Copyright: ©Author(s) 2026.
World J Gastrointest Endosc. Apr 16, 2026; 18(4): 117233
Published online Apr 16, 2026. doi: 10.4253/wjge.v18.i4.117233
Published online Apr 16, 2026. doi: 10.4253/wjge.v18.i4.117233
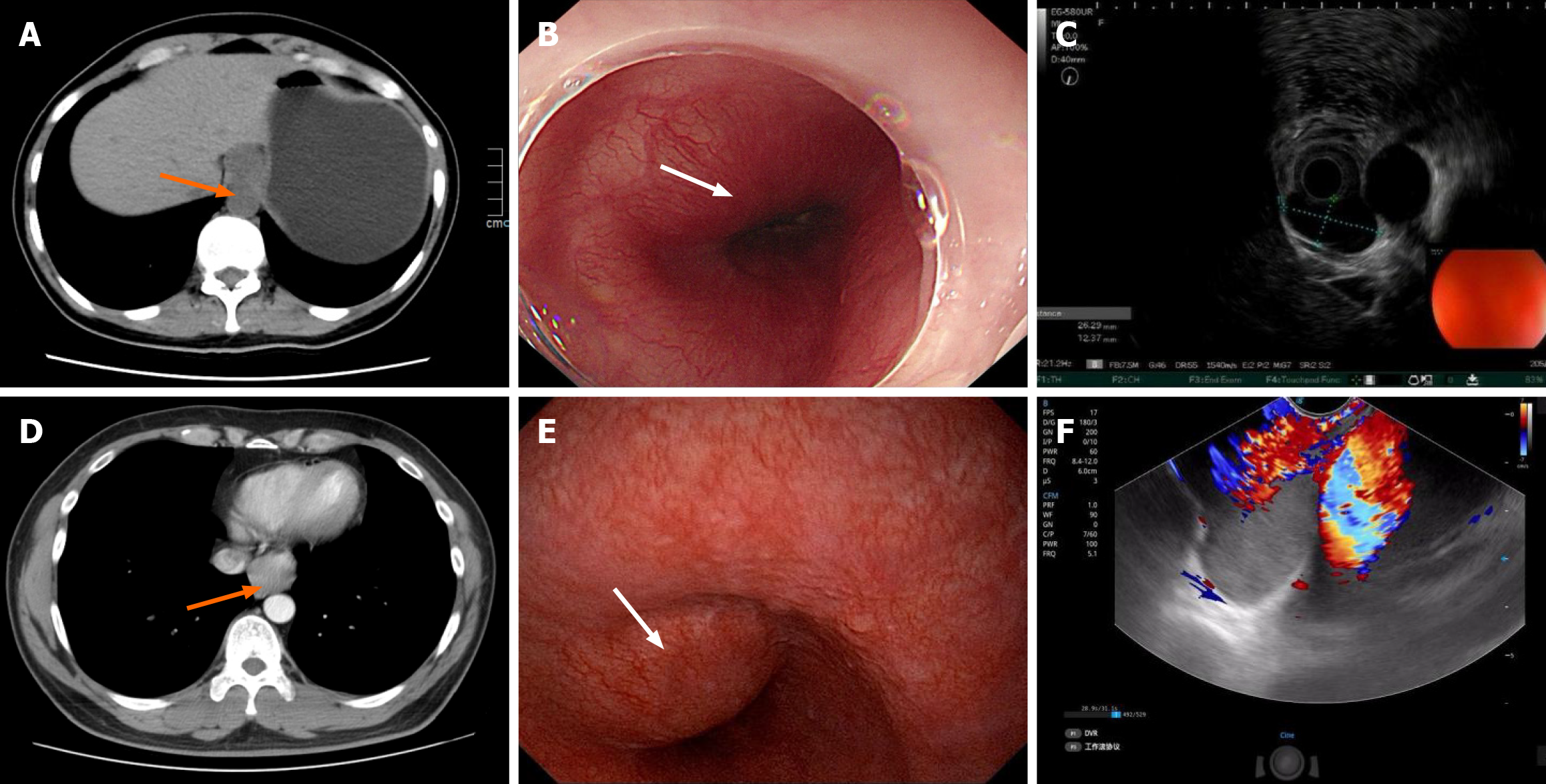
Figure 1 Preoperative imaging and endoscopic findings.
A: Computed tomography shows a well-circumscribed, low-density mass at the gastroesophageal junction (case 1) (arrow indicate the lesions); B: Endoscopy reveals a smooth submucosal bulge 35 cm from the incisors (case 1) (arrow indicate the lesions); C: Endoscopic ultrasonography demonstrates a hypoechoic, irregularly shaped lesion arising from the muscularis propria with clear margins (case 1); D: Contrast-enhanced computed tomography shows a mass adjacent to the gastroesophageal junction with mild enhancement and luminal narrowing (case 2) (arrow indicate the lesions); E: Endoscopy revealing a smooth, intact submucosal bulge 38 cm from the incisors (case 2) (arrow indicate the lesions); F: Endoscopic ultrasonography showing a hypoechoic lesion originating from the muscularis propria, with no vascular signal on color Doppler flow imaging and intermediate stiffness on elastography (case 2).
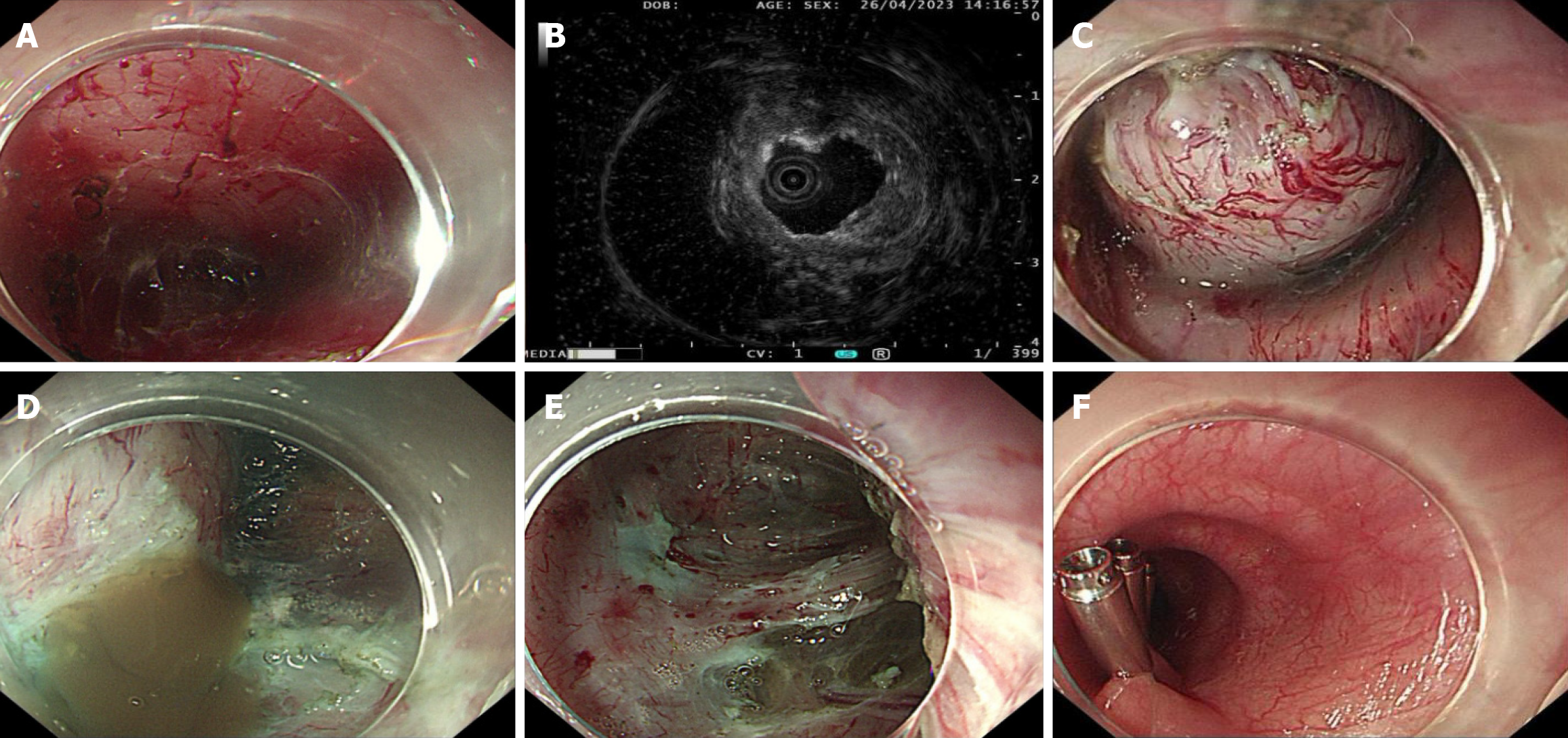
Figure 2 Intraoperative findings during mediastinal bronchogenic cyst resection (case 1).
A: Creation of the submucosal tunnel; no lesion was observed within the submucosal layer; B: Intraoperative endoscopic ultrasonography confirmed the presence of the lesion; C: Full-thickness myotomy and careful dissection of the muscularis propria exposed the cyst; D: Yellowish gelatinous fluid was released from the cyst cavity; E: Surgical field following cyst removal; F: Mucosal entry site securely closed with endoscopic clips.
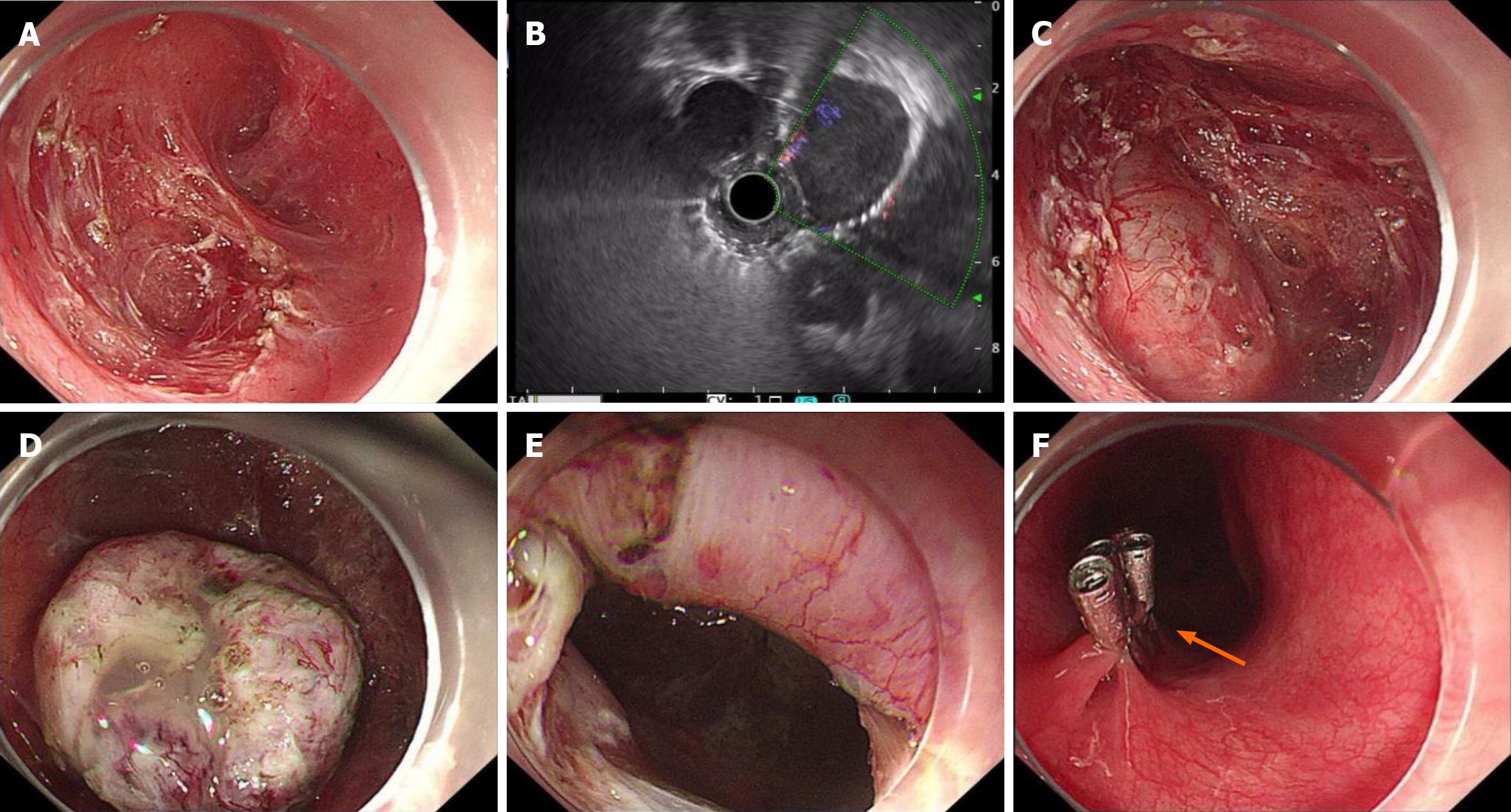
Figure 3 Intraoperative findings during mediastinal bronchogenic cyst resection (case 2).
A: Creation of a submucosal tunnel; no lesion was visible within the submucosal layer; B: Intraoperative endoscopic ultrasonography confirmed the presence of the cyst; C: The cyst wall was exposed following full-thickness myotomy and careful dissection of the muscularis propria; D: The cyst was thin-walled and fragile, containing yellow gelatinous fluid; E: Surgical cavity after complete cyst removal; F: Mucosal entry site securely closed with multiple endoscopic clips (arrow indicates the mucosal entry site).
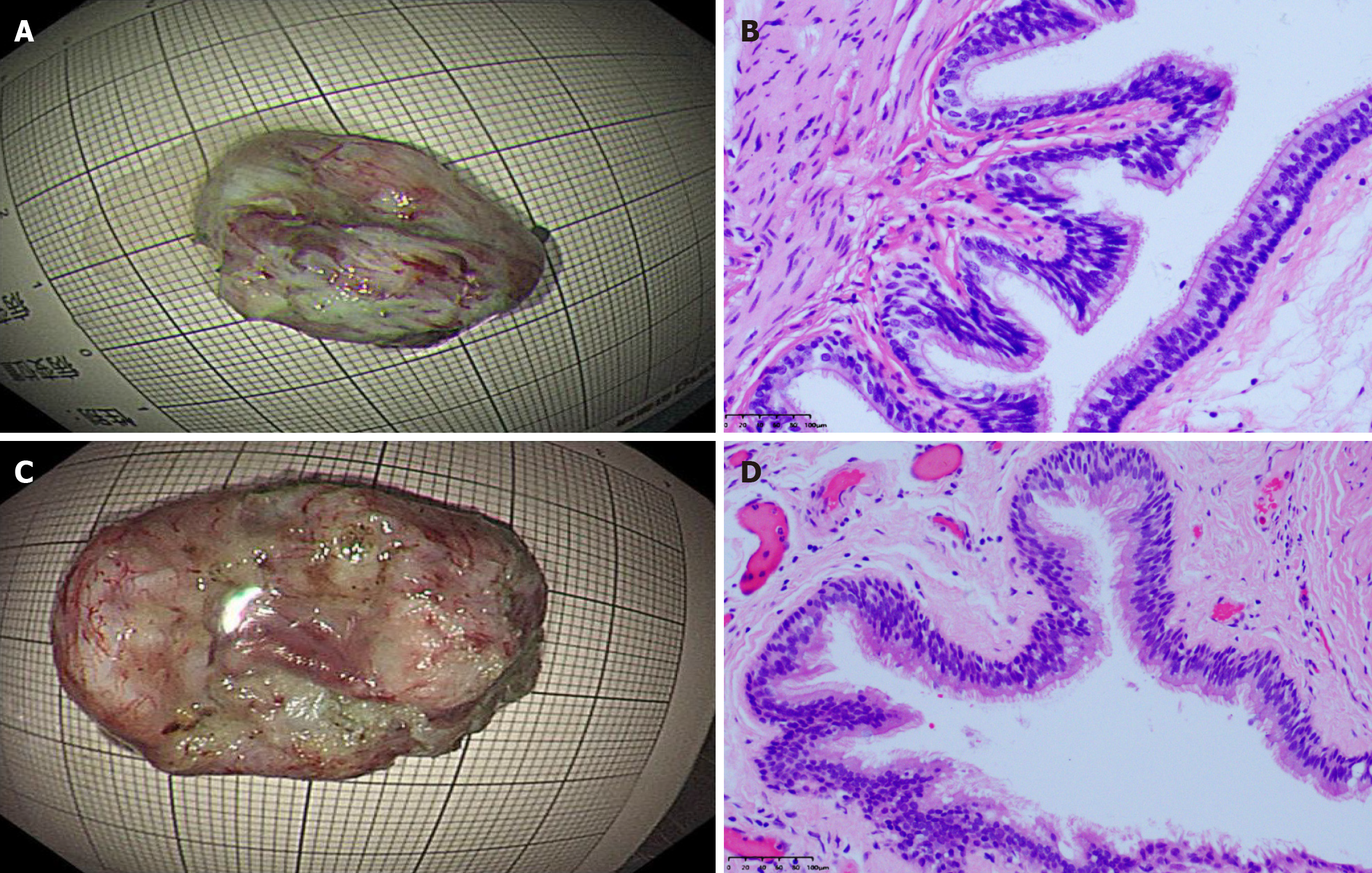
Figure 4 Gross specimens and histopathological findings of the two cases.
A: Resected cystic lesions from case 1; B: Histological examination revealed a cyst wall lined with pseudostratified ciliated columnar epithelium, consistent with a bronchogenic cyst (case 1); C: Resected cystic lesions from case 2; D: Histological examination revealed pseudostratified ciliated columnar epithelium with underlying smooth muscle and fibrous tissue, further supporting the diagnosis of a bronchogenic cyst (case 2).
- Citation: Ma JM, Ji CG, Liu L, Yin KG. Bronchogenic cysts treated with submucosal tunneling endoscopic resection and natural orifice transluminal endoscopy: Two case reports and review of literature. World J Gastrointest Endosc 2026; 18(4): 117233
- URL: https://www.wjgnet.com/1948-5190/full/v18/i4/117233.htm
- DOI: https://dx.doi.org/10.4253/wjge.v18.i4.117233