Published online Mar 7, 2026. doi: 10.3748/wjg.v32.i9.114758
Revised: December 7, 2025
Accepted: January 4, 2026
Published online: March 7, 2026
Processing time: 153 Days and 2.3 Hours
Esophageal epiphrenic diverticulum (ED) often occurs in patients with esophageal motility disorders, and its incidence rate is approximately 3%-7% in achalasia (AC). A distinct septum has been observed in some patients with AC coexisting with ED during gastroscopy. Digestive endoscopic tunnel technique has emerged as a promising therapeutic approach for these patients.
To evaluate the therapeutic effectiveness of specific treatment methods for ED with septum (ED + S) or ED without septum (ED - S) in AC patients.
This retrospective cohort study included 31 patients with AC and esophageal diverticula (21 patients with septum and 10 patients without septum) between January 2016 and January 2025. In ED + S group, submucosal tunneling myotomy combined with diverticular septotomy was performed, while patients in the ED - S group underwent submucosal myotomy alone. The Eckardt scores before and after surgery were compared to evaluate symptom relief and clinical success. The Gastroesophageal Reflux Disease Questionnaire (GERD-Q) score and gastroscopy findings were used to evaluate postoperative gastroesophageal reflux.
The corresponding operation steps were completed in both groups, with a technical success rate of 100%. We successfully followed up with 18 and 10 patients in the ED + S and ED - S group, with a median follow-up period of 2.5 years and 3.0 years, respectively. The postoperative Eckardt scores [median (interquartile range)] were significantly lower in both groups compared with preoperative scores [ED + S group: 6.0 (4.0-8.0) vs 0 (0-2.0), P < 0.05; ED - S group: 6.0 (3.75-8.25) vs 1.0 (0-3.0), P < 0.05]. The clinical success rates (Eckardt score ≤ 3) were 88.9% and 90.0%, respectively. The GERD-Q score was used to evaluate postoperative gastroesophageal reflux, and 3 patients (3/18, 16.7%) in ED + S group and 2 patients (2/10, 20%) in ED - S group experienced symptomatic reflux (GERD-Q score ≥ 8).
In AC patients with ED + S, submucosal tunneling myotomy with diverticular septotomy can achieve good thera
Core Tip: Epiphrenic diverticulum (ED) often occurs in patients with esophageal motility disorders, with achalasia (AC) being the most common. During gastroscopy in patients with AC coexisting with ED, a distinct septum is sometimes observed, while it is absent in others. In response to this clinical situation, we conducted a retrospective study to evaluate the safety and effectiveness of specific treatment methods in different clinical scenarios. The study demonstrated that submucosal myotomy combined with diverticular septotomy offers good clinical outcomes for AC patients with ED and obvious septum, and peroral endoscopic myotomy is effective for AC patients without septum.
- Citation: Hao XW, Bi YW, Wang ZM, Niu XT, Xiang JY, Su S, Li LS, Linghu EQ, Chai NL. Simultaneous treatment of concomitant achalasia coexisting with epiphrenic diverticulum: The practice of submucosal tunneling technique. World J Gastroenterol 2026; 32(9): 114758
- URL: https://www.wjgnet.com/1007-9327/full/v32/i9/114758.htm
- DOI: https://dx.doi.org/10.3748/wjg.v32.i9.114758
Achalasia (AC) is an esophageal motility disorder characterized by loss of esophageal peristalsis and incomplete relaxation of the lower esophageal sphincter (LES), which leads to symptoms of dysphagia, regurgitation, chest pain, or weight loss[1]. Peroral endoscopic myotomy (POEM) is a minimally invasive method of myotomy first used clinically in 2010[2], which is a safe and effective option in the treatment of AC[3,4]. Approximately 3%-7% of patients with AC develop an epiphrenic diverticulum (ED)[5]. Epiphrenic diverticula are pulsion-type diverticula lacking a muscle layer usually located within 10 cm of the gastroesophageal junction (GEJ) in the distal esophagus[6]. AC with accompanying esophageal diverticula is usually managed surgically with laparoscopic Heller myotomy, anterior fundoplication, and diverticulectomy. However, complications are relatively frequent and severe, such as leaks and pneumonia[7,8].
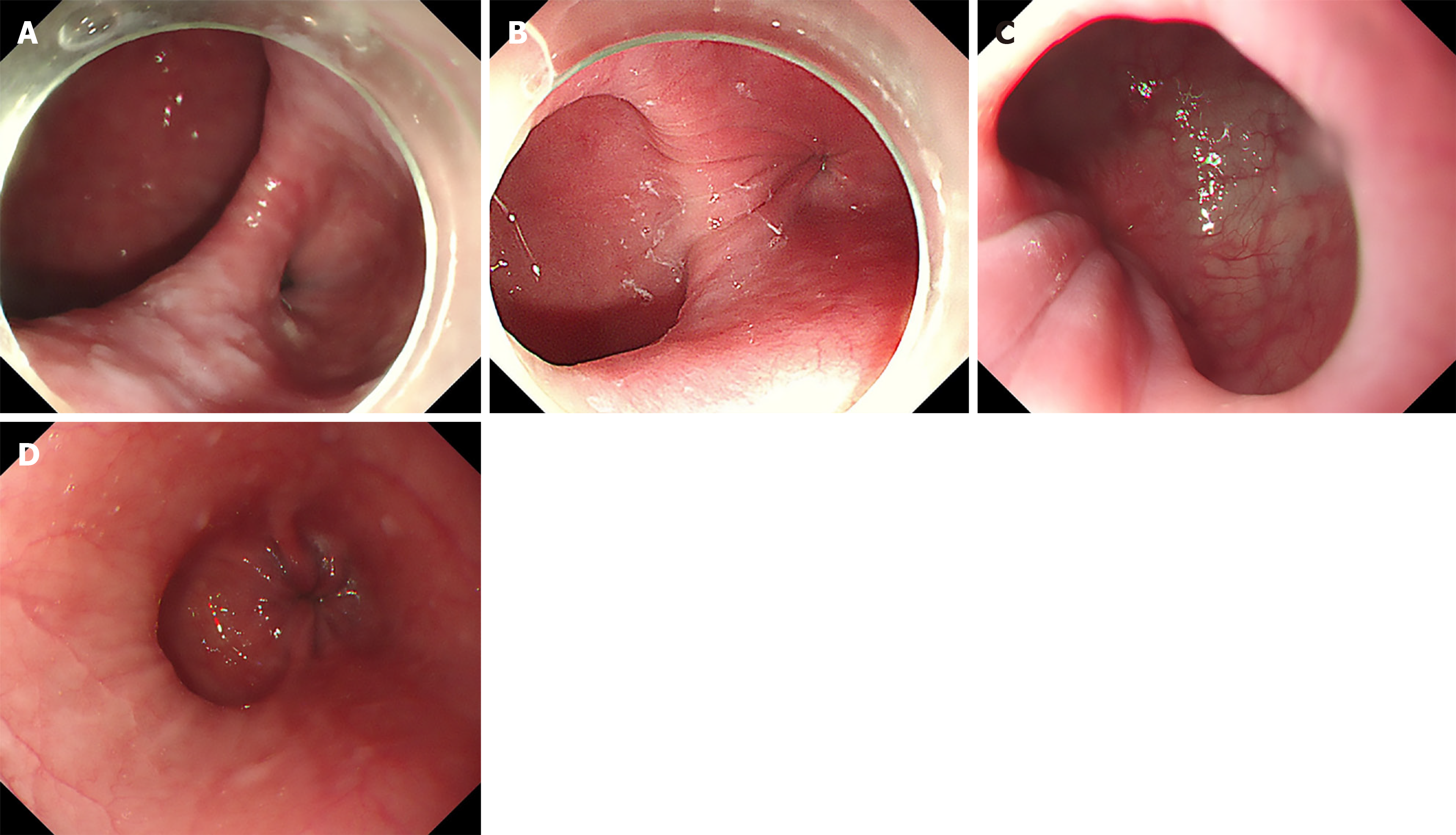
The advancement of digestive endoscopic tunneling techniques has provided new therapeutic options for ED. Although both myotomy alone and myotomy combined with septotomy are effective methods[9-14], there is currently no clinical guidance regarding the choice of surgical approach depending on the presence or absence of a septum. Based on the different presentations during gastroscopy, we categorized diverticula into two types: With or without septum (Figure 1). ED with septum (ED + S) are relatively distant from the cardia, and a distinct septum can be observed during gastroscopy when fully inflated. ED without septum (ED - S) are close to the cardia, and the lower edge of the diverticulum is located near the cardia. No obvious septum can be seen after full inflation during gastroscopy. The aim of this study was to evaluate safety and effectiveness of specific treatment methods for epiphrenic diverticula in different locations in AC patients. This will assist gastroenterologists in choosing treatment methods during the operation.
The data of AC patients who underwent POEM in our center between January 2016 and January 2025 were reviewed. Inclusion criteria were as follows: (1) Patients with ED + S who underwent myotomy combined with diverticular septo
Before the surgery, the presence of ED was determined using gastroscopy and a barium esophagram. Cases with severe dilatation and tortuous angulation of the esophageal body were excluded. The integrated relaxation pressure (IRP) and Chicago classification of AC were determined using high-resolution manometry (HRM). If the manometry catheter insertion into the stomach failed, the Chicago classification was based on the patterns of pressurization and contraction of the body of the esophagus on HRM. AC was diagnosed based on symptoms, HRM, endoscopic findings of retained saliva with a puckered GEJ or a barium meal showing a dilated esophagus with the bird beak sign. Other types of esophageal motility disorders, such as esophagogastric junction outlet obstruction, distal esophageal spasm, or jackhammer esophagus were excluded. Symptom severity was assessed using the Eckardt score with components for dysphagia, regurgitation, chest pain, and weight loss.
For patients with ED + S, technical success was defined as completion of all of the steps of POEM with septotomy, with complete septotomy achieved. For ED - S, technical success was defined as completion of all the steps of POEM. Clinical success was defined by an Eckardt score ≤ 3 without the use of additional treatments. Major adverse events were defined as conditions that resulted in vital sign instability, an intensive care unit stay or those that required other salvage procedures (such as surgery). Insufflation-related events requiring needle drainage, mucosal injuries requiring closure with titanium clips, and intra-procedural or post-procedural events leading to prolongation of hospital stay were considered as minor adverse events. The Gastroesophageal Reflux Disease Questionnaire (GERD-Q) score was used to evaluate postoperative gastroesophageal reflux, and GERD-Q score ≥ 8 was defined as symptomatic reflux.
All patients were required to fast for 48 hours before the operation, and endoscopy confirmed no food residue in the esophageal lumen.
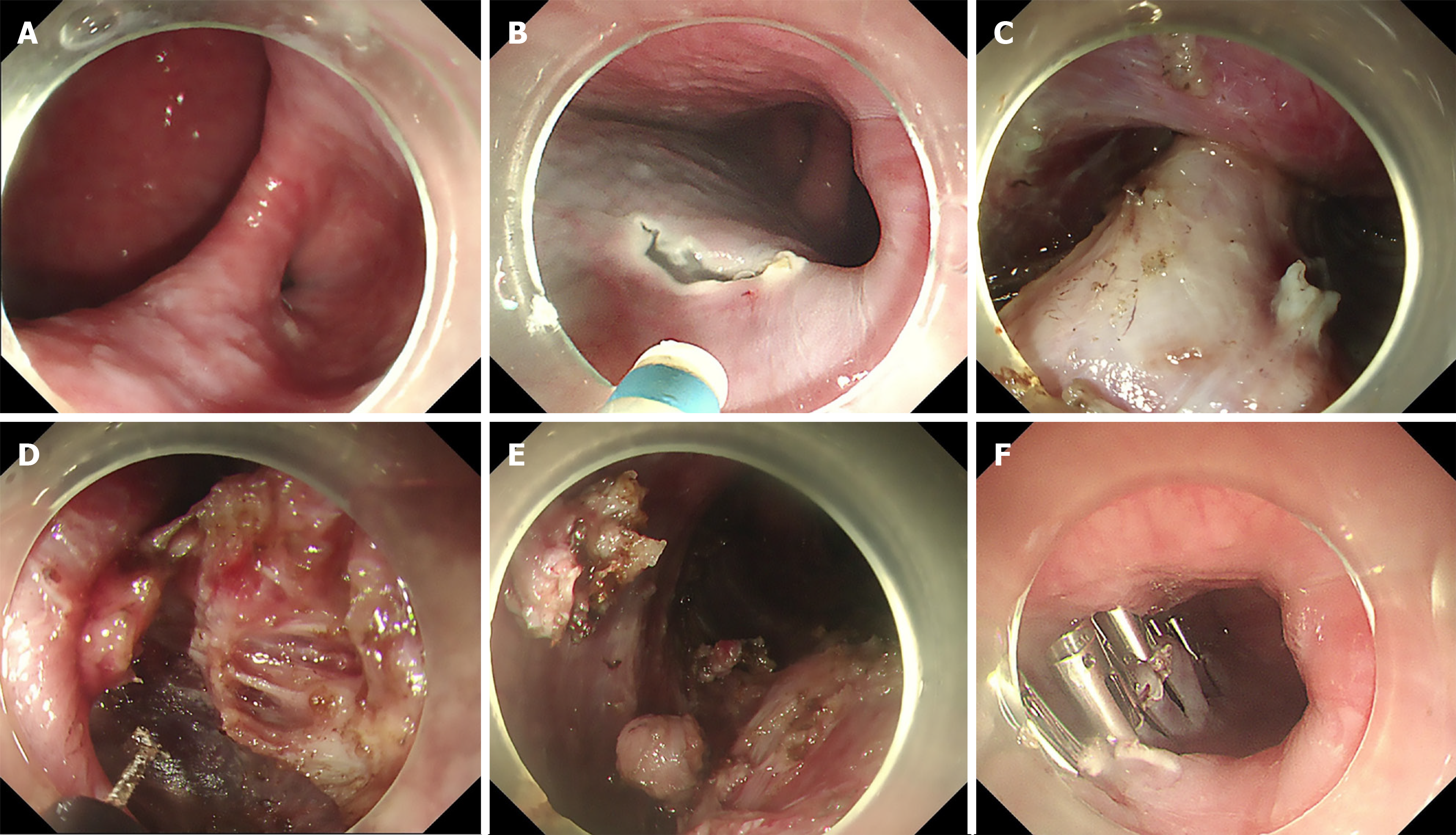
The POEM procedure with diverticular septotomy generally consisted of the following major steps (Figure 2). First, patients were placed in the supine position with the right shoulder raised. A submucosal injection of methylene blue saline solution (1:10000) was administered. Then, an inverted T-shaped mucosal incision was made approximately 2-3 cm above the proximal margin of the diverticulum. Submucosal dissection was performed in the posterior wall of the esophagus, and the septum between the esophageal lumen and the diverticulum was exposed. Submucosal tunneling was extended 2 cm beyond the GEJ. Subsequently, the muscle of the diverticulum septum was completely cut off, which lowered and flattened the ledge of the diverticulum. Then, myotomy was performed on the lower-esophageal sphincter and extended 2 cm into the stomach. Finally, after assuring hemostasis and verifying that the endoscope could easily pass the cardia, the mucosal incision was closed with clips.
For patients in ED - S group, the standard endoscopic submucosal myotomy technique was performed[15]. When the patient had received prior POEM therapy, the submucosal tunnel was created in an unscarred area to avoid the previous myotomy site.
Adequate extension of the submucosal tunnel across the GEJ was confirmed with a vascular pattern and visualization of the blanched gastric mucosa. Carbon dioxide gas was used for insufflation with a CO2 insufflator (UCR; Olympus) during procedures.
All patients continued to fast for 3 days after the procedure. A liquid diet was started for an additional day. Antibiotics and proton pump inhibitors (PPIs) were administered intravenously during the fasting period. An oral PPI was required for at least 4 weeks.
The Eckardt score, GERD-Q score, and postoperative complications to assess the severity of AC and gastroesophageal reflux symptoms were recorded in the outpatient clinic or obtained by telephone. To evaluate the LES pressure and acid exposure, endoscopy, HRM, and 24-hour esophageal pH monitoring were performed for at least 3 months after the operation, when possible.
Data were analyzed using IBM SPSS version 24.0 statistical software (IBM Corporation, Armonk, NY, United States). Continuous variables were presented as mean ± SD or median (interquartile range), and categorical variables were expressed as n (%). For normally distributed continuous data, statistical significance was assessed by the Student’s t test; for categorical data, significance was assessed by the χ2 test with Yates’ correction when appropriate or by the Fisher’s exact test; and for non-normally distributed continuous data, statistical significance was assessed by the Wilcoxon test. The multivariable linear regression analysis was performed to adjust for potential confounders. Statistical significance was set at an α level of 0.05 for two-tailed tests.
In total, 31 patients were enrolled in the study. Among these patients, 21 patients with ED + S underwent myotomy combined with diverticular septotomy and 10 patients with ED - S underwent myotomy. The demographic and clinical characteristics of the patients are summarized in Table 1. A formal comparative analysis was not performed between the two groups due to the study design and sample size.
| Characteristics | ED + S (n = 21) | ED - S (n = 10) |
| Age (years) | 50 (13-77) | 46.4 (19-77) |
| Sex | ||
| Male | 8 (38.1) | 4 (40.0) |
| Female | 13 (61.9) | 6 (60.0) |
| BMI (kg/m2) | 20.4 (15.6-26) | 22.1 (16.9-27.8) |
| Ling classification | ||
| Ling IIIR | 11 (52.4) | 5 (50.0) |
| Ling IIIL | 8 (38.1) | 3 (30.0) |
| Ling IIILR | 2 (9.5) | 2 (20.0) |
| EMIA classification | ||
| A | 7 (33.3) | 4 (40.0) |
| B | 9 (42.9) | 4 (40.0) |
| C | 3 (14.3) | 1 (10.0) |
| D | 2 (9.5) | 1 (10.0) |
| SMF classification | ||
| A0 | 2 (9.5) | 0 |
| A1 | 9 (42.9) | 2 (20.0) |
| A2 | 9 (42.9) | 7 (70.0) |
| A3 | 1 (4.7) | 1 (10.0) |
| Disease course (months) | 109 (1-360) | 208 (16-840) |
| Patients with prior treatment | ||
| Pneumatic balloon dilation | 2 (9.5) | 0 |
| Botulinum toxin injection | 2 (9.5) | 1 (10.0) |
| Per-oral endoscopic myotomy | 1 (4.7) | 2 (20.0) |
| Heller myotomy | 0 | 4 (40.0) |
| Chicago classification | ||
| Type I | 3 (14.3) | 7 (70.0) |
| Type II | 14 (66.7) | 3 (30.0) |
| Type III | 1 (4.7) | 0 |
| Missing | 3 (14.3) | 0 |
| IRP (mmHg) | 30.9 (13-58.2); n = 9 | 26.4 (16.7-36.0); n = 2 |
| 24-hour esophageal pH monitoring | ||
| Pathological reflux | 0 | 0 |
| Acid fluid retention | 3 (14.3) | 1 (10.0) |
| Normal | 9 (42.9) | 9 (90.0) |
| Missing | 9 (42.9) | 0 |
In ED + S group, the diverticulum was located on the right wall of the esophagus in 11 patients and on the left wall in 8 patients. There was a diverticulum in each of the right and left walls of the esophagus in 2 patients. The average disease course was 9.1 years (range, 1 month-30 years). Five patients (23.8%) had undergone prior treatments, including botulinum toxin injection, pneumatic balloon dilation, and POEM. HRM was performed in 18 patients, including 3 of Chicago I, 14 of Chicago II, and 1 of Chicago III. However, because of the presence of esophageal diverticulum, the manometry catheter insertion into the specified position failed after several attempts, LES parameters were only detected in 9 patients, with an average IRP of 30.9 (13-58.2).
In ED - S group, the diverticulum was located on the right wall of the esophagus in 5 patients and on the left wall in 3 patients. There was a diverticulum in each of the right and left walls of the esophagus in 2 patients. The average disease course was 17.3 years (range 16 month to 70 years). Seven patients (70.0%) had undergone prior treatments, including botulinum toxin injection, POEM, and Heller myotomy. HRM were performed in all patients, including 7 of Chicago I and 3 of Chicago II. For the same reason, LES parameters were successfully detected in only 2 patients, with an average IRP of 26.4 (16.7-36.0).
The procedure-related characteristics are summarized in Table 2. All procedures were successfully performed in both patient groups, with a clinical success rate of 100%. For the ED + S group and ED - S group, the mean procedure time was 61 minutes (range 26-123 minutes) and 58.4 minutes (range 22-128 minutes), respectively. The mean lengths of the tunnel and myotomy were 9.3 cm (range 6-13 cm) and 7.1 cm (range 5-10 cm) in ED + S group, while they were 9.7 cm (range 7-12 cm) and 7.0 cm (range 5-10 cm) in ED - S group, respectively. Progressive full-thickness myotomy was the most common type of myotomy in both groups (81% in ED + S group and 70.0% in ED - S group). The remaining patients underwent full-thickness myotomy, of which the tunnel length was ≤ 8 cm. Two patients (9.5%) exhibited mucosal injury in the ED + S cohort, which were closed with titanium clips and did not prolong the length of stay (LOS). Eight (38.1%) and five (50%) patients, respectively, had transient fever and an elevated hemogram after surgery, and their temperature returned to normal the next day after antibiotic treatment. No obvious gas-related adverse events occurred in either cohort.
| Characteristics | DE + S (n = 21) | DE - S (n = 10) |
| Technical success | 21 (100) | 10 (100) |
| Length of tunnel (cm) | 9.3 (6-13) | 9.7 (7-12) |
| Length of myotomy (cm) | 7.1 (5-10) | 7.0 (5-10) |
| Types of myotomy | ||
| Progressive full-thickness myotomy | 17 (81.0) | 7 (70.0) |
| Full-thickness myotomy | 4 (19.0) | 3 (30.0) |
| Distance from the cardia (cm) | 1.8 (1-5) | 0 |
| Procedure time (minutes) | 61 (26-123) | 58.4 (22-128) |
| Hospital stays after operation (days) | 6.8 (4-11) | 7.0 (4-12) |
| Complications | ||
| Mucosa injury | 2 (9.5) | 0 |
| Gas-related adverse event | 0 | 0 |
| Bleeding | 0 | 0 |
We successfully followed up with 28 patients (18 patients in ED + S group and 10 patients in ED - S group). Of the 3 patients who were lost to follow-up, 2 patients could not be contacted due to a changed telephone number, and 1 patient was unable to access follow-up data because of mental illness.
For the ED + S group, the median follow-up period was 2.5 years (range, 3 months-8.6 years). The Eckardt score after the median 2.5-year follow-up was significantly lower than that before surgery [6.0 (4.0-8.0) vs 0 (0-2.0); P < 0.05]. Considering a post-operative Eckardt score of ≤ 3 as successful treatment, 16 patients achieved clinical success (success rate: 88.9%). For the ED - S group, the median follow-up period was 3.0 years (range, 4 months-9.1 years). The Eckardt score after the median 3.0-year follow-up was also significantly lower than that before surgery [6.0 (3.75-8.25) vs 1.0 (0-3.0); P < 0.05]. Nine patients achieved clinical success (success rate: 90.0%).
Patients who did not achieve clinical success had lower Eckardt scores and less severe dysphagia than before surgery. The comparison of preoperative and postoperative Eckardt scores of each group are summarized in Tables 3 and 4. The results of the multivariable linear regression analysis are presented in Supplementary Tables 1 and 2. Factors such as body mass index, duration of symptoms, prior treatments, and Chicago classification did not significantly affect POEM outcomes (P > 0.05).
| Eckardt score (n = 18) | Pre-operation | Post-operation | P value |
| Dysphagia | 3.0 (1.75-3.0) | 0 (0-1.0) | < 0.05 |
| Chest pain | 0 (0-0.25) | 0 (0-0) | 0.083 |
| Regurgitation | 2.0 (1.0-3.0) | 0 (0-1.0) | < 0.05 |
| Weight loss | 1.0 (0-3.0) | 0 (0-0) | < 0.05 |
| Eckardt score | 6.0 (4.0-8.0) | 0(0-2.0) | < 0.05 |
| Eckardt score (n =10) | Pre-operation | Post-operation | P value |
| Dysphagia | 2.5 (2.0-3.0) | 1.0 (0-1.25) | < 0.05 |
| Chest pain | 1.0 (0-1.0) | 0 (0-0.25) | < 0.05 |
| Regurgitation | 1.5 (0-2.0) | 0 (0-1.0) | < 0.05 |
| Weight loss | 2.5 (0.75-3.0) | 0 (0-0) | < 0.05 |
| Eckardt score | 6.0 (3.75-8.25) | 1.0 (0-3.0) | < 0.05 |
Gastroesophageal reflux disease is the most common adverse event after POEM treatment. Reflux esophagitis is typically identified on endoscopy and assessed using the Los Angeles classification. We used the GERD-Q score to evaluate postoperative gastroesophageal reflux, and GERD-Q score ≥ 8 was defined as symptomatic reflux. In the ED + S group, 3 patients (3/18, 16.7%) experienced symptomatic reflux. Four of 6 patients (66.7%) who underwent gastroscopy after the procedure showed reflux esophagitis (3 Los Angeles type A, 1 Los Angeles type B). In the ED - S group, 2 patients (2/10, 20.0%) experienced symptomatic reflux. Two of 5 patients (40%) who underwent gastroscopy after the procedure showed reflux esophagitis (1 Los Angeles type A, 1 Los Angeles type C). All patients were managed with medical therapy. Table 5 summarizes the details of postoperative gastroesophageal reflux.
| Clinical reflux evaluation | ED + S (n = 18) | ED - S (n = 10) |
| GERD-Q score | ||
| ≥ 8 | 3 (16.7) | 2 (20.0) |
| < 8 | 15 (83.3) | 8 (80.0) |
| Endoscopic monitoring | n = 6 | n = 5 |
| Reflux esophagitis by gastroscopy | 4 (66.7) | 1 (20.0) |
| LA-A | 3 (50) | 0 |
| LA-B | 1 (16.7) | 0 |
| LA-C | 0 | 1 (20.0) |
Epiphrenic diverticula are pulsion-type diverticula that often occur in patients with esophageal motility disorders. Recent studies have shown that approximately 75%-100% of patients with ED have esophageal motility disorders, with AC being the most common[16]. In patients with AC, owing to the increased LES pressure, prolonged food retention in the lower esophagus leads to protrusion of the mucosal and submucosal layers outward toward the muscle layers, which could cause ED.
With the development of digestive endoscopic tunneling techniques, the adoption of submucosal tunneling septotomy by diverticular POEM (D-POEM) has grown since its first proposed use for Zenker diverticulum[17]. Subsequently, D-POEM has gradually been adopted in the treatment of esophageal diverticulum, as it yields a greater curative effect and fewer postoperative complications[18-21]. However, this method only divided the septum but did not manage the increased LES pressure. In patients with AC combined with ED, only diverticular endoscopic septotomy (D-POEM) without LES myotomy may be less effective.
Therefore, in 2016, POEM combined with diverticular septotomy was first reported in the treatment of AC with esophageal diverticulum[13]. Significant symptom resolution was observed without obvious complications. Nabi et al[22] also demonstrated that this procedure is effective in cases with ED. Reports have shown successful treatment with myotomy alone, in which endoscopic myotomy of the side opposite to the diverticulum is performed without septotomy[14,23,24]. Shrigiriwar et al[25] reported the largest cohort to date in their multicenter retrospective study of 85 patients with ED and an underlying motility disorder. Patients underwent POEM with or without septotomy, and the use of septum incision did not affect safety or effectiveness.
During gastroscopy, we have found that some EDs are accompanied by a distinct septum, while others are not. In response to this clinical situation, we conducted a retrospective study to assist endoscopists in making clinical decisions. We included 31 patients with AC and ED (21 in ED + S group and 10 in ED - S group). Patients with ED + S underwent myotomy combined with diverticular septotomy, and patients with ED - S underwent myotomy alone. Both procedures were performed through a single submucosal tunnel. Twenty-eight patients were successfully followed up over a median follow-up period of more than 2 years. Symptoms such as dysphagia were significantly resolved after surgery, and the Eckardt score was significantly lower than that before the procedure (P < 0.05) in both groups. The follow-up data demonstrated that symptomatic relief was primarily driven by marked improvements in dysphagia and regurgitation, while chest pain showed a non-significant trend towards improvement. This finding may be attributed to both low pre-operative scores for chest pain and the limited sample size. Patients who failed to achieve clinical success (Eckardt score > 3) complained that they were unable to consume liquid food or even drink water before operation. Although dysphagia symptoms were present at every meal after the operation, they were significantly alleviated compared to the preoperative period. We did not compare the efficacy of the two treatment methods. Instead, we evaluated the safety and effectiveness of specific treatment methods in different clinical scenarios. We hope these findings can guide endoscopists in selecting the appropriate treatment strategy during endoscopic interventions.
For ED + S patients, our research holds a positive attitude towards the treatment of diverticular septum. The presence of the diverticular ridge may hinder the passage of food through the cardia, and food is more likely to be retained in the diverticular. Prolonged food retention can lead to adverse events, such as mucosal inflammation and acid fermentation, and it can even increase the risk of esophageal cancer. Moreover, while establishing the submucosal tunnel, only the diverticular septum needs to be additionally exposed, without significantly increasing the submucosal dissection area, adding significant procedural time or risk of adverse events. Ultimately, simultaneous treatment of LES and diverticular septum within the same submucosal tunnel was achieved. Therefore, in patients with diverticular septum, submucosal myotomy combined with diverticular septotomy can achieve good therapeutic effects.
Dilation of a distal segment of the esophagus was observed to form a pseudo-diverticulum structure in patients with recurrent symptoms after myotomy, which is referred to as blown-out myotomy (BOM)[26]. BOM is defined as a distal wide-mouthed (> 2 cm) diverticulum in the area of the previous myotomy with > 50% increase in esophageal diameter[27]. The pressure of bolus retention on the esophageal wall, which leads to increased strain and deformation, may cause diverticulum formation. The underlying mechanism is related to persistently elevated LES pressure and localized weakening caused by insufficient myotomy. It has been demonstrated that salvage POEM could be an effective treatment option for patients with symptomatic BOM[28]. In our study, Heller myotomy or POEM was previously performed in 60% of patients in the ED - S group and only 4.7% of patients in the ED + S group (P = 0.002). We hypothesize that this may be due to the myotomy extending approximately 2 cm below the cardia in patients who have previously undergone myotomy, leading to inherent weakness of the muscular layer at the GEJ. When intraluminal pressure increases proximally due to residual outflow resistance or hypercontractile activity, the mucosa at the cardia herniates through the weakened wall[29], forming a diverticulum without an intercostal septum. However, the exact mechanism requires further investigation. Whether it is a BOM or primary diverticulum without septum, pathologically they are both pseudo-diverticulum lacking the muscular layer. A primary reason for diverticulum formation is the high LES pressure, causing herniation of the mucosal and submucosal layers. Therefore, POEM to reduce LES pressure is an effective option for these patients.
One patient in the ED + S group had a preoperative Eckardt score of 0 and was admitted to our hospital for severe belching with asphyxia. HRM revealed Chicago III with an IRP of 26, and barium meal examination showed a large diverticulum in the right wall of the esophagus and bird’s beak sign. After surgery, the symptoms of belching and asphyxia significantly improved.
The GERD-Q score showed that 16.7% (3/18) and 20% (2/10) of patients had postoperative gastroesophageal reflux symptoms respectively, and these could be controlled with PPIs in all patients. Postoperative gastroscopy was performed in 33.3% (6/18) and 50% (5/10) of patients in the ED + S group and ED - S group, respectively. During the follow-up period, many patients refused regular invasive examinations such as endoscopy, HRM, and 24-hour esophageal pH monitoring because of the absence of clinical symptoms such as dysphagia and acid reflux. The 66.7% and 20% patients who underwent postoperative gastroscopy experienced reflux esophagitis. Unfortunately, not all patients in our cohort underwent postoperative endoscopy or 24-hour pH monitoring for the assessment of gastroesophageal reflux, as some cases of reflux following POEM can be asymptomatic[30], which also suggests the necessity to perform endoscopic monitoring after POEM.
Previous literature suggests that 24.5% of patients with combined BOM experience increasing esophageal acid exposure, specifically related to delayed reflux clearance in the diverticulum[26]. All 6 patients in the ED - S group with prior myotomy underwent preoperative 24-hour esophageal pH monitoring, one of whom (patient A) demonstrated acidic food retention. Regrettably, postoperative pH monitoring was performed in only one patient (patient B) following salvage POEM, and the results indicated newly emerged acidic food retention. Notably, none of the patients reported reflux symptoms. These findings underscore the necessity of timely endoscopic reevaluation and pH monitoring during follow-up. Furthermore, for patients with diverticula and a history of myotomy, the choice of myotomy length and method during reintervention is also crucial. However, due to the small sample size, we did not explore this in greater detail, and we anticipate further studies to clarify the optimal management strategy.
Our study has some limitations. First, this is a single-center retrospective study with a small sample size and the potential for selection bias. Second, the effectiveness of the surgery was compared only using preoperative and postoperative Eckardt scores without objective physiological measures (post-operative IRP data). Third, postoperative esophageal manometry and 24-hour pH monitoring were not performed in all patients. The GERD-Q score does not fully reflect the postoperative reflux status. Multicenter studies with larger sample sizes are needed to further validate our results.
In AC patients with ED + S, submucosal tunneling myotomy combined with diverticular septotomy can achieve good therapeutic effects. When ED is close to the cardia and there is no obvious septum, submucosal tunneling myotomy can reduce LES pressure.
We sincerely thank the endoscopy team of the First Medical Center of Chinese PLA General Hospital for their professional expertise and continuous support throughout the data collection and clinical implementation stages of this research.
| 1. | Vaezi MF, Pandolfino JE, Yadlapati RH, Greer KB, Kavitt RT. ACG Clinical Guidelines: Diagnosis and Management of Achalasia. Am J Gastroenterol. 2020;115:1393-1411. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 397] [Cited by in RCA: 304] [Article Influence: 50.7] [Reference Citation Analysis (0)] |
| 2. | Werner YB, Hakanson B, Martinek J, Repici A, von Rahden BHA, Bredenoord AJ, Bisschops R, Messmann H, Vollberg MC, Noder T, Kersten JF, Mann O, Izbicki J, Pazdro A, Fumagalli U, Rosati R, Germer CT, Schijven MP, Emmermann A, von Renteln D, Fockens P, Boeckxstaens G, Rösch T. Endoscopic or Surgical Myotomy in Patients with Idiopathic Achalasia. N Engl J Med. 2019;381:2219-2229. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 467] [Cited by in RCA: 381] [Article Influence: 54.4] [Reference Citation Analysis (0)] |
| 3. | de Moura ETH, Jukemura J, Ribeiro IB, Farias GFA, de Almeida Delgado AA, Coutinho LMA, de Moura DTH, Aissar Sallum RA, Nasi A, Sánchez-Luna SA, Sakai P, de Moura EGH. Peroral endoscopic myotomy vs laparoscopic myotomy and partial fundoplication for esophageal achalasia: A single-center randomized controlled trial. World J Gastroenterol. 2022;28:4875-4889. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 18] [Cited by in RCA: 19] [Article Influence: 4.8] [Reference Citation Analysis (3)] |
| 4. | Shiwaku H, Inoue H, Sato H, Onimaru M, Minami H, Tanaka S, Sato C, Ogawa R, Okushima N, Yokomichi H. Peroral endoscopic myotomy for achalasia: a prospective multicenter study in Japan. Gastrointest Endosc. 2020;91:1037-1044. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 72] [Article Influence: 12.0] [Reference Citation Analysis (0)] |
| 5. | Nadaleto BF, Herbella FAM, Patti MG. Treatment of Achalasia and Epiphrenic Diverticulum. World J Surg. 2022;46:1547-1553. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 12] [Reference Citation Analysis (0)] |
| 6. | Sato H, Takeuchi M, Hashimoto S, Mizuno KI, Furukawa K, Sato A, Yokoyama J, Terai S. Esophageal diverticulum: New perspectives in the era of minimally invasive endoscopic treatment. World J Gastroenterol. 2019;25:1457-1464. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 54] [Cited by in RCA: 50] [Article Influence: 7.1] [Reference Citation Analysis (5)] |
| 7. | Westcott CJ, O'Connor S, Preiss JE, Patti MG, Farrell TM. Myotomy-First Approach to Epiphrenic Esophageal Diverticula. J Laparoendosc Adv Surg Tech A. 2019;29:726-729. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 9] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 8. | Bowman TA, Sadowitz BD, Ross SB, Boland A, Luberice K, Rosemurgy AS. Heller myotomy with esophageal diverticulectomy: an operation in need of improvement. Surg Endosc. 2016;30:3279-3288. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 9. | Li W, Liu F, Wu L. Peroral endoscopic myotomy and simultaneous endoscopic diverticuloseptotomy in a case of achalasia with diverticula. Endoscopy. 2020;52:E168-E169. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 10. | Lian J, Xu A, Chen T, Xu M. Kill two birds with one stone: one submucosal tunnel for achalasia combined with large epiphrenic diverticulum. Endoscopy. 2023;55:E1073-E1074. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 11. | Bhalla S, Reddy CA, Watts L, Chang AC, Law R. Greater-curvature peroral endoscopic myotomy with diverticuloseptotomy for the treatment of achalasia in a patient with a large epiphrenic diverticulum. VideoGIE. 2020;5:77-79. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 12. | Basile P, Gonzalez JM, Le Mouel JP, Irarrazaval R, Caillo L, Barthet M. Per-oral endoscopic myotomy with septotomy for the treatment of distal esophageal diverticula (D-POEM). Surg Endosc. 2020;34:2321-2325. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 29] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 13. | Chai N, Linghu E, Zhang X, Yao G, Niu X. Simultaneous performance of one-tunnel per-oral endoscopic myotomy, submucosal tunneling endoscopic resection, and diverticulotomy. Gastrointest Endosc. 2016;84:846-847. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 5] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 14. | Kinoshita M, Tanaka S, Kawara F, Sakaguchi H, Abe H, Ariyoshi R, Toyonaga T, Kodama Y. Peroral endoscopic myotomy alone is effective for esophageal motility disorders and esophageal epiphrenic diverticulum: a retrospective single-center study. Surg Endosc. 2020;34:5447-5454. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 28] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 15. | Inoue H, Minami H, Kobayashi Y, Sato Y, Kaga M, Suzuki M, Satodate H, Odaka N, Itoh H, Kudo S. Peroral endoscopic myotomy (POEM) for esophageal achalasia. Endoscopy. 2010;42:265-271. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1502] [Cited by in RCA: 1250] [Article Influence: 78.1] [Reference Citation Analysis (0)] |
| 16. | Soares R, Herbella FA, Prachand VN, Ferguson MK, Patti MG. Epiphrenic diverticulum of the esophagus. From pathophysiology to treatment. J Gastrointest Surg. 2010;14:2009-2015. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 98] [Cited by in RCA: 64] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 17. | Li QL, Chen WF, Zhang XC, Cai MY, Zhang YQ, Hu JW, He MJ, Yao LQ, Zhou PH, Xu MD. Submucosal Tunneling Endoscopic Septum Division: A Novel Technique for Treating Zenker's Diverticulum. Gastroenterology. 2016;151:1071-1074. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 135] [Cited by in RCA: 110] [Article Influence: 11.0] [Reference Citation Analysis (0)] |
| 18. | Yang J, Zeng X, Yuan X, Chang K, Sanaei O, Fayad L, Kumbhari V, Singh V, Kalloo AN, Hu B, Khashab MA. An international study on the use of peroral endoscopic myotomy (POEM) in the management of esophageal diverticula: the first multicenter D-POEM experience. Endoscopy. 2019;51:346-349. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 91] [Cited by in RCA: 83] [Article Influence: 11.9] [Reference Citation Analysis (13)] |
| 19. | Maydeo A, Patil GK, Dalal A. Operative technical tricks and 12-month outcomes of diverticular peroral endoscopic myotomy (D-POEM) in patients with symptomatic esophageal diverticula. Endoscopy. 2019;51:1136-1140. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 41] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 20. | Zeng X, Bai S, Zhang Y, Ye L, Yuan X, Hu B. Peroral endoscopic myotomy for the treatment of esophageal diverticulum: an experience in China. Surg Endosc. 2021;35:1990-1996. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 24] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 21. | Ren L, Ye H, Zhu Y, Xie W, Liang Y, Liu Y, Dong J, Chen W, Chen X, Wang B, Pan L, Shi R. Diverticular peroral endoscopic myotomy (D-POEM) for symptomatic oesophageal diverticulum: a multicentre cohort study with a minimum follow-up of 3 years. Surg Endosc. 2024;38:253-259. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 8] [Article Influence: 4.0] [Reference Citation Analysis (1)] |
| 22. | Nabi Z, Chavan R, Asif S, Ramchandani M, Basha J, Darisetty S, Goud R, Kotla R, Reddy DN. Per-oral Endoscopic Myotomy with Division of Septum (D-POEM) in Epiphrenic Esophageal Diverticula: Outcomes at a Median Follow-Up of Two Years. Dysphagia. 2022;37:839-847. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 22] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 23. | Demeter M, Bánovčin P Jr, Ďuriček M, Kunda R, Hyrdel R. Peroral endoscopic myotomy in achalasia and large epiphrenic diverticulum. Dig Endosc. 2018;30:260-262. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 25] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 24. | Demeter M, Ďuriček M, Vorčák M, Hyrdel R, Kunda R, Bánovčin P. S-POEM in treatment of achalasia and esophageal epiphrenic diverticula - single center experience. Scand J Gastroenterol. 2020;55:509-514. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 22] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 25. | Shrigiriwar A, Mony S, Fayyaz F, Onimaru M, Monachese M, Zhang L, Corre F, Azmeera P, Wu H, Wu CCH, Choi K, Gandhi A, Chalikonda D, Keane MG, Ghandour B, Villamarin-Corrales J, Schlachterman A, Tinto RR, Arévalo FE, Arbizu EA, Bapaye A, Velanovich V, Nieto J, Pawa R, Pawa S, Samanta J, Sedarat A, Eleftheriadis N, Saxena P, Bechara R, Al-Haddad MA, Familiari P, Ujiki M, Ramchandani M, Barret M, Chang K, Moll F, Pioche M, Inoue H, Khashab M. Clinical outcomes of peroral endoscopic myotomy with and without septotomy for management of epiphrenic diverticula: an international multicenter experience (with video). Gastrointest Endosc. 2024;100:840-848. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 5] [Article Influence: 2.5] [Reference Citation Analysis (1)] |
| 26. | Kuipers T, Ponds FA, Fockens P, Bastiaansen BAJ, Pandolfino JE, Bredenoord AJ. Focal Distal Esophageal Dilation (Blown-Out Myotomy) After Achalasia Treatment: Prevalence and Associated Symptoms. Am J Gastroenterol. 2024;119:1983-1989. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 14] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 27. | Triggs JR, Krause AJ, Carlson DA, Donnan EN, Campagna RAJ, Jain AS, Kahrilas PJ, Hungness ES, Pandolfino JE. Blown-out myotomy: an adverse event of laparoscopic Heller myotomy and peroral endoscopic myotomy for achalasia. Gastrointest Endosc. 2021;93:861-868. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 49] [Article Influence: 9.8] [Reference Citation Analysis (0)] |
| 28. | Zhang ZC, Xu JQ, Pan HT, Liu XY, Chen SY, Zhong YS, Zhang YQ, Ma LL, Hu JW, Cai MY, Qin WZ, Li QL, Chen WF, Zhou PH. Peroral endoscopic myotomy for symptomatic blown-out myotomy following previous myotomy for achalasia. Endoscopy. 2025;57:876-882. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 29. | Nabi Z, Aggarwal M, Inavolu P, Reddy DN. Blown-out myotomy: emerging phenotype in post-myotomy failure after POEM and Heller myotomy. Esophagus. 2025;. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 30. | Repici A, Fuccio L, Maselli R, Mazza F, Correale L, Mandolesi D, Bellisario C, Sethi A, Khashab MA, Rösch T, Hassan C. GERD after per-oral endoscopic myotomy as compared with Heller's myotomy with fundoplication: a systematic review with meta-analysis. Gastrointest Endosc. 2018;87:934-943. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 251] [Cited by in RCA: 204] [Article Influence: 25.5] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/