Published online Apr 15, 2026. doi: 10.4251/wjgo.v18.i4.116137
Revised: January 4, 2026
Accepted: January 27, 2026
Published online: April 15, 2026
Processing time: 133 Days and 22.9 Hours
Patients diagnosed with middle- and late-stage digestive tract tumors often experience persistent pain, which seriously affects their quality of life (QoL) and treatment adherence. Although traditional nursing models of pain management rely primarily on regular assessments by medical personnel and simple pharmacological interventions, they lack attention to patients’ individualized needs and continuous nursing support. However, the development of “Internet+” technologies and the 5A (Ask, Assess, Advise, Assist, And Arrange) nursing model, along with their application medical care, has gradually attracted attention.
To explore the effect of the Internet+ 5A nursing model on patients experiencing middle- and late-stage digestive tract tumor pain.
One hundred patients experiencing pain from middle- and late-stage digestive tract tumors were prospectively divided into two groups: control [routine pain management (n = 50)] and observation [Internet+ 5A nursing model (n = 50)]. The Numerical Rating Scale (NRS), European Organization for Research and Treat
After 1 month of nursing intervention, the NRS score of the observation group was significantly lower than that of the control group (P < 0.05). Both groups exhibited significant improvements in all items of the EORTC QLQ-C30 scale (P < 0.05); however, the observation group exhibited higher scores in cognitive, role, emotional, physical, and social functions (P < 0.05). After one month of treatment, the increases in all C-SUPPH scores in the observation group were greater than those in the control group (P < 0.05). Moreover, the observation group had lower scores for pain intensity, activity interference, sleep interference, emotion, and adverse reactions related to pain treatment drugs on the APS-POQ-C scale, with a higher score for pain management perception than the control group (P < 0.05).
The Internet+ 5A nursing model reduces pain intensity in patients with middle- and late-stage digestive tract tumors, improves enhances QoL, thereby supporting its implementation in clinical practice.
Core Tip: This study investigates the effect of the Internet+ 5A nursing model on patients with middle- and late-stage digestive tract tumors pain. A prospective study of 100 patients demonstrated that the intervention group, compared to the control group receiving routine care, yielded superior outcomes. Specifically, it significantly reduced pain intensity (Numerical Rating Scale), and enhanced overall quality of life (European Organization for Research and Treatment of Cancer Quality of Life Questionnaire-Core 30). The model also boosted self-management efficacy and improved various patient-reported outcomes. The Internet+ 5A nursing model is concluded to be effective and merits clinical application.
- Citation: Wang L, Ma XQ, Ju CX, Fu J. Effect of the Internet+ 5A nursing model on patients with middle- and late-stage digestive tract tumors pain. World J Gastrointest Oncol 2026; 18(4): 116137
- URL: https://www.wjgnet.com/1948-5204/full/v18/i4/116137.htm
- DOI: https://dx.doi.org/10.4251/wjgo.v18.i4.116137
Patients diagnosed with middle- and late-stage digestive tract tumors often experience persistent pain that seriously affects their quality of life (QoL) and treatment adherence[1-3]. Pain not only causes physical suffering but also leads to psychological problems such as anxiety and depression, which further affect patients’ immune function and treatment outcomes[4]. Traditional nursing models of pain management rely primarily on regular assessments by medical staff and simple pharmacological interventions, but lack attention to patients’ individualized needs and continuous nursing support[5]. Moreover, traditional models are often limited to in-hospital care, failing to address the long-term self-management needs of patients in home settings, especially for symptom monitoring and timely intervention[6].
With the continuous development of “Internet+” technology, its application in the field of medical care has gradually attracted attention. Internet technologies provide more convenient and efficient information transmission and communication channels for nursing services, which can overcome the limitations of time and space, enabling patients to receive timely nursing guidance and psychological support, even outside hospital settings[7]. A series of systematic reviews and empirical studies have confirmed the effectiveness of Internet-based interventions in cancer care: For example, web-based collaborative care interventions have been shown to effectively manage cancer-related symptoms in palliative care settings[8]; nurse-led telehealth interventions significantly improve symptom control in patients receiving systemic or radiation therapy[9]; and Internet-based interventions can alleviate chemotherapy-related symptoms and improve QoL[10]. Additionally, the development and feasibility of web applications specifically designed for cancer pain monitoring have been verified, providing practical tools for remote pain management[11]. Technology-based interven
The “5A” nursing model is a patient-centered nursing model that provides comprehensive, personalized, and continuous nursing services for patients through the following five aspects: Ask, Assess, Advise, Assist, And Arrange[13]. Existing studies have demonstrated the versatility of the 5A model in cancer care: It improves sleep quality in cancer patients through self-management guidance[14], and enhances QoL and self-care efficacy in patients undergoing chemotherapy after hepatocellular carcinoma surgery[15]. However, current studies investigating the application of the Internet+ 5A nursing model in patients with middle- and late-stage digestive tract tumor pain are relatively limited, and some studies have not been fully verified. Therefore, the present study aimed to develop an Internet+-based 5A nursing model and investigate its impact on patients experiencing middle- and late-stage digestive tract tumor pain, providing new concepts and methods for clinical nursing practice.
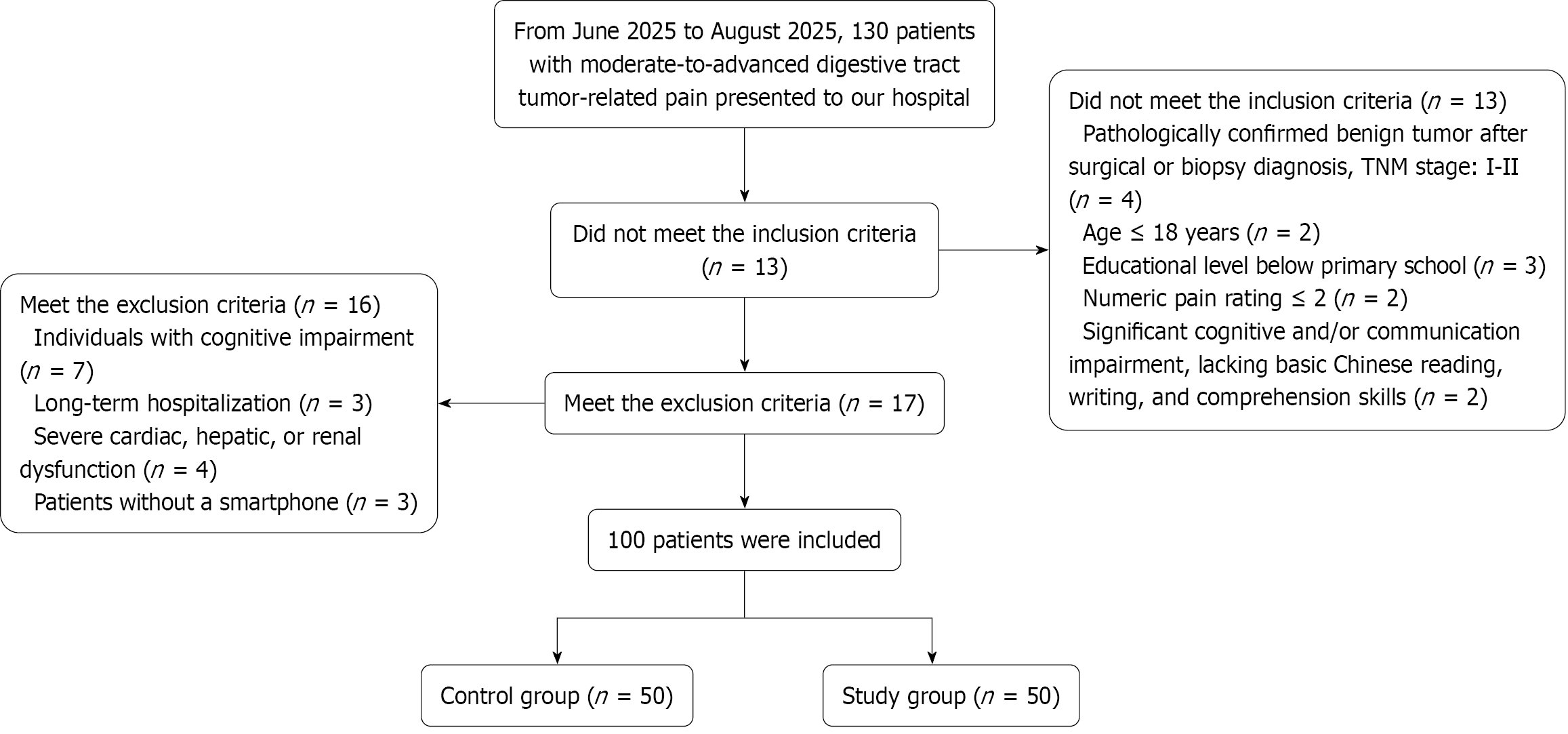
This was a prospective study. From June 2025 to August 2025, a total of 130 patients with advanced digestive tract tumors (moderate to advanced stage) complicated by pain were screened. Among these, 30 patients were excluded for not meeting the inclusion and exclusion criteria, and 100 eligible patients were ultimately included in the study. A flow diagram illustrating the enrollment process, including the application of inclusion and exclusion criteria and the final grouping of participants, is presented in Figure 1. Patients were divided into two groups using a random number table method: A control group (receiving conventional pain management, n = 50) and an experimental group (receiving Internet+ 5A nursing model intervention in addition to conventional pain care, n = 50). Statistical analysis of the general data from the two patient groups revealed no significant differences (P > 0.05; Table 1). This study was approved by the hospital ethics committee.
| Group | n | Age (years) | Male | Female |
| Control group | 50 | 65.23 ± 3.15 | 28 | 22 |
| Observation group | 50 | 65.18 ± 3.21 | 30 | 20 |
| t/χ² value | - | 0.079 | 0.164 | 0.164 |
| P value | - | 0.938 | 0.685 | 0.685 |
The sample size for this study was estimated using the formula for comparing means between two independent samples: n = 2[(Zα/2 + Zβ)σ/δ]2. The parameters were set as follows: α = 0.05 for a two-sided test, resulting in Zα/2 = 1.96; β = 0.2, resulting in Zβ = 0.842. Based on preliminary experiment results, the difference in Numerical Rating Scale (NRS) scores between groups (δ) was set at 1.2, and the SD (σ) was set at 1.5. The calculation yielded a required sample size of approximately 42 participants per group. Considering potential factors such as loss to follow-up, the sample size was increased by 20%. Consequently, 50 patients were included in each group, totaling 100 patients. Power analysis confirmed that with 50 subjects per group, the study had sufficient statistical power (power > 0.8) to detect differences in NRS scores between the two groups.
Inclusion criteria: (1) Diagnosed with advanced (TNM stage III-IV) digestive tract malignancy confirmed by pathological examination (surgical or biopsy), including common types such as esophageal cancer, gastric cancer, colorectal cancer, liver cancer, pancreatic cancer, etc.; (2) Age between 18 years and 85 years; (3) NRS score ≥ 1 point; (4) Mini-Mental State Examination score ≥ 24 points, without communication barriers, and possessing basic literacy and comprehension skills; and (5) Expected survival > 3 months and voluntary participation in the study.
Exclusion criteria: (1) Patients with severe mental disorders (e.g., schizophrenia, major depression) or cognitive impairment (e.g., Alzheimer’s disease, vascular dementia); (2) Patients with continuous hospitalization > 1 month or already receiving palliative care; (3) Patients with severe dysfunction of vital organs, such as severe cardiac insufficiency (New York Heart Association class III-IV), hepatic insufficiency (Child-Pugh class C), or renal insufficiency (creatinine clearance rate < 30 mL/minute); (4) Patients unable to cooperate with internet-based nursing interventions; and (5) Patients simultaneously participating in other similar clinical studies.
The control group underwent routine pain management, which included the following measures: A comprehensive, accurate, and dynamic assessment of pain intensity. The head nurse taught patients to use the NRS for pain scoring: Pain scores < 4 points were assessed once per day and pain scores ≥ 4 points were reassessed every 30 minutes until the pain score was < 4 points. If patients experienced breakthrough pain with a pain score ≥ 4 points, analgesic drugs were administered as prescribed by physicians, and dynamic assessment of pain intensity was continued. The time of assess
Medication guidance was strengthened as follows: Provide health education to patients regarding pain-related knowledge, usage methods of analgesic drugs, precautions, and adverse reactions. Communication with patients should be strengthened, their psychological needs understood, and comfort and encouragement provided. Conduct telephone follow-ups once per week for four consecutive weeks after patient discharge from the hospital.
The observation group received an Internet+ 5A nursing model intervention based on routine pain care. A comprehensive set of nursing interventions was provided to patients through five key steps: Ask, Assess, Advise, Assist, and Arrange.
Through multiparty communication and negotiation, an intervention team consisting of two oncologists, one pharmacist, one dietitian, one psychological counselor, one oncology specialist nurse, one traditional Chinese Medicine (TCM) specialist nurse, two head nurses, and the researcher (serving as the team leader). The physicians had intermediate or higher professional titles in the hospital, the dietitian was an expert from the hospital’s nutrition department, and the psychological counselor was a psychological expert who obtained the national second-level psychological counselor qualification certificate. All specialized nurses held municipal or higher specialized nursing qualifications, and the head nurses had > 10 years of work experience and had obtained senior nursing titles or higher. The team members received unified training that covered theoretical knowledge related to cancer pain, knowledge of analgesic drugs, non-pharmacological treatments for cancer pain, self-management, and the 5A model. The researcher and two head nurses were required to master the use of the scales, follow-up procedures, and other relevant content. The training content was assessed, and those who failed the assessment received further training until they fully mastered the relevant knowledge.
Ask: After the patients underwent pain screening, the head nurse communicated with them to understand their sub
Assess: The Chinese Version of the Self-Management Efficacy Scale for Cancer Patients (C-SUPPH), Research and Treatment of Cancer Quality of Life Questionnaire-Core 30 (EORTC QLQ-C30), and Chinese version of the American Pain Society Patient Outcome Questionnaire (APS-POQ-C) were used to conduct a detailed assessment. The patients’ medication adherence, self-management ability, QoL, and full-course management of cancer pain were analyzed and sorted. Subsequently, team members developed individualized intervention plans for patients based on the assessment results. A pain rating scale and pain recording form were placed at the end of hospital beds, with patients encouraged to score and record their pain every 8 hours. Patients were instructed to report to physicians and nurses as soon as their pain score reached 4 points or higher, so that analgesic measures could be implemented on time. A head nurse was selected as the liaison to communicate with patients at any time. At the beginning of daily treatment, the attending head nurse observed and assessed the patient’s pain, focused on disease reactions, and evaluated changes in pain. During the treatment process, clues were identified through observation and/or inquiries using simple methods.
Advice: During the implementation of the intervention plan, team members solicited patients’ opinions and incorporated reasonable and feasible suggestions. The head nurse queried the patients’ and their family members’ understanding of cancer pain treatment and identified whether they had misunderstandings about pain treatment (e.g., whether patients took drugs on demand or on time, whether they worried about addiction to analgesic drugs, whether they endured pain, whether they only used analgesic drugs when the pain was severe, and whether they worried about adverse drug reactions). Targeted, individualized knowledge education was provided to address misunderstandings regarding cancer pain treatment among patients and their family members. Any incorrect perceptions of patients and their family members regarding pain and analgesic drugs were corrected, and accurate beliefs about pain and related knowledge were established. The patients and their family members were provided with a detailed in-person explanation of cancer pain-related knowledge and pain management methods. On the day after health education, the degree of patients’ and their family members’ understanding of the relevant knowledge was assessed until they had a full understanding, so that they could comprehend the necessity and importance of cancer pain treatment and improve their treatment adherence. Patients were guided and encouraged to actively adopt non-pharmacological pain management measures, such as changing body positions, TCM acupoint stimulation, distraction, cognitive therapy, and relaxation therapy. TCM-specialized nurses guided the patients using the TCM acupoint pressing method. When patients experienced increased pain due to external examinations or other reasons, they were encouraged to communicate with physicians and nurses according to their own conditions and to use analgesic drugs preventively, as prescribed by physicians, to avoid inducing breakthrough pain. Pain education manuals were distributed. Health education on pain was provided to patients once a month. Offline, regular pain lectures were held in the department. Additionally, online, pain-related knowledge was shared twice a week in the WeChat group.
Assist: A WeChat group was established, and patients or their family members were guided to join the group by scanning the appropriate QR code. The group included members of a full-course pain management team, patients experiencing pain, and family members. Patients and their family members were guided to learn the method of reading and sending WeChat messages on mobile phones and were informed on how to utilize the WeChat platform to report their pain management status in a timely manner. The WeChat platform provides health education for patients with cancer pain twice a week, covering content such as prevention and response methods for adverse reactions to opioid analgesic drugs, non-pharmacological pain treatment, and correct understanding of pain. The content was presented in various forms, such as text, pictures, and videos. If the patients had questions, they could ask them directly in the WeChat group or send videos to the group. The nursing staff and attending physicians responded in plain language. The patients were encouraged to express their true thoughts and feelings, correct their negative emotions, and face the disease with a positive attitude. If necessary, private chats or one-on-one video calls were conducted according to the patient’s actual situation to provide individualized health guidance and education. Patients were encouraged to communicate with one another in the group and share their rehabilitation experiences to enhance their confidence in the rehabilitation treatment. Patients or their family members were instructed to follow the hospital’s official WeChat account. The functions and usage methods of each module on the WeChat platform were explained in detail to ensure that users could flexibly master and effectively utilize the platform's resources. Patients and their family members were guided to register appointments and pay fees through the official account and were taught how to query inspection and test reports to shorten the wait time for medical treatment. Patients were guided on the operation method of the home care platform and informed that if they had needs such as catheter maintenance, wound care, or blood glucose monitoring after discharge and found it inconvenient to visit the hospital, they could place an order online to choose home care services. During the intervention, the experience of using the WeChat platform by patients and their family members was continuously tracked and evaluated. A self-designed questionnaire was used to investigate the operative proficiency and patient satisfaction after two weeks of intervention. The results showed that 95% of patients (47/50) could proficiently use the core functions of the WeChat platform (including message reading, pain status reporting, and online consultation), and 8% of patients (4/50) initially had mild operational difficulties (such as QR code scanning and message sending) that were resolved through one-on-one guidance by the nursing team within 3 days. The overall satisfaction rate of patients with the WeChat platform intervention was 92% (46/50), primarily due to the convenience of information acquisition and timely communication with medical staff. No technical failures occurred during the study period that affected the intervention process.
Arrange (follow-up): Before patients were discharged from the hospital, a pain diary was distributed to record, in detail, changes in pain, medication status, and the degree of adverse drug reactions during the patients’ home stay so that accurate information could be provided to medical staff during follow-up. The patients were instructed to complete their pain records on a daily basis. Patients were instructed to take drugs as prescribed by their physicians after discharge, and guidance was provided on how to deal with drug adverse reactions and home life. A follow-up form for discharged patients was formulated.
On days 3, 10, and 17 after discharge, the head nurse was responsible for conducting remote video follow-ups using the WeChat video-call function to gain an intuitive understanding of the patients’ pain manifestations, mental state, and living environment. The follow-up content included pain score, pain intensity, location and nature of pain, drug use status, efficacy, and adverse reactions to analgesic drugs, physical function, and psychological state. Personalized rehabilitation guidance and suggestions were provided according to each patient’s specific condition(s). If necessary, the patients were urged to return for reexamination.
A polite language template for telephone follow-up communication was established, including opening remarks and identity confirmation, care and inquiries about recent status, pain assessment and treatment progress, drug use and adverse reactions, psychological support and emotional assessment, requests for feedback and suggestions, and closing remarks and blessings. For example: Hello! Is this Mr./Ms. XX? This is Nurse XX (name or position), from Ward X of XX Hospital. I hope I did not disturb you”. “Thank you for taking the time to answer our call. The purpose of this follow-up was to understand your recent pain management situation and provide you with the necessary support and help”. “Did you experience any adverse reactions during the drug use process, such as nausea, vomiting, constipation, etc.”?
The head nurse was responsible for the follow-up. The follow-up staff should understand the patient’s condition when discharged from the hospital, communicate gently with the patient, listen carefully to the patient’s statements during follow-up, and answer the patient’s questions. Communication was conducted item by item, following the polite language template used for the telephone follow-up. Patients were reminded to maintain a pain diary that detailed changes in pain, medication status, and the degree of adverse drug reactions during their home stay, so that accurate information could be provided to medical staff during follow-up. Follow-up was conducted once per week for four consecutive weeks. If a patient was readmitted to the hospital within four weeks, the readmission time was recorded in the follow-up time column. Telephone follow-up was conducted between 2:00 PM. and 5:00 PM. The head nurse recorded the follow-up results in the patient’s pain file.
Members of the full-course pain management team receive regular training on pain-related knowledge and skills. At the end of each month, team members conducted work summaries and quality control. During the research design stage, experts were invited to provide guidance, and relevant personnel received thorough training. Standard questionnaires were used, and data were collected by professional investigators. Questionnaires were collected to ensure authenticity and screened for invalid responses. Double data entry was employed during data entry, with repeated verification. The statistical analysis was supervised and guided by experts.
Comparison of NRS scores between the 2 groups: Before and 1 month after the intervention, the NRS (Cronbach’s α = 0.77)[16] was used to measure the pain intensity experienced by patients in the two. The total score ranges from 0 to 10 points and is proportional to the patient's pain intensity. The specific criteria were as follows: No pain, 0 points; mild pain, 1-3 points; moderate pain, 4-6 points; severe pain, 7-9 points; and severe pain, 10 points.
Comparison of EORTC QLQ-C30 scores: Before and 1 month after the intervention, the EORTC QLQ-C30 (Cronbach’s α = 0.648)[17] was used to measure patient QoL in the 2 groups. The scale includes five items: Cognitive, role, emotional, physical, and social. The total score for each item ranged from 0 to 100 points and was proportional to the patient’s QoL.
Comparison of C-SUPPH scores: Before the intervention and 1 month after the intervention, the C-SUPPH (Cronbach’s α = 0.970)[18] was used to assess the self-management efficacy of patients in both groups. It includes three dimensions: Self-stress reduction (10-50 points), positive attitude (15-75 points), and self-decision-making (3-15 points). The total score ranged from 28 to 140 points and was proportional to the patient’s self-efficacy.
Comparison of APS-POQ-C scores: Before and 1 month after the intervention, the APS-POQ-C (Cronbach’s α = 0.735)[19] was used to measure the pain nursing outcomes of patients in both groups. The scale includes 6 dimensions (21 items): Pain intensity, activity interference, sleep interference, emotion, adverse reactions related to pain treatment drugs, and perception of pain management. A 0-10 scoring method was used, and each dimension was scored separately. The average score was considered the final score. Higher scores in the first 5 dimensions indicate worse pain outcomes, while higher scores in the last dimension (perception of pain management) indicate better pain nursing outcomes.
Data were analyzed using SPSS (version 24.0; IBM Corp., Armonk, NY, United States). Quantitative data were expressed as mean ± SD and compared using the t-test, while qualitative data are expressed as the n (%) and compared using the χ2 test. Intergroup comparisons were performed using t-tests, and intragroup comparisons were performed using paired t-tests. Differences with P < 0.05 were considered to be statistically significant.
After 1 month of nursing, the observation group exhibited lower NRS scores than the control group (P < 0.05; Table 2).
Both groups exhibited significant improvements in all items of the EORTC QLQ-C30 scale after one month of treatment (P < 0.05); however, the observation group had higher scores for cognitive, role, emotional, physical, and social functions than the control group (P < 0.05; Table 3).
| Group | n | Cognitive function | Role function | Emotional function | Physical function | Social function | |||||
| Before nursing | After nursing | Before nursing | After nursing | Before nursing | After nursing | Before nursing | After nursing | Before nursing | After nursing | ||
| Control group | 50 | 85.23 ± 6.12 | 91.56 ± 4.34a | 82.12 ± 4.23 | 89.56 ± 4.18a | 68.56 ± 4.89 | 75.12 ± 6.65a | 88.56 ± 6.23 | 92.34 ± 2.89a | 82.85 ± 0.56 | 89.34 ± 4.45a |
| Observation group | 50 | 85.56 ± 6.08 | 95.89 ± 1.67a | 82.34 ± 4.18 | 94.87 ± 3.56a | 68.78 ± 4.92 | 81.45 ± 9.21a | 88.78 ± 6.18 | 97.12 ± 1.45a | 82.92 ± 0.62 | 93.12 ± 3.32a |
| t value | - | 0.27 | 6.584 | 0.262 | 6.839 | 0.224 | 3.94 | 0.177 | 10.453 | 0.592 | 4.814 |
| P value | - | 0.787 | < 0.01 | 0.794 | < 0.01 | 0.823 | < 0.01 | 0.86 | < 0.01 | 0.555 | < 0.01 |
After 1 month of treatment, the increase in C-SUPPH scores in the observation group was greater than that in the control group (P < 0.05; Table 4).
| Group | n | Self-stress reduction | Positive attitude | Self-decision-making | |||
| Before nursing | After nursing | Before nursing | After nursing | Before nursing | After nursing | ||
| Control group | 50 | 37.34 ± 3.12 | 42.56 ± 4.89a | 47.65 ± 3.23 | 62.12 ± 3.89a | 7.77 ± 1.23 | 9.12 ± 1.89a |
| Observation group | 50 | 37.56 ± 3.08 | 46.23 ± 2.45a | 47.45 ± 3.18 | 68.01 ± 4.21a | 7.89 ± 1.18 | 12.34 ± 1.23a |
| t value | - | 0.355 | 4.745 | 0.312 | 7.266 | 0.498 | 10.097 |
| P value | - | 0.724 | < 0.01 | 0.756 | < 0.01 | 0.620 | < 0.01 |
After one month of treatment, the observation group exhibited lower scores for pain intensity, activity interference, sleep interference, emotion, and adverse reactions related to pain treatment drugs on the APS-POQ-C scale, while having a higher score in the perception of pain management than the control group (P < 0.05; Table 5).
| Group | n | Pain intensity | Activity interference | Sleep interference | Emotion | Adverse reactions related to pain treatment drugs | Perception of pain management | ||||||
| Before nursing | After nursing | Before nursing | After nursing | Before nursing | After nursing | Before nursing | After nursing | Before nursing | After nursing | Before nursing | After nursing | ||
| Control group | 50 | 2.23 ± 0.23 | 1.45 ± 0.25a | 7.67 ± 1.23 | 3.92 ± 0.89a | 8.56 ± 2.23 | 4.12 ± 1.05a | 7.23 ± 1.04 | 3.95 ± 1.05a | 7.64 ± 0.23 | 2.97 ± 1.56a | 3.56 ± 0.23 | 6.12 ± 1.85a |
| Observation group | 50 | 2.20 ± 0.22 | 0.18 ± 0.04a | 7.92 ± 1.08 | 2.12 ± 0.56a | 8.78 ± 2.18 | 2.34 ± 0.29a | 7.25 ± 1.03 | 2.08 ± 0.28a | 7.67 ± 0.18 | 1.21 ± 0.09a | 3.60 ± 0.18 | 8.45 ± 1.06a |
| t value | - | 0.667 | 38.47 | 1.08 | 12.104 | 0.499 | 11.555 | 0.097 | 12.168 | 0.726 | 6.539 | 0.968 | 7.727 |
| P value | - | 0.507 | < 0.01 | 0.283 | < 0.01 | 0.619 | < 0.01 | 0.923 | < 0.01 | 0.469 | < 0.01 | 0.335 | < 0.01 |
Patients with middle- and late-stage digestive tract malignancies frequently experience persistent nociception, which not only impairs physiological homeostasis but also exacerbates psychological distress, ultimately compromising treatment adherence and prognosis. The Internet+ integrated 5A nursing model represents an emerging evidence-based nursing paradigm that synthesizes Internet-enabled telehealth technologies using a patient-centered 5A framework (Ask, Assess, Advise, Assist, And Arrange), addressing the inherent limitations of traditional pain management, including fragmented care delivery, delayed intervention responses, and inadequate individualization. The 5A model has been validated for efficacy across diverse disease populations, including interstitial lung disease and primary liver cancer, demonstrating its versatility in improving rehabilitation outcomes and modulating disease-related pathophysiological processes[20,21]. The study findings are interpreted below by contextualizing them within theoretical frameworks, elucidating the mechanistic links between intervention components and outcome metrics, and conducting critical comparisons with the existing literature to underscore the model’s scientific novelty and clinical relevance.
In the present study, the observation group exhibited a substantial reduction in NRS scores from 2.20 ± 0.22 at baseline to 0.18 ± 0.04 post-intervention, representing a 91.8% relative decrease, which was significantly superior to the control group’s 35.0% reduction (from 2.23 ± 0.23 to 1.45 ± 0.25; P < 0.001). This analgesic effect may stems from the synergistic interplay of three core intervention mechanisms inherent to the Internet+ 5A model: First, the “Assist” module established a patient-reported outcome-driven real-time communication platform via WeChat, enabling bidirectional transmission of pain-related data (e.g., breakthrough pain episodes, medication side effects) and facilitating nurse-led triage within 60 minutes. This aligns with the findings of Gao et al[22], who reported that Internet-based continuous nursing significantly improved pain control in elderly patients with advanced malignant tumors by overcoming time-space barriers. In collaboration with oncologists, the team implemented preemptive analgesic adjustments, such as optimizing rescue medication timing prior to diagnostic procedures to mitigate procedural pain and aligning with the World Health Organization ladder of cancer pain management. The 5A model may enhance holistic care outcomes in patients with cancer. Secondly, the “Arrange” module’s structured follow-up protocol—incorporating remote video assessments on post-discharge days 3, 10, and 17, supplemented by weekly telephone follow-up—addressed the time-space constraints of traditional outpatient follow-up. This intensive monitoring is similar to that validated by Basch et al[23] in patients with severe adrenal tumors, enabling the early identification of pain precipitants (e.g., non-adherence to analgesic regimens, diet-induced visceral irritation) and timely intervention, thereby preventing the progression from mild to moderate to severe nociception.
Both cohorts exhibited significant improvements in all dimensions of the EORTC QLQ-C30 after one month of intervention (P < 0.05). However, the observation group achieved superior scores in cognitive, role, emotional, physical, and social functions (P < 0.001). This multidimensional enhancement reflects the model’s alignment with holistic person-centered care, as psychological resilience, social support, and symptom cluster management are closely intertwined with health-related QoL (HRQoL) in patients with digestive tract tumors[24]. (1) Cognitive function: Reduced nociceptive input alleviates the cognitive load associated with persistent pain, while disease-specific health education enhances health literacy, addressing the cognitive burden of fear of cancer recurrence, a key psychological stressor in this population; (2) Role function: Pain relief enables patients to resume instrumental activities of daily living, supported by digestive tract function protection strategies analogous to those validated in patients with gastric cancer; (3) Emotional function: Targeted psychological support delivered by certified counselors via one-on-one video sessions mitigates anxiety and depression. Peer support within WeChat groups fosters social connectedness; (4) Physical function: The combination of optimized pharmacotherapy, non-pharmacological interventions (e.g., progressive muscle relaxation), and improved adherence reduced pain-related fatigue, mirroring the physical function improvements reported in patients with thyroid eye disease receiving Internet+ nursing; and (5) Social function: Telehealth-enabled access to care reduces the healthcare-related burden, while peer interaction diminishes social isolation, a critical contributor to HRQoL, as emphasized in studies of care transitions in oncology.
The observation group also demonstrated significantly greater improvements in the C-SUPPH across all dimensions (self-stress reduction, positive attitude, and self-decision-making; P < 0.001), indicating enhanced patient empowerment. This outcome is consistent with cross-disease evidence that the 5A model strengthens self-management efficacy from polycystic ovary syndrome to gestational diabetes mellitus[25]—by integrating baseline needs assessment, tailored skill training, and continuous feedback. The “Ask” module’s comprehensive baseline assessment identified individual barriers to self-management, while the “Advise” module provided targeted training in pain self-assessment and management of adverse reactions. The “Assist” module’s continuous telehealth support, as validated in systematic reviews of Internet-based interventions[26], allowed patients to apply these skills in real-world settings, reinforcing self-efficacy through mastery experiences—an essential component of self-determination theory. Furthermore, the model’s (precision) care delivery aligns with the effectiveness of big data-driven nursing for patients with digestive tract tumors[27], emphasizing the value of an individualized intervention design.
In addition to the core dimensions of QoL, self-management efficacy, and pain care-specific outcomes, which are the focus of this study, significant improvements were also achieved. Mechanistic analysis of improvements in self-management efficacy (C-SUPPH) and APS-POQ-C. The results of this study showed that the improvement of the observation group on the C-SUPPH and its various dimensions (stress reduction, positive attitude, and self-determination) was significantly better than that of the control group. This effect stems directly from the interlocking em
Regarding the APS-POQ-C, the observation group exhibited lower scores for pain intensity, activity interference, sleep interference, emotional distress, and analgesic-related adverse reactions and higher scores for pain management satis
Despite these strengths, this study has several limitations. First, the single-center design and relatively small sample size (n = 100) may have limited the generalizability of the findings. Future multicenter studies incorporating diverse geographic regions and healthcare settings are warranted to validate the applicability of this model across heterogeneous populations. Second, the 1-month follow-up period was insufficient to evaluate the long-term efficacy, as pain management in advanced digestive tract cancer is a chronic process that requires sustained intervention. Future studies should extend the follow-up duration to 6-12 months to assess pain recurrence, long-term adherence, and sustained improvements in HRQoL, which is consistent with the long-term focus of the 5A model interventions in other disease contexts. Third, subgroup analyses (e.g., by age, tumor type, and baseline pain intensity) were not performed to identify the populations most likely to benefit from the model.
In conclusion, the Internet+ 5A nursing model not only effectively reduced pain intensity in patients experiencing middle- and late-stage digestive tract tumors pain, improved enhanced QoL, but also strengthened their self-management efficacy and optimized pain nursing outcomes.
| 1. | Cheville AL, Alberts SR, Rummans TA, Basford JR, Lapid MI, Sloan JA, Satele DV, Clark MM. Improving Adherence to Cancer Treatment by Addressing Quality of Life in Patients With Advanced Gastrointestinal Cancers. J Pain Symptom Manage. 2015;50:321-327. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 44] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 2. | Henson LA, Maddocks M, Evans C, Davidson M, Hicks S, Higginson IJ. Palliative Care and the Management of Common Distressing Symptoms in Advanced Cancer: Pain, Breathlessness, Nausea and Vomiting, and Fatigue. J Clin Oncol. 2020;38:905-914. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 302] [Cited by in RCA: 232] [Article Influence: 38.7] [Reference Citation Analysis (0)] |
| 3. | Xu Y, Yang J. The effect of 5A nursing combined with psychological nursing on the immune function, cancer-related fatigue and complications of patients undergoing radical resection of colorectal cancer. Cell Mol Biol (Noisy-le-grand). 2022;68:169-176. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 10] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 4. | Xu L, Zhou MZ. Effect of internet multiple linkage mode-based extended care combined with in-hospital comfort care on colorectal cancer patients undergoing colostomy. World J Gastrointest Surg. 2023;15:1959-1968. [PubMed] [DOI] [Full Text] |
| 5. | Manzano A, Ziegler L, Bennett M. Exploring interference from analgesia in patients with cancer pain: a longitudinal qualitative study. J Clin Nurs. 2014;23:1877-1888. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 20] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 6. | You E. Nontraditional and Home-Based Self-management Interventions in Cancer Patients With Pain: A Mixed-Method Systematic Review. Holist Nurs Pract. 2020;34:138-149. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 6] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 7. | Fallon M, Giusti R, Aielli F, Hoskin P, Rolke R, Sharma M, Ripamonti CI; ESMO Guidelines Committee. Management of cancer pain in adult patients: ESMO Clinical Practice Guidelines. Ann Oncol. 2018;29:iv166-iv191. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 721] [Cited by in RCA: 583] [Article Influence: 72.9] [Reference Citation Analysis (0)] |
| 8. | Steel JL, Geller DA, Kim KH, Butterfield LH, Spring M, Grady J, Sun W, Marsh W, Antoni M, Dew MA, Helgeson V, Schulz R, Tsung A. Web-based collaborative care intervention to manage cancer-related symptoms in the palliative care setting. Cancer. 2016;122:1270-1282. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 107] [Cited by in RCA: 97] [Article Influence: 9.7] [Reference Citation Analysis (0)] |
| 9. | Kwok C, Degen C, Moradi N, Stacey D. Nurse-led telehealth interventions for symptom management in patients with cancer receiving systemic or radiation therapy: a systematic review and meta-analysis. Support Care Cancer. 2022;30:7119-7132. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 38] [Cited by in RCA: 33] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 10. | Moradian S, Voelker N, Brown C, Liu G, Howell D. Effectiveness of Internet-based interventions in managing chemotherapy-related symptoms in patients with cancer: a systematic literature review. Support Care Cancer. 2018;26:361-374. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 45] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 11. | Oldenmenger WH, Baan MAG, van der Rijt CCD. Development and feasibility of a web application to monitor patients' cancer-related pain. Support Care Cancer. 2018;26:635-642. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 32] [Cited by in RCA: 24] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 12. | Agboola SO, Ju W, Elfiky A, Kvedar JC, Jethwani K. The effect of technology-based interventions on pain, depression, and quality of life in patients with cancer: a systematic review of randomized controlled trials. J Med Internet Res. 2015;17:e65. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 129] [Cited by in RCA: 101] [Article Influence: 9.2] [Reference Citation Analysis (0)] |
| 13. | Ito A, Yoshida S, Hosokawa M, Hirayama H, Sasaki K, Miyashita M. A systematic review of randomized controlled trials on telecommunication technologies for pain management in patients with advanced cancer: incorporating electronic patient-reported outcomes (ePROs). Ann Palliat Med. 2025;14:579-591. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 14. | Dastafkan E, Khaledi B, Salari N, Visi-Rayegani A, Abdi A. The effect of the 5A Self-Management Model approach on sleep quality of patients with cancer. Int J Palliat Nurs. 2025;31:173-180. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 15. | Zhang X, Lai M, Wu D, Luo P, Fu S. The Effect of 5A nursing intervention on living quality and self-care efficacy of patients undergoing chemotherapy after hepatocellular carcinoma surgery. Am J Transl Res. 2021;13:6638-6645. [PubMed] |
| 16. | Stijic M, Messerer B, Meißner W, Avian A. Numeric rating scale for pain should be used in an ordinal but not interval manner. A retrospective analysis of 346,892 patient reports of the quality improvement in postoperative pain treatment registry. Pain. 2024;165:707-714. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 17. | Greimel ER, Kuljanic Vlasic K, Waldenstrom AC, Duric VM, Jensen PT, Singer S, Chie W, Nordin A, Bjelic Radisic V, Wydra D; European Organization for Research and Treatment of Cancer Quality-of-Life Group. The European Organization for Research and Treatment of Cancer (EORTC) Quality-of-Life questionnaire cervical cancer module: EORTC QLQ-CX24. Cancer. 2006;107:1812-1822. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 260] [Cited by in RCA: 232] [Article Influence: 11.6] [Reference Citation Analysis (0)] |
| 18. | Qian HJ, Yuan CR. [The reliability and validity of Chinese version of Strategies Used by People to Promote Health]. Zhonghua Huli Zazhi. 2011;46:3. [DOI] [Full Text] |
| 19. | Yu WH, Yang H, Lu YH, MaXX. [Cross-cultural adaptation of the American Pain Society Patient Outcome Questionnaire and evaluation of its reliability and validity in cancer pain patients]. Zhongguo Shiyong Huli Zazhi. 2020;36:331-336. [DOI] [Full Text] |
| 20. | Li M, Chang Y, Fan J, Liang B, Qu D. Effects of a 10-week pulmonary rehabilitation program based on the 5A nursing model in patients with interstitial lung disease: a quasi-experimental study. BMC Nurs. 2025;24:591. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 21. | Su X, Li X, Zhang J, Fang H, Zhang L, He L. Impact of the 5A nursing model on immune balance and lymph node metastasis in primary liver cancer patients post-CyberKnife treatment. BMC Cancer. 2025;25:1024. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 22. | Gao P, Zhao M, Cao J, Bai J. The impact of internet multidisciplinary continuity care on the living quality of home-based patients with malignant tumors undergoing PICC catheterization. Am J Transl Res. 2024;16:4001-4010. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 23. | Basch E, Deal AM, Dueck AC, Scher HI, Kris MG, Hudis C, Schrag D. Overall Survival Results of a Trial Assessing Patient-Reported Outcomes for Symptom Monitoring During Routine Cancer Treatment. JAMA. 2017;318:197-198. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1930] [Cited by in RCA: 1685] [Article Influence: 187.2] [Reference Citation Analysis (0)] |
| 24. | Sihvola S, Kuosmanen L, Kvist T. Resilience and related factors in colorectal cancer patients: A systematic review. Eur J Oncol Nurs. 2022;56:102079. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 58] [Article Influence: 14.5] [Reference Citation Analysis (0)] |
| 25. | Rokni S, Rezaei Z, Noghabi AD, Sajjadi M, Mohammadpour A. Evaluation of the effects of diabetes self-management education based on 5A model on the quality of life and blood glucose of women with gestational diabetes mellitus: an experimental study in eastern Iran. J Prev Med Hyg. 2022;63:E442-E447. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 26. | Huang Y, Li Q, Zhou F, Song J. Effectiveness of internet-based support interventions on patients with breast cancer: a systematic review and narrative synthesis. BMJ Open. 2022;12:e057664. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 29] [Cited by in RCA: 26] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 27. | Healthcare Engineering JO. Retracted: Application Effect Analysis of Operating Room Detailed Nursing Based on Medical Big Data in Patients Undergoing Gastrointestinal Tumor Surgery. J Healthc Eng. 2023;2023:9864567. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 28. | Bennett B, Gardner L, Ryan P. Peptide Receptor Radionuclide Therapy Using 177Lu-DOTATATE: Nursing Roles in Managing Patients With Gastroenteropancreatic Neuroendocrine Tumors. Clin J Oncol Nurs. 2024;28:79-87. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 29. | Liu T, Xu J, Cheng H, Zhang Y, Wang S, Lin L, Tian L. Effects of internet-based cognitive behavioral therapy on anxiety and depression symptoms in cancer patients: A meta-analysis. Gen Hosp Psychiatry. 2022;79:135-145. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 25] [Article Influence: 6.3] [Reference Citation Analysis (0)] |