Published online Apr 16, 2026. doi: 10.4253/wjge.v18.i4.117389
Revised: December 25, 2025
Accepted: January 28, 2026
Published online: April 16, 2026
Processing time: 128 Days and 19.2 Hours
While laparoscopic cholecystectomy (LC) is the gold standard procedure for sy
To compare the cosmetic, operative, and clinical outcomes of MTP, SP, and TP LC.
This retrospective cohort study included 142 patients with symptomatic gal
All procedures were completed laparoscopically. MTP LC demonstrated the shor
MTP LC balances the cosmetic benefit of SP LC with the efficiency and safety of TP technique, though its generalizability requires prospective validation.
Core Tip: This retrospective cohort study compares modified two-port (MTP), single-port (SP), and three-port (TP) laparoscopic cholecystectomy (LC) to determine the optimal balance between invasiveness, efficiency, safety, and cosmetic outcomes. MTP LC demonstrated the shortest operative and recovery times, no complications, and excellent scar con
- Citation: Hawanga GD, Zhang XL, Li ZX, Li MX, Pan J, Wang KM, Qian DH. Clinical outcomes of single-port, modified two-port, and three-port laparoscopic cholecystectomy: A comparative retrospective cohort study. World J Gastrointest Endosc 2026; 18(4): 117389
- URL: https://www.wjgnet.com/1948-5190/full/v18/i4/117389.htm
- DOI: https://dx.doi.org/10.4253/wjge.v18.i4.117389
Laparoscopic cholecystectomy (LC) is universally considered the best-practice approach for managing gallbladder pathologies such as cholecystitis and cholelithiasis, owing to its minimally invasive nature, reduced postoperative pain, and rapid recovery[1-3]. In recent years, the focus of surgical innovation has shifted toward further reduction in invasiveness to address patient demands for improved cosmetic outcomes and faster return to daily activities[2,3]. Although three-port (TP) LC is well established as a safe and effective technique, reduced-port approaches—including single-port (SP) and modified two-port (MTP) LC—have gained increasing attention for their potential to minimize incision numbers and sizes[2-4].
These reduced-port techniques aim to reduce tissue trauma, alleviate postoperative pain, and enhance scar aesthetics[5]. However, SP LC is associated with technical challenges, including compromised instrument triangulation, ergonomic difficulties, and the need for specialized instruments, which may prolong operative time and increase complication risks[6-9]. While previous studies have compared two of these approaches (e.g., SP vs TP), few have systematically evaluated MTP, SP, and TP LC in a single cohort to clarify their relative advantages[10,11]. A critical knowledge gap exists: Whether MTP LC can integrate the superior cosmesis of SP LC with the proven efficiency and safety of TP LC, as existing evidence on MTP LC is limited and lacks rigorous comparative analysis.
This study addresses this gap by conducting a comprehensive retrospective cohort analysis of 142 patients who underwent MTP, SP, or TP LC. We hypothesized that MTP LC would achieve SP-LC-like cosmetic outcomes while maintaining TP-LC-like operative efficiency and safety[12]. The primary objective was to compare scar visibility among the three approaches, with secondary endpoints including operative duration, intraoperative blood loss, hospital stay, and postoperative complications. The findings will provide evidence-based guidance for surgical decision-making in symptomatic gallbladder disease.
A total of 142 patients (age 17-84 years) diagnosed with symptomatic gallbladder pathologies (e.g., gallstones, polyps, chronic cholecystitis, gallbladder atrophy, adenomyosis, or gallstone entrapment) were enrolled from the Second Department of Hepatobiliary Surgery, First Affiliated Hospital of Wannan Medical College, from January 2024 to January 2025.
Inclusion criteria: (1) Age 17-84 years; (2) Body mass index (BMI) < 40 kg/m2; (3) Preoperative diagnosis of symptomatic gallstones, gallbladder polyps, gallstones with chronic cholecystitis, gallbladder atrophy, gallbladder adenomyosis, or gallstone entrapment; and (4) Provision of written informed consent and agreement to adhere with the study protocol.
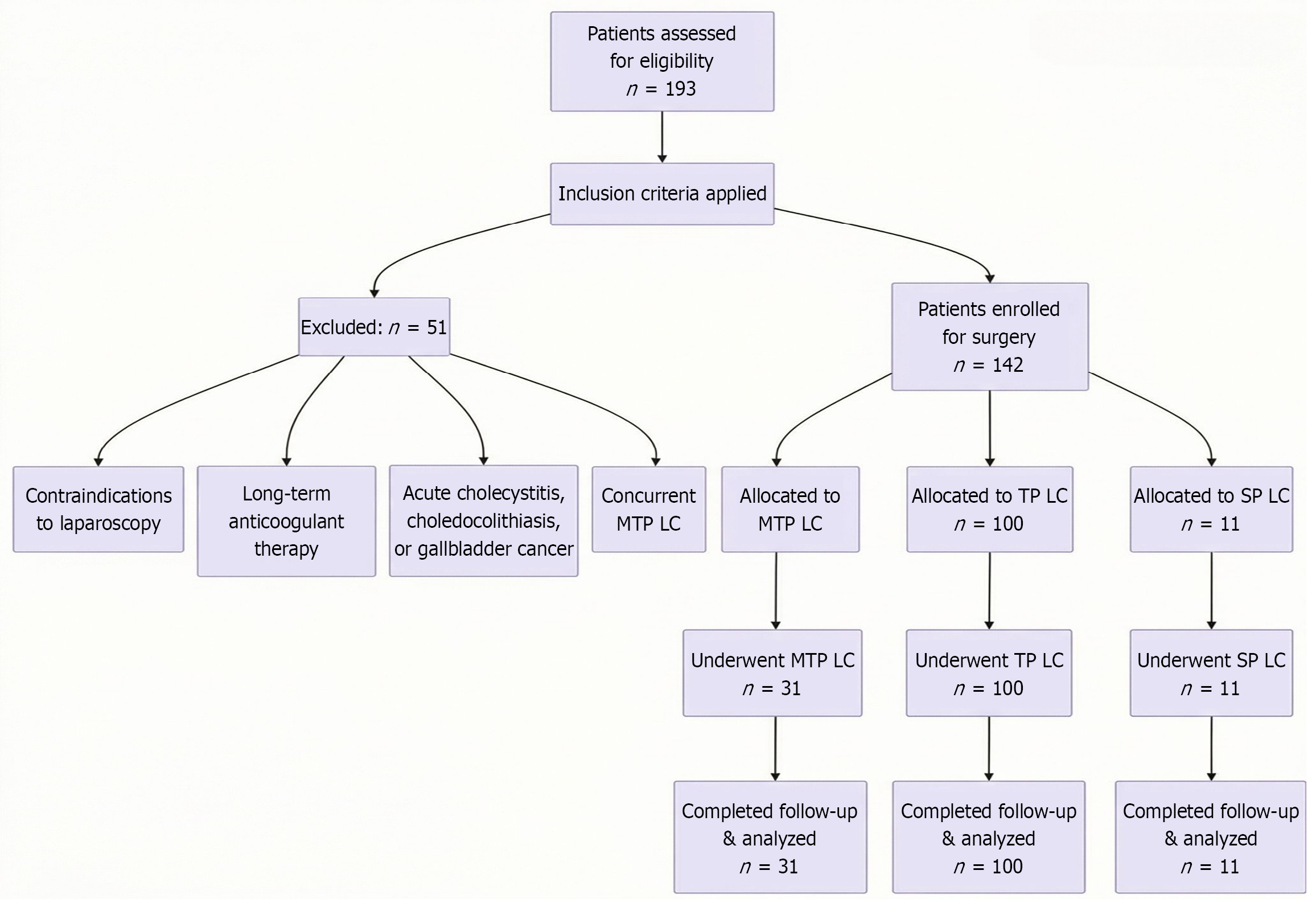
Exclusion criteria: (1) Contraindications to laparoscopy; (2) Long-term anticoagulant therapy; (3) Diagnosis of acute cholecystitis, choledocholithiasis, or gallbladder cancer; and (4) Concurrent liver cysts, liver tumors, or abdominal hernias requiring repair. The patient selection process is summarized in Figure 1.
All patients underwent routine preoperative evaluations, including blood tests (complete blood count, liver function, and albumin measurement), electrocardiography, abdominal ultrasound, and chest X-ray.
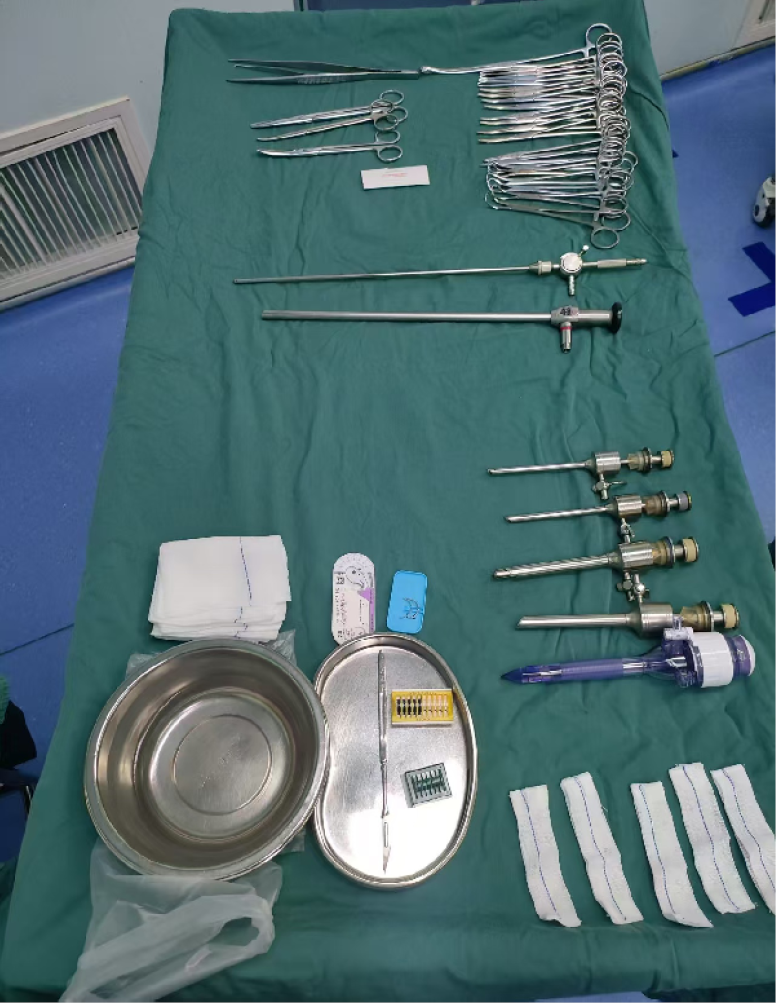
Patients were placed in the supine position to allow intravenous access, induction of general anesthesia, and subsequent endotracheal intubation. The surgical instruments are shown in Figure 2. All procedures were performed by a single consultant surgeon experienced in all the three techniques (> 600 LCs performed).
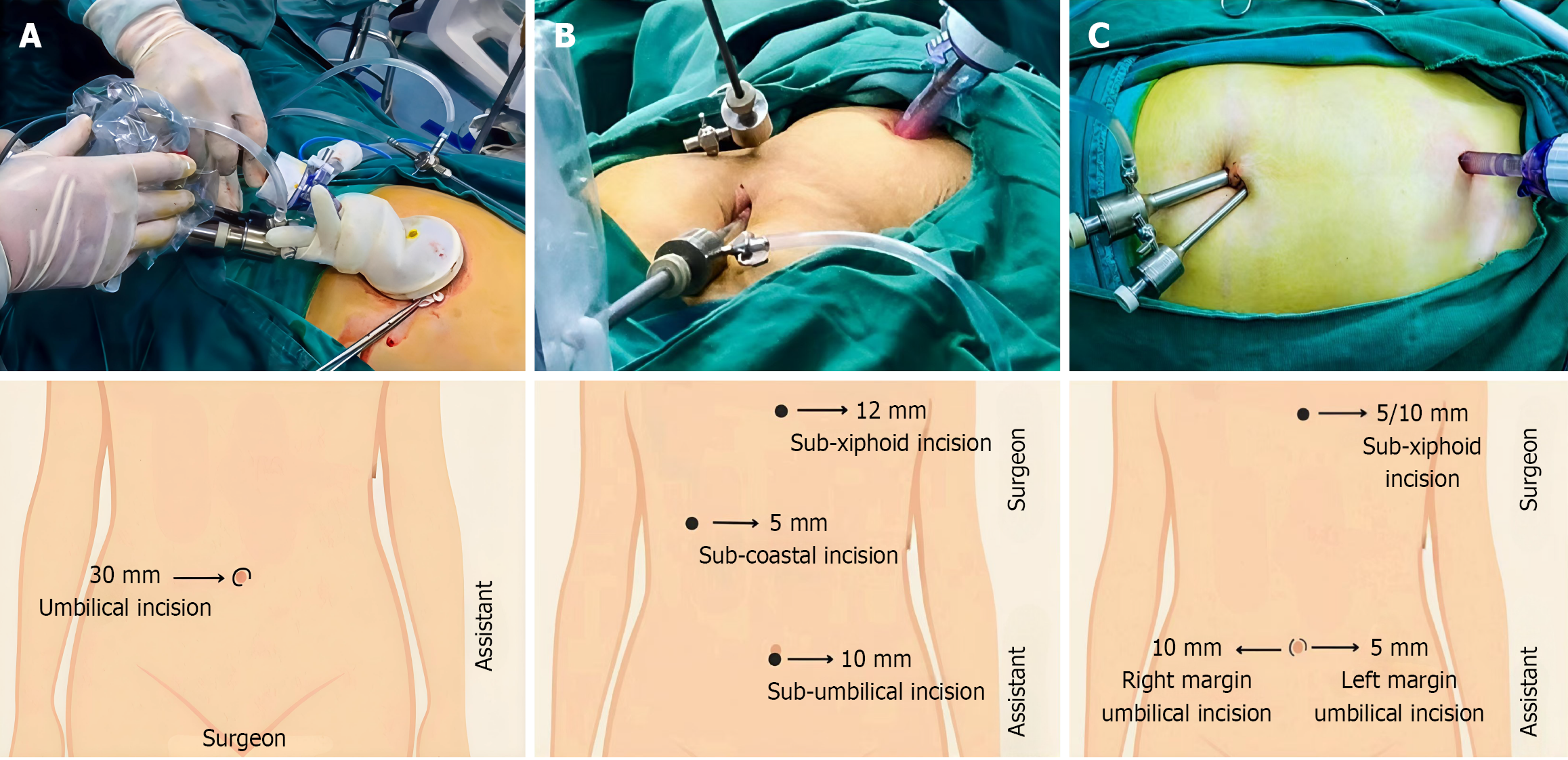
SP LC: The operating surgeon stood between the patient’s legs, and the assistant (laparoscope handler) stood on the patient’s left side. A single bracket-shaped incision (25-30 mm) was made along the inner margin of the umbilicus. A SP access device was placed, through which a laparoscope, grasper, and electrocautery hook were introduced (Figure 3A).
TP LC: The operating surgeon and assistant both stood on the patient’s left side. Incisions included a subumbilical incision (10 mm trocar for laparoscope), sub-xiphoid incision (10 mm trocar for electrocautery hook), and right subcostal incision (5 mm trocar for grasper) (Figure 3B).
MTP LC: This technique utilizes three incisions but functions as a clustered approach to minimize visible scarring and fascial trauma. The surgeon and assistant both stood on the patient’s left side. Incisions included a right inner marginal umbilical incision (10 mm trocar for laparoscope), left inner marginal umbilical incision (5 mm trocar for grasper), and a sub-xiphoid incision (5 mm or 10 mm trocar for electrocautery hook) (Figure 3C). All incisions are concealed within natural body folds, reducing cosmetic impact.
For all groups, fascial defects ≥ 10 mm were closed with 0-vicryl figure-of-eight sutures. Skin closure was performed with 4-0 monocryl subcuticular sutures.
Primary outcome: Cosmetic satisfaction was assessed via a standardized telephone interview at one month postoperatively by a trained research nurse blinded to the surgical technique. Patients rated their scar appearance on a 10-point scale (1 = highly visible, raised, or discolored; 10 = nearly invisible). Scores 8-10 were categorized as “excellent/minimally visible”, and 1-7 as “visible/acceptable”. While a validated scale (e.g., Patient and Observer Scar Assessment Scale) was not used due to retrospective constraints, the standardized 10-point scale was piloted in 10 preliminary patients to ensure consistency.
Secondary outcomes: Operative time (recorded from skin incision to closure), intraoperative blood loss (estimated by the surgeon and anaesthetist), length of hospital stay (from surgery to discharge eligibility), postoperative complications (e.g., infection, bleeding, and bile leak), and postoperative pain (assessed via a Verbal Numerical Rating Scale, 0-10 at 24 hours and 48 hours postoperatively; data were extracted from electronic medical records where available).
Data were analyzed using IBM SPSS Statistics for Windows, version 27.0. Continuous variables, presented as the mean ± SD with 95% confidence intervals (CIs), were compared using the one-way analysis of variance. Categorical variables, presented as frequencies and percentages with 95%CIs, were compared using the χ2 test or Fisher’s exact test (for small cell sizes). P < 0.05 was considered statistically significant. The study was reported in accordance with the Strengthening the Reporting of Observational Studies in Epidemiology guidelines[13].
Patient demographics and preoperative parameters are summarized in Table 1. All 142 procedures were completed laparoscopically without conversion to open surgery. The cohort comprised 93 females (65.5%) and 49 males (34.5%). Gender distribution differed significantly: The SP group had no male patients, whereas the MTP and TP groups included 9 (29.1%) and 40 (40%) males, respectively (P < 0.05)[14]. The mean age was 45.8 ± 16.2 years (MTP), 53.3 ± 11.3 years (TP), and 40.5 ± 12.4 years (SP), with significant differences between MTP and TP (P = 0.005) and between TP and SP (P = 0.001). The SP group had a significantly lower mean BMI (22.3 ± 2.1 kg/m2) compared to the MTP group (24.8 ± 2.9 kg/m2, P = 0.012). These baseline imbalances (younger age, lower BMI, and exclusive female enrollment in the SP group) are acknowledged as potential selection bias. No significant differences were observed in white blood cell count, liver function (aspartate transaminase and alanine transaminase), albumin levels, comorbidities (diabetes and hypertension), or prior abdominal surgery among the three groups.
| Index | MTP (n = 31) | TP (n = 100) | SP (n = 11) | P value (MTP vs TP) | P value (MTP vs SP) | P value (TP vs SP) |
| Age (years) | 48.5 ± 16.2 (42.7-54.3) | 53.3 ± 11.3 (51.0-55.6) | 40.5 ± 12.4 (33.4-47.6) | 0.005 | 0.322 | 0.001 |
| Gender | ||||||
| Male | 9 (29.1) | 40 (40.0) | 0 (0.0) | 0.270 | 0.044 | 0.009 |
| Female | 22 (70.9) | 60 (60.0) | 11 (100.0) | |||
| BMI (kg/m2) | 24.8 ± 2.9 (23.8-25.8) | 24.6 ± 3.3 (24.0-25.2) | 22.3 ± 2.1 (20.9-23.7) | 0.749 | 0.012 | 0.280 |
| WBC (× 109/L) | 5.9 ± 1.6 (5.4-6.4) | 5.8 ± 1.7 (5.5-6.1) | 5.2 ± 1.5 (4.3-6.1) | 0.813 | 0.199 | 0.232 |
| AST (U/L) | 36.5 ± 48.4 (20.1-52.9) | 44.9 ± 100 (25.1-64.7) | 20.3 ± 10.0 (14.0-26.6) | 0.653 | 0.281 | 0.420 |
| ALT (U/L) | 26.6 ± 15.4 (21.5-31.7) | 34.9 ± 54.9 (24.1-45.7) | 25.5 ± 8.2 (20.3-30.5) | 0.408 | 0.825 | 0.573 |
| ALB (U/L) | 45.6 ± 3.7 (44.4-46.8) | 44.6 ± 3.5 (44.0-45.2) | 43.9 ± 4.3 (41.0-46.8) | 0.150 | 0.203 | 0.537 |
| Comorbidities | ||||||
| Diabetes | 0 (0.0) | 3 (3.0) | 0 (0.0) | 0.632 | 0.772 | 1.000 |
| Hypertension | 3 (9.7) | 11 (11.0) | 0 (0.0) | |||
| None | 28 (90.3) | 86 (86.0) | 11 (100.0) | |||
| Prior abdominal surgery | ||||||
| Yes | 12 (38.7) | 40 (40.0) | 5 (45.5) | 0.795 | 0.473 | 0.974 |
| No | 19 (61.3) | 60 (60.0) | 6 (54.5) |
Intraoperative outcomes are detailed in Table 2. SP LC had a significantly longer operative time (103.1 ± 34.9 minutes; 95%CI: 82.3-123.9) compared to both MTP (52.5 ± 19.5 minutes; 95%CI: 45.8-59.2, P < 0.01) and TP LC (55.2 ± 23.0 minutes; 95%CI: 50.7-59.7, P < 0.01), though there was no significant difference between MTP and TP LC (P = 0.566). After adjusting for age, BMI, and sex, the difference in operative time between the SP and MTP/TP groups remained significant (P < 0.001). All patients had minimal intraoperative blood loss (< 10 mL), with no significant differences among groups.
| Outcome measure | MTP (n = 31) | TP (n = 100) | SP (n = 11) | P value (MTP vs TP) | P value (MTP vs SP) | P value (TP vs SP) |
| Operative time (minutes) | 52.5 ± 19.5 (45.8-59.2) | 55.2 ± 23.0 (50.7-59.7) | 103.1 ± 34.9 (82.3-123.9) | 0.566 | 0.009 | 0.000 |
| Intraoperative blood loss | 31 (100) (89.1-100.0) | 100 (100) (96.3-100.0) | 11 (100) (71.5-100.0) | 1.000 | 1.000 | 1.000 |
| Hospital stay (days) | 1.2 ± 0.5 (1.0-1.4) | 1.3 ± 0.6 (1.2-1.4) | 1.5 ± 0.5 (1.2-1.8) | 0.341 | 0.136 | 0.384 |
| Postoperative complications | 0 (0) (0.0-10.9) | 0 (0) (0.0-3.6) | 1 (9.1) (1.1-31.0) | < 0.001 | 0.089 | 0.0087 |
| Postoperative pain (VNRS) | ||||||
| 24 hours | 2.1 ± 1.0 (1.8-2.4) | 2.3 ± 1.1 (2.1-2.5) | 2.5 ± 1.2 (1.8-3.2) | 0.320 | 0.210 | 0.450 |
| 48 hours | 1.2 ± 0.8 (0.9-1.5) | 1.4 ± 0.9 (1.2-1.6) | 1.6 ± 1.0 (1.0-2.2) | 0.280 | 0.170 | 0.390 |
Postoperative outcomes are detailed in Table 2. The MTP group had the shortest mean hospital stay (1.2 ± 0.5 days; 95%CI: 1.0-1.4), followed by the TP (1.3 ± 0.6 days; 95%CI: 1.2-1.4) and SP groups (1.5 ± 0.5 days; 95%CI: 1.2-1.8), but differences were not statistically significant (P > 0.05). One case of postoperative abdominal infection occurred in the SP group (9.1%; 95%CI: 1.1-31.0), but its incidence was not statistically different from that of the TP (0%; 95%CI: 0.0-3.6, P = 0.087 after Bonferroni correction) or MTP group (0%, 95%CI: 0.0-10.9, P = 0.241). No complications were reported in the MTP group. The abdominal infection was managed successfully with antibiotics. No other major complications, such as bile duct injury or postoperative hemorrhage, were recorded in any group. Postoperative pain data were available for 89% of patients (n = 126). At 24 hours, mean Verbal Numerical Rating Scale scores were 2.1 ± 1.0 (MTP), 2.3 ± 1.1 (TP), and 2.5 ± 1.2 (SP), with no significant differences (P = 0.32). At 48 hours, scores were 1.2 ± 0.8 (MTP), 1.4 ± 0.9 (TP), and 1.6 ± 1.0 (SP), again not statistically different (P = 0.28).
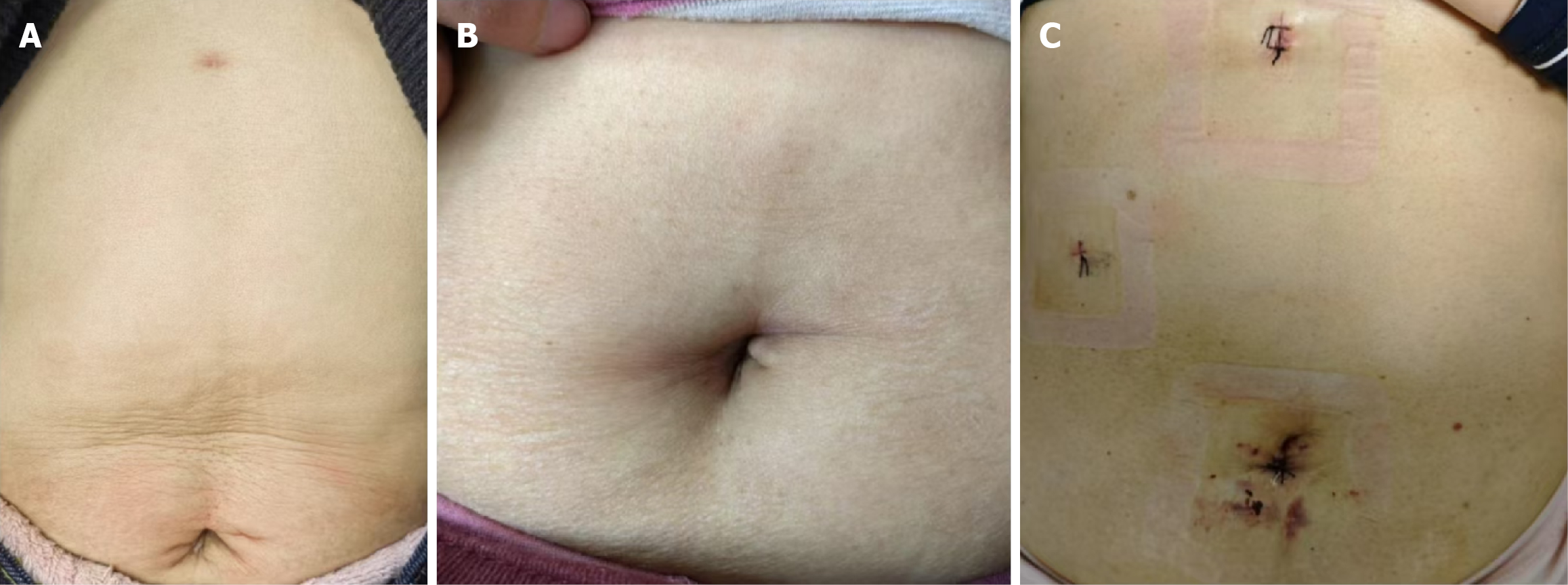
At the 1-month follow-up, the MTP and SP groups achieved excellent scar visibility (scores 8-10) in all patients, while the TP group had significantly lower rates of excellent cosmesis (P < 0.05). Representative postoperative scar appearances are shown in Figure 4.
Figure 4A demonstrates the remarkable cosmetic result achieved through the MTP LC technique. The incision sites, located within the umbilicus and sub-xiphoid, are nearly imperceptible, reflecting minimal scarring and excellent healing, highlighting the aesthetic advantage of the MTP method. Figure 4B demonstrates the remarkable cosmetic result achieved through the SP LC technique. The incision site, located within the umbilicus, is nearly imperceptible, indicating minimal scarring and excellent healing, highlighting the aesthetic advantage of the SP method. Figure 4C displays three well-placed incision sites with mild bruising and early signs of healing. While the presence of multiple ports affects cosmetic appearance compared to lesser port methods, the outcome remains clinically acceptable and within expected post
This retrospective cohort study systematically compared MTP, SP, and TP LC, focusing on cosmetic outcomes, operative efficiency, safety, and recovery. The key novelty lies in the comprehensive evaluation of three techniques in a single cohort, addressing the lack of rigorous comparative data on MTP LC.
SP LC was associated with significantly longer operative times (103.1 ± 34.9 minutes) compared to MTP and TP LC. This aligns with previous studies highlighting technical challenges of SP surgery, including limited instrument triangulation, restricted maneuverability, and ergonomic constraints that prolong dissection and retraction[15-17]. In contrast, MTP LC balanced minimal invasiveness with surgical feasibility: Its operative time (52.5 ± 19.5 minutes) was comparable to that of TP LC (55.2 ± 23.0 minutes), indicating that the clustered port design (dual umbilical + sub-xiphoid incisions) resolves the technical limitations of SP LC without compromising efficiency.
All groups had minimal blood loss (< 10 mL), reflecting the inherent advantage of laparoscopic surgery in reducing tissue and vascular trauma[18]. The SP group had a 9.1% rate of abdominal infection, but this was not statistically significant from that of the other two groups after Bonferroni correction and adjusting for baseline covariates. This finding is consistent with reports of potential higher complication risks in SP procedures due to concentrated instrument insertion through a single incision, but the small sample size in the SP group (n = 11) makes it vulnerable to single-event outliers, limiting definitive safety conclusions[19,20]. MTP had no postoperative complications, likely due to its balanced port placement (distributing instruments across two umbilical incisions and a sub-xiphoid incision) that reduces local tissue stress and infection risk.
MTP also had the shortest hospital stay (1.2 ± 0.5 days), attributed to minimal tissue trauma, short operative time, and absence of complications, factors that collectively accelerate recovery. While length of stay differences were not statistically significant among groups, the clinical relevance of shorter hospital stays (e.g., reduced healthcare costs and faster return to normal activities) supports MTP LC as a patient-centered option. Postoperative pain scores were similar across all groups, suggesting that reduced-port techniques do not offer significant analgesic benefits compared to TP LC in this cohort. This may be due to the overall minimally invasive nature of LC, with pain primarily driven by peritoneal irritation rather than incision number.
Cosmesis is a key patient-reported outcome in reduced-port surgery[20-23]. Both MTP and SP achieved excellent scar visibility, as their incisions were concealed within umbilical folds or sub-xiphoid regions. In contrast, TP’s three separate incisions (subumbilical, sub-xiphoid, and right subcostal) resulted in more visible scarring. This finding confirms that reduced-port techniques prioritize patient aesthetic preferences, with MTP offering the added benefit of avoiding SP’s technical drawbacks.
Gender distribution varied significantly: The SP and MTP groups had a higher proportion of female patients, reflecting greater emphasis on cosmetic outcomes among women[22,23]. The TP group had a higher mean age, likely due to its established safety profile, making it preferred for elderly patients who may be less tolerant of prolonged operative times or increased complication risks associated with SP LC[22,23]. The SP group’s lower BMI (22.3 ± 2.1 kg/m2) suggests that surgeons may select this procedure for patients with lower body fat to ensure adequate surgical exposure, as higher BMI can exacerbate SP’s technical challenges[22,23]. These patient selection patterns highlight the presence of selection bias, which was addressed via multivariable adjustment but remains a limitation of the retrospective design.
Our study has limitations. First, its retrospective and non-randomized design introduced potential selection bias, as evidenced by the younger age, lower BMI, and exclusively female enrollment in the SP group, reflecting surgeon selection for technically favorable cases. Second, scar assessment was based on a subjective 10-point telephone scale rather than a validated tool (e.g., Patient and Observer Scar Assessment Scale, Vancouver Scar Scale), lacking inter-rater reliability. Third, postoperative pain data were incomplete (available for 89% of patients) and not systematically recorded preoperatively, limiting robust evaluation of analgesic outcomes. This is a major limitation in reduced-port surgery research. Fourth, the sample size for the SP group was small (n = 11), and long-term follow-up (> 6 months) is lacking, so incisional hernia rates (a potential risk in SP surgery[23]) cannot be confirmed. Fifth, all procedures were performed by a single surgeon, which improves consistency but limits external validity and generalizability to other centers or less experienced surgeons. We have initiated a 3-year follow-up study to address these gaps.
The choice of surgical technique should be individualized based on patient priorities and characteristics: For patients prioritizing cosmesis and minimal invasiveness without compromising efficiency or safety, MTP LC is a promising option (hypothesis-generating, not definitive guidance). SP LC may be considered for patients with low BMI (≤ 22 kg/m2) who strongly prioritize a single scar, but patients should be counseled on longer operative times and potential for higher infection risks (limited by small sample size). TP LC remains a safe choice for elderly patients, those with high BMI, or those for whom operative time is a critical factor (e.g., comorbidities requiring shorter anesthesia exposure).
This study demonstrates that MTP LC is a balanced approach among the three techniques evaluated. It successfully bridges the gap between the superior cosmesis of SP surgery and the proven efficiency and safety of the conventional TP technique. While SP offers excellent cosmesis, its longer operative time and potential for higher complication risk restrict broad applicability. TP LC remains a safe alternative but is less favorable for patients prioritizing aesthetics. For surgeons and patients seeking an optimal balance between minimal scarring and operative practicality, MTP LC may be considered a preferred approach in selected cases, but conclusions are tempered by the retrospective design, selection bias, and small SP cohort. Future prospective studies with long-term follow-up and larger sample sizes are needed to confirm these findings and definitively establish the role of MTP LC in the surgical management of gallbladder disease.
| 1. | Nassar AHM, Hodson J, Ng HJ, Vohra RS, Katbeh T, Zino S, Griffiths EA; CholeS Study Group, West Midlands Research Collaborative. Predicting the difficult laparoscopic cholecystectomy: development and validation of a pre-operative risk score using an objective operative difficulty grading system. Surg Endosc. 2020;34:4549-4561. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 79] [Cited by in RCA: 82] [Article Influence: 13.7] [Reference Citation Analysis (1)] |
| 2. | Siddiqui MA, Rizvi SAA, Sartaj S, Ahmad I, Rizvi SWA. A Standardized Ultrasound Scoring System for Preoperative Prediction of Difficult Laparoscopic Cholecystectomy. J Med Ultrasound. 2017;25:227-231. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 23] [Article Influence: 2.6] [Reference Citation Analysis (1)] |
| 3. | Randhawa JS, Pujahari AK. Preoperative prediction of difficult lap chole: a scoring method. Indian J Surg. 2009;71:198-201. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 70] [Article Influence: 4.1] [Reference Citation Analysis (1)] |
| 4. | Kim EJ, Hwang EJ, Yoo YM, Kim KH. Prevention, diagnosis, and treatment of opioid use disorder under the supervision of opioid stewardship programs: it's time to act now. Korean J Pain. 2022;35:361-382. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 5. | Blichfeldt-Eckhardt MR, Ording H, Andersen C, Licht PB, Toft P. Early visceral pain predicts chronic pain after laparoscopic cholecystectomy. Pain. 2014;155:2400-2407. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 73] [Article Influence: 6.1] [Reference Citation Analysis (1)] |
| 6. | Evers L, Bouvy N, Branje D, Peeters A. Single-incision laparoscopic cholecystectomy versus conventional four-port laparoscopic cholecystectomy: a systematic review and meta-analysis. Surg Endosc. 2017;31:3437-3448. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 53] [Cited by in RCA: 63] [Article Influence: 6.3] [Reference Citation Analysis (1)] |
| 7. | Koo CH, Hwang JY, Shin HJ, Ryu JH. The Effects of Erector Spinae Plane Block in Terms of Postoperative Analgesia in Patients Undergoing Laparoscopic Cholecystectomy: A Meta-Analysis of Randomized Controlled Trials. J Clin Med. 2020;9:2928. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 24] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
| 8. | Wang J, Echevarria GC, Doan L, Ekasumara N, Calvino S, Chae F, Martinez E, Robinson E, Cuff G, Franco L, Muntyan I, Kurian M, Schwack BF, Bedrosian AS, Fielding GA, Ren-Fielding CJ. Effects of a single subanaesthetic dose of ketamine on pain and mood after laparoscopic bariatric surgery: A randomised double-blind placebo controlled study. Eur J Anaesthesiol. 2019;36:16-24. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 37] [Article Influence: 5.3] [Reference Citation Analysis (1)] |
| 9. | Saleem SZ, Akhtar SMM, Fareed A, Shaik AA, Asghar MS. Redefining pain management: investigating the efficacy and safety of erector spinae plane block and oblique subcostal transversus abdominis plane block in laparoscopic cholecystectomy - a meta analysis of randomized controlled trials. BMC Anesthesiol. 2025;25:182. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 10. | Iwashita Y, Hibi T, Ohyama T, Honda G, Yoshida M, Miura F, Takada T, Han HS, Hwang TL, Shinya S, Suzuki K, Umezawa A, Yoon YS, Choi IS, Huang WS, Chen KH, Watanabe M, Abe Y, Misawa T, Nagakawa Y, Yoon DS, Jang JY, Yu HC, Ahn KS, Kim SC, Song IS, Kim JH, Yun SS, Choi SH, Jan YY, Shan YS, Ker CG, Chan DC, Wu CC, Lee KT, Toyota N, Higuchi R, Nakamura Y, Mizuguchi Y, Takeda Y, Ito M, Norimizu S, Yamada S, Matsumura N, Shindoh J, Sunagawa H, Gocho T, Hasegawa H, Rikiyama T, Sata N, Kano N, Kitano S, Tokumura H, Yamashita Y, Watanabe G, Nakagawa K, Kimura T, Yamakawa T, Wakabayashi G, Mori R, Endo I, Miyazaki M, Yamamoto M. An opportunity in difficulty: Japan-Korea-Taiwan expert Delphi consensus on surgical difficulty during laparoscopic cholecystectomy. J Hepatobiliary Pancreat Sci. 2017;24:191-198. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 51] [Article Influence: 5.7] [Reference Citation Analysis (1)] |
| 11. | Kim H, Lee S. Effects of pain neuroscience education on kinesiophobia in patients with chronic pain: a systematic review and meta-analysis. Phys Ther Rehabil Sci. 2020;9:309-317. [DOI] [Full Text] |
| 12. | Borle FR, Mehra B, Ranjan Singh A. Comparison of Cosmetic Outcome Between Single-Incision Laparoscopic Cholecystectomy and Conventional Laparoscopic Cholecystectomy in Rural Indian Population: A Randomized Clinical Trial. Indian J Surg. 2015;77:877-880. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 11] [Article Influence: 0.9] [Reference Citation Analysis (1)] |
| 13. | von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP; STROBE Initiative. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet. 2007;370:1453-1457. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15623] [Cited by in RCA: 14437] [Article Influence: 759.8] [Reference Citation Analysis (7)] |
| 14. | Matsushima K, Ciesielski KM, Mandelbaum RS, Matsuo K. Clinical Demographics of Laparoscopic Cholecystectomy: A Gender-Specific Analysis. Am Surg. 2024;90:528-532. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (1)] |
| 15. | Lee YJ, Moon JI, Choi IS, Lee SE, Sung NS, Kwon SW, Yoon DS, Choi WJ, Park SM. A large-cohort comparison between single incision laparoscopic cholecystectomy and conventional laparoscopic cholecystectomy from a single center; 2080 cases. Ann Hepatobiliary Pancreat Surg. 2018;22:367-373. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 13] [Article Influence: 1.6] [Reference Citation Analysis (1)] |
| 16. | van der Linden YT, Bosscha K, Prins HA, Lips DJ. Single-port laparoscopic cholecystectomy vs standard laparoscopic cholecystectomy: A non-randomized, age-matched single center trial. World J Gastrointest Surg. 2015;7:145-151. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 7] [Cited by in RCA: 8] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 17. | Singh A, Kaur M, Baig MK, Swaminathan C, Subramanian A, Sajid MS. Cost-comparison of robotic versus laparoscopic colorectal resections: a mapped systematic review and meta-analysis of published studies. Transl Gastroenterol Hepatol. 2024;9:21. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 6] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 18. | Shi Z. Laparoscopic vs. open surgery: A comparative analysis of wound infection rates and recovery outcomes. Int Wound J. 2024;21:e14474. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 16] [Article Influence: 8.0] [Reference Citation Analysis (1)] |
| 19. | Agarwal R, Prabhu VMD, Rao NAR. From the operating room: Surgeons' views on difficult laparoscopic cholecystectomies. Ann Hepatobiliary Pancreat Surg. 2025;29:150-156. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 20. | Bae SU, Jeong WK, Baek SK. Single-port laparoscopic appendectomy for perforated appendicitis using ArtiSential® wristed articulated instrument. J Minim Access Surg. 2023;19:168-171. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 13] [Article Influence: 4.3] [Reference Citation Analysis (1)] |
| 21. | Rafiq MS, Khan MM. Scar Pain, Cosmesis and Patient Satisfaction in Laparoscopic and Open Cholecystectomy. J Coll Physicians Surg Pak. 2016;26:216-219. [PubMed] |
| 22. | Zapf M, Denham W, Barrera E, Butt Z, Carbray J, Wang C, Linn J, Ujiki M. Patient-centered outcomes after laparoscopic cholecystectomy. Surg Endosc. 2013;27:4491-4498. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 25] [Article Influence: 1.9] [Reference Citation Analysis (1)] |
| 23. | Haueter R, Schütz T, Raptis DA, Clavien PA, Zuber M. Meta-analysis of single-port versus conventional laparoscopic cholecystectomy comparing body image and cosmesis. Br J Surg. 2017;104:1141-1159. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 91] [Cited by in RCA: 92] [Article Influence: 10.2] [Reference Citation Analysis (1)] |