Published online Mar 27, 2026. doi: 10.4254/wjh.v18.i3.113700
Revised: October 22, 2025
Accepted: December 31, 2025
Published online: March 27, 2026
Processing time: 206 Days and 18.5 Hours
Biliary obstruction is an important pathological condition in childhood, with complex etiologies and often non-specific clinical manifestations. Children with suspected biliary obstruction commonly present with clinical symptoms such as jaundice, abdominal pain, fever, vomiting, and abnormal liver function bio
To explore the application value of endoscopic retrograde cholangiopancreatography (ERCP) technology in pediatric common bile duct stone disease and summarize the pediatric experience.
Clinical data of children suspected of biliary obstruction who received ERCP treatment in the Department of General Surgery at Anhui Provincial Children’s Hospital from May 2022 to June 2025 were collected. The clinical characteristics were summarized, changes in liver function before and after ERCP were com
A total of 62 children with suspected biliary obstruction underwent 101 ERCP procedures, of which 97 were successful and 4 failed. The diagnoses were clarified as 20 cases of common bile duct stones, 15 cases of biliary infection, 22 cases of choledochal cysts, 6 cases of abnormal pancreatobiliary junction, and 10 cases of acu
ERCP technology can assist in determining the etiology of children with suspected biliary obstruction before surgery, especially in the treatment of biliary obstruction caused by common bile duct stones, proving to be both safe and effective.
Core Tip: This study demonstrates that endoscopic retrograde cholangiopancreatography (ERCP) is a safe and effective minimally invasive technique for both diagnosing and treating common bile duct stones in children. It achieved a 100% technical success rate in 29 procedures for 20 pediatric common bile duct stones patients, significantly improving liver function with a low complication rate (6.9%, all mild post-ERCP pancreatitis). ERCP is a valuable tool for managing biliary obstruction in children, offering precise diagnosis and therapeutic intervention.
- Citation: Zhang T, Tang R, Hu XY, Qi SQ, Pan ZB. Application of endoscopic retrograde cholangiopancreatography in the diagnosis and treatment of pediatric common bile duct stone disease. World J Hepatol 2026; 18(3): 113700
- URL: https://www.wjgnet.com/1948-5182/full/v18/i3/113700.htm
- DOI: https://dx.doi.org/10.4254/wjh.v18.i3.113700
Biliary obstruction is an important pathological condition in childhood, with complex etiologies and often non-specific clinical manifestations. Children with suspected biliary obstruction commonly present with clinical symptoms such as jaundice, abdominal pain, fever, vomiting, and abnormal liver function biochemical markers, including significantly elevated serum total bilirubin, direct bilirubin, alkaline phosphatase, γ-glutamyltransferase, and transaminase levels[1,2]. Common causes include common bile duct stones, biliary tract infections, choledochal cysts, abnormal pancreatobiliary junction, and acute or chronic pancreatitis. Among these, if common bile duct stones are not promptly and effectively managed, they may progress to severe complications such as suppurative cholangitis and biliary pancreatitis, which not only exacerbate the condition but may also cause long-term adverse effects on the child’s growth, development, and quality of life.
Endoscopic retrograde cholangiopancreatography (ERCP) is now widely used in the diagnosis and treatment of adult biliary and pancreatic diseases, becoming one of the gold standards in this field. However, its application in the pediatric field still faces many challenges. In pediatric patients, the bile duct system is smaller in diameter, the duct walls are thinner, and the cooperation during the procedure is poor, which increases the difficulty of operation and raises the risk of complications. A study by Lorio et al[3] reported on 287 pediatric ERCP cases, with a success rate of 95.5%, no deaths, but an adverse event rate of 12.7%, with a higher success rate in biliary diseases compared to pancreatic diseases. The younger the age, the more complex the condition, and the higher the risk of adverse events. The incidence of post
This study retrospectively analyzes the clinical data of children with suspected biliary obstruction who received ERCP treatment in the Department of General Surgery at Anhui Provincial Children’s Hospital. The focus is to evaluate the clinical efficacy, operational safety, and technical key points of ERCP in the diagnosis and treatment of pediatric common bile duct stones. The aim is to summarize practical experience in pediatric ERCP operations and provide evidence-based medical support for promoting the standardized and safe application of this technique in pediatric patients in China.
A retrospective collection of clinical data from children with suspected biliary obstruction who received ERCP treatment in the Department of General Surgery at Anhui Provincial Children’s Hospital from May 2022 to June 2025. Inclusion criteria were: (1) Preliminary indication of biliary obstruction based on clinical symptoms, laboratory tests, and imaging examinations [such as abdominal ultrasound, magnetic resonance cholangiopancreatography (MRCP), etc.]; (2) Clear indication for ERCP with no contraindications; (3) Age ≤ 18 years; and (4) Complete clinical and follow-up data. Exclusion criteria were: (1) Coexisting severe liver or renal insufficiency or other systemic diseases; and (2) Missing or lost critical clinical data. A total of 62 children were included, with 30 males and 32 females. The median age was 8.5 (4.3, 13.7) years, with an age range of 3 years to 18 years. The study protocol was approved by the Ethics Committee of Anhui Provincial Children’s Hospital, and all legal guardians of the children provided informed consent and signed written consent forms.
In this study, all pediatric ERCP procedures were performed according to the 2018 Chinese ERCP Guidelines and the 2019 European Society of Gastrointestinal Endoscopy ERCP Guidelines[5,6]. Pediatric biliary tract diseases mainly include common bile duct stones, Mirizzi syndrome, biliary obstruction, biliary stricture, biliary leakage, primary sclerosing cholangitis, congenital choledochal cysts, suspected Oddi sphincter dysfunction, and acute biliary pancreatitis. Pancreatic diseases include recurrent acute pancreatitis, chronic pancreatitis (with complications such as pancreatic duct stones, strictures, or obstructions), pancreatic divisum (with recurrent pancreatitis), symptomatic pancreatic pseudocysts (requiring internal drainage), pancreatobiliary maljunction (PBM), pancreatic duct injuries, or pancreatic leaks. Pre
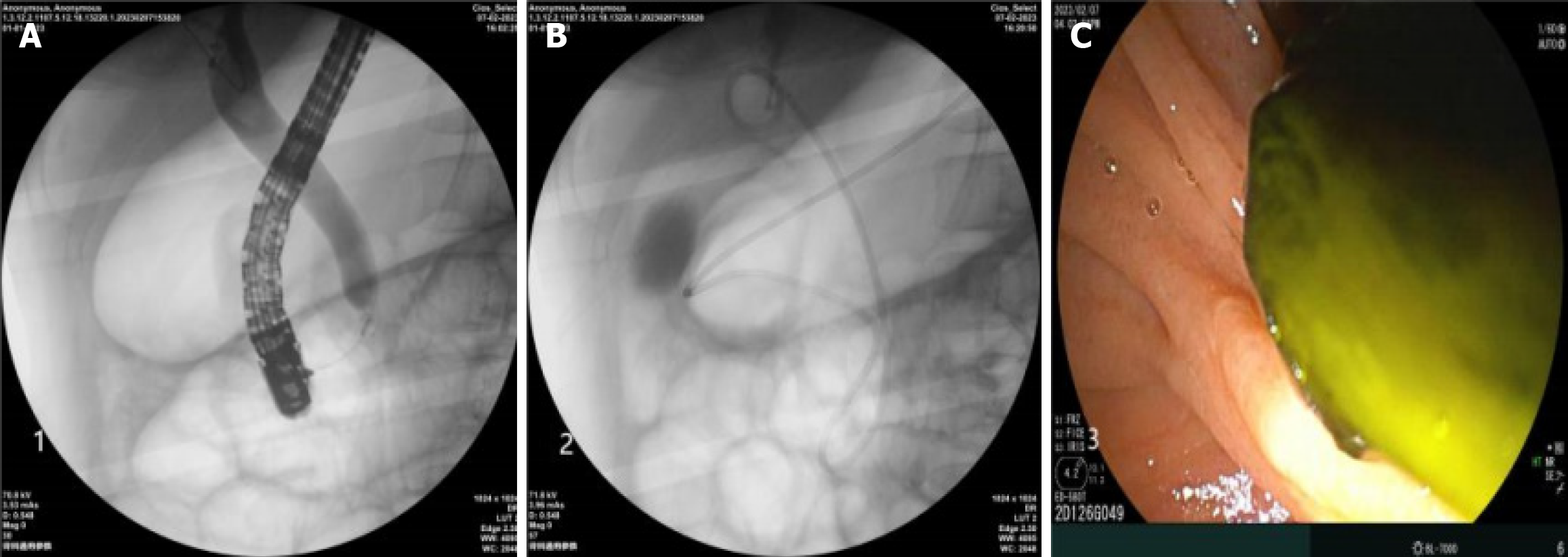
After a definitive diagnosis, appropriate treatment was implemented based on the findings. For patients with confirmed common bile duct stones, stone extraction was performed using a balloon catheter or basket to either trap or retrieve the stone. If stone removal was difficult, EST or EPBD was performed to enlarge the papillary opening. Stone removal was then attempted again using the same method. After stone removal, an endoscopic nasobiliary drainage tube was placed for external drainage, or a plastic biliary stent (endoscopic retrograde biliary drainage) was inserted for internal drainage. For patients diagnosed with common bile duct cysts, biliary infections, pancreatic divisum syndrome, or acute/chronic pancreatitis, corresponding measures were taken intraoperatively, including biliary drainage, pancreatic duct stent insertion, and nasopancreatic tube placement, to ensure smooth pancreatic and biliary drainage. After ERCP, the endoscope was removed, and after recovery, the child was returned to the ward. Postoperative fasting was maintained for 6-8 hours, and symptomatic supportive treatment such as fluid resuscitation, anti-infection, and enzyme inhibition was provided. Close monitoring of abdominal pain, body temperature, amylase, and bilirubin levels was performed to prevent postoperative complications such as pancreatitis, perforation, bleeding, or infection. The entire ERCP procedure emphasized precise understanding of pediatric pancreatobiliary anatomy and the principle of minimal trauma. Figure 1 shows the typical steps of ERCP for common bile duct stones.
The age, sex, white blood cell count, total bilirubin, direct bilirubin, aspartate aminotransferase, alanine aminotransferase, γ-glutamyltransferase, amylase, ERCP operation time, hospital stay duration, and postoperative complications were recorded and organized for all children. Post-ERCP pancreatitis (PEP) is defined as serum amylase and lipase levels exceeding three times the upper normal limit, accompanied by clinical symptoms such as abdominal pain, lasting for more than 24 hours. The clinical diagnosis of cholangitis requires the presence of the following three criteria[7]: (1) Systemic inflammatory response: At least one of the following indicators: Fever (temperature > 38 °C), abnormal white blood cell count (< 4000/mm3 or > 10000/mm3), or elevated serum C-reactive protein levels; (2) Biliary obstruction signs: At least one of the following indicators: Jaundice (serum total bilirubin ≥ 2 mg/dL) or liver function abnormalities (alkaline phosphatase, γ-glutamyltransferase, aspartate aminotransferase, and alanine aminotransferase exceeding 1.5 times the upper normal limit); and (3) Imaging evidence: At least one of the following findings: Bile duct dilation or imaging findings (such as ultrasound, computed tomography, magnetic resonance imaging/MRCP, ERCP) showing causative factors (such as strictures, stones, stent obstruction, etc.).
Statistical analysis was performed using SPSS 27.0 and GraphPad Prism 10.0 software. For normally distributed qu
All children in this study were successfully followed up using a combination of outpatient visits and telephone follow-ups, with follow-up durations ranging from 3 months to 3 years.
Among 62 children after surgery, 20 were clearly diagnosed with common bile duct stones, and the other diagnoses are shown in Table 1. Among these 20 children with common bile duct stones, a total of 29 ERCP procedures were per
| Item | Case (s) |
| Sex (male/female) | 24/38 |
| Age (years), median (interquartile range) | 8.3 (4.5, 14.0) |
| Success rate | 97 (96.0) |
| Diagnosis | |
| Common bile duct stones | 20 (27.4) |
| Biliary infection | 15 (20.5) |
| Choledochal cysts | 22 (30.1) |
| Abnormal pancreatobiliary junction | 6 (8.2) |
| Acute/chronic pancreatitis | 10 (13.7) |
| Treatment measures for common bile duct stones | |
| EPBD | 18 (25.0) |
| ENBD | 7 (9.7) |
| ERBD | 13 (18.1) |
| Biliary stone extraction (basket/balloon) | 20 (27.8) |
| Removal of biliary stent | 9 (12.5) |
| EST | 5 (6.9) |
For the 20 children with common bile duct stones who underwent ERCP stone extraction, significant improvement in liver function markers was observed after the procedure. The results showed that postoperative total bilirubin decreased from 85.47 ± 26.83 μmol/L to 42.15 ± 12.69 μmol/L, and direct bilirubin decreased from 38.92 (35.14, 45.61) μmol/L to 19.87 (15.42, 23.75) μmol/L. Additionally, aspartate aminotransferase decreased from 268.5 (255.3, 275.1) U/L to 124.6 (118.9, 130.2) U/L, alanine aminotransferase decreased from 315.8 (308.4, 335.2) U/L to 172.3 (165.8, 185.6) U/L, and γ-glutamyltransferase decreased from 218.6 ± 82.4 U L to 128.7 ± 38.5 U/L. All differences in these parameters were statistically significant (all P < 0.05) (Table 2).
| Parameter | Preoperative | Postoperative | T/Z value | P value |
| WCC (× 109/L) | 6.96 ± 2.01 | 7.68 ± 2.54 | -1.21 | 0.23 |
| Tbil (μmmol/L) | 85.47 ± 26.83 | 42.15 ± 12.69 | 9.40 | < 0.01 |
| Dbil (μmmol/L) | 38.92 (35.14, 45.61) | 19.87 (15.42, 23.75) | 4.72 | < 0.01 |
| AST (U/L) | 268.5 (255.3, 275.1) | 124.6 (118.9, 130.2) | 4.70 | < 0.01 |
| ALT (U/L) | 310.8 (308.4, 335.2) | 172.3 (165.8, 185.6) | 5.04 | < 0.01 |
| GGT (U/L) | 218.6 ± 82.4 | 100.4 ± 38.5 | 8.16 | < 0.01 |
| AMY (U/L) | 90.14 ± 77.40 | 108.09 ± 100.16 | -1.04 | 0.29 |
After ERCP, 2 out of 20 children developed complications, resulting in an incidence rate of 10.0%. Both cases were mild PEP, which were resolved after conservative treatment, including fasting, fluid resuscitation, somatostatin, and its analogs. No child experienced bleeding, perforation, acute cholangitis, contrast agent allergies, or anesthesia-related adverse events. Notably, both of the PEP cases had an incident of guidewire misplacement into the pancreatic duct during the procedure and both underwent EST.
After discharge, all children were followed up, with a median follow-up time of 18 months (interquartile range: 9-24 months). During the follow-up period, two children were found to have recurrent common bile duct stones upon reexamination at 2 months and 6 months post-surgery, with the largest stone diameters measuring 4.0 mm and 5.2 mm, re
This study successfully identified the etiology of biliary obstruction in 62 children with suspected biliary tract obstruction through ERCP, accurately differentiating diseases such as common bile duct stones, choledochal cysts, and PBM. Notably, PBM, an important congenital anomaly, is a key factor in increasing the risk of choledochal cysts, recurrent pancreatitis, and biliary carcinoma in children. Its diagnosis heavily relies on clear imaging of the pancreatobiliary junction provided by ERCP[8]. Although non-invasive techniques such as MRCP have seen increasing resolution, the dynamic imaging capability of ERCP remains irreplaceable for diagnosing minute bile leaks, Oddi sphincter dysfunction, and certain forms of PBM[9]. Additionally, ERCP offers advantages over computed tomography and magnetic resonance imaging in the diagnosis of choledochal cysts and biliary infections[10]. The high success rate (97.0%) of this study suggests that ERCP, when performed at an experienced pediatric endoscopy center, is a safe and reliable diagnostic tool. For cases where the cause of biliary obstruction remains unclear after non-invasive examinations, ERCP should be actively considered to obtain a definitive diagnosis, particularly for the treatment of common bile duct stones, which has shown significant clinical benefits and warrants further research and clinical application.
The results of this study are consistent with recent reports on pediatric ERCP, which indicate that, although success rates and complication rates vary across studies, pediatric ERCP generally achieves high success rates with a low incidence of severe complications. For example, a large ERCP study involving 127 children reported a success rate of 98.3%[11], which is similar to the 97.0% success rate observed in this study. In the treatment of common bile duct stones, the procedural success rate (100%) and post-operative pancreatitis incidence (6.9%) in this study are consistent with the findings of Dişçi et al[12], who also support the preferential use of EPBD in children. It is worth noting that due to the smaller size of pediatric bile ducts and the greater procedural difficulty compared to adults, there is limited experience in pediatric biliary ERCP. Therefore, this study aims to report the single-center ERCP experience from our hospital to enhance understanding of pediatric ERCP.
The implementation of pediatric ERCP presents unique challenges, with a steep learning curve. First, the smaller lumen and more fragile walls of the pediatric digestive tract require operators to possess higher precision and force control, otherwise, the risk of bleeding or perforation may increase. Secondly, the narrower diameter of the pediatric common bile duct makes the use of adult-sized instruments for selective cannulation or stone retrieval (e.g., balloon or basket) significantly more difficult than in adults. Additionally, children cannot actively cooperate during the procedure and must undergo the entire process under general anesthesia, which requires close collaboration between the en
In this study, all 20 children with common bile duct stones underwent successful ERCP treatment, with significant improvements in bilirubin and liver function markers postoperatively. All children with bile duct obstruction showed marked improvement in abdominal pain and jaundice symptoms on the first day after ERCP, which further corroborates the excellent efficacy of ERCP as a first-line treatment. However, there were no significant differences in white blood cell count and amylase levels between groups, possibly due to the low likelihood of biliary tract infection secondary to bile duct stones and the relatively easy bile duct cannulation during surgery, which minimizes the probability of mis
Compared to traditional open or laparoscopic exploration of the common bile duct, ERCP avoids the need for T-tube placement, thus preventing surgical trauma, prolonged anesthesia times, and postoperative recovery periods, significantly reducing the child’s suffering[14]. Our technique prioritizes (EPBD, 18 times) over standard sphincterotomy (EST, 5 times), which is consistent with other reported studies. Research shows that for this specific pediatric population, EPBD can preserve Oddi sphincter function and significantly reduce the risk of long-term adverse events (such as stone recurrence and reflux cholangitis), offering a safer alternative[15].
In this study, the average ERCP procedure time was 54.2 ± 18.7 minutes, and the average hospital stay was 7.0 ± 2.8 days, significantly reducing the child’s disease-related pain and hospital costs compared to traditional surgical methods, thereby greatly saving medical resources and aligning with the accelerated recovery surgical approach. Therefore, ERCP, with its minimally invasive, efficient, and repeatable characteristics, has become the preferred method for treating pediatric common bile duct stones. The complication rate in this study was 6.9% (2/29), with all cases being mild PEP and no serious adverse events, a result highly consistent with recent data from large pediatric specialty centers[16]. This demonstrates that ERCP can be performed safely in children when operated by experienced physicians at high-volume centers. Both cases of PEP were associated with guidewire misplacement into the pancreatic duct during the procedure, confirming that repeated pancreatic duct cannulation is the core risk factor for PEP[17,18]. This urges us to consider optimization strategies such as using guidewire-assisted deep cannulation techniques, cone-shaped catheters, and, when necessary, pre-placement of pancreatic duct stents, or the preoperative use of indomethacin suppositories, all of which have been proven in randomized controlled trials to effectively reduce PEP incidence[19,20].
A study by Jiang et al[21] on the risk of pancreatitis after common bile duct stone removal found that pancreatic duct stent insertion significantly reduced the risk of pancreatitis after ERCP (P < 0.05). The incidence of pancreatitis in patients with pancreatic duct stent insertion was 11.84% (9/76), compared to 39.31% (46/117) in those without. The serum amylase levels at 6 hours, 12 hours, and 24 hours post-ERCP were lower in patients who received pancreatic duct stent insertion. Our positive outcomes are attributed to strict adherence to these evidence-based principles and provide a replicable safe operating model for other centers. The recurrence rate of 10.0% (2/20) suggests that while ERCP resolves mechanical obstruction, it does not eliminate the metabolic or anatomical basis for stone formation. Pediatric pigment stones are commonly found in children with biliary stasis (such as those receiving long-term total parenteral nutrition) or hemolytic diseases[22].
In this study, two children with recurrent stones experienced resolution after treatment with oral ursodeoxycholic acid, highlighting the importance of adjunctive pharmacological therapy. Ursodeoxycholic acid promotes bile secretion and improves the composition of bile acid pools, dissolving small stones and altering the bile environment in favor of preventing stone formation[23]. Therefore, ERCP should not be considered the endpoint of treatment but rather the beginning of screening for potential causes (such as hemolysis markers, bile composition analysis) and long-term pharmacological management, forming a complete diagnostic and therapeutic loop from obstruction relief to recurrence prevention. This will be a future direction for minimally invasive standardized treatment of common bile duct stones in children.
The limitation of this study lies in its single-center, retrospective design. Future multicenter, prospective studies are needed to establish more rigorous pediatric ERCP indications guidelines. Additionally, analyzing the composition of removed stones and conducting metabolic profiling studies on bile will help understand the root causes of pediatric cholelithiasis and provide evidence for personalized prevention strategies[24]. With the application of new technologies such as SpyGlass, diagnostic ERCP may be partially replaced by more accurate intraluminal diagnostic techniques in the future[25], but therapeutic ERCP, as a core minimally invasive intervention, will remain irreplaceable in the foreseeable future.
In conclusion, ERCP has demonstrated significant value in the diagnosis and treatment of pediatric biliary diseases, especially in the management of common bile duct stones. ERCP accurately identifies various causes of biliary ob
| 1. | Squires JE, McKiernan P. Molecular Mechanisms in Pediatric Cholestasis. Gastroenterol Clin North Am. 2018;47:921-937. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 12] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 2. | Pryor JP, Volpe CM, Caty MG, Doerr RJ. Noncalculous biliary obstruction in the child and adolescent. J Am Coll Surg. 2000;191:569-578. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.2] [Reference Citation Analysis (1)] |
| 3. | Lorio E, Moreau C, Hernandez B, Rabbani T, Michaud K, Hachem J, Aggarwal P, Stolow E, Brown L, Michalek JE, Patel S. Pediatric ERCP: Factors for Success and Complication-A 17-Year, Multisite Experience. J Pediatr Gastroenterol Nutr. 2023;77:413-421. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 11] [Article Influence: 3.7] [Reference Citation Analysis (1)] |
| 4. | Freeman ML. Pancreatic stents for prevention of post-endoscopic retrograde cholangiopancreatography pancreatitis. Clin Gastroenterol Hepatol. 2007;5:1354-1365. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 165] [Cited by in RCA: 130] [Article Influence: 6.8] [Reference Citation Analysis (2)] |
| 5. | ERCP group; Chinese Society of Digestive Endoscopology; Biliopancreatic group; Chinese Association of Gastroenterologist and Hepatologist; National Clinical Research Center for Digestive Diseases. [Chinese guidelines for endoscopic retrograde cholangiopancreatography (2018 edition)]. Linchuang Gandanbing Zazhi. 2018;34:2537-2554. [DOI] [Full Text] |
| 6. | ASGE Standards of Practice Committee; Buxbaum JL, Abbas Fehmi SM, Sultan S, Fishman DS, Qumseya BJ, Cortessis VK, Schilperoort H, Kysh L, Matsuoka L, Yachimski P, Agrawal D, Gurudu SR, Jamil LH, Jue TL, Khashab MA, Law JK, Lee JK, Naveed M, Sawhney MS, Thosani N, Yang J, Wani SB. ASGE guideline on the role of endoscopy in the evaluation and management of choledocholithiasis. Gastrointest Endosc. 2019;89:1075-1105.e15. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 489] [Cited by in RCA: 402] [Article Influence: 57.4] [Reference Citation Analysis (6)] |
| 7. | Miura F, Okamoto K, Takada T, Strasberg SM, Asbun HJ, Pitt HA, Gomi H, Solomkin JS, Schlossberg D, Han HS, Kim MH, Hwang TL, Chen MF, Huang WS, Kiriyama S, Itoi T, Garden OJ, Liau KH, Horiguchi A, Liu KH, Su CH, Gouma DJ, Belli G, Dervenis C, Jagannath P, Chan ACW, Lau WY, Endo I, Suzuki K, Yoon YS, de Santibañes E, Giménez ME, Jonas E, Singh H, Honda G, Asai K, Mori Y, Wada K, Higuchi R, Watanabe M, Rikiyama T, Sata N, Kano N, Umezawa A, Mukai S, Tokumura H, Hata J, Kozaka K, Iwashita Y, Hibi T, Yokoe M, Kimura T, Kitano S, Inomata M, Hirata K, Sumiyama Y, Inui K, Yamamoto M. Tokyo Guidelines 2018: initial management of acute biliary infection and flowchart for acute cholangitis. J Hepatobiliary Pancreat Sci. 2018;25:31-40. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 366] [Cited by in RCA: 317] [Article Influence: 39.6] [Reference Citation Analysis (2)] |
| 8. | Balassone V, Imondi C, Caldaro T, De Angelis P, Dall'Oglio L. Direct visualization of biliary stump polyp in a boy with recurrent pancreatitis after surgery for pancreatobiliary maljunction associated with choledocal cyst. VideoGIE. 2022;7:42-43. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (1)] |
| 9. | Coté GA, Elmunzer BJ, Nitchie H, Kwon RS, Willingham F, Wani S, Kushnir V, Chak A, Singh V, Papachristou GI, Slivka A, Freeman M, Gaddam S, Jamidar P, Tarnasky P, Varadarajulu S, Foster LD, Cotton P. Sphincterotomy for biliary sphincter of Oddi disorder and idiopathic acute recurrent pancreatitis: the RESPOnD longitudinal cohort. Gut. 2024;74:58-66. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 6] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 10. | Oh SH, Chang SH, Kim HJ, Cho JM, Hwang JH, Namgoong JM, Kim DY, Cho YA, Yoon CH, Kim KM. Cholangiographic characteristics of common bile duct dilatation in children. World J Gastroenterol. 2015;21:6229-6235. [PubMed] [DOI] [Full Text] |
| 11. | Yu ZP, Zhu L, Yang XP, Cao RL, Chen YX. [Efficacy and safety of endoscopic retrograde cholangiopancreatography in children]. Zhonghua Er Ke Za Zhi. 2022;60:1295-1301. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 12. | Dişçi E, Peksöz R, Yıldız M, Yıldırgan Mİ, Albayrak Y, Fakirullahoğlu M, Fırıncı B, Atamanalp SS. Endoscopic Retrograde Cholangiopancreatography in Pediatric Patients. J Laparoendosc Adv Surg Tech A. 2022;32:320-324. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 5] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 13. | Syrén EL, Sandblom G, Enochsson L, Eklund A, Isaksson B, Österberg J, Eriksson S. Outcome of ERCP related to case-volume. Surg Endosc. 2022;36:5339-5347. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 19] [Article Influence: 4.8] [Reference Citation Analysis (1)] |
| 14. | Baucom RB, Feurer ID, Shelton JS, Kummerow K, Holzman MD, Poulose BK. Surgeons, ERCP, and laparoscopic common bile duct exploration: do we need a standard approach for common bile duct stones? Surg Endosc. 2016;30:414-423. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 53] [Article Influence: 5.3] [Reference Citation Analysis (1)] |
| 15. | Kouchi K, Takenouchi A, Matsuoka A, Yabe K, Yoshizawa H, Nakata C, Fujishiro J, Sugiyama H. Case Series of Endoscopic Papillary Balloon Dilation for Children with Common Bile Duct Stones and a Review of the Literature. J Clin Med. 2024;13:2251. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 16. | Hassan AM, Lin TK, Smith MT, Hornung L, Abu-El-Haija M, Nathan JD, Vitale DS. Risk Factors for Post-ERCP Pancreatitis in Pediatric and Young Adult Patients. J Pediatr Gastroenterol Nutr. 2023;76:807-812. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 19] [Article Influence: 6.3] [Reference Citation Analysis (2)] |
| 17. | Zhu P. Analysis of risk factors and construction of predictive model for post-endoscopic retrograde cholangiopancreatography pancreatitis. Pak J Med Sci. 2023;39:1642-1646. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (2)] |
| 18. | Yang L, Fu Y, Sun ZH, Zhou J, Tang J, Ni J. [Risk factors for pancreatitis after endoscopic retrograde cholangiopancreatography in children]. Zhongguo Dang Dai Er Ke Za Zhi. 2024;26:690-694. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 19. | Elmunzer BJ, Foster LD, Serrano J, Coté GA, Edmundowicz SA, Wani S, Shah R, Bang JY, Varadarajulu S, Singh VK, Khashab M, Kwon RS, Scheiman JM, Willingham FF, Keilin SA, Papachristou GI, Chak A, Slivka A, Mullady D, Kushnir V, Buxbaum J, Keswani R, Gardner TB, Forbes N, Rastogi A, Ross A, Law J, Yachimski P, Chen YI, Barkun A, Smith ZL, Petersen B, Wang AY, Saltzman JR, Spitzer RL, Ordiah C, Spino C, Durkalski-Mauldin V; SVI Study Group. Indomethacin with or without prophylactic pancreatic stent placement to prevent pancreatitis after ERCP: a randomised non-inferiority trial. Lancet. 2024;403:450-458. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 85] [Article Influence: 42.5] [Reference Citation Analysis (2)] |
| 20. | Bai B, Wang S, Du Y, Li M, Huang Q, Liu S, Zhang C, Fang Y, Chen X, Hong J, Li Y, Xu Z, Liu X, Hong R, Bao J, Mei Q. Indomethacin Does Not Reduce Post-ERCP Pancreatitis in High-Risk Patients Receiving Pancreatic Stenting. Dig Dis Sci. 2024;69:3442-3449. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 8] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
| 21. | Jiang F, Zhang J, Hu Z. Risk factors for pancreatitis occurrence after gallstone treatment using endoscopic retrograde cholangiopancreatography. Afr Health Sci. 2023;23:231-238. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (1)] |
| 22. | Ignacio RC Jr, Kelley-Quon LI, Ourshalimian S, Padilla BE, Jensen AR, Shew SB, Lofberg KM, Smith CA, Roach JP, Pandya SR, Russell KW, Wang K; Western Pediatric Surgery Research Consortium Choledocholithiasis Investigative Group. Pediatric DUCT Score: A Highly Specific Predictive Model for Choledocholithiasis in Children. J Am Coll Surg. 2023;236:961-970. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 15] [Article Influence: 5.0] [Reference Citation Analysis (1)] |
| 23. | Yuan WH, Zhang Z, Pan Q, Mao BN, Yuan T. Risk factors for recurrence of common bile duct stones after surgical treatment and effect of ursodeoxycholic acid intervention. World J Gastrointest Surg. 2024;16:103-112. [PubMed] [DOI] [Full Text] |
| 24. | Wang Y, Wang J, Zhou T, Chen Z, Wang W, Liu B, Li Y. Investigating the potential mechanism and therapeutic effects of SLXG for cholesterol gallstone treatment. Phytomedicine. 2024;132:155886. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 25. | Li G, Pang Q, Zhai H, Zhang X, Dong Y, Li J, Jia X. SpyGlass-guided laser lithotripsy versus laparoscopic common bile duct exploration for large common bile duct stones: a non-inferiority trial. Surg Endosc. 2021;35:3723-3731. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 15] [Article Influence: 3.0] [Reference Citation Analysis (1)] |