Published online Apr 19, 2026. doi: 10.5498/wjp.v16.i4.114215
Revised: October 27, 2025
Accepted: December 10, 2025
Published online: April 19, 2026
Processing time: 197 Days and 20.1 Hours
Psychotherapy research has long investigated the factors that influence the suc
To investigate the detailed process and course of psychoanalytic therapeutic work using the Psychoanalytic Core Competency Q-Sort.
We conducted a retrospective, single-center observational reanalysis of data from 90 depressed patients originally included in the Munich Psychotherapy Study, which was conducted at Medical University Vienna as a psychotherapy research center. All patients were analyzed using audio recordings of the sessions. One-third of the patients received behavioral therapy, 1/3 received psychodynamic psychotherapy and 1/3 received classical psychoanalytical treatment. Data from the first and last sessions of psychoanalytic treatments of severely depressed pa
Using Core Competency Q-Sort Coding to provide a detailed description of the process and course of therapeutic work, interesting findings were made regarding the core analytical competencies that revolve around curative work on the unc
Precise adaptation and attunement to the patient’s inner life and socialization history-relevant representations in the present moment ensured a successful therapeutic process.
Core Tip: This article investigated long-term effectiveness of professional competencies, which deals with detailed description of process and progression of therapeutic work using Core Competency Q-Sort Coding. Interesting findings were made with regard to core competencies that cluster around healing work on implicit memory: More confrontational inter
- Citation: Löffler-Stastka H, Narath U. Professional interventions affect outcome in depressed patients. World J Psychiatry 2026; 16(4): 114215
- URL: https://www.wjgnet.com/2220-3206/full/v16/i4/114215.htm
- DOI: https://dx.doi.org/10.5498/wjp.v16.i4.114215
Various studies have clearly shown that psychotherapy leads to significant success in terms of symptom improvement and psychostructural change[1,2]. This raises the question of whether certain methodological and technical treatment efforts can trigger these changes in the form of symptom reduction or improved psychological competence of patients, i.e., whether the treatment “process” itself can change the patient’s psychic structure and psychic functioning, or whether other processes must be considered. For example, some studies show that working through intrapsychic conflicts or active self-analysis at the end of psychoanalytic therapy are important for lasting healthy psychic functioning[3]. Another current term is “mastery”, which can be considered a success variable. It has been applied in relation to resolution of interpersonal conflicts[4]. The short definition is “emotional self-control and intellectual self-understanding in the context of interpersonal relationships”[4,5]. Valid instruments are also required to track and document these processes.
The Munich Psychotherapy Study (MPS)[6] opened up research opportunities based on recorded therapy sessions conducted by experienced behavioral therapists, psychoanalytically oriented therapists and psychoanalysts.
With particular regard to the therapeutic process[7], questions that can be linked to course of therapy can be investigated. These include questions about the quality of the patient’s interaction with their therapist, questions about the the
To date, the following instruments have been used for this purpose. The Psychotherapy Process Q-Set (PQS)[8,9] was developed and used to examine the overall process in general[10]; it provides results and considerations for capturing therapist variables[11] and their effects on different treatments. This decomposition process provided insight into the interaction between patient variables[12], such as affect regulation[13], and therapists’ emotional responses[14], to better understand intervention techniques and therapeutic style of different therapists[15]. The next step is to create the pos
The assessment tool “Psychoanalytic Core Competency (PCC) Q-Sort Q-Sort”[18] was also subjected to initial construct validity tests using the Munich protocols, which were promising. As an extended study concept, it is currently being used both to improve the PCC Q-Sort in terms of test theory using a larger sample[17] and to perform cross-validation with the PQS[8] values already available. Based on previous findings on core competencies[16], clinical experience and theory, there is reason to believe that certain techniques or interventions generally have a positive influence on depression scores. The null hypothesis is therefore that neither attitude nor framework conditions, intervention, nor enactment values have an influence on depression scores or psychic functioning.
The hypothesis was that “attitude items”, “setting items”, “clinical theory items”, “intervention items”, and “enactment items” occur consistently throughout treatment and influence the patient’s depressive symptoms and psychic fun
Sustainable changes in treatments and psychoanalytic therapy were observed in patients, which were linked to structural changes and examined in this data set prior to this study[19]. This study primarily investigated the interventions and procedures used by therapists. A retrospective single-center analysis was performed to examine the effectiveness and competencies of the treating therapists. This study was approved by the Medical Ethics Committee of Medical University Vienna, approval No. 1561/2023.
Participants in the MPS[6,7] are a group of randomized patients with diagnoses of depression. One-third of the patients with personality disorders were treated with psychodynamic psychotherapy (n = 31), 1/3 were treated with psychoanalysis (n = 35) and 1/3 were treated with behavioral therapy (n = 34). The sessions are available as audio recordings. The research results were originally published by Huber and Klug[7], with key findings corresponding to practical work, namely that specific techniques are more important than the number of therapy sessions[19,20], especially in long-term therapy for comorbid patients.
Process research: For the purpose of this study, there are a total of three audio recordings of the sessions per patient at the beginning, middle and end of treatment.
Experts: The treatments were performed by highly experienced practitioners. To examine the competencies of the professionals, 30 psychoanalytic sessions from the initial, middle, and final phases of treatment were evaluated using the PCC Q-Sort in the first validation study[18], which analyzed internal consistency and reported details on evaluation areas, scoring ranges, sample training procedures, interrater reliability coefficients, and psychometric validation.
Raters: To ensure the quality of the raters, six additional sessions were used to calculate the interrater reliability by hav
Data from 29 psychoanalytic treatments are available: 10 cases were processed as part of another scientific study[18]; for the study presented here, audio recordings that had sufficient audio quality and for which all other test values [Beck Depression Inventory (BDI), Affect Regulation and Experience Q-Sort Test (AREQ)] were available were selected[13]. The audio recordings were distributed to the evaluator at random. A total of 58 hours were evaluated for the present study, with all 9 hours being evaluated in some cases. Of a total of 13 patient-analyst dyads, at least one initial and one final ses
Outcome research: The first and last sessions for each patient were primarily used for further processing. The MPS pro
All data in this study comes from recorded therapy sessions and were evaluated by a professional psychoanalyst.
The PCC Q-Sort is an assessment tool developed for research purposes to best describe the work analysts in a single session. Therefore, this survey focuses on the analyst’s interventions rather than those of the patient. However, some results data are available, allowing conclusions to be drawn about the effects of certain interventions.
The history of the PCC begins with Tuckett[21]. In 2007, he took on the commendable task of developing a system that would make the various psychoanalytic approaches discussable on the basis of case studies. His method is based on the idea that innovation arises from differences, whereby the development of this system served not only to postulate the
In the first step, each intervention by the treating analyst is examined by the evaluator or rating group within the following framework: (1) Is it an intervention aimed at maintaining the basic attitude? (2) Is it an additional element to promote the unconscious process? (3) Is it a question, clarification, or reformulation intended to sharpen awareness? (4) Is it a naming of the emotional and fantasized meaning that the situation has for the person being analyzed in the here and now? (5) Is it a construction intended to reveal a more nuanced meaning? and (6) Is it an abrupt and seemingly cons
In the second step, the evaluators discuss what beliefs the case presentation may reveal, i.e., how the situation between the analyst and the patient is perceived overall. The framework for this step comprises four pillars with typical questions: (1) Listening to the unconscious: Careful attention should be paid to finding examples in the session report that suggest that the analyst is substituting meanings or introducing reverie[1]; (2) What promotes the process? After reviewing the in
The PCC Q-Sort instrument consists of 27 items that the evaluators ask themselves while listening to the interventions of the treating analyst and evaluate using the Q-Sort method[18]. The first step focuses on whether specific intervention or attitude of the analyst can be rated as “typical”/“rather typical” or “atypical”/“rather atypical” for the course of the session. Neutral items are rated as zero. This results in a 5-point scale.
Items relating to analytical attitude (e.g., neutrality, indifference to wishes and demands, maintaining a metacognitive attitude, balance of emotional reactions/countertransference, etc.): 4 items. Items relating to the environment (e.g., is the framework of treatment addressed? Frequency, breaks, financing, tardiness/early arrival, etc.): 3 items. Items that reveal the clinical theory of the analyzing person: 2 items. Items that outline the interventions of the analyzing person (e.g., is interpretation typically used in this unit? Are clarifications, confrontations used, in what way, in a timely manner, does containment take place, is it worked through? Is the dominant affect addressed in the actively presented object rela
The primary endpoint was the proportion of patients with a clinical response, measured with the BDI[22] in the original study. Therefore, the results already available include the values (mean, SD, min-max at baseline and at the end) from the BDI[6]. Secondary endpoints were clinical remission and stability in affect experience and affect regulation, measured using the AREQ[13]. The question now arises as to how the competencies can be assessed in relation to variables from other instruments, e.g., the outcome variable from the BDI[22]. There is reason to believe that certain techniques or interventions generally have a positive influence on depression scores. The null hypothesis is therefore that neither attitude nor framework conditions, inter
In this study, SPSS was primarily used in the form of Spearman correlations, but partial correlation was also used where appropriate. The item bundles/subdimensions of the PCC were then examined in more detail with regard to differences between or stability in the analysts’ approach in relation to the first and last sessions in the psychoanalysis units at hand. The hypothesis was that “attitude items”, “framework items”, “clinical theory items”, “intervention items”, and “en
Furthermore, the correlation between the PCC and positive treatment outcomes based on the results of BDI is of interest: Are there markers in the analysts’ approach that influence depression scores? Another question relates to available data from the AREQ[13]: Can statements be made about improved affect perception and regulation during the course of treatment based on the evaluated data sample? Finally, case studies are used for microanalyses to determine whether treatment processes can be mapped using the PCC assessment tool. The hypothesis is that the graphs clearly show the analysts’ approach and allow conclusions to be drawn about the course of the analysis.
The original study included 90 patients treated with psychotherapy[6,7]. Of these, 13 patients were included in the eva
| Patient | BDI: Change scores | BDI: End-of-treatment scores | BDI: Baseline scores |
| 1 | -14.00 | 7.00 | 21.00 |
| 2 | -34.00 | 0.00 | 34.00 |
| 3 | -21.00 | 3.00 | 24.00 |
| 4 | -19.00 | 11.00 | 30.00 |
| 5 | -7.00 | 10.00 | 17.00 |
| 6 | -37.00 | 0.00 | 37.00 |
| 7 | -24.00 | 12.00 | 36.00 |
| 8 | -17.00 | 0.00 | 17.00 |
| 9 | -21.00 | 1.00 | 22.00 |
| 10 | -3.00 | 27.00 | 30.00 |
| 11 | -29.00 | 6.00 | 35.00 |
| 12 | -8.00 | 9.00 | 17.00 |
| 13 | -18.00 | 0.00 | 18.00 |
| mean n = 13 | 19.39 | 6.62 | 26.00 |
Table 2 provides an overview of PCC-Q-Sort scales correlated with changes in BDI scores and contains the results of the respective scales in the first few hours. With regard to the interventions, one significant finding can be made; the use of interventions in the first few hours leads to the predictability of improved depression scores.
| Characteristic | Attitude | Framework | Interventions | Enactment |
| BDI-change score | ||||
| Correlation | -0.282 | 0.203 | -0.577 | 0.383 |
| Significance | 0.375 | 0.527 | 0.05 | 0.219 |
Because the data in this study originate from the treatment of symptomatically depressed patients with persistent change and remission[19], improvements should be observed at least in AREQ[13] factor 2, “positive affects”, and a decrease in factor 3, “intense negative affects” with regard to the regulatory factors, particular attention is paid to factor 4, “reality-focused response”. The remaining scales represent different diagnostic constructs. For example, the items in factor 5 (“externalizing defense”) appear to be less meaningful for depressed patients and may even operate in the opposite direction, such that greater externalization could reduce the space available for self-destructive thoughts and behaviors.
In the processed sample, the sum values across the six factors were tested for significance using the Wilcoxon test in a before-and-after comparison, with r indicating the effect size for significant results[23]. The results are shown in Table 3. As expected, affect perception improves in factor 2 (“positive affect”). The result for factor 3 is surprising, as the signi
| Affect regulation | Value | Effect sizes | ||
| Affect experience | Factor 1: Socialized negative affect | Z = -1.149 | Not significant | - |
| P value = 0.251 | ||||
| Factor 2: Positive affect | Z = -2.176 | Significant | r = 0.60 | |
| P value = 0.030 | ||||
| Factor 3: Intense negative affect | Z = -2.060 | Significant | r = 0.57 | |
| P value = 0.039 | ||||
| Affect regulation | Factor 4: Reality focused response | Z = -1.029 | Not significant | - |
| P value = 0.304 | ||||
| Factor 5: Externalizing defense | Z = -2.952 | Significant | r = 0.82 | |
| P value = 0.003 | ||||
| Factor 6: Avoidant defense | Z = -0.134 | Not significant | - | |
| P value = 0.894 | ||||
Individual professional attitudes, interventions, and enactments can be interpreted in the following individual ass
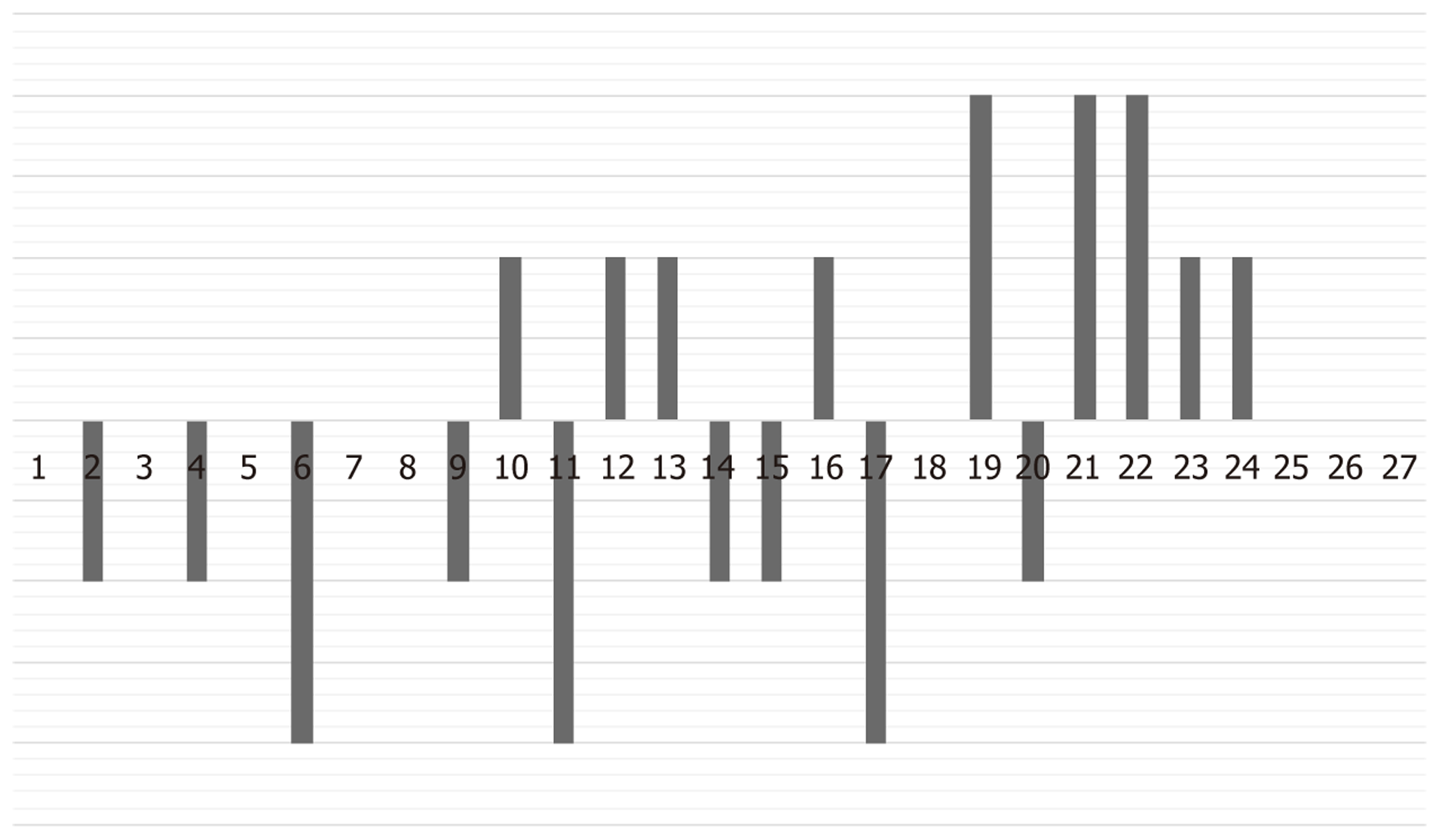
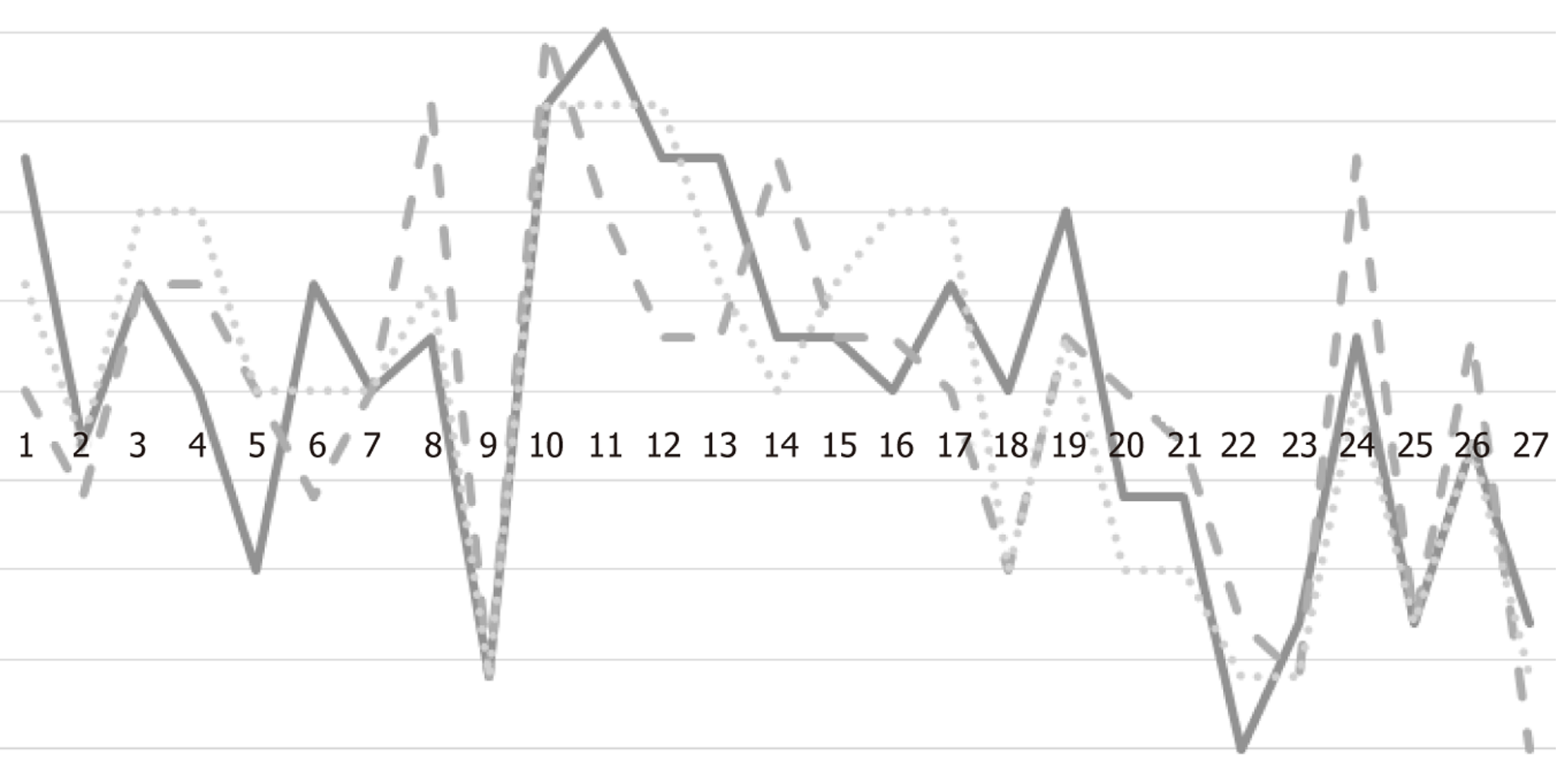
Another way of presenting results is to calculate average values for the individual items over the entire course of therapy. If there are three initial, middle and final sessions available, in this case nine sessions, we can begin to make stable conclusions about the analyst’s actions can be drawn. Figure 2 shows comparison diagrams for the three phases, from which the following conclusions can be drawn: The analyst intervenes very consistently; there is hardly any tendency to work differently in the middle phase of treatment than at the beginning or end of treatment. The evaluation places most interventions in the positive range (above the X-axis), which corresponds to typical analytical intervention practice. Regarding the attitude scale (items 1-4), the item neutrality shows a slightly lower positive tendency, which means that the analyst consistently uses neutrality not as a specific tool but as an attitude. It could also be a tactical measure if the analyst’s working hypothesis is that the patient needs a certain attitude from the analyst, as is common in some analytical schools. This example can therefore be considered a successful outcome, as the depression score (BDI) has developed from a high baseline (severe depression) to an almost unremarkable clinical picture. The solid line represents the mean PCC item values (1-27) of the first sessions, the dashed line represents the mean values of the middle sessions, and the dotted line represents the mean values of last sessions.
The subdimensions mentioned (attitude, framework conditions, interventions, enactment) and the differences were also tested using a Wilcoxon test[23], with the following results (Table 4). There are statistically significant differences in the before-and-after comparison in the “framework conditions” and “interventions” dimensions. In terms of interventions, the average value decreases at the end of the analysis, which means that fewer interventions are carried out. On the other hand, the framework conditions are rated more positively at the end of the analysis.
| Characteristic | P value | Effect sizes | |
| Attitude before/after | P value = 0.797 | Not significant | - |
| Framework before/after | P value = 0.045 | Significant | r = 0.56 |
| Interventions before/after | P value = 0.003 | Significant | r = 0.76 |
| Enactment before/after | P value = 0.086 | Not significant | - |
The relationship between the individual sub-dimensions also appears to be important: This allows the design of the procedure to be reviewed. For example, it is assumed that the typical analytical “attitude” negatively correlates with the “enactment” dimension. Using Spearman’s correlation, we found the following for the first hours (n = 13): Attitude - enactment (Spearman’s rho -0.752; P = 0.003). “attitude” and “enactment” are also opposite in relation to the last sessions (n = 13): Attitude - enactment (Spearman’s rho -0.828; P = 0.000). Because the hypothesis was that the “interventions” dimension also negatively correlates with “enactment”, the following correlation values for “interventions” with “enactment” were obtained at the beginning and end: Start (n = 13): Interventions - enactment (Spearman’s rho -0.670; P = 0.012), end (n = 13): Interventions - enactment (Spearman’s rho -0.8049, P = 0.001). “Enactment” contradicts analytical “interventions”.
As demonstrated by the summary calculations, it is possible to monitor patients in terms of their treatment progress. If the values are unfavorable, measures can be taken. One example is PCC assessment. At the end of the analysis, the ana
One limitation of the study is the small number of hourly logs evaluated and the resulting question of external validity and generalizability. Given the small sample size, the retrospective design, and nature of evaluations, the results should be considered preliminary and hypothesis-generating rather than conclusive. Further studies are needed to track the dev
The main objective of our study was to evaluate professional interventions and their effect on depressive symptoms and affect regulation in practice. Our study confirms the effectiveness of a neutral attitude and appropriate interventions.
The classification of the PCC Q-Sort into the categories of attitude, framework conditions, clinical theory, interventions, and enactment allows us to conclude the following. At the end of treatment, analytical attitude characteristics such as balanced attention, abstinence, focus on latent content, and neutrality are more pronounced than at the beginning of tre
The subdimension “framework concept” comprises three items, but according to the classical understanding, only one item, namely “analytical framework concept” is the feature that selects the situation surrounding the analytic session as the content of the work. In the results presented, work on the framework concept is found in the rather atypical area, i.e., it is only addressed to a limited extent by the analysts in the sample. The “analytical framework” tends to be emphasized more strongly at the end of treatment but remains less pronounced when adherence to treatment is used as a guideline. This could be related to different regional traditions in analytic work, as Tuckett[21] has previously suggested, and sho
The question of whether a clear clinical theory can be derived from the analysts’ comments tends to be answered in the negative and does not seem to be very helpful as a question in the procedure. It is known that the use of theory, especially in form of intellectualization and rationalization, does not help the patient, as only affects can be considered as facts[1].
As the term suggests, the subdimension of interventions comprises theory-driven items that can be understood as describable communicative figures used by the analysts and that occur with particular frequency, especially at the beg
Finally, the “enactment” subdimension shows an increase in item values at the end of the analyses, which means that enactments are rather atypical, but tend to occur more frequently at the end of analysis than at the beginning.
The other question addressed in the study concerned the relationships between the subdimensions. Here, it was clearly shown that both at the beginning and at the end of the analyses, enactment items negatively correlate with intervention and attitude items. This could mean that concentrated listening and restraint on the part of the analyst can keep ena
Objective symptom changes from the available data could be used for further processing, yielding interesting findings. Because the application of intervention elements clearly correlated with improved depression scores, the PCC subdi
Patients’ affect perception and regulation appear to be a sustainable indicator for outcome assessment, particularly regarding the stability of therapy success and the lasting change from negative introjects to positive ones[19] or the con
The individual case analyses at the end of the paper show that the PCC Q-sort is a helpful tool for describing the wor
This work focused on the treating, analyzing person and how they could proceed in the service of successful therapeutic work. This is relevant not only for the training of analysts, but also for the sustainable structural change of patients.
The PCC Q-Sort instrument is helpful for representing technical and attitude-related elements but could be supplemented by a description of the emotional situation of the analyzing person and the sequence of processes, e.g., in relation to interpretive skills and the development of insight-promoting sub-steps of interpretations.
Consistent with the innovation in International Classification of Disease-11[24], the assessment of severity and the number of activity areas that are affected seem to have a higher prognostic value than so-called structural deficits. However, further research on the topic of “coping” (via “working through”) is promising, as patients should be emp
In any case, this study provides considerable evidence that the quality of the intervention, i.e., the professional com
The authors would like to thank Jürgen Fuchshuber for his statistical expertise in relation to[23] and Gavin Lord and Shawn Egan Bryan for their expertise as native English speakers who corrected the style.
| 1. | Leuzinger-Bohleber M, Kächele H. An Open Door Review of Outcome and Process Studies in Psychoanalysis. 3rd ed. London: International Psychoanalytic Association, 2015. |
| 2. | Leichsenring F, Abbass A, Luyten P, Hilsenroth M, Rabung S. The emerging evidence for long-term psychodynamic therapy. Psychodyn Psychiatry. 2013;41:361-384. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 67] [Cited by in RCA: 48] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 3. | Falkenström F, Grant J, Broberg J, Sandell R. Self-analysis and post-termination improvement after psychoanalysis and long-term psychotherapy. J Am Psychoanal Assoc. 2007;55:629-674. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 41] [Cited by in RCA: 30] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 4. | Rosbrow T. Review of Understanding Transference: The CCRT Method, by Luborsky and Crits-Christoph. Psychoanal Psychol. 1995;12:607-610. [DOI] [Full Text] |
| 5. | Poscheschnik G, Crepaldi G. Only chance and circumstances? Or, how Freudian are Freudian slips? A review of research literature concerning parapraxes. Psychoanal Psychol. 2022;39:189-197. [DOI] [Full Text] |
| 6. | Huber D, Zimmermann J, Henrich G, Klug G. Comparison of cognitive-behaviour therapy with psychoanalytic and psychodynamic therapy for depressed patients - a three-year follow-up study. Z Psychosom Med Psychother. 2012;58:299-316. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 44] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 7. | Huber D, Klug G. Münchner Psychotherapiestudie. Psychotherapeut. 2016;61:462-467. [RCA] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 8] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 8. | Bonalume L, Corbelli L, Ferro M, Mazzoleni AL, Roggero MP. Developing a prototype for relationship therapy psychoanalysis: an empirical study with the Psychotherapy Process Q-set. Res Psychother. 2023;26:674. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 9. | Ablon JS, Jones EE. On analytic process. J Am Psychoanal Assoc. 2005;53:541-68; discussion 569. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 39] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 10. | Freudenreich O, Huffman JC, Sharpe M, Beach SR, Celano CM, Chwastiak LA, Cohen MA, Dickerman A, Fitz-Gerald MJ, Kontos N, Mittal L, Nejad SH, Niazi S, Novak M, Philbrick K, Rasimas JJ, Shim J, Simpson SA, Walker A, Walker J, Wichman CL, Zimbrean P, Söllner W, Stern TA. Updates in Psychosomatic Medicine: 2014. Psychosomatics. 2015;56:445-459. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 0.4] [Reference Citation Analysis (1)] |
| 11. | Hau C, Huber D, Klug G, Benecke C, Löffler-Stastka H. Vergleich therapeutenspezifischer Wirkfaktoren im psychoanalytischen, psychoanalytisch orientierten und kognitiv-verhaltenstherapeutischen Therapieprozess der Depression. Psychotherapie Forum. 2015;20:38-46. [DOI] [Full Text] |
| 12. | Lokko HN, Stern TA. Confrontations with Difficult Patients: The Good, the Bad, and the Ugly. Psychosomatics. 2015;56:556-560. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (1)] |
| 13. | Löffler-Stastka H, Stigler K. [The Affect Experience and Affect Regulation Q-Sort Test (AREQ): validation and short version]. Psychother Psychosom Med Psychol. 2011;61:225-232. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 14. | Knaus S, Grassl R, Seidman C, Seitz T, Karwautz A, Löffler-Stastka H. Psychiatrists' emotional reactions: Useful for precise diagnosis in adolescence? Bull Menninger Clin. 2016;80:316-325. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 10] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 15. | Braus N, Flückiger C, Wichmann J, Frankman C, Gräfenkämper R, Zemp M, Hunger-Schoppe C. Who determines the outcome? A three-level meta-analysis on systemic therapy in children and adolescents. Psychother Res. 2025;1-15. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 16. | Parth K, Loeffler-Stastka H. Psychoanalytic core competence. Front Psychol. 2015;6:356. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 17. | Viguera AC, Milano N, Laurel R, Thompson NR, Griffith SD, Baldessarini RJ, Katzan IL. Comparison of Electronic Screening for Suicidal Risk With the Patient Health Questionnaire Item 9 and the Columbia Suicide Severity Rating Scale in an Outpatient Psychiatric Clinic. Psychosomatics. 2015;56:460-469. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 71] [Cited by in RCA: 57] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 18. | Parth K, Wolf I, Löffler-Stastka H. Capturing the Unconscious-The "Psychoanalytic Core Competency Q-Sort". An Innovative Tool Investigating Psychodynamic Therapeutic Skills. Int J Environ Res Public Health. 2019;16:4700. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 2] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 19. | Zimmermann J, Löffler-Stastka H, Huber D, Klug G, Alhabbo S, Bock A, Benecke C. Is It All about the Higher Dose? Why Psychoanalytic Therapy Is an Effective Treatment for Major Depression. Clin Psychol Psychother. 2015;22:469-487. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 40] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 20. | Lutz W, Schwartz B, Vehlen A, Eberhardt ST, Delgadillo J. Advances in personalization of psychological interventions. World Psychiatry. 2025;24:343-345. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 21. | Tuckett D. Does anything go? . Int J Psychoanal. 2005;86:31-49. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 144] [Cited by in RCA: 82] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 22. | Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4:561-571. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27906] [Cited by in RCA: 22884] [Article Influence: 352.1] [Reference Citation Analysis (3)] |
| 23. | Rosenthal R, Rubin DB. r equivalent: A simple effect size indicator. Psychol Methods. 2003;8:492-496. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 318] [Cited by in RCA: 227] [Article Influence: 9.9] [Reference Citation Analysis (0)] |
| 24. | Bach B, First MB. Application of the ICD-11 classification of personality disorders. BMC Psychiatry. 2018;18:351. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 204] [Cited by in RCA: 136] [Article Influence: 17.0] [Reference Citation Analysis (0)] |
| 25. | Sammet I, Brockmann J, Schauenburg H. Therapeutische Intervention bei Suizidalität. Forum Psychoanal. 2007;23:18-32. [RCA] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 26. | Abram J. »Holding« und »Containing«: Zur spezifischen Natur der Objektbeziehungen bei Winnicott. Psyche - Zeitschrift für Psychoanalyse. 2023;77:768-796. [DOI] [Full Text] |
| 27. | Grevenhaus CJ, Flückiger C, Theimer L, Benecke C. Does technique matter? A multilevel meta-analysis on the association between psychotherapeutic techniques and outcome. Res Psychother. 2024;27:803. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |