Copyright: ©Author(s) 2026.
World J Gastrointest Surg. Apr 27, 2026; 18(4): 115698
Published online Apr 27, 2026. doi: 10.4240/wjgs.v18.i4.115698
Published online Apr 27, 2026. doi: 10.4240/wjgs.v18.i4.115698
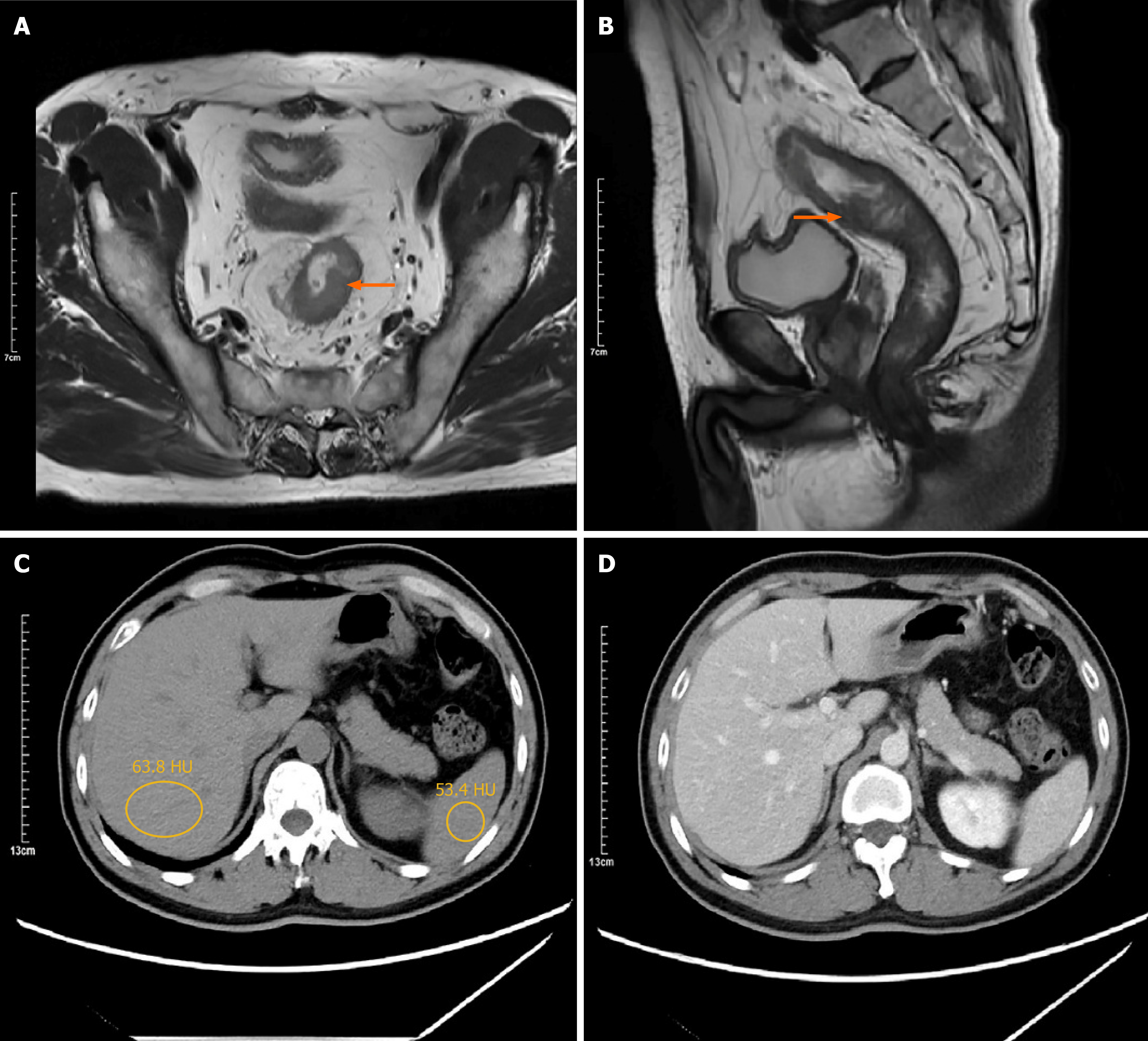
Figure 1 Preoperative abdominal computed tomography and magnetic resonance imaging.
A: The transverse image shows a rectal lesion (indicated by the orange arrow) in the middle segment of the rectum with no obvious lymph node metastasis; B: The sagittal image clearly demonstrates the lesion in the middle rectal segment (orange arrow) and further confirms the absence of significant lymph node metastasis; C: The plain abdominal computed tomography scan indicates no significant liver metastasis (the circle mean hepatic attenuation: 63.8 HU; splenic attenuation: 53.4 HU); D: The contrast-enhanced abdominal computed tomography scan further confirms the absence of significant metastatic lesions in the liver.
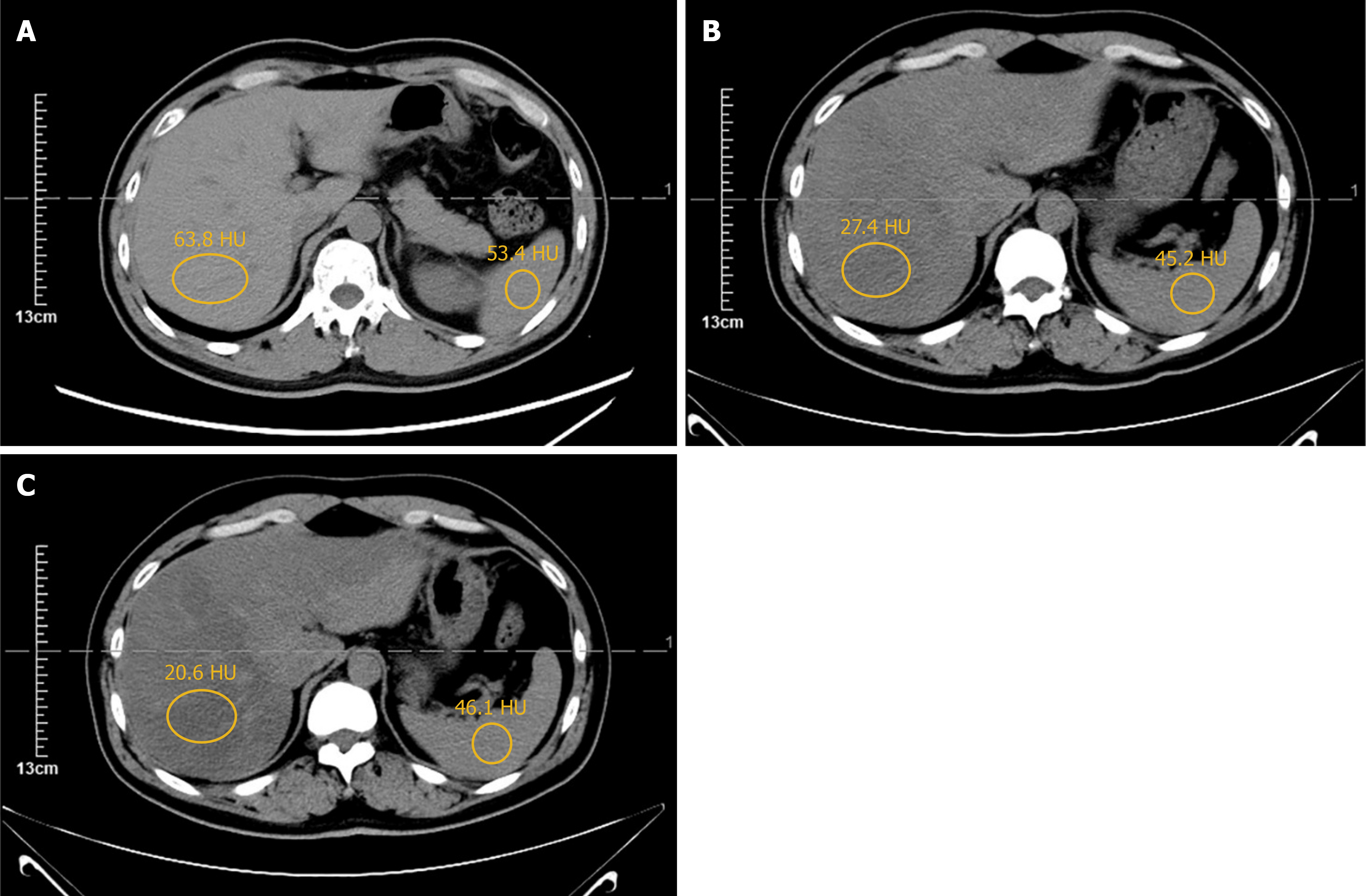
Figure 2 Abdominal computed tomography scans after the first procedure.
A-C: Scans obtained at 3, 6, and 9 months postoperatively, respectively (the circle: Hepatic/splenic attenuation in HU: A: 63.8/53.4; B: 27.4/45.2; C: 20.6/46.1).
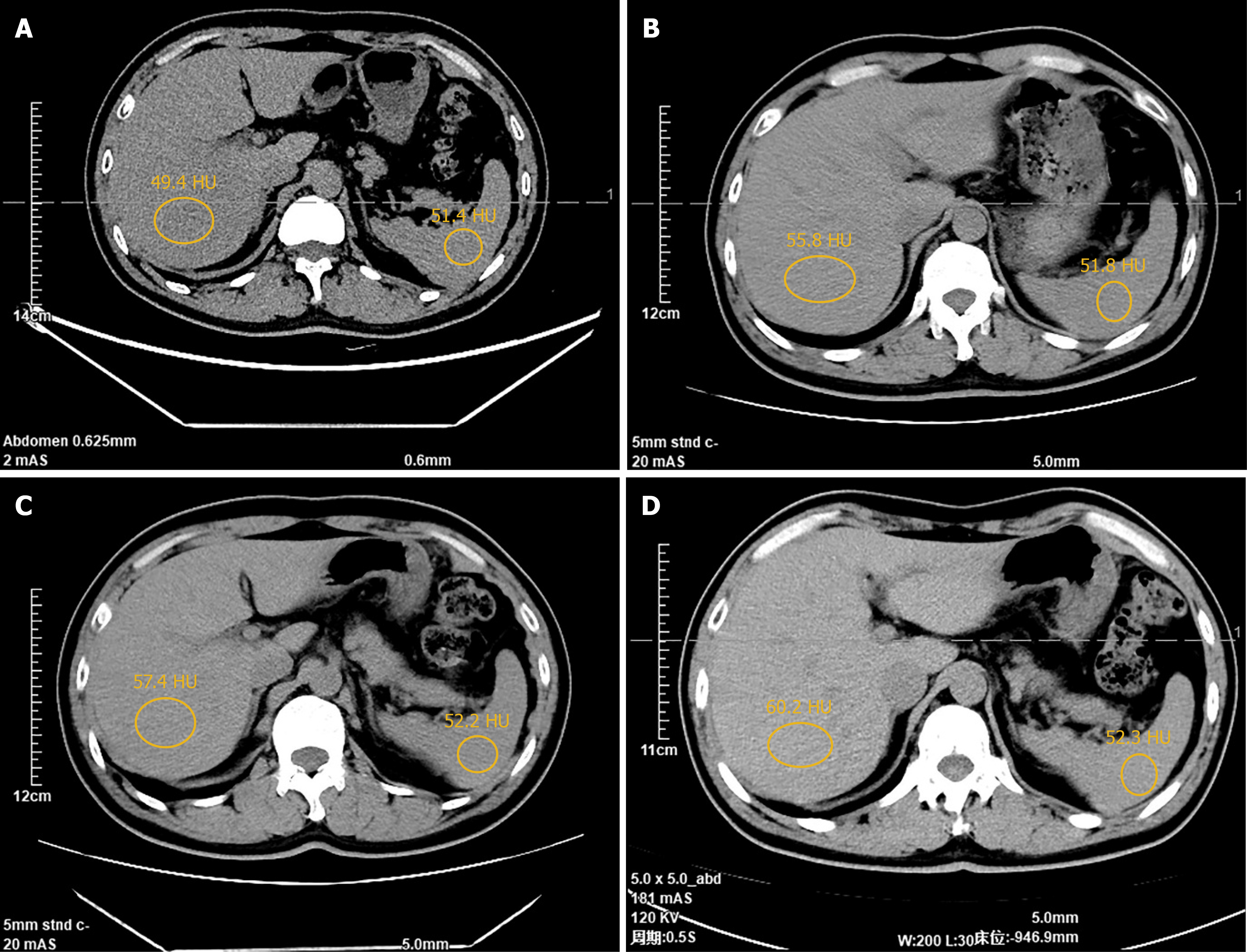
Figure 3 Postoperative abdominal computed tomography scans obtained at 3, 6, 9, and 18 months after the reversal operation.
A-D: Scans correspond to the 3-, 6-, 9-, and 18-month timepoints, respectively (the circle hepatic/splenic attenuation in HU: A: 49.4/51.4; B: 55.8/51.8; C: 57.4/52.2; D: 60.2/52.3).
- Citation: Liang YK, Zhang JH, Liang S, Wu SW, Feng XY. Loop ileostomy-induced reversible nonalcoholic fatty liver disease in a rectal cancer patient: A case report and review of literature. World J Gastrointest Surg 2026; 18(4): 115698
- URL: https://www.wjgnet.com/1948-9366/full/v18/i4/115698.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i4.115698