TO THE EDITOR
Hepatocellular carcinoma (HCC) is a significant health concern as it constitutes the seventh most common cancer and the third leading cause of cancer-related deaths worldwide[1]. According to the Barcelona Clinic Liver Cancer criteria, the treatment approach for a patient with HCC in the context of liver cirrhosis depends on the tumor burden, the severity of the underlying liver disease, and the patient’s overall performance status[2]. In cases of early-stage HCC, characterized by either a single tumor sized > 2 cm to ≤ 5 cm or up to three tumors no larger than 3 cm each, in a patient with a good performance status, preserved liver function, and no microvascular invasion or extrahepatic metastases, the recommended treatment options include liver resection, percutaneous ablation, and liver transplantation, as these interventions may offer potentially curative outcomes[2]. While liver transplantation is considered the optimal choice, as it addresses both HCC and the underlying cirrhosis, the shortage of suitable liver donors and the requirement for specialized medical centers can make this procedure challenging. As a result, most patients with early HCC are treated through surgical resection (SR) or ablation.
ADDRESSING KEY FEATURES THAT INFLUENCE TREATMENT’S OUTCOMES
To date, studies have yielded conflicting results regarding which of these two procedures is superior in treating early HCC. In a 2012 study, Peng et al[3] did not find a statistically significant difference between radiofrequency ablation (RFA) and SR in disease-free survival (DFS). However, patients in the RFA group had significantly better overall survival (OS) and fewer major complications. Interestingly, in the sub-analysis, the authors demonstrated that RFA outperformed SR in OS among patients with central HCCs located at least 3 cm from the liver capsule. In contrast, for peripheral HCCs, the two methods appeared to be equivalent, highlighting the importance of HCC location in treatment decision-making[3]. In accordance with the above, Kang et al[4] demonstrated that in small HCCs located in the left lateral liver segments, SR was associated with a trend toward better OS than RFA (94.4% vs 80.0%, P = 0.075). Moreover, DFS was higher in the former group, with 1-year, 3-year, and 5-year DFS rates of 100%, 84.5%, and 74.4%, respectively, vs 86.9%, 40.2%, and 33.4% in the RFA group (P < 0.001 for all comparisons). According to the above findings, it appears that RFA provides better results when applied to central HCCs, likely because these tumors are surrounded by sufficient liver tissue, allowing for greater peritumoral necrosis, which in turn limits recurrence rates. On the other hand, in peripheral HCCs with limited peri-tumoral margins, SR might ensure higher rates of complete tumor removal, decreasing the possibility of recurrence. The importance of HCC location in patients’ outcomes has also been established, even among patients who are exclusively treated with SR. Sakuraoka et al[5] recently showed that left-sided HCCs treated with SR have a poorer prognosis than the right-sided ones. Specifically, the 5-year OS and DFS rates were 49.5% and 19.1% in the left-sided group, and 55.6% and 24.5% in the right-sided group, respectively (P = 0.026). These results emphasize the importance of achieving adequate tumor-free margins to improve patients’ prognosis, regardless of the invasive procedure used[5]. The superiority of RFA vs SR in the treatment of early HCCs, as reported by Peng et al[3], was not confirmed by other investigators. Hence, Song et al[6] did not find any differences in 1-year, 3-year, and 5-year OS and DFS between the two methods. Additionally, Hu et al[7] reported, in a recent meta-analysis of 36 studies, that SR was associated with greater OS and DFS than RFA in patients with early-stage HCC. Similar findings were observed in the meta-analysis of Chen et al[8], where SR was associated with a significantly higher 3-year OS (risk ratio = 1.14, 95%CI: 1.08-1.20, P < 0.00001), along with higher 1- and 3-year DFS compared to RFA in patients with small HCCs, even though the 1-year OS did not differ between the two groups. In addition, SR was associated with a significantly lower local and intrahepatic distant recurrence rate compared to RFA. On the other hand, RFA was associated with a lower incidence of postoperative complications, including the development of ascites, and a shorter hospital stay[8]. It seems that differences in patients’ OS treated with RFA or SR for small HCCs below 3 cm reported in studies are not attributable to variations in liver function among the participants as assessed by the Child-Pugh score. Hatanaka et al[9] recently demonstrated no significant difference in OS between the two treatment methods, even when patients with more borderline liver function (Child-Pugh B) were included. The authors described similar OS for both 41 and 456 Child-Pugh B patients who underwent SR and RFA, employing an inverse probability of treatment weighting analysis to support their findings[9]. The discrepancy observed across the studies appears to be partially attributable to differences in liver tumor size. While early HCCs are considered “small”, typically less than 3 cm or less than 5 cm, the exact size within this range matters. For instance, Peng et al[3] enrolled patients with HCC measuring approximately 2 cm, for which RFA is more efficient than in tumors of larger size. By contrast, Song et al[6] included many patients with HCCs 3-5 cm (20% in the RFA group). The significance of tumor size in treatment response and recurrence rates was established in the sensitivity analysis of Hu et al’s study[7]. According to this analysis, the subgroup of patients in the Barcelona Clinic Liver Cancer 0 stage (very early HCC, smaller than 2 cm) had similar OS and DFS regardless of whether RFA or SR was chosen. However, when the tumor size increased to 3 cm, SR provided better DFS than RFA, although the difference in OS was not significant. Improved results in the RFA group, with OS and DFS comparable to SR, were achieved when the ablation margin exceeded 1 cm. However, when the ablation margins were close to or slightly larger than 0.5 cm, RFA yielded inferior OS compared with SR. As the tumor grows, the likelihood of achieving sufficient ablation margins with RFA declines, and the risk of poorer outcomes increases[7]. Another critical issue that appears to affect the outcome is the type of ablation modality used. Radosevic et al[10], in a randomized controlled trial (RCT), showed that significantly larger ablation zones were obtained when microwave ablation (MWA) was performed instead of RFA (P = 0.036). Sugimoto et al[11] recently confirmed the superiority of MWA in tumors up to 4 cm, reporting lower rates of local tumor progression compared to RFA at 2-year follow-up (risk ratio = 0.54; P = 0.007). While no significant difference in OS was observed between the two methods, likely due to the short follow-up period, the apparent effectiveness of MWA over RFA in generating larger ablation zones and reducing local tumor progression rates suggests that MWA may emerge as the preferred ablation technique in the future. Except for the ablation modality, the technique used to access the tumor is crucial. Ablation guided by contrast-enhanced ultrasonography (CEUS), computer tomography, or magnetic resonance imaging appears to be technically more feasible and effective compared to a conventional ultrasound-guided procedure, as tumor visibility is enhanced[12]. In contrast to RFA, in SR, the surgical technique applied does not appear to affect patient outcomes, as research has shown equal results between robotic, laparoscopic, or open approaches concerning overall complications, recurrence rates, recurrence-free survival, or OS in patients treated for very early or early HCC[13-15].
THE LANDSCAPE IS BECOMING CLEARER, BUT SEVERAL ISSUES STILL NEED TO BE ADDRESSED
I read the study by Lei et al[16], published in the current issue of the World Journal of Gastroenterology, aimed to clarify further which treatment, SR or RFA, is more effective for small HCCs. Most patients included in the study (over 90%) had a single tumor, with an average HCC size of around 3 cm in both treatment groups. The only surgical technique used was laparoscopic resection, while RFA was performed with the assistance of CEUS. A critical aspect of the RFA procedure involved the goal of completely eradicating the tumor. This was achieved by employing CEUS not only for preoperative lesion mapping but also during the operation. If any residual tumor or suspected remnants were identified during the procedure, additional ablation was carried out[16]. The authors found that SR was more frequently associated with intra- and postoperative complications, including greater blood loss, a higher need for blood transfusion, biliary fistula, pleural effusion, and intra-abdominal infection, which were accompanied by more extended hospital stays and higher hospitalization costs. Nevertheless, SR was associated with better 3-year OS and DFS, indicating that if a patient overcomes post-surgical complications, long-term outcome will be more favorable than that provided by RFA. Notably, the multivariate analysis revealed that the use of SR, a platelet count lower than 125.42 × 109/L, and a tumor size of up to 2.84 cm were independently associated with better DFS. At the same time, SR was the only independent predictor of OS[16]. In addition to the significant data mentioned above, the study by Lei et al[16] has some limitations. Firstly, all the results were derived from a single center, following center-specific practice patterns. Secondly, this was a retrospective study, which may have introduced selection bias, as the decision between RFA and SR was made on clinical judgment and patient-specific factors rather than by randomization. Thirdly, data obtained from patients undergoing SR or RFA covered a three-year period, from 2022 to 2025[16]. Over such an extended interval, operator experience is typically expected to improve and become more successful. Additionally, surgical procedures and protocols continue to evolve with the emergence of more minimally invasive techniques and more efficient ablation tools. Therefore, patients treated by either SR or RFA in 2025 have theoretically been treated more properly than those treated in 2022[17]. Furthermore, MWA, which is supposedly more effective than RFA, was not utilized. Tumor recurrence often results from microscopic disease in the surrounding area, microvascular invasion, and the formation of satellite micronodules[18]. Compared to RFA, SR may be more effective at completely removing these areas of concern, as it allows removal of a healthy tissue margin along with the primary tumor. In contrast, RFA cannot eliminate disease beyond the ablation zone, particularly if microscopic extensions are beyond the intended treatment area[19]. Based on the authors' findings, RFA may be a more suitable and efficient treatment option for tumors smaller than 2.84 cm in diameter. In such cases, it could be the preferred choice, particularly for high-risk patients, such as the elderly, due to the lower risk of peri- and postoperative complications. On the contrary, when tumor size exceeds 2.84 cm, SR should be favored as it is potentially more effective not only in removing the tumor, but also in clearing any peritumoral spread.
CONCLUSION
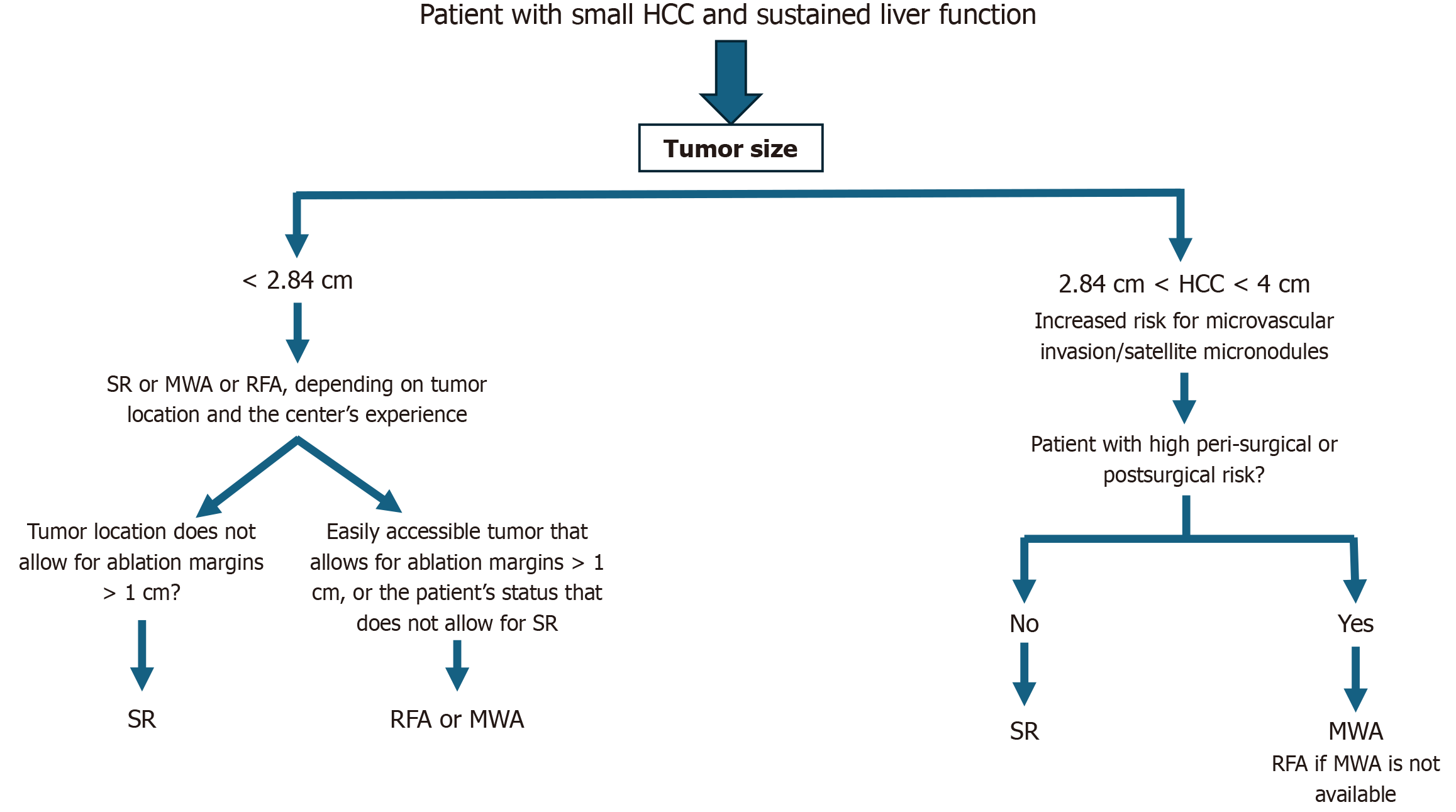
SR appears to be more effective than RFA in treating early HCC, especially in cases involving a single tumor measuring close to or larger than 3cm, as most studies indicate a correlation between SR and improved DFS and OS. The recent study by Lei et al[16], published in the latest issue of the World Journal of Gastroenterology, supports this contention. On the other hand, RFA is often associated with fewer post-procedure complications. Consequently, RFA might be preferred for patients at a higher risk of surgical complications or those with tumors smaller than 3 cm who cannot undergo surgery due to comorbidities. In addition, substituting RFA for MWA could further reduce local tumor progression rates. A proposed framework for decision-making regarding the identification of patients most suitable for SR or RFA is illustrated in Figure 1. Nevertheless, drawing definitive conclusions regarding the comparison of SR and RFA in the treatment of HCC remains challenging. This arises primarily because most studies conducted have not evaluated SR and RFA in patient populations that are completely homogenous with respect to the number of tumors, the exact tumor size, the same tumor location, and the presence of features indicative of macrovascular invasion. To determine the most effective treatment strategy for small HCCs, future RCTs must be systematically designed with patient cohorts that share similar characteristics with respect to the previously mentioned factors. In these investigations, it is recommended that contemporary ablation techniques, such as MWA, be prioritized over RFA for comparative analysis with SR. This recommendation is based on recent RCT findings demonstrating the superior efficacy of MWA in reducing local tumor progression compared to RFA.
Figure 1 Proposed protocol for the optimal management of patients with small hepatocellular carcinoma using surgical resection or ablation.
HCC: Hepatocellular carcinoma; MWA: Microwave ablation; RFA: Radiofrequency ablation; SR: Surgical resection.
Peer review: Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Gastroenterology and hepatology
Country of origin: Greece
Peer-review report’s classification
Scientific quality: Grade A, Grade B
Novelty: Grade B, Grade C
Creativity or innovation: Grade C, Grade C
Scientific significance: Grade B, Grade B
P-Reviewer: Giacomelli L, PhD, Italy S-Editor: Luo ML L-Editor: A P-Editor: Zhang L