Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.113441
Revised: September 29, 2025
Accepted: December 10, 2025
Published online: February 27, 2026
Processing time: 176 Days and 1.9 Hours
Endoscopic submucosal dissection (ESD) has become the standard endoscopic treatment for early gastric cancer (EGC), offering high en bloc resection and cu
To construct ESD for patients with EGC assisted by digestive endoscopy, the perioperative MDT nursing model for ESD treatment was adopted, and its effect was evaluated.
A total of 99 patients diagnosed with EGC in our hospital from April 2022 to April 2025 were prospectively selected as the observation group research subjects to receive the MDT nursing mode. Another 99 patients were selected in a 1:1 ratio as the control group to receive the conventional nursing mode. Both groups received ESD treatment. The recovery of intestinal rumbling sounds after surgery, the time of first getting out of bed for activities, the average length of hospital stay, and the satisfaction situation were compared between the two groups.
Intergroup comparisons revealed that the observation group patients had significantly better outcomes in terms of time to bowel sound recovery (12.53 ± 1.21) hours, first time out of bed activity (23.53 ± 2.34) hours, length of hospital stay (6.63 ± 0.46) days, and overall complication rate (3.03%), along with a significantly higher satisfaction rate of 100% compared to 80.81% in the control group (P < 0.05).
MDT can significantly promote the recovery of EGC patients after ESD treatment assisted by digestive endoscopy, improve the treatment effect of patients, and increase patient satisfaction. It is worthy of clinical promotion and application.
Core Tip: This study constructed a perioperative multidisciplinary team (MDT) nursing model for patients with early gastric cancer undergoing digestive endoscopy-assisted endoscopic submucosal dissection. Compared to conventional care, the MDT model significantly shortened postoperative bowel sound recovery time, first ambulation time, and hospital stay, while achieving a 100% patient satisfaction rate. The findings demonstrate that the MDT approach optimizes recovery outcomes and enhances the quality of nursing care for early gastric cancer patients, warranting clinical promotion.
- Citation: Qian YP, Cai H, Tang SY, Zhou HP, Han Q, Tu HM. Perioperative multidisciplinary nursing model for endoscopic gastric submucosal dissection development and effect evaluation. World J Gastrointest Surg 2026; 18(2): 113441
- URL: https://www.wjgnet.com/1948-9366/full/v18/i2/113441.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i2.113441
Gastric cancer (GC) is a common malignant tumor of the digestive tract. Epidemiological data show[1] that the incidence and mortality rates are significantly higher in men, with 15.8 new cases and 11 deaths per 100000 people annually, com
General information: A total of 99 patients diagnosed with EGC in our hospital from April 2022 to April 2025 were prospectively selected as the observation group, and another 99 patients were included in the control group at a 1:1 ratio. No significant differences were observed in the general characteristics between the two groups, as shown in Table 1. Based on the Gastric Cancer Diagnosis and Treatment Guidelines[7], pathological diagnosis was defined as a malignant tumor invading only the gastric mucosal layer or submucosa, regardless of lymph node metastasis or tumor size.
| Group | Control group (n = 99) | Observation group (n = 99) | t | P value | |
| Gender | Male | 53 (53.54) | 51 (51.53) | 0.081 | 0.775 |
| Female | 46 (46.46) | 48 (48.48) | |||
| Age (mean ± SD, years) | 61.75 ± 9.82 | 61.10 ± 9.16 | 0.451 | 0.63 | |
| Place of residence | Countryside | 52 (52.53) | 51 (51.52) | 0.02 | 0.887 |
| Town | 47 (47.47) | 48 (48.48) | |||
| Educational level | Primary school and below | 55 (55.56) | 53 (53.54) | 0.233 | 0.972 |
| Junior high school | 22 (22.22) | 24 (24.24) | |||
| High school | 15 (15.15) | 16 (16.16) | |||
| College degree or above | 7 (7.07) | 6 (6.06) | |||
| Coronary heart disease or diabetes | Yes | 36 (36.36) | 33 (33.33) | 0.2 | 0.654 |
| None | 63 (63.64) | 66 (66.67) | |||
| Pathological staging of the disease | I | 33 (33.33) | 31 (31.31) | 1.173 | 0.756 |
| II | 18 (18.18) | 21 (21.21) | |||
| III | 33 (33.33) | 28 (28.28) | |||
| IV | 15 (15.15) | 19 (19.19) | |||
| BMI (mean ± SD, kg/m2) | 20.57 ± 1.23 | 20.34 ± 1.89 | 1.014 | 0.311 | |
| PG-SGA score (mean ± SD, points) | 10.45 ± 3.67 | 10.78 ± 3.12 | 0.681 | 0.496 | |
Inclusion criteria: Meeting the diagnostic criteria for EGC[7]; meeting the indications for ESD[8]: (1) Tumor infiltration limited to the mucosal layer (Tis or T1a); (2) Histologically assessed as differentiated GC, with no size restriction if non-ulcerative, or tumor diameter ≤ 3 cm if ulcerated; and (3) Histologically assessed as undifferentiated GC, which must be non-ulcerative and have a tumor diameter ≤ 2 cm.
Exclusion criteria: (1) Presence of other malignant tumors; (2) Previous radical treatments such as radiotherapy or chemotherapy; (3) Preoperative evidence of distant tumor metastasis, involvement of adjacent organs, or signs of tumor recurrence; (4) Severe impairment of liver or kidney function, or inadequate function of vital organs rendering the patient unable to tolerate surgery; and (5) Surgical procedures performed under emergency conditions.
Literature search selection criteria: First, literature retrieval strategy: The search keywords include: EGC, endoscopic mucosal dissection, digestive endoscopy-assisted ESD, emergency rescue room, nursing quality, and nursing evaluation. Search English databases such as PubMed, EMBASE, Ovid, etc. Literature screening criteria: (1) Exclude literature with similar or duplicated content; (2) Exclude non Chinese or English literature; (3) Exclude literature that cannot be obtained in full or read; (4) Exclude conference abstracts, case studies, and other types of literature; and (5) Exclude literature with a quality rating of C. Literature quality assessment[9]: It includes 6 criteria, each corresponding to 4 evaluation result options: Compliant, non compliant, applicable and not applicable. When the content of the literature is completely consistent with the criteria description, it indicates that the risk of bias is at its lowest level, which is Class A; if the content of the literature partially meets the criteria and the risk of bias is moderate, it will be classified as level B; if it is completely inconsistent and has a high risk of bias, it is classified as level C. Second, extraction of evaluation indicators: The research team used a self-designed literature information extraction table to collect relevant data, including literature titles, types, publication years, research recommendations, and quality assessment conclusions. Two researchers indepen
Compilation of inquiry questionnaire: The research team designed the first round of the inquiry questionnaire through collective discussion, which consists of three main parts. The specific content is as follows: (1) Introduction: Including acknowledgements, research objectives, research scope, and guidelines for filling out; (2) Expert background investigation: Basic information of the expert, level of understanding of the content, and evaluation criteria. Basic information includes age, educational background, professional title, work experience, etc. According to the level of understanding of the content, it is divided into five levels, with corresponding scores ranging from 1 to 5. The evaluation criteria include intuitive judgment, theoretical reasoning, practical experience, and literature review, and are divided into three levels based on the degree of influence of expert evaluation: High, medium, and low; and (3) Questionnaire subject: It includes 3 primary indicators, 17 secondary indicators, and 42 tertiary indicators. According to the importance of the indicators, they are divided into five levels, ranging from 1 to 5 points, for experts to provide additional opinions and suggestions.
Selection of inquiry experts: In this study, experts participating in the inquiry were selected based on strict criteria, as follows: (1) Experts must have work experience in multidisciplinary nursing management, nursing education, and related fields; (2) Having worked in the aforementioned fields for over 10 years; (3) Holding a vice senior or higher professional title; (4) Having a bachelor’s degree or higher; and (5) Have a good understanding of the research project and have a high enthusiasm for the research content. Based on this, a total of 16 experts were selected to participate in the inquiry.
Inquiry implementation process: After discussion by the research team, considering convenience, email was chosen as the method of sending the questionnaire. The researchers sent an electronic questionnaire to the experts’ email through a dedicated email and notified them by phone to download the questionnaire. They also communicated that the qu
Treatment methods: Using a high-definition electronic gastroscope (Olympus, CV-290 model, Japan) system to determine the exact location of the lesion, and using a high-frequency electric knife (VIO300D model, Germany) to mark around the lesion. Inject a small amount of glycerol fructose solution into multiple points in the submucosal layer of the marked area until the mucosa is locally raised and separated from the muscle layer. Then, use the Olympus KD-650 L along the marked points. High frequency electric knife is used to cut open the mucosa and peel off the diseased tissue in the sub
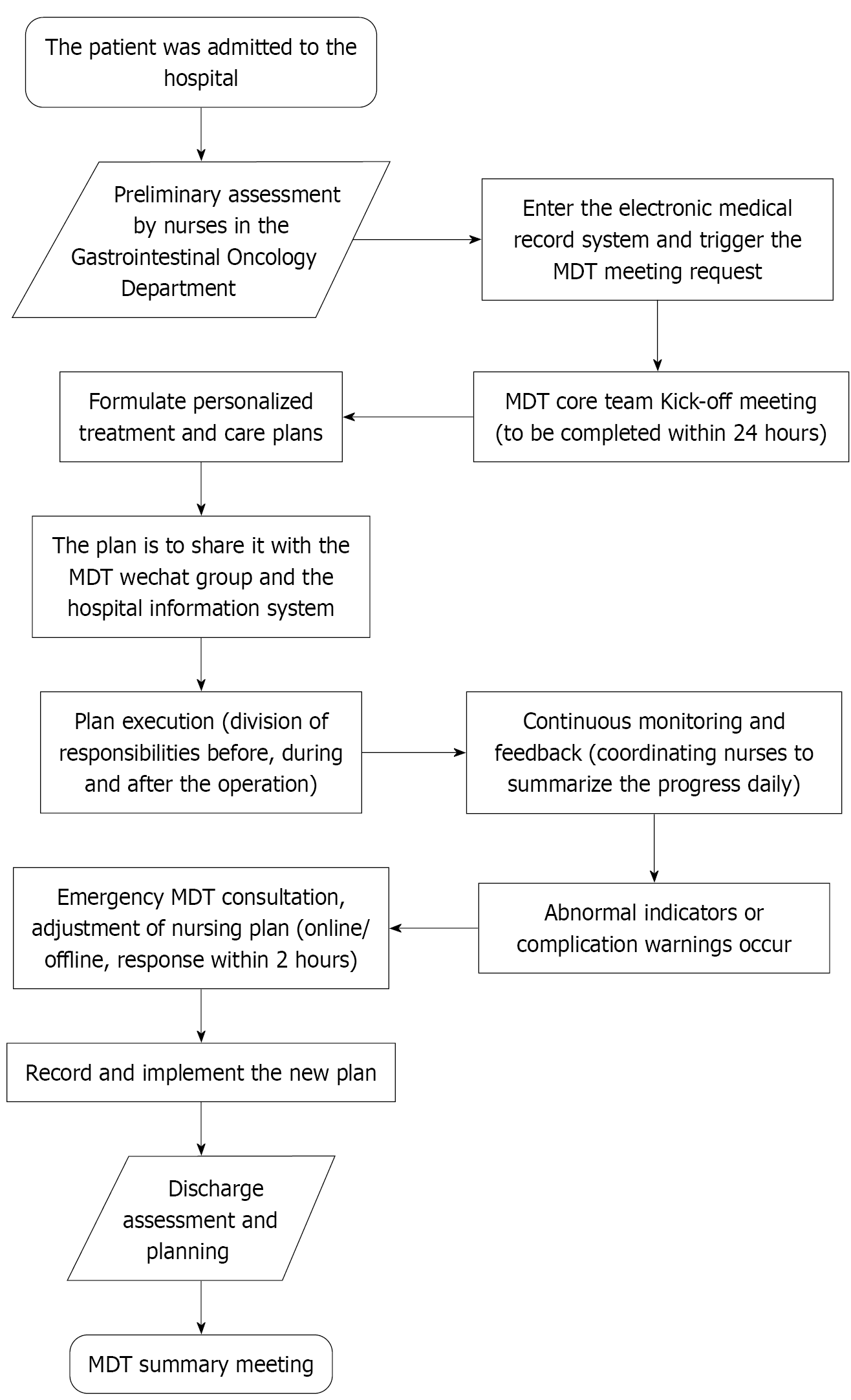
Perioperative MDT method: Control group: Receiving standard care, nursing content: Observing the condition, assisting the physician in completing surgery, changing medication according to medical advice, providing health education, dietary advice, and other routine nursing measures. Observation group: Receive MDT collaborative care based on the control group. (1) Establish a multidisciplinary nursing team consisting of nurses specializing in digestive endoscopy and surgical personnel specializing in gastrointestinal tumors. The team includes 5 gastrointestinal oncology nurses (res
Objective indicators: According to the hospital medical record system, the recovery time of postoperative bowel sounds, the first time of getting out of bed activity, and the average length of hospital stay were collected for two groups of research subjects.
Satisfaction survey: Research on evaluating nursing satisfaction through self-made measurements. After evaluation, the Cronbach’s alpha coefficient of the scale reached 0.91, indicating high reliability and validity. The scale adopts a multidimensional evaluation architecture, consisting of 6 dimensions, each with 5 sub-items, for a total of 30 items. Divide the evaluation results into four levels: Satisfied, somewhat satisfied, average, and dissatisfied. After the intervention phase, conduct a satisfaction questionnaire survey and statistics.
The participation enthusiasm of experts is reflected in the proportion of valid questionnaires collected. The data analysis was conducted using SPSS 27.0 software, and the Analytic Hierarchy Process was used to determine the weights of each indicator. The calculation of indicator weights is carried out using the Yaanalytic Hierarchy Process V0.6.0 software to construct a hierarchical structure model. Measurement data, results (mean ± SD) represent inter-group comparison t-test; count data, display results in proportion, and compare between groups using a χ2 test. Using P < 0.05 as the testing criterion.
This study selected 16 experts to participate in the inquiry, including 3 males and 13 females; age ≤ 40 years old, 41-50 years old, 51-55 years old, 5, 7, and 4 cases respectively; 12 cases with bachelor’s and master’s degrees; 5 cases of intermediate professional title, 7 cases of deputy senior title, and 4 cases of senior professional title; work experience of 8-14 years, 15-20 years, ≥ 21 years, 5, 6, 5 cases; professional directions include clinical nursing, nursing management, nursing research, and medical care for 5, 6, 2, and 3 cases.
This study used the Delphi expert inquiry method to collect professional opinions from two rounds of experts. During each round of inquiry, questionnaires were distributed to 16 experts, and both rounds of questionnaires achieved 100% effective responses. The experts have a high willingness and enthusiasm to participate in this study. The authoritative evaluation of experts adopts Cr as a quantitative evaluation, consisting of two dimensions: Expert familiarity (Cs) and judgment basis (Ca). The calculation formula is Cr = (Ca + Cs)/2, and the results are shown in Table 2.
| Round | Cs | Ca | Cr |
| Round one | 0.803 | 0.712 | 0.758 |
| The second round | 0.903 | 0.753 | 0.828 |
This study reflects the concentration of expert opinions through the ratio of the indicator importance score to the full score. The results of the second round of inquiry showed that the importance scores of each indicator were between 4.25 points and 5.00 points, and the full score ratio reached or exceeded 53.6%, indicating that experts generally recognize and attach great importance to these indicators.
In this study, the Kendall’s W coefficient was used to evaluate the degree of coordination among expert opinions, with values ranging from 0 to 1. During the two rounds of expert inquiry in this study, the Kendall harmony coefficients obtained were 0.416 and 0.439, respectively. Through comparative analysis, it can be seen that the coordination of expert opinions in the second round of expert inquiry showed an improvement trend compared to the first round, and there was a statistical difference (P < 0.05).
In this study, the coefficient of variation is used to measure the degree of dispersion of experts’ opinions on a certain indicator. The calculation method for the coefficient of variation is the ratio of s to. The results of the second round of expert inquiries showed that the coefficient of variation for the primary indicators ranged from 0.00 to 0.12, for the secondary indicators from 0.00 to 0.23, and for the tertiary indicators from 0.04 to 0.19. This indicates that there are differences in the volatility of expert opinions among different levels of indicators, with the first level indicator having the most concentrated expert opinions, while the third level indicator has relatively greater volatility.
Table 3 shows the inquiry results of the MDT nursing quality index system for EGC patients during the perioperative period.
| Indicator | Importance (mean ± SD, points) | Coefficient of variation | Weight |
| 1 Structural indicators | 4.50 ± 0.55 | 0.12 | 0.1200 |
| 1.1 Human resource allocation | 4.70 ± 0.45 | 0.10 | 0.0900 |
| 1.1.1 Nurse-to-patient ratio | 4.60 ± 0.40 | 0.08 | 0.0080 |
| 1.1.2 Nurse skill level composition ratio | 4.75 ± 0.30 | 0.06 | 0.0070 |
| 1.1.3 Presence of a multidisciplinary enhanced recovery after surgery (ERAS) team | 4.90 ± 0.25 | 0.05 | 0.0120 |
| 1.1.4 Average nursing hours per 24 hours per hospitalized patient | 4.70 ± 0.50 | 0.10 | 0.0030 |
| 1.2 Skill level and concept | 4.75 ± 0.35 | 0.07 | 0.1100 |
| 1.2.1 Pass rate of nurse specialist skill training and assessment | 4.85 ± 0.25 | 0.05 | 0.0230 |
| 1.2.2 Implementation rate of nurse training on ERAS concepts | 4.80 ± 0.30 | 0.06 | 0.0230 |
| 1.3 Nursing protocols and procedures | 4.70 ± 0.35 | 0.07 | 0.1200 |
| 1.3.1 Pass rate of training on perioperative gastric cancer nursing protocols | 4.85 ± 0.25 | 0.05 | 0.0230 |
| 1.3.2 Pass rate of training on nasoenteric tube care protocols | 4.80 ± 0.30 | 0.06 | 0.0070 |
| 1.3.3 Pass rate of training on abdominal drainage tube care protocols | 4.75 ± 0.25 | 0.05 | 0.0070 |
| 1.3.4 Pass Rate of training on venous catheter maintenance procedures | 4.70 ± 0.30 | 0.06 | 0.0070 |
| 1.4 Equipment | 4.41 ± 0.25 | 0.13 | 0.0894 |
| 1.4.1 Ratio of monitors, mobile IV stands, walkers to beds | 4.63 ± 0.25 | 0.14 | 0.0157 |
| 2 Process indicators | 6.00 | 0.00 | 0.7332 |
| 2.1 Health education | 4.65 ± 0.40 | 0.09 | 0.0690 |
| 2.1.1 Implementation rate of perioperative education on significance and methods of early postoperative ambulation | 4.70 ± 0.40 | 0.09 | 0.0070 |
| 2.1.2 Mastery rate of postoperative oral nutritional solution preparation methods | 4.60 ± 0.50 | 0.11 | 0.0030 |
| 2.1.3 Mastery rate of preoperative lung function exercise methods (for patients with underlying pulmonary diseases) | 4.75 ± 0.35 | 0.07 | 0.0160 |
| 2.1.4 Implementation rate of discharge guidance | 4.70 ± 0.40 | 0.09 | 0.0150 |
| 2.2 Psychological care | 4.20 ± 0.60 | 0.14 | 0.0290 |
| 2.2.1 Screening rate for perioperative anxiety and depression | 4.65 ± 0.650 | 0.11 | 0.0090 |
| 2.2.2 Intervention rate for perioperative anxiety and depression | 4.60 ± 0.55 | 0.12 | 0.0060 |
| 2.3 Intraoperative temperature managemen | 4.75 ± 0.35 | 0.07 | 0.1003 |
| 2.3.1 Implementation rate of intraoperative temperature management measures | 4.85 ± 0.25 | 0.05 | 0.0402 |
| 2.3.2 Intraoperative normothermia achievement rate | 4.80 ± 0.30 | 0.06 | 0.0402 |
| 2.4 Cooperation in tumor-free protective isolation techniques | 6.00 | 0.00 | 0.3958 |
| 2.4.1 Implementation rate of supervision and cooperation in tumor-free protective isolation techniques | 6.00 | 0.00 | 0.3958 |
| 2.5 Venous thromboembolism (VTE) management | 4.65 ± 0.50 | 0.11 | 0.0440 |
| 2.5.1 VTE assessment rate | 4.70 ± 0.40 | 0.09 | 0.0130 |
| 2.5.2 Implementation rate of VTE preventive measures | 4.65 ± 0.45 | 0.10 | 0.0130 |
| 2.6 Pain management | 4.55 ± 0.60 | 0.13 | 0.0320 |
| 2.6.1 Postoperative pain assessment rate | 4.75 ± 0.35 | 0.07 | 0.0082 |
| 2.6.2 Mastery rate of patient- or family-controlled intravenous analgesia pump knowledge | 4.60 ± 0.40 | 0.09 | 0.0020 |
| 2.6.3 Implementation rate of multimodal analgesia | 4.70 ± 0.35 | 0.07 | 0.0082 |
| 2.7 Nutrition management | 4.85 ± 0.25 | 0.05 | 0.2060 |
| 2.7.1 Preoperative nutrition assessment rate | 4.80 ± 0.35 | 0.06 | 0.0252 |
| 2.7.2 Preoperative nutrition intervention rate | 4.87 ± 0.35 | 0.07 | 0.0252 |
| 2.7.3 Implementation rate of postoperative early ONS1 | 4.93 ± 0.26 | 0.05 | 0.0772 |
| 2.8 Tube management | 4.82 ± 0.35 | 0.07 | 0.1057 |
| 2.8.1 Venous catheter care compliance rate | 4.82 ± 0.35 | 0.07 | 0.0182 |
| 2.8.2 Nasoenteric tube care compliance rate | 4.75 ± 0.35 | 0.07 | 0.0200 |
| 2.8.3 Abdominal drainage tube care compliance rate | 4.75 ± 0.35 | 0.07 | 0.0200 |
| 2.8.4 Implementation rate of urinary catheter removal on postoperative day 1 (for clinically stable patients) | 4.55 ± 0.50 | 0.11 | 0.0070 |
| 2.9 Early ambulation | 4.65 ± 0.59 | 0.09 | 0.0692 |
| 2.9.1 Completion rate of bedside activities on the day of surgery | 4.75 ± 0.52 | 0.09 | 0.0216 |
| 2.9.2 Completion rate of ambulation on postoperative day 1 | 4.75 ± 0.35 | 0.09 | 0.0216 |
| 3 Outcome indicators | 4.73 ± 0.46 | 0.07 | 0.2395 |
| 3.1 Adverse events | 4.75 ± 0.35 | 0.09 | 0.2825 |
| 3.1.1 Incidence of stage 2 or above pressure injuries in hospitalized patients | 4.80 ± 0.41 | 0.09 | 0.0117 |
| 3.1.2 Incidence of central venous catheter (CVC)-related bloodstream infections | 4.87 ± 0.35 | 0.07 | 0.0187 |
| 3.1.3 Incidence of falls in hospitalized patients | 4.73 ± 0.59 | 0.13 | 0.0041 |
| 3.1.4 Proportion of fall-related injuries in hospitalized patients | 4.80 ± 0.56 | 0.12 | 0.0104 |
| 3.1.5 Incidence of deep vein thrombosis | 4.84 ± 0.35 | 0.07 | 0.0166 |
| 3.1.6 Unplanned extubation rate | 4.83 ± 0.56 | 0.12 | 0.0060 |
| 3.2 Complications | 4.87 ± 0.35 | 0.07 | 0.4732 |
| 3.2.1 Incidence of aspiration during anesthesia recovery | 4.84 ± 0.35 | 0.07 | 0.0852 |
| 3.2.2 Unplanned tube occlusion rate | 4.83 ± 0.56 | 0.12 | 0.0281 |
| 3.3 Bowel function recovery | 4.70 ± 0.45 | 0.10 | 0.1223 |
| 3.3.1 Bowel sound recovery rate within 12-24 hours postoperatively | 4.87 ± 0.25 | 0.05 | 0.0291 |
| 3.4 Length of stay | 4.70 ± 0.45 | 0.10 | 0.1223 |
| 3.4.1 Average length of stay for discharged patients | 4.87 ± 0.26 | 0.05 | 0.0291 |
Intergroup comparisons showed that the observation group had significantly better outcomes than the control group in terms of time to bowel sound recovery (12.53 ± 1.21 hours), first time out-of-bed activity (23.53 ± 2.34 hours), length of hospital stay (6.63 ± 0.46 days), and overall complication rate (3.03%), with a significantly higher satisfaction rate (100% vs 80.81%; P < 0.05), as shown in Table 4.
| Indicator | Observation group (n = 99) | Control group (n = 99) | t/χ² | P value |
| Time to bowel sound recovery (hours, mean ± SD) | 12.53 ± 1.21 | 17.16 ± 1.07 | 28.521 | 0.000 |
| First time out-of-bed activity (hours, mean ± SD) | 23.53 ± 2.34 | 29.06 ± 1.89 | 18.293 | 0.000 |
| Length of hospital stay (days, mean ± SD) | 6.63 ± 0.46 | 9.26 ± 0.37 | 44.327 | 0.000 |
| Patient satisfaction | 100.0 | 80.81 | 21.017 | 0.000 |
| Postoperative bleeding rate | 1.01 | 5.05 | 1.547 | 0.214 |
| Perforation incidence rate | 0.00 | 6.06 | 4.297 | 0.038 |
| Postoperative infection rate | 2.02 | 7.07 | 1.862 | 0.172 |
| Overall complication rate | 3.03 | 18.18 | 11.986 | 0.001 |
With the evolution of medical models and the development of patients’ health needs, alleviating symptom burden and suffering has become one of the research priorities for patients with EGC after treatment. Therefore, reasonable and effective nursing interventions are crucial for improving patient prognosis[10]. Conventional nursing interventions are often empirical and lack specificity. The promotion and application of the MDT enable healthcare professionals to integrate specialized expertise and develop personalized nursing plans for patients, breaking down disciplinary barriers and achieving efficient information integration and synchronization through a structured communication platform[11]. At the same time, the MDT is not a simple stacking of personnel, but rather a precise allocation of resources based on patient needs. In this study, a coordinating nurse acted as a “hub”, ensuring that various nursing interventions were carried out by the right professionals at the right time, thereby avoiding waste or overlap of nursing resources. This aligns with the recently emphasized concept of “precision nursing”. Gandhi et al[12] argue that the early involvement of dietitians during the preoperative phase, rather than intervening only after signs of malnutrition appear, is key to shortening the length of hospital stay. Furthermore, Wu et al[13], through MDT-based care, placed patients at the center and significantly enhanced their disease awareness and self-efficacy via systematic, multi-faceted health education. This demonstrates that when patients fully understand the purpose of various interventions, their compliance improves substantially, thereby actively and proactively engaging in the rehabilitation process.
This study employed the Delphi method to establish a perioperative nursing indicator system for patients with EGC based on the three-dimensional theoretical model of structure-process-outcome. In terms of expert selection, all consulted experts possessed 8 years to 25 years of nursing experience in gastrointestinal diseases, ensuring the professionalism and reliability of the evidence sources. Additionally, two rounds of questionnaire surveys were conducted during the research process, achieving a 100% response rate for both rounds. The authority coefficients of the experts were 0.758 and 0.828 for the two rounds, respectively, meeting methodological requirements. The indicator system constructed in this study aligns with the nursing implications of current treatment concepts, closely focuses on key perioperative nodes, and features easily quantifiable and collectible indicators with strong clinical practicality. Through dynamic monitoring of outcome indicators, closed-loop management of nursing quality can be achieved.
With the rise of precision medicine, it is particularly important to construct a targeted quality evaluation indicator system for nursing care of EGC as a single disease category[14]. Current research mainly focuses on the severe physiological and psychological impact of the disease burden of EGC on patients’ families, while attention to perioperative interventions addressing issues such as negative emotions and intraoperative hypothermia remains insufficient[15]. The process indicators of the MDT model constructed in this study, based on previous research and expert opinions, fully considered various stressors. Expert weight analysis revealed that psychological nursing and intraoperative temperature management received relatively high weights of 0.0290 and 0.1003, respectively, suggesting that the MDT approach can reduce patient stress and is highly significant for promoting postoperative recovery. EGC patients face the risk of various complications after surgical treatment. One study indicated[16] that the readmission rate due to complications after treatment for EGC patients is 7.2%. Considering China’s national context, where current team service motivation is low and the support system is underdeveloped, the outcome indicators of the MDT model constructed in this study focus on the postoperative characteristics of EGC patients. Combined with expert weighting, the results indicate that complications are a critical factor affecting patient recovery. This highlights the need, during the critical window for postoperative complications, to optimize the “green channel” process for patient readmission. This ensures patients can receive timely medical assistance to the greatest extent, prevents nursing risks, and enhances nursing quality and patient safety[17].
Jeong et al[18] have confirmed that postoperative nursing interventions can significantly reduce bed rest time, ac
In summary, the perioperative MDT model for EGC patients constructed using the Delphi method in this study demonstrates high reliability. It effectively improves treatment outcomes, promotes the recovery of postoperative physiological indicators, and prevents complications. With its strong practicality and positive prognostic impact, this model warrants clinical promotion and application.
| 1. | Conti CB, Agnesi S, Scaravaglio M, Masseria P, Dinelli ME, Oldani M, Uggeri F. Early Gastric Cancer: Update on Prevention, Diagnosis and Treatment. Int J Environ Res Public Health. 2023;20:2149. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 143] [Cited by in RCA: 115] [Article Influence: 38.3] [Reference Citation Analysis (0)] |
| 2. | Chiarello MM, Fico V, Pepe G, Tropeano G, Adams NJ, Altieri G, Brisinda G. Early gastric cancer: A challenge in Western countries. World J Gastroenterol. 2022;28:693-703. [PubMed] [DOI] [Full Text] |
| 3. | Kim GH. Endoscopic submucosal dissection for early gastric cancer: It is time to consider the quality of its outcomes. World J Gastroenterol. 2023;29:5800-5803. [PubMed] [DOI] [Full Text] |
| 4. | Hatta W, Tsuji Y, Yoshio T, Kakushima N, Hoteya S, Doyama H, Nagami Y, Hikichi T, Kobayashi M, Morita Y, Sumiyoshi T, Iguchi M, Tomida H, Inoue T, Koike T, Mikami T, Hasatani K, Nishikawa J, Matsumura T, Nebiki H, Nakamatsu D, Ohnita K, Suzuki H, Ueyama H, Hayashi Y, Sugimoto M, Yamaguchi S, Michida T, Yada T, Asahina Y, Narasaka T, Kuribasyashi S, Kiyotoki S, Mabe K, Nakamura T, Nakaya N, Fujishiro M, Masamune A. Prediction model of bleeding after endoscopic submucosal dissection for early gastric cancer: BEST-J score. Gut. 2021;70:476-484. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 134] [Cited by in RCA: 123] [Article Influence: 24.6] [Reference Citation Analysis (0)] |
| 5. | ASGE standards of practice committee; Forbes N, Elhanafi SE, Al-Haddad MA, Thosani NC, Draganov PV, Othman MO, Ceppa EP, Kaul V, Feely MM, Sahin I, Buxbaum JL, Calderwood AH, Chalhoub JM, Coelho-Prabhu N, Desai M, Fujii-Lau LL, Kohli DR, Kwon RS, Machicado JD, Marya NB, Pawa S, Ruan W, Sheth SG, Storm AC, Thiruvengadam NR, Qumseya BJ; (ASGE Standards of Practice Committee Chair). American Society for Gastrointestinal Endoscopy guideline on endoscopic submucosal dissection for the management of early esophageal and gastric cancers: summary and recommendations. Gastrointest Endosc. 2023;98:271-284. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 101] [Cited by in RCA: 89] [Article Influence: 29.7] [Reference Citation Analysis (2)] |
| 6. | Ma W, Zhang L, Wang C, Xu X. Effect of Multidisciplinary Team Collaborative Nursing Model Combined with Mind Mapping Teaching Method on Postoperative Complications and Mental Health of Patients with Advanced Pancreatic Cancer. Iran J Public Health. 2022;51:535-543. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 7] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 7. | Japanese Gastric Cancer Association. Japanese gastric cancer treatment guidelines 2018 (5th edition). Gastric Cancer. 2021;24:1-21. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1472] [Cited by in RCA: 1434] [Article Influence: 286.8] [Reference Citation Analysis (2)] |
| 8. | Al Ghamdi SS, Ngamruengphong S. Endoscopic Submucosal Dissection in the Stomach and Duodenum: Techniques, Indications, and Outcomes. Gastrointest Endosc Clin N Am. 2023;33:67-81. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 9. | Eriksen MB, Frandsen TF. The impact of patient, intervention, comparison, outcome (PICO) as a search strategy tool on literature search quality: a systematic review. J Med Libr Assoc. 2018;106:420-431. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 857] [Cited by in RCA: 654] [Article Influence: 81.8] [Reference Citation Analysis (0)] |
| 10. | Coffman TJ. Gastric cancer: Nursing care and impact. Nursing. 2025;55:16-22. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 11. | Jiang XH, Chen YH, Ye WF, Lin YJ, Chen XJ, Sun Q, Peng JS. Development and evaluation of an intelligent individualized nutrition management (iNutrition) applet for postdischarge gastric cancer patients following gastrectomy. Support Care Cancer. 2025;33:460. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 12. | Gandhi S, Amakiri IC, Pittman J, White A. Perioperative Nutritional Optimization in Spine Surgery. J Am Acad Orthop Surg. 2025;33:1015-1023. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 13. | Wu L, Cheng H, Wu L, Yao Y, Li D, Dai X, Yao D. The Impact of the ERAS-MDT-Based Nursing Interventions on Postoperative Recovery, Nutritional Status, and Complications in Patients Undergoing Total Laryngectomy for Laryngeal Cancer. Br J Hosp Med (Lond). 2025;86:1-16. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 14. | Wang Y, Zhang L, Yang Y, Lu S, Chen H. Progress of Gastric Cancer Surgery in the era of Precision Medicine. Int J Biol Sci. 2021;17:1041-1049. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 92] [Cited by in RCA: 77] [Article Influence: 15.4] [Reference Citation Analysis (1)] |
| 15. | Wei XN, Cai WY, Wu KL, Zeng FG. Application effect of gastrointestinal bundle nursing on the protection of gastrointestinal function in patients with gastric cancer. Medicine (Baltimore). 2023;102:e34308. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 4] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 16. | Chen WS, Huang ZX, Zhang HH, Chen XD, Cai YQ, Chen WJ, Zhu GB, Huang YS. Lactate Dehydrogenase and Risk of Readmission with Gastric Cancer: A Propensity Score Matching Analysis. J Invest Surg. 2023;36:2172488. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 17. | Ścisło L, Bodys-Cupak I, Walewska E, Kózka M. Nutritional Status Indicators as Predictors of Postoperative Complications in the Elderly with Gastrointestinal Cancer. Int J Environ Res Public Health. 2022;19:13453. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 9] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 18. | Jeong O, Jang A, Jung MR, Kang JH, Ryu SY. The benefits of enhanced recovery after surgery for gastric cancer: A large before-and-after propensity score matching study. Clin Nutr. 2021;40:2162-2168. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 22] [Article Influence: 4.4] [Reference Citation Analysis (1)] |
| 19. | Yuan W, Huang G, Dai P, Zhong Y, Ai Q, Liao Q. Application of enhanced recovery after surgery in perioperative patients undergoing laparoscopic surgery for gastric cancer: A meta-analysis. Medicine (Baltimore). 2023;102:e32962. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 20. | Fan Y, Li N, Zhang J, Fu Q, Qiu Y, Chen Y. The Effect of immunonutrition in patients undergoing pancreaticoduodenectomy: a systematic review and meta-analysis. BMC Cancer. 2023;23:351. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 12] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 21. | Yu R, Sun M, Xia S, Zhang L. Effects of ESPCS mode nursing on the surgical tolerance, gastrointestinal tract recovery and selfmanagement efficacy of patients with colon cancer. Oncol Lett. 2024;27:247. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 22. | Wang L, Wang H, Fang S, Yao M. Effectiveness of homogenized nursing care intervention in postoperative bladder irrigation of urological system in primary hospitals-Taking the incidence of postoperative complications as an example: A retrospective study. Medicine (Baltimore). 2024;103:e38270. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 23. | Zhang J, Zang X, Li C. Analysis of the effect of application and satisfaction of targeted nursing interventions in the care of gastric cancer patients undergoing chemotherapy. Minerva Gastroenterol (Torino). 2023;69:449-451. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 24. | Cui X, Shan T, Qiao L. Effect of Self-Transcendence Theory Combined with Comprehensive Nursing Intervention under Tumor Nutrition Education on Symptom Improvement, Nutritional Status, and Positive Psychology of Elderly Patients with Gastric Cancer. Contrast Media Mol Imaging. 2022;2022:6084732. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 7] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/