Published online Feb 27, 2026. doi: 10.4240/wjgs.v18.i2.115072
Revised: December 7, 2025
Accepted: January 12, 2026
Published online: February 27, 2026
Processing time: 142 Days and 6.5 Hours
Pancreatic duct stones often develop in the late stage of chronic pancreatitis. How
A young man who had been smoking for 10 years and drinking alcohol for 5 years had a history of abdominal pain for 8 years and diarrhea for 2 years. The patient was diagnosed with “chronic pancreatitis combined with pancreatic duct stones” in other hospitals and underwent several endoscopic treatments, but the abdo
The main contribution of this case is the development of a modified surgical procedure for chronic pancreatitis complicated by complex pancreatic duct stones. For chronic pancreatitis complicated by stones that respond poorly to pharmacotherapy or endoscopic treatment, surgery is a worthy early treatment option. Early surgical inter
Core Tip: This case report detailed the development of a novel surgical approach by our team for the treatment of pancreatic duct stones, drawing on the contributions of previous researchers. For patients with multiple pancreatic duct stones complicated by pancreatic duct dilatation, this surgical approach can maximize the removal of pancreatic duct stones, reduce the risk of stone recurrence, and alleviate postoperative pain.
- Citation: Gou HX, Deng C, Wen Y, Yin ZL, Yang TY, Wang T, Luo H, Cheng L. Pancreatic head resection alongside side-to-side pancreatic duct-jejunostomy for pancreatic stones: A case report and review of literature. World J Gastrointest Surg 2026; 18(2): 115072
- URL: https://www.wjgnet.com/1948-9366/full/v18/i2/115072.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i2.115072
Pancreatic duct stones are mainly manifested in patients with chronic pancreatitis[1]. Chronic pancreatitis is caused by a variety of factors. Its pathological and morphological characteristics include chronic, persistent inflammatory damage to the pancreatic parenchyma, irreversible fibrosis, and irreversible changes, such as pancreatic duct dilatation, pancreatic calcification, or formation of pancreatic duct stones. These changes can lead to both pancreatic endocrine and exocrine insufficiency[2-4]. The main clinical manifestations of chronic pancreatitis are persistent abdominal pain, steatorrhea, diabetes, and weight loss. If pancreatic head stones are accompanied by inflammatory masses, they may compress the bile duct and cause biliary obstruction[5,6]. A small number of patients may develop splenic vein thrombosis, showing symptoms of regional portal hypertension, such as splenomegaly and esophageal varices[7]. Impacted stones in the pancreatic duct are commonly associated with pancreatic duct stenosis, impaired drainage of pancreatic secretions, and pancreatic duct hypertension, which are considered the principal etiological factors for the aforementioned symptoms. Additionally, prolonged chronic inflammation has been implicated in the development of secondary malignancies[8].
Endoscopic techniques, such as endoscopic retrograde cholangiopancreatography (ERCP), play an increasingly vital role in managing chronic pancreatitis complicated by pancreatic duct stones[5]. However, owing to the presence of severe pancreatic duct stenosis or complete occlusion, ductal variations, and extensive, calcified pancreatic duct stones, some patients with pancreatic duct stones may still require surgical treatment[9]. Depending on the pancreatic duct pathology and stone distribution, different surgical approaches can be applied. Some of these procedures are principally designed for drainage, such as the Partington and Puestow procedures; others primarily concentrate on resection, such as the Whipple and Beger procedures; and some, such as the Frey procedure, combine both resection and drainage. Each of these surgical approaches possesses its own advantages and limitations[10].
This study reports a case of chronic pancreatitis complicated by pancreatic duct stones who underwent duodenum-preserving total pancreatic head resection, combined with complete incision of the pancreatic duct in the body and tail, and side-to-side pancreaticojejunostomy. This approach successfully achieved both lesion resection and adequate drainage of the pancreatic duct, resulting in excellent therapeutic outcomes. This surgical technique, pioneered by our team, has not been previously reported. Additionally, a literature review provides a comparative analysis of this novel approach with traditional surgical methods, systematically discussing their respective advantages, disadvantages, and areas of application.
A 24-year-old unmarried man was admitted to our hospital with severe abdominal pain for one week.
The patient had a 10-year history of smoking and a 5-year history of alcohol abuse, with an average daily intake of approximately 200 g of Chinese liquor. The primary concern is recurrent epigastric pain, which has been ongoing for 8 years, and chronic diarrhea has persisted for approximately 2 years. The patient has sought medical attention at several hospitals due to the exacerbation of pain. Diagnostic evaluations demonstrated a diagnosis of chronic pancreatitis with pancreatic duct stones, and the patient has undergone six ERCP procedures and pancreatic duct stone removal at external institutions. However, each time the patient presented with pain, new pancreatic duct stones were identified, which had developed after the previous stone removal. Furthermore, there was progressive dilation of the pancreatic duct, accompanied by atrophy of the pancreatic parenchyma. One week prior, the patient presented to our hospital with significantly worsened abdominal pain. The pain was persistent and dull in nature, and although the diarrhea had not worsened, the patient reported no other complaints.
The patient had been hospitalized multiple times in the past, but no disease was diagnosed except for pancreatic duct stones.
The patient denied any other medical history or family history of genetic disorders.
On admission, the patient’s vital signs were normal, his body mass index was within normal limits, and only diffuse, mild abdominal tenderness was noted.
A complete blood biochemistry test revealed a serum amylase level of 152 U/L (normal range: 25-125 U/L, enzyme-coupled assay). No other significant abnormalities were found.
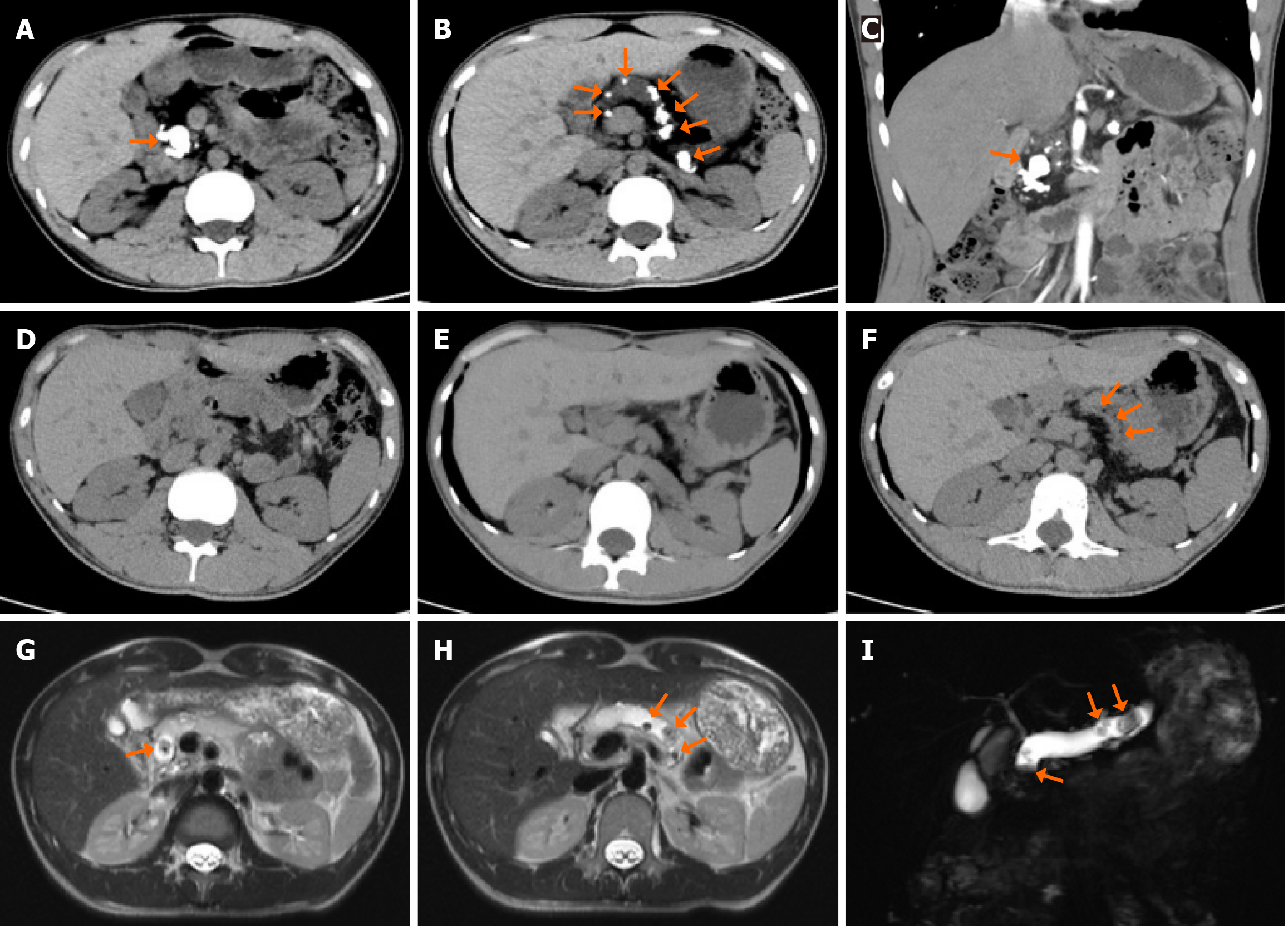
Computed tomography (CT) scan revealed remarkable pancreatic atrophy and a prominent dilatation of the main pancreatic duct, reaching 1.6 cm. Multiple high-density stones were observed in the main pancreatic duct and pancreatic parenchyma. Magnetic resonance imaging confirmed the presence of pancreatic duct dilation, approximately 1.5 cm at its widest point. Multiple nodular filling defects were identified in the main pancreatic duct, and their largest reached a diameter of 1.2 cm (Figure 1).
The patient was diagnosed with chronic pancreatitis combined with multiple pancreatic duct stones.
Utilizing imaging examinations, numerous stones were lodged in the main pancreatic duct and the uncinate duct in the pancreatic head, and additional stones were scattered throughout the pancreatic body and tail. The patient has expe
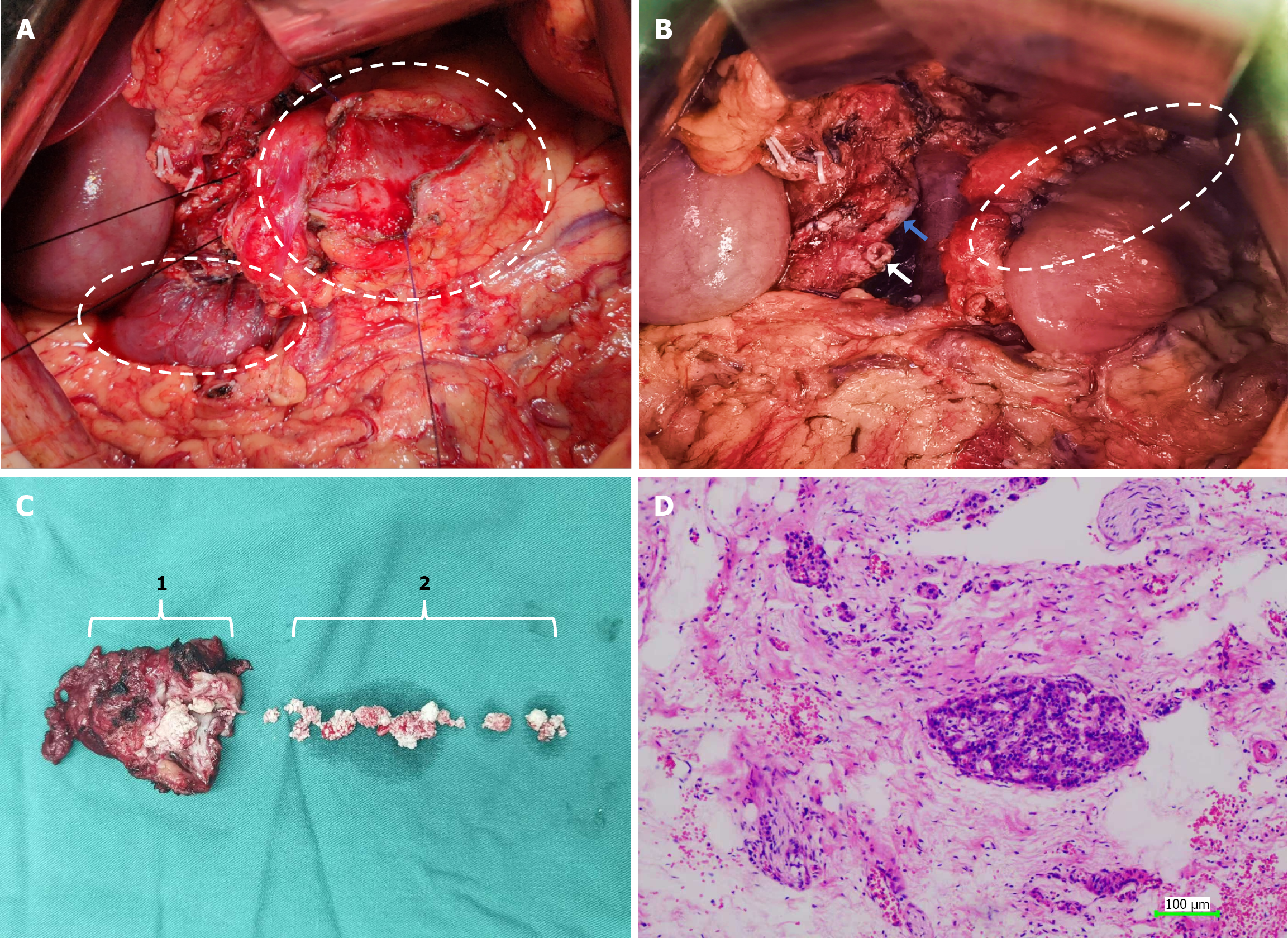
Postoperative pathology revealed cystic dilatation of the pancreatic duct, periductal fibrosis, and chronic inflammatory cell infiltration. Pancreatic tissue degeneration, glandular atrophy, and interstitial fibrosis were also identified, thereby confirming chronic pancreatitis (Figure 2D). Postoperative blood biochemistry monitoring revealed transient leukocytosis and elevated serum amylase level, peaking on the first day after surgery and returning to normal after one week. The patient’s blood sugar remained normal postoperatively.
One year after surgery, the patient’s abdominal pain was completely resolved. The follow-up CT scan demonstrated complete stone removal with no recurrence (Figure 1D and E). Compared with the preoperative level, the patient’s post
Pancreatic duct stones are a late complication of chronic pancreatitis, and approximately 50%-90% of patients with chro
The patient had previously undergone 6 ERCP-guided stone removal procedures or endoscopic treatments at other hospitals. CT and magnetic resonance imaging examinations, performed at the time of the presentation, revealed re
The main cause of abdominal pain caused by pancreatic duct stones is obstruction of the pancreatic duct by stones, impeding pancreatic fluid drainage and increasing pressure in the distal pancreatic duct. As a result, some researchers have proposed surgical drainage of pancreatic fluid to mitigate pain. Duval[21] was the first to implement a surgical procedure for chronic pancreatitis associated with pancreatic duct stones, involving resecting the pancreatic tail and spleen, followed by an end-to-end anastomosis between the pancreatic duct and jejunum. However, this procedure lacked adequate treatment of pancreatic duct lesions, leading to the progressive segmental stenosis of the duct and, consequently, long-term decompression failure[21-25]. To address this problem, Puestow and Gillesby[23], building on Duval’s method[21], performed a longitudinal incision of the pancreatic duct and a side-to-side anastomosis of the pancreatic duct with the jejunum. Partington and Rochelle[25], on the basis of Puestow and Gillesby’s method[23], only incised the entire pancreatic duct, preserving the pancreatic tail, and subsequently conducted a side-to-side anastomosis of the pancreatic duct and jejunum[24,25]. The Partington and Puestow procedures are effective in resolving stones in the pancreatic body and tail, and in providing adequate drainage of pancreatic fluid, significantly lowering the risk of recurrence of pancreatic duct stones. However, these procedures do not address the underlying etiology of abdominal pain resulting from stones and inflammation in the pancreatic head[26].
As procedures, such as the Partington and Puestow, that primarily concentrate on drainage, have limitations in ma
Compared with Whipple, PPPD, and TP procedures, duodenum-preserving pancreatic head resection (DPPHR) significantly preserves pancreatic function and avoids overtreatment. Beger first proposed a procedure involving pancreatic head resection with end-to-end anastomosis of the pancreatic duct and jejunum[32]. This procedure signifi
Compared with the Beger procedure, the Frey procedure provides a more targeted approach for treating the pancreatic head. The Frey procedure selectively removes the inflammatory mass in the pancreatic head, longitudinally opens the main pancreatic duct, and then performs a side-to-side pancreatic duct-jejunal anastomosis. This procedure has a larger anastomotic opening, remarkably reducing the possibility of anastomotic stenosis and the probability of stone recurrence. However, it is inferior to the Beger procedure in terms of postoperative pain relief[27], which may be associated with the narrow excision of the pancreatic head, residual stenosis of the main pancreatic duct, and incomplete treatment of the branch pancreatic ducts. Gloor et al[36] developed a relatively smaller pancreaticojejunostomy (Berne procedure) based on the Frey procedure. This modification requires lower technical expertise, promoting a faster operation, and it is associated with fewer postoperative complications[36,37]. The Frey procedure requires a full longitudinal pancreatic duct-jejunum anastomosis and is easier to perform in patients with pancreatic duct dilatation. The Beger and Berne procedures, on the other hand, involve only end-to-end anastomosis or short side-to-side anastomosis and may be more appropriate for patients with lesions confined to the pancreatic head and without significant pancreatic duct dilatation. DPPHR is a combination of resection and drainage. Although DPPHR provides comparable pain relief to simple resection, its overall postoperative complications and long-term pain remission rates are superior to those of simple resection or drainage[13]. The Table 1 shows the short-term and long-term pain relief outcomes of common surgical procedures for treating chronic pancreatitis[38].
| Comparison of surgical methods | Short-term pain relief | Long-term pain relief | ||
| OR | 95%CI | MD | 95%CI | |
| PPPD vs Frey | 0.61 | 0.13-2.6 | 0.37 | -10.0 to 12.0 |
| PPPD vs Beger | 0.71 | 0.30-1.61 | - | - |
| PPPD vs Berne | 0.83 | 0.19-3.85 | - | - |
| Beger vs Frey | 0.86 | 0.19-3.8 | -0.74 | -11.0 to 0.0 |
| Beger vs Berne | 1.16 | 0.28-4.84 | - | - |
A novel surgical approach was described, integrating the advantages of total pancreatic head resection with the decompressive effect of the Partington procedure. Complete resection of the pancreatic head could effectively remove stones in both the pancreatic head and the uncinate process. In contrast, when only the pancreatic duct in the body and tail is opened, and a choledochoscope is used to remove stones, complete stone removal is often compromised due to the complex pancreatic ductal system in the head, or because the large angle of the uncinate process may prevent the choledochoscope from passing through[11,39]. Total resection of the pancreatic head eliminates residual inflammatory tissue and prevents postoperative recurrence of stones, which can arise from the complexity of the pancreatic duct system in this region. Additionally, given the dense distribution of nerves in the pancreatic head, complete removal addresses the primary source of pain, thereby reducing the risk of postoperative pain recurrence[27]. Throughout the procedure, the anatomical integrity and function of the duodenum and common bile duct are preserved with precision. Special attention is required to avoid injury to the vascular arch formed by the superior and inferior pancreaticoduodenal arteries to protect the blood supply to the duodenum. The pancreatic duct is then longitudinally incised for approximately 10 cm along the body and tail of the pancreas to fully expose the stones in the duct lumen. The pancreatic duct in the body and tail is opened throughout, and all stones can be removed under direct vision, so that the pancreatic duct in the body and tail is fully decompressed.
Lithotomy forceps and a choledochoscope are used in combination to thoroughly remove all stones in the pancreatic duct and to ensure patency of the duct lumen. Finally, the digestive tract is reconstructed. The jejunum is transected 20 cm distal to the ligament of Treitz, and the distal jejunum is then mobilized to the pancreas, where a side-to-side anastomosis is performed with the opened pancreatic duct. Furthermore, its large-caliber side-to-side anastomosis minimizes the possibility of postoperative stenosis, possesses advantages in terms of preserving the endocrine and exocrine functions of the pancreas, and a better long-term prognosis may be achieved.
The proposed surgical approach is applicable to cases of chronic complicated pancreatitis with stones obstructing the main pancreatic duct, particularly in cases of significant ductal dilation. This procedure should be considered as an alternative treatment for complicated pancreatitis following the failure of endoscopic interventions. It effectively removes stones that are difficult to extract endoscopically or by other interventional methods. Additionally, compared with conservative treatment or selective visceral nerve transection, this surgical approach possesses the advantage of complete resection of the primary lesion, resulting in more stable long-term pain relief.
However, this surgical approach has limitations and foreseeable risks, similar to other surgical options[13,38]. Long-term, recurrent pancreatic inflammation causes severe edema in the pancreatic head, obscuring anatomical clearances. Under these conditions, performing total pancreatic head resection with duodenum preservation is technically cha
The main contribution of this case report is the development of a modified surgical procedure for chronic pancreatitis complicated by complex pancreatic duct stones. For chronic pancreatitis complicated by stones that respond poorly to pharmacotherapy or endoscopic treatment, surgery is a worthy early treatment option. Early surgical intervention can effectively drain pancreatic juice, delay pancreatic atrophy, and protect pancreatic function. The proposed modified procedure can more thoroughly remove stones and reduce the recurrence rate of stones and pain. Although this proce
| 1. | McCarty TR, Sobani Z, Rustagi T. Per-oral pancreatoscopy with intraductal lithotripsy for difficult pancreatic duct stones: a systematic review and meta-analysis. Endosc Int Open. 2020;8:E1460-E1470. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 36] [Cited by in RCA: 33] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 2. | Rösch T, Daniel S, Scholz M, Huibregtse K, Smits M, Schneider T, Ell C, Haber G, Riemann JF, Jakobs R, Hintze R, Adler A, Neuhaus H, Zavoral M, Zavada F, Schusdziarra V, Soehendra N; European Society of Gastrointestinal Endoscopy Research Group. Endoscopic treatment of chronic pancreatitis: a multicenter study of 1000 patients with long-term follow-up. Endoscopy. 2002;34:765-771. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 358] [Cited by in RCA: 291] [Article Influence: 12.1] [Reference Citation Analysis (0)] |
| 3. | Kaushik N, Dasari V, Jain D. Management of Pancreatic Calculi in Chronic Pancreatitis: A Review Article. Cureus. 2023;15:e35788. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 9] [Article Influence: 3.0] [Reference Citation Analysis (3)] |
| 4. | Wang D, Bi YW, Xu H, Wang T, Li ZS, Xu ZL, Hu LH. Rapid formation of a radiolucent pancreatic stone: a case report (with video). J Int Med Res. 2020;48:300060520951418. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 5. | Choi EK, Lehman GA. Update on endoscopic management of main pancreatic duct stones in chronic calcific pancreatitis. Korean J Intern Med. 2012;27:20-29. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 16] [Article Influence: 1.1] [Reference Citation Analysis (1)] |
| 6. | Abdallah AA, Krige JE, Bornman PC. Biliary tract obstruction in chronic pancreatitis. HPB (Oxford). 2007;9:421-428. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 128] [Cited by in RCA: 99] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 7. | Heider TR, Azeem S, Galanko JA, Behrns KE. The natural history of pancreatitis-induced splenic vein thrombosis. Ann Surg. 2004;239:876-80; discussion 880. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 127] [Cited by in RCA: 107] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 8. | Iwata K, Iwashita T, Mukai T, Iwasa Y, Okuno M, Yoshida K, Maruta A, Uemura S, Yasuda I, Shimizu M. Peroral Pancreatoscopy-Guided Lithotripsy Compared with Extracorporeal Shock Wave Lithotripsy in the Management of Pancreatic Duct Stones in Chronic Pancreatitis: A Multicenter Retrospective Cohort Study. Diagnostics (Basel). 2024;14:891. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 9. | Ahmed Ali U, Pahlplatz JM, Nealon WH, van Goor H, Gooszen HG, Boermeester MA. Endoscopic or surgical intervention for painful obstructive chronic pancreatitis. Cochrane Database Syst Rev. 2015;2015:CD007884. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 36] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 10. | Zhao X, Cui N, Wang X, Cui Y. Surgical strategies in the treatment of chronic pancreatitis: An updated systematic review and meta-analysis of randomized controlled trials. Medicine (Baltimore). 2017;96:e6220. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 33] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 11. | Han S, Miley A, Akshintala V, Freeman ML, Kahaleh M, Othman M, Patel S, Papachristou GI, Raijman I, Sankey N, Sayana H, Singh V, Tarnasky P, Trikudanathan G, Shah RJ. Per-oral pancreatoscopy-guided lithotripsy vs. extracorporeal shock wave lithotripsy for treating refractory main pancreatic duct stones in chronic pancreatitis: Protocol for an open-label multi-center randomized clinical trial. Pancreatology. 2022;22:1120-1125. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 17] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 12. | Rijk FEM, Stassen PMC, van der Wiel SE, Boermeester MA, Issa Y, Kempeneers MA, Verdonk RC, Bruno MJ, de Jonge PJF. Long-term outcomes of pancreatoscopy-guided electrohydraulic lithotripsy for the treatment of obstructive pancreatic duct stones. Endosc Int Open. 2023;11:E296-E304. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 9] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 13. | Dankha R, Sparrelid E, Gilg S, Löhr JM, Ghorbani P. Surgical management of chronic pancreatitis: A narrative review. United European Gastroenterol J. 2025;13:44-54. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 9] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 14. | Noda A, Okuyama M, Murayama H, Takeuchi K, Yokota T, Kobayashi T, Takayama T. Dissolution of pancreatic stones by oral trimethadione in patients with chronic calcific pancreatitis. J Gastroenterol Hepatol. 1994;9:478-485. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 11] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 15. | Cahen DL, Gouma DJ, Nio Y, Rauws EA, Boermeester MA, Busch OR, Stoker J, Laméris JS, Dijkgraaf MG, Huibregtse K, Bruno MJ. Endoscopic versus surgical drainage of the pancreatic duct in chronic pancreatitis. N Engl J Med. 2007;356:676-684. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 701] [Cited by in RCA: 507] [Article Influence: 26.7] [Reference Citation Analysis (0)] |
| 16. | Udd M, Kylänpää L, Kokkola A. The Role of Endoscopic and Surgical Treatment in Chronic Pancreatitis. Scand J Surg. 2020;109:69-78. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 18] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 17. | Buscher HC, Jansen JB, van Dongen R, Bleichrodt RP, van Goor H. Long-term results of bilateral thoracoscopic splanchnicectomy in patients with chronic pancreatitis. Br J Surg. 2002;89:158-162. [PubMed] [DOI] [Full Text] |
| 18. | Phillips AM. Chronic pancreatitis; pathogenesis and clinical features: study of twenty-eight cases. AMA Arch Intern Med. 1954;93:337-354. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 10] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 19. | Cahow CE, Hayes MA. Operative treatment of chronic recurrent pancreatitis. Am J Surg. 1973;125:390-398. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 6] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 20. | Abdel Aziz AM, Lehman GA. Current treatment options for chronic pancreatitis. Curr Treat Options Gastroenterol. 2007;10:355-368. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 15] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 21. | Duval MK Jr. Caudal pancreatico-jejunostomy for chronic relapsing pancreatitis. Ann Surg. 1954;140:775-785. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 156] [Cited by in RCA: 118] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 22. | Zollinger RM, Keith LM Jr, Ellison EH. Pancreatitis. N Engl J Med. 1954;251:497-502. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 63] [Cited by in RCA: 52] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 23. | Puestow CB, Gillesby WJ. Retrograde surgical drainage of pancreas for chronic relapsing pancreatitis. AMA Arch Surg. 1958;76:898-907. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 267] [Cited by in RCA: 188] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 24. | Andersen DK, Frey CF. The evolution of the surgical treatment of chronic pancreatitis. Ann Surg. 2010;251:18-32. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 92] [Cited by in RCA: 70] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 25. | Partington PF, Rochelle RE. Modified Puestow procedure for retrograde drainage of the pancreatic duct. Ann Surg. 1960;152:1037-1043. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 313] [Cited by in RCA: 210] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 26. | Bhandari S, Sanghvi K, Sharma A, Bondade N, Maydeo A. Endoscopic management of large pancreatic stones in patient after lateral pancreaticojejunostomy. Gastrointest Endosc. 2016;83:659-660. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 27. | D'Haese JG, Ceyhan GO, Demir IE, Tieftrunk E, Friess H. Treatment options in painful chronic pancreatitis: a systematic review. HPB (Oxford). 2014;16:512-521. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 49] [Cited by in RCA: 37] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 28. | Traverso LW, Longmire WP Jr. Preservation of the pylorus in pancreaticoduodenectomy a follow-up evaluation. Ann Surg. 1980;192:306-310. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 165] [Cited by in RCA: 149] [Article Influence: 3.2] [Reference Citation Analysis (4)] |
| 29. | Whipple AO. Radical Surgery for Certain Cases of Pancreatic Fibrosis associated with Calcareous Deposits. Ann Surg. 1946;124:991-1006. [PubMed] |
| 30. | Izbicki JR, Bloechle C, Broering DC, Knoefel WT, Kuechler T, Broelsch CE. Extended drainage versus resection in surgery for chronic pancreatitis: a prospective randomized trial comparing the longitudinal pancreaticojejunostomy combined with local pancreatic head excision with the pylorus-preserving pancreatoduodenectomy. Ann Surg. 1998;228:771-779. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 294] [Cited by in RCA: 228] [Article Influence: 8.1] [Reference Citation Analysis (1)] |
| 31. | Bramis K, Gordon-Weeks AN, Friend PJ, Bastin E, Burls A, Silva MA, Dennison AR. Systematic review of total pancreatectomy and islet autotransplantation for chronic pancreatitis. Br J Surg. 2012;99:761-766. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 89] [Cited by in RCA: 74] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 32. | Ratnayake CBB, Kamarajah SK, Loveday BPT, Nayar M, Oppong K, White S, French JJ, Windsor JA, Pandanaboyana S. A Network Meta-analysis of Surgery for Chronic Pancreatitis: Impact on Pain and Quality of Life. J Gastrointest Surg. 2020;24:2865-2873. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 9] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 33. | Bonin EA, Canzi Almada de Souza R, Taglieri E, Silveira Cathcart N, Dos Santos EC, Schmitt de Bem R, Ardengh JC. Peroral antegrade pancreatoscopy for pancreaticolithiasis after endoscopic ultrasound-guided recanalization of a complete pancreaticojejunal stenosis. Endoscopy. 2018;50:E333-E335. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 34. | Tandan M, Talukdar R, Reddy DN. Management of Pancreatic Calculi: An Update. Gut Liver. 2016;10:873-880. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 81] [Cited by in RCA: 61] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 35. | Jawad ZAR, Tsim N, Pai M, Bansi D, Westaby D, Vlavianos P, Jiao LR. Short and long-term post-operative outcomes of duodenum preserving pancreatic head resection for chronic pancreatitis affecting the head of pancreas: a systematic review and meta-analysis. HPB (Oxford). 2016;18:121-128. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 21] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 36. | Gloor B, Friess H, Uhl W, Büchler MW. A modified technique of the Beger and Frey procedure in patients with chronic pancreatitis. Dig Surg. 2001;18:21-25. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 162] [Cited by in RCA: 116] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 37. | Strobel O, Büchler MW, Werner J. [Duodenum-preserving pancreatic head resection: technique according to Beger, technique according to Frey and Berne modifications]. Chirurg. 2009;80:22-27. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 9] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 38. | Mou Y, Song Y, Chen HY, Wang X, Huang W, Liu XB, Ke NW. Which Surgeries Are the Best Choice for Chronic Pancreatitis: A Network Meta-Analysis of Randomized Controlled Trials. Front Surg. 2021;8:798867. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 6] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 39. | Motomura D, Irani S, Larsen M, Kozarek RA, Ross AS, Gan SI. Multicenter retrospective cohort of EUS-guided anterograde pancreatic duct access. Endosc Int Open. 2023;11:E358-E365. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/