Copyright: ©Author(s) 2026.
World J Gastroenterol. Mar 21, 2026; 32(11): 115723
Published online Mar 21, 2026. doi: 10.3748/wjg.v32.i11.115723
Published online Mar 21, 2026. doi: 10.3748/wjg.v32.i11.115723
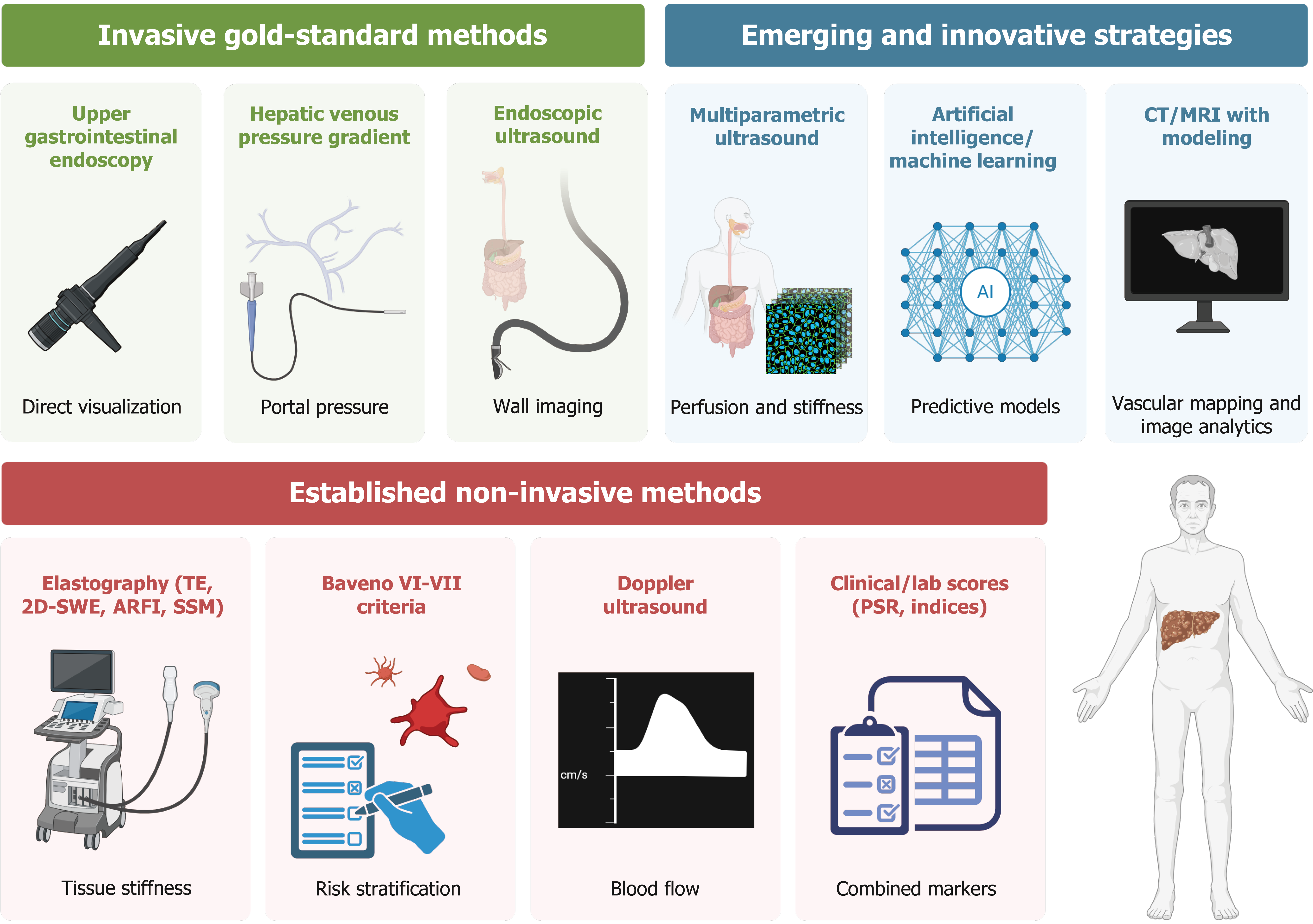
Figure 1 Diagnostic approaches for esophageal varices in patients with cirrhosis: From invasive standards to emerging noninvasive tools.
The figure summarizes the spectrum of available diagnostic tools for the assessment of esophageal varices and portal hypertension in patients with cirrhosis, ranging from traditional invasive standards to novel noninvasive strategies that are currently under development. Invasive methods, such as upper gastrointestinal endoscopy, hepatic venous pressure gradient measurement, and endoscopic ultrasound, remain the cornerstone for diagnosis and hemodynamic characterization but are resource intensive and associated with patient discomfort. Noninvasive methods, including elastography-based techniques, the Baveno VI-VII consensus criteria, Doppler ultrasound, and combined clinical/Laboratory indices, provide valuable surrogate markers of tissue stiffness, hemodynamics, and risk stratification, enabling a reduction in the number of unnecessary endoscopic examinations for selected patients. Nonetheless, they remain affected by operator and equipment variability and have a limited ability to predict posttreatment outcomes. Emerging approaches such as multiparametric ultrasound, artificial intelligence, and machine learning-based predictive models, as well as advanced cross-sectional imaging with computed tomography/magnetic resonance imaging computational modeling, represent promising strategies to achieve comprehensive, noninvasive evaluation of portal hypertension and the risk of variceal bleeding. These approaches offer multiparametric integration and potential improvements in precision but currently face challenges related to cost, technical expertise, and lack of standardized validation. Together, these modalities reflect an ongoing transition toward individualized, less invasive, and more precise management of cirrhotic patients. CT: Computed tomography; MRI: Magnetic resonance imaging; TE: Transient elastography; 2D-SWE: Two-dimensional shear wave elastography; ARFI: Acoustic radiation force impulse; SSM: Spleen stiffness measurement; PSR: Platelet-to-spleen ratio.
- Citation: Martínez-Díaz FM, Jiménez-Cuevas EA, Morales-Galicia AE, Ramírez-Mejía MM, Qi XS, Poo JL, Méndez-Sánchez N. Toward noninvasive prediction of treatment outcomes in patients with variceal bleeding. World J Gastroenterol 2026; 32(11): 115723
- URL: https://www.wjgnet.com/1007-9327/full/v32/i11/115723.htm
- DOI: https://dx.doi.org/10.3748/wjg.v32.i11.115723