©Author(s) (or their employer(s)) 2026.
World J Gastrointest Surg. Feb 27, 2026; 18(2): 115427
Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.115427
Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.115427
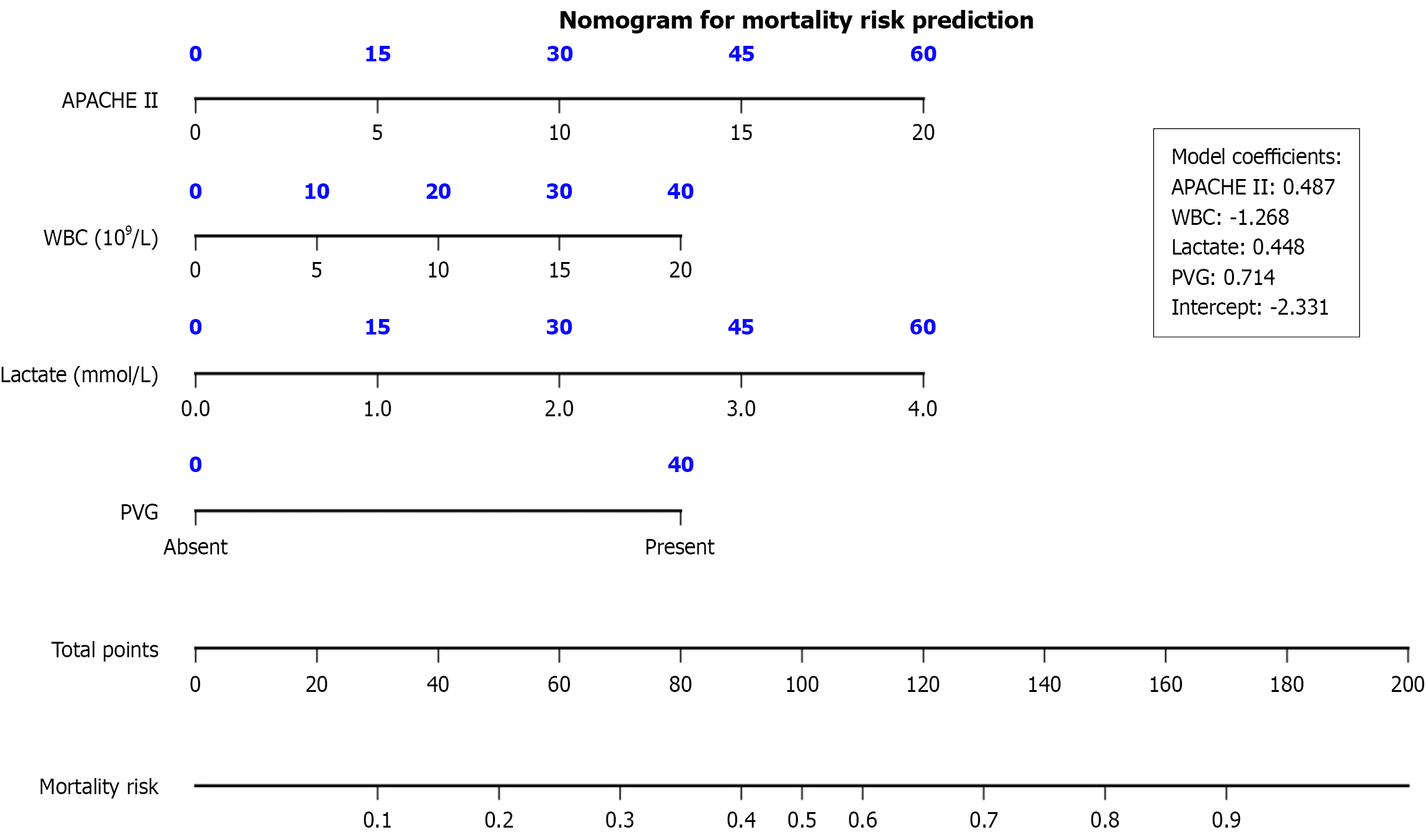
Figure 1 Nomogram.
A visual nomogram for predicting 30-day post-operative mortality in patients with colonic perforation. To determine the probability of death, the patient’s Acute Physiology and Chronic Health Evaluation II score, lactate level, white blood cell count, and presence (yes) or absence (no) of portal venous gas on their respective axes were located; a vertical line was drawn up to the points axis to score each variable. The points are summed, and the vertical line is dropped from the total points axis to the lower risk axis to determine the individual mortality probability. APACHE II: Acute Physiology and Chronic Health Evaluation II; WBC: White blood cell; PVG: Portal venous gas.
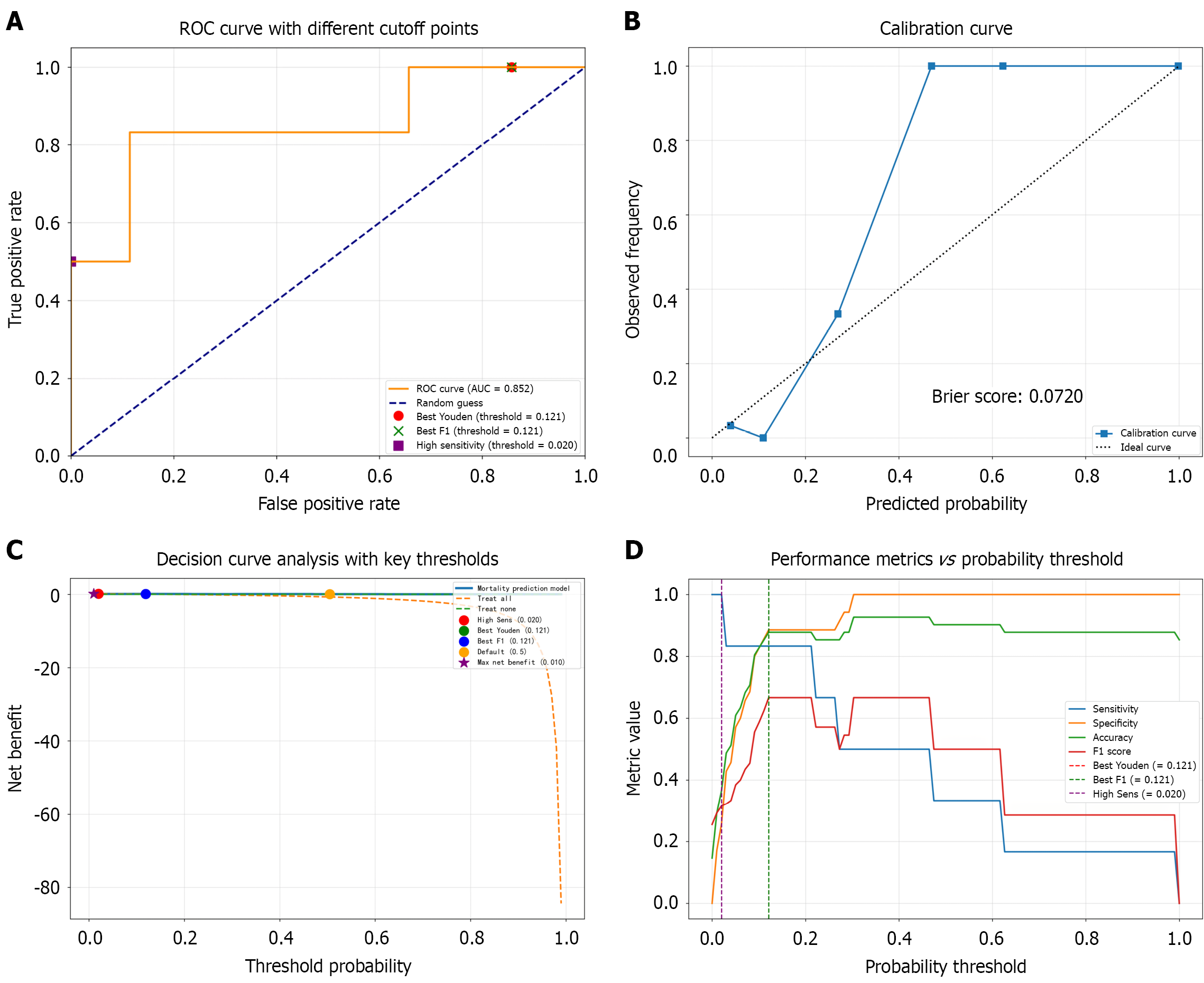
Figure 2 Model performance.
A: Receiver operating characteristic curve of the four-variable nomogram. The area under the curve (AUC) value was 0.852 (95% confidence interval: 0.791-0.913), indicating excellent discrimination for 30-day mortality; B: Calibration plot comparing predicted vs observed mortality probabilities. The dashed 45° line represents perfect calibration; the solid line represents the model-based fit. A Brier score = 0.072 and slope ≈ 1 indicate high agreement across the entire risk range, supporting direct clinical use without further probability recalibration; C: Decision curve analysis. Decision curve for the nomogram across clinically relevant threshold probabilities (1%-40%). The net benefit of the model exceeds that of the “treat-all” (orange dashed) and “treat-none” (green dashed) strategies over the entire range, confirming clinical utility; D: Threshold sensitivity plot. Sensitivity, specificity, accuracy and F1 score vs probability threshold. The vertical dotted lines mark the two selected cut-offs: 0.020 (high-sensitivity screen) and 0.121 (optimal Youden/F1 point), supporting the dual-threshold funnel strategy. ROC: Receiver operating characteristic.
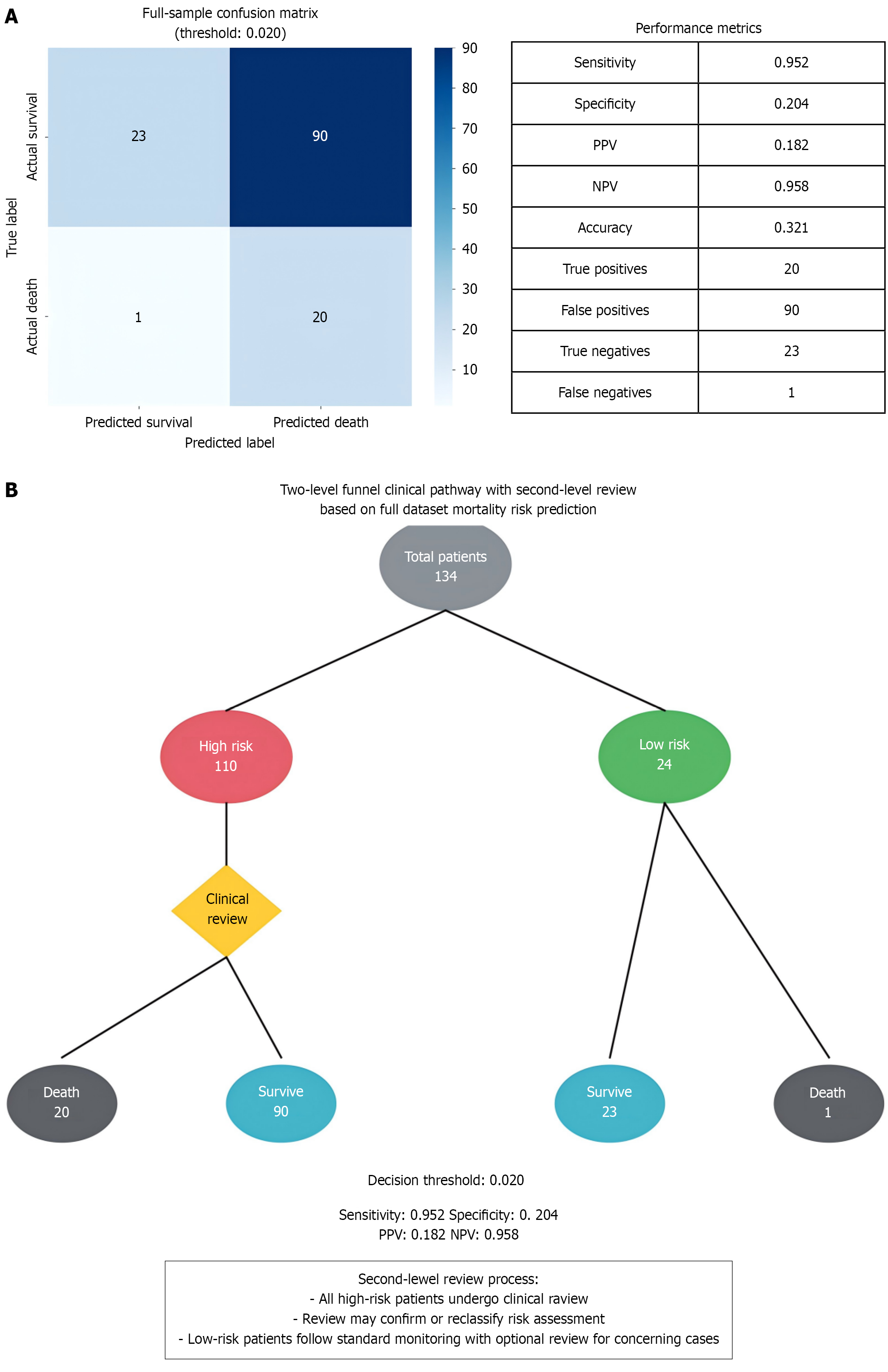
Figure 3 Dual-cut-off funnel validation.
A: Confusion matrix (high-sensitivity cut-off of 0.020). Confusion matrix for the entire cohort (n = 134) at the screening threshold of 0.020. The model correctly identified 20 of 21 deaths (sensitivity = 95.2%) with only one false-negative case, achieving a negative predictive value of 95.8% and supporting its use as a high-sensitivity screening criterion; B: Funnel pathway diagram. Flow chart of the dual-cut-off funnel strategy. Step 1 (≥ 0.020) flagged 92 high-risk patients (68.7%). Step 2 (≥ 0.121) confirmed 17 for intensive intervention while downgrading 75 to standard care, reducing advanced resource use by 53% in this cohort.
- Citation: Xu XJ, Zhang HD, Cheng CJ, Zhang YM, Zhang Q. Risk factor analysis and nomogram model construction for mortality in patients following colonic perforation surgery. World J Gastrointest Surg 2026; 18(2): 115427
- URL: https://www.wjgnet.com/1948-9366/full/v18/i2/115427.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i2.115427