Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.113103
Revised: November 6, 2025
Accepted: December 10, 2025
Published online: February 27, 2026
Processing time: 163 Days and 1.6 Hours
In the current laparoscopic surgery practice of colorectal cancer (CRC), the four-port technique is more traumatic, whereas the single-port surgery is associated with technical difficulty and a limited field of view. Thus, the two-port technique, which is less traumatic and more feasible, becomes increasingly significant in clinical practice.
To compare the clinical effects of two-port and four-port laparoscopic techniques for CRC treatment.
In the review of the medical records of patients with CRC from March 2022 to March 2025, 80 cases of two-port laparoscopic radical resection (two-port group) and 70 cases of four-port laparoscopic resection (four-port group) were identified for direct surgical comparison. These groups were evaluated and compared for surgical indicators (surgical duration, total intraoperative hemorrhage, and total length of incision), postoperative recovery (time to first flatus/ambulation, and total hospitalization duration), postoperative complications (ileus, anastomotic fistula, surgical site infection, bleeding, uroschesis, and intraperitoneal abscess), gastrointestinal function (gastrin and motilin), oncological indices (carcinoembryonic antigen, cytokeratin 19 fragment antigen 21-1, and carbohydrate antigen 125), and humoral immunity [immunoglobulin (Ig) A/G/M].
The two-port and four-port groups were comparable in terms of operation time and total intraoperative bleeding. However, the two-port group showed lower values with respect to the total incision length, time to flatus/ambu
Compared with patients with CRC who underwent four-port laparoscopic surgery, those who underwent two-port laparoscopic resection recovered faster and were fairly safe. In addition, the gastrointestinal hormone disturbance was relatively mild, the serum tumor markers were significantly reduced, and the humoral immune response was enhanced.
Core Tip: This study compares the efficacy of two-port with that of four-port laparoscopic radical resection of colorectal cancer. The two-port approach shows clinical superiority, with reduced total incision length, quicker postoperative recovery, fewer total complications, and better gastrointestinal/humoral immune functions. The results can provide better surgical treatment options for patients with colorectal cancer.
- Citation: Xia HX, Peng S. Two-port vs four-port laparoscopic resection for colorectal cancer: Efficacy and outcomes. World J Gastrointest Surg 2026; 18(2): 113103
- URL: https://www.wjgnet.com/1948-9366/full/v18/i2/113103.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i2.113103
Colorectal cancer (CRC) is a fatal and multifactorial tumor disease. Sedentary lifestyles, smoking, obesity, spicy diet, alcohol abuse, and other factors may increase the risk of CRC[1,2]. As the third most common tumor globally, CRC is likely to occur in high-income countries, such as Europe, North America, and Australia, while presenting a low risk in low-income countries[3]. The pathological mechanism of CRC is related to mucosal inflammation. Continuous inflammation on epithelial proliferation can easily induce cancerization. Moreover, abnormal conditions, such as oxidative damage and DNA double-strand breaks, can further increase the risk of carcinogenesis[4]. Laparoscopic surgery is a curative treatment for CRC. Compared with open surgery, it reduces bleeding, promotes recovery, and reduces complications[5]. Traditional laparoscopic surgery in patients with CRC often requires placing 4 and 5 surgical ports, which may cause concurrent wound infection and greater damage to organs, hindering therapeutic effects[6,7]. The single-port technique often has limited clinical applications because of increased operative complexity, small surgical field of view, and prolonged operation time[8]. Thus, the two-port laparoscopic approach was developed based on a single-port to widen the operating field and reduce surgical complexity[9]. However, few relevant studies and reports have investigated its application to patients with CRC.
Based on the above background, this study attempted to evaluate the clinical effects of two-port in comparison with four-port laparoscopic surgery for CRC from a multidimensional perspective to provide new insights to optimize the surgical outcomes of patients with CRC. The results are clinically significant to further improve the medical experience of these patients.
From March 2022 to March 2025, 150 patients with CRC admitted to the study hospital were selected. The patients were divided according to the treatment method: (1) 80 patients who underwent two-port laparoscopic resection for CRC (two-port group); and (2) 70 patients who received four-port laparoscopic surgical treatment (four-port group). The sample size calculation did not rely on precalculated statistical power but was based on selecting eligible patients with CRC treated between March 2022 and March 2025.
The eligibility requirements were as follows: (1) Diagnosis of CRC[10]; (2) Age 18-80 years; (3) Stage I-III disease[11]; (4) First-time surgical candidates for laparoscopic radical surgery; and (5) Complete medical data.
The exclusion criteria were as follows: (1) Other malignancies; (2) Recent endocrine, chemotherapy, or radiotherapy treatment; (3) Severe immunosuppressive status; (4) Abdominal operation history; (5) Organic (cardiac, cerebral, pulmonary, hepatic, or renal) diseases; (6) Peritonitis, intestinal obstruction, or perforation; (7) Cognitive/communicative defects; and (8) American Association of Anesthesiologists score > III[12].
Patients in the two-port group underwent two-port laparoscopic radical resection for CRC. Briefly, patients were placed in the lithotomy position, and general anesthesia was administered via endotracheal intubation. Following routine disinfection and dressing, a 2-3 cm incision was made on the left side of the patient’s navel. The skin and tissues were incised, which served as the auxiliary operation port. An artificial CO2 pneumoperitoneum was established, and a Trocar was inserted approximately two fingers’ width from the anterior superior iliac spine on the right side, which served as the main operation port. After visualizing the lesion with the laparoscope, the tumor was resected: The right pararectal sulcus was incised, revealing the left Toldt, which was expanded. The inferior mesenteric artery lymph nodes were cleared, and a ligature was applied approximately 1 cm from the root of the ligament. The ligament of the inferior mesenteric vein was expanded outward at the same level. The sigmoid colon was freed, ensuring protection of the ureters and pelvic nerve plexus. Subsequently, the retrorectal, lateral, and anterior spaces were dissected. After the tumor was removed, the intestinal tube was disconnected to complete the resection. The resected tissue was placed in a specimen bag. The incision was sutured to achieve hemostasis, a drainage tube was then placed, and the abdominal cavity was closed.
The four-port group underwent four-port laparoscopic surgery as follows: Patients were placed in the lithotomy position, and general anesthesia was induced through tracheal intubation. A 100-mm Trocar was inserted at the upper edge of the navel as the main observation port. The location of the main operation port was the same as that in the two-port group. A secondary operation port was placed on the right side, and the assistant operation port was located at the midpoint of the line connecting the navel and the left anterior superior iliac spine. An auxiliary incision measuring 6-8 cm was made in the middle of the lower part of the umbilicus. Subsequent procedures, including specimen extraction, drainage tube placement, and intestinal anastomosis, were performed identically to the two-port technique.
Operative measures: This included surgical duration, intraoperative hemorrhage volume, and cumulative incision length in each cohort.
Postoperative recovery: This included the time to first flatus, ambulation initiation, and hospital stay duration.
Complications: Patients were monitored for ileus, anastomotic fistula, surgical site infection (SSI), postoperative bleeding, uroschesis, and intraperitoneal abscess, with their frequency rates computed.
Gastrointestinal function markers: Specifically, 5-mL fasting venous blood was obtained during morning hours before surgical intervention and after a 30-day recovery. Centrifuged serum specimens were subjected to radioimmunological determination of gastrin (GAS) and motilin (MT) concentrations.
Oncological biomarkers: Serum carcinoembryonic antigen (CEA), cytokeratin 19 fragment antigen 21-1 (Cyfra 21-1), and carbohydrate antigen 125 (CA125) were assessed using automated immunoassay systems before surgery and 1 month after surgery.
Humoral immunity: Preoperative and postoperative (1 month) serum immunoglobulin (Ig) A/G/M measurements were performed by turbidimetric immunoassay.
In this study, quantitative data deviating from a normal distribution are expressed as the median (interquartile range) [M(Q1, Q3)]. Normally distributed quantitative data are presented as mean ± SD. Between-group differences for quantitative variables were examined through independent t-tests, whereas within-group changes (e.g., preoperative vs postoperative measurements) were analyzed using paired t-tests. Categorical variables, summarized as n (%), were subjected to χ² tests to determine group differences. IBM SPSS Statistics version 5.0 facilitated all computations, with significance indicated by P < 0.05.
The intergroup comparison (Table 1) showed comparable baseline patient features (e.g., sex, age, body mass index, tumor, node, metastasis stage, lesion location, and tumor diameter; P > 0.05).
| General data | Two-port group (n = 80) | Four-port group (n = 70) | χ2/Z/t | P value |
| Sex | 0.058 | 0.809 | ||
| Male | 45 (56.25) | 38 (54.29) | ||
| Female | 35 (43.75) | 32 (45.71) | ||
| Age (years) | 57.20 ± 7.30 | 59.29 ± 9.21 | 1.549 | 0.124 |
| Body mass index (kg/m2) | 22.00 (20.00, 24.00) | 22.00 (20.00, 25.00) | -0.195 | 0.845 |
| Tumor, node, metastasis stage | 1.306 | 0.520 | ||
| I | 24 (30.00) | 17 (24.29) | ||
| II | 22 (27.50) | 25 (35.71) | ||
| III | 34 (42.50) | 28 (40.00) | ||
| Lesion location | 0.076 | 0.782 | ||
| Colon cancer | 52 (65.00) | 47 (67.14) | ||
| Rectal cancer | 28 (35.00) | 23 (32.86) | ||
| Tumor diameter (cm) | 4.09 ± 1.24 | 3.83 ± 1.39 | 1.211 | 0.228 |
The two groups were comparable with respect to surgical duration and intraoperative hemorrhage volume (P > 0.05). However, the two-port group exhibited a smaller cumulative incision length than the four-port group (P < 0.001; Table 2).
| Operative measures | Two-port group (n = 80) | Four-port group (n = 70) | t value | P value |
| Surgical duration (minutes) | 99.69 ± 13.85 | 103.07 ± 17.51 | 1.319 | 0.189 |
| Intraoperative hemorrhage volume (mL) | 28.27 ± 8.53 | 30.63 ± 10.85 | 1.489 | 0.139 |
| Cumulative incision length (cm) | 5.58 ± 0.80 | 8.96 ± 1.20 | 20.520 | < 0.001 |
The two-port group had shorter time to first flatus/ambulation and shorter hospital stays than the four-port group (P < 0.001; Table 3).
| Postoperative recovery indexes | Two-port group (n = 80) | Four-port group (n = 70) | t value | P value |
| Time to first flatus (hours) | 46.64 ± 7.98 | 65.54 ± 10.67 | 12.376 | < 0.001 |
| Ambulation initiation (hours) | 29.52 ± 7.97 | 35.11 ± 10.05 | 3.795 | < 0.001 |
| Hospital stays duration (days) | 8.46 ± 1.76 | 10.66 ± 2.39 | 6.470 | < 0.001 |
Table 4 summarizes the postoperative complication rates. The rates of ileus, anastomotic fistula, SSI, postoperative bleeding, uroschesis, and intraperitoneal abscess were lower in the two-port group than in the four-port group (P = 0.019).
| Complications | Two-port group (n = 80) | Four-port group (n = 70) | χ2 | P value |
| Ileus | 0 (0.00) | 1 (1.43) | ||
| Anastomotic fistula | 2 (2.50) | 2 (2.86) | ||
| Surgical site infection | 1 (1.25) | 3 (4.29) | ||
| Postoperative bleeding | 0 (0.00) | 2 (2.86) | ||
| Uroschesis | 2 (2.50) | 5 (7.14) | ||
| Intraperitoneal abscess | 3 (3.75) | 4 (5.71) | ||
| Total | 8 (10.00) | 17 (24.29) | 5.486 | 0.019 |
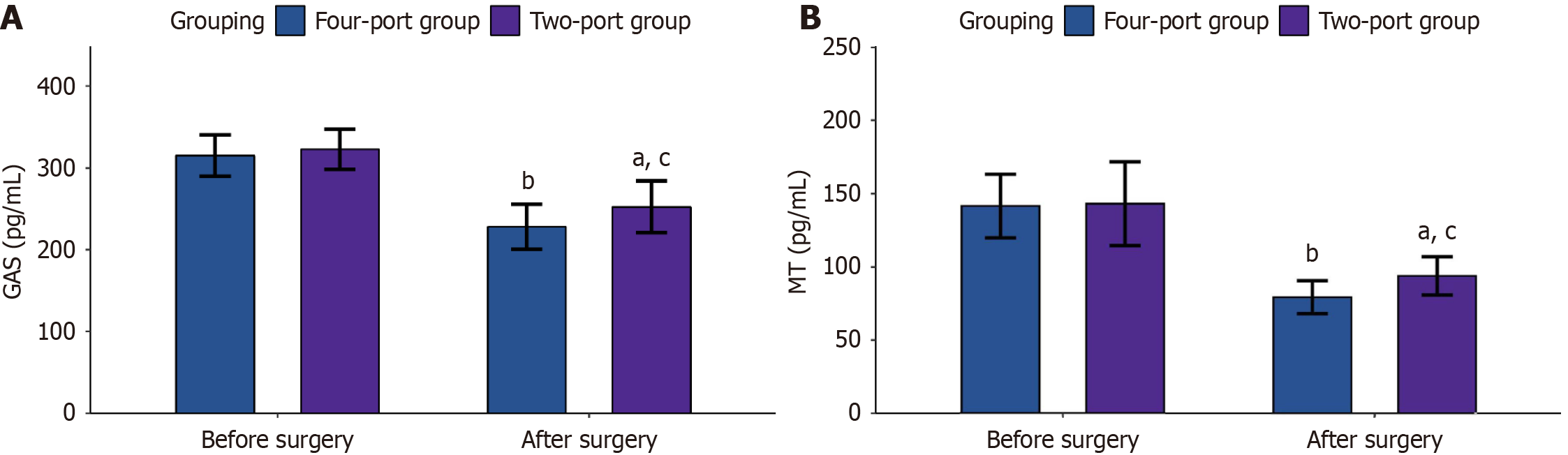
The preoperative values for all gastrointestinal (GI) function markers (GAS and MT) were comparable across the study groups (P > 0.05; Figure 1). Postoperatively, all values decreased markedly (all P < 0.001); however, the two-port approach maintained superior GAS and MT concentrations relative to the four-port technique (all P < 0.001).
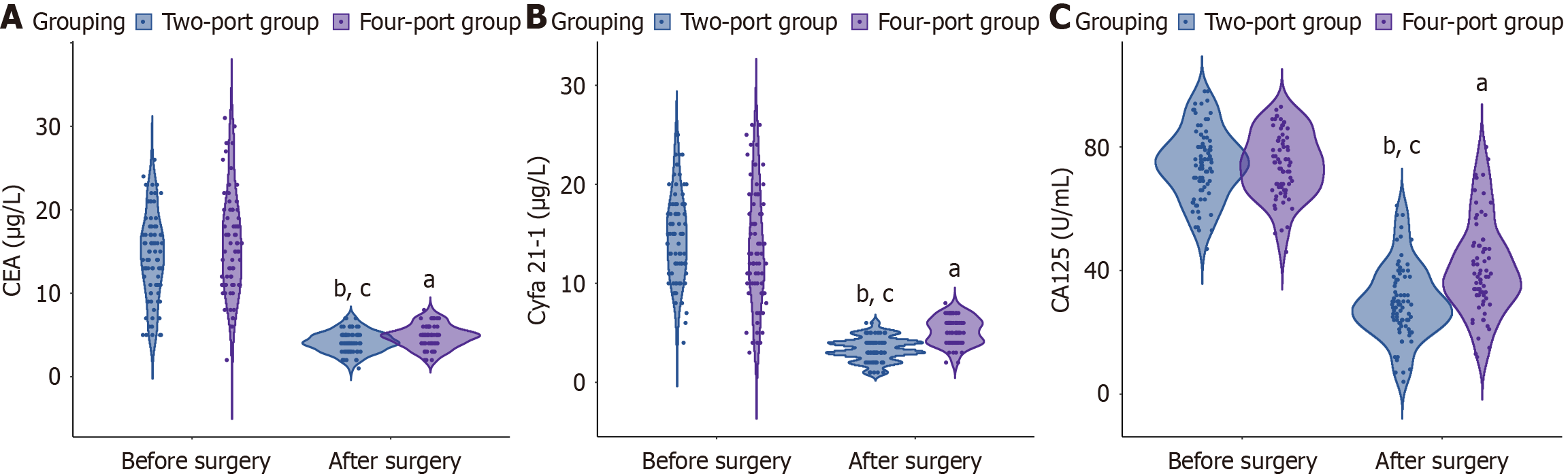
Figure 2 demonstrates comparable preoperative concentrations of CEA, Cyfra 21-1, and CA125 between the two cohorts (P > 0.05). Following surgery, both groups demonstrated significant decreases in all tumor markers (all P < 0.001), with the two-port approach showing superior reduction in CEA (P = 0.004), Cyfra 21-1 (P < 0.001), and CA125 (P < 0.001) concentrations relative to the four-port technique.
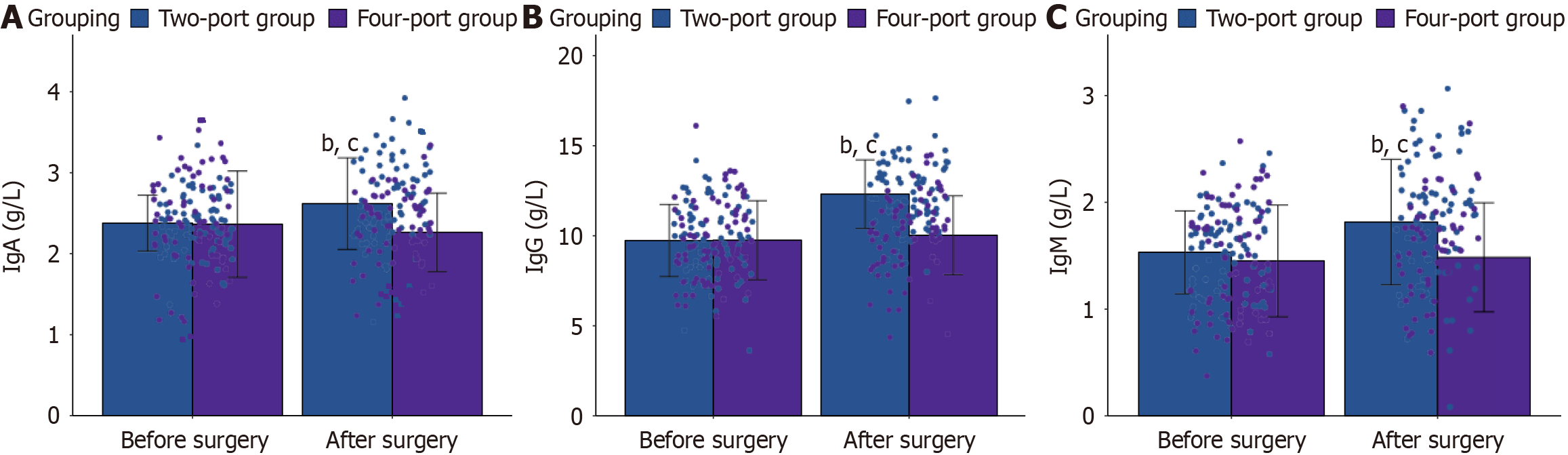
Before surgery, IgA, IgG, and IgM measurements did not differ significantly between the groups (P > 0.05). The two-port group had higher postoperative Ig levels than the four-port group (P < 0.001; Figure 3).
CRC has high late diagnosis and mortality rates, with considerable geographical differences in the risk of onset and death. Moreover, CRC tends to become more prevalent among younger people in developed countries[13,14]. To prevent and treat CRC and optimize related management, this study tried to compare and analyze the clinical effects of two surgical techniques and seek better solutions for laparoscopic surgical therapy for patients with CRC.
Initially, no significant intergroup variations were found in surgical duration and intraoperative bleeding; however, cumulative incision length was markedly reduced in the two-port group. This finding highlights the advantages of the two-port technique in achieving smaller incisions. Gu et al[15] did not find a significant difference in the operation time and blood loss volume between the single-incision and multi-port laparoscopic surgery for patients with CRC, similar to the results of the present study. Kim et al[16] also did not observe a significant difference in the operation time and intraoperative blood loss between the two-port and four-port laparoscopic techniques in patients undergoing ovarian cystectomy, aligning with our findings.
Moreover, time to first flatus/ambulation and overall hospitalization durations were shorter with the two-port approach, indicating enhanced postoperative recovery. In the study of Jiang et al[17], the two-port laparoscopic approach for patients with sigmoid colon cancer and upper rectal cancer resulted in a shorter total incision length than the four-port laparoscopic approach. This approach also facilitated a shorter time to first ambulation, exhaust, defecation, and liquid diet, which complements the results of this study.
Furthermore, significant reductions were observed in the overall complications (ileus, anastomotic fistula, SSI, postoperative bleeding, uroschesis, and intraperitoneal abscess) in the two-port group. In the study by Wang et al[18], single-incision plus single-port surgery was found to have certain clinical safety and minimally invasive characteristics when applied to patients with colon cancer, supporting the results of the present study. Additionally, Angulo et al[19] reported the higher effectiveness of the two-port than the four-port laparoscopic approach for radical cystectomy in reducing postoperative pain. This finding provides another potential clinical advantage for the clinical application of two-port laparoscopic surgery in CRC.
The postoperative levels of GAS and MT of the two-port group significantly decreased, but were still markedly higher than those in the four-port group, suggesting that the two-port group offered better protection of GI function. GAS and MT, both GI hormones, are closely related to the GI function of patients with CRC undergoing surgery, and can indicate whether patients experienced surgery-related stress[20]. Past evidence revealed markedly downregulated GAS and MT levels in patients with CRC following laparoscopic radical surgery. Hence, higher postoperative GAS and MT levels are indicative of relatively lesser surgical trauma and better GI function recovery[21], which is consistent with the outcomes of the two-port laparoscopic surgeries in the present study. The marked decreases in postoperative CEA, Cyfra21-1, and CA125 levels in the two-port group, lower than those in the four-port group, suggest that the two-port laparoscopic approach is more effective in preventing the progression of CRC. In previous studies, CEA has been shown as a reliable predictor of recurrence and clinical outcomes of laparoscopic radical surgery for CRC. Cyfa 21-1 is the most sensitive biological indicator of patients with recurrent CRC and is closely related to Dukes’ staging. CA125 shows a close connection with CRC outcomes. All three are strongly linked to CRC development[22-24].
The notable postoperative increases in IgA, IgG, and IgM expression in the two-port group in comparison with those in the four-port group support the former’s better performance in enhancing humoral immunity. In patients with CRC, short-term postoperative intervention with abdominal surgery may lead to weakened cellular immune function because of surgical trauma and stress. As patients’ condition improves and GI function enhances, their humoral immune function usually recovers well 1 month after surgery, which is similar to the results of Xu et al[25] and Bohne et al[26].
Several limitations should be noted. First, given the lack of sleep/life quality and adverse mood evaluations, supplementary analyses in these areas can help elucidate the potential advantages of two-port laparoscopic radical resection in CRC. Second, long-term patient outcomes (5-10 years) should be tracked to understand the lasting effects of the two approaches. Finally, a health economic analysis of the two approaches is necessary for the clinical promotion of the two-port technique. These deficiencies will be addressed in future research.
The results reveal that for CRC treatment, the two-port laparoscopic radical resection has more clinical merits than the four-port approach. It stands out particularly in shortening the cumulative incision length, boosting postoperative recovery, lowering the total complication rate, safeguarding patients’ GI and humoral immune functions, and curbing disease progression.
| 1. | Pardamean CI, Sudigyo D, Budiarto A, Mahesworo B, Hidayat AA, Baurley JW, Pardamean B. Changing Colorectal Cancer Trends in Asians: Epidemiology and Risk Factors. Oncol Rev. 2023;17:10576. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 45] [Cited by in RCA: 34] [Article Influence: 11.3] [Reference Citation Analysis (1)] |
| 2. | Xu L, Zhao J, Li Z, Sun J, Lu Y, Zhang R, Zhu Y, Ding K, Rudan I, Theodoratou E, Song P, Li X; Global Health Epidemiology Research Group (GHERG). National and subnational incidence, mortality and associated factors of colorectal cancer in China: A systematic analysis and modelling study. J Glob Health. 2023;13:04096. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 28] [Reference Citation Analysis (0)] |
| 3. | Papier K, Bradbury KE, Balkwill A, Barnes I, Smith-Byrne K, Gunter MJ, Berndt SI, Le Marchand L, Wu AH, Peters U, Beral V, Key TJ, Reeves GK. Diet-wide analyses for risk of colorectal cancer: prospective study of 12,251 incident cases among 542,778 women in the UK. Nat Commun. 2025;16:375. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 54] [Cited by in RCA: 47] [Article Influence: 47.0] [Reference Citation Analysis (0)] |
| 4. | Sato Y, Tsujinaka S, Miura T, Kitamura Y, Suzuki H, Shibata C. Inflammatory Bowel Disease and Colorectal Cancer: Epidemiology, Etiology, Surveillance, and Management. Cancers (Basel). 2023;15:4154. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 84] [Cited by in RCA: 74] [Article Influence: 24.7] [Reference Citation Analysis (1)] |
| 5. | Vilsan J, Maddineni SA, Ahsan N, Mathew M, Chilakuri N, Yadav N, Munoz EJ, Nadeem MA, Abbas K, Razzaq W, Abdin ZU, Ahmed M. Open, Laparoscopic, and Robotic Approaches to Treat Colorectal Cancer: A Comprehensive Review of Literature. Cureus. 2023;15:e38956. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 11] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 6. | Liu ZM, Yao QJ, Pei F, He F, Zhao Y, Huang J. Efficacy and safety of reduced-port laparoscopic surgery versus conventional laparoscopic surgery for colorectal cancer. BMC Cancer. 2025;25:187. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 7. | Mostafa OES, Zaman S, Beedham W, Kakaniaris G, Husain N, Kumar L, Akingboye A, Waterland P. Systematic review and meta-analysis comparing outcomes of multi-port versus single-incision laparoscopic surgery (SILS) in Hartmann's reversal. Int J Colorectal Dis. 2024;39:190. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 8. | Lv C, Wu S, Wu Y, Shi J, Su Y, Fan Y, Kong J, Yu X. Single-incision laparoscopic versus traditional multiport laparoscopic colorectal surgery--a cumulative meta-analysis and systematic review. Int J Colorectal Dis. 2013;28:611-621. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 13] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 9. | Yi SW. Postoperative abdominopelvic adhesion and umbilical wound validation after single-port laparoscopy or two-port laparoscopy for gynecological surgery: a comparison with conventional laparoscopy. Arch Gynecol Obstet. 2025;311:1599-1607. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 10. | Ness RM, Llor X, Abbass MA, Bishu S, Chen CT, Cooper G, Early DS, Friedman M, Fudman D, Giardiello FM, Glaser K, Gurudu S, Hall M, Huang LC, Issaka R, Katona B, Kidambi T, Lazenby AJ, Maratt J, Markowitz AJ, Marsano J, May FP, Mayer RJ, Olortegui K, Patel S, Peter S, Porter LD, Shafi M, Stanich PP, Terdiman J, Vu P, Weiss JM, Wood E, Cassara CJ, Sambandam V. NCCN Guidelines® Insights: Colorectal Cancer Screening, Version 1.2024. J Natl Compr Canc Netw. 2024;22:438-446. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 28] [Article Influence: 14.0] [Reference Citation Analysis (0)] |
| 11. | Chizhikova M, López-Úbeda P, Martín-Noguerol T, Díaz-Galiano MC, Ureña-López LA, Luna A, Martín-Valdivia MT. Automatic TNM staging of colorectal cancer radiology reports using pre-trained language models. Comput Methods Programs Biomed. 2025;259:108515. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 5] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 12. | Matsubara D, Soga K, Ikeda J, Konishi T, Uozumi Y, Takeda R, Kanazawa H, Komatsu S, Shimomura K, Taniguchi F, Shioaki Y, Otsuji E. Laparoscopic Surgery for Elderly Colorectal Cancer Patients With High American Society of Anesthesiologists Scores. Anticancer Res. 2023;43:5637-5644. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 13. | Anugwom C, Braimoh G, Sultan A, Johnson WM, Debes JD, Mohammed A. Epidemiology and genetics of early onset colorectal cancer-African overview with a focus on Ethiopia. Semin Oncol. 2023;50:28-33. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 11] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 14. | Roshandel G, Ghasemi-Kebria F, Malekzadeh R. Colorectal Cancer: Epidemiology, Risk Factors, and Prevention. Cancers (Basel). 2024;16:1530. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 292] [Cited by in RCA: 217] [Article Influence: 108.5] [Reference Citation Analysis (4)] |
| 15. | Gu C, Wu Q, Zhang X, Wei M, Wang Z. Single-incision versus conventional multiport laparoscopic surgery for colorectal cancer: a meta-analysis of randomized controlled trials and propensity-score matched studies. Int J Colorectal Dis. 2021;36:1407-1419. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 16] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 16. | Kim ML, Song T, Seong SJ, Yoon BS, Joo WD, Jung YW, Kang JH, Jun HS. Comparison of single-port, two-port and four-port laparoscopic surgery for cyst enucleation in benign ovarian cysts. Gynecol Obstet Invest. 2013;76:57-63. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 17. | Jiang F, Ji M, Jin F, Liu J, Liu X. Clinical application of two-port laparoscopic surgery in sigmoid colon and upper rectal cancer resection. Front Oncol. 2023;13:1248280. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 18. | Wang Y, Deng H, Mou T, Li J, Liu H, Zhou H, Li G. Short-term outcomes of single-incision plus one-port laparoscopic versus conventional laparoscopic surgery for rectosigmoid cancer: a randomized controlled trial. Surg Endosc. 2019;33:840-848. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 29] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 19. | Angulo JC, García-Tello A, Mateo E, Gimbernat H, Redondo C, Andrés G. Two-Port Approach Compared to Standard Laparoscopic Radical Cystectomy. J Endourol. 2015;29:1030-1037. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 20. | Li WB, Li J, Yu W, Gao JH. Short-term efficacy of laparoscopic radical resection for colorectal cancer and risk of unplanned reoperation after surgery. World J Gastrointest Surg. 2025;17:102442. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 21. | Liu B, Yao C, Li H. Laparoscopic Radical Resection of Colorectal Cancer in the Treatment of Elderly Colorectal Cancer and Its Effect on Gastrointestinal Function. Front Surg. 2022;9:840461. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 22. | Baqar AR, Wilkins S, Staples M, Angus Lee CH, Oliva K, McMurrick P. The role of preoperative CEA in the management of colorectal cancer: A cohort study from two cancer centres. Int J Surg. 2019;64:10-15. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 62] [Article Influence: 8.9] [Reference Citation Analysis (0)] |
| 23. | Lee JH. Clinical Usefulness of Serum CYFRA 21-1 in Patients with Colorectal Cancer. Nucl Med Mol Imaging. 2013;47:181-187. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 14] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 24. | Björkman K, Mustonen H, Kaprio T, Kekki H, Pettersson K, Haglund C, Böckelman C. CA125: A superior prognostic biomarker for colorectal cancer compared to CEA, CA19-9 or CA242. Tumour Biol. 2021;43:57-70. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 39] [Article Influence: 7.8] [Reference Citation Analysis (1)] |
| 25. | Xu D, Li J, Song Y, Zhou J, Sun F, Wang J, Duan Y, Hu Y, Liu Y, Wang X, Sun L, Wu L, Ding K. Laparoscopic surgery contributes more to nutritional and immunologic recovery than fast-track care in colorectal cancer. World J Surg Oncol. 2015;13:18. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 20] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 26. | Bohne A, Grundler E, Knüttel H, Fürst A, Völkel V. Influence of Laparoscopic Surgery on Cellular Immunity in Colorectal Cancer: A Systematic Review and Meta-Analysis. Cancers (Basel). 2023;15:3381. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 9] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/