Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.114137
Revised: November 11, 2025
Accepted: December 29, 2025
Published online: February 27, 2026
Processing time: 165 Days and 23 Hours
Colitis cystica profunda (CCP) is a rare condition with multiple cystic lesions in the mucosal/submucosal layers, predominantly involving the rectum and sig
Herein, we report a 32-year-old man with a history of colonoscopy detection of two submucosal colonic elevations (20 cm and 18 cm from the anal verge) 2 weeks ago, without any disturbing symptoms. Endorectal ultrasound showed two cystic masses in the sigmoid’s intrinsic muscular and submucosal layers. Computed tomography showed rectosigmoid thickening. We performed a laparoscopic ope
CCP is rare and the clinical symptoms are not typical, and pre-operative diagnosis is difficult. Histopathology is required for definitive diagnosis. Surgical excision is widely reported as the surgical treatment of choice for CCP.
Core Tip: Colitis cystica profunda is a rare, benign but easily misdiagnosed cystic mucin-filled lesion that favors the recto-sigmoid wall, may be clinically silent or masquerade as mucinous neoplasm, and can only be confidently distinguished from malignancy by histopathologic examination of the fully excised specimen, so complete surgical removal and thorough pathologic assessment remain the cornerstone of management.
- Citation: Zhao T, Jia XR, Li KJ, Zheng WF, Liu XJ. Colitis cystica profunda diagnosed by laparoscopic excision: A case report and review of literature. World J Gastrointest Surg 2026; 18(2): 114137
- URL: https://www.wjgnet.com/1948-9366/full/v18/i2/114137.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i2.114137
Colitis cystica profunda (CCP) is an uncommon benign condition of the colon and rectum that can be mistaken for suspicious polyps, mucinous adenocarcinomas, or carcinoid tumors, with few cases reported in the literature[1]. Stark first documented submucosal cysts in the colon in 1766 while performing autopsies on two patients suffering from chronic dysentery. Virchow introduced the term colitis cystica polyposa to describe multiple polypoid cystic submucosal lesions 1863. Goodall and Sinclair changed the name to CCP and finalized the terminology in 1957[2]. Its etiology is not entirely clear, with many experts suggesting inflammatory, ischemic, and post-traumatic processes as contributing factors[3]. CCP is an uncommon benign lesion occurring in the rectum or colon, most commonly located in the anterior rectal wall. Its key pathological trait lies in mucus-filled cysts that extend into the submucosa, muscular layer, or even the serous layer. These cysts contain substantial amounts of mucus and lack the hallmarks of malignant neoplasms[4]. Few case reports on ultrasonography of CCP have been previously published in the literature.
We conducted a literature search of case reports of CCP published from 1955 to 2025. The keywords searched included “colitis cystica profunda”, “submucosal cysts of the colon”, and “heterotopic submucosal colon glands”. We also reported a retrospective case from our group and compared it with cases from the existing literature.
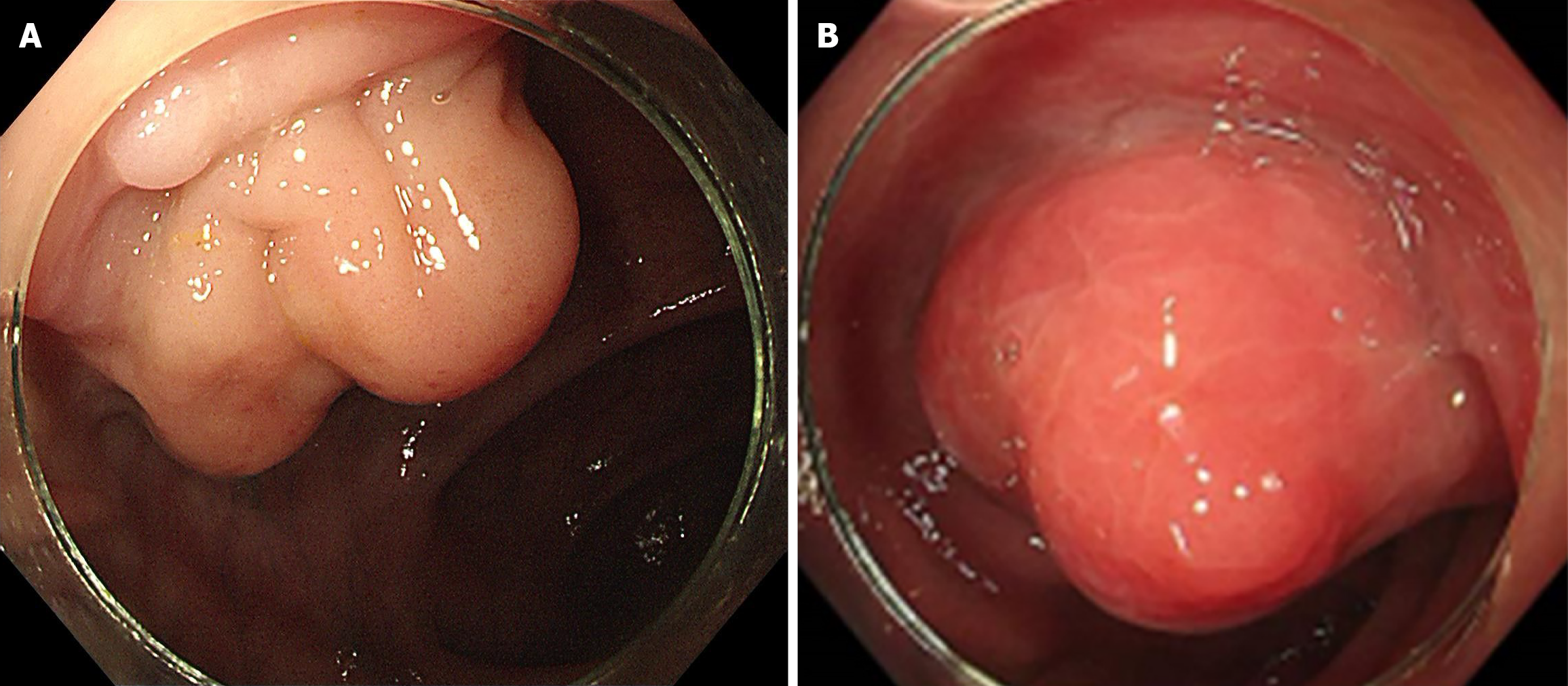
A 32-year-old man presented for consultation with a history of colonoscopy detection of two submucosal colonic elevations (20 cm and 18 cm from the anal verge) 2 weeks ago (Figure 1) without any disturbing symptoms.
The patient reported no specific complaints or discomfort.
The patient denies a history of diabetes mellitus, tuberculosis, typhoid fever, malaria, heart disease, cerebrovascular disease, or mental illness. No history of trauma or surgery. Denies any food or drug allergies.
The patient denied any family history of malignant tumors.
Physical examination revealed stable vital signs, with a blood pressure of 126/69 mmHg, and pulse of 65/minute and no abnormal findings on abdominal and cardiac examination.
Levels of serum tumor (carbohydrate antigen 72-4, carbohydrate antigen 199, carcinoembryonic antigen) markers were normal. Other blood tests revealed no abnormalities.
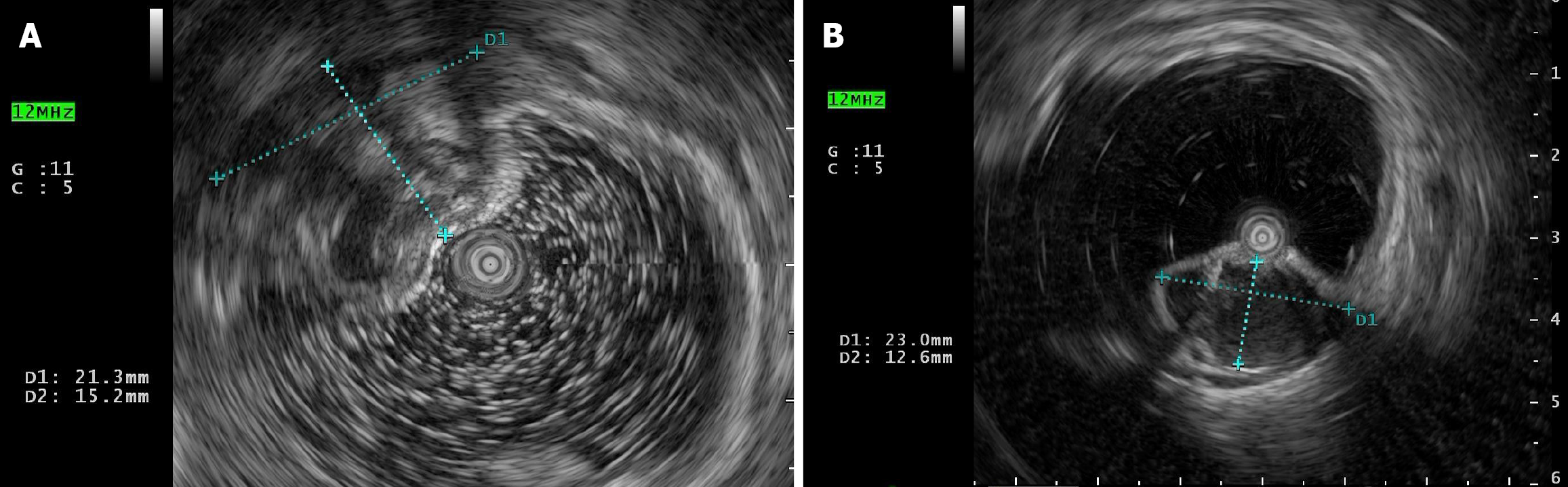
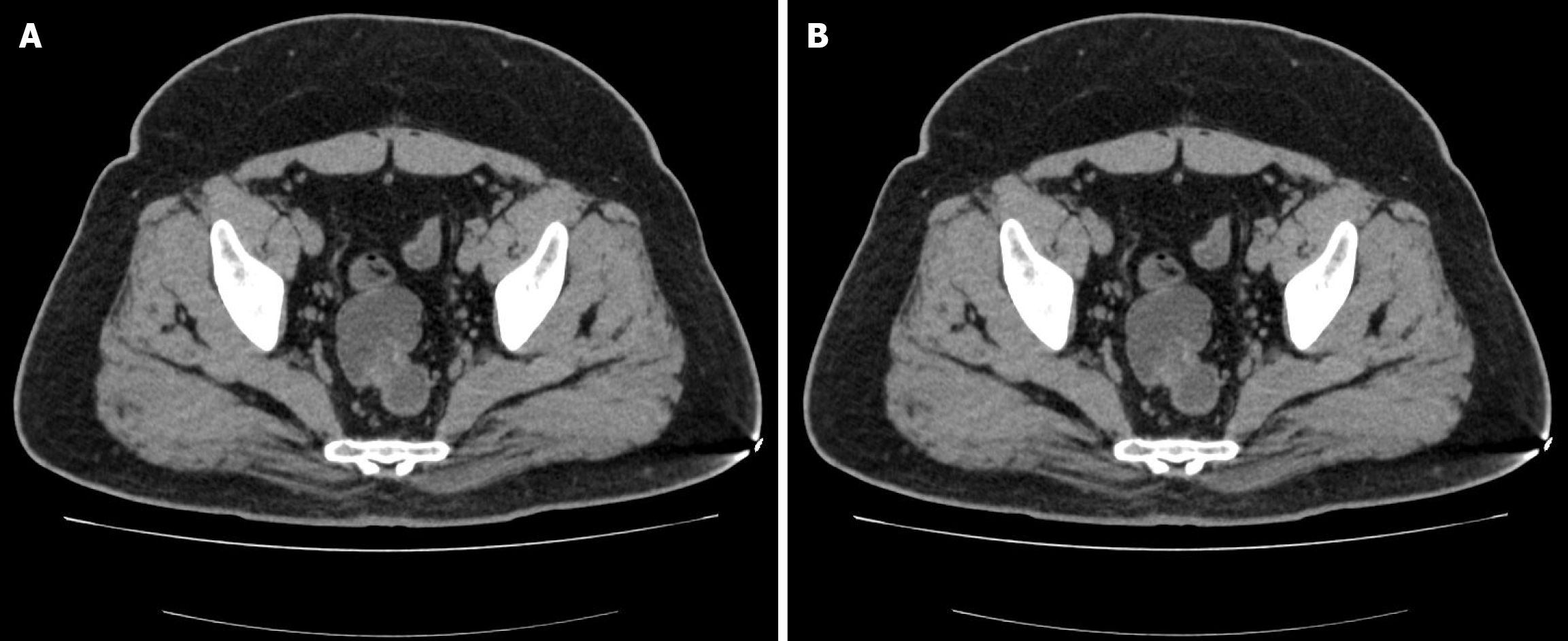
Colonoscopy revealed two large submucosal mass 20 cm and 18 cm from the anal verge (Figure 1). Endorectal ultrasound revealed two cystic mass was observed at the 20 o'clock direction in the left lateral position, in the intrinsic muscular layer and submucosal layer of the sigmoid, with a size of 23.0 mm × 12.6 mm and 21.3 mm × 15.2 mm in diameter, regular morphology, clear boundary, protruding into the lumen, with poor internal transmission and heterogeneous echogenicity or anechoic echogenicity (Figure 2). No abnormalities were found in the physical exam of the patient, and his laboratory tests, such as routine blood work and tumor markers, were within normal limits. Computed tomography (CT) scan of the abdomen displayed an irregular focal thickening of the rectosigmoid wall, with mild to moderate enhancement (Figure 3).
The patient was diagnosed with CCP.
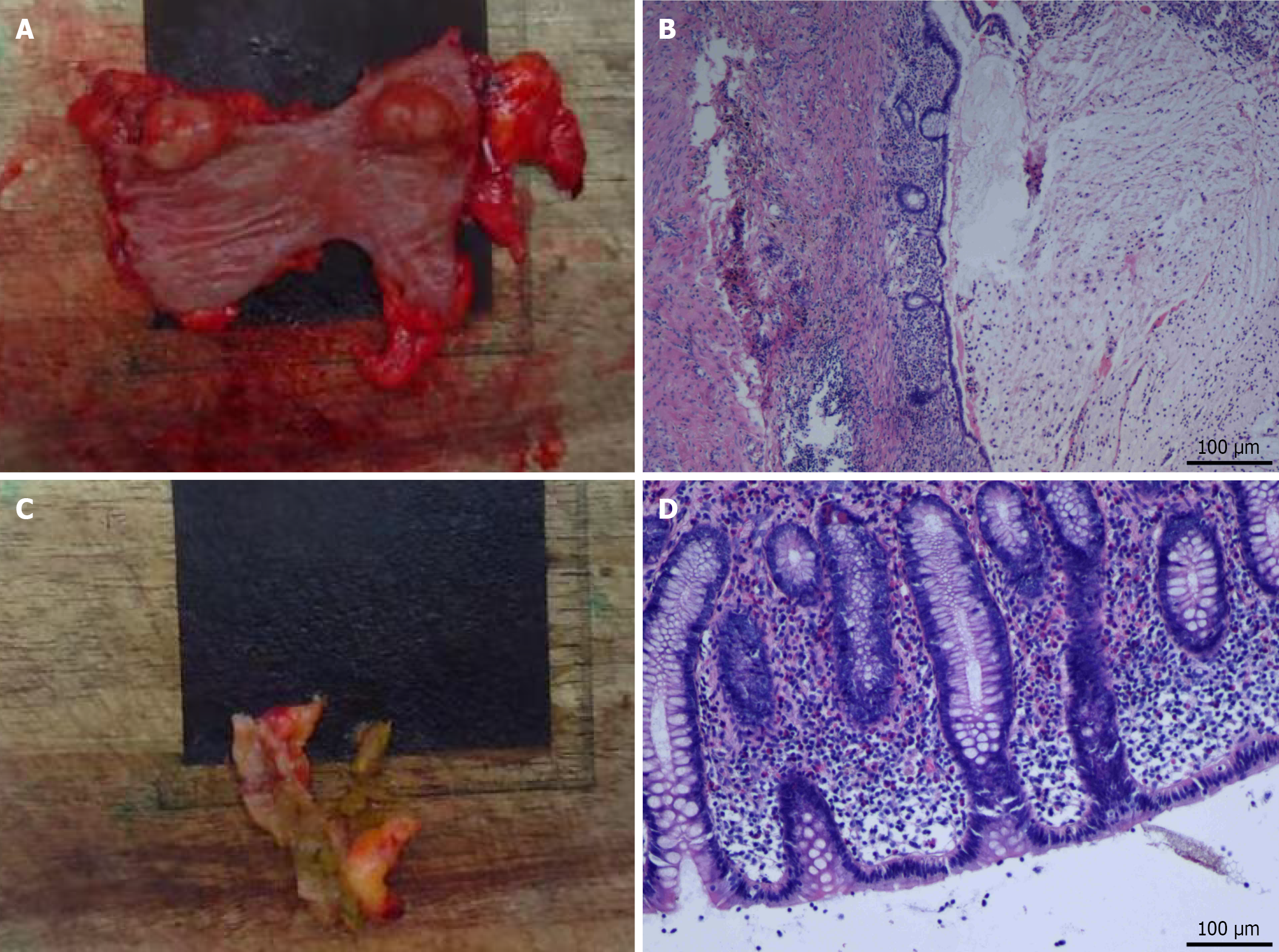
We suspected gastrointestinal stromal tumor. In conjunction with the patient willingness, we performed a laparoscopic operation to remove the lump. Pathological examination showed no abnormalities in the mucosa. The mass 20 cm from the anal was appeared soft and grayish-white, and showed obvious jelly-like changes, measured 2.5 cm × 2 cm × 1.7 cm. The pathological manifestations of the mass 18 cm from the anal was similar with the mass 20 cm from the anal, measured 2.5 cm × 1.8 cm × 1.5 cm (Figure 4A).
Intraoperative frozen-section pathology suggested low-grade mucinous neoplasms (Figure 4B). However, the low-grade mucinous neoplasms in most cases are from mucinous tumors arising from the appendix. Subsequently, com
The patient was discharged five days later and had follow-up visits with no signs of relapse for a period of 3 months.
Up to now, there have been 106 documented cases of CCP, not counting the one mentioned in this report. The clinical and treatment details for these cases are outlined in Table 1. In total, 106 cases were identified, including 66 men (62.3%) and 40 women (37.7%), with a male-to-female ratio of 1.65. The mean age of the patients was 39.1 (range, 5-82) years old. Among the cases, 57.5% (n = 61) of lesions were located in the rectum, 32.1% (n = 34) of lesions were located in the colon, one case of lesions was located in the junction of the rectum and sigmoid colon, 2.8% (n = 3) of lesions were located in the small intestine. The location of 2 cases was not described. In 5 patients, multiple lesions were in colon rectum and small intestine. Of the patients, 52% (n = 26) had previously received abdominal surgery. The main manifestations of CCP included mucus and bloody stool, abdominal pain, diarrhea and tenesmus. Of the 106 cases, only 7 were diagnosed before the surgical procedure, and the others were diagnosed through histopathologic examination after surgery.
| Ref. | Age | Sex | Lesion location | History of stomach surgery | Symptoms | Treatment |
| Epstein et al[11], 1966 | 55 | Female | Rectum | No | Hemafecia | Excision |
| Grant and Roller[12], 1967 | 23 | Female | Rectum | No | Hemafecia | Conservative |
| Sullivan et al[13], 1968 | 19 | Male | Rectum | No | Diarrhea, mucous stool, emaciation | Excision |
| Sullivan et al[13], 1968 | 23 | Male | Rectum | No | Diarrhea | Excision |
| Scruggs and Duckworth[14], 1968 | 31 | Female | Rectum | No | Rectal pain, hemafecia, tenesmus, hemorrhoids, mucopurulent bloody stool | Conservative |
| Scruggs and Duckworth[14], 1968 | 15 | Female | Rectum | No | Abdominal pain, tenesmus, diarrhea, mucopurulent bloody stool | Excision |
| Fechner[15], 1967 | 62 | Male | Colon | Laparotomy, colotomy, a segmental resection | Hemafecia | Excision |
| Barner[16], 1967 | 36 | Male | Colon transversum | No | Diarrhea, hemafecia, emaciation | Transverse colectomy, a double colostomy |
| Stolar and Silver[17], 1969 | 49 | Female | Rectum | Fistulotomy, biopsy | Mucopurulent bloody stool | Abdominoperineal resection |
| Ghani[18], 1970 | 31 | Male | Rectum | No | Mucopurulent bloody stool | Excision |
| Clark and Muldoon[19], 1970 | 60 | Female | Sigmoid colon | No | Diarrhea, hemafecia | Colotomy, transcolonic polypectomy |
| Burt et al[20], 1970 | 76 | Female | Sigmoid colon | Sigmoidoscopy, double mastoidectomy and hysteroscopy | Abdominal pain, mucopurulent bloody stool | The transverse colon with end-to-end anastomosis |
| O'Brien et al[21], 1971 | 65 | Male | Sigmoid colon | No | Mucopurulent bloody stool | A segmental resection of the sigmoid colon |
| Talerman[22], 1971 | 25 | Male | Rectum | No | Mucopurulent bloody stool | Excision |
| Ballas et al[23], 1971 | 27 | Male | Rectum | No | No symptoms | Excision |
| Young et al[24], 1972 | 17 | Male | Rectum | History of anal fissure surgery | Abdominal pain, hemafecia | Extensive local resection |
| Herman and Nabseth[25], 1973 | 36 | Male | Rectum | Cholecystectomy, appendectomy | Diarrhea, tenesmus | Colostomy |
| Green et al[26], 1974 | 25 | Female | Rectum | Hemorrhoidectomy, perianal condyloma acuminatum | Mucopurulent bloody stool, tenesmus | Excision |
| Farman et al[27], 1974 | 70 | Female | Sigmoid | Cholecystectomy | No symptoms | Laparotomy |
| Farman et al[27], 1974 | 23 | Male | Rectum | No | Rectal pain, hemafecia, diarrhea | Conservative |
| Farman et al[27], 1974 | 52 | Female | Rectum | No | Recurrent ventral hernia | Conservative |
| Lasser and Acosta[28], 1975 | 37 | Male | Sigmoid colon | Bilateral ureterosigmoidostomy | Confusion, weakness, lethargy, vomiting, metabolic acidosis | Partial colonic resection, ileal loop diversion |
| Friedman and Tueller[29], 1975 | 26 | Male | Rectum | No | Watery diarrhea | Corticosteroid enemas |
| Tedesco et al[30], 1976 | 36 | Male | Rectum | No | Mucopurulent bloody stool | Conservative |
| Tedesco et al[30], 1976 | 27 | Female | Rectum | No | Diarrhea, mucopurulent bloody stool | Local excision |
| Tedesco et al[30], 1976 | 31 | Female | Rectum | No | Diarrhea, rectal pruritus | Conservative |
| Tedesco et al[30], 1976 | 19 | Male | Descending colon and sigmoid colon | No | Mucopurulent bloody stool (history of ulcerative colitis) | Total colectomy |
| Tedesco et al[30], 1976 | 60 | Male | The junction of the descending and sigmoid colon | No | Diarrhea, abdominal pain | Endoscopic polypectomy, anterior colonic resection |
| Bhuta and Prathikanti[31], 1976 | 27 | Male | Rectum | No | Hemafecia, tenesmus, abdominal pain, vomiting | Wide local excision |
| Rosen et al[32], 1976 | 37 | Female | Colon | No | Abdominal gunshot wound | Colostomy |
| Nagasako et al[33], 1977 | 19 | Male | Rectum | No | Mucopurulent bloody stool | Abdominoperineal resection |
| Kyriakos and Condon[34], 1978 | 48 | Male | Ileum | Appendectomy side-to-side anastomosis of the jejune | Abdominal pain, abdominal distension, vomiting, diarrhea | Wedge resection of the jejunal segment |
| Baratz et al[35], 1978 | 57 | Male | Ileum, The ileocecal junction, colon | Right nephrectomy, radiotherapy for clear cell renal cell carcinoma | Astriction | Right hemicolectomy, ileotransverse anastomosis |
| Ledesma-Medina et al[36], 1978 | 13 | Female | Rectum | No | Type I rectal prolapse with bleeding | Excision |
| Shinohara et al[37], 1981 | 49 | Male | Rectum | No | Diarrhea, astriction, rectal pain, anal bleeding | Perineal rectal resection |
| Magidson and Lewin[38], 1981 | 20 | Male | Sigmoid colon | No | Mucopurulent bloody stool | Total proctocolectomy |
| Krummel et al[39], 1983 | 14 | Male | Rectum | No | Anal pain, tenesmus, hemafecia | Excision |
| Suzuki and Matsumoto[40], 1983 | 14 | Male | Rectum | No | Diarrhea, hemafecia | Extirpation of the polyp |
| Suzuki and Matsumoto[40], 1983 | 15 | Female | Rectum | No | Mucopurulent bloody stool | Conservative |
| Nielsen et al[41], 1984 | 33 | Male | No | No | Mucopurulent bloody stool (history of ulcerative colitis) | Conservative |
| Gardiner et al[42], 1984 | 55 | Female | Colon | Radiotherapy for squamous carcinoma of the cervix (stage A), cholecystectomy | Bloody diarrhea, abdominal distension | Resection of the sigmoid colon with primary anastomosis, defunctioning transverse loop colostomy |
| Yashiro et al[43], 1985 | 70 | Male | Sigmoid colon | No | Follow-up study | Polyp removal and surgery |
| Bentley et al[44], 1985 | 52 | Male | Sigmoid colon | Decompression loop colostomy of the transverse colon, total colectomy + cecal sigmoid anastomosis | Abdominal pain, fever, hemafecia, mucoid loose stools, vomiting | Abdominal perineal resection, Koch ileostomy |
| Walker et al[45], 1986 | 36 | Male | Rectum | Splenectomy | Abdominal pain, hemafecia, marasmus, mucoid loose stools | Rectal resection |
| Spjut et al[46], 1987 | 39 | Male | Colon transversum jejunum | History of duodenal ulcer | Abdominal distension, rectal bleeding | Segmental resection of the transverse colon |
| Guy and Hall[47], 1988 | 17 | Male | Rectum | No | Astriction, diarrhea, rectal bleeding, tenesmus | Mucosal sleeve resection |
| Hulsmans et al[48], 1991 | 48 | Male | Rectum | No | No | Conservative |
| Kim et al[49], 1992 | 31 | Male | Transverse colon | No | Hemafecia | Segmental resection with end-to-end anastomosis of the descending colon |
| Zidi et al[50], 1994 | 48 | Female | Anterior wall of rectum, sigmoid transverse colon | Transabdominal rectopexy, diverting transverse colostomy | Hemafecia | Sigmoidectomy, low-sited colorectal anastomosis |
| Heusinkveld and Barnard[51], 1994 | 13 | Male | Rectum | No | Hemafecia | Rectal resection |
| Lifshitz et al[52], 1994 | 37 | Female | Rectum | No | Hemafecia | Transanal local excision |
| Valenzuela et al[53], 1996 | 30 | Female | Rectum | No | Mucopurulent bloody stool | Conservative |
| Valenzuela et al[53], 1996 | 45 | Male | Rectum | No | Abdominal pain, tenesmus, mucopurulent bloody stool | Conservative |
| Petritsch et al[54], 1996 | 30 | Male | No | Mucopurulent bloody stool | EMR | |
| Petritsch et al[54], 1996 | 27 | Male | Rectum | No | Presented with rectal polyps for consultation | Conservative |
| Karnak et al[55], 1997 | 5 | Male | 100 cm distal to the ligament of Trietze and 120 cm proximal to the ileocecal valve | No | Abdominal pain, fever, biliary vomiting, ileal intussusception | Partial ileal segment resection and ileoileal anastomosis |
| Sakurai et al[56], 2000 | 53 | Male | Colon transversum | No | Ulcerative colitis | Transverse colectomy |
| Wang et al[57], 2001 | 73 | Male | Rectum | Spinal cord injury | Mucopurulent bloody stool | Transverse colostomy |
| Wang et al[57], 2001 | 47 | Male | Rectum | Spinal cord injury | Mucopurulent bloody stool | Mesalamine enemas |
| Wang et al[57], 2001 | 75 | Male | 40 cm from the anal margin | Spinal cord injury | Irregular bowel movements, fecal incontinence | Left hemicolectomy and transverse colostomy |
| Madan and Minocha[58], 2002 | 37 | Male | Sigmoid colon | Multiple sclerosis | Bloody diarrhea, abdominal pain, bile vomiting | Sigmoidectomy and end colostomy |
| Krüger et al[59], 2005 | 39 | Female | Colon transversum | Crohn’s disease | Recurrent of bowel obstruction | Partial left hemicolectomy |
| Kayaçetin and Kayaçetin[60], 2005 | 18 | Male | Rectum | No | Mucopurulent bloody stool, tenesmus, fatigue | Anterior resection with a protective colostomy, closure of the colostomy |
| Sarzo et al[61], 2005 | No | Female | Rectum, sigmoid colon | No | Mucopurulent bloody stool | Anterior resection of the sigmoid colon and upper rectum |
| Dewandel et al[62], 2001 | 39 | Female | Colon descendens | No | Abdominal pain, diarrhea | Excision |
| Inan et al[63], 2007 | 16 | Male | Rectum | No | Mucopurulent bloody stool, tenesmus | EMR |
| Sztarkier et al[64], 2006 | 64 | Female | Rectum | No | Hemafecia, ulcerative proctitis | Full-thickness transanal excision |
| Tajika et al[65], 2007 | 48 | Male | Colon descendens | No | Positive fecal occult blood experiment | Right hemicolectomy |
| Kornprat et al[66], 2007 | 48 | Female | Rectum | No | Astriction, rectal pain, rectal prolapse | Perineal proctectomy (altemeier procedure) |
| Laurent et al[67], 2007 | 66 | Male | Rectum | Anorectal dysfunction resulting from a history of spinal surgery | Anal mass with prolapse, astriction, tenesmus | EMR |
| de Toro et al[68], 2007 | 35 | Female | Sigmoid colon | Postoperative radiotherapy and chemotherapy for cervical cancer | Abdominal pain, vomiting | Proximal sigmoid colostomy |
| Dolar et al[69], 2007 | 44 | Male | Rectum | No | Mucopurulent bloody stool tenesmus, rectal incontinence and prolapse | Low anterior resection with colon-anal anastomosis |
| Higuera Alvarez et al[70], 2008 | 50 | Male | Ileum, sigmoid, colon transversum, caecum | No | Anorexia, weight loss, perianal abscess | Conservative |
| Toll and Palazzo[71], 2009 | 16 | Male | Colon | No | Ulcerative colitis | Proctocolectomy |
| Fernández Salazar et al[72], 2009 | 70 | Male | Sigmoid colon | No | Diarrhea, abdominal pain, weight loss, anemia, ulcerative colitis | Colectomy |
| Baltar-Arias et al[73], 2010 | 63 | Female | Rectum | No | Mucopurulent bloody stool | Conservative |
| Jung et al[74], 2010 | 38 | Male | Sigmoid | History of polypectomy of the colon | Hemafecia | EMR |
| Qayed et al[75], 2011 | 42 | Male | Sigmoid colon | No | Abdominal pain, fever with chills, hemafecia, vomiting | Sigmoid colectomy and descending colostomy |
| Arana et al[76], 2014 | 49 | Male | The junction of the rectum and sigmoid colon | No | Mucopurulent bloody stool, ulcerative colitis | Total proctosigmoidectomy with preservation of the anus and terminal ileostomy |
| Sultan et al[77], 2014 | 27 | Male | Rectum | No | Hemafecia | Conservative |
| Cecinato et al[78], 2014 | 39 | Male | Colon descendens | No | Colonoscopy follow-up (history of ulcerative colitis) | Segmental colectomy |
| Shin et al[79], 2014 | 65 | Male | Sigmoid colon | No | Colonoscopy follow-up | EMR |
| Hernandez-Prera and Polydorides[80], 2014 | 46 | Female | Colon | No | Abdominal pain, astriction, vomiting (history of Crohn’s disease) | Partial colectomy with end-to-end anastomosis |
| Lord et al[3], 2015 | 28 | Female | Rectum | No | Astriction, hemafecia, full-thickness rectal prolapse | Laparoscopic surgery and ileostomy |
| Wang et al[8], 2015 | 29 | Female | Rectum | No | Abdominal pain | ESD |
| Spicakova et al[6], 2017 | 45 | Male | Rectum | No | Mucopurulent bloody stool (family history of ulceration) | Low anterior resection and prophylactic appendectomy |
| Spicakova et al[6], 2017 | 16 | Female | Rectum | No | Hemafecia, astriction | Conservative |
| Ayantunde et al[1], 2016 | 34 | Female | Rectum | No | Tenesmus, mucopurulent bloody stool | Complete dissection from the submucosa is achieved through a vertical mucosal incision |
| Masood et al[7], 2018 | 21 | Male | Rectum | No | Hemafecia, weight loss | Laparoscopic surgery and ileostomy |
| Jeruc et al[81], 2019 | 32 | Male | Colon | No | Mucopurulent bloody stool (history of Crohn’s disease) | Total colectomy |
| Rumi et al[9], 2019 | 65 | Female | Rectum | No | Mucopurulent bloody stool, tenesmus | Anterior resection of the rectum |
| Abe et al[82], 2021 | 48 | Male | Rectum | No | Hemafecia (intellectual disability, frequently inserting fingers into the anus after defecation) | ESD |
| Zhou et al[83], 2021 | 14 | Male | Colon transversum | No | Hemafecia, diarrhea, iron-deficiency anemia (history of Crohn’s disease) | Partial colectomy |
| Zaki et al[5], 2022 | 58 | Male | Rectum | No | Diarrhea | Surgical resection |
| Chen et al[10], 2023 | 62 | Male | Rectum | Cholecystectomy | Rectal submucosal eminence | ESD |
| Suter and Skinner[84], 2023 | 25 | Female | Rectum | No | Hemafecia | EMR |
| Zhang et al[85], 2023 | 14 | Male | Rectum | Transanal resection of the rectal lesions | Hemafecia | Conservative |
| Jiang et al[4], 2023 | 34 | Male | Rectum | No | Mucous defecation | EMR |
| Jiang et al[4], 2023 | 27 | Female | Rectum | No | Mucopurulent bloody stool, tenesmus | EMR |
| Bhagwanani et al[86], 2023 | 49 | Female | Rectum | No | Rectal prolapse | Surgical resection |
| Denis et al[87], 2024 | 72 | Female | Colon | Sigmoid colectomy for colon cancer (stage T2N0) | Asymptomatic | Right hemicolectomy |
| Chebbo et al[88], 2024 | 29 | Female | Sigmoid colon | Appendicectomy | Abdominal pain, hemafecia | EMR |
| Rosano et al[89], 2024 | 65 | Female | Sigmoid colon | No | Abdominal pain, diverticulosis (family history of colon cancer, history of atrial fibrillation) | Laparoscopic sigmoidectomy |
| Früh et al[90], 2024 | 82 | Female | 50 cm from the anal margin | No | Hemafecia | Loop excision |
| Guduguntla et al[91], 2025 | 20 | Female | Rectum | No | Hemafecia (family history of colon cancer) | No |
| Zhou et al[92], 2025 | 48 | Male | Colon descendens | No | A mass in the descending colon mucosa | ESD |
CCP is a rare and non-cancerous condition marked by several mucus-filled submucosal cysts, typically found in the rectum and sigmoid colon[4]. In medical literature, fewer than 200 cases have been documented. The most common symptoms of CCP include altered bowel habits, rectal tenesmus, hematochezia, mucus secretion in feces, and obstructive defecation. However, the reported patient had no symptoms and were detected incidentally at a medical check-up. Both lesions have approximately the same diameter and histopathological findings, which is very rare. This is inconsistent with previous studies.
The underlying causes of CCP are not fully understood, but a weakness in the mucosal wall, whether congenital or acquired, is thought to be a factor in its development. This vulnerability may be induced by infection, inflammation, ischemia, or trauma, leading to the implantation of mucosal epithelium into the submucosa[4]. There are diffuse and localized types, depending on the level of invasion[5]. In the diffuse type, the entire colon is involved and characterized by ulcers or villous or polypoid lesions, mainly due to intestinal inflammation and ulceration, which is associated with Crohn’s disease, infectious colitis, ulcerative colitis, and radiation enteritis[4]. The local type is mainly observed in the anterior wall of the rectum, manifesting as nodules or polyps. It is associated with rectal prolapse and isolated rectal ulcer syndrome. The literature shows that the local type is the mostly frequent, with the diffuse type comprising less than 15% of cases[6]. A young patient in this study presented with mucous excretion as a clinical manifestation. Located 18-20 cm from the anal verge on the anterior rectal wall, the lesion exhibited nodularity and was classified as the local type, consistent with prior research findings.
With advances in endoscopic ultrasonography (EUS) technology, this method is crucial for pre-surgical diagnosis. It has been reported that there are three main forms of CCP in EUS: (1) Anechoic; (2) Mixed echoic; and (3) Hypoechoic. Under EUS, the typical imaging features of CCP were that the lesions originated from the mucosa or submucosa, and gradually extended to the submucosa or muscularis propria. The echoic area is observed with no color flow imaging. The primary differential diagnosis is mucinous carcinoma, which showed abundant blood flow signal. EUS enables clear identification of the intestinal wall’s distinct layers and assessment of the integrity of the mucosal, muscularis propria, and serosal layers. While EUS cannot definitively diagnose, it is crucial to rule out malignant tumors. Moreover, EUS can be repeated as a follow-up examination. EUS remains there commended as a follow-up management examination. It is easy to perform safe, noninvasive, nonradioactive and well tolerated. In this study, EUS revealed submucosal cystic lesions in both cases, with intact mucosal and serous layers. On CT, CCP manifests as a non-infiltrating submucosal mass with well-defined borders and variable-sized cystic lumens[4]. Magnetic resonance imaging showed low signal on T1-weighted imaging, a submucosal high-signal nodule on T2-weighted imaging, no obvious enhancement on contrast-enhanced sequences, high signal on diffusion-weighted imaging, no diffusion restriction on apparent diffusion coefficient, and marked high signal on T2-weighted imaging - consistent with mucin-containing lesions[7]. Even though colonoscopy provide the benefit of taking biopsies, misdiagnosis can occur when the biopsy depth is limited and the sampling is not enough[4]. Wang et al[8] reported viscous yellow fluid was seen flowing from the lesion during endoscopic resection. Examination of shed showed the presence of neutrophils, lymphocytes, columnar epithelial cells and squamous cells. In our case, the yellow fluid was aspirated by an assistant, and the surgeries were completed uneventfully. This is similar to the study by Wang et al[8]. Ultimately, the definite diagnosis of CCP was eventually determined based on the operative findings and postoperative pathology.
Histologically, CCP is identified as a nonmalignant lesion with submucosal cysts filled with mucin of various sizes, covered by epithelium without atypical cells, extending under the muscularis mucosa and intruding into the muscularis propria in many instances. Moreover, the connective tissue around the lesion may also display signs of chronic inflammation and fibrosis[9].
The main differential diagnosis is benign or malignant colorectal tumors (adenomatous polyps, polypoid inflammatory granulomas, leiomyomas, lipomas, sarcomas, adenocarcinomas, mucinous carcinomas) and inflammatory bowel disease (Crohn's disease, ulcerative colitis and ischemic colitis or proctitis)[5]. Interestingly, intraoperative frozen-section pathology of the patient suggested low-grade mucinous neoplasms. However, the low-grade mucinous neoplasms in most cases are from mucinous tumors arising from the appendix. Subsequently, the patient underwent an appendectomy. The results were described as simple appendicitis. This result differs from the one we imagined. Finally, the conclusion was reached after discussion by the pathologists. This is not low-grade mucinous neoplasms. Ultimately, the patient was diagnosed with CCP. Thus, the differential diagnosis is important.
The treatment of CCP aims to alleviate symptoms. The first step is conservative management with a high-fiber diet and lifestyle changes to avoid constipation and straining during bowel movements. In many instances, conservative treatment is ineffective, requiring surgical intervention for severe bowel obstruction, rectal prolapse, and bleeding. Recently, the use of endoscopic submucosal dissection has become widespread due to its benefits of quick healing, minimal damage, and maintaining colonic integrity[4,10]. In our case, the risk of perforation by endoscopic treatment was concerned. The patient declined any endoscopic therapy, and thus, laparoscopic excision was pursued. Actually, if endoscopic removal fails, surgery is warranted.
In summary, it is crucial to identify CCP. Once misdiagnosed, it causes patients to perform unnecessary painful surgeries and brings risks to physicians. It is especially vital for appendectomy patients. Meanwhile, imaging studies with CT and magnetic resonance imaging and EUS significantly contribute to disease detection and the differentiation of malignant conditions, but also limited. Thus, further research is required to distinctly identify and differentiate CCP from other similar conditions.
| 1. | Ayantunde AA, Strauss C, Sivakkolunthu M, Malhotra A. Colitis cystica profunda of the rectum: An unexpected operative finding. World J Clin Cases. 2016;4:177-180. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 6] [Cited by in RCA: 8] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 2. | Papalampros A, Vailas MG, Sotiropoulou M, Baili E, Davakis S, Moris D, Felekouras E, Deladetsima I. Report of a case combining solitary Peutz-Jeghers polyp, colitis cystica profunda, and high-grade dysplasia of the epithelium of the colon. World J Surg Oncol. 2017;15:188. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 6] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 3. | Lord A, Hompes R, Arnold S, Venkatasubramaniam A. Ultra-low anterior resection with coloanal anastomosis for recurrent rectal prolapse in a young woman with colitis cystica profunda. Ann R Coll Surg Engl. 2015;97:e32-e33. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 4. | Jiang Q, Qin S, Zhang H, Liu G. Colitis cystica profunda: A report of two cases. Clin Case Rep. 2023;11:e8042. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 5. | Zaki TA, Mbah M, Mir M, Sims RD, Amin A, Shah SL. Colitis Cystica Profunda: A Rare Mimicker of Colorectal Neoplasia. Dig Dis Sci. 2022;67:2693-2695. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 6. | Spicakova K, Pueyo BA, de la Piscina PR, Urtasun L, Ganchegui I, Campos A, Estrada S, García-Campos F. Colitis cystica profunda: A report of 2 cases with a 15-year follow-up. Gastroenterol Hepatol. 2017;40:406-408. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 7] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 7. | Masood L, Sayeed S, Asghar M. MRI Appearances of Colitis Cystica Profunda: A Rare Benign Mimicker of Colorectal Malignancy. J Coll Physicians Surg Pak. 2018;28:S162-S163. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 8. | Wang LB, He C, Tang TY, Xu H. Multi-Colitis Cystica Profunda: A Case Report. Chin Med J (Engl). 2015;128:3254-3255. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 9. | Rumi N, Cilla S, De Ninno M, Berardi S, Spera G, D'amico R, Rotondi F, Sallustio G, Pierro A. Colitis cystica profunda of the rectum with adenomatous dysplastic features: Radiologic-pathologic correlation. Radiol Case Rep. 2019;14:740-745. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 7] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 10. | Chen G, Jiang W, Yue M. Colitis cystica profunda of the rectum diagnosed by endoscopic submucosal dissection. Rev Esp Enferm Dig. 2023;115:91-92. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 11. | Epstein SE, Ascari WQ, Ablow RC, Seaman WB, Lattes R. Colitis cystica profunda. Am J Clin Pathol. 1966;45:186-201. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 100] [Cited by in RCA: 72] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 12. | Grant KB, Roller GJ. Colitis cystica profunda. A lesion of increasing significance to radiologists and pathologists. Radiology. 1967;89:100-111. [PubMed] |
| 13. | Sullivan JJ, Friend WD, Lee JF. Localized submucosal mucous cysts of the rectum (colitis cystica profunda). Med J Aust. 1968;1:133-135. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 14. | Scruggs FL, Duckworth JK. Colitis cystica profunda. South Med J. 1968;61:619-620. [PubMed] |
| 15. | Fechner RE. Polyp of the colon possessing features of colitis cystica profunda. Dis Colon Rectum. 1967;10:359-364. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 16] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 16. | Barner JL. Colitis cystica profunda. Radiology. 1967;89:435-437. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 9] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 17. | Stolar J, Silver H. Differentiation of pseudoinflammatory colloid carcinoma from colitis cystica profunda. Dis Colon Rectum. 1969;12:63-66. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 18. | Ghani A. Colitis cystica profunda. Br J Surg. 1970;57:596-598. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 7] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 19. | Clark JF, Muldoon JP. Colitis cystica profunda in an adenoma (adenomatous polyp): report of a case. Dis Colon Rectum. 1970;13:387-389. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 14] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 20. | Burt CA, Handler BJ, Haddad JR. Colitis cystica profunda concurrent with and differentiated from mucinous adenocarcinoma: report of a case. Dis Colon Rectum. 1970;13:460-469. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 17] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 21. | O'Brien SE, Shier KJ, Tuttle RJ. Colitis cystica profunda: a rare lesion of the colon. Can J Surg. 1971;14:53-55. [PubMed] |
| 22. | Talerman A. Enterogenous cysts of the rectum (colitis cystica profunda). Br J Surg. 1971;58:643-647. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 13] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 23. | Ballas M, Nunez L, Miller EM. Localized colitis cystica profunda. Arch Surg. 1971;103:406-408. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 8] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 24. | Young VT, Miller CF, Broady JL, Beals DF. Diagnostic features of colloid adenocarcinoma of anal ducts and colitis cystica profunda. South Med J. 1972;65:1035-1039. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 4] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 25. | Herman AH, Nabseth DC. Colitis cystica profunda: localized, segmental, and diffuse. Arch Surg. 1973;106:337-341. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 19] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 26. | Green GI, Ramos R, Bannayan GA, McFee AS. Colitis cystica profunda. Am J Surg. 1974;127:749-752. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 15] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 27. | Farman J, Dallemand S, Robinson T, Keohane MF. Colitis cystica profunda, an unusual solitary tumor: Report of three cases. Dis Colon Rectum. 1974;17:565-569. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 6] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 28. | Lasser A, Acosta AE. Colonic neoplasms complicating ureterosigmoidostomy. Cancer. 1975;35:1218-1222. [PubMed] [DOI] [Full Text] |
| 29. | Friedman E, Tueller EE. Colitis cystica profunda: colonoscopic and pathological findings. Gastrointest Endosc. 1975;22:40-41. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 30. | Tedesco FJ, Sumner HW, Kassens WD Jr. Colitis cystica profunda. Am J Gastroenterol. 1976;65:339-343. [PubMed] |
| 31. | Bhuta I, Prathikanti V. Colitis cystica profunda. South Med J. 1976;69:495-496. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 9] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 32. | Rosen Y, Vaillant JG, Yermakov V. Submucosal mucous cysts at a colostomy site: relationship to colitis cystica profunda and report of a case. Dis Colon Rectum. 1976;19:453-457. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 6] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 33. | Nagasako K, Nakae Y, Kitao Y, Aoki G. Colitis cystica profunda: report of a case in which differentiation from rectal cancer was difficult. Dis Colon Rectum. 1977;20:618-624. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 9] [Article Influence: 0.2] [Reference Citation Analysis (1)] |
| 34. | Kyriakos M, Condon SC. Enteritis cystica profunda. Am J Clin Pathol. 1978;69:77-85. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 20] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 35. | Baratz M, Werbin N, Wiznitzer T, Rozen P. Irradiation-induced colonic stricture and colitis cystica profunda: report of a case. Dis Colon Rectum. 1978;21:75-79. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 13] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 36. | Ledesma-Medina J, Reid BS, Girdany BR. Colitis cystica profunda. AJR Am J Roentgenol. 1978;131:529-530. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 2] [Article Influence: 0.0] [Reference Citation Analysis (0)] |
| 37. | Shinohara Y, Yamashita S, Morimatsu M, Nakashima T, Fujiyoshi T. Colitis cystica profunda--report of a surgical case. Kurume Med J. 1981;28:177-180. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 0.0] [Reference Citation Analysis (0)] |
| 38. | Magidson JG, Lewin KJ. Diffuse colitis cystica profunda. Report of a case. Am J Surg Pathol. 1981;5:393-399. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 14] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 39. | Krummel TM, Bell S, Kodroff MB, Berman WF, Salzberg AM. Colitis cystica profunda: a pediatric case report. J Pediatr Surg. 1983;18:314-315. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 40. | Suzuki H, Matsumoto K. Colitis cystica profunda. J Pediatr Surg. 1983;18:964. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 41. | Nielsen OS, Søndergaard JO, Aru A. Colitis cystica profunda lokalisata. Acta Chir Scand. 1984;150:191-192. [PubMed] |
| 42. | Gardiner GW, McAuliffe N, Murray D. Colitis cystica profunda occurring in a radiation-induced colonic stricture. Hum Pathol. 1984;15:295-298. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 15] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 43. | Yashiro K, Murakami Y, Iizuka B, Hasegawa K, Nagasako K, Yamada A. Localized colitis cystica profunda of the sigmoid colon. Endoscopy. 1985;17:198-199. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 44. | Bentley E, Chandrasoma P, Cohen H, Radin R, Ray M. Colitis cystica profunda: presenting with complete intestinal obstruction and recurrence. Gastroenterology. 1985;89:1157-1161. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 8] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 45. | Walker JP, Wiener I, Rowe EB. Colitis cystica profunda: diagnosis and management. South Med J. 1986;79:1167-1170. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 8] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 46. | Spjut HJ, Helgason AH, Trabanino JG 2nd. Jejunitis cystica profunda in a hamartomatous polyp. Report of a case. Am J Surg Pathol. 1987;11:328-332. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 47. | Guy PJ, Hall M. Colitis cystica profunda of the rectum treated by mucosal sleeve resection and colo-anal pullthrough. Br J Surg. 1988;75:289. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 8] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 48. | Hulsmans FJ, Tio TL, Reeders JW, Tytgat GN. Transrectal US in the diagnosis of localized colitis cystica profunda. Radiology. 1991;181:201-203. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 18] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 49. | Kim WH, Choe GY, Kim YI, Kim JP. Localized form of colitis cystica profunda--a case of occurrence in the descending colon. J Korean Med Sci. 1992;7:76-78. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 50. | Zidi SH, Marteau P, Piard F, Coffin B, Favre JP, Rambaud JC. Enterocolitis cystica profunda lesions in a patient with unclassified ulcerative enterocolitis. Dig Dis Sci. 1994;39:426-432. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 8] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 51. | Heusinkveld DC, Barnard JA 3rd. Colitis cystica profunda in a pediatric patient. J Pediatr Gastroenterol Nutr. 1994;18:395-398. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 1] [Article Influence: 0.0] [Reference Citation Analysis (0)] |
| 52. | Lifshitz D, Cytron S, Yossiphov J, Lelcuk S, Rabau M. Colitis cystica profunda: self-inflicted by rectal trauma? Report of a case. Dig Dis. 1994;12:318-320. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 53. | Valenzuela M, Martín-Ruiz JL, Alvarez-Cienfuegos E, Caballero AM, Gallego F, Carmona I, Rodríguez-Téllez M. Colitis cystica profunda: imaging diagnosis and conservative treatment: report of two cases. Dis Colon Rectum. 1996;39:587-590. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 12] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 54. | Petritsch W, Hinterleitner TA, Aichbichler B, Denk H, Hammer HF, Krejs GJ. Endosonography in colitis cystica profunda and solitary rectal ulcer syndrome. Gastrointest Endosc. 1996;44:746-751. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 7] [Article Influence: 0.2] [Reference Citation Analysis (1)] |
| 55. | Karnak I, Göğüş S, Senocak ME, Akçören Z, Hiçsönmez A. Enteritis cystica profunda causing ileoileal intussusception in a child. J Pediatr Surg. 1997;32:1356-1359. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 9] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 56. | Sakurai Y, Kobayashi H, Imazu H, Hasegawa S, Matsubara T, Ochiai M, Funabiki T, Mizoguchi Y. The development of an elevated lesion associated with colitis cystica profunda in the transverse colonic mucosa during the course of ulcerative colitis: report of a case. Surg Today. 2000;30:69-73. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 3] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 57. | Wang F, Frisbie JH, Klein MA. Solitary rectal ulcer syndrome (colitis cystica profunda) in spinal cord injury patients: 3 case reports. Arch Phys Med Rehabil. 2001;82:260-261. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 11] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 58. | Madan A, Minocha A. First reported case of colitis cystica profunda in association with Crohn's disease. Am J Gastroenterol. 2002;97:2472-2473. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 7] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 59. | Krüger S, Noack F, Feller AC, Birth M. Colitis cystica profunda and giant inflammatory pseudopolyp in Crohn's disease. Int J Colorectal Dis. 2005;20:383-384. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 6] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 60. | Kayaçetin E, Kayaçetin S. Colitis cystica profunda simulating rectal carcinoma. Acta Chir Belg. 2005;105:306-308. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 6] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 61. | Sarzo G, Finco C, Parise P, Vecchiato M, Savastano S, Luongo B, Degregori S, Bocus P, Marino F, Poletti A, De Lazzari F, Merigliano S. Colitis cystica profunda of the rectum: report of a case and review of the literature. Chir Ital. 2005;57:789-798. [PubMed] |
| 62. | Dewandel P, Schraepen T, Vanbeckevoort D, Geboes K, Delvaux V, Gevers A, Aerts R, Ponette E. Colitis cystica profunda. JBR-BTR. 2001;84:111-113. [PubMed] |
| 63. | Inan N, Arslan AS, Akansel G, Anik Y, Gürbüz Y, Tugay M. Colitis cystica profunda: MRI appearance. Abdom Imaging. 2007;32:239-242. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 11] [Article Influence: 0.6] [Reference Citation Analysis (1)] |
| 64. | Sztarkier I, Benharroch D, Walfisch S, Delgado J. Colitis cystica profunda and solitary rectal ulcer syndrome-polypoid variant: Two confusing clinical conditions. Eur J Intern Med. 2006;17:578-579. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 7] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 65. | Tajika M, Nakamura T, Kawai H, Sawaki A, Mizuno N, Takahashi K, Yokoi T, Yatabe Y, Hirai T, Yamao K, Kato T. A case of colonic morule with colitis cystica profunda. Gastrointest Endosc. 2007;65:162-163; discussion 163. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 66. | Kornprat P, Langner C, Pfeifer J, Mischinger HJ. Colitis cystica profunda associated with rectal prolapse: report of a case. Int J Colorectal Dis. 2007;22:1555-1556. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 9] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 67. | Laurent V, Corby S, Meyer-Bisch L, Ciprian-Corby S, Barbary C, Beot S, Bresler L, Régent D. [MRI aspect of rare rectal pseudotumor associated with dyschezia: colitis cystica profunda]. J Radiol. 2007;88:585-588. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 2] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 68. | de Toro C G, Villaseca H M, Roa S JC. [Colitis cystica profunda: report of one case]. Rev Med Chil. 2007;135:759-763. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 69. | Dolar E, Kiyici M, Yilmazlar T, Gürel S, Nak SG, Gülten M. Colitis cystica profunda. Turk J Gastroenterol. 2007;18:206-207. [PubMed] |
| 70. | Higuera Alvarez R, García Jde L, San Miguel G, Castro B. [Colitis cystica profunda]. Rev Esp Enferm Dig. 2008;100:240-242. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 71. | Toll AD, Palazzo JP. Diffuse colitis cystica profunda in a patient with ulcerative colitis. Inflamm Bowel Dis. 2009;15:1454-1455. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 8] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 72. | Fernández Salazar LI, Velayos Jiménez B, Martínez García G, Herreros Rodríguez J, Abril Vega C, González Hernández JM. [Relapsing colitis cystica profunda]. Rev Esp Enferm Dig. 2009;101:226-227. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 73. | Baltar-Arias R, Ulla-Rocha JL, Moreno-López E, Fernández-Salgado E, Vázquez-Rodríguez S, Díaz-Saa W, Carrera-González V, Vázquez-Astray E. Rectal polyp as presentation form of colitis cystica profunda. Rev Esp Enferm Dig. 2010;102:53-54. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 74. | Jung ME, Cho GM, Byun SW, Do KR, Kim HK, Cho YS, Chae HS, Shin OR, Kim SS. Colitis cystica profunda presenting with a mucus pool within the stalk of a pedunculated colon polyp. Endoscopy. 2010;42 Suppl 2:E114-E115. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 1] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 75. | Qayed E, Srinivasan S, Wehbi M. A case of colitis cystica profunda in association with diverticulitis. Am J Gastroenterol. 2011;106:172-173. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 5] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 76. | Arana R, Fléjou JF, Parc Y, El-Murr N, Cosnes J, Svrcek M. Cap polyposis and colitis cystica profunda: a rare association. Histopathology. 2014;64:604-607. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 77. | Sultan M, Chalhoub W, Gottlieb K, Marino G. Endosonographic Findings in Colitis Cystica Profunda. ACG Case Rep J. 2014;1:122-123. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 78. | Cecinato P, Scaioli E, Leonardi F, Liverani E, Cardamone C, Rosati G, Balbi T, Belluzzi A. A rare case of giant pseudopolyp and colitis cystica profunda coexistence in an ulcerative colitis patient. Rev Esp Enferm Dig. 2014;106:297-298. [PubMed] |
| 79. | Shin O, Kim N, Choi S, Cho Y. Gastrointestinal: large mucin pool within the remnant stalk of an adenomatous polyp after resection and its association with colitis cystica profunda. J Gastroenterol Hepatol. 2014;29:1949. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 80. | Hernandez-Prera JC, Polydorides AD. Colitis cystica profunda indefinite for dysplasia in Crohn disease: a potential diagnostic pitfall. Pathol Res Pract. 2014;210:1075-1078. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 8] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 81. | Jeruc J, Drobne D, Zidar N. Diffuse Colitis Cystica Profunda in Crohn's Disease: A Potential Diagnostic Pitfall. J Crohns Colitis. 2019;13:1362. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 82. | Abe T, Hamamoto M, Nagai T, Nariyasu T, Hanzawa M, Hiroshima Y, Murakami K. Colitis cystica profunda mimicking mucinous adenocarcinoma of the rectum diagnosed by endoscopic submucosal dissection. Endoscopy. 2021;53:E157-E159. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 83. | Zhou T, Patel K, Harris RA, Seghers V, Walsh SM, Rodriguez R, Kellermayer R, Wu H. SULT1A1 and SULT1A2 Associated Extensive Prolapse-Type Inflammatory Polyposis in Crohn's Colitis. Ann Clin Lab Sci. 2021;51:868-874. [PubMed] |
| 84. | Suter KJL, Skinner SA. Rare presentation of colitis cystica profunda in a single rectal ulcer. ANZ J Surg. 2023;93:1058-1059. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 85. | Zhang Y, Tian F, Li H. Solitary Rectal Ulcer Syndrome Coexisting with Colitis Cystica Profunda-Is Mucosal Resection Radical or Not? Inflamm Bowel Dis. 2023;29:1008-1009. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 86. | Bhagwanani A, Kearns C, Vijan A, Brun-Vergara ML. Colitis Cystica Profunda. Radiographics. 2023;43:e230184. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 87. | Denis R, Hobbs M, Felix M, Lujan HJ. Colitis Cystica Profunda of the Hepatic Flexure: A Case Report. Cureus. 2024;16:e58342. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 88. | Chebbo H, Yazbak A, Saleh S, Karam K, Azizi L, Fiani E. An Intimate Relationship Lies Between the Appendix and the Colon: A Case Report of Colitis Cystica Profunda Post-Laparoscopic Appendectomy. Eur J Case Rep Intern Med. 2024;11:004783. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 89. | Rosano GN, Aiello E, Pisheh SK, Deiana E, Memeo L, Colarossi C. Colitis cystica profunda associated with diverticulosis and calcification mimicking colorectal carcinoma: a case report and a brief literature review. Pathologica. 2024;116:249-253. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 90. | Früh J, Früh L, Daubitz T. Colitis Cystica Profunda—A Rare Cause of Rectal Bleeding. Dtsch Arztebl Int. 2024;121:615. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 91. | Guduguntla BA, Chapman WC Jr, Shenoy K, Trieu JA. Colitis Cystica Profunda: A Rare Cause of Rectal Bleeding. Am J Gastroenterol. 2025;120:20. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 92. | Zhou W, Ruan L, Zhang L, Zhang T. Colitis cystica profunda: A rare mimicker of submucosal tumour. Dig Liver Dis. 2025;57:923-924. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/