Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.113979
Revised: October 26, 2025
Accepted: December 10, 2025
Published online: February 27, 2026
Processing time: 169 Days and 20 Hours
Anal fistula is a common anorectal disorder for which conventional surgical pro
To systematically evaluate and compare the clinical efficacy, safety, and post
In accordance with Preferred Reporting Items for Systematic reviews and Meta-Analyses guidelines, we conducted a comprehensive systematic search of both Chinese and international databases to identify RCTs published during January 2014 to 2025. Studies were deemed eligible if they directly compared LIFT with conventional surgical approaches, such as seton placement, fistulotomy, and fis
In total, 107 RCTs involving 9401 participants met the inclusion criteria. LIFT yiel
The LIFT procedure demonstrated clear advantages over conventional surgical methods in terms of clinical effi
Core Tip: Ligation of the intersphincteric fistula tract offers a sphincter-preserving alternative to conventional surgery for anal fistula. This systematic review of randomized controlled trials demonstrates that the procedure improves cure rates, reduces recurrence and complications, shortens wound-healing time, and better preserves anal function. These findings highlight its potential as a preferred treatment option and provide strong evidence for clinical decision-making.
- Citation: Li X, Zhi CC, Wang XL, Zheng LH, Cheng YC. Ligation of the intersphincteric fistula tract vs conventional surgery for anal fistula in Chinese patients. World J Gastrointest Surg 2026; 18(2): 113979
- URL: https://www.wjgnet.com/1948-9366/full/v18/i2/113979.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i2.113979
Anal fistula represents a chronic, suppurative inflammatory disorder of the anorectal region that typically develops secondary to an infection of the anal glands. Obstruction and subsequent infection of these glands lead to crypt abscess formation and the creation of an abnormal tract connecting the anal canal with the perianal skin. Clinically, this disease is characterized by perianal pain, purulent discharge, and recurrent abscesses, which collectively contribute to substantial discomfort and morbidity. The global incidence of this disorder is estimated at approximately 10-20 per 10000 person-years, with a strong male predominance and peak onset at the age of 30-50 years[1,2]. In the absence of timely and stan
The conventional procedures (seton placement, fistulotomy, fistulectomy, and musculocutaneous flap repair) remain the cornerstone of management but often entail partial division of the anal sphincter complex, increasing the risks of delayed wound healing, incontinence, and recurrence (10%-30%)[4,5]. To address these challenges, various sphincter-preserving procedures have been developed, including transanal opening of the intersphincteric space, endoscopic fistula closure, and laser ablation. Although these newer methods aim to reduce complications and improve functional preservation, their long-term efficacy remains inconsistent and inadequately supported by large-scale evidence[6-8].
In 2007, the ligation of the intersphincteric fistula tract (LIFT) procedure offers a promising, minimally invasive alternative designed to eradicate infection while preserving the sphincter integrity. This technique involves identifying and ligating the fistula tract within the intersphincteric space, thereby preventing the proximal spread of infection and maintaining the sphincter continuity[9]. Multiple clinical studies, including small randomized controlled trials (RCTs) and observational cohorts, have reported primary healing rates of 70%-90% and recurrence rates of 5%-20%, with fewer postoperative complications relative to those with conventional procedures[10-13]. Nevertheless, these data remain heterogeneous in terms of follow-up duration, patient selection, and outcome measures, and large, high-quality RCTs providing definitive evidence remain lacking[14-16].
In this context, we conducted a systematic review and meta-analysis of RCTs, designed in accordance with the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) guidelines, to critically assess the comparative effectiveness and safety of LIFT vs conventional surgical techniques for anal fistula. This study aimed to integrate the available evidence regarding cure rates, recurrence, postoperative complications, pain levels, wound-healing duration, anal sphincter function, and operative time, thereby establishing an updated and evidence-based framework for clinical decision-making in the management of anal fistula.
This systematic review was prospectively registered in International Prospective Register of Systematic Reviews (No. CRD420251053697)[17]. The protocol was developed in accordance with the PRISMA guidelines and prespecified a detailed methodological framework for comparing the effectiveness of LIFT with conventional surgery in patients with anal fistulas[18].
A comprehensive literature search was conducted across both international and Chinese databases, combining electronic retrieval with manual searches. The databases included China National Knowledge Infrastructure, Wanfang, VIP, and PubMed, covering publications from January 2014 to January 2025. The electronic search strategy incorporated both Medical Subject Headings (MeSH) and free-text terms. The primary search components included: (1) “Anal fistula”, including exploded MeSH terms such as “Anal Fistula”, “fistula surgery”, and “fistula operation”; (2) “Ligation of the intersphincteric fistula tract”, comprising exploded MeSH terms such as “LIFT” and “sphincter interspace ligation”; (3) “Conventional surgery”, containing exploded MeSH terms such as “fistulotomy”, “seton”, and “fistula incision”; and (4) “Randomized controlled trials”, including exploded MeSH terms such as “randomized controlled trial”, “RCT”, and “clinical trial”. These components were combined using the Boolean operator: 1 AND 2 AND 3 AND 4.
All retrieved titles and abstracts were independently screened by two reviewers (Li X and Cheng YC) to identify potentially eligible studies, with subsequent full-text assessments performed in duplicate to minimize any selection bias. To ensure completeness and methodological rigor, the reference lists of included articles and relevant systematic reviews were examined for additional or gray literature. Furthermore, Zhi CC and Wang XL manually screened high-impact journals in colorectal surgery and gastroenterology for potentially relevant studies not captured in database searches. Zheng LH also reviewed major clinical trial registries, including the World Health Organization International Clinical Trials Registry Platform (https://www.who.int/clinical-trials-registry-platform) and the Chinese Clinical Trial Registry (http://www.chictr.org.cn), to identify ongoing or unpublished RCTs pertinent to this topic.
PICOS framework: P (population): Patients diagnosed with anal fistula; I (intervention): LIFT; C (comparison): Conventional surgical techniques other than LIFT; O (outcomes): Primary outcomes: Cure rate, recurrence rate, and complication rate. Secondary outcomes: When available, postoperative pain, wound-healing time, anal sphincter function, operative duration, and overall clinical effectiveness; S (study design): RCTs.
Inclusion criteria: Eligible studies met the following conditions: (1) RCT study design; (2) Participants were diagnosed with anal fistula based on clearly defined or internationally accepted diagnostic criteria; (3) Fistula complexity was classified according to the American Society of Colon and Rectal Surgeons 2022 guidelines; (4) The intervention compared the LIFT procedure with conventional surgical techniques addressing the same clinical indication; and (5) At least one of the predefined primary or secondary outcomes was reported. Studies published primarily between January 2014 and January 2025 were included, with supplemental searches extending to database inception to ensure comprehensiveness. Most included RCTs focused on patients with cryptoglandular fistulas. No cryptoglandular etiologies such as Crohn’s disease, tuberculosis, trauma, or malignancy were either excluded or rarely reported. Consequently, the findings of this review predominantly reflect outcomes in cryptoglandular anal fistulas.
Exclusion criteria: Past studies were excluded if they lacked accessible full-text reports, represented duplicate publications or overlapping datasets (the earliest or most complete version was retained), or contained incomplete data or major methodological errors (the most accurate dataset was used when available).
Two reviewers independently screened titles and abstracts to identify potentially eligible studies, followed by full-text evaluations based on the inclusion and exclusion criteria. From each included trial, the following data were extracted: First author, publication year, country or region, sample size, patient characteristics, diagnostic criteria, fistula classification, type of intervention, and primary and secondary outcomes (cure, recurrence, complications, pain, healing time, operative duration, anal function, and overall clinical effectiveness). The methodological quality of RCTs was assessed using the Cochrane risk-of-bias 2.0 tool. Disagreements were resolved through discussion or consultation with a third reviewer. The overall certainty of the evidence across outcomes was evaluated using the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) framework.
Risk-of-bias assessments were performed using the Cochrane risk-of-bias 2.0 tool, which evaluated randomization, allocation concealment, blinding, completeness of outcome data, and selective reporting across five domains of potential bias. The certainty of evidence for each outcome was subsequently graded in accordance with the GRADE approach[19]. Factors considered included the risk of bias, inconsistency, indirectness, imprecision, and potential publication bias. Evidence quality was categorized as high, moderate, low, or very low. All assessments were performed independently by two reviewers, with discrepancies resolved via consensus or arbitration by a senior reviewer to ensure objectivity and methodological rigor.
Meta-analyses were performed using Review Manager version 6.1. Between-study heterogeneity was evaluated using the Q test (with P < 0.05 indicating significant heterogeneity) and quantified with the I2 statistic. A fixed-effect model was applied when I2 ≤ 50%; otherwise, a random-effects model was used. For dichotomous outcomes, pooled effect estimates were calculated as relative risks (RRs) or odds ratios (ORs) with 95% confidence intervals (CIs). The continuous outcomes were synthesized as weighted mean differences (MDs) with corresponding 95%CIs. Sensitivity analyses were conducted to explore the influence of individual studies on pooled estimates when heterogeneity was substantial.
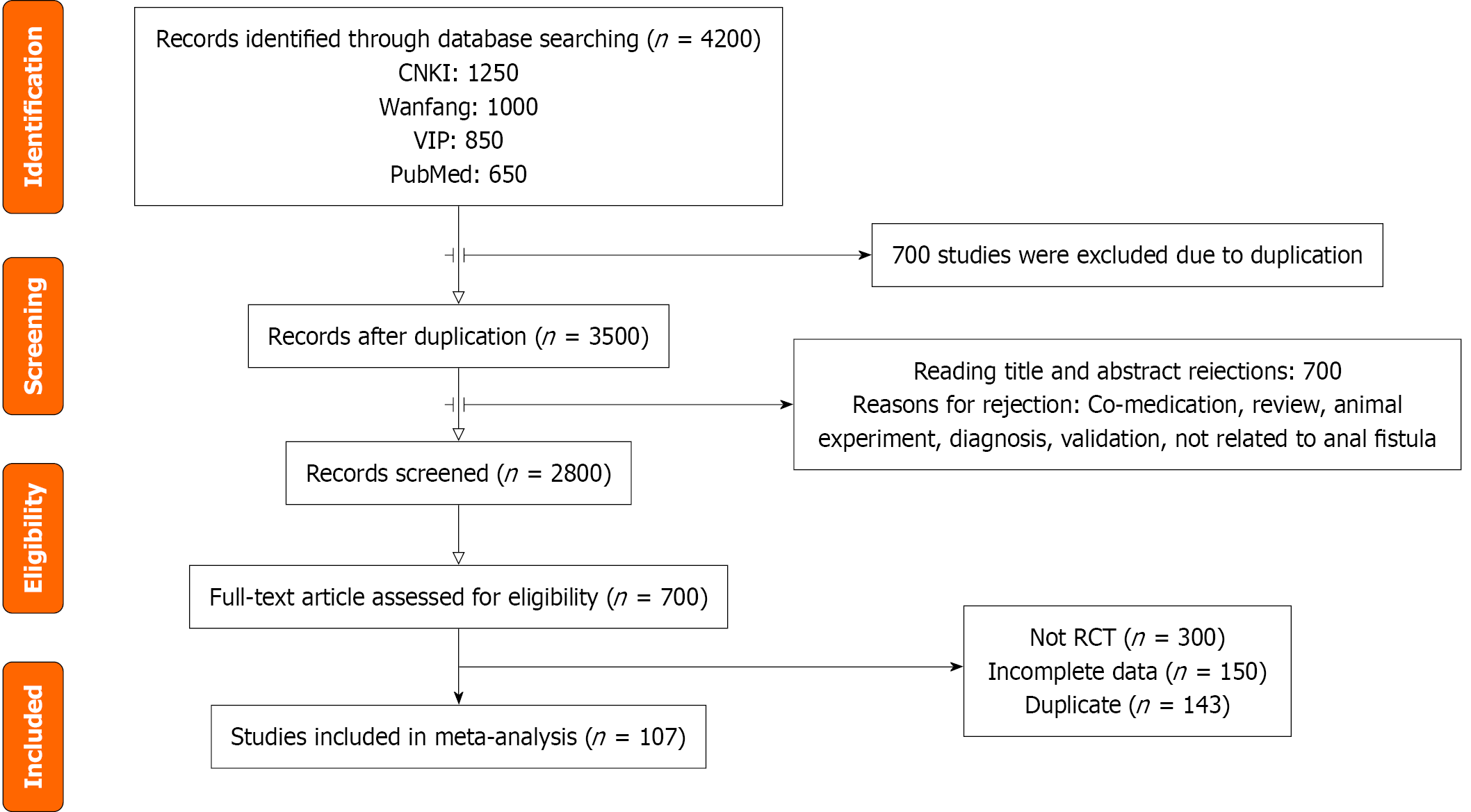
A total of 107 RCTs published between 2014 and 2025 met the inclusion criteria, encompassing 9401 patients in total. Of these, 4691 patients were treated using the LIFT procedure (experimental group), while 4710 underwent conventional surgical approaches (control group). The process of study identification and inclusion is illustrated in Figure 1.
The included trials collectively covered a wide spectrum of fistula morphologies, such as high- and low-complex fistulas, high and low simple fistulas, trans-sphincteric and intersphincteric fistulas, as well as fistulas of glandular origin. Control interventions varied across studies, but most frequently included seton placement with fistulotomy, fistulectomy, conventional intersphincteric tract ligation, and standard fistulotomy. All studies were RCTs that directly compared the efficacy and safety of the LIFT procedure with at least one conventional surgical technique. The principal characteristics of these studies are summarized in Supplementary Table 1.
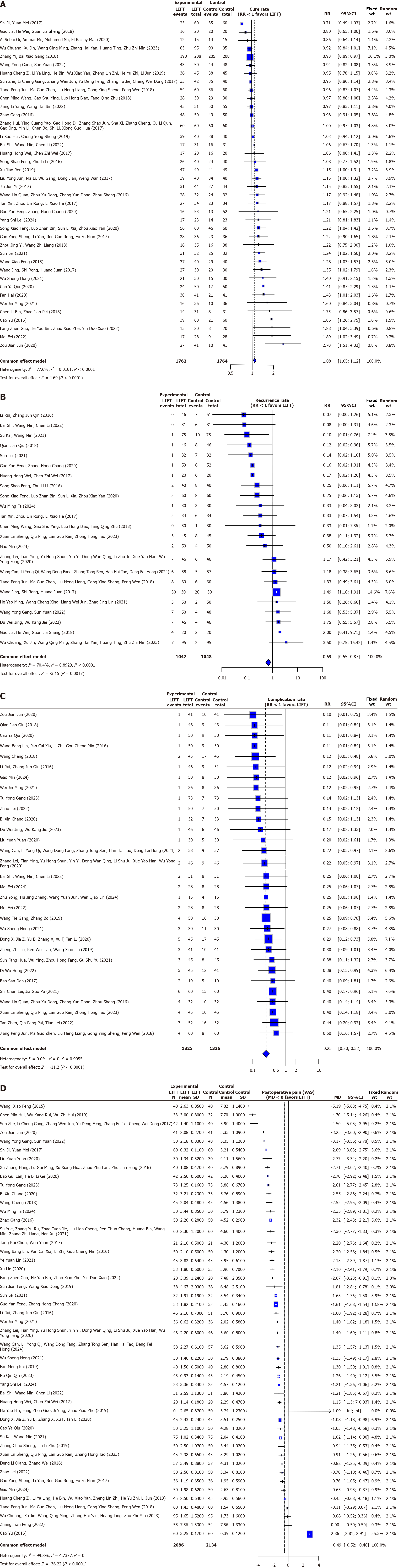
Cure rate: Thirty-nine studies reported cure rate data. The pooled analysis demonstrated that the LIFT procedure was associated with a significantly higher cure rate than conventional surgical methods (RR = 1.08; 95%CI: 1.02-1.14; P = 0.0074). Moderate heterogeneity was observed (Q = 102.97; P < 0.0001; I2 = 63.1%), suggesting some interstudy variation in effect estimates (Figure 2A; Table 1).
| Outcome | Studies | Q | P value (Q test) | I2 (%) | 95%CI of I2 (%) | RR | RR P value | RR 95%CI | MD | MD P value | MD 95%CI |
| Cure rate | 39 | 102.97 | < 0.0001 | 63.1 | 48.0-73.8 | 1.0762 | 0.0074 | 1.0198-1.1356 | |||
| Recurrence rate | 23 | 52.04 | 0.0003 | 57.7 | 32.8-73.4 | 0.6124 | 0.0323 | 0.3909-0.9595 | |||
| Complication rate | 31 | 13.07 | 0.9969 | 0.0 | 0.0-40.2 | 0.2536 | < 0.0001 | 0.1994-0.3224 | |||
| Overall effectiveness | 67 | 128.13 | < 0.0001 | 48.5 | 31.5-61.3 | 1.1385 | < 0.0001 | 1.1094-1.1684 | |||
| VAS | 48 | 23290.42 | 0 | 99.8 | -1.7216 | < 0.0001 | -2.1018 to | ||||
| Wound healing time | 61 | 3691.79 | 0 | 98.4 | 98.2-98.6 | -8.4489 | < 0.0001 | -9.7276 to | |||
| Anal function | 33 | 6307.39 | 0 | 99.5 | 99.5-99.6 | -1.3793 | < 0.0001 | -1.9136 to | |||
| Operative time | 41 | 8043.29 | 0 | 99.5 | 99.5-99.6 | 3.7127 | 0.0914 | -0.5975 to 8.0230 |
Recurrence rate: Twenty-three RCTs provided recurrence data. The pooled estimate indicated a significantly lower recurrence rate following LIFT compared with conventional surgery (RR = 0.61; 95%CI: 0.39-0.96; P = 0.0323). Moderate heterogeneity was again present (Q = 52.04; P = 0.0003; I2 = 57.7%; Figure 2B; Table 1).
Complication rate: A total of 31 studies evaluated postoperative complications. Meta-analysis revealed a markedly reduced complication rate in the LIFT group compared with the control group (RR = 0.25; 95%CI: 0.20-0.32; P < 0.0001). Heterogeneity testing suggested consistent findings across studies (Q = 13.07; P = 0.9969; I2 = 0.0%), supporting the robustness of this outcome (Figure 2C; Table 1).
Overall clinical effectiveness: Sixty-seven trials assessed the overall clinical effectiveness. The pooled estimate demonstrated a significantly greater overall clinical success with LIFT when compared with conventional surgery (RR = 1.14; 95%CI: 1.11-1.17; P < 0.0001). Moderate heterogeneity was present (Q = 128.13; P < 0.0001; I2 = 48.5%; Supplementary Figure 1; Table 1).
Postoperative pain: Forty-eight studies measured postoperative pain using Visual Analog Scale (VAS) scores. The pooled weighted MD indicated substantially less pain after LIFT (MD = -1.72; 95%CI: -2.10 to -1.34; P < 0.0001). Heterogeneity among studies was high (Q = 23,290.42; P < 0.0001; I2 = 99.8%), likely reflecting variations in the pain assessment timing and postoperative care protocols (Figure 2D; Table 1).
Wound healing time: Sixty-one trials reported wound-healing duration. Patients undergoing LIFT experienced significantly faster healing than those who underwent conventional surgery (MD = -8.45 days; 95%CI: -9.73 to -7.17; P < 0.0001). Substantial heterogeneity (Q = 3,691.79; P < 0.0001; I2 = 98.4%) suggested clinical and methodological differences across studies (Supplementary Figure 2; Table 1).
Anal function: Thirty-three studies evaluated postoperative anal function. The meta-analysis revealed superior preservation of anal function following LIFT (MD = -1.38; 95%CI: -1.91 to -0.85; P < 0.0001). Despite this consistent effect, heterogeneity remained considerable (Q = 6307.39; P < 0.0001; I2 = 99.5%), which may be attributable to differing evaluation scales and follow-up durations (Supplementary Figure 3; Table 1).
Operative time: Forty-one trials compared the operative duration. The pooled estimate showed no significant difference between LIFT and conventional surgery (MD = 3.71 minutes; 95%CI: -0.60 to 8.02; P = 0.0914). High heterogeneity (Q = 8043.29; P < 0.0001; I2 = 99.5%) likely reflects procedural variations and surgeon expertise across centers (Supplementary Figure 4; Table 1). Forest plots for primary outcomes (cure, recurrence, and complication rates and postoperative pain) are presented in Figure 2, while the secondary outcome plots (healing time, anal function, operative time, and overall clinical effectiveness) are shown in the Supplementary Figures 1-4.
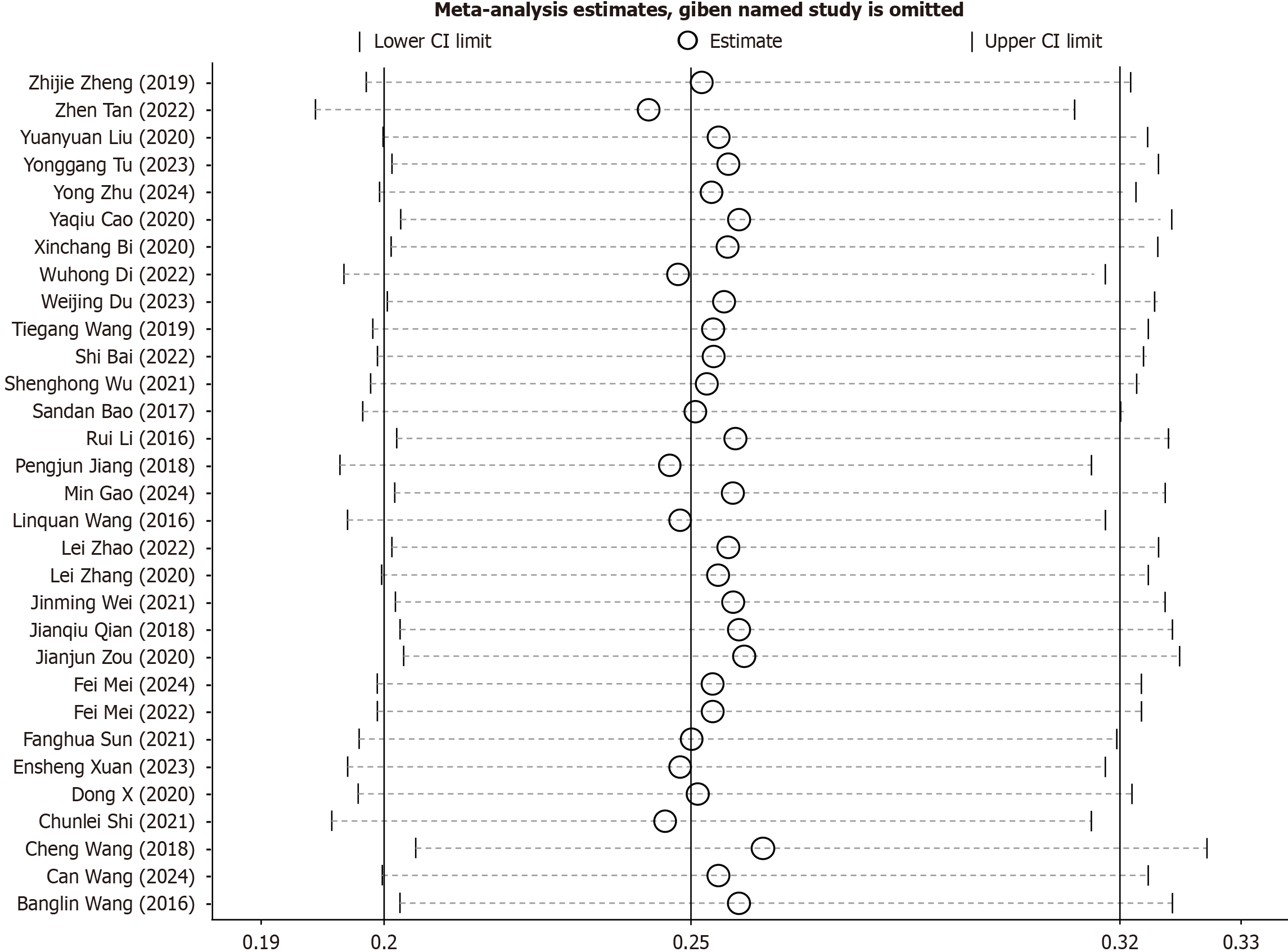
Sensitivity analyses were performed to assess the stability of the pooled results. Exclusion of individual studies did not materially affect overall estimates or their 95%CIs, confirming the robustness of the meta-analytic findings (Figure 3; Supplementary Figures 5-11). For continuous outcomes, the pooled MDs for postoperative pain (MD = -1.72; 95%CI: -2.10 to -1.34) and wound-healing time (MD = -8.45 days; 95%CI: -9.73 to -7.17) consistently excluded zero, reinforcing their statistical significance. Similarly, the pooled MD for anal function (MD = -1.38; 95%CI: -1.91 to -0.85) remained stable across iterations, indicating minimal influence of any single trial on the aggregated results.
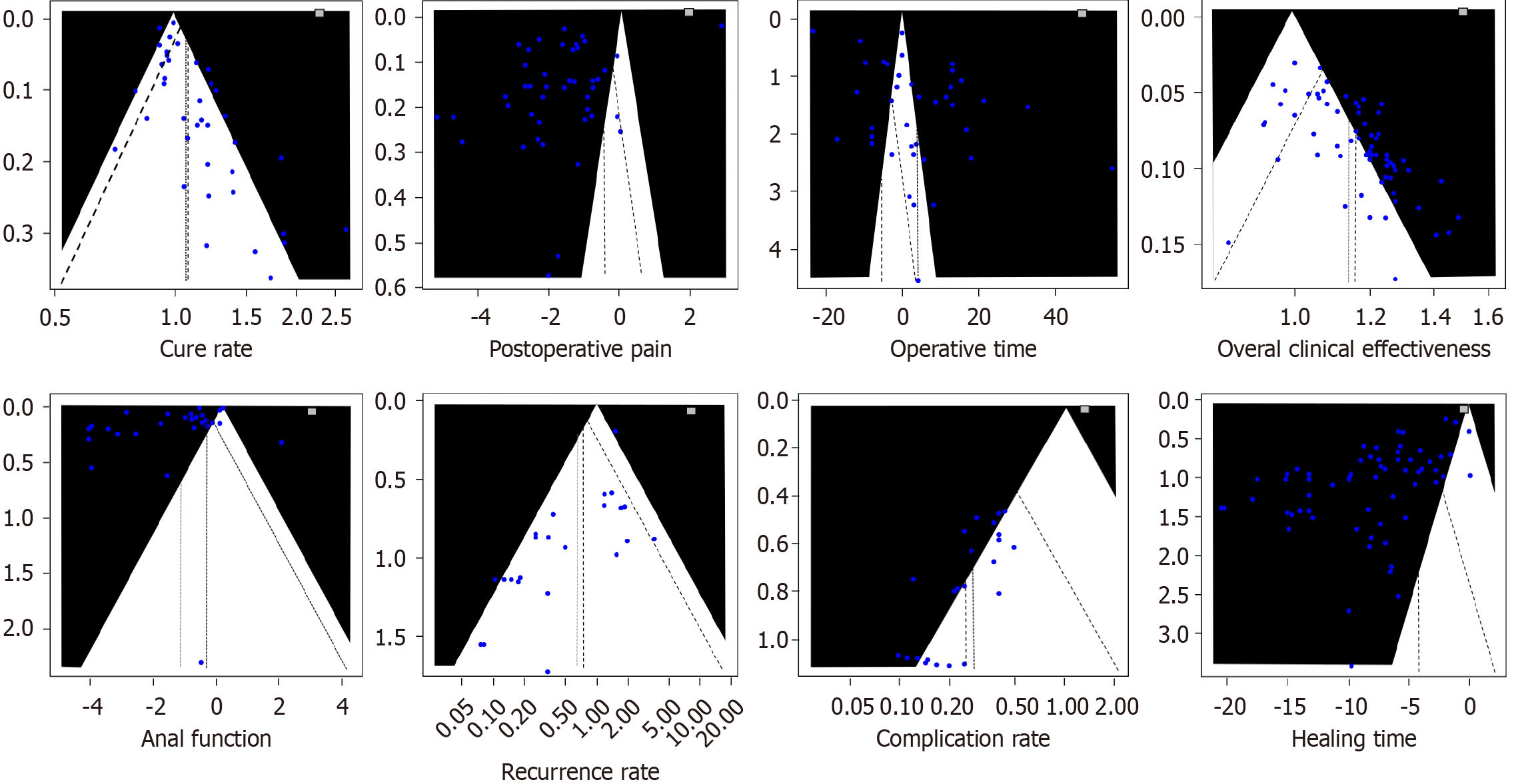
Funnel plots generated for all eight analyzed outcomes (Figure 4) demonstrated generally symmetrical distributions, indicating no substantial asymmetry suggestive of small-study effects. Egger’s regression analyses yielded intercept P > 0.05 across all outcomes, providing no statistical evidence of publication bias.
The certainty of evidence was evaluated by applying the GRADE approach. For the primary outcomes, the cure rate was supported by moderate-certainty evidence, downgraded one level due to the identified risks of bias and inconsistency across trials. Similarly, the recurrence rate was evaluated as moderate certainty, reflecting limitations in the study quality and moderate heterogeneity. In contrast, the complication rate was assessed as low certainty, with downgrades applied for multiple domains, including the risk of bias and inconsistency, yielding reduced confidence in the pooled estimate. Among the secondary outcomes, most were rated as moderate certainty, indicating a fair degree of confidence in the observed associations. However, operative time was downgraded for imprecision, as reflected by wide CIs and a lack of statistical significance (Table 2).
| Outcome | Number of studies (RCTs) | LIFT group (n) | Conventional group (n) | Effect (95%CI) | Certainty of evidence | Reasons for downgrading |
| Dichotomous outcomes | ||||||
| Cure rate | 39 | 1379/1762 | 1273/1764 | RR = 1.08 (1.02-1.14) | Moderate | Serious risk of bias, inconsistency |
| Recurrence rate | 23 | 96/1047 | 139/1048 | RR = 0.61 (0.39-0.96) | Moderate | Serious risk of bias, inconsistency |
| Complication rate | 31 | 75/1325 | 295/1326 | RR = 0.25 (0.20-0.32) | Low | Serious risk of bias, imprecision |
| Overall clinical effectiveness | 67 | 2568/2709 | 2221/2709 | RR = 1.14 (1.11-1.17) | Moderate | Serious risk of bias, inconsistency |
| Continuous outcomes | ||||||
| Postoperative pain (VAS) | 48 | 2086 | 2134 | MD = -1.72 (-2.10 to -1.34) | Moderate | Serious risk of bias, inconsistency |
| Wound healing time (days) | 61 | 2588 | 2640 | MD = -8.45 (-9.73 to -7.17) | Moderate | Serious risk of bias, inconsistency |
| Anal function (score) | 33 | 1300 | 1347 | MD = -1.38 (-1.91 to -0.85) | Moderate | Serious risk of bias, inconsistency |
| Operative time (minutes) | 41 | 1789 | 1811 | MD = 3.71 (-0.60 to 8.02) | Moderate | Serious risk of bias, inconsistency |
Subgroup analyses stratified by fistula position and complexity (Supplementary Table 2) provided additional insights into the comparative performance of LIFT. For high-position fistulas, LIFT yielded a slightly higher cure rate (RR = 1.14; 95%CI: 1.01-1.29; P = 0.040) and a significantly lower complication rate (RR = 0.30; 95%CI: 0.16-0.60; P < 0.001). Conversely, low-position fistulas revealed no significant difference in the cure rate between the groups (RR = 1.04; 95%CI: 0.92-1.18; P = 0.54). In terms of fistula complexity, the LIFT procedure provided modest improvements in the cure rate for complex fistulas (RR = 1.08; 95%CI: 0.99-1.18) and a substantially lower complication rate (RR = 0.35; 95%CI: 0.25-0.49; P < 0.001), while outcomes for simple tracts were largely comparable to conventional surgery. Collectively, these findings suggest that LIFT may be particularly advantageous for anatomically complex or high-position fistulas where sphincter preservation is clinically prioritized.
This systematic review and meta-analysis synthesized findings from 107 RCTs encompassing 9401 patients, offering a comprehensive evaluation of the comparative efficacy and safety of LIFT vs conventional surgery for anal fistula. The pooled results consistently indicated that LIFT confers distinct advantages in terms of the healing rate, recurrence, complication profile, and postoperative recovery metrics. The discussion below contextualizes these findings within the existing literature, explores potential mechanisms, and highlights methodological limitations and directions for future research.
The healing rate in the LIFT group was modestly but significantly higher than that in the control group (RR = 1.08; 95%CI: 1.02-1.14). This aligns with the initial healing rates of 80%-90% reported by Elshamy et al[20] and compares favorably with the 70%-80% success rates commonly reported with traditional seton placement and fistulotomy techniques[21,22]. The improved outcomes with LIFT may stem from the procedure’s anatomic precision: By ligating the intersphincteric tract at its origin, LIFT effectively eradicated the source of infection while maintaining sphincter integrity. This preservation of the sphincter complex sustains local vascular perfusion and tissue tension, both of which are critical for epithelial regeneration and healing.
LIFT was associated with a significant reduction in postoperative recurrence (RR = 0.61; 95%CI: 0.39-0.96), which is consistent with the results reported across several cohort studies and RCTs[23-26]. This effect likely reflects the an
The pooled analysis demonstrated a marked reduction in complication rates with LIFT (RR = 0.25; 95%CI: 0.20-0.32), highlighting a substantial decrease in the adverse events, including incontinence, infection, and persistent postoperative pain, based on high-quality RCT data[27,28]. Mechanistically, smaller incisions, reduced intraoperative bleeding, mi
Regarding the overall clinical effectiveness, LIFT exhibited a 14% relative improvement when compared with conventional surgery (RR = 1.14; 95%CI: 1.11-1.17). This composite outcome incorporates both objective healing measures and patient-centered indicators such as symptom relief and recovery time, providing a holistic assessment of the treatment efficacy[29]. These results underscore the importance of integrating patient-reported outcome measures in future trials. Nonetheless, variability in criteria for defining clinical effectiveness remains a limitation, highlighting the need for standardized evaluation frameworks.
For continuous outcomes, 48 studies reported postoperative pain using VAS scores. LIFT was associated with an average reduction in the VAS scores of 1.72 points (95%CI: -2.10 to -1.34), despite substantial heterogeneity (I2 = 99.8%)[30,31]. Factors contributing to lower pain scores may include reduced surgical trauma, smaller incisions, and fewer postoperative dressing changes. Similarly, LIFT was linked to a shorter wound-healing time, with a mean reduction of 8.45 days when compared with conventional surgery (95%CI: -9.73 to -7.17)[32]. This quantitative synthesis of healing duration adds valuable precision to the existing literature; however, varying definitions of wound healing (e.g., complete epithelialization vs absence of discharge) indicates the need for future research to incorporate objective imaging ass
A total of 33 studies assessed postoperative anal function, showing a mean decline of only 1.38 points following LIFT (95%CI: -1.91 to -0.85), which is consistent with the reported incontinence rates of 0%-5%[33-35]. These findings reinforce the sphincter-preserving advantage of LIFT, likely attributable to the maintained sphincter continuity and reduced muscle fiber disruption. Such evidence strengthens the functional outcome profile of LIFT and informs potential pro
Operative time did not significantly differ between LIFT and conventional surgery (MD = 3.71 minutes; 95%CI: -0.60 to 8.02)[36-41], suggesting comparable technical complexity and efficiency. Although debates regarding the learning curve and surgical difficulty persist, this pooled estimate provides a useful reference for clinical practice and surgical training programs.
Recent studies from Western centers offer long-term perspectives on sphincter-preserving approaches for complex anal fistulas. Stellingwerf et al[42] conducted a systematic review and meta-analysis comparing endorectal advancement flap and LIFT for both cryptoglandular and Crohn’s high perianal fistulas, reporting overall healing rates of 60%-80% with preserved continence in the majority of cases. Similarly, Schiano di Visconte and Bellio[43] performed a prospective two-year comparative study of endorectal advancement flap vs collagen paste injection and found healing rates of 65% and 52%, respectively, with continence deterioration in 16% vs 5% of patients. These findings contextualize LIFT within broader sphincter-sparing strategies and highlight its role as an effective, function-preserving intervention for anatomically complex anal fistulas[44].
Long-term European data on sphincter-preserving techniques demonstrated substantial variability in the outcomes. Wilhelm et al[30] reported 5-year healing rates of 64%-70% following FiLaC™ (fistula laser closure). Similarly, Meinero et al[45] observed 2-year success rates of 60%-67% with video-assisted anal fistula treatment. Several case series evaluating the LIFT procedure and its biologically reinforced variant, BioLIFT, have reported long-term closure rates of approximately 62%-75% with excellent preservation of continence[46,47]. Collectively, these studies illustrate that although sphincter-preserving approaches generally maintain functional outcomes, the durability of fistula closure is highly technique-dependent and can vary considerably across patient populations and follow-up intervals.
In contrast, the Chinese RCTs included in this meta-analysis reported higher early healing rates (80%-90%) and low complication rates (< 5%), yet most studies had follow-up periods of ≤ 12 months. Integrating these findings with Western data suggests that LIFT achieves robust short-term efficacy and functional preservation. However, the evidence regarding long-term durability remains limited. These comparisons underscore the importance of multicenter trials with standardized follow-up periods of at least 24 months to evaluate sustained fistula closure and recurrence prevention. Although LIFT appears to outperform conventional surgery in the early postoperative period, long-term outcomes of different sphincter-preserving modalities are comparable, highlighting the necessity of harmonized and extended follow-up protocols.
Considerable heterogeneity in continuous outcomes (I2 > 90%) likely reflects the differences in patient-selection criteria, procedural modifications, definitions of outcomes, and duration of follow-up. Notably, several single-center Chinese RCTs lack detailed methodology regarding randomization or blinding, employing relatively short follow-up intervals (< 12 months), which may have led to the overestimation of effect sizes. Accordingly, the pooled estimates derived from these studies should be interpreted with caution. Future investigations should adopt standardized outcome measures, validated assessment tools, and multicenter designs with extended follow-up to enhance the reliability and comparability of findings.
Subgroup analyses provided additional insight into the potential influence of fistula type and anatomical position on the comparative performance of LIFT. For high-position fistulas, LIFT was associated with a modest increase in cure rate and a lower complication rate compared with conventional surgery, which may suggest a relative benefit when a larger proportion of the sphincter complex is involved and sphincter preservation is an important consideration. In contrast, among low-position fistulas, cure rates appeared generally comparable between LIFT and conventional approaches, although the complication profile tended to favor LIFT. With respect to fistula complexity, the LIFT procedure was linked to modest improvements in cure rate and a lower complication rate in complex fistulas, whereas outcomes for simple tracts were largely similar to those of conventional surgery. Taken together, these observations suggest that both fistula complexity and anatomy may modulate the relative effect of LIFT: The procedure may offer greater advantages in anatomically complex or high-position cryptoglandular fistulas, whereas in simple or low tracts, the choice of technique may depend more on surgeon experience, patient preference, and local practice patterns.
Finally, because the included studies predominantly addressed cryptoglandular fistulas, the generalizability of these findings to noncryptoglandular etiologies, including Crohn’s disease, tuberculosis, trauma, or malignancy, remains uncertain. Future research should incorporate etiologic stratification to determine whether the observed benefits of LIFT extend to these less common fistula subtypes, particularly regarding healing, recurrence, and functional outcomes.
This study was conducted in strict accordance with PRISMA and Cochrane guidelines, including comprehensive eva
Future research should address these gaps by following these steps: (1) Designing rigorously conducted multicenter RCTs with transparent randomization, blinding, and allocation concealment; (2) Developing and adopting standardized, clearly reported definitions for key outcomes, including healing, recurrence, postoperative complications, wound-healing time, and anal functional recovery, and using validated scoring systems (e.g., structured incontinence scales and widely accepted complication grading systems) to facilitate comparison across trials; (3) Incorporating substantially longer and more uniform follow-up periods to reliably evaluate long-term efficacy, recurrence, sphincter function preservation, and the durability of the LIFT procedure; and (4) Systematically reporting fistula morphology, particularly tract number and complexity, and exploring combined approaches that integrate LIFT with endoscopic, laser, or biologic techniques to further optimize efficacy and quality of life.
LIFT demonstrates clear advantages over conventional surgical approaches in terms of cure rates, recurrence, com
| 1. | Steele SR, Kumar R, Feingold DL, Rafferty JL, Buie WD; Standards Practice Task Force of the American Society of Colon and Rectal Surgeons. Practice parameters for the management of perianal abscess and fistula-in-ano. Dis Colon Rectum. 2011;54:1465-1474. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 261] [Cited by in RCA: 168] [Article Influence: 11.2] [Reference Citation Analysis (1)] |
| 2. | Sarveazad A, Bahardoust M, Shamseddin J, Yousefifard M. Prevalence of anal fistulas: a systematic review and meta-analysis. Gastroenterol Hepatol Bed Bench. 2022;15:1-8. [PubMed] |
| 3. | Garg P, Bhattacharya K, Yagnik VD, Mahak G. Recent advances in the diagnosis and treatment of complex anal fistula. Ann Coloproctol. 2024;40:321-335. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 19] [Cited by in RCA: 16] [Article Influence: 8.0] [Reference Citation Analysis (0)] |
| 4. | Madbouly KM, El Shazly W, Abbas KS, Hussein AM. Ligation of intersphincteric fistula tract versus mucosal advancement flap in patients with high transsphincteric fistula-in-ano: a prospective randomized trial. Dis Colon Rectum. 2014;57:1202-1208. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 83] [Cited by in RCA: 57] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 5. | An Y, Gao J, Xu J, Qi W, Wang L, Tian M. Efficacy and safety of 13 surgical techniques for the treatment of complex anal fistula, non-Crohn CAF: a systematic review and network meta-analysis. Int J Surg. 2024;110:441-452. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 14] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 6. | Warsinggih, Aryanti C, Faruk M. Optimum management for complex anal fistula: A network meta-analysis of randomized controlled trials. Surg Open Sci. 2024;18:117-122. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 9] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 7. | Duda JR, de Oliveira LGAM, Ferreira LF, Nunes BCM, do Carmo MCN, Diedrich DB, Franco MC, da Costa MCP, Baraldo S. Effectiveness of Laser-Based Fistula Therapies with and without Adjunctive Measures in Anal Fistulas Management: A Systematic Review and Single-Arm Meta-Analysis. Int J Colorectal Dis. 2025;40:196. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 6] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 8. | Wang C, Huang T, Wang X. Efficacy and safety of transanal opening of intersphincteric space in the treatment of high complex anal fistula: A metaanalysis. Exp Ther Med. 2024;28:306. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 15] [Article Influence: 7.5] [Reference Citation Analysis (1)] |
| 9. | Emile SH, Khan SM, Adejumo A, Koroye O. Ligation of intersphincteric fistula tract (LIFT) in treatment of anal fistula: An updated systematic review, meta-analysis, and meta-regression of the predictors of failure. Surgery. 2020;167:484-492. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 122] [Cited by in RCA: 80] [Article Influence: 13.3] [Reference Citation Analysis (1)] |
| 10. | Awad PBA, Hassan BHA, Awad KBA, Elkomos BE, Nada MAM. A comparative study between high ligation of the inter-sphincteric fistula tract via lateral Approach Versus Fistulotomy and primary sphincteroplasty in High Trans-Sphincteric Fistula-in-Ano: a randomized clinical trial. BMC Surg. 2023;23:224. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (1)] |
| 11. | Sørensen KM, Möller S, Qvist N. Video-assisted anal fistula treatment versus fistulectomy and sphincter repair in the treatment of high cryptoglandular anal fistula: a randomized clinical study. BJS Open. 2021;5:zrab097. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 9] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 12. | Tan IJ, Siew BE, Lau J, Yap CPL, Soon SMME, Tan KK. Is the ligation of the intersphincteric fistula tract (LIFT) procedure truly a sphincter preserving procedure for anal fistula? A scoping review of the literature. Eur J Med Res. 2025;30:243. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 13. | Meinero P, Mori L. Video-assisted anal fistula treatment (VAAFT): a novel sphincter-saving procedure for treating complex anal fistulas. Tech Coloproctol. 2011;15:417-422. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 244] [Cited by in RCA: 187] [Article Influence: 12.5] [Reference Citation Analysis (1)] |
| 14. | Wilhelm A. A new technique for sphincter-preserving anal fistula repair using a novel radial emitting laser probe. Tech Coloproctol. 2011;15:445-449. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 186] [Cited by in RCA: 135] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 15. | Garg P, Kaur B, Menon GR. Transanal opening of the intersphincteric space: a novel sphincter-sparing procedure to treat 325 high complex anal fistulas with long-term follow-up. Colorectal Dis. 2021;23:1213-1224. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 41] [Article Influence: 8.2] [Reference Citation Analysis (0)] |
| 16. | Emile SH, Garoufalia Z, Aeschbacher P, Horesh N, Gefen R, Wexner SD. Endorectal advancement flap compared to ligation of inter-sphincteric fistula tract in the treatment of complex anal fistulas: A meta-analysis of randomized clinical trials. Surgery. 2023;174:172-179. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 17] [Article Influence: 5.7] [Reference Citation Analysis (0)] |
| 17. | Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9803] [Reference Citation Analysis (0)] |
| 18. | Shamseer L, Moher D, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA; PRISMA-P Group. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015: elaboration and explanation. BMJ. 2015;350:g7647. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9935] [Cited by in RCA: 8605] [Article Influence: 782.3] [Reference Citation Analysis (1)] |
| 19. | Guyatt G, Oxman AD, Akl EA, Kunz R, Vist G, Brozek J, Norris S, Falck-Ytter Y, Glasziou P, DeBeer H, Jaeschke R, Rind D, Meerpohl J, Dahm P, Schünemann HJ. GRADE guidelines: 1. Introduction-GRADE evidence profiles and summary of findings tables. J Clin Epidemiol. 2011;64:383-394. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8771] [Cited by in RCA: 7864] [Article Influence: 524.3] [Reference Citation Analysis (0)] |
| 20. | Elshamy MT, Emile SH, Abdelnaby M, Khafagy W, Elbaz SA. A pilot randomized controlled trial on ligation of intersphincteric fistula tract (LIFT) versus modified parks technique and two-stage seton in treatment of complex anal fistula. Updates Surg. 2022;74:657-666. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 3] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 21. | Sun XL, Wen K, Chen YH, Xu ZZ, Wang XP. Long-term outcomes and quality of life following ligation of the intersphincteric fistula tract for high transsphincteric fistulas. Colorectal Dis. 2019;21:30-37. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 29] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 22. | Salgado-Nesme N, Alvarez-Bautista FE, Mongardini FM, Docimo L, Hoyos-Torres A, Ruiz-Muñoz EA, Vergara-Fernàndez O, Suastegui HOG, Illanes MFR, Reyes NDM. LIFT procedure: postoperative outcomes, risk factors for fistula recurrence and continence impairment. Updates Surg. 2024;76:989-997. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 7] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 23. | Raja Ram NK, Chan KK, Md Nor SF, Sagap I. A prospective evaluation of the outcome of submucosal ligation of fistula tract. Colorectal Dis. 2020;22:2199-2203. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 8] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 24. | Kumar P, Sarthak S, Singh PK, Mishra TS, Sasmal PK. Ligation of Intersphincteric Fistulous Tract vs Endorectal Advancement Flap for High-Type Fistula in Ano: A Randomized Controlled Trial. J Am Coll Surg. 2023;236:27-35. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 13] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 25. | Hong KD, Kang S, Kalaskar S, Wexner SD. Ligation of intersphincteric fistula tract (LIFT) to treat anal fistula: systematic review and meta-analysis. Tech Coloproctol. 2014;18:685-691. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 146] [Cited by in RCA: 100] [Article Influence: 8.3] [Reference Citation Analysis (1)] |
| 26. | Lau YC, Brown KGM, Cheong J, Byrne C, Lee PJ. LIFT and BioLIFT: a 10-Year Single-Centre Experience of Treating Complex Fistula-In-Ano With Ligation of Intersphincteric Fistula Tract Procedure With or Without Bio-prosthetic Reinforcement (BioLIFT). J Gastrointest Surg. 2020;24:671-676. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 13] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 27. | Wallin UG, Mellgren AF, Madoff RD, Goldberg SM. Does ligation of the intersphincteric fistula tract raise the bar in fistula surgery? Dis Colon Rectum. 2012;55:1173-1178. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 87] [Cited by in RCA: 67] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 28. | Daodu OO, O'Keefe J, Heine JA. Draining Setons as Definitive Management of Fistula-in-Ano. Dis Colon Rectum. 2018;61:499-503. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 19] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 29. | Hinksman M, Naidu S, Loon K, Grundy J. Long term efficacy of Video-Assisted Anal Fistula Treatment (VAAFT) for complex fistula-in-ano: a single-centre Australian experience. ANZ J Surg. 2022;92:1132-1136. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 30. | Wilhelm A, Fiebig A, Krawczak M. Five years of experience with the FiLaC™ laser for fistula-in-ano management: long-term follow-up from a single institution. Tech Coloproctol. 2017;21:269-276. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 162] [Cited by in RCA: 103] [Article Influence: 11.4] [Reference Citation Analysis (0)] |
| 31. | Giamundo P, Esercizio L, Geraci M, Tibaldi L, Valente M. Fistula-tract Laser Closure (FiLaC™): long-term results and new operative strategies. Tech Coloproctol. 2015;19:449-453. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 129] [Cited by in RCA: 86] [Article Influence: 7.8] [Reference Citation Analysis (0)] |
| 32. | Reyes Díaz ML, Hinojosa-Ramirez F, Ramallo Solís IM, Jiménez Rodríguez RM, Tortolero JP, García Cabrera AM, Vázquez Monchul JM, Portilla de Juan F. Results at one year of the TROPIS technique in the treatment of complex anal fistula. Cir Esp (Engl Ed). 2025;103:135-142. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 6] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 33. | Zhang L, Zhan C, Li L, Shao W, Sun G, Chen Y, Chen G, Lang Y, Xiao Z, Xiao X. Ligation of the intersphincteric fistula tract (LIFT) for high transsphincteric fistulas: a double-center retrospective study with long-term follow-up. Ann Coloproctol. 2025;41:77-83. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 34. | van Oostendorp JY, Verkade C, Han-Geurts IJM, van der Mijnsbrugge GJH, Wasowicz-Kemps DK, Zimmerman DDE. Ligation of intersphincteric fistula tract (LIFT) for trans-sphincteric cryptoglandular anal fistula: long-term impact on faecal continence. BJS Open. 2024;8:zrae055. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 5] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 35. | Bayrak M, Altintas Y. Predictive Factors Affecting Recurrence of Anal Fistula after LIFT Procedure. J Coll Physicians Surg Pak. 2022;32:1470-1473. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 36. | Fuschillo G, Pata F, D'Ambrosio M, Selvaggi L, Pescatori M, Selvaggi F, Pellino G. Failure rates and complications of four sphincter-sparing techniques for the treatment of fistula-in-ano: a systematic review and network meta-analysis. Tech Coloproctol. 2025;29:116. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 11] [Article Influence: 11.0] [Reference Citation Analysis (3)] |
| 37. | Shanwani A, Nor AM, Amri N. Ligation of the intersphincteric fistula tract (LIFT): a sphincter-saving technique for fistula-in-ano. Dis Colon Rectum. 2010;53:39-42. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 176] [Cited by in RCA: 132] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 38. | Sirany AM, Nygaard RM, Morken JJ. The ligation of the intersphincteric fistula tract procedure for anal fistula: a mixed bag of results. Dis Colon Rectum. 2015;58:604-612. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 59] [Cited by in RCA: 43] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 39. | Van Hoof S, Van Dessel E, Cools P. LIFT: a feasible option for primary and recurrent fistulas. Acta Chir Belg. 2021;121:420-426. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 40. | Rojanasakul A. LIFT procedure: a simplified technique for fistula-in-ano. Tech Coloproctol. 2009;13:237-240. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 202] [Cited by in RCA: 140] [Article Influence: 8.2] [Reference Citation Analysis (1)] |
| 41. | Torkzad MR, Karlbom U. MRI for assessment of anal fistula. Insights Imaging. 2010;1:62-71. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 49] [Cited by in RCA: 40] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 42. | Stellingwerf ME, van Praag EM, Tozer PJ, Bemelman WA, Buskens CJ. Systematic review and meta-analysis of endorectal advancement flap and ligation of the intersphincteric fistula tract for cryptoglandular and Crohn's high perianal fistulas. BJS Open. 2019;3:231-241. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 165] [Cited by in RCA: 115] [Article Influence: 16.4] [Reference Citation Analysis (3)] |
| 43. | Schiano di Visconte M, Bellio G. Comparison of porcine collagen paste injection and rectal advancement flap for the treatment of complex cryptoglandular anal fistulas: a 2-year follow-up study. Int J Colorectal Dis. 2018;33:1723-1731. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 8] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 44. | Han JG, Wang ZJ, Zheng Y, Chen CW, Wang XQ, Che XM, Song WL, Cui JJ. Ligation of Intersphincteric Fistula Tract vs Ligation of the Intersphincteric Fistula Tract Plus a Bioprosthetic Anal Fistula Plug Procedure in Patients With Transsphincteric Anal Fistula: Early Results of a Multicenter Prospective Randomized Trial. Ann Surg. 2016;264:917-922. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 30] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 45. | Meinero P, Mori L, Gasloli G. Video-assisted anal fistula treatment: a new concept of treating anal fistulas. Dis Colon Rectum. 2014;57:354-359. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 35] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 46. | Chew MH, Lee PJ, Koh CE, Chew HE. Appraisal of the LIFT and BIOLIFT procedure: initial experience and short-term outcomes of 33 consecutive patients. Int J Colorectal Dis. 2013;28:1489-1496. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 16] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 47. | Ellis CN. Outcomes with the use of bioprosthetic grafts to reinforce the ligation of the intersphincteric fistula tract (BioLIFT procedure) for the management of complex anal fistulas. Dis Colon Rectum. 2010;53:1361-1364. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 98] [Cited by in RCA: 66] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/