Published online Apr 28, 2026. doi: 10.4329/wjr.v18.i4.119450
Revised: February 11, 2026
Accepted: March 18, 2026
Published online: April 28, 2026
Processing time: 86 Days and 15.7 Hours
This study is based on American Association of Physicist in Medicine (AAPM) task group (TG) report 204 to compare the displayed and calculated Radiation dose imparted to the patient in computed tomography (CT) head examination and the effective dose.
To identify whether there is a difference between displayed radiation doses and size-specific dose in CT head imaging. For ruling out the possibility of dose esti
A prospective cross-sectional study was done on CT head examinations using multidetector CT. The study included subjects aged between 18 and 60 years with no obvious morphological head deformities. We compared the size-specific dose estimate (SSDE) displayed and calculated where we used f factor for effective diameter from AAPM report 204 and manually calculated the SSDE for comparison. We also calculated the effective dose for head CT manually using dose-length product and k value from AAPM report 96.
The difference between SSDE Calculated and displayed was found to be -11.99%, the negative value depicts that the SSDE displayed in the patient dose chart in CT is much lower than the calculated SSDE. Hence it highly underestimates the dose received by the patient and further cancer risk estimation. We also found that the radiation dose received by patient is inversely related to the effective diameter of their head.
The observed difference between the calculated and displayed dose values falls within the acceptable range of 10%-20% as recommended by the AAPM TG report 204, indicating consistency with established guidelines.
Core Tip: Since radiation can cause various effects in humans whether it is somatic or genetic, this study aims to determine whether there are any differences in the displayed and calculated radiation dose in case of head computed tomography (CT). To rule out the probability of under or over estimation of radiation dose for the same, as it is essential for radiation to be within the acceptable limits to prevent risk of cancer and other stochastic and deterministic effects. In our study we found that the size specific dose estimate is severely underestimated in the patient dose chart. This indicates the patient is exposed to much greater radiation than estimated so, there is a need for maintaining lowest possible dose criteria for scanning to prevent any probability of radiation induced effects in the patient. Study of this type has not been done in this area and provides impactful insights on the dose underestimation in head CT.
- Citation: Chauhan A, Sharma S, Mishra A, Pathak A, Mittal KK. Study of displayed radiation dose and size-specific dose estimate from computed tomography brain examinations in accordance to head sizes. World J Radiol 2026; 18(4): 119450
- URL: https://www.wjgnet.com/1949-8470/full/v18/i4/119450.htm
- DOI: https://dx.doi.org/10.4329/wjr.v18.i4.119450
The computed tomography (CT) scan has readily evolved since its introduction in 1972 to become one of the most important medical instrumentations for radiological examinations. High-quality CT imaging is essential to medical imaging because it helps patients and offers aids in precise diagnosis. As a result, CT is routinely employed in all medical facilities for the initial diagnosis of head trauma and other pathologies and is acknowledged as the gold standard for both the identification of intracranial abnormalities and the acute management of patients with closed head injuries[1] Because of its high contrast resolution, high spatial resolution, and speedier image capture than other modalities, CT offers nu
With the introduction of dual-section capable scanners in 1992, multi-section CT was first used. It was enhanced in 1998 with the creation of quad-section technology. Multi slice CT scanners are now up to eight times faster than tradi
Radiation exposure from diagnostic medical procedures is regularly assessed to make sure they are as minimal as is reasonable while still yielding the necessary diagnostic data[5]. When optimizing the dosages given to patients, the risks and benefits of medical operations are taken into account. Due to the relatively high doses involved, CT is a commonly utilized imaging modality that accounts for a significant fraction of the total effective dose from medical exposures. As a result, strategies for reducing CT scan dosages to a minimum have received great attention during the past 20 years[6].
To improve the safety precautions to be taken to limit radiation exposure (both ionizing and non-ionizing), accurate dose estimation is crucial. Since the Ionizing radiation damages cells’ DNA, which can lead to uncontrollable cell division and cancer if the damage is not effectively repaired. Additionally, it can cause somatic damage to the entire body or genetic damage to eggs and sperm[7].
Medical physicists and radiologists utilize an enhanced measure called the size-specific dose estimate (SSDE) to calculate each patient’s exposure during body CT scans. Compared to the conventional dose metrics of volume CT dose index (CTDI) and dose-length product (DLP), SSDE offers a more accurate estimation of patient dose. To estimate each patient’s dose, SSDE is computed using automated or manual patient size measurements and multiplied by CTDI vol[8,9].
In view of the increasing use of CT for neuroimaging and the associated radiation exposure, there is a need for patient-specific dose assessment that accounts for variations in head size. Conventional displayed dose metrics may not accurately reflect the actual radiation dose received by individual patients. Therefore, this prospective study was undertaken at a tertiary health care center in western India to evaluate the relationship between CT scanner-displayed radiation dose parameters and SSDE in CT brain examinations, with particular emphasis on variations in patient head size. The primary objective of this study was to compare displayed CT dose indices with SSDE values and to assess the influence of head size on radiation dose estimation, with the aim of improving dose optimization and radiation safety in routine clinical practice.
Multi-detector CT imaging was performed using a 128-slice CT scanner (Incisive CT, Philips, Israel) at Uttar Pradesh University of Medical Sciences, Saifai, Etawah, with a 5.0 mm slice thickness, covering the region from the base of the skull to the vertex (Table 1).
| Protocol parameter | CT head |
| Tube voltage (kVp) | 120 |
| Reference noise (mAs) | 299.27 ± 3.58 |
| Pitch | 0.43 ± 0.09 |
| Slice thickness (mm) | 5 |
| Scanning mode | Helical |
| Orientation | Caudocranial |
| CTDI vol (mGy) | 46.83 ± 1.43 |
| DLP (mGy.cm) | 869.44 ± 98.47 |
| Scanning range (mm) | 16.77 ± 0.76 |
| SSDE calculated (mGy) | 46.95 ± 2.07 |
| SSDE displayed (mGy) | 41.64 ± 2.07 |
| E (mSv) | 1.83 ± 0.21 |
A prospective cross-sectional imaging study was conducted in the Department of Radiodiagnosis at Uttar Pradesh University of Medical Sciences, Saifai, Etawah, involving patients referred from Neurology, Psychiatry, and the Emergency and Trauma Unit for contrast enhanced CT (CECT) and non-contrast enhanced CT (NCCT) head examinations. The sample size was calculated using a convenience sampling frame with randomized patient selection, and informed consent (verbal and written) was obtained after explaining the study’s objectives. This study was approved by the University Ethics Committee with No. 232/2024-25. It is a prospective observational study. The Duration of data collection was two Months from May 2025 to June 2025.
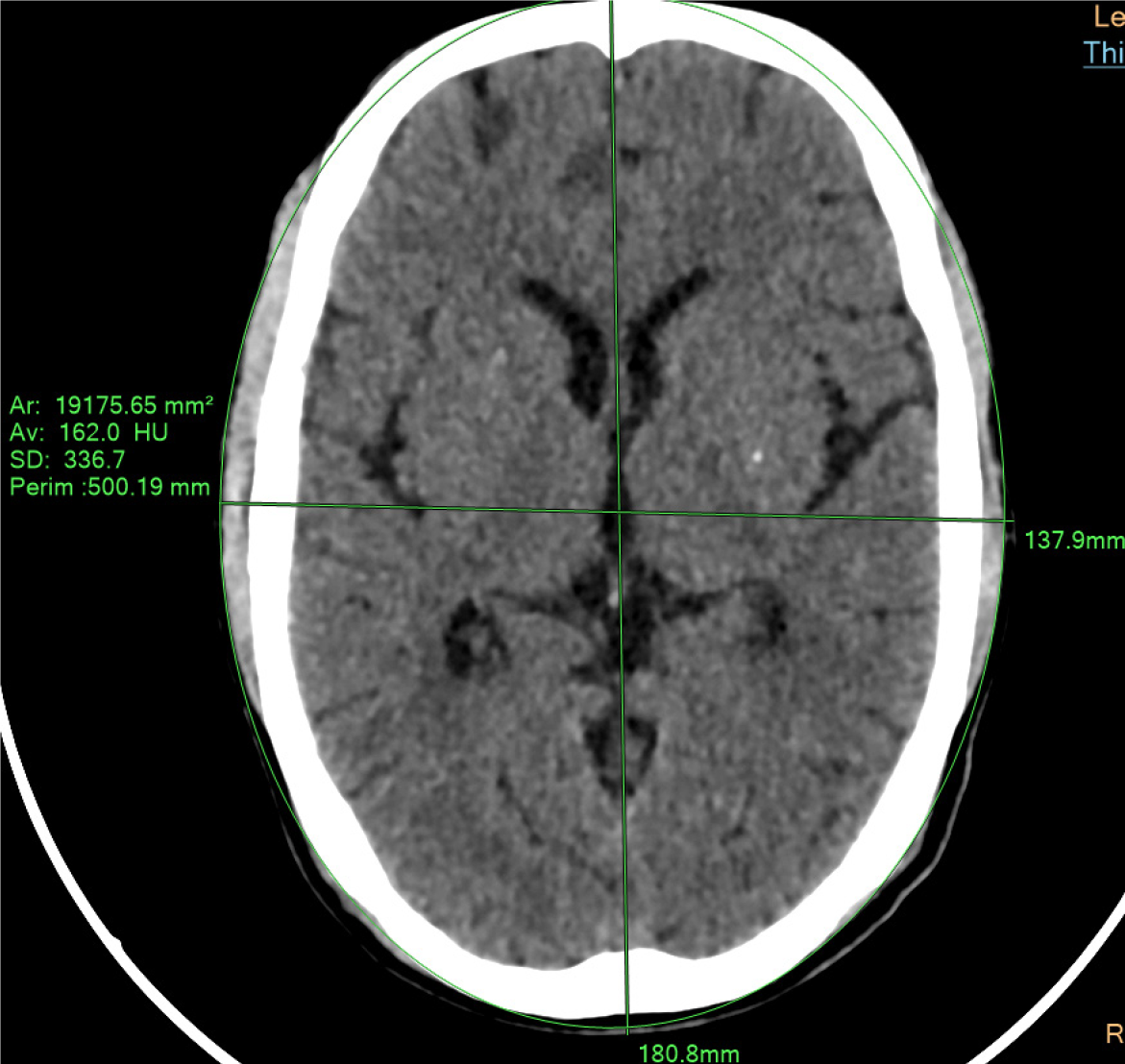
The patient position was head first supine with head resting on dedicated head rest and the laser beam centered at 2 inches above vertex. The slices were selected at the mid brain level i.e., at the mid-Thalami and the diameter is calculated in anterio-posterior (AP) and lateral (LAT). The standard protocols for CT head were incorporated without any intervention for the study including kVp, mAs, etc., which were machine based while the variables that can be easily manually manipulated such as pitch and slice thickness were used as the standard norm for the type of examination. The tube voltage (kVp) was 120 based on type of examination along with other variables as mAs, Pitch, slice thickness. The orientation for the examination was Caudo-cranial which scans from foot side to head i.e., from base of skull to vertex.
The AP length of the brain was measured along the Falx Cerebri, whereas the length of LAT was measured from right to left. using the measuring tools in CT post processing Techniques at the workstation extension, i.e., ruler and shape selector which can cover the entire head circumference and can measure the area under consideration (Figure 1).
The Deff was calculated using the AP and LAT dimensions of the diameter of brain using the formula as described in American Association of Physicist in Medicine (AAPM) report 204. Deff = (AP × LAT)1/2. It was unique for every patient as the measurements were different for AP and LAT diameters. The formula was used for manual calculation of dose.
The SSDE was calculated based on the following formula: SSDE = CTDI vol × f; where the conversion coefficient factor, f was taken from AAPM report No. 204 based on the value of Deff.
Effective dose (E) was estimated by multiplying DLP with the conversion coefficient factor k, The formula is defined as: E (mSv) = k × DLP; the k value is taken from AAPM Report 96 i.e., 0.0021 mSv for head CT[8]. Radiation dose information such as CTDI vol (mGy), SSDE (mGy) and DLP (mGy.cm) were obtained from the dose information table from the CT console.
A total of 195 patients were included (mean age 36.99 ± 12.93 years, range 18-60). Patient demographics are summarized in Table 2. Of these, 124 (63.6%) were male and 71 (36.4%) were female. Most examinations were NCCT, n = 192, 98.5%, with only 3 contrast-enhanced scans (1.5%) (Table 3). The majority of patients were referred from the emergency department (121/195, 62.1%); others came from outpatient (55/195, 28.2%) or inpatient (19/195, 9.7%) services (Tables 2, 3 and 4).
| Gender | Frequency | Percentage, % |
| F | 71 | 36.4 |
| M | 124 | 63.6 |
| Total | 195 | 100.0 |
| Exam | Frequency | Percentage, % |
| CECT head | 3 | 1.5 |
| NCCT head | 192 | 98.5 |
| Total | 195 | 100.0 |
| Department | Frequency | Percentage, % |
| EMG | 121 | 62.1 |
| IPD | 19 | 9.7 |
| OPD | 55 | 28.2 |
| Total | 195 | 100.0 |
All patients referred to the radiology department for CT head examination. With the exclusion criteria being patients younger than 18 years old or older than 60 years old, pregnant patients, CT procedures, critically ill patients, unstable patients, facial CT, temporal CT.
Statistical analyses were performed using the R programming software. Quantitative data are presented as mean ± SD. Paired-sample t-tests were used to assess statistical significance, with a P value < 0.05 considered statistically significant.
The patient size and dose metrics are summarized in Table 5. The mean AP diameter was 186.54 ± 8.84 mm and LAT diameter was 142.67 ± 7.46 mm (effective diameter; 163.08 ± 6.88 mm, i.e. 16.31 ± 0.69 cm). All scans used 120 kVp, and the mean tube current was 299.27 ± 3.58 mAs. The mean scanner-displayed SSDE was 41.64 ± 2.07 mGy and the mean calculated SSDE was 46.95 ± 2.07 mGy, corresponding to an average relative difference of -11.99% (calculated value higher). The mean CTDI vol was 46.83 ± 1.43 mGy and the mean DLP was 869.44 ± 98.47 mGy.cm. The effective dose across patients ranged from 0.14 mSv to 2.58 mSv (1.83 ± 0.21 mSv). In summary, the observed CTDI, DLP, SSDE, and effective dose values were consistent with standard head CT practice, but the displayed SSDE was systematically lower than the SSDE calculated via task group (TG)-204 (Table 5).
| Descriptive statistics | n | Minimum | Maximum | Mean | SD |
| AGE | 195 | 18.0 | 60.0 | 36.99 | 12.92 |
| AP (mm) | 195 | 162.5 | 205.8 | 186.54 | 8.84 |
| LAT (mm) | 195 | 125.2 | 160.1 | 142.67 | 7.46 |
| AP (cm) | 195 | 16.25 | 20.58 | 18.65 | 0.88 |
| LAT (cm) | 195 | 12.52 | 16.01 | 14.26 | 0.74 |
| Effective diameter (mm) | 195 | 145.12 | 178.77 | 163.08 | 6.88 |
| Effective diameter (cm) | 195 | 14.52 | 17.87 | 16.31 | 0.68 |
| Kvp | 195 | 120.0 | 120.0 | 120.00 | 0.00 |
| mAs | 195 | 298.0 | 349.0 | 299.27 | 3.58 |
| SSDE displayed | 195 | 35.75 | 46.15 | 41.64 | 2.07 |
| SSDE calculated | 195 | 40.77 | 55.56 | 46.95 | 2.07 |
| Pitch | 195 | 0.40 | 0.70 | 0.43 | 0.09 |
| CTDI vol | 195 | 42.03 | 55.01 | 46.83 | 1.43 |
| CTDI w | 195 | 16.82 | 33.02 | 20.19 | 3.76 |
| DLP displayed (mGy.cm) | 195 | 687.8 | 1230.06 | 869.44 | 98.47 |
| SCAN length (cm) | 195 | 14.10 | 18.69 | 16.77 | 0.76 |
| Effective dose (mSv) | 195 | 0.14 | 2.58 | 1.83 | 0.21 |
Correlation analysis (Table 6) showed that effective diameter was significantly inversely correlated with SSDE. Pearson correlation coefficients were r = -0.429 (P < 0.001) for effective diameter vs SSDE displayed, and r = -0.677 (P < 0.001) for effective diameter vs SSDE calculated, indicating that larger head size corresponded to lower SSDE. By contrast, SSDE displayed and SSDE calculated were positively correlated (r = 0.571, P = 0.001). All correlations were statistically significant at P < 0.01. A paired t-test confirmed that the mean SSDE displayed was significantly lower than the mean SSDE calculated (P = 0.001). These findings indicate that the scanner-reported SSDE underestimates patient-specific dose relative to the AAPM TG-204 calculation (Tables 5 and 6).
| Paired samples statistics | Mean | n | SD | Correlation | t test statistics |
| Effective diameter (mm) | 163.08 | 195 | 6.88 | 1.00 | 331.01 |
| Effective diameter (cm) | 16.31 | 195 | 0.68 | P = 0.0001 | P = 0.001 |
| SSDE displayed | 41.64 | 195 | 2.07 | -0.43 | 144.24 |
| SSDE displayed | 41.64 | 195 | 2.07 | P = 0.0001 | P = 0.001 |
| SSDE calculated | 46.95 | 195 | 2.07 | 0.571 | 38.620 |
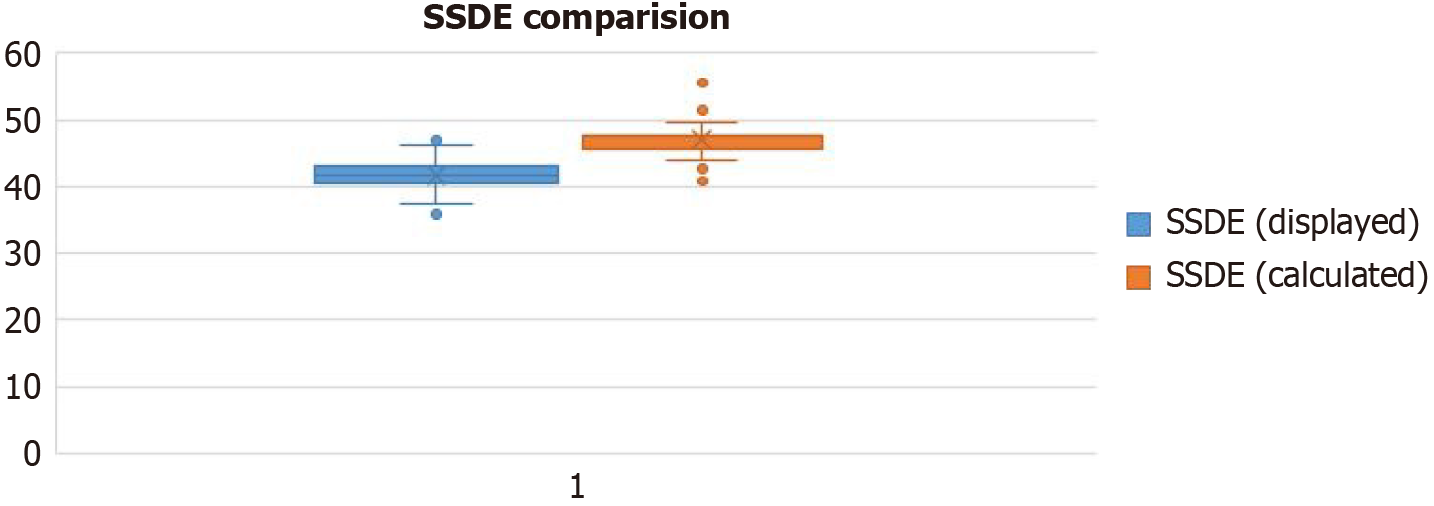
There is a statically significant difference in radiation dose imparted to the patient for which we have used the term SSDE Displayed and Calculated, with the mean percentage change being -11.99%. since there is a negative sign, we can conclude that the calculated dose is higher than the displayed dose (Figure 2).
There is no separate risk model for “Brain” in the BEIR VII report’s main 11-cancer summary tables. Instead, brain cancer is usually classified as “Other” or “Remainder” or computed using particular extension, such as those by Berrington de Gonzalez et al[10] that apply the BEIR VII methodology to brain tissue.
The additional lifetime risk of brain/central nervous system cancer in the general population (mixed age and sex) is roughly 0.002% to 0.003% per mGy, or about 2 to 3 cases per 100000 people per mGy. Using BEIR VII technique, a frequently accepted central estimate for “Other/Brain” solid tumors is roughly 2.3 × 10-6 per mGy (incidence). For solid tumors at low dosages, BEIR VII recommends a linear no-threshold model, which is assumed in the computation. Utilized Risk Coefficient: The approximate population average for the brain/nervous system is 2.3 × 10-6 (Tables 7, 8 and 9).
| Parameter | SSDE displayed | SSDE calculated |
| Dose | 41.63 ± 2.07 | 46.94 ± 2.07 |
| Calculated mean risk (LAR) | 9.57 × 10-5 | 1.08 × 10-4 |
| Risk probability | 1 in 10450 | 1 in 9260 |
| Risk range (± 1 SD) | 9.10 × 10-5-1.00 × 10-4 | 1.03 × 10-4-1.13 × 10-4 |
| Parameter | SSDE displayed | SSDE calculated |
| Mean dose (mGy) | 41.63 | 46.94 |
| Mean risk (average) | 2.08 × 10-4 | 2.34 × 10-4 |
| Risk probability | 1 in 4800 | 1 in 4270 |
| Risk range (age 18-60) | 0.8 × 10-4-4.6 × 10-4 | 0.9 × 10-4-5.1 × 10-4 |
| Parameter | SSDE displayed | SSDE calculated |
| Mean dose (mGy) | 41.63 | 46.94 |
| Mean risk (average) | 0.66 × 10-4 | 0.74 × 10-4 |
| Risk probability | 1 in 15150 | 1 in 13500 |
| Risk range (age 18-60) | 0.3 × 10-4-1.4 × 10-4 | 0.3 × 10-4-1.6 × 10-4 |
An extra 1.22 × 10-5 (or around 1.2 extra cases per 100000 people) is the risk associated with the mean dosage increase from 41.63 mGy to 46.94 mGy. The stochastic effect in SSDE Calculated is 12.8% greater than that in SSDE Displayed. Overlap The dose distributions overlap considerably given the standard deviation (2.07 mGy), but the change in the mean indicates a clear rise in the central estimate of stochastic risk (Table 7).
At these exposure levels, males in this age range are almost three times more likely than females to acquire radiation-induced brain cancer. The relative risk increases by 12.8% when the dose is increased from 41.63 mGy to 46.94 mGy. This is an absolute increase of about 2.6 additional instances per 100000 for males. This is an absolute increase of about 0.8 additional instances per 100000 for females. Age is a significant factor. Because the risk coefficients decrease with age at exposure, a 19-year-old has around five times the risk of a 60-year-old receiving the same dose. Risk for any individual can differ by about ± 5% from the mean values above, given the standard deviation of 2.07 mGy (Tables 8 and 9).
For the sample size of 195 patients, the SSDE calculated ranges from 40.77-55.56 which is higher than the computer-generated value of SSDE being 35.75-46.15. The mean values of doses for SSDE manually calculated is 46.95 while for SSDE displayed by CT machine is 41.64 confirming the under estimation of individual dose (Table 5). The mean effective dose is 1.83 ± 0.21 for head CT examination The pitch ranges from 0.4-0.7 where 0.7 was used for quick scanning and 0.4 for routine scans (Table 1). Table 5 and 6 show Mean, standard deviation, co-relation and t test statistics for the variables used for this study with the sample size of 195 patients. The P value for all is less than 0.05 with SSDE displayed and calculated varying by approximately 5 mGy.
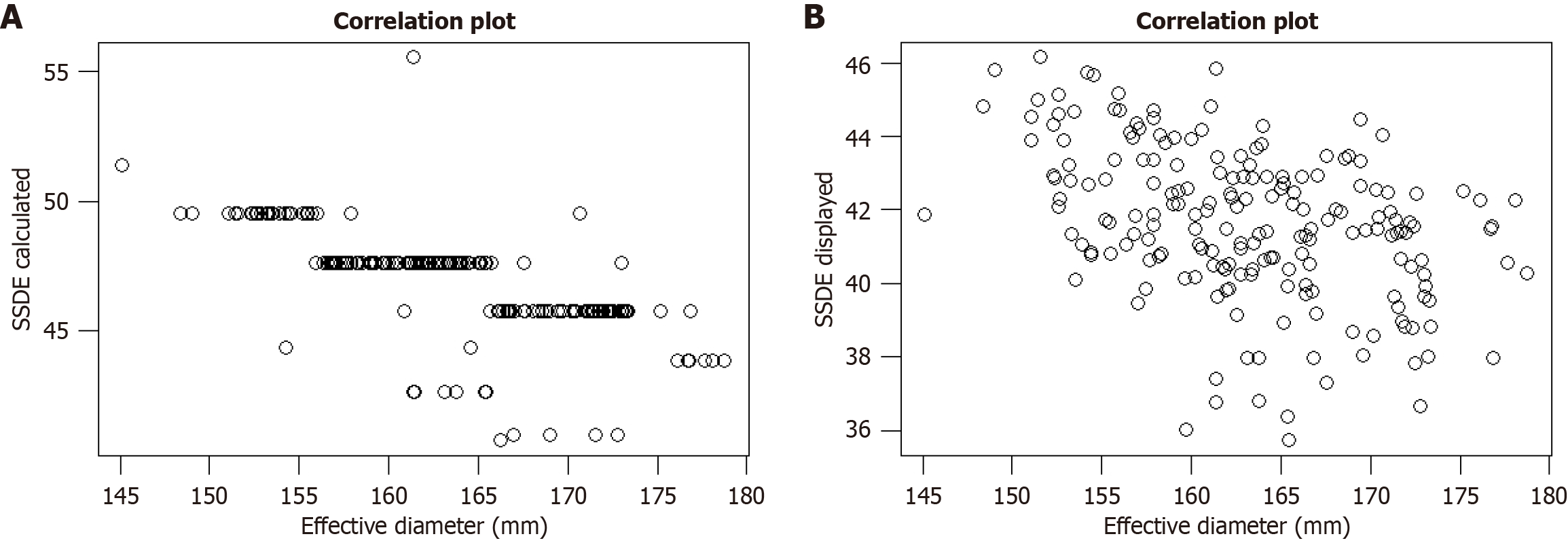
The correlation plot between effective diameter of head and SSDE calculated dose shows that most of the values align well with each other with less scattering showing the calculated dose is more specific for individual patients. Correlation plot between effective diameter of head and SSDE displayed dose shows that most of the values are scattered along the graph indicating rather poor correlation in comparison to the calculated values for the same (Figure 3).
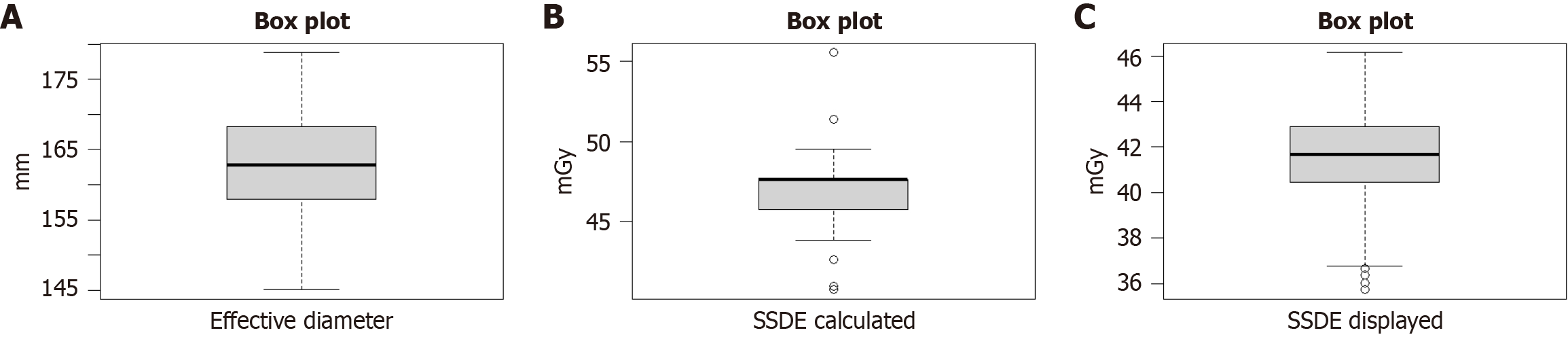
The effective diameter lies in the range of 155 to 170 here, out of 195 subjects more than half of are males having greater head circumference that females. The box plot shows SSDE Calculated manually lies in the range of 40-50 mGy which is specific for individual examination of patients. The box plot shows SSDE Calculated by machine lying in the range of 40-44 mGy which is tailored for individual examination of patients and also it underestimated the dose imparted to them during the examination.
The effective dose is predominantly between 0.14 mSv to 2.58 mSv (Table 5) and the effective diameter is mostly concentrated between 155-165 mm (Figure 4A). Females generally have lower effective diameter as compared to males (Figure 4A).
Typical effective dose values for CT head were found to be well within the defined range from AAPM report 96 i.e., 1-2 mSv. We found the mean effective dose to be 1.83 ± 0.21. The DLP value varied greatly among the patients due to variations in scan length, therefore a range of effective dose was obtained upon calculation. The difference in displayed and calculated dose is found to be 11.99 where calculated dose is higher than the displayed dose. The P value calculated using t-test statics is P = 0.001. Therefore, the alternate hypothesis of this study is significant i.e., The radiographic examination shows substantial differences between calculated and displayed radiation doses. Since it is already mentioned in the AAPM report 204 that the variation of 10-20 percent is likely to occur, results are within the range[7-11] (Figure 4B and C).
The routine underutilization of radiation dose-optimization strategies for routine CT scans results in higher doses than necessary[12]. The most commonly used dose descriptor, volumetric CTDI vol, is not a reliable indicator of dosage for patients. Specifically, it has been demonstrated that CTDI vol overestimates the skin dose to the head[13]. When the CTDI vol is converted to the SSDE, it reveals that the actual dosages to the patients’ organs are 20% to 50% lower than the CTDI vol values and do not decrease as much with patient size[8]. Because of the wide inter-patient variability, the approximation made by calculating SSDE based on geometric size only, rather than taking full tissue attenuation into consideration, may fluctuate significantly[12]. The SSDE computed using the size descriptors LAT, AP, and f factor for effective diameter over the samples under consideration showed variances that were nearly always within 10%-15% of the measurement position, but with LAT and AP, the corresponding SSDE varied by more than 20%. Furthermore, even while SSDE calculated using LAT and AP may differ by up to 10% from the reference obtained using f factor for effective diameter, the size parameter selection seems to have no such serious repercussions[14]. Possible overexposure concerns were found in certain instances when age group dosages exceeded those documented in the published data by up to 25.3% in CTDI vol and 25.8% in SSDE, respectively[15]. With percentage deviations below 10%, the machine consistently underestimates the size-specific dosimetric index[16]. The SSDE is a practical method that may help CT users understand how to use it to optimize radiation dosage in CT rather than CTDI vol, particularly for setting diagnostic reference values[17]. When tube current modulation is engaged for thoracic exams, the radiation dose (SSDE) drops as the patient’s diameter shrinks. If tube current modulation is not active, the radiation dosage (SSDE) for head exams rises as the patient’s diameter decreases[18]. Compared to CTDI vol, SSDE provides a more accurate representation of patient dose and accounts for patient size[19].
According to Table 3, a total of 195 examinations were performed. Out of these, 3 were CECT Head examinations, accounting for 1.5% of the total. The remaining 192 examinations were NCCT head, making up 98.5% of all examinations. This is mainly because most of the patients are referred from the Emergency and Trauma department which need quick scanning and reports. So, the results are focused mainly on non-contrast enhanced CT head examination.
The cancer risk for women is relatively lower but they are more susceptible to radiation induced risks since the effective dose for females is also lower.
The difference in displayed and calculated dose is found to be 11.99% where calculated dose is higher than the displayed dose which agrees with study done by Noferini et al[14], where SSDE computed using the size descriptors LAT, AP, and f factor for effective diameter over the samples under consideration showed variances that were nearly always within 10%-15% of the measurement position. Our CT unit also underestimates the SSDE as shown by the study of Zancopè et al[16].
We found that there is a negative correlation with the effective diameter and radiation dosage as depicted by the study of Anam et al[18] whereas the dose increases the head size or effective diameter decreases. Hence, it can be said that these are practically inversely proportional to each other.
We found that SSDE is a much more practical method for dose estimation rather than CTDI vol as it is similar in most of the cases and not tailored to the individual patient (Table 5). Barreto et al[19] found that the value of SSDE is much different for every patient.
The P value for the variables is less than 0.05 as shown in Table 6 with mean and standard deviation for SSDE calculated and displayed varying by a factor of around 5 mGy which can cause great difference in risk estimation for head CT examination based on radiation exposure, causing misleading results in risks of mainly stochastic effects and radiation absorbed by the eye lens.
As depicted in Figure 3, the effective diameter is more aligned with the calculated dose while there is noticeably more scattering in case of displayed dose as the calculated dose take into account the effective diameter it is more specific for individuals. Also, the range of dose is higher in calculated dose which indicates that displayed doses are less reliable for risk estimation.
Now that we have a clear understanding of dose under estimation by the machine, we need to be extra careful for the dose limitation factors which can be handled manually such as collimation, scan length, pitch etc. to prevent patients from excessive radiation exposure.
This study was conducted on a single 128-slice Philips CT scanner at one tertiary care center, which may limit the generalizability of the findings to other vendors and lower-slice CT systems. One observer conducted effective diameter measurements, and inter-rater reliability was not evaluated, potentially introducing observer-dependent variability. Furthermore, subgroup analyses based on gender, age, and contrast use were constrained by the small sample size, and quantitative image quality parameters were not assessed.
Multicenter, multi-vendor studies with larger and more varied populations should be a part of future research. The robustness of SSDE estimation will be increased by combining automated measurement techniques or multi-observer techniques with quantitative image quality evaluation. To improve dose accuracy and patient safety, it is advised to conduct routine institutional audits that include recurring manual SSDE verification and closer coordination with manufacturers to align dose-reporting software with AAPM TG-204 guidelines.
The calculated radiation dose was found to be higher than the displayed dose i.e., SSDE. However, it is already mentioned in the AAPM report 204 that the variation of 10-20 percent is likely to occur. Our results align well with the range with the variation of -11.99 percent in SSDE values for calculated and displayed. The percentage is negative as the calculated dose is higher than the displayed dose. The effective dose is ranged between 1-2 mSv i.e., the mean effective dose is found to be 1.83 ± 0.21 as the dose reference level provided by the competent authorities for CT Head exami
We would like to express our sincere gratitude to the entire team of Department of Radiology and Imaging Techniques UPUMS Saifai, Etawah (U.P.)-206130 India.
| 1. | Boone JM, Brink JA, Edyvean S, Huda W, Leitz W, Mccollough CH, Mcnitt-Gray MF. Report 87. J Int Comm Radiat Units Meas. 2012;12. [DOI] [Full Text] |
| 2. | Park JE, Choi YH, Cheon JE, Kim WS, Kim IO, Cho HS, Ryu YJ, Kim YJ. Image quality and radiation dose of brain computed tomography in children: effects of decreasing tube voltage from 120 kVp to 80 kVp. Pediatr Radiol. 2017;47:710-717. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 26] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 3. | Charles MW. ICRP Publication 103: Recommendations of the ICRP. Radiat Prot Dosim. 2007;129:500-507. [DOI] [Full Text] |
| 4. | Rydberg J, Buckwalter KA, Caldemeyer KS, Phillips MD, Conces DJ Jr, Aisen AM, Persohn SA, Kopecky KK. Multisection CT: scanning techniques and clinical applications. Radiographics. 2000;20:1787-1806. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 267] [Cited by in RCA: 199] [Article Influence: 7.7] [Reference Citation Analysis (1)] |
| 5. | IAEA. Radiation Protection and Safety of Radiation Sources: International Basic Safety Standards. Vienna, Austria: International Atomic Energy Agency, 2014. [DOI] [Full Text] |
| 6. | Kayun Z, Abdul Karim MK, Harun HH, Shaari AH, Mahmud R, Hamid HA, Sabarudin A, Chew MT. Radiation doses and size-specific dose estimate from CT brain examinations according to head sizes in a tertiary hospital in Malaysia. Radiat Phys Chem. 2021;189:109694. [RCA] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 6] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 7. | Boone J, Strauss K, Cody D, Mccollough C, Mcnitt-Gray M, Toth T, Goske M, Frush D. Size-Specific Dose Estimates (SSDE) in Pediatric and Adult Body CT Examinations. 2011. [DOI] [Full Text] |
| 8. | Sookpeng S, Martin CJ, Butdee C. A Study to Determine Whether the Volume-Weighted Computed Tomography Dose Index Gives Reasonable Estimates of Organ Doses for Thai Patients Undergoing Abdomen and Pelvis Computed Tomography Examinations. J Med Phys. 2017;42:266-272. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 9. | Gabusi M, Riccardi L, Aliberti C, Vio S, Paiusco M. Radiation dose in chest CT: Assessment of size-specific dose estimates based on water-equivalent correction. Phys Med. 2016;32:393-397. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 30] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 10. | Berrington de Gonzalez A, Iulian Apostoaei A, Veiga LH, Rajaraman P, Thomas BA, Owen Hoffman F, Gilbert E, Land C. RadRAT: a radiation risk assessment tool for lifetime cancer risk projection. J Radiol Prot. 2012;32:205-222. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 91] [Cited by in RCA: 116] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 11. | National Research Council. Health Risks from Exposure to Low Levels of Ionizing Radiation: BEIR VII Phase 2. Washington: The National Academies Press, 2006. [DOI] [Full Text] |
| 12. | Trattner S, Pearson GDN, Cynthia Chin C, Cody DD, Gupta R, Hess CP, Kalra MK, Kofler JM, Krishnam MS, Einstein AJ. Standardization and Optimization of CT Protocols to Achieve Low Dose. J Am Coll Radiol. 2014;11:271-278. [RCA] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 70] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 13. | Nawfel RD, Young GS. Measured Head CT/CTA Skin Dose and Intensive Care Unit Patient Cumulative Exposure. AJNR Am J Neuroradiol. 2017;38:455-461. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 8] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 14. | Noferini L, Fulcheri C, Taddeucci A, Bartolini M, Gori C. Considerations on the practical application of the size-specific dose estimation (SSDE) method of AAPM Report 204. Radiol Phys Technol. 2014;7:296-302. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 12] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 15. | Sulemana H, Mumuni AN, Abubakari IOM. Establishment of baseline size-specific dose estimate (SSDE) for paediatric head computed tomography (CT) examinations. Egypt J Radiol Nucl Med. 2024;55:238. [DOI] [Full Text] |
| 16. | Zancopè N, De Monte F, Simeone E, Giannone A, Lombardi R, Mele A, Zorz A, Di Paola A, Causin F, Paiusco M. Validation of SSDE calculation in a modern CT scanner and correlation with effective dose. Sci Rep. 2025;15:6091. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 17. | El Mansouri M, Choukri A, Semghouli S, Talbi M, Eddaoui K, Saga Z. Size-Specific Dose Estimates for Thoracic and Abdominal Computed Tomography Examinations at Two Moroccan Hospitals. J Digit Imaging. 2022;35:1648-1653. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 18. | Anam C, Haryanto F, Widita R, Arif I, Dougherty G. A fully automated calculation of size-specific dose estimates (SSDE) in thoracic and head CT examinations. J Phys: Conf Ser. 2016;694:012030. [RCA] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 19. | Barreto I, Verma N, Quails N, Olguin C, Correa N, Mohammed TL. Patient size matters: Effect of tube current modulation on size-specific dose estimates (SSDE) and image quality in low-dose lung cancer screening CT. J Appl Clin Med Phys. 2020;21:87-94. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 6] [Article Influence: 1.0] [Reference Citation Analysis (0)] |