Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.115417
Revised: November 18, 2025
Accepted: December 17, 2025
Published online: February 27, 2026
Processing time: 133 Days and 15.1 Hours
A significant post-pancreatic surgery effect we could mention is the postoperative pancreatic fistula (POPF). In this way, it contributes to a large degree to morbidity and long-term recovery. Only clinically significant fistulas (grades B/C) are asso
Core Tip: Postoperative pancreatic fistula (POPF) remains a major challenge in pancreatic surgery. Somatostatin and its analogs reduce exocrine secretion and have been widely evaluated for POPF prevention and management. Evidence from recent meta-analyses and randomized trials suggests that while these agents significantly lower POPF incidence, their effect on mortality is minimal. Current research focuses on patient risk stratification and long-acting depot formulations, such as preoperative lanreotide, to enhance compliance and cost-effectiveness. A tailored, risk-adjusted prophylaxis strategy may represent the future standard of care.
- Citation: Lazaridou L, Dimaki A, Vakalou K, Zervas V, Papadopoulos P, Koumarelas KE, Christodoulidis G. Somatostatin and its analogs in the management of postoperative pancreatic fistulas: A comprehensive review. World J Gastrointest Surg 2026; 18(2): 115417
- URL: https://www.wjgnet.com/1948-9366/full/v18/i2/115417.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i2.115417
The consequences of pancreatic surgery remain significant despite remarkable advances in surgical technique as well as in anesthesia and perioperative care. Of all the adverse outcomes, postoperative pancreatic fistula (POPF) is the most clinically significant. Incidence rates range from 20%-50%, while mortality rates reach 20% in some cases[1,2]. Addi
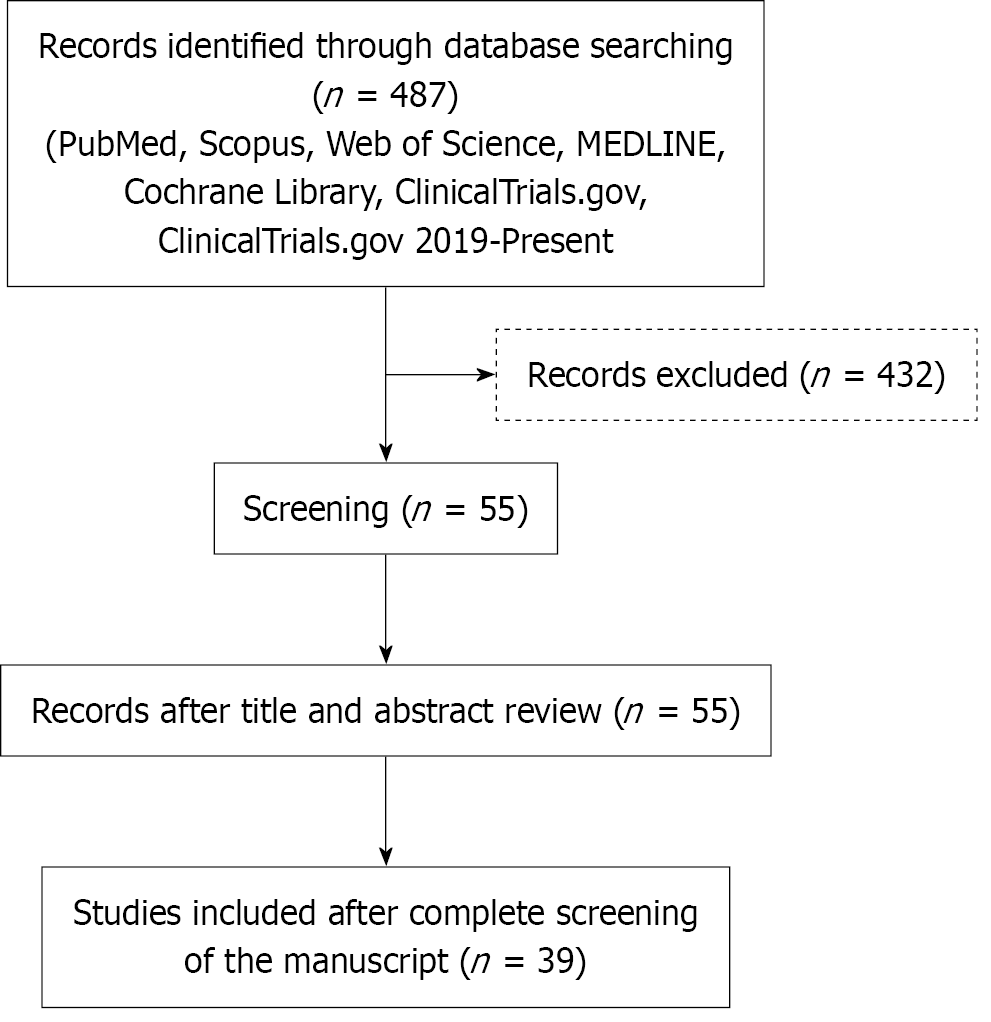
This study is designed as a narrative review that aims to synthesize and critically evaluate the existing literature on the role of somatostatin and its analogs in the prevention and management of POPF. The research question is structured according to the population/patient, intervention/exposure, comparator, and outcome framework. It focuses on patients undergoing pancreatic surgery who are at risk of developing a POPF. The intervention of interest is the perioperative administration of somatostatin or its analogs, such as octreotide or pasireotide, compared with standard postoperative management or placebo. The outcomes assessed include the incidence and severity of POPF, along with associated morbidity, mortality, and cost-effectiveness. PubMed, Cochrane Library, MEDLINE, Scopus Clinical Trial Register, and Web of Science databases were initially searched to retrieve studies reporting data on the prophylactic or therapeutic use of somatostatin and its analogs in the management of POPF from inception up to September 2025, according to PRISMA guidelines. The following medical subject heading terms alone or matched by the logical operators “OR” and “AND” were used: ‘Somatostatin’, ‘octreotide’, ‘lanreotide’, ‘pasireotide’, ‘postoperative pancreatic fistula’, ‘pancreatic surgery’, ‘pancreaticoduodenectomy’, ‘distal pancreatectomy’. The inclusion criteria encompassed studies evaluating the use of somatostatin or its analogs (including octreotide, lanreotide, pasireotide, or somatostatin-14) for the prevention or management of POPF following pancreatic surgery. Eligible study designs included randomized controlled trials (RCTs), prospective or retrospective cohort studies, meta-analyses, and systematic reviews that reported clinical outcomes related to the incidence, severity, or associated morbidity and mortality of POPF. Only studies conducted in adult human populations (≥ 18 years) and published in English were considered. Furthermore, eligible studies were required to employ established diagnostic criteria or classifications for POPF, such as the International Study Group on Pancreatic Fistula (ISGPF)/International Study Group on Pancreatic Surgery (ISGPS) definitions from 2005 or 2016, and to report on the perioperative or postoperative administration of somatostatin or its analogs in the context of pancreaticoduodenectomy, distal pancreatectomy, or other pancreatic resections. The exclusion criteria included animal or in vitro studies, as well as case reports, conference abstracts, letters, and editorials lacking sufficient clinical data or outcome analysis. Studies were excluded if they did not specifically address POPF for example, those examining somatostatin for alter
POPF remains one of the most serious and challenging complications following pancreatic surgery. However, despite substantial advances in operative technique, perioperative care and critical management POPF continues to be a major determinant of postoperative morbidity and mortality as well as a key factor influencing recovery, readmission rates and the administration of adjuvant therapy definition and diagnostic criteria[1-3,15,16]. The concept and diagnostic framework of POPF have evolved significantly over the past two decades largely through the efforts of the ISGPF and its successor the ISGPS. In 2005 the original definition of ISGPF defined POPF as any drain with an amylase content exceeding three times the upper limit of normal serum amylase activity on or after day three postoperatively[1,17]. In this early classification based on clinical severity and the degree of deviation from the normal postoperative course fistulas were classified into grades A, B and C. Recognizing the need for a more clinically relevant definition in 2016, the ISGPS revised the criteria[1,3,18].
According to the updated definition, a POPF is characterized by any measurable volume of drain fluid with an amylase concentration greater than three times the upper limit of the normal serum value, accompanied by a clinically relevant condition directly attributable to the fistula. This revision excluded asymptomatic biochemical abnormalities previously designated as grade A fistulas and reclassified them as biochemical leak entities without clinical consequence that no longer qualify as true fistulas[6]. In terms of diagnosing a CR-POPF, you need to see a significant spike in drain amylase levels, three times the normal upper limit of what you’d expect in the blood. Coming hotfooting from surgery, a CR-POPF will also require a change in the way the patient is being treated. This could be antibiotics, feeding tubes, prolonged drainage, keyhole or tube procedures, repeat surgery, or sorting out any infections or failing organs. Well-known for its clear-cut criteria, the ISGPS (2016) classification system gives us three categories: Biochemical leak, grade B pancreatic fistula and grade C pancreatic fistula. Biochemical leak used to be known as grade A, but now it’s basically a false alarm, where the drain amylase is high, but the patient doesn’t have any symptoms and doesn’t need any treatment, and the surgery goes according to plan[13,19].
Grade B is where the pancreatic fistula is serious enough to require a rethink in the recovery plan, and may involve feeding tubes, antibiotics, or imaging-guided injections through the skin or down the nose, although isn’t immediately fatal, it can delay the patient’s recovery and send them home from hospital later than they should be. Grade C is the worst case, and is associated with organ failure, second surgeries, and death, and patients who are in this category are often put in the intensive care unit. If a grade B fistula starts to cause systemic problems or organ failure, it gets reclassified as a grade C.
When discussing POPF following pancreatic surgery, it is still a major concern in the field of pancreatic surgery. Even though the mortality rate for pancreaticoduodenectomy has dropped to less than 3% at high-volume centers, the rate of CR-POPF remains a problem, making up a sizeable proportion of the complications in these patients[10]. The incidence of POPF is affected by the surgical procedure in question, gland characteristics, duct diameter and the experience of the institution.
Reported rates for relevant POPF after pancreaticoduodenectomy are 10%-28%, and 20%-30% for distal pancreatectomy. When we count all leaks, the overall rate of POPF can reach 27%-40%. Meta-analyses have shown that biochemical leaks happen in about 27% of cases but only 19% of them are clinically significant. In severe cases, the mortality rate due to grade C POPF could be as high as 25%[18,20].
The factors that contribute to the formation of POPF are also well-documented. These include a soft texture of the pancreas, a small pancreatic duct less than three millimeters in diameter, high body mass index, male sex, excessive blood loss during surgery, and smoking[10]. Interestingly, a firm fibrotic pancreas is less likely to be affected, and is often a consequence of chronic pancreatitis.
Predictive models for POPF, such as the updated alternative fistula risk score, have been developed to classify patients into low and high-risk categories for the development of CR-POPF, and aid in surgical planning and medical decision-making including drainage and the duration it is needed. When looking at the global picture, pancreatic fistulae, or POPF, happen to occur in anywhere from 10% to 30% of cases, this is largely due to the size of the surgical procedure, the skill level of the hospital, and sticking to standardized definitions. Well-known strategies for preventing POPF, such as the use of proven perioperative protocols and regular scoring systems, have been proven to cut down the number of cases, and a surgeon’s experience is the single best way to stop POPF from happening in the first place. The use of sharper anastomotic techniques, selective use of somatostatin medications, and tweaking the way drains are managed are all part of the battle against POPF, but no single strategy can completely eliminate the risk[3,21]. The way we’re con
A dreaded complication called postoperative pancreatic fistula, or POPF, can occur, when pancreatic surgery goes awry. Coming from a combination of mechanical and chemical problems that compromise the seal between the pancreas and its surrounding tissues, POPF has continued to be a challenge to treat and understand. The root of the problem lies in pancreatic juice leaking out of the pancreas, leading to self-digestion, inflammation and tissue death in the area around the pancreas[2,13].
A hairline fracture in a pancreatic duct or a failed suture is often the starting point for POPF that sends pancreatic juice containing digestive enzymes like trypsinogen, lipase, and elastase into the surrounding tissues[3,6]. When trypsinogen gets converted to trypsin outside the pancreas, it sets off a destructive chain reaction, similar to a severe pancreatitis, that causes local damage and sends inflammation spreading through the body[3,23]. The end result is peripancreatic fat necrosis, damage to the blood vessels, and a generalized inflammatory response.
Established research now shows that pancreatitis triggered by the stress of the surgery and the way the pancreas was manipulated during the operation are a major contributors to POPF[24], while also causing a sort of “knot” in the blood vessels and a decrease in blood flow to the area[25]. The shape and texture of the pancreas and the size of its main duct are also factors that can be measured, and those with a very soft pancreas, tiny main ducts, or poor tensile strength are at higher risk for mechanical failure, microleaks and fistulas. It’s a sign that the body is still leaking the enzyme through the pancreatic fistula, and damaging the surrounding tissue, when amylase levels are still elevated after surgery. How high the amylase levels go, directly corresponds to the severity of the fistula and the clinical picture[11,26]. Basically, it can tell the difference between a minor biochemical leak and a clinically significant POPF[11].
The histopathologic studies demonstrate that the release of inflammatory cytokines in response to enzyme leakage increases vascular permeability, amplifying peripancreatic edema and necrosis[23]. It is this inflammatory/ischemic interplay that explains the progressive nature of POPF from minor leaks to life-threatening complications such as post-pancreatectomy hemorrhage.
A dysregulation of the pancreatic exocrine control is involved in the molecular framework of POPF. Analogues of somatostatin inhibit cyclic adenosine monophosphate-mediated enzyme secretion by acting on somatostatin receptor (SSTR) 2 and SSTR5 receptors, thereby reducing pancreatic juice output and intraductal pressure[27]. The continuous intravenous somatostatin infusion produces uniform receptor activation and mimics physiologic inhibition. It limits premature enzyme activation and tissue injury[26]. Meierhofer et al[26] has refined this understanding in recent years. Histopathologic evidence reveals that digestive proteases directly degrade vascular elastin and collagen in the peripancreatic tissues while imaging-based analyses demonstrate that early postoperative pancreatitis correlates with perianastomotic ischemia zones. Local microthrombi and delayed perfusion on computed tomography have been linked to subsequent fistula development[28].
In the case of the gastrointestinal and endocrine systems, somatostatin is a hormone that has a far-reaching inhibitory control. It is produced in the delta cells of the pancreatic islets, the gastric and intestinal mucosa, and the hypothalamus, acting as a sort of ‘brake pedal’ on hormonal and exocrine secretions. It has 5 receptor types, SSTR1 through to SSTR5, that are spread out across different tissues and organs[13,19,29].
Physiologically, somatostatin clamps down on the release of insulin, glucagon, growth hormone, pancreatic enzymes and gut hormones. In the pancreas, the δ-cells sense glucose and send out somatostatin which then suppresses the α and β-cells close by, balancing insulin and glucagon levels[30,31]. Through its predominant action at SSTR2 and SSTR5, somatostatin reduces pancreatic exocrine secretion, gut motility and splanchnic blood flow, while enhancing water and mineral absorption, effects that are clinically relevant for pancreatic surgery. This helps explain why somatostatin is so good at preventing pancreatic fistulas after surgery[6].
When somatostatin is at the cellular level, it gets its job done by activating Gi-proteins, which in turn knocks out adenylate cyclase activity, lowers the levels of cyclic adenosine monophosphate inside the cell and severely reduces the release of secretory vesicles by a calcium-dependent process. Functionally, this results in less pancreatic juice and slower secretory activity[21].
Well-known for its anti-inflammatory and blood constricting properties, somatostatin reduces the amount of blood flow to the splanchnic region, and helps to keep the area around the pancreas nice and dry. Both of which are great for stabilizing the surgical site and protecting any anastomoses[17,30].
For the native somatostatin hormone, its inhibitory effects are impressive, but unfortunately, it’s gone from the body in just one to three minutes. This very short half-life means it does not last long enough in the circulation to be used as a practical long-term therapy, and that’s why scientists created synthetic versions, such as octreotide, lanreotide, pasireo
Octreotide is one of the first synthetic somatostatin analogues, an eight amino acid peptide that sticks to the SSTR2 and SSTR5 receptors, which are the main types found in the pancreas and gastrointestinal tract[29,32]. Its half-life is approximately two hours, allowing for irregular subcutaneous injections, and works fantastically well at reducing pancreatic enzyme production and circulation, which in turn reduces the volume and concentration of pancreatic secretions[33,34]. Classic pharmacokinetic studies by Battershill and Clissold[34] show that octreotide still packs a punch even after many years, with high receptor affinity, making it suitable for use in the perioperative period. In clinical practice, typical perioperative regimens use intermittent subcutaneous dosing, with adverse effects mainly including transient gastroin
Concerning somatostatin analogues, lanreotide and pasireotide have their own profiles in the market. Lanreotide’s receptor affinity is mostly for SSTR2 and SSTR5 and has a 23-day half-life, making its injections less frequent[38,39]. Its long half-life permits depot formulations with infrequent injections, which maintains suppression of pancreatic exocrine function and improves treatment adherence, with a generally favorable tolerability profile[15,33,39].
Pasireotide is basically the second generation of these sorts of drugs and has a much broader receptor affinity, hitting SSTR1, 2, 3 and 5 with lots of strength. Pharmacologically, it’s got a half-life of around 11 hours and completely knocks out pancreatic secretion. Allen et al[9] showed that pasireotide can cut down on POPF rates in patients, but the results of more recent trials have been mixed, and don’t always show that pharmacological superiority translates to real-world benefits. Clinically important adverse effects include a higher incidence of hyperglycaemia due to more pronounced suppression of insulin release[9,19,20,36,37].
Concerning somatostatin analogues, the natural peptide form of somatostatin-14 is significantly more potent than synthetic analogues. The continuous intravenous administration of somatostatin-14, has been shown to be very effective in blocking the release of pancreatic enzymes and has an almost equal or even better performance than octreotide in clinical trials[1,16,22,26]. Despite this, its need for continuous infusion limits convenience compared with longer-acting analogues.
Well-known to be different, however, is the expression of SSTR subtypes in various tissues of the human body so the clinical effect of each analogue varies according to the target tissue. It turns out that the main functional receptor in the pancreas is SSTR2, which helps explain why octreotide and lanreotide are so effective in suppressing pancreatic secretion (according to research in the year ‘12’ and ‘03’). Pasireotide has a broader range of receptor coverage, which leads to an additional reduction in hormonal and exocrine activity, but comes with the downside of much higher blood glucose levels, mainly because it squashes insulin release[13,31,32].
Collectively these agents share a class effect inhibiting exocrine secretions modulating hormone release and reducing splanchnic blood flow while differing in receptor selectivity, pharmacokinetics and metabolic side effects. Meta-analyses confirm that somatostatin and its analogues significantly reduce POPF overall and clinically relevant. However, no individual compound has demonstrated unequivocal superiority[33]. The somatostatin serves as a central regulator of pancreatic physiology and its analogues extend this role pharmacologically through receptor-specific sustained inhibition of exocrine and endocrine function. These combined effects underpin their clinical utility in the prevention and manage
| Agent | Mechanism | Evidence level | Effect on POPF | Limited factors |
| Somatostatin (IV infusion) | Pancreatic enzyme suppression (SSTR1-5) | High | Decrease POPF (strong, consistent) | Requires IV infusion |
| Pasireotide | Broad SSTR1-5 affinity | High (RCT + meta-analyses) | Decrease CR-POPF (56% RRR) | Cost, hyperglycemia |
| Octreotide | SSTR2, SSTR5 selective | Moderate | Decrease biochemical leaks; inconsistent CR-POPF | Dosing variability |
| Lanreotide | Long-acting SSTR2, SSTR5 | Moderate | Modest POPF reduction | Limited data |
| Combined protocols (SSA + drainage) | Synergistic mechanical and pharmacologic control | Moderate-high | Decrease POPF and severity | Implementation complexity |
POPF remains one of the most severe complications after pancreatic resection, causing increased morbidities, longer hospital stays and postponed adjuvant therapy. The pharmacological inhibition of the pancreatic exocrine secretion with somatostatin and its analogues is one of the most thoroughly studied prophylactic strategies. These peptides downregu
The SSTR2 and SSTR5 receptors on the pancreatic acinar and ductal cells are the main targets of somatostatin and its analogues (octreotide, lanreotide, pasireotide) to bind to. As a result, both volume and enzymatic concentration of the pancreatic secretions is reduced[19,34]. In order to maintain the inhibitory effect throughout the critical early postopera
The pivotal Allen et al[9] RCT showed that pasireotide (SOM230) 900 μg subcutaneously twice daily reduced the incidence of CR-POPF by 56% compared with placebo (9% vs 21%) in patients undergoing pancreaticoduodenectomy or distal pancreatectomy. This was the first large, double-blind, placebo-controlled study to show a significant pharmacologic preventive effect. Although somatostatin analogues consistently reduce biochemical pancreatic leakage, large randomized trials and meta-analyses demonstrate inconsistent benefits for clinically significant POPF[8,11,16,34].
The studies that followed the first one verified its results albeit with different degrees of impact. Li et al[12] indicated the same tendency of decreased POPF with the use of pasireotide but at the same time mentioned that the adherence was brought down by two factors, namely cost and risk of hyperglycemia. Meta-analyses and network analyses comprising Hou et al[36] proved that there were significant drops in overall as well as CR-POPF (odds ratio approximately 0.6), however, there was no gain in survival.
The quest for an effective POPF-preventive pharmacotherapy continues, with somatostatin and its analogues (octreo
Though octreotide among them still leads the way in terms of studies performed on it, the results have been mixed. Ontogeny of this drug has passed through various stages, i.e., trials, meta-analyses, biochemical assessment etc. resulting in inconsistent effects on CR-POPF[8,11]. The long-acting depots formulation of the substance lanreotide, on the other hand, gave small reductions in pancreatic enzyme leakage without the clinical superiority being established[7]. On the contrary, the continuous infusion of intravenous somatostatin has become more and more consistent in preventing the occurrence of POPF in many trials and meta-analyses probably owing to the constant receptor engagement and the intensive suppression of exocrine output[16,36].
A systemic review done in 2020 with the participation of 25 RCTs reached the conclusion that somatostatin analogues lead to the overall reduction of POPF by approximately 30% [relative risk (RR) approximately 0.7]. There are two drugs at the top of the list for the strongest potency - continuous somatostatin and pasireotide[16,36]. The two groups of resear
The prophylactic benefit of somatostatin analogues is most pronounced in high-risk patients, specifically those with a soft pancreas, a small pancreatic duct (< 3 mm), or elevated body mass index, in whom both biochemical and clinically relevant leaks are more effectively reduced[10,19]. The biochemical and clinically relevant leaks are reduced even more with very early administration (< 24 hours post-op) have reported octreotide to be effective in soft-pancreas pancreaticoduodenectomy cases as well[19]. On the other hand, some large-scale reviews state that there is no benefit in low-risk or fibrotic glands[3].
Latest findings differ from one another. Alzelfawi et al[37] included a total of 78 trials in their study and came to the conclusion that somatostatin analogues reduce POPF incidence significantly but have no effect on mortality. Cullinane et al[23] and Chauhan et al[13] were in favor of universal prophylaxis as the only solution to the problem, arguing that it would still be beneficial in the case of heterogeneous populations with different levels of CR-POPF reduction. On the other hand, Hou et al’s network meta-analysis[36] was to the contrary, as it declared that both somatostatin and octreotide have the same effect on POPF when the former is given continuously rather than by subcutaneous dosing.
In spite of the proof of biochemical efficacy, the high cost coupled with the metabolic side-effects (hyperglycemia) of pasireotide have ruled it out for general application[3]. On the other hand, octreotide and lanreotide are still present in the market but they come with smaller effect sizes. As a result, most current reviews and expert recommendations are in favor of a selective, risk-adjusted prophylaxis strategy somatostatin analogs kept for high-risk patients only[3,6]. A multimodal prevention scheme which pharmacological suppression is combined with early drain removal and careful surgical technique yields the best results available today[26].
The new evidence taken together proves that somatostatin and its equivalents decrease significantly the occurrence of POPF but their efficacy on the clinically significant fistulas is inconsistent. Pasireotide and continuous infusion of somatostatin are very effective whereas octreotide and lanreotide are not quite effective. A blanket prophylaxis for all patients is not advisable. Instead, risk patient selective pharmacologic prophylaxis provides the optimum balance of benefit, safety, and cost[1,6,12,34].
When it comes to the prevention of POPF, somatostatin and its analogues, or somatostatin analogs, have been given a lot of attention in pancreatic surgery, and the reason for this is sound. They slow down the excretion of pancreatic fluids by activating the SSTR2 and SSTR5 receptors, which reduces the pressure within the pancreatic duct and therefore cuts down on leakage from the stump[35]. However, the clinical benefits of using somatostatin analogs in the prevention of POPF, has been spotty.
One of the things that’s making it difficult to understand the results of studies on this topic, is the extreme difference in the way that these studies are set up (Table 2). Changes in the way that pancreatic fistulas were classified, especially in the 2016 revision of the International Study Group of Pancreatic Surgery guidelines, have caused lots of confusion[38]. Other things like the way that surgeons cut open the pancreas, put in drains, and take them out also play a huge role, and can cancel out any potential effects from the medication. These sources of heterogeneity significantly weaken the certainty of the pooled evidence and complicate any direct comparison across trials.
| Ref. | Study group | Intervention | Outcome |
| Pillarisetty et al[15] | 98 patients undergoing either PD or DP | A single dose of preoperative lanreotide (120 mg) | CR-POPF or intraabdominal abscess was observed in 8 (8%) patients in the total cohort: 7 (11.2%) in the PD group and 1 (2.7%) in the DP group. Biochemical leak was detected in 12 (12.2%) patients |
| Vuorela et al[11] | A total of 258 patients who underwent DP between 2000 and 2016 at Helsinki University Hospital | 900-μg pasireotide administered subcutaneously twice daily for a maximum of 7 days or octreotide administrated through a 200-μg infusion twice daily for 3 days | 40 CR-POPF grade B and C (16%; P = 0.739). CR-POPF in the pasireotide group was 7 (15%), 3 (10%) in the octreotide group and 28 (17%) in the control group (P = 0.630) |
| Yoon et al[8] | Patients who underwent PD at Samsung Medical Center from June 2019 to July 2020 (totally 263 patients, 81 patients in the low-risk group and 182 patients in the high-risk group). CR-POPF was calculated using the nomogram-based web calculator (http://popf.smchbp.org) | Postoperative octreotide for more than three days | No statistically significant differences of CR-POPF between octreotide group and the control group in all patients (15.0% vs 14.7%, P = 0.963) and in the high-risk group (16.1% vs 23.6%, P = 0.206) |
| Herzberg et al[3] | Patients undergoing pancreatic surgery (PD and rescue pancreatectomy) for pancreatic cancer at Reinbek Hospital St. Adolf-Stift, Germany, from January 2013 till December 2022 | Fail-safe protocol included 0.2 mg of octreotide intravenously before the start of the pancreatic resection, in order to block the exocrine pancreatic secretion. Continued by 0.1 mg octreotide every 8 hours subcutaneously for the first 5 postoperative days | Fail-safe protocol in oncologic pancreatic head surgery can lower the rates of overall POPF grade B/C rate of 4.2% vs 18.8% (P = 0.012) before implementation of the fail-safe protocol |
| Potter et al[10] | A total of 100 patients undergoing elective PD or DP between January 2013 and April 2020 who received perioperative pasireotide therapy | Full course of pasireotide: Either a preoperative dose plus 7 days of postoperative therapy, or pasireotide continued until day of surgical drain removal in the setting of low drain amylase or partial course: A single preoperative dose and early discontinuation due to side effects | Relative to patients receiving full-course pasireotide, a single preprocedure dose was not associated with higher odds of any POPF (OR = 0.90, 95%CI: 0.31-2.61, P = 0.85) |
| Bootsma et al[7] | 1992 patients who underwent elective, open pancreatoduodenectomy between 2014 and 2017 at all 16 Dutch centers for pancreatic surgery | 6 protocols based on the hospital the operation took place: (1) No SA administered; (2) Octreotide 100 mg subcutaneous injection three times a day for seven days, starting the day before surgery; (3) Lanreotide 120 mg subcutaneous injection at home a few days before surgery; (4) Pasireotideo 900 μg of subcutaneous pasireotide twice daily beginning preoperatively and continuing for 7 days (14 doses). Administered in patients deemed as high-risk; (5) Octreotide HR 100 mg subcutaneous injection three times a day for five-seven days, starting the day before surgery or on the first postoperative day; and (6) Lanreotide HR 120 mg subcutaneous injection at home a few days before surgery or on the first postoperative day | POPF occurred less often in patients treated according to lanreotide protocol (n = 75, 10.0%) and octreotide-HR (n = 15, 9.4%) and no SA protocol (n = 30, 12.7%), compared to a higher incidence in hospitals with lanreotide-HR (n = 52, 15.1%), octreotide (n = 54, 17.8%) and pasireotide protocol (n = 35, 19.1%). The rate of grade C POPF did not differ significantly (P = 0.358) between hospitals with octreotide-HR protocol (n = 4, 2.5%), lanreotide-HR protocol (n = 23, 2.9%), no protocol (n = 7, 3.0%), lanreotide (n = 23, 3.1%), octreotide (n = 12, 4.0%), and pasireotide protocol (n = 12, 6.0%) |
| Gaujoux et al[1] | Adult patients (≥ 18 years) who were scheduled to undergo either PD or DP with or without splenectomy | Continuous intravenous somatostatin 6 mg per day for 6 days and 3 mg on POD 7 or subcutaneous octreotide 100 μg subcutaneously 3 times per day until POD 6 and then 100 μg 2 times on POD 7. Treatment initiation starting intraoperatively just after surgical exploration | No statistically significant difference in the incidence of grade B or C POPF between patients treated with somatostatin (24.1%) and patients treated with octreotide (22.9%) (P = 0.73). Comparing all grades of POPF in the ISGPS classification (A/B/C) there was no difference between the two groups (51.9% in the somatostatin arm vs 48.3% in the octreotide arm, P = 0.37) |
Coming out of the United Kingdom, the study by Allen et al[9] showed a massive 56% reduction in CR-POPFs when using pasireotide, giving people hope that these medications might be more effective than they were initially thought. However, more recent, larger studies and meta-analyses have provided much more muted results, in a 7000-patient synthesis, Cullinane et al[23] showed no significant decrease in CR-POPFs with somatostatin analog therapy, which is quite the opposite of what was initially hoped for. The same thing happened with octreotide and lanreotide, which were shown to be completely without significant effect[8,11,13]. The contrast between early single-center success and later multicenter or pooled analyses highlights the fragility of the evidence base and raises concerns about publication bias and center-specific practice effects.
Through advanced network analysis, the comparative efficacy of different analogues has been recently clarified. Hou et al[36] a Bayesian-based meta-analysis of 24 randomized trials (n = 4054) showed that pasireotide achieved the lowest RR for overall POPF (RR = 0.46), while somatostatin and octreotide achieved more moderate reductions (RR = 0.60). However, the protective effect appeared greater in pancreaticoduodenectomy than in distal pancreatectomy suggesting procedure-specific physiology influences pharmacological response. The meta-analyses of Li et al[12] and Bootsma et al[7] have both demonstrated reductions in biochemical leaks but less consistent effects on grade B/C fistulas.
Recent investigations have shifted attention to the mode of administration and the real-world feasibility of the project. Continuous somatostatin maintains stable receptor occupancy and is physiologically advantageous but logistically demanding and expensive[7]. The subcutaneous octreotide is simpler to use but produces fluctuating plasma levels that may weaken sustained suppression. PrefIPS multicenter RCT compared these two regimens and found no significant difference in grade B/C POPF (24.1% vs 22.9%)[1]. Current trials are now investigating depot formulations that could bridge this gap. The SWOG S2408 phase III study (fluorescence activated cell sorting bulletin 2025) evaluates a single preoperative dose of lanreotide 120 mg in distal pancreatectomy stratified by drain use an approach that prioritizes compliance[39].
Economic and metabolic implications shape clinical decision-making increasingly. However, pasireotide is associated with significant hyperglycemia and high cost despite its broad receptor affinity (SSTR15) and potent suppression of exocrine output. Health-economic modeling suggests its routine use is cost-effective only in the highest-risk subset of patients with soft gland texture, small duct diameter (3 mm) or high body-mass index[19]. Octreotide and lanreotide offer lower efficacy but greater affordability and tolerability supporting a selective risk-adjusted prophylaxis approach rather than universal administration[7]. The limited cost-effectiveness across unselected populations further restricts the generalizability of existing findings.
Contemporary perioperative prevention strategies emphasize increasingly synergy between pharmacologic suppre
However, despite extensive research there are still several gaps. Many trials for clinically relevant endpoints are under
To sum up, somatostatin and its analogues occupy a refined but limited role in modern POPF prevention. Somatostatin infusion and pasireotide remain the most potent pharmacologic options yet their routine use is constrained by cost and metabolic lanreotide and subcutaneous octreotide offer more practical but modest advantages. The results of the SWOG S2408 trial and future meta-analyses will help define whether somatostatin analogs can achieve clinically meaningful and cost-effective risk reduction in the evolving consensus the shift from universal pharmacologic intervention to precision-guided integration of somatostatin analogs within broader perioperative strategies favors selective, patient-specific and multimodal prophylaxis. However, until stronger evidence emerges, somatostatin analog use should be individualized rather than standardized, given the modest overall benefit and the variability in outcomes across centers.
Such an approach aligns the pharmacologic rationale with the individualized surgical risk, offering the most sustainable path toward reducing POPF-associated morbidity in contemporary pancreatic surgery. But cost is a big issue, especially with pasireotide. It’s expensive and can put a serious strain on hospital budgets[23]. Recent studies show that POPF leads to longer hospital stays and higher resource use[3,7,10,18]. So, using somatostatin analogs as a preventive measure only makes sense for patients who already face a really high-risk[4,23]. Standardized care pathways have already cut down on complications and costs on their own[3,28]. In hospitals where these pathways work well, adding somatostatin analogs doesn’t seem to help much[23]. Then, Cullinane et al[23] found that somatostatin analogs don’t make a real difference in stopping clinically important POPF. If the drug doesn’t help, you just can’t justify spending so much on it. Bootsma et al[7] also looked at real-world data and found that complication rates vary widely from one hospital to another. That means the actual value of somatostatin analogs depends a lot on where you are. Most experts now agree: Don’t give somatostatin analogs to everyone[4,22,26]. It makes more sense to use them only for people who really need it, based on their risk. This targeted approach saves money and resources. Looking ahead, future trials need to track not just clinical results but also costs and patient-centered outcomes[22,26]. That’s the only way to know if somatostatin analog prophy
Despite three decades of research, the role of somatostatin analogues continues to evolve in POPF prophylaxis. Collectively, available evidence suggests that pasireotide and continuous IV somatostatin can reduce POPF rates when used in carefully selected patients and combined with multimodal preventive strategies. In high-risk scenarios their benefit appears greatest, while universal prophylaxis remains disputed. POPF prevention lies in personalized risk stratification optimized pharmacologic suppression and evidence-based surgical treatment.
| 1. | Gaujoux S, Regimbeau JM, Piessen G, Truant S, Foissac F, Barbier L, Buc E, Adham M, Fuks D, Deguelte S, Muscari F, Sulpice L, Vaillant JC, Schwarz L, Sa Cunha A, Muzzolini M, Dousset B, Sauvanet A; Collaborators. Somatostatin Versus Octreotide for Prevention of Postoperative Pancreatic Fistula: The PREFIPS Randomized Clinical Trial: A FRENCH 007-ACHBT Study. Ann Surg. 2024;280:179-187. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 10] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 2. | Schorn S, Vogel T, Demir IE, Demir E, Safak O, Friess H, Ceyhan GO. Do somatostatin-analogues have the same impact on postoperative morbidity and pancreatic fistula in patients after pancreaticoduodenectomy and distal pancreatectomy? - A systematic review with meta-analysis of randomized-controlled trials. Pancreatology. 2020;20:1770-1778. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 26] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 3. | Herzberg J, Strate T, Acs M, Piso P, Guraya SY, Honarpisheh H. Reduction of Postoperative Complications in Pancreatic Surgery by Standardizing Perioperative Management: An Observational Cohort Study. Visc Med. 2024;40:184-193. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 4. | Hallet J, Theodosopoulos E, Abou-Khalil J, Bertens K, Pelletier JS, Segedi M, Ouellet JF, Barkun J, Coburn N; Canadian Hepato-Pancreato-Biliary Association working group. Prevention of postoperative pancreatic fistula after pancreatectomy: results of a Canadian RAND/UCLA appropriateness expert panel. Can J Surg. 2022;65:E135-E142. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 5. | Mungroop TH, van der Heijde N, Busch OR, de Hingh IH, Scheepers JJ, Dijkgraaf MG, Groot Koerkamp B, Besselink MG, van Eijck CH. Randomized clinical trial and meta-analysis of the impact of a fibrin sealant patch on pancreatic fistula after distal pancreatectomy: CPR trial. BJS Open. 2021;5:zrab001. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 28] [Cited by in RCA: 25] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 6. | Hain E, Challine A, Tzedakis S, Mare A, Martinino A, Fuks D, Adham M, Piessen G, Regimbeau JM, Buc E, Barbier L, Vaillant JC, Jeune F, Sulpice L, Muscari F, Schwarz L, Deguelte S, Sa Cunha A, Truant S, Dousset B, Sauvanet A, Gaujoux S. Study Protocol of the PreFiPS Study: Prevention of Postoperative Pancreatic Fistula by Somatostatin Compared With Octreotide, a Prospective Randomized Controlled Trial. Front Med (Lausanne). 2020;7:488. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 7. | Bootsma BT, Plat VD, van de Brug T, Huisman DE, Botti M, van den Boezem PB, Bonsing BA, Bosscha K, Dejong CHC, Groot-Koerkamp B, Hagendoorn J, van der Harst E, de Hingh IH, de Meijer VE, Luyer MD, Nieuwenhuijs VB, Pranger BK, van Santvoort HC, Wijsman JH, Zonderhuis BM, Kazemier G, Besselink MG, Daams F; Dutch Pancreatic Cancer Group. Somatostatin analogues for the prevention of pancreatic fistula after open pancreatoduodenectomy: A nationwide analysis. Pancreatology. 2022;22:421-426. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 26] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 8. | Yoon SJ, Lee O, Jung JH, Shin SH, Heo JS, Han IW. Prophylactic octreotide for postoperative pancreatic fistula in patients with pancreatoduodenectomy: Risk-stratified analysis. Medicine (Baltimore). 2022;101:e29303. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 8] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 9. | Allen PJ, Gönen M, Brennan MF, Bucknor AA, Robinson LM, Pappas MM, Carlucci KE, D'Angelica MI, DeMatteo RP, Kingham TP, Fong Y, Jarnagin WR. Pasireotide for postoperative pancreatic fistula. N Engl J Med. 2014;370:2014-2022. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 379] [Cited by in RCA: 298] [Article Influence: 24.8] [Reference Citation Analysis (0)] |
| 10. | Potter KC, Sutton TL, O'Grady J, Gilbert EW, Pommier R, Mayo SC, Sheppard BC. Risk factors for postoperative pancreatic fistula in the Era of pasireotide. Am J Surg. 2022;224:733-736. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 11. | Vuorela T, Mustonen H, Kokkola A, Haglund C, Seppanen H. Impact of pasireotide on postoperative pancreatic fistulas following distal resections. Langenbecks Arch Surg. 2021;406:735-742. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 12. | Li T, D'Cruz RT, Lim SY, Shelat VG. Somatostatin analogues and the risk of post-operative pancreatic fistulas after pancreatic resection - A systematic review & meta-analysis. Pancreatology. 2020;20:158-168. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 24] [Article Influence: 4.0] [Reference Citation Analysis (2)] |
| 13. | Chauhan SSB, Vierra B, Park JO, Pillarisetty VG, Davidson GH, Sham JG. Prophylactic somatostatin analogs for postoperative pancreatic fistulas: a cross-sectional survey of AHPBA surgeons. HPB (Oxford). 2024;26:1229-1236. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 14. | Gans SL, van Westreenen HL, Kiewiet JJ, Rauws EA, Gouma DJ, Boermeester MA. Systematic review and meta-analysis of somatostatin analogues for the treatment of pancreatic fistula. Br J Surg. 2012;99:754-760. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 94] [Cited by in RCA: 70] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 15. | Pillarisetty VG, Abbasi A, Park JO, Sham JG. A phase II trial of lanreotide for the prevention of postoperative pancreatic fistula. HPB (Oxford). 2022;24:2029-2034. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 12] [Reference Citation Analysis (0)] |
| 16. | Cao Z, Qiu J, Guo J, Xiong G, Jiang K, Zheng S, Kuang T, Wang Y, Zhang T, Sun B, Qin R, Chen R, Miao Y, Lou W, Zhao Y. A randomised, multicentre trial of somatostatin to prevent clinically relevant postoperative pancreatic fistula in intermediate-risk patients after pancreaticoduodenectomy. J Gastroenterol. 2021;56:938-948. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 10] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 17. | Garnier J, Ewald J, Marchese U, Palen A, Mokart D, Piana G, Delpero JR, Turrini O. Double purse-string telescoped pancreaticogastrostomy is not superior in preventing pancreatic fistula development in high-risk anastomosis: a 6-year single-center case-control study. Langenbecks Arch Surg. 2022;407:1073-1081. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 18. | Kamarajah SK, Bundred JR, Lin A, Halle-Smith J, Pande R, Sutcliffe R, Harrison EM, Roberts KJ; PARANOIA Study Group. Systematic review and meta-analysis of factors associated with post-operative pancreatic fistula following pancreatoduodenectomy. ANZ J Surg. 2021;91:810-821. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 48] [Article Influence: 9.6] [Reference Citation Analysis (0)] |
| 19. | Rompen IF, Merz DC, Alhalabi KT, Klotz R, Kalkum E, Pausch TM, Strothmann H, Probst P. Perioperative Drug Treatment in Pancreatic Surgery-A Systematic Review and Meta-Analysis. J Clin Med. 2023;12:1750. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 11] [Reference Citation Analysis (0)] |
| 20. | Dalton EC, Johns MS, Rhodes L, Merritt WT 3rd, Petrelli NJ, Tiesi GJ. Meta-Analysis on the Effect of Pasireotide for Prevention of Postoperative Pancreatic Fistula. Am Surg. 2020;86:1728-1735. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 10] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 21. | Furbetta N, Gianardi D, Guadagni S, Di Franco G, Palmeri M, Bianchini M, Pisani K, Di Candio G, Morelli L. Somatostatin administration following pancreatoduodenectomy: a case-matched comparison according to surgical technique, body mass index, American Society of Anesthesiologists' score and Fistula Risk Score. Surg Today. 2021;51:1044-1053. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 22. | Rykina-Tameeva N, Samra JS, Sahni S, Mittal A. Non-Surgical Interventions for the Prevention of Clinically Relevant Postoperative Pancreatic Fistula-A Narrative Review. Cancers (Basel). 2023;15:5865. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 6] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 23. | Cullinane C, Devine M, Alazzawi M, Suilleabhain CO, Sullivan AO. "Somatostatin analogues do not reduce the risk of clinically relevant post-operative fistula rates in patients undergoing pancreatic surgery", a systematic review and meta-analysis. HPB (Oxford). 2025;27:746-757. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 24. | Chui JN, Sahni S, Samra JS, Mittal A. Postoperative pancreatitis and pancreatic fistulae: a review of current evidence. HPB (Oxford). 2023;25:1011-1021. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 18] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 25. | Seki Y, Ishizawa T, Mitsuhashi K, Inagaki NF, Mori K, Watanabe G, Komatsu T, Urano Y, Abe H, Ushiku T, Ito T, Hasegawa K. Mechanisms of histopathologic vascular damage caused by pancreatic juice leakage: Implications for preventing hemorrhagic complications. Surgery. 2025;186:109591. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 26. | Meierhofer C, Fuegger R, Biebl M, Schoefl R. Pancreatic Fistulas: Current Evidence and Strategy-A Narrative Review. J Clin Med. 2023;12:5046. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 27. | Pagnanelli M, De Gaetano F, Nappo G, Capretti G, Costantino ML, Zerbi A. The Choice of the Most Appropriate Suture Threads for Pancreatic Anastomoses on the Basis of Their Mechanical Characteristics. Biomedicines. 2023;11:1055. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 28. | Nebbia M, Capretti G, Nappo G, Zerbi A. Updates in the management of postoperative pancreatic fistula. Int J Surg. 2024;110:6135-6144. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 9] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 29. | Ludvigsen E, Olsson R, Stridsberg M, Janson ET, Sandler S. Expression and distribution of somatostatin receptor subtypes in the pancreatic islets of mice and rats. J Histochem Cytochem. 2004;52:391-400. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 59] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 30. | Denwood G, Tarasov A, Salehi A, Vergari E, Ramracheya R, Takahashi H, Nikolaev VO, Seino S, Gribble F, Reimann F, Rorsman P, Zhang Q. Glucose stimulates somatostatin secretion in pancreatic δ-cells by cAMP-dependent intracellular Ca(2+) release. J Gen Physiol. 2019;151:1094-1115. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 30] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 31. | Montorsi RM, Zonderhuis BM, Daams F, Busch OR, Kazemier G, Marchegiani G, Malleo G, Salvia R, Besselink MG. Treatment strategies to prevent or mitigate the outcome of postpancreatectomy hemorrhage: a review of randomized trials. Int J Surg. 2024;110:6145-6154. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 14] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 32. | Kailey B, van de Bunt M, Cheley S, Johnson PR, MacDonald PE, Gloyn AL, Rorsman P, Braun M. SSTR2 is the functionally dominant somatostatin receptor in human pancreatic β- and α-cells. Am J Physiol Endocrinol Metab. 2012;303:E1107-E1116. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 103] [Cited by in RCA: 130] [Article Influence: 9.3] [Reference Citation Analysis (0)] |
| 33. | Shamsi BH, Chatoo M, Xu XK, Xu X, Chen XQ. Versatile Functions of Somatostatin and Somatostatin Receptors in the Gastrointestinal System. Front Endocrinol (Lausanne). 2021;12:652363. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 56] [Cited by in RCA: 48] [Article Influence: 9.6] [Reference Citation Analysis (0)] |
| 34. | Battershill PE, Clissold SP. Octreotide. A review of its pharmacodynamic and pharmacokinetic properties, and therapeutic potential in conditions associated with excessive peptide secretion. Drugs. 1989;38:658-702. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 83] [Cited by in RCA: 85] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 35. | Alvikas J, Dahiya S, Dubrovsky G. A Review of Post-Operative Pancreatic Fistula Following Distal Pancreatectomy: Risk Factors, Consequences, and Mitigation Strategies. Cancers (Basel). 2025;17:2741. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 36. | Hou Z, Hou S, Wang Z, Wang H, Deng M, Fan H. The influence of somatostatin analogues on the incidence of pancreatic fistulas and postoperative morbidity in patients undergoing pancreatic resection: A Bayesian network meta-analysis. PLoS One. 2025;20:e0331909. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 37. | Alzelfawi L, Almajed E, AlZabin A, Alruwaili E, Alomar L, Alkhudairy A, Malaika L, Alshamrani A, Albishri S. Prevention of Postoperative Pancreatic Fistula: Systematic Review and Meta-Analysis. Surgeries. 2024;5:875-895. [DOI] [Full Text] |
| 38. | Bassi C, Marchegiani G, Dervenis C, Sarr M, Abu Hilal M, Adham M, Allen P, Andersson R, Asbun HJ, Besselink MG, Conlon K, Del Chiaro M, Falconi M, Fernandez-Cruz L, Fernandez-Del Castillo C, Fingerhut A, Friess H, Gouma DJ, Hackert T, Izbicki J, Lillemoe KD, Neoptolemos JP, Olah A, Schulick R, Shrikhande SV, Takada T, Takaori K, Traverso W, Vollmer CM, Wolfgang CL, Yeo CJ, Salvia R, Buchler M; International Study Group on Pancreatic Surgery (ISGPS). The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 Years After. Surgery. 2017;161:584-591. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3570] [Cited by in RCA: 3302] [Article Influence: 366.9] [Reference Citation Analysis (4)] |
| 39. | Boertien TM, Drent ML, Booij J, Majoie CBLM, Stokkel MPM, Hoogmoed J, Pereira AM, Biermasz NR, Simsek S, Veldman RG, Weterings AJ, Vink JM, Tanck MWT, Fliers E, Bisschop PH. Lanreotide versus placebo for tumour reduction in patients with a (68)Ga-DOTATATE PET-positive, clinically non-functioning pituitary macroadenoma (GALANT study): a randomised, multicentre, phase 3 trial with blinded outcome assessment. Lancet Reg Health Eur. 2024;42:100923. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/