Published online Mar 18, 2026. doi: 10.13105/wjma.v14.i1.114237
Revised: October 8, 2025
Accepted: December 22, 2025
Published online: March 18, 2026
Processing time: 177 Days and 3.4 Hours
Malnutrition is a common issue among hospitalised patients that contributes to increased risk of hospital readmission post-discharge. Current studies show that nutritional interventions improve recovery, but there is still limited literature on which specific type of nutritional intervention is most effective in reducing read
To investigate the effectiveness of various post-discharge nutritional interventions in reducing hospital readmissions.
We systematically searched PubMed, EMBASE, and other databases for relevant studies including patients discharged home after hospitalisation for acute ill
Thirteen studies involving 1543 participants were included and categorised into five subgroups: (1) Follow-up counselling (n = 7); (2) Pre-planned meals (n = 1); (3) Individualised nutrition care plans (n = 3); (4) Oral nutritional supplementation with whey protein (n = 1); and (5) Diet supplementation with watermelon (n = 1). Evidence for follow-up counselling was mixed, with only 3 of 7 studies reporting reduced 3-month and 6-month readmission rates. Studies on individualised nutrition care plans also show mixed results, with only 1 of 3 studies observing reduced 6-month readmission rates. The single study of oral nutritional supplementation with whey protein also saw a reduction of 1-month readmission rates. The re
Some nutritional interventions show potential in reducing readmission rates but generalisability is limited by inconsistent findings, inadequate sample sizes, and risk of bias. Further research with larger, high-quality ran
Core Tip: Unplanned hospital readmissions are costly and often preventable. This systematic review synthesised 13 trials assessing nutritional interventions delivered after discharge, including dietary counselling, oral nutritional supplements, and structured follow-up. Results were mixed. Comprehensive and sustained strategies, especially those involving dietitians and caregiver support, were most effective at reducing readmissions in older adults. Even when readmission was unaffected, improvements in nutritional status, quality of life, and physical function were noted. Integrating dietitians into discharge planning may represent a cost-effective strategy to reduce unplanned hospital readmissions and improve patient outcomes.
- Citation: Lim D, Chwa A, See KC. Impact of post-discharge nutritional interventions on hospital readmissions: A systematic review. World J Meta-Anal 2026; 14(1): 114237
- URL: https://www.wjgnet.com/2308-3840/full/v14/i1/114237.htm
- DOI: https://dx.doi.org/10.13105/wjma.v14.i1.114237
Unplanned hospital readmissions carry serious consequences for both the patient and the healthcare institution[1]. Patients with recurrent readmissions often experience progressive functional decline and a delay in recovery[2]. Some studies have also linked readmissions with an increased risk of death[3]. Beyond clinical outcomes, there is a substantial financial burden on patients, with the average cost of a hospital readmission in the United States estimated at United State Dollar 15200 in 2018[4]. For hospitals, unplanned hospital readmissions place additional strain on already limited resources. In 2004, unplanned hospital readmissions accounted for United State Dollar 17.6 billion in Medicare expendi
The World Health Organization defines malnutrition as the “deficiencies or excess in nutrient intake, imbalance of essential nutrients or impaired nutrient utilization”[8]. It may arise from underlying disease processes or from social and economic constraints. Malnutrition is common in the acute hospital setting, with Australian and other international studies reporting prevalence rates of approximately 40%[9]. Despite this, it often goes underreported. For example, one study found that only 7.6% of the medical records in Danish hospitals documented patients as being nutritionally at risk[10].
Malnutrition is a significant risk factor for unplanned hospital readmissions. One study found that malnourished patients are more than twice as likely to be readmitted within 30 days [odds ratio (OR) = 2.28; 95% confidence interval (CI): 1.26-4.12; P < 0.006] compared with non-malnourished patients[11]. Some specific mechanisms by which malnutrition contributes to hospital readmissions include its association with adverse health outcomes such as immunodeficiency and delayed recovery along with impaired wound healing[12]. One study proposed that malnutrition further complicates the post-discharge period by impairing physiological systems, depleting functional reserves and exacerbating previously stable comorbidities[13]. Evidence suggests that nutritional status often deteriorates further with each subsequent admission, contributing to a cycle of worsening effects[14].
The severity of malnutrition also has a measurable impact on outcomes such as unplanned hospital readmissions and post-discharge mortality. In a previous cohort study, participants were stratified into four categories of increasing severity: (1) Non-malnourished; (2) At risk of malnutrition; (3) Non-specific malnutrition; and (4) Protein-energy malnutrition. Compared with non-malnourished patients, the odds of 30-day hospital readmission were 1.2-fold, 1.5-fold, and 2.1-fold higher in those at risk, with non-specific malnutrition, and with protein-energy malnutrition, respectively[15]. Similarly, the odds of 90-day post-discharge mortality were 1.4-fold, 2.4-fold, and 5.0-fold higher in these same groups[15].
With the strong association between malnutrition and unplanned hospital readmission rates, nutritional interventions have gained increasing attention in recent years[1]. Nutritional interventions include oral nutritional supplements, individualised dietary counselling, and enteral nutrition. In addition to improving nutritional status, these interventions, particularly enteral nutrition and oral supplements, also offer physiological benefits including enhanced gastrointestinal function, improved gut mucosal integrity, and better immune responses. These physiological benefits enhance overall recovery and reduce the risk of potential complications[16].
Despite the growing focus on nutritional interventions, there is limited literature on which specific type of nutritional intervention is most effective in reducing unplanned hospital readmissions. Previous systematic reviews mainly focused on a single mode of intervention such as telehealth[17]. In earlier studies that looked at multiple types of nutritional interventions, direct comparison between the different approaches was not a primary objective[18]. Thus, there is a gap in existing literature on the relative effectiveness of the various nutritional interventions.
This systematic review examines the effectiveness of post-discharge nutritional interventions in reducing unplanned hospital readmissions, exploring the potential advantages and disadvantages of the different types. By synthesising current evidence, this study seeks to guide healthcare providers in improving post-discharge outcomes through targeted nutritional support.
A comprehensive and systematic search of the literature was conducted to identify all relevant published articles studying the impact of post-discharge nutritional interventions on hospital readmissions. The search was guided by the population, intervention, comparator, and outcome framework. Electronic databases PubMed and EMBASE were searched from inception to the date of the search on August 17, 2025. Google Scholar was used for supplementary searching and grey literature, where the first five pages of results were reviewed to look for known key articles and additional eligible articles. Medical subject headings and key words used in relation to the population, intervention, comparator, and outcome framework were: (1) Population: Patient discharge and post-hospitalisation; (2) Intervention: Nutritional support, dietary counselling, oral supplements; and (3) Outcome: Readmission and rehospitalisation. The full electronic search strategy for each database is outlined in Table 1 to ensure transparency and reproducibility. This systematic review was registered on PROSPERO and done in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analysis guidelines.
| Database search strategy |
| PubMed |
| ("Patient discharge"[MeSH] OR post-discharge OR after hospitalization) AND ("nutritional support"[MeSH] OR nutrition intervention OR oral supplements OR dietary counselling OR malnutrition) AND (readmission OR rehospitalization OR 30-day readmission) |
| EMBASE |
| ('Patient discharge'/exp OR 'post discharge':ab,ti OR 'after hospitalization':ab,ti) AND ('nutritional support'/exp OR 'nutrition intervention':ab,ti OR 'oral supplements':ab,ti OR 'dietary counselling':ab,ti OR malnutrition:ab,ti) AND (readmission:ab,ti OR rehospitalization:ab,ti OR '30 day readmission':ab,ti) |
All records retrieved from the searches were exported into a reference management software (EndNote 21) for deduplication. The selection process was divided into two stages and did not utilise any automation tools. First, two reviewers independently screened the titles and abstracts of all retrieved records against the pre-defined eligibility criteria. Inclusion criteria included patients discharged home after hospitalisation for acute illnesses, nutritional intervention, and unplanned hospital readmission up to 180 days after discharge. Exclusion criteria included paediatric populations, patients admitted for elective procedures, and nutritional intervention only during the admission period. Full inclusion and exclusion criteria are as documented in Table 2.
| Inclusion criteria | |
| Population | Patients discharged home after a period of hospitalisation for acute illnesses |
| Intervention/comparison | Any nutritional intervention (dietary counselling, oral nutritional supplementation, feeding support, etc.) |
| Control | Usual nutrition |
| Outcome | Unplanned hospital readmission (any definition, e.g., 30-day readmission, unplanned readmission) |
| Study design | Randomised controlled trials, cohort studies, case-control studies |
| Setting | Any healthcare setting, worldwide |
| Exclusion criteria | |
| Population | Paediatric populations: Patients admitted for elective procedures or rehabilitation |
| Setting | Nutritional intervention only during inpatient admission period |
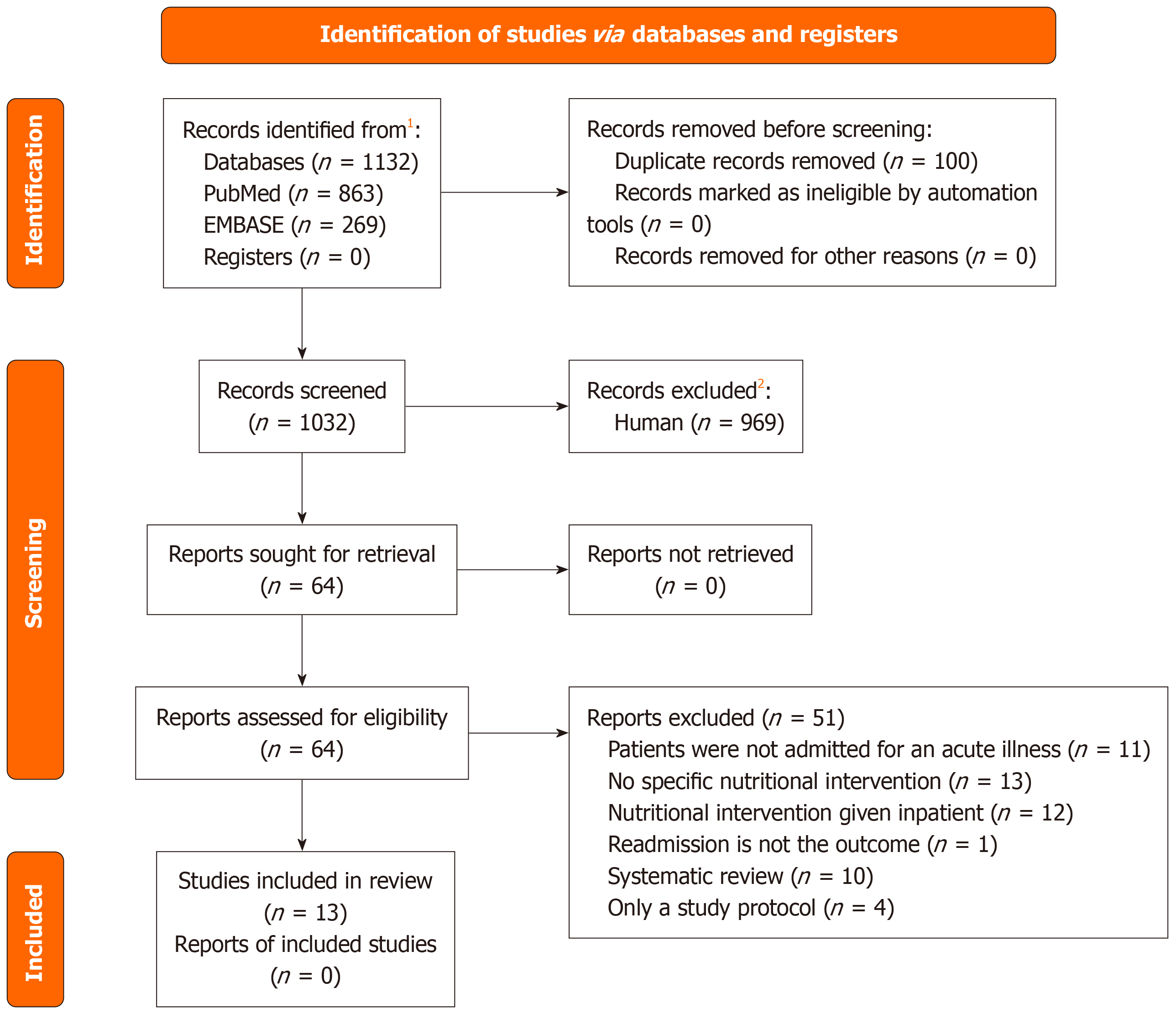
All articles that clearly did not meet the criteria were excluded after this stage. Second, the full-texts of potentially eligible articles were obtained and independently assessed by two independent reviewers. Reasons for exclusion at this stage were recorded systematically. Reasons for exclusion at this stage included reviews with no independent data, interventions started prior to discharge, and presence of multimodal intervention programmes. Reference lists of reviews were screened to identify any additional relevant articles. Disagreements at either stage were resolved through discussion. If a consensus was not reached, a third reviewer adjudicated. The study selection process was documented in a Preferred Reporting Items for Systematic Reviews and Meta-Analysis flow diagram (Figure 1), showing the number of records identified, screened, assessed for eligibility, and included in the review, along with reasons for exclusion.
Data were extracted independently by two independent reviewers, with discrepancies resolved through discussion. The following information was extracted: Study characteristics, population characteristics, intervention details, comparator, outcomes, conclusions, and funding sources or conflicts of interest where reported. Main outcomes sought were readmission to hospital at 1, 3, or 6 months. The main effect measure of readmission was ORs comparing the intervention group to the control/comparator group. All extracted data were stored in a secure database (Excel). No additional information was sought from study investigators in the event of required information being unclear or unavailable in the study publications and reports. Individual participant data or study datasets were not sought.
The methodological quality and risk of bias of included studies was assessed independently by two independent reviewers, with disagreements resolved through discussion. The Cochrane risk of bias 2 tool was used for randomised controlled trials (RCTs). The risk of bias assessments was summarised in a tabular format. The overall certainty of the evidence for each outcome was evaluated using the grading of recommendations, assessment, development, and evaluation framework, accounting for study limitations, consistency, directness, precision, and risk of publication bias.
Quantitative synthesis was not possible due to the heterogeneity in types of nutritional interventions, comparators, outcomes, and analytic methods. Therefore, a narrative synthesis of the results was performed.
The study selection process is outlined in Figure 1. A total of 1132 studies were identified from PubMed and EMBASE after a systematic search of the literature, and 100 duplicate records were removed. A total of 1032 records were screened at the first stage of the selection process. Only 64 articles clearly met the inclusion criteria and did not meet the exclusion criteria. These were sought for full-text retrieval and screening for eligibility. Thirteen studies were included for the final review, with 51 reports excluded due to reasons as listed in Figure 1. The key characteristics of the 13 included studies were summarised and tabulated to guide grouping decisions. Key characteristics include study design, population and comparator details, type of nutritional intervention, and hospital readmission rate as the primary outcome (Table 3)[14,19-30]. The full study characteristics are as summarised in Supplementary Table 1[14,19-30].
| Ref. | Type of study, patient demographics and number | Nutritional intervention | Comparator/control group | Conclusions |
| Follow-up counselling by clinical nutritionists or dietitians | ||||
| Beck et al[14] | RCT. Geriatric patients (> 75), n = 71 | A discharge Liaison-Team in cooperation with a dietician, who performed a total of three home visits with the aim of developing and implementing an individual nutritional care plan | For the comparator group, the team did not include the dietician | Adding a dietician to the discharge Liaison-Team after discharge of geriatric patients may reduce the number of times hospitalized within 6 months |
| Blondal et al[19] | Secondary analysis of RCT. Geriatric patients (> 65), n = 106 | The clinical nutritionist provided the intervention group with nutrition therapy during five home visits (conducted the day after hospital discharge and at one, 3, 6, and 12 weeks from discharge) | The control group did not receive any further nutritional care or service by the hospital, primary care sector and community | Six-month nutrition therapy in older Icelandic adults discharged from hospital reduced hospital readmissions and shortens length of stay at the hospital up to 18-months post-discharge. However, it did not affect mortality, emergency room visits, nor need of long-term care residence in this group |
| Cramon et al[24] | Pilot RCT. Geriatric patients, n = 40 | The nutritionists conducted two visits to the patients’ homes in the course of the 4 weeks subsequent to discharge. Patients received follow-up phone calls between visits, if necessary | The patients in the control group received standard treatment and were offered nutritional guidance after the last follow-up | Individual nutritional intervention did not prevent readmission among geriatric patients in this trial |
| Sharma et al[23] | RCT. Geriatric patients, n = 148 | Individualized nutrition care plan and monthly post-discharge telehealth follow-up | Control patients were allowed to follow the same intervention until hospital discharge, but did not receive any additional post-discharge telephone follow-up | There is no significant difference in complication rate during hospitalization, quality of life and mortality at 3 months or readmission rate at 1 month, 3 months, or 6 months following hospital discharge |
| Wyers et al[21] | RCT. Geriatric patients (> 55), n = 152 | Weekly dietetic consultation, energy-protein-enriched diet, and oral nutritional supplements (400 mL per day) for 3 months | Control patients received usual nutritional care as provided in the hospital, rehabilitation clinic, or at home | Intensive nutritional intervention after hip fracture did not improve clinical outcomes (did not affect readmissions) |
| Lindegaard Pedersen et al[20] | RCT. Geriatric patients (> 75), n = 208 | Individualized nutritional counselling of the patient and the patient's daily home carer by a clinical dietician 1, 2, and 4 weeks after discharge from hospital | Control patients received standard care in hospital and on discharge | Individualized nutritional follow-up performed as home visits seems to reduce readmission to hospital 30 days and 90 days after discharge. Intervention by telephone consultations may also prevent readmission, but only among participants who receive the full intervention |
| Munk et al[22] | RCT. Geriatric patients, n = 191 | Dietetic counselling including a recommendation of daily training, an individual nutrition plan and a package containing foods and drinks covering dietary requirements for the next 24 hours. Further, a goodie-bag containing samples of protein-rich milk-based drinks were provided. The dietician performed telephone follow-ups on day 4 and 30 and a home visit at 16 weeks | The control group received standard care at discharge following the standard procedure for ward discharge of patients | The present study, using a multimodal nutritional approach, revealed no significant effect on readmissions however a significant positive effect on nutritional status, quality of life and physical function was found |
| Individualised meals thrice a day (as evaluated and enhanced by dietitian) | ||||
| Buys et al[25] | Pilot RCT. Geriatric patients (> 65), n = 21 | The intervention group received three meals per day for 10 days. Meals were based upon National Institute on Aging’s recommendations from What’s on Your Plate: Smart Choices for Healthy Aging 2021 and the Academy of Nutrition and Dietetics 2012 Position Statement on Food and Nutrition for Older Adults living in the community | Control participants received the care or treatment as prescribed by their attending physician or nurse practitioner (usual care) | Conducting a randomized controlled trial to assess outcomes of providing home-delivered meals to older adults after hospital discharge in partnership with a small nonprofit organization is feasible and warrants future research. This study did not show any statistical differences in hospital readmission |
| Individualised nutrition care plans | ||||
| Beck et al[28] | RCT. Geriatric patients (> 65), n = 152 | The registered dietitians performed a comprehensive nutritional assessment at the first home visit as a basis for developing a nutrition care plan consistent with estimated nutritional requirements and nutritional rehabilitation goals | Discharge follow-up by general practitioners was planned to consist of three contacts, conducted approximately 1, 3, and 8 weeks after discharge in both control and intervention participants | Follow-up home visits with registered dietitians have a positive effect on the functional and nutritional status of geriatric medical patients after discharge. A larger study with a longer intervention period is needed to see if there is a positive effect on risk of re-admission and mortality |
| Yang et al[26] | RCT. Geriatric patients, n = 82 | Individualized nutritional intervention program, according to energy and protein intake requirements in addition to dietary advice based on face-to-face interviews with their family caregivers during hospitalization, with phone calls post-discharge for prescribing individualized nutritional iNIP | The standard care group was only provided standard nutritional supplements according to the Kaohsiung Chang Gung Memorial Hospital Nutrition Department, and patients’ family caregivers were not provided dietary advice | A 6-month iNIP under dietitian and patient family nutritional support for malnourished older adults with pneumonia can significantly improve their nutritional status and reduce the readmission rate |
| Terp et al[27] | RCT. Geriatric patients, n = 144 | Individual dietary plan for home, including pre-discharge advice on nutritional intake, combined with three follow-up visits after discharge (1, 4, and 8 weeks) | Patients in the control group received usual care, which meant screening for nutritional risk within 24 hours of hospital admission using Nutritional Risk Screening-2002 and weekly monitoring of their nutritional status | There is no effect on readmissions noted |
| Oral nutritional supplementation (with whey protein) | ||||
| Deer et al[29] | RCT. Geriatric patients, n = 100 | One of five post-hospital interventions: Whey protein supplementation, in-home rehabilitation with placebo supplementation, in-home rehabilitation with protein supplementation, single testosterone injection, or isocaloric placebo supplementation, the control group | The control group received an isocaloric placebo supplementation together with usual care | Post-hospital protein supplementation, in-home exercise, and testosterone interventions are safe, can accelerate recovery, and may reduce readmission rates in geriatric patients |
| Diet supplementation with watermelon | ||||
| Tan et al[30] | RCT. Pregnant patients, n = 128 | Participants randomized to watermelon and dietary advice leaflet were supplied with two fresh red-fleshed watermelon (approximately 4 kg weight) to take home in addition to the dietary advice leaflet which they were advised to read and heed | Participants randomized to advice leaflet were provided with an identical advice leaflet to read and heed | Adding watermelon to the diet after hospital discharge for HG improves body weight, HG symptoms, appetite, wellbeing and satisfaction (no effect on hospitalisation) |
Ten studies were RCTs, two were pilot RCTs, and one was secondary analysis of an RCT. The demographics studied were all geriatric patients in different age groups, ranging from above 55 years old to above 75 years old, with the exception of one study that explored the demographic of pregnant patients. No funding sources or conflicts of interests were declared.
Interventions were nutrition-focused and varied in components and frequency or intensity. Then the studies were grouped based on type of nutritional intervention for qualitative synthesis. These subgroups were: (1) Follow-up counselling by clinical nutritionists or dieticians; (2) Individualised meals three times a day (as evaluated and enhanced by a dietician); (3) Individualised nutrition care plans; (4) Oral nutritional supplementation (with whey protein); and (5) Diet supplementation with watermelon. Comparator groups were typically treated with standard or usual nutritional care.
The primary outcome measured was readmissions, typically at 1 (30 days), 3 (90 days), or 6 months (180 days) after discharge from the hospital for an acute illness. Generally, results fell into two broad categories: (1) One where the intervention reduced readmission rates; and (2) One where the intervention had no effect on readmission rates.
In each subgroup, descriptive comparisons were made between each study. As some studies reported several readmission rates over different periods (1 month, 3 months, and 6 months), outcomes were standardised where necessary. Any available summary statistics such as ORs and CIs were mentioned as well. Studies without these effect measures were still included in the qualitative synthesis. Subgroup analysis was conducted to explore the possible causes of heterogeneity. Table 4 details the process of determining the certainty of each group of studies, based on the grading of recommendations, assessment, development, and evaluation framework.
| Intervention | Number of participant (studies) | Readmission windows | Risk of bias | Inconsistency | Indirectness | Imprecision | Publication bias | Effect | Certainty |
| Follow-up counselling by clinical nutritionists or dieticians | 916 (7) | 1 month, 6 months, 12 months, 18 months | Some concerns in 2/7 | Very serious | Not serious | Serious | Low suspicion | Mixed results (3/7 studies show reduction in readmission rates) | Very low |
| Individualised meals thrice a day (as evaluated and enhanced by a dietician) | 21 (1) | 1 month | Some concerns | NA (only 1 study) | Not serious | Very serious | Low suspicion | No significant difference (single-study evidence) | Very low |
| Individualised nutrition care plans | 378 (3) | 3 months, 6 months | Some concerns in 2/3 | Serious | Not serious | Serious | Low suspicion | Mixed results (1/3 studies show reduction in readmission rates) | Low |
| Oral nutritional supplementation (with whey protein) | 100 (1) | 1 month | High | NA (only 1 study) | Not serious | Very serious | Low suspicion | Trend towards benefit (single-study evidence) | Very low |
| Diet supplementation with watermelon | 128 (1) | 2 weeks | Some concerns | NA (only 1 study) | Very serious | Very serious | Low suspicion | No significant difference (single-study evidence) | Very low |
As shown in Supplementary Figures 1 and 2, and Supplementary Table 2, bias assessment with the Cochrane risk of bias 2 tool was performed for 13 studies, which were published from 2012 onwards. Most studies were adequately powered except for 3 studies. One was a pilot RCT by Buys et al[25], which had a very small sample size of 21 participants. Another was an RCT by Blondal et al[19], which was adequately powered to detect anthropometric differences between the intervention and control groups, but was underpowered for readmission rates. Similarly, the RCT by Terp et al[27] calculated power based on changes in nutritional status, and was therefore underpowered for detecting differences in readmission outcomes. Underpowered studies contributed to imprecision rather than bias and were noted separately in the certainty assessment.
One (7%) study had high risk of bias, 6 (46%) studies had some risk of bias, and 6 (46%) trials had low risk of bias (Supplementary Figures 1 and 2 and Supplementary Table 2). The study that was classified as having the highest risk of bias did not provide details on their randomisation process. Common limitations were the lack of blinding in participants, staff, and outcome assessors.
Formal assessment of publication bias was not possible due to the absence of meta-analysis. The possibility of undetected publication or reporting bias cannot be excluded.
The 13 included studies were categorised into five subgroups: (1) Follow-up counselling by clinical nutritionists or dieticians (n = 7); (2) Individualised meals three times a day (as evaluated and enhanced by a dietician) (n = 1); (3) Individualised nutrition care plans (n = 3); (4) Oral nutritional supplementation (with whey protein) (n = 1); and (5) Diet supplementation with watermelon (n = 1). Findings along with certainty of evidence in each subgroup are summarised in Table 4. Rationale and implications of certainty assessments are detailed in the Discussion section.
Overall, evidence for follow-up counselling on readmission rates was mixed, with only 3 of the 7 studies demonstrating benefit.
Seven studies evaluated the impact of follow-up counselling by clinical nutritionists or dieticians. Five were RCTs, one was a pilot RCT, and the last one was a secondary analysis of a previous RCT. Sample sizes ranged from 40 participants to 208 participants. All studies compared follow-up counselling with standard treatment. Follow-up periods ranged from 1 month to 18 months, with four studies reporting hospital readmission rates at multiple time points.
Only three studies reported a reduction in readmission rates. Two studies demonstrated a reduction in 6-month readmission rates with statistical significance. Beck et al[14] observed an OR of 0.33 (P = 0.017) and Blondal et al[19] reported an OR of 0.367 (P = 0.014). The RCT by Lindegaard Pedersen et al[20] also saw a statistically significant reduction in 3-month readmission rates, with a hazard ratio of 0.4 (95%CI: 0.2-0.8, P < 0.01).
The four remaining studies concluded that there was no reduction in readmission rates. The three RCTs by Wyers et al[21], Munk et al[22], and Sharma et al[23] found no significant change in the primary outcome. However, Wyers et al[21] and Munk et al[22] noted that intervention groups still saw an improvement in nutritional intake, experiencing weight gain rather than weight loss. The former saw an average gain in weight by 1.9 kg after 3 months (95%CI: 0.6-3.3; P < 0.01) whereas the latter saw an average gain in weight by 0.7 kg at the 4-month mark (95%CI: 0.8-3.4; P = 0.002). On the other hand, the pilot RCT by Cramon et al[24] found that follow-up counselling resulted in increased readmission rates (29% vs 11%), although not statistically significant (P = 0.24).
Hence, follow-up counselling does demonstrate potential benefit in certain settings. However, there is very low certainty in evidence, arising from inconsistency in the findings of the studies and imprecision from their small sample size.
Only one study looked at how pre-planned, individualised meals can affect post-discharge readmission rates. Buys et al[25] conducted a pilot RCT involving 21 older adults over a follow-up period of 45 days, assessing for readmission rates at the 1-month mark.
Participants in the intervention group received three meals per day for 10 days. These meals were made following national guidelines and modified by a registered dietician and health behaviour expert. Participants in the control group received usual care.
This pilot RCT found that individuals in the intervention group actually had a higher risk of being readmitted within 1 month of discharge (27.7% vs 8.3%; P = 0.59). Findings were not statistically significant[25]. Potential explanations for this observation are explored in the Discussion section.
As such, it can be said that individualised meals do not decrease readmission rates. There is very low certainty in this conclusion, given that the evidence comes solely from a pilot RCT.
Evidence for individualised nutritional care plans is mixed, with only one of the three studies showing a reduction in readmission rates.
Three studies assessed the impact of individualised nutrition care plans on post-discharge readmission rates, all of which were RCTs. Sample sizes ranged from 82 participants to 152 participants, and all studies compared individualised nutrition care plans with standard care. Follow-up durations ranged between 3 months and 6 months, with two RCTs only assessing 6-month readmission rates and one RCT looking at only 3-month readmission rates.
Only one RCT reported a reduction in readmission rates, with statistical significance. Yang et al[26] found that the 6-month readmission rate for pneumonia decreased by 77% in the intervention group compared to the control group (OR: 0.228, 95%CI: 0.06-0.87; P = 0.03).
The other two RCTs showed that there were no noticeable reductions in readmission rates. While Terp et al[27] found that 3-month readmission rates were roughly the same between intervention and control groups (39% vs 34%; P = 0.547), Beck et al[28] actually saw a higher 6-month readmission rate for the intervention group (53% vs 42%; P = 0.07). Both findings were not statistically significant.
Hence, individualised nutrition care plans may reduce readmission rates; however, the inconsistency of findings for this nutritional intervention limits our confidence this relationship.
One study examined how whey protein supplementation could influence 1-month hospital readmission rates among older adults post-discharge. Deer et al[29] conducted an RCT involving 100 geriatric patients over a follow-up period of 4 weeks post-discharge, looking at 1-month readmissions.
The 100 participants were randomised into one of four interventions: (1) Whey protein supplementation; (2) In-home rehabilitation; (3) In-home rehabilitation and whey protein supplementation; and (4) Single testosterone injection. The control group received an isocaloric placebo supplementation together with usual care.
Deer et al[29] observed that 1-month readmission rates were reduced for participants on whey protein supplementation compared to the control group, although not statistically significant (12% vs 28%; P = 0.06). If whey protein supplementation was combined with in-home rehabilitation, the readmission rate dropped even lower to 11%. Interestingly, the group on the single testosterone injection had the lowest 1-month readmission rate at 5%[29]. This finding is further examined in the Discussion section.
Therefore, oral nutritional supplementation with whey protein can potentially reduce readmission rates; however, as this conclusion was drawn from a single study, there is limited generalisability.
There was only one study that investigated the relationship between hospital readmission rates and diet supplementation with watermelon. Tan et al[30] conducted an RCT involving 128 pregnant patients who were admitted for hyperemesis gravidarum (HG), on follow-up until 2 weeks post-discharge. Each participant in the intervention group received dietary advice along with two watermelons (approximately 4 kg in weight), whereas participants in the control group only received usual post-discharge instructions. Tan et al[30] observed that 2-week readmission rate for HG were similar (9.4% vs 9.5%, 95%CI: 0.34-2.89; P = 0.98).
Diet supplementation with watermelon did not reduce the readmission rate for HG. This finding was based on a single study with a small sample size in a narrowly defined population of pregnant patients, restricting its relevance to other patient groups.
This systematic review synthesised evidence from 13 studies, which evaluated nutritional interventions after hospital discharge for acute illnesses. While the target population of this review were simply adults over the age of 18, the included studies all focused on geriatric patients except for one trial studying pregnant women with HG. General observations are presented first, followed by interpretation of evidence for each specific nutritional intervention.
Trials that demonstrated positive outcomes generally implemented interventions sustained beyond the immediate post-discharge period, with readmission rates longer intervention durations associated with greater reductions in readmission rates. Blondal et al[19] noted a significant 63.3% reduction in readmissions after 6 months (P = 0.017). Similarly, Lindegaard Pedersen et al[20] evaluated regular nutritional counselling by a dietitian but only followed patients for 3 months, observing that readmission rates did drop significantly at 60% (P < 0.01), although not as much the former study.
Furthermore, studies that incorporate multiple nutritional interventions tend to demonstrate greater success. For example, comprehensive programmes combining regular dietary counselling with oral nutritional supplements such as the study by Munk et al[22] appeared more effective at reducing readmissions compared to single-component interventions. However, this highlights a limitation of the systematic review, as the effect of specific nutritional interventions may be obscured by these multi-faceted approaches.
Overall, findings were mixed for each type of nutritional intervention explored in this review. The certainty of the evidence is generally low as well. There is limited confidence in the estimated effect of each intervention, and their true effect may be vastly different from what the data suggests.
For follow-up counselling, results were mixed. Only three of seven studies showed that 3-month and 6-month readmission rates improved when patients were regularly seen by a clinical nutritionist or dietitian. These findings align with an editorial published in 2024, which describes nutritional counselling as a cornerstone in improving health outcomes. This editorial by Ferraris and De Amicis[31] suggests that beyond providing tailored dietary advice, counsellors manage stress and enhance motivation as well. This ensures that the dietary advice is not just suitable but more importantly, sustainable[31]. The National Council on Aging in America also supports these findings, stating that nutritional counselling plays a key role in weight loss and nutrient balance, reducing risk for heart disease, stroke, and coronavirus disease 2019 complications[32].
To account for the four remaining studies that found no appreciable benefit in readmission rates, one can consider that nutritional counselling is more recognised in the management of chronic diseases rather than any acute illness, which is the focus of this review. A narrative review by Vasiloglou et al[33] discusses how counselling is proven effective for chronic kidney disease and cancer. Hence, there is a possibility that nutritional counselling can help in reducing readmissions due to acute complications of chronic conditions rather than all acute illnesses.
This serious inconsistency in views across these seven studies gives us very low certainty in this body of evidence. A possible explanation for these contrasting findings could be heterogeneity in the methodology of the studies. Besides the varying follow-up durations, the type of follow-up was also not consistent. Some studies such as Beck et al[14] conducted purely in-person counselling, some studies such as Sharma et al[23] only conducted telehealth counselling, and some studies applied both methods (notably Blondal et al[19] and Wyers et al[21]). Another plausible explanation would be that while some RCTs mentioned follow-up counselling as their main nutritional intervention, the presence of secondary interventions likely introduced uncertainty in the true effects of follow-up counselling. Key examples would be the studies conducted by Blondal et al[19], Wyers et al[21] and Munk et al[22] which both provided their intervention groups with oral nutritional supplements on top of follow-up counselling.
Another reason for the very low certainty in these studies is their imprecision, arising from their small sample sizes ranging between 40 participants and 208 participants. The study by Blondal et al[19] was also underpowered to detect differences in readmission rates.
Pre-planned meals showed no significant benefit in reducing readmission rates. This finding contradicts a study by Maneesing et al[34], which reported that a portioned meal box programme achieved superior glucose control compared to general nutritional counselling, with a greater reduction in in glycated hemoglobin levels. Improved glycaemic control lowers the likelihood of acute and chronic diabetes-related complications. Currently, meal preparation is mainly recognised for reducing the risk of chronic diseases such as type 2 diabetes mellitus rather than the prevention of acute hospitalisations[35].
The surprising finding that individuals in the intervention group had higher 1-month readmission rates (27.7% vs 8.3%; P = 0.59) warrants further consideration. One possible explanation is the presence of unmeasured confounders. Buys et al[25] acknowledged that the study did not adjust for key variables such as severity of illness or complications from comorbid conditions. Another explanation relates to baseline differences between the intervention and control groups. The intervention group had a higher prevalence of diabetes and related complications, with two readmissions directly attributable to these conditions[25].
In addition, the study population may not be representative of the general patient population. Most participants were living below the poverty line and lacked adequate home support (widowed, divorced, or single), as many eligible patients with stronger support systems and sufficient financial resources for purchasing food declined participation[25]. Consequently, the study may have disproportionately included individuals who were more unwell and inherently at greater risk of readmission.
Overall, these conclusions were drawn from a single pilot RCT with only 21 participants, rendering the findings imprecise and underpowered to detect true differences in readmission rates. Combined with the lack of adjustment for confounders, the risk of bias is high and the certainty of the findings for this study were therefore very low.
Evidence for individualised nutritional care plans was mixed as only one of the three studies showed a reduction in readmission rates. To complement this study that demonstrated a positive relationship, we can consider a separate study on meal planning that reported significant weight loss and lower odds of obesity[36]. This thereby lowers the risk of obesity-related complications, including cardiac events that may necessitate frequent hospitalisation.
For the other two studies that saw no noticeable reductions in readmission rates, the duration of nutritional plans may have been insufficient. A systematic review by Ingstad et al[37] suggested that while individualised nutritional care plans can improve outcomes such as reducing readmissions, follow-up of at least 6 months post-discharge may be required to observe more meaningful benefits. Another plausible explanation would be the patient-centred nature of this nutritional intervention. In all three RCTs, although care plans were developed by specialists, their implementation relied heavily on patient adherence. It is possible that only Yang et al[26] saw an improvement in readmission rates because that study actively involved the patients’ caregivers in the intervention process. This likely improved participant adherence, addressing a common challenge in implementing personalised nutritional interventions as stated in another systematic review by Shyam et al[38].
Across the three studies there was an inconsistency in findings, with only one RCT showing a reduction in readmission rates. While this same study is the only study with statistical significance, the small sample sizes ranging between 82 and 152 also make this body of evidence imprecise. Terp et al[27] also noted that their study was underpowered in detecting for differences in readmission rates.
Another point worth mentioning for the RCT by Yang et al[26] is its inclusion criteria for readmission rates. The study only recorded readmission rates for pneumonia, indicating that readmissions for other acute illnesses may not have been considered[26].
One study demonstrated that patients discharged with whey protein supplementation experienced a notable reduction in readmission rates. This conclusion agrees with a prior systematic review and meta-analysis conducted by Stratton et al[39], which found that protein supplementation plays a crucial role in maintaining body weight and preserving muscle strength in frail patient populations. By improving nutritional status and preventing further functional decline, protein supplements were shown to significantly lower the risk of readmission[39].
Another noteworthy finding is that the group that received a single testosterone injection demonstrated the lowest 1-month readmission rate, even when compared to whey protein supplementation (5% vs 12%; P = 0.06)[29]. This ob
Regardless, there is very low certainty in this evidence as this is single-study data with only 100 participants[29]. Furthermore, the risk of bias was high in this study as the randomisation process was not detailed. This limits the generalisability of the findings and hence the role of whey protein supplementation in reducing readmissions remains uncertain.
A single study investigated the effect of dietary watermelon supplementation on hospital readmission rates but found no significant difference between the intervention and control groups. Existing literature on the health benefits of watermelon in pregnancy is limited. For instance, Fulgoni et al[43] evaluated the nutritional effects of watermelon in adults and children but excluded pregnant participants from their analysis. However, the study discussed how watermelon consumption improved overall nutritional status and also provided high bioavailability of antioxidant components such as lycopene and l-citrulline[43]. Additional studies have reported that watermelon extracts may reduce blood pressure in individuals with hypertension[44] and decrease total cholesterol in patients with dyslipidaemia[45]. Nevertheless, further research is warranted to clarify the potential benefits of watermelon specifically in pregnant populations.
The certainty of evidence for this nutritional intervention is very low, limited by single-study data with a small sample size. Although the study population met the inclusion criteria of adults discharged following hospitalisation for an acute illness, most other studies in this review focussed on geriatric patients rather than pregnant women. As a result, the applicability of these findings to the broader target population is limited and considered indirect.
Several limitations of this review should be acknowledged. First, there was a high risk of bias in the majority of the included studies. Of the 13 studies, 1 was rated as having a high risk of bias due to not clearly outlining its randomisation process. In addition, six studies were assessed as having some concerns for risk of bias, largely because of inadequate blinding of participants, staff, and outcome assessors. These methodological limitations reduce the reliability of the findings and limit the confidence that can be placed in the overall evidence.
Another limitation would be the varying participant populations between studies. The populations studied were heterogenous, spanning different clinical populations and demographics. The only common factor was patient age group; the country, location, and cultural differences between studied populations may have caused difficulty in collating data. Most significantly, the review included a study on pregnant patients, in contrast to the general trend of studies focusing on geriatric patients. In the future, a meta-analysis may be considered if studied populations are similar and share more common characteristics.
In addition, the choice of outcome for this systematic review was not well-defined. The primary outcomes of the 13 included studies varied, with some studies not designating hospital readmission as their main endpoint. Follow-up durations after discharge also differed widely, ranging from 1 month to 18 months, resulting in a lack of a common timeframe for comparison. This variability likely contributed to inconsistency in the results. Furthermore, the reasons for readmission were often not specified, raising the possibility that many readmissions were unrelated to nutritional status. Future research should adopt a standardised follow-up period and clearly distinguish between nutrition-related and unrelated readmissions to strengthen the validity of findings.
The wide diversity of nutritional interventions also makes it challenging to identify the most effective strategy for specific patient groups. Some studies were multimodal and incorporated multiple intervention strategies into their care plan. In most studies, a single primary intervention was not easily identified, and the role of each intervention was not readily quantifiable. The effect of each intervention was not distinguishable from others.
These findings highlight the potential for nutritional interventions to be integrated as part of routine discharge planning to reduce hospital readmissions, especially in malnourished older adults. Nutritional screening and individualised support post-discharge can be considered by clinicians, and policymakers should view nutritional programmes as an effective strategy to reduce long-term healthcare costs.
For future research, large and multi-centre RCTs with standardised definitions of readmission and a longer follow-up period are needed to strengthen the evidence base. Studies should also compare different modes of interventions to identify the most effective approaches. Incorporating cost-effectiveness analyses can further support policy decision-making at a national level.
This systematic review examined 13 trials on post-discharge nutritional interventions, mainly in older adults. Interventions included dietary counselling with follow-up, home visits or telephone consultations, oral nutritional supplements, and tailored meal provision.
Results were mixed. Some studies, such as the HOMEFOOD trial or the individualised nutritional intervention program for pneumonia, reported significant reductions in readmission rates, while other showed no effects, possibly due to small sample sizes and brief intervention periods. Though readmissions remained unaffected, improvements in nutritional status and quality of life were observed.
Overall, structured nutritional support after discharge has the potential to reduce hospital readmissions, but current evidence is heterogenous and may not be of the strongest quality. Larger trials are needed to confirm both effectiveness and cost-effectiveness. Integrating dietitians and structured nutritional care into discharge planning has the potential to improve patient recovery and reduce preventable readmissions.
We acknowledge the support of the National University of Singapore for providing access to library resources.
| 1. | Lærum-Onsager E, Molin M, Olsen CF, Bye A, Debesay J, Hestevik CH, Bjerk M, Pripp AH. Effect of nutritional and physical exercise intervention on hospital readmission for patients aged 65 or older: a systematic review and meta-analysis of randomized controlled trials. Int J Behav Nutr Phys Act. 2021;18:62. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 8] [Article Influence: 1.6] [Reference Citation Analysis (1)] |
| 2. | Bortolani A, Fantin F, Giani A, Zivelonghi A, Pernice B, Bortolazzi E, Urbani S, Zoico E, Micciolo R, Zamboni M. Predictors of hospital readmission rate in geriatric patients. Aging Clin Exp Res. 2024;36:22. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 7] [Article Influence: 3.5] [Reference Citation Analysis (1)] |
| 3. | Yen HY, Chi MJ, Huang HY. Effects of discharge planning services and unplanned readmissions on post-hospital mortality in older patients: A time-varying survival analysis. Int J Nurs Stud. 2022;128:104175. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 13] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 4. | Weiss AJ, Jiang HJ. Overview of Clinical Conditions With Frequent and Costly Hospital Readmissions by Payer, 2018. 2021 Jul 20. In: Healthcare Cost and Utilization Project (HCUP) Statistical Briefs [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2006 Feb-. [PubMed] |
| 5. | Stefan MS, Pekow PS, Nsa W, Priya A, Miller LE, Bratzler DW, Rothberg MB, Goldberg RJ, Baus K, Lindenauer PK. Hospital performance measures and 30-day readmission rates. J Gen Intern Med. 2013;28:377-385. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 82] [Cited by in RCA: 70] [Article Influence: 5.4] [Reference Citation Analysis (1)] |
| 6. | Dhaliwal JS, Dang AK. Reducing Hospital Readmissions. 2024 Jun 7. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. [PubMed] |
| 7. | Turner SF, Badial V, Barter R, Hayter E, Anakwe RE. Unadjusted Unplanned 30-Day Hospital Readmission Rates are Not a Useful Quality Measure for Planned or Urgent Orthopaedic Inpatient Care: A Retrospective Cohort Study. JB JS Open Access. 2025;10:e24.00237. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 8. | World Health Organization. Malnutrition. 2022. Available from: https://www.who.int/health-topics/malnutrition#tab=tab_1. |
| 9. | Barker LA, Gout BS, Crowe TC. Hospital malnutrition: prevalence, identification and impact on patients and the healthcare system. Int J Environ Res Public Health. 2011;8:514-527. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 736] [Cited by in RCA: 610] [Article Influence: 40.7] [Reference Citation Analysis (1)] |
| 10. | Rasmussen HH, Kondrup J, Staun M, Ladefoged K, Kristensen H, Wengler A. Prevalence of patients at nutritional risk in Danish hospitals. Clin Nutr. 2004;23:1009-1015. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 151] [Cited by in RCA: 141] [Article Influence: 6.4] [Reference Citation Analysis (2)] |
| 11. | Lengfelder L, Mahlke S, Moore L, Zhang X, Williams G 3rd, Lee J. Prevalence and impact of malnutrition on length of stay, readmission, and discharge destination. JPEN J Parenter Enteral Nutr. 2022;46:1335-1342. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 42] [Article Influence: 10.5] [Reference Citation Analysis (1)] |
| 12. | Kabashneh S, Alkassis S, Shanah L, Ali H. A Complete Guide to Identify and Manage Malnutrition in Hospitalized Patients. Cureus. 2020;12:e8486. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.5] [Reference Citation Analysis (1)] |
| 13. | Sharma Y, Miller M, Kaambwa B, Shahi R, Hakendorf P, Horwood C, Thompson C. Malnutrition and its association with readmission and death within 7 days and 8-180 days postdischarge in older patients: a prospective observational study. BMJ Open. 2017;7:e018443. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 63] [Cited by in RCA: 53] [Article Influence: 5.9] [Reference Citation Analysis (1)] |
| 14. | Beck A, Andersen UT, Leedo E, Jensen LL, Martins K, Quvang M, Rask KØ, Vedelspang A, Rønholt F. Does adding a dietician to the liaison team after discharge of geriatric patients improve nutritional outcome: a randomised controlled trial. Clin Rehabil. 2015;29:1117-1128. [PubMed] [DOI] [Full Text] |
| 15. | Mogensen KM, Horkan CM, Purtle SW, Moromizato T, Rawn JD, Robinson MK, Christopher KB. Malnutrition, Critical Illness Survivors, and Postdischarge Outcomes: A Cohort Study. JPEN J Parenter Enteral Nutr. 2018;42:557-565. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 57] [Cited by in RCA: 40] [Article Influence: 5.0] [Reference Citation Analysis (1)] |
| 16. | Yartsev A. Enteral nutrition vs parenteral nutrition in the critically ill. Gastrointestinal Intensive Care. Australia: Deranged Physiology, 2024. |
| 17. | Marx W, Kelly JT, Crichton M, Craven D, Collins J, Mackay H, Isenring E, Marshall S. Is telehealth effective in managing malnutrition in community-dwelling older adults? A systematic review and meta-analysis. Maturitas. 2018;111:31-46. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 79] [Cited by in RCA: 59] [Article Influence: 7.4] [Reference Citation Analysis (4)] |
| 18. | Muscaritoli M, Krznarić Z, Singer P, Barazzoni R, Cederholm T, Golay A, Van Gossum A, Kennedy N, Kreymann G, Laviano A, Pavić T, Puljak L, Sambunjak D, Utrobičić A, Schneider SM. Effectiveness and efficacy of nutritional therapy: A systematic review following Cochrane methodology. Clin Nutr. 2017;36:939-957. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76] [Cited by in RCA: 68] [Article Influence: 7.6] [Reference Citation Analysis (1)] |
| 19. | Blondal BS, Geirsdottir OG, Halldorsson TI, Beck AM, Jonsson PV, Ramel A. HOMEFOOD Randomised Trial - Six-Month Nutrition Therapy in Discharged Older Adults Reduces Hospital Readmissions and Length of Stay at Hospital Up to 18 Months of Follow-Up. J Nutr Health Aging. 2023;27:632-640. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 9] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 20. | Lindegaard Pedersen J, Pedersen PU, Damsgaard EM. Nutritional Follow-Up after Discharge Prevents Readmission to Hospital - A Randomized Clinical Trial. J Nutr Health Aging. 2017;21:75-82. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 47] [Cited by in RCA: 40] [Article Influence: 4.4] [Reference Citation Analysis (1)] |
| 21. | Wyers CE, Reijven PLM, Breedveld-Peters JJL, Denissen KFM, Schotanus MGM, van Dongen MCJM, Eussen SJPM, Heyligers IC, van den Brandt PA, Willems PC, van Helden S, Dagnelie PC. Efficacy of Nutritional Intervention in Elderly After Hip Fracture: A Multicenter Randomized Controlled Trial. J Gerontol A Biol Sci Med Sci. 2018;73:1429-1437. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 52] [Cited by in RCA: 47] [Article Influence: 5.9] [Reference Citation Analysis (1)] |
| 22. | Munk T, Svendsen JA, Knudsen AW, Østergaard TB, Thomsen T, Olesen SS, Rasmussen HH, Beck AM. A multimodal nutritional intervention after discharge improves quality of life and physical function in older patients - a randomized controlled trial. Clin Nutr. 2021;40:5500-5510. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 26] [Article Influence: 5.2] [Reference Citation Analysis (1)] |
| 23. | Sharma Y, Thompson CH, Kaambwa B, Shahi R, Hakendorf P, Miller M. Investigation of the benefits of early malnutrition screening with telehealth follow up in elderly acute medical admissions. QJM. 2017;110:639-647. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 34] [Article Influence: 3.8] [Reference Citation Analysis (1)] |
| 24. | Cramon MØ, Raben I, Beck AM, Andersen JR. Individual nutritional intervention for prevention of readmission among geriatric patients-a randomized controlled pilot trial. Pilot Feasibility Stud. 2021;7:206. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 9] [Article Influence: 1.8] [Reference Citation Analysis (1)] |
| 25. | Buys DR, Campbell AD, Godfryd A, Flood K, Kitchin E, Kilgore ML, Allocca S, Locher JL. Meals Enhancing Nutrition After Discharge: Findings from a Pilot Randomized Controlled Trial. J Acad Nutr Diet. 2017;117:599-608. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 34] [Cited by in RCA: 34] [Article Influence: 3.8] [Reference Citation Analysis (1)] |
| 26. | Yang PH, Lin MC, Liu YY, Lee CL, Chang NJ. Effect of Nutritional Intervention Programs on Nutritional Status and Readmission Rate in Malnourished Older Adults with Pneumonia: A Randomized Control Trial. Int J Environ Res Public Health. 2019;16:4758. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 47] [Cited by in RCA: 43] [Article Influence: 6.1] [Reference Citation Analysis (1)] |
| 27. | Terp R, Jacobsen KO, Kannegaard P, Larsen AM, Madsen OR, Noiesen E. A nutritional intervention program improves the nutritional status of geriatric patients at nutritional risk-a randomized controlled trial. Clin Rehabil. 2018;32:930-941. [PubMed] [DOI] [Full Text] |
| 28. | Beck AM, Kjær S, Hansen BS, Storm RL, Thal-Jantzen K, Bitz C. Follow-up home visits with registered dietitians have a positive effect on the functional and nutritional status of geriatric medical patients after discharge: a randomized controlled trial. Clin Rehabil. 2013;27:483-493. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 83] [Cited by in RCA: 74] [Article Influence: 5.7] [Reference Citation Analysis (1)] |
| 29. | Deer RR, Dickinson JM, Baillargeon J, Fisher SR, Raji M, Volpi E. A Phase I Randomized Clinical Trial of Evidence-Based, Pragmatic Interventions to Improve Functional Recovery After Hospitalization in Geriatric Patients. J Gerontol A Biol Sci Med Sci. 2019;74:1628-1636. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 23] [Article Influence: 3.3] [Reference Citation Analysis (1)] |
| 30. | Tan PC, Ramasandran G, Sethi N, Razali N, Hamdan M, Kamarudin M. Watermelon and dietary advice compared to dietary advice alone following hospitalization for hyperemesis gravidarum: a randomized controlled trial. BMC Pregnancy Childbirth. 2023;23:450. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 31. | Ferraris C, De Amicis R. Editorial: Nutritional counseling for lifestyle modification. Front Nutr. 2024;11:1472316. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 32. | National Council on Aging. What is nutrition counseling? 2024. Available from: https://www.ncoa.org/article/what-is-nutrition-counseling-is-it-right-for-me/. |
| 33. | Vasiloglou MF, Fletcher J, Poulia KA. Challenges and Perspectives in Nutritional Counselling and Nursing: A Narrative Review. J Clin Med. 2019;8:1489. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 62] [Cited by in RCA: 48] [Article Influence: 6.9] [Reference Citation Analysis (1)] |
| 34. | Maneesing TU, Dawangpa A, Chaivanit P, Songsakul S, Prasertsri P, Yumi Noronha N, Watanabe LM, Nonino CB, Pratumvinit B, Sae-Lee C. Optimising blood glucose control with portioned meal box in type 2 diabetes mellitus patients: a randomised control trial. Front Nutr. 2023;10:1216753. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 2] [Article Influence: 0.7] [Reference Citation Analysis (1)] |
| 35. | Klein L, Parks K. Home Meal Preparation: A Powerful Medical Intervention. Am J Lifestyle Med. 2020;14:282-285. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 7] [Article Influence: 1.2] [Reference Citation Analysis (1)] |
| 36. | Ducrot P, Méjean C, Aroumougame V, Ibanez G, Allès B, Kesse-Guyot E, Hercberg S, Péneau S. Meal planning is associated with food variety, diet quality and body weight status in a large sample of French adults. Int J Behav Nutr Phys Act. 2017;14:12. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 93] [Cited by in RCA: 77] [Article Influence: 8.6] [Reference Citation Analysis (1)] |
| 37. | Ingstad K, Uhrenfeldt L, Kymre IG, Skrubbeltrang C, Pedersen P. Effectiveness of individualised nutritional care plans to reduce malnutrition during hospitalisation and up to 3 months post-discharge: a systematic scoping review. BMJ Open. 2020;10:e040439. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 13] [Article Influence: 2.2] [Reference Citation Analysis (1)] |
| 38. | Shyam S, Lee KX, Tan ASW, Khoo TA, Harikrishnan S, Lalani SA, Ramadas A. Effect of Personalized Nutrition on Dietary, Physical Activity, and Health Outcomes: A Systematic Review of Randomized Trials. Nutrients. 2022;14:4104. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 62] [Cited by in RCA: 32] [Article Influence: 8.0] [Reference Citation Analysis (1)] |
| 39. | Stratton RJ, Hébuterne X, Elia M. A systematic review and meta-analysis of the impact of oral nutritional supplements on hospital readmissions. Ageing Res Rev. 2013;12:884-897. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 153] [Cited by in RCA: 127] [Article Influence: 9.8] [Reference Citation Analysis (1)] |
| 40. | Baillargeon J, Deer RR, Kuo YF, Zhang D, Goodwin JS, Volpi E. Androgen Therapy and Rehospitalization in Older Men With Testosterone Deficiency. Mayo Clin Proc. 2016;91:587-595. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 0.6] [Reference Citation Analysis (1)] |
| 41. | Donovitz GS. A Personal Prospective on Testosterone Therapy in Women-What We Know in 2022. J Pers Med. 2022;12:1194. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 12] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 42. | Huang LT, Wang JH. The Therapeutic Intervention of Sex Steroid Hormones for Sarcopenia. Front Med (Lausanne). 2021;8:739251. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 42] [Cited by in RCA: 38] [Article Influence: 7.6] [Reference Citation Analysis (0)] |
| 43. | Fulgoni K, Fulgoni VL 3rd. Watermelon Intake Is Associated with Increased Nutrient Intake and Higher Diet Quality in Adults and Children, NHANES 2003-2018. Nutrients. 2022;14:4883. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 3] [Article Influence: 0.8] [Reference Citation Analysis (1)] |
| 44. | Figueroa A, Sanchez-Gonzalez MA, Wong A, Arjmandi BH. Watermelon extract supplementation reduces ankle blood pressure and carotid augmentation index in obese adults with prehypertension or hypertension. Am J Hypertens. 2012;25:640-643. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75] [Cited by in RCA: 57] [Article Influence: 4.1] [Reference Citation Analysis (4)] |
| 45. | Massa NM, Silva AS, de Oliveira CV, Costa MJ, Persuhn DC, Barbosa CV, Gonçalves MD. Supplementation with Watermelon Extract Reduces Total Cholesterol and LDL Cholesterol in Adults with Dyslipidemia under the Influence of the MTHFR C677T Polymorphism. J Am Coll Nutr. 2016;35:514-520. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 25] [Article Influence: 2.5] [Reference Citation Analysis (0)] |