Reference Citation Analysis (0)] |
| 25. | Moy ML. Maintenance Pulmonary Rehabilitation: An Update and Future Directions. Respir Care. 2024;69:724-739. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 8] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 26. | Parekh TM, Ramachandran R, Kim YI, Haider Z, Bhavnani D, Wells JM, Matsui E, Dransfield MT. Psychobiologic Correlates of Stress in Individuals With COPD. Chronic Obstr Pulm Dis. 2025;12:213-222. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Reference Citation Analysis (0)] |
| 27. | Marpaung FR, Mayasari V, Sidjabat H, Soehita S, Semedi BP, Parwati I, Wihastuti TA, Iskandar A, Aryati. Analysis of Adrenocorticotropic Hormone and Cortisol Levels in Acute Respiratory Distress Syndrome COVID-19 Patients. Dis Markers. 2022;2022:3191285. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 28. | Thomas AJ, Gunasekaran D, Venkatesh C, Chhavi N, Palanisamy S. Cord Blood Cortisol Level - A Possible Predictor for Respiratory Distress Syndrome in Preterm Neonates. Curr Pediatr Rev. 2025;21:276-282. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 29. | Marchetta E, Mancini GF, Morena M, Campolongo P. Enhancing Psychological Interventions for Post-Traumatic Stress Disorder (PTSD) Treatment with Memory Influencing Drugs. Curr Neuropharmacol. 2023;21:687-707. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (1)] |
| 30. | Fernandes I, Santos A, Rodrigues G, Oliveira A, Marques A. Functional status following pulmonary rehabilitation in people with ECOPD: A systematic review and meta-analysis. Respir Med Res. 2023;84:101045. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Reference Citation Analysis (0)] |
| 31. | Tonga KO, Oliver BG. Effectiveness of Pulmonary Rehabilitation for Chronic Obstructive Pulmonary Disease Therapy: Focusing on Traditional Medical Practices. J Clin Med. 2023;12:4815. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 24] [Cited by in RCA: 19] [Article Influence: 6.3] [Reference Citation Analysis (1)] |
| 32. | Mujovic N, Nikolic D, Markovic F, Stjepanovic M, Zekovic M, Ali HSH, Zivanovic D, Savic M, Laban M. The Effects of Six Weeks Pulmonary Rehabilitation on Functional and Psychological Outcomes in Long-COVID Patients: Preliminary Results from Serbian Single Center Study. Medicina (Kaunas). 2024;60:671. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (1)] |