Published online Mar 18, 2026. doi: 10.13105/wjma.v14.i1.113251
Revised: October 8, 2025
Accepted: December 11, 2025
Published online: March 18, 2026
Processing time: 202 Days and 18.3 Hours
Incisional hernia (IH) is a common late complication following orthotopic liver transplantation, with reported incidences up to 46%. Incision type, particularly the use of the Mercedes incision, has been implicated as a modifiable risk factor due to its midline component and associated fascial disruption.
To determine whether the Mercedes incision increases the risk of IH compared with Chevron and J-shaped incisions in adult liver transplant recipients.
We conducted a systematic review and meta-analysis in accordance with PRISMA 2020 guidelines (PROSPERO: CRD42020161632). PubMed, MEDLINE, EMBASE, Google Scholar, and Cochrane Library were searched up to June 2025 for studies reporting IH incidence stratified by incision type. Observational studies with ≥ 12 months follow-up in adults were included. Random-effects meta-analysis was performed to estimate pooled odds ratios (OR) with 95%CI. Heterogeneity was assessed using the I² statistic. Exploratory subgroup analyses examined closure technique, incision closure approach, and suture material.
Eight observational studies (n = 2965) met the inclusion criteria. Pooled analysis showed the Mercedes incision was associated with a higher IH risk compared with Chevron or J-shaped incisions (OR = 1.93, 95%CI: 1.06–3.51; I² = 76%). Sensitivity analysis excluding a zero-event study reduced the OR to 1.79 (95%CI: 0.99–3.25). Single-layer closure (OR = 3.75, 95%CI: 2.22–6.35) and absorbable sutures (OR = 3.06, 95%CI: 1.18–7.93) were associated with increased IH rates in exploratory analyses.
The Mercedes incision is likely associated with a higher risk of IH after liver transplantation compared with Chevron or J-shaped incisions. Surgical planning should consider incision type alongside patient and technical factors to reduce long-term abdominal wall morbidity.
Core Tip: This systematic review and meta-analysis of 2965 liver transplant recipients demonstrates that the Mercedes incision increases the risk of incisional hernia compared with Chevron or J-shaped incisions. The midline extension inherent to the Mercedes approach may contribute to fascial weakness. Technical factors such as two-layer closure and use of non-absorbable sutures may reduce this risk. Incision choice should be individualized to balance optimal surgical exposure with preservation of long-term abdominal wall integrity.
- Citation: Kanchustambam SRV, Peters PA, True H, Jones BG. Mercedes incision and risk of incisional hernia following liver transplantation: A systematic review. World J Meta-Anal 2026; 14(1): 113251
- URL: https://www.wjgnet.com/2308-3840/full/v14/i1/113251.htm
- DOI: https://dx.doi.org/10.13105/wjma.v14.i1.113251
Incisional hernias (IH) remain a prevalent late complication following orthotopic liver transplantation (OLT), with reported incidences ranging from 5% to 46%[1]. These hernias can lead to pain, bowel obstruction, impaired quality of life, and frequently necessitate surgical repair in a patient population already burdened by immunosuppression and complex postoperative care. The development of IH following liver transplantation poses a significant clinical challenge, impacting patient morbidity, healthcare costs, and long-term outcomes[2].
The development of IH is multifactorial. Patient-related risk factors include obesity, poor nutritional status, immunosuppressive therapy, and prior abdominal surgery[3]. Technical factors, particularly the type of abdominal incision and closure technique, also play a crucial role in influencing postoperative abdominal wall integrity[4]. In particular, midline incisions, often used in liver transplantation for optimal exposure, have been historically associated with higher IH rates compared to transverse incisions[1]. Understanding the interplay between incision type, patient characteristics, and surgical technique is crucial for developing strategies to minimize IH formation after liver trans
This study aims to systematically evaluate the incidence of IH in adult patients undergoing liver transplantation using Mercedes, Chevron, or J-shaped incisions. The primary objective is to assess whether the Mercedes incision increases IH risk in comparison to the Chevron or J-shaped incision. In addition, we explore secondary technical variables, including closure technique and suture material, with the aim of supporting more informed surgical decision-making and identifying directions for future research.
The Mercedes incision, a bilateral subcostal incision with a vertical midline extension, has been widely adopted in liver transplantation due to its superior operative exposure. However, its association with increased midline tension and more extensive fascial disruption has raised concerns about a higher risk of IH[5]. Alternatives such as the Chevron incision (bilateral subcostal without midline extension) and the J-shaped incision (right subcostal with midline extension) are increasingly used in some centers, offering comparable access with a potentially lower risk of hernia formation[6]. The J-shaped right subcostal incision, known for its good exposure during partial hepatectomy, may be associated with less morbidity.
Despite the clinical relevance of IH post-liver transplantation and the importance of incision choice, there remains no consensus on the optimal incision to minimize hernia risk[2]. Most of the existing literature comprises small, retrospective series with heterogeneous outcomes and follow-up durations. To date, no systematic review and meta-analysis has quantitatively compared IH incidence across these commonly used incision types.
This systematic review and meta-analysis was conducted in accordance with the PRISMA 2020 guidelines and was registered with PROSPERO (CRD42020161632).
We searched PubMed, MEDLINE, EMBASE, Google Scholar, and the Cochrane Library using MeSH terms and keywords including “liver transplantation”, “incisional hernia”, “Mercedes incision”, “Chevron incision”, “J incision”, “subcostal incision”, and “laparotomy”. The search was conducted up to June 2025.
Eligibility criteria: Studies were eligible if they reported IH incidence after liver transplantation, stratified by incision type (Mercedes, Chevron, or J-shaped). Studies were eligible for inclusion if they met the following PICO-based criteria: Population: Adult patients (≥ 18 years) undergoing OLT.
Intervention/exposure: Mercedes (inverted ‘Y’ subcostal) incision. Comparator: Chevron or J-shaped right subcostal incisions. Outcome: Incidence of IH, as diagnosed clinically or radiologically, with a minimum follow-up of 12 months.
Study design: Retrospective or prospective observational studies published in peer-reviewed journals. Exclusion criteria included case reports, reviews, animal studies, studies involving non-adult populations, or those lacking incision-type differentiation. Patients with more than one organ transplanted were also excluded from this review.
Three reviewers independently extracted data on study design, patient demographics, incision types, hernia incidence, follow-up duration, and risk of bias. Disagreements were resolved through consensus. The quality of included studies was assessed using the Methodological Index for Non-Randomized Studies (MINORS) criteria.
The primary outcome was the incidence of IH following liver transplantation. Subgroup analyses were conducted to explore variation in hernia incidence by incision type (Mercedes vs Chevron vs J-shaped). Additional exploratory subgroup comparisons included closure technique (single vs two-layer), incision closure approach (open vs mixed), and suture material (absorbable vs. non-absorbable). These subgroup findings were reported descriptively due to heterogeneity and incomplete reporting across studies.
The primary outcome was the development of an IH following liver transplantation. Diagnosis was based on clinical examination, radiological imaging (e.g., ultrasound or CT), or surgical re-exploration, as reported in the included studies. Most studies defined IH as any abdominal wall defect detected at or near the transplant incision site during the follow-up period, with a minimum follow-up of 12 months to ensure adequate capture of late-presenting hernias.
Random-effects meta-analysis using DerSimonian and Laird methodology was performed to estimate pooled odds ratios (OR) with 95%CI. Heterogeneity was assessed using the I² statistic. Sensitivity analysis was performed excluding studies with extreme or zero-event data. Forest plots were generated to visualize the results.
MINORS tool. This validated instrument assigns a score out of 24 based on 12 criteria including study aim, inclusion of consecutive patients, follow-up, endpoint assessment, and statistical analysis. The included studies demonstrated moderate-to-good quality with scores ranging from 15 to 21 out of a maximum of 24 (Table 1).
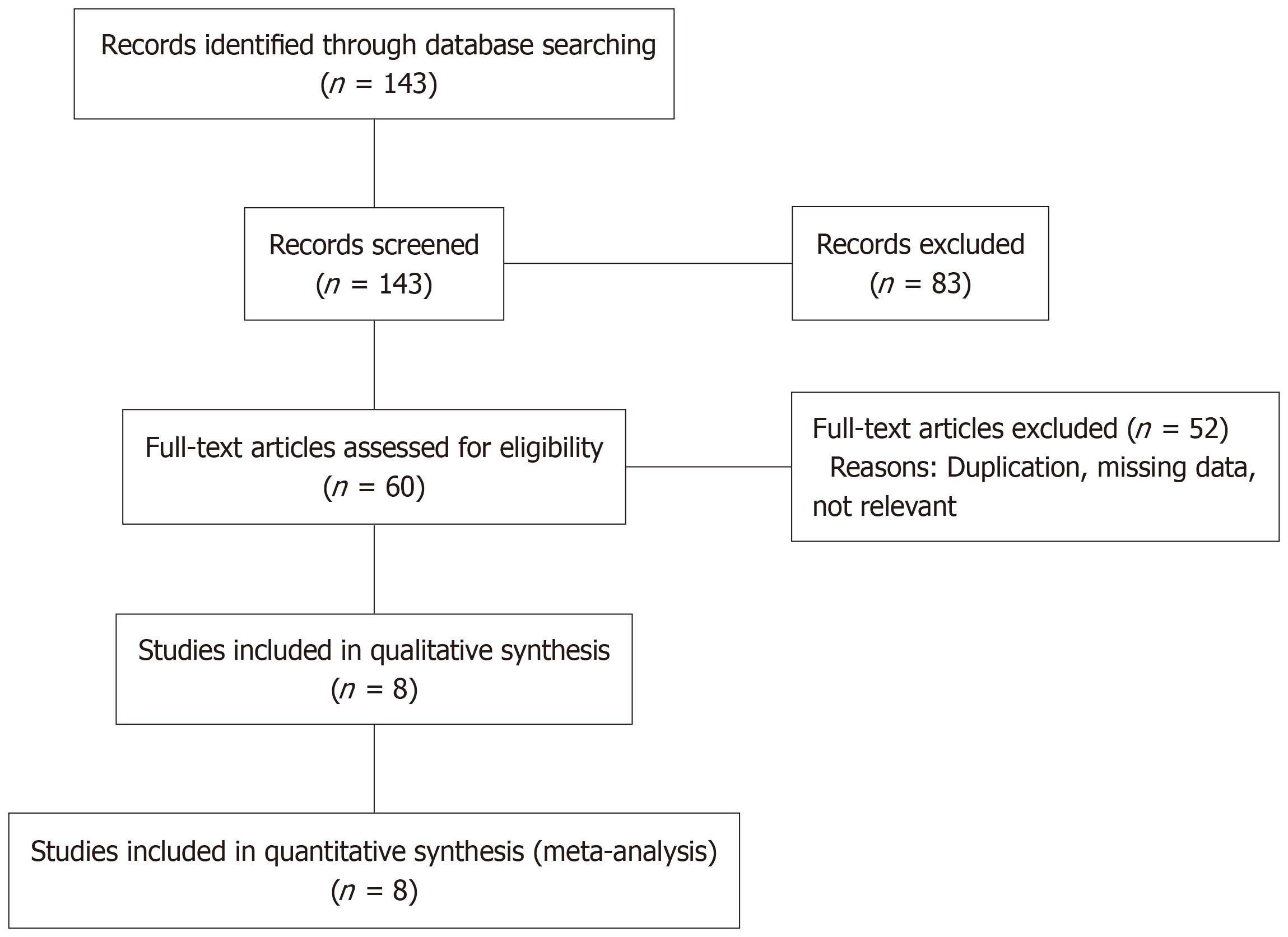
The initial search identified 143 articles. After removing irrelevant studies and screening full texts, 8 studies met the eligibility criteria for quantitative synthesis. These studies included 2965 patients undergoing liver transplantation, with varying proportions undergoing Mercedes incisions (1971), and Chevron or J-shaped incisions (994). We did not identify any randomized trials. The mean follow-up ranged from 12 months to 48 months. All studies were observational in design, and study quality was moderate (Figure 1).
A summary of key study-level features is presented in Table 2, including design, sample size, incision types compared, and IH outcomes (Table 2).
| Reference | Design | Sample size | Follow-up | Incision type | Incisional hernia rate |
| Perrakis et al[1] (2020) | Retrospective cohort | 176 | Mean 42 months | Mercedes vs chevron | 32.4% vs 19.3% |
| Cos et al[2] (2020) | Retrospective cohort | 231 | Median 36 months | Mercedes vs J-shaped | 27.5% vs 15.6% |
| Nevo et al[3] (2024) | Retrospective cohort | 312 | Mean 24 months | Mercedes vs chevron | 29.2% vs 18.4% |
| Garmpis et al[4] (2019) | Review-based cohort | 150 | Not stated | Various | 35.0% (overall) |
| Butler et al[5] (2020) | Systematic review/meta-analysis | 891 (aggregated) | Varied | Various | Range: 5%–38% |
| Smith et al[6] (2024) | Retrospective cost analysis | 210 | 12 months | Mixed | 25.2% overall |
| Donataccio et al[7] (2006) | Prospective feasibility | 120 | 12–18 months | Right subcostal (J) | 12.5% |
| Zarbaliyev et al[10] (2021) | Retrospective comparative | 195 | 24 months | Mercedes vs J-shaped | 28.4% vs 16.7% |
Meta-analysis of IH incidence showed a trend towards higher odds of IH formation with the Mercedes incision compared to the Chevron or J-shaped incisions. Specifically, one study showed that IH frequently occur at the junction of midline and transverse incisions[7].
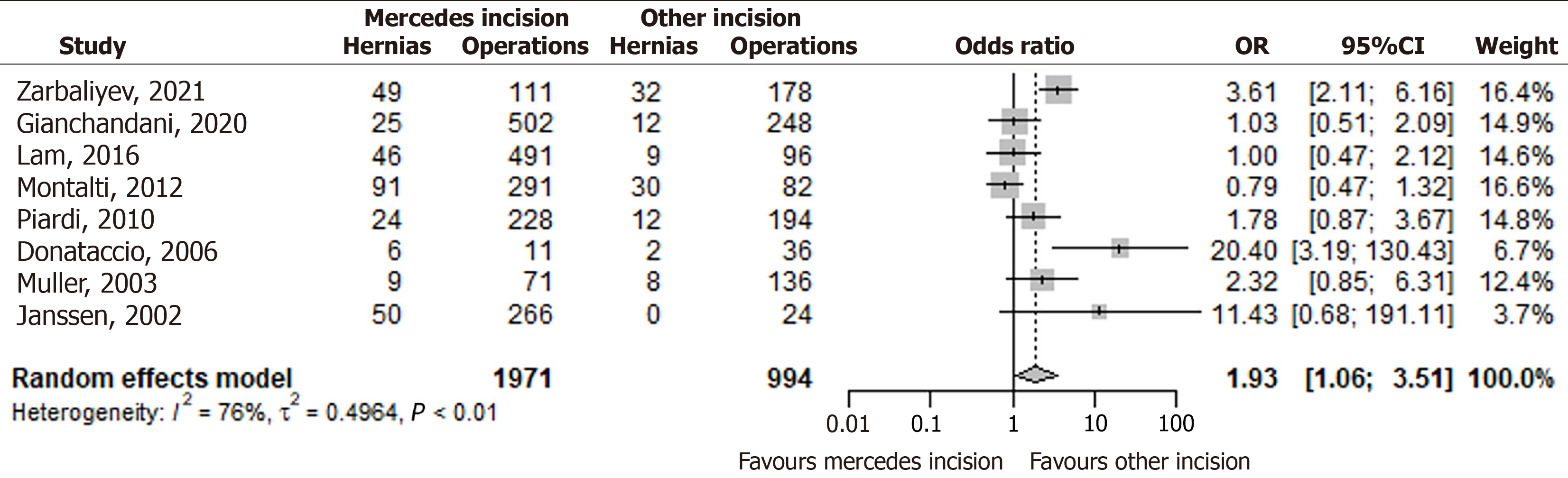
Pooled meta-analysis demonstrated a significantly higher risk of IH with the Mercedes incision compared to Chevron or J incisions (Figure 2): OR: 1.93 (95%CI: 1.06–3.51). Heterogeneity: I² = 76%.
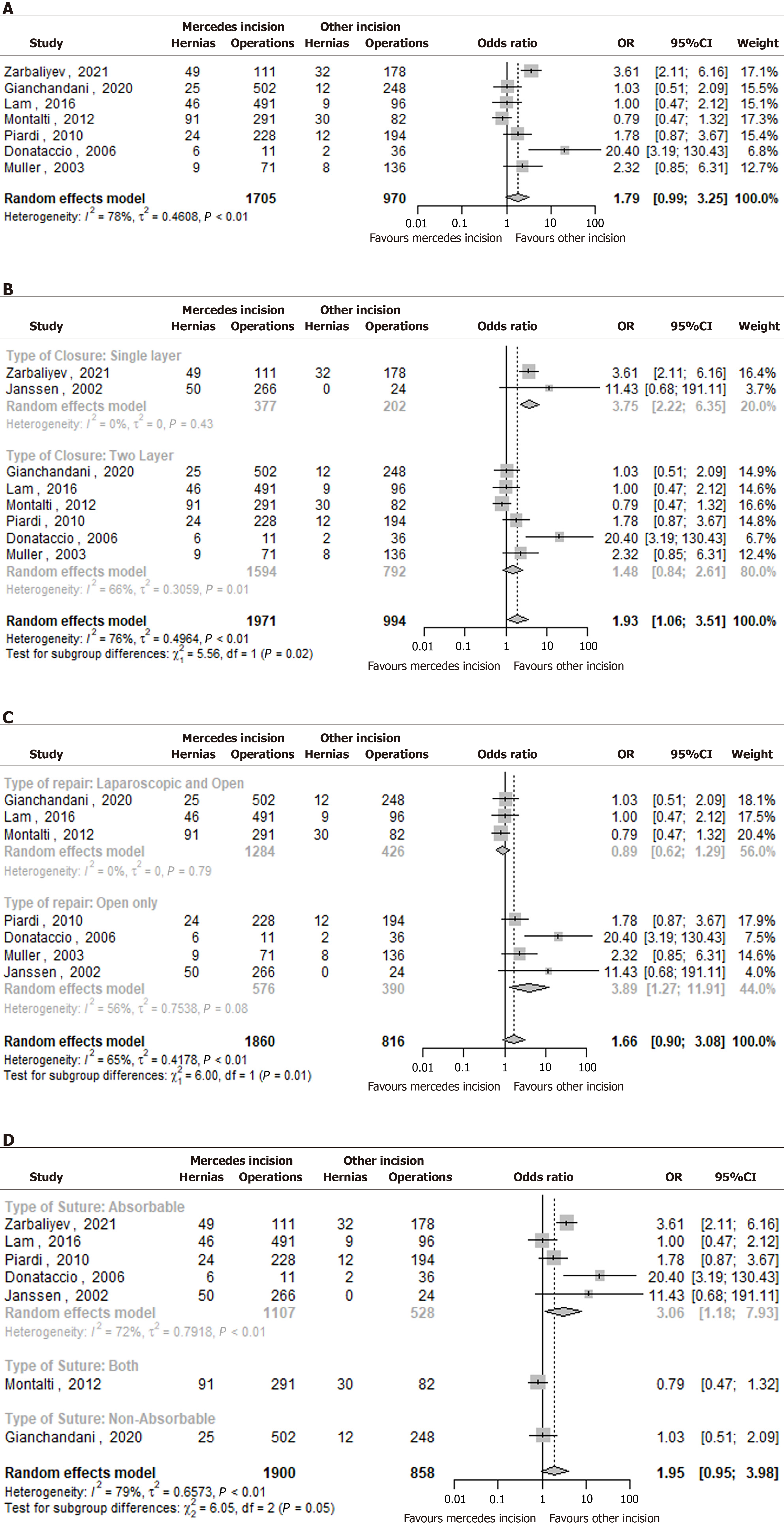
Exclusion of Janssen et al[8], which reported no IH events in the comparator group, resulted in a reduced but still elevated OR of 1.79 (95%CI: 0.99–3.25) (Figure 3A).
The increased risk of IH associated with the Mercedes incision appeared greater among studies using single-layer closure (OR = 3.75, 95%CI: 2.22–6.35), compared to those using two-layer closure (OR = 1.48, 95%CI: 0.84–2.61) (Figure 3B).
The risk associated with the Mercedes incision was higher in studies where open techniques were used for hernia repair (OR = 3.89, 95%CI: 1.27–11.91), compared to those using mixed repair approaches (OR = 0.89, 95%CI: 0.62–1.29) (Figure 3C).
Studies using absorbable suture materials showed a higher risk of IH associated with the Mercedes incision (OR = 3.06, 95%CI: 1.18–7.93), though the data were limited and heterogeneity was high (Figure 3D): These subgroup findings are exploratory and should be interpreted cautiously due to inconsistency and heterogeneity among studies.
This systematic review and meta-analysis demonstrates that the Mercedes incision is associated with a higher incidence of IH following liver transplantation compared to Chevron or J-shaped incisions. This finding corroborates prior single-center observations and now provides pooled evidence across a broader dataset.
The increased hernia risk with the Mercedes incision may be attributed to the greater fascial disruption and higher tension along the midline component of the incision. The observed association aligns with evidence from general surgery, where midline incisions have been linked to elevated hernia rates[9]. However, the high degree of heterogeneity highlights the variability in surgical techniques and patient populations across studies.
The rationale for avoiding midline extension, as in the Mercedes incision, is further supported by recent literature. A 2022 cohort study by Zarbaliyev et al[10] confirmed that the J-shaped incision is associated with a significantly lower risk of IH without compromising surgical exposure. These findings have contributed to the increasing adoption of J incisions in donor hepatectomies and selected transplant cases, offering a balance between operative visibility and long-term abdominal wall integrity.
Moreover, a recent meta-analysis by Butler et al[5] reported a pooled IH incidence of 15.1% across 981 patients, with a mean time to IH development of 42.9 months. This underscores the chronic nature of this complication and highlights the need for long-term vigilance. Notably, midline components of incisions remain particularly susceptible to herniation, reinforcing the biomechanical disadvantage of the Mercedes approach.
While this meta-analysis focuses primarily on incision type, technical factors such as closure technique and suture material may further modulate IH risk. Our exploratory subgroup analysis suggests that single-layer closure and absorbable sutures are associated with increased IH rates due to the Mercedes incision relative to others. These findings align with emerging studies reporting that running non-absorbable sutures (e.g., PDS loop) may provide superior fascial strength and reduce herniation rates[11].
Closure technique: The findings highlight the possibility that single-layer closure may exacerbate the risk associated with the Mercedes incision, though residual confounding factors cannot be excluded. The observed difference in OR between single- and two-layer closures suggests a potential interaction rather than a direct causal effect of closure technique alone.
Repair type: Similarly, the increased risk seen in studies utilizing open hernia repair techniques may suggest that open repairs are more frequently associated with negative outcomes of Mercedes incisions. This observation may also reflect underlying differences in surgical practice or patient selection criteria across centers.
Suture material: The subgroup analysis involving suture materials suggests a possible interaction between absorbable sutures and incision type, with studies using absorbable materials showing a higher risk of IH in the Mercedes group. However, due to limited data and high heterogeneity, these findings should be interpreted with caution and require further validation.
Additionally, several patient-specific risk factors, including diabetes mellitus, hypoalbuminemia, high body mass index (BMI), and surgical site infections, are now well-established contributors to IH formation. A recent single-center study emphasized that minimizing intraoperative blood loss, limiting transfusions, and early postoperative ascites management can reduce IH risk. In cases requiring re-laparotomy, reinforced fascial reconstruction may be prudent[6]. These should be considered potential confounders. High BMI has consistently been associated with increased intra-abdominal pressure and impaired wound healing[12]. Similarly, diabetes mellitus impairs collagen synthesis and angiogenesis, both of which are critical to fascia closure. Chronic immunosuppressive therapy, a mainstay of post-transplant management, may further reduce tissue integrity and delay healing[13]. The presence of ascites can exert persistent tension on the abdominal wall and incision site, increasing mechanical stress during the recovery period. Lastly, surgical site infections or superficial wound infections are well-established contributors to early fascial dehiscence and subsequent hernia formation[14,15]. These factors were variably reported across the included studies and may partly explain the heterogeneity in IH rates.
Despite these insights, interpretation of our findings must consider several limitations. All included studies were observational, with variable definitions of IH and heterogeneous follow-up durations. The high statistical heterogeneity (I² = 76%) indicates variability in outcomes and methodology. Moreover, our sensitivity analysis revealed that exclusion of a single zero-event study (Janssen et al[8]) reduced the pooled effect size and led to borderline statistical significance, underscoring the fragility of the estimate.
The consistent trend across multiple studies, now supported by recent evidence, suggests that incision type should be a deliberate factor in surgical planning. While the Mercedes incision offers excellent exposure, particularly in complex vascular reconstructions, the trade-off with increased IH risk is clinically meaningful, especially in high-risk patients. The results indicate that the Mercedes incision may be associated with a higher risk of IH compared to Chevron or J-shaped incisions following liver transplantation, which aligns with other studies that the incidence rates of IH have varied from 0%-33%[12]. However, this association should be interpreted with caution due to the high degree of heterogeneity among included studies, variability in follow-up duration, and the influence of patient- and technique related confounders.
Future high-quality prospective studies, ideally randomized or leveraging high-quality transplant registries, are essential to confirm these associations. Investigations should also explore whether mesh prophylaxis, advanced closure techniques, or personalized incision selection based on risk profiling can improve long-term outcomes.
The authors would like to thank the East Lancashire Hospitals NHS Trust Library Services for their assistance with the literature search strategy.
| 1. | Perrakis A, Knüttel D, Rahimli M, Andric M, Croner RS, Vassos N. Incisional hernia after liver transplantation: mesh-based repair and what else? Surg Today. 2021;51:733-737. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 16] [Article Influence: 3.2] [Reference Citation Analysis (1)] |
| 2. | Cos H, Ahmed O, Garcia-Aroz S, Vachharajani N, Shenoy S, Wellen JR, Doyle MM, Chapman WC, Khan AS. Incisional hernia after liver transplantation: Risk factors, management strategies and long-term outcomes of a cohort study. Int J Surg. 2020;78:149-153. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 22] [Article Influence: 3.7] [Reference Citation Analysis (2)] |
| 3. | Nevo N, Jacover A, Nizri E, Cuccurullo D, Rispoli C, Pery R, Elizur Y, Horesh N, Eshkenazy R, Nachmany I, Pencovich N. Linking factors to incisional hernia following pancreatic surgery: a 14-year retrospective analysis. Hernia. 2024;28:1397-1404. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 4. | Garmpis N, Spartalis E, Schizas D, Patsouras D, Damaskos C, Spartalis M, Garmpi A, Nikiteas NI, Dimitroulis D. Incisional Hernias Post Liver Transplantation: Current Evidence of Epidemiology, Risk Factors and Laparoscopic Versus Open Repair. A Review of the Literature. In Vivo. 2019;33:1059-1066. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 28] [Cited by in RCA: 27] [Article Influence: 3.9] [Reference Citation Analysis (7)] |
| 5. | Butler JR, O'Brien DC, Kays JK, Kubal CA, Ekser B, Fridell JA, Mangus RS, Powelson JA. Incisional Hernia After Orthotopic Liver Transplantation: A Systematic Review and Meta-analysis. Transplant Proc. 2021;53:255-259. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 19] [Article Influence: 3.8] [Reference Citation Analysis (1)] |
| 6. | Smith L, Wilkes E, Rolfe C, Westlake P, Cornish J, Brooks P, Torkington J. Incidence, Healthcare Resource Use and Costs Associated With Incisional Hernia Repair. J Abdom Wall Surg. 2024;3:12452. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 12] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 7. | Donataccio M, Genco B, Donataccio D. Right subcostal incision in liver transplantation: prospective study of feasibility. Transplant Proc. 2006;38:1109-1110. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 18] [Article Influence: 0.9] [Reference Citation Analysis (2)] |
| 8. | Janssen H, Lange R, Erhard J, Malagó M, Eigler FW, Broelsch CE. Causative factors, surgical treatment and outcome of incisional hernia after liver transplantation. Br J Surg. 2002;89:1049-1054. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 58] [Article Influence: 2.4] [Reference Citation Analysis (1)] |
| 9. | Brown SR, Goodfellow PB. Transverse verses midline incisions for abdominal surgery. Cochrane Database Syst Rev. 2005;2005:CD005199. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 72] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 10. | Zarbaliyev E, Sevmiş M, Kilercik H, Çelik S, Aktaş S, Çağlıkülekçi M, Sevmiş Ş. Is the incision type important for the development of hernia in liver transplant patients? Clin Transplant. 2022;36:e14497. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 11. | Sarkar J, Minarich MJ, Smucker LY, Hardy AN, Schwarz RE. Low incisional hernia incidence using a large-bite, low-tension technique for celiotomy closure. Surg Open Sci. 2023;13:94-98. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 2] [Article Influence: 0.7] [Reference Citation Analysis (1)] |
| 12. | Piazzese E, Montalti R, Beltempo P, Bertelli R, Puviani L, Pacilè V, Nardo B, Cavallari A. Incidence, predisposing factors, and results of surgical treatment of incisional hernia after orthotopic liver transplantation. Transplant Proc. 2004;36:3097-3098. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 54] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 13. | Lu H, Zheng P, Chen RY, Chen M. Analysis of risk factors for impaired wound healing after kidney transplantation. Int Wound J. 2023;20:140-144. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (1)] |
| 14. | Xu G, Hou B, Xue C, Xu Q, Qu L, Hao X, Liu Y, Wang D, Li Z, Jin X. Acute Retinal Necrosis Associated with Pseudorabies Virus Infection: A Case Report and Literature Review. Ocul Immunol Inflamm. 2024;32:594-601. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 12] [Article Influence: 6.0] [Reference Citation Analysis (1)] |